Building a Parkinson-Network–Experiences from Germany
Abstract
1. Introduction
2. Methods
3. Results
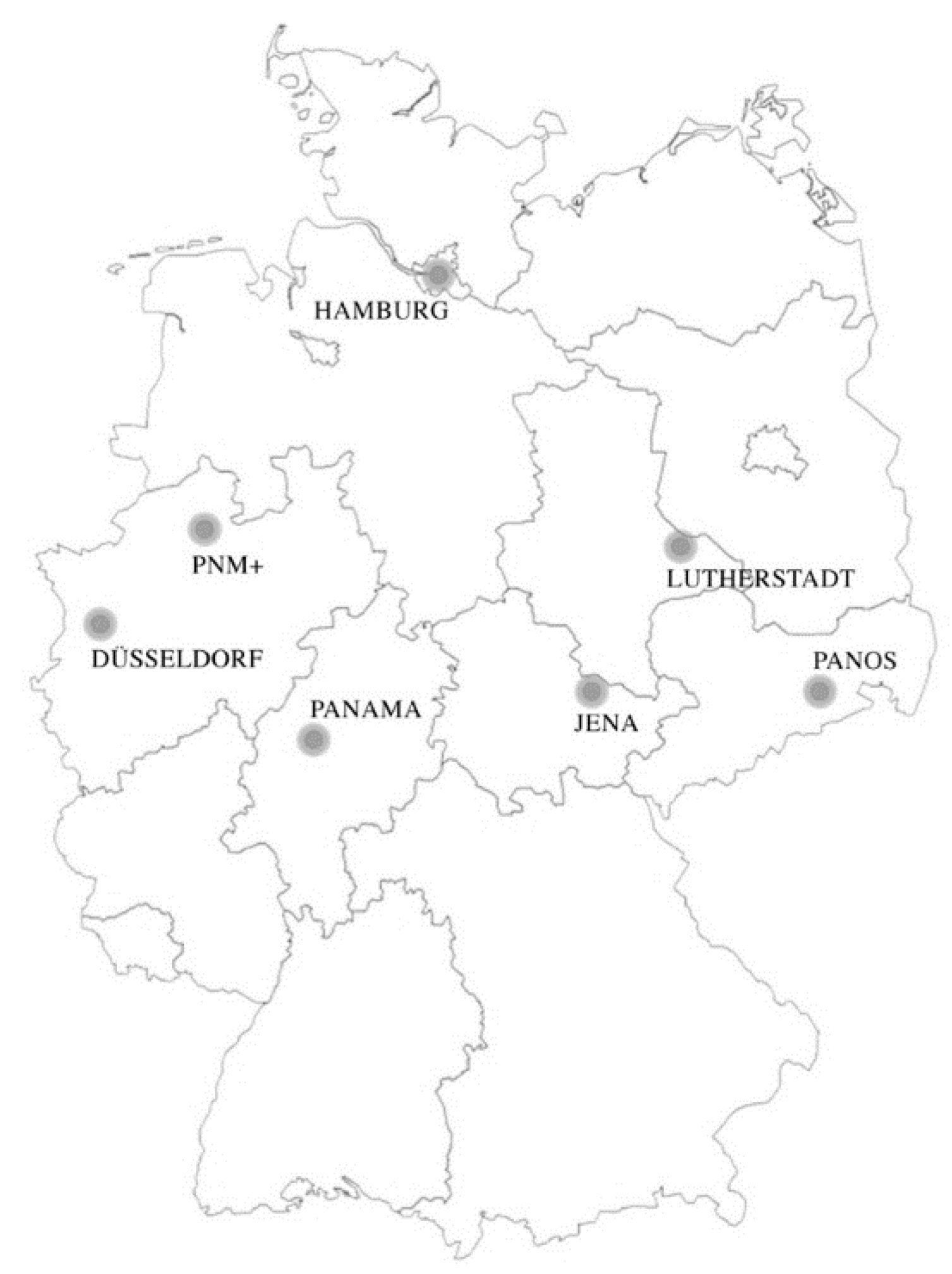
3.1. Parkinson-Networks in Germany
3.1.1. Hamburg (Satellite Network Hamburg)
3.1.2. Lutherstadt (Parkinson Network Central Germany)
3.1.3. Jena
3.1.4. Düsseldorf
3.1.5. Münster and Osnabrück (Parkinson Network Münsterland+; PNM+)
3.1.6. East Saxony (Parkinson Network East Saxony; PANOS)
3.1.7. Marburg (Parkinson Network Alliance Marburg; PANAMA)
3.2. Network Modules
3.2.1. Deep Brain Stimulation Consultation
3.2.2. Evaluation
3.2.3. Financing Strategies
3.2.4. Homepage
3.2.5. Multi-Disciplinary Plenary Meetings
3.2.6. Multimodal Complex Treatment
3.2.7. Online Communication Platform
3.2.8. Outpatient Video-Supported Therapy
3.2.9. Parkinson Academy
3.2.10. Parkinson Assistant (PASS) Training
3.2.11. Parkinson Board
3.2.12. Parkinson Nurse
3.2.13. Parkinson Summer Festival
3.2.14. Parkinson Symposium
3.2.15. Parkinson’s Info-Cafe
3.2.16. Quickcards
3.2.17. Regional Demand Analysis and Target Formulation
3.2.18. Regional Public Relations
3.2.19. Regional Utilities Atlas
3.2.20. Rehab
3.2.21. Standardized Treatment Path
3.2.22. Steering Committee
3.2.23. Structured Patient School according to the Self-Management Concept
3.2.24. Virtual Visits
3.2.25. Working Group
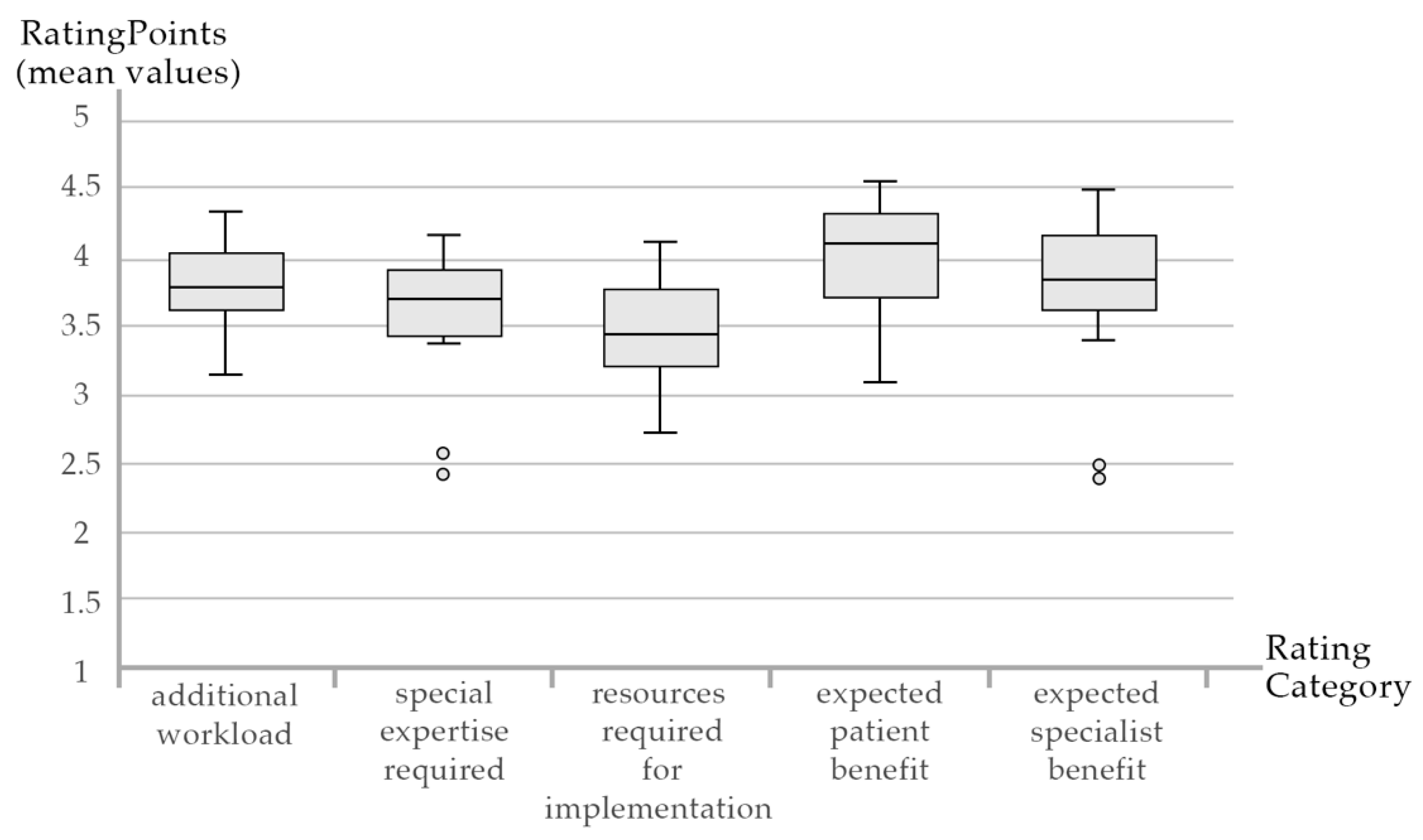
3.3. Expert Rating
4. Discussion
- The purpose and focus of a network may vary across time and settings, but all aspects of integrated care should be covered in a network.
- When building or expanding a network module may be a valuable tool for orientation and priority may be given to modules with the best resource-benefit ratio.
- Fostering knowledge exchange and strengthening commitment are essential during each phase of development and sound project management should be present within each network.
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Dorsey, E.R.; Bloem, B.R. The Parkinson pandemic—A call to action. JAMA Neurol. 2018, 75, 9–10. [Google Scholar] [CrossRef]
- Nerius, M.; Fink, A.; Doblhammer, G. Parkinson’s disease in Germany: Prevalence and incidence based on health claims data. Acta Neurol. Scand. 2017, 136, 386–392. [Google Scholar] [CrossRef] [PubMed]
- Federal Statistical Office Deaths, Cases per 100,000 Inhabitants (Age-Standardized) (from 1998). Available online: http://www.gbe-bund.de/oowa921-install/servlet/oowa/aw92/dboowasys921.xwdevkit/xwd_init?gbe.isgbetol/xs_start_neu/&p_aid=i&p_aid=15887793&nummer=6&p_sprache=E&p_indsp=38758141&p_aid=94182765 (accessed on 10 August 2020).
- Dorsey, E.R.; Constantinescu, R.; Thompson, J.P.; Biglan, K.M.; Holloway, R.G.; Kieburtz, K.; Marshall, F.J.; Ravina, B.M.; Schifitto, G.; Siderowf, A.; et al. Projected number of people with Parkinson disease in the most populous nations, 2005 through 2030. Neurology 2007, 68, 384–386. [Google Scholar] [CrossRef] [PubMed]
- Heinzel, S.; Berg, D.; Binder, S.; Ebersbach, G.; Hickstein, L.; Herbst, H.; Lorrain, M.; Wellach, I.; Maetzler, W.; Petersen, G.; et al. Do We Need to Rethink the Epidemiology and Healthcare Utilization of Parkinson’s Disease in Germany? Front. Neurol. 2018, 9, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Kalia, L.V.; Kalia, S.K.; Lang, A.E. Disease-modifying strategies for Parkinson’s disease. Mov. Disord. 2015, 30, 1442–1450. [Google Scholar] [CrossRef] [PubMed]
- Stangl, S.; Haas, K.; Eggers, C.; Reese, J.P.; Tönges, L.; Volkmann, J. Care of patients with Parkinson’s disease in Germany. Nervenarzt 2020. [Google Scholar] [CrossRef]
- Stember, M. Advancing the social sciences through the interdisciplinary enterprise. Soc. Sci. J. 1991, 28, 1–14. [Google Scholar] [CrossRef]
- Goodwin, N. Understanding Integrated Care. Int. J. Integr. Care 2016, 16. [Google Scholar] [CrossRef]
- Goodwin, N.; Stein, V.; Amelung, V. What Is Integrated Care? In Handbook Integrated Care; Amelung, V., Stein, V., Goodwin, N., Balicer, R., Nolte, E., Suter, E., Eds.; Springer International Publishing: Cham, Switzerland, 2017; pp. 3–23. [Google Scholar]
- Eggers, C.; Dano, R.; Schill, J.; Fink, G.R.; Hellmich, M.; Timmermann, L.; Adams, S.; Assmann, K.; Böhme, A.; Bonmann, E.; et al. Patient-centered integrated healthcare improves quality of life in Parkinson’s disease patients: A randomized controlled trial. J. Neurol. 2018, 265, 764–773. [Google Scholar] [CrossRef]
- Rajan, R.; Brennan, L.; Bloem, B.R.; Dahodwala, N.; Gardner, J.; Goldman, J.G.; Grimes, D.A.; Iansek, R.; Kovács, N.; McGinley, J.; et al. Integrated Care in Parkinson’s Disease: A Systematic Review andMeta-Analysis. Mov. Disord. 2020, 708. [Google Scholar] [CrossRef]
- Binder, S.; Groppa, S.; Woitalla, D.; Müller, T.; Wellach, I.; Klucken, J.; Eggers, C.; Liersch, S.; Amelung, V.E. Patients’ Perspective on Provided Health Services in Parkinson’s Disease in Germany—A Cross-Sectional Survey. Aktuelle Neurol. 2018, 45, 703–713. [Google Scholar] [CrossRef]
- WHO. Integrated Care Models: An Overview Working Document. 2016. Available online: https://www.euro.who.int/__data/assets/pdf_file/0005/322475/Integrated-care-models-overview.pdf (accessed on 17 June 2020).
- Peterson, K.; Anderson, J.; Bourne, D.; Charns, M.P.; Gorin, S.S.; Hynes, D.M.; McDonald, K.M.; Singer, S.J.; Yano, E.M. Health Care Coordination Theoretical Frameworks: A Systematic Scoping Review to Increase Their Understanding and Use in Practice. J. Gen. Intern. Med. 2019, 34, 90–98. [Google Scholar] [CrossRef] [PubMed]
- Eggers, C.; Wolz, M.; Warnecke, T.; Prell, T.; Tönges, L. Parkinson Networks in Germany: Future or Utopia? Fortschr. Neurol. Psychiatr. 2020, 6–10. [Google Scholar] [CrossRef]
- Evans, J.M.; Grudniewicz, A.; Gray, C.S.; Wodchis, W.P.; Carswell, P.; Baker, G.R. Organizational context matters: A research toolkit for conducting standardized case studies of integrated care initiatives. Int. J. Integr. Care 2017, 17. [Google Scholar] [CrossRef] [PubMed]
- Valentijn, P.P.; Boesveld, I.C.; van der Klauw, D.M.; Ruwaard, D.; Struijs, J.N.; Molema, J.J.W.; Bruijnzeels, M.A.; Vrijhoef, H.J.M. Towards a taxonomy for integrated care: A mixed-methods study. Int. J. Integr. Care 2015, 15. [Google Scholar] [CrossRef]
- Minkman, M. The development model for integrated care: A validated tool for evaluation and development. J. Integr. Care 2016, 24, 38–52. [Google Scholar] [CrossRef]
- Radder, D.L.M.; Nonnekes, J.; van Nimwegen, M.; Eggers, C.; Abbruzzese, G.; Alves, G.; Browner, N.; Chaudhuri, K.R.; Ebersbach, G.; Ferreira, J.J.; et al. Recommendations for the Organization of Multidisciplinary Clinical Care Teams in Parkinson’s Disease. J. Parkinsons. Dis. 2020, 1–12. [Google Scholar] [CrossRef]
- Bloem, B.R.; Rompen, L.; de Vries, N.M.; Klink, A.; Munneke, M.; Jeurissen, P. ParkinsonNet: A low-cost health care innovation with a systems approach from the Netherlands. Health Aff. 2017, 36, 1987–1996. [Google Scholar] [CrossRef]
- Tönges, L.; Ehret, R.; Lorrain, M.; Riederer, P.; Müngersdorf, M. Epidemiology of Parkinson‘s Disease and Current Concepts of Outpatient Care in Germany. Fortschr. Neurol. Psychiatr. 2017, 85, 329–335. [Google Scholar] [CrossRef]
- Groot, M.M.; Vernooij-Dassen, M.J.F.J.; Verhagen, S.C.A.; Crul, B.J.P.; Grol, R.P.T.M. Obstacles to the delivery of primary palliative care as perceived by GPs. Palliat. Med. 2007, 21, 697–703. [Google Scholar] [CrossRef]
- Valentijn, P.P.; Ruwaard, D.M.; Vrijhoef, H.J.; de Bont, A.; Arends, R.Y.; Bruijnzeels, M.A. Collaboration processes and perceived effectiveness of integrated care projects in primary care: A longitudinal mixed-methods study. BMC Health Serv. Res. 2015. [Google Scholar] [CrossRef]
- Briggs, A.M.; Araujo De Carvalho, I. Actions required to implement integrated care for older people in the community using the World Health Organization’s ICOPE approach: A global Delphi consensus study. PLoS ONE 2018. [Google Scholar] [CrossRef] [PubMed]
- Hartelt, E.; Scherbaum, R.; Kinkel, M.; Gold, R.; Muhlack, S.; Tönges, L. Parkinson’s Disease Multimodal Complex Treatment (PD-MCT): Analysis of Therapeutic Effects and Predictors for Improvement. J. Clin. Med. 2020, 9, 1874. [Google Scholar] [CrossRef]
- Scherbaum, R.; Hartelt, E.; Kinkel, M.; Gold, R.; Muhlack, S.; Tönges, L. Parkinson’s Disease Multimodal Complex Treatment improves motor symptoms, depression and quality of life. J. Neurol. 2020, 267, 954–965. [Google Scholar] [CrossRef] [PubMed]
- Lorig, K.R.; Holman, H.R. Self-management education: History, definition, outcomes, and mechanisms. Ann. Behav. Med. 2003, 26, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Vlaanderen, F.P.; Rompen, L.; Munneke, M.; Stoffer, M.; Bloem, B.R.; Faber, M.J. The voice of the Parkinson customer. J. Parkinsons. Dis. 2019, 9, 197–201. [Google Scholar] [CrossRef] [PubMed]
- Jarman, B.; Hurwitz, B.; Cook, A.; Bajekal, M.; Lee, A. Effects of community based nurses specialising in Parkinson’s disease on health outcome and costs: Randomised controlled trial. Br. Med. J. 2002, 324, 1072–1075. [Google Scholar] [CrossRef][Green Version]
- Munneke, M.; Nijkrake, M.J.; Keus, S.H.; Kwakkel, G.; Berendse, H.W.; Roos, R.A.; Borm, G.F.; Adang, E.M.; Overeem, S.; Bloem, B.R. Efficacy of community-based physiotherapy networks for patients with Parkinson’s disease: A cluster-randomised trial. Lancet Neurol. 2010, 9, 46–54. [Google Scholar] [CrossRef]
- Prell, T.; Siebecker, F.; Lorrain, M.; Eggers, C.; Lorenzl, S.; Klucken, J.; Warnecke, T.; Buhmann, C.; Tönges, L.; Ehret, R.; et al. Recommendations for Standards of Network Care for Patients with Parkinson’s Disease in Germany. J. Clin. Med. 2020, 9, 1455. [Google Scholar] [CrossRef]
- Eggers, C.; Dano, R.; Schill, J.; Fink, G.R.; Timmermann, L.; Voltz, R.; Golla, H.; Lorenzl, S. Access to End-of Life Parkinson’s Disease Patients Through Patient-Centered Integrated Healthcare. Front. Neurol. 2018, 9. [Google Scholar] [CrossRef]
| Module | Rating Criteria | Number of Responses | Mean (SD 1) | Visualized Results 2 |
|---|---|---|---|---|
| Deep Brain Stimulation Consultation | Additional workload | n = 16 | 3.44 (± 0.89) | ★ ★ ★ ☆ ☆ |
| Special expertise required | 4.06 (± 1.06) | ★ ★ ★ ★ ☆ | ||
| Resources required for implementation | 3.19 (± 0.98) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 4.31 (± 1.01) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.94 (± 1.00) | ★ ★ ★
 ☆ ☆
| ||
| Evaluation | Additional workload | n = 16 | 4.13 (± 0.83) | ★ ★ ★ ★ ☆ |
| Special expertise required | 4.07 (± 1.10) | ★ ★ ★ ★ ☆ | ||
| Resources required for implementation | 4.07 (± 0.80) | ★ ★ ★ ★ ☆ | ||
| Expected patient benefit | 3.73 (± 1.16) | ★ ★ ★
 ☆ ☆ | ||
| Expected specialist benefit | 4.13 (± 0.83) | ★ ★ ★ ★ ☆ | ||
| Financing Strategies | Additional workload | n = 16 | 4.31 (± 0.60) | ★ ★ ★ ★ ☆ |
| Special expertise required | 3.56 (± 0.81) | ★ ★ ★
 ☆ ☆ | ||
| Resources required for implementation | 3.94 (± 0.57) | ★ ★ ★
 ☆ ☆ | ||
| Expected patient benefit | 3.38 (± 1.20) | ★ ★ ★ ☆ ☆ | ||
| Expected specialist benefit | 3.63 (± 1.09) | ★ ★ ★
 ☆ ☆ | ||
| Homepage | Additional workload | n = 16 | 3.81 (± 0.83) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 3.38 (± 1.09) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.63 (± 0.81) | ★ ★ ★
 ☆ ☆ | ||
| Expected patient benefit | 3.88 (± 1.02) | ★ ★ ★
 ☆ ☆ | ||
| Expected specialist benefit | 3.81 (± 0.75) | ★ ★ ★
 ☆ ☆ | ||
| Multi-Disciplinary Plenary Meetings | Additional workload | n = 17 | 3.88 (± 0.86) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 3.35 (± 1.06) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.47 (± 0.80) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 3.88 (± 0.60) | ★ ★ ★
 ☆ ☆ | ||
| Expected specialist benefit | 4.47 (± 0.72) | ★ ★ ★ ★ ☆ | ||
| Multimodal Complex Treatment | Additional workload | n = 16 | 3.75 (± 0.86) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 4.13 (± 0.96) | ★ ★ ★ ★ ☆ | ||
| Resources required for implementation | 3.88 (± 0.89) | ★ ★ ★
 ☆ ☆ | ||
| Expected patient benefit | 4.56 (± 0.73) | ★ ★ ★ ★
 | ||
| Expected specialist benefit | 3.38 (± 1.09) | ★ ★ ★ ☆ ☆ | ||
| Online Communication Platform | Additional workload | n = 16 | 3.63 (± 1.20) | ★ ★ ★
 ☆ ☆
|
| Special expertise required | 3.44 (± 1.03) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.69 (± 0.87) | ★ ★ ★
 ☆ ☆ | ||
| Expected patient benefit | 3.94 (± 1.06) | ★ ★ ★
 ☆ ☆ | ||
| Expected specialist benefit | 4.38 (± 0.72) | ★ ★ ★ ★ ☆ | ||
| Outpatient Video-Supported Therapy | Additional workload | n = 16 | 4.00 (± 1.10) | ★ ★ ★ ★ ☆ |
| Special expertise required | 4.13 (± 0.81) | ★ ★ ★ ★ ☆ | ||
| Resources required for implementation | 4.13 (± 0.96) | ★ ★ ★ ★ ☆ | ||
| Expected patient benefit | 4.44 (± 0.73) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.75 (± 1.06) | ★ ★ ★  ☆ ☆ | ||
| Parkinson Academy | Additional workload | n = 16 | 4.00 (± 0.65) | ★ ★ ★ ★ ☆ |
| Special expertise required | 3.80 (± 0.94) | ★ ★ ★  ☆ ☆ | ||
| Resources required for implementation | 347 (± 0.83) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 3.67 (± 0.82) | ★ ★ ★  ☆ ☆ | ||
| Expected specialist benefit | 3.73 (± 0.96) | ★ ★ ★  ☆ ☆ | ||
| Parkinson Assistant (PASS) Training | Additional workload | n = 16 | 3.56 (± 1.09) | ★ ★ ★  ☆ ☆ |
| Special expertise required | 3.38 (± 0.81) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.19 (± 0.91) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 4.13 (± 0.89) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.63 (± 1.15) | ★ ★ ★  ☆ ☆ | ||
| Parkinson Board | Additional workload | n = 16 | 3.38 (± 0.72) | ★ ★ ★ ☆ ☆ |
| Special expertise required | 3.88 (± 1.02) | ★ ★ ★  ☆ ☆ | ||
| Resources required for implementation | 2.75 (± 0.68) | ★ ★  ☆ ☆ ☆ ☆ | ||
| Expected patient benefit | 4.00 (± 0.82) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.94 (± 1.06) | ★ ★ ★  ☆ ☆ | ||
| Parkinson Nurse | Additional workload | n = 16 | 3.75 (± 0.93) | ★ ★ ★  ☆ ☆ |
| Special expertise required | 3.81 (± 0.83) | ★ ★ ★  ☆ ☆ | ||
| Resources required for implementation | 3.56 (± 0.81) | ★ ★ ★  ☆ ☆ | ||
| Expected patient benefit | 4.38 (± 0.89) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.50 (± 1.21) | ★ ★ ★  ☆ ☆ | ||
| Parkinson Summer Festival | Additional workload | n = 15 | 3.53 (± 0.83) | ★ ★ ★  ☆ ☆ |
| Special expertise required | 2.40 (± 0.91) | ★ ★ ☆ ☆ ☆ | ||
| Resources required for implementation | 3.47 (± 0.99) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 3.33 (± 1.11) | ★ ★ ★ ☆ ☆ | ||
| Expected specialist benefit | 2.47 (± 0.99) | ★ ★ ☆ ☆ ☆ | ||
| Parkinson Symposium | Additional workload | n = 15 | 3.73 (± 0.80) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 3.73 (± 1.10) | ★ ★ ★
 ☆ ☆ | ||
| Resources required for implementation | 3.47 (± 0.64) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 3.13 (± 0.92) | ★ ★ ★ ☆ ☆ | ||
| Expected specialist benefit | 4.27 (± 0.88) | ★ ★ ★ ★ ☆ | ||
| Parkinson Info-Café | Additional workload | n = 16 | 3.13 (± 0.81) | ★ ★ ★ ☆ ☆ |
| Special expertise required | 2.56 (± 0.73) | ★ ★  ☆ ☆ ☆ ☆ | ||
| Resources required for implementation | 2.75 (± 0.86) | ★ ★  ☆ ☆ ☆ ☆ | ||
| Expected patient benefit | 4.13 (± 1.09) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 2.38 (± 0.96) | ★ ★ ☆ ☆ ☆ | ||
| Quickcards | Additional workload | n = 16 | 3.47 (± 0.74) | ★ ★ ★ ☆ ☆ |
| Special expertise required | 3.67 (± 0.62) | ★ ★ ★ ★
 ☆ ☆ | ||
| Resources required for implementation | 3.40 (± 0.99) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 4.27 (± 1.03) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 4.40 (± 0.99) | ★ ★ ★ ★ ☆ | ||
| Regional Demand Analysis and Target Formulation | Additional workload | n = 16 | 3.69 (± 0.60) | ★ ★ ★  ☆ ☆ |
| Special expertise required | 3.44 (± 0.81) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.38 (± 0.50) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 4.38 (± 0.62) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 4.13 (± 0.72) | ★ ★ ★ ★ ☆ | ||
| Regional Public Relations | Additional workload | n = 16 | 3.71 (± 0.69) | ★ ★ ★  ☆ ☆ |
| Special expertise required | 3.53 (± 0.94) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.06 (± 0.83) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 3.94 (± 0.83) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.82 (± 0.88) | ★ ★ ★  ☆ ☆ | ||
| Regional Utilities Atlas | Additional workload | n = 17 | 4.00 (± 0.61) | ★ ★ ★ ★ ☆ |
| Special expertise required | 3.35 (± 0.86) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.63 (± 0.62) | ★ ★ ★  ☆ ☆ | ||
| Expected patient benefit | 4.59 (± 0.51) | ★ ★ ★ ★  | ||
| Expected specialist benefit | 3.82 (± 0.81) | ★ ★ ★  ☆ ☆ | ||
| Rehab | Additional workload | n = 16 | 4.06 (± 0.85) | ★ ★ ★ ★ ☆ |
| Special expertise required | 4.06 (± 1.24) | ★ ★ ★ ★ ☆ | ||
| Resources required for implementation | 3.44 (± 1.03) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 4.19 (± 0.91) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.56 (± 1.15) | ★ ★ ★  ☆ ☆ | ||
| Standardized Treatment Path | Additional workload | n = 16 | 4.06 (± 0.68) | ★ ★ ★ ★ ☆ |
| Special expertise required | 3.81 (± 0.98) | ★ ★ ★
 ☆ ☆ | ||
| Resources required for implementation | 3.69 (± 0.79) | ★ ★ ★
 ☆ ☆ | ||
| Expected patient benefit | 4.31 (± 0.79) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 4.00 (± 1.10) | ★ ★ ★ ★ ☆ | ||
| Steering Committee/Project Management | Additional workload | n = 17 | 3.81 (± 0.66) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 3.63 (± 1.02) | ★ ★ ★
 ☆ ☆ | ||
| Resources required for implementation | 3.44 (± 0.81) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 3.56 (± 1.15) | ★ ★ ★
 ☆ ☆ | ||
| Expected specialist benefit | 4.00 (± 0.89) | ★ ★ ★ ★ ☆ | ||
| Structured Patient School according to the Self-management Concept | Additional workload | n = 16 | 3.94 (± 0.85) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 3.81 (± 0.91) | ★ ★ ★
 ☆ ☆ | ||
| Resources required for implementation | 3.88 (± 0.81) | ★ ★ ★
 ☆ ☆ | ||
| Expected patient benefit | 4.56 (± 0.63) | ★ ★ ★ ★
 | ||
| Expected specialist benefit | 3.69 (± 1.01) | ★ ★ ★
 ☆ ☆ | ||
| Virtual Visits | Additional workload | n = 16 | 3.81 (± 0.98) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 3.88 (± 1.02) | ★ ★ ★
 ☆ ☆ | ||
| Resources required for implementation | 3.88 (± 0.50) | ★ ★ ★
 ☆ ☆ | ||
| Expected patient benefit | 419 (± 0.75) | ★ ★ ★ ★ ☆ | ||
| Expected specialist benefit | 3.56 (± 1.03) | ★ ★ ★
 ☆ ☆ | ||
| Working Groups | Additional workload | n = 17 | 3.76 (± 0.83) | ★ ★ ★
 ☆ ☆ |
| Special expertise required | 3.47 (± 0.94) | ★ ★ ★ ☆ ☆ | ||
| Resources required for implementation | 3.18 (± 0.64) | ★ ★ ★ ☆ ☆ | ||
| Expected patient benefit | 3.76 (± 0.97) | ★ ★ ★
 ☆ ☆ | ||
| Expected specialist benefit | 4.41 (± 0.71) | ★ ★ ★ ★ ☆ |
 = ≥0.5; ☆ = ≤0.5; ★ = 1.0; ★★ = 2.0; ★★★ = 3.0; ★★★★ = 4.0; ★★★★★ = 5.0.
= ≥0.5; ☆ = ≤0.5; ★ = 1.0; ★★ = 2.0; ★★★ = 3.0; ★★★★ = 4.0; ★★★★★ = 5.0.© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
van Munster, M.; Tönges, L.; Loewenbrück, K.F.; Warnecke, T.; Eggers, C. Building a Parkinson-Network–Experiences from Germany. J. Clin. Med. 2020, 9, 2743. https://doi.org/10.3390/jcm9092743
van Munster M, Tönges L, Loewenbrück KF, Warnecke T, Eggers C. Building a Parkinson-Network–Experiences from Germany. Journal of Clinical Medicine. 2020; 9(9):2743. https://doi.org/10.3390/jcm9092743
Chicago/Turabian Stylevan Munster, Marlena, Lars Tönges, Kai F. Loewenbrück, Tobias Warnecke, and Carsten Eggers. 2020. "Building a Parkinson-Network–Experiences from Germany" Journal of Clinical Medicine 9, no. 9: 2743. https://doi.org/10.3390/jcm9092743
APA Stylevan Munster, M., Tönges, L., Loewenbrück, K. F., Warnecke, T., & Eggers, C. (2020). Building a Parkinson-Network–Experiences from Germany. Journal of Clinical Medicine, 9(9), 2743. https://doi.org/10.3390/jcm9092743