1. Introduction
Adult-onset dementia disorders are among the prevalent global medical issues in industrialized countries that have a high impact on individuals’ lifestyles. These disorders represent a great challenge for the community over their advancement from early diagnosis to end of life [
1]. Statistical studies have estimated that every three seconds, a new dementia case is developing in the world. This means that approximately 50 million patients are suffering from this disease worldwide [
1,
2]. These numbers might double every twenty years and possibly reach 100 million patients by 2040.
Dementia is a syndrome that develops largely in older adults. It affects brain functionality, daily activities, and communication efficiency [
1,
3]. Alzheimer’s disease (AD) represents the prevalent form of adult-onset dementias. Some studies have highlighted that the early diagnosis of dementia is useful for starting treatments and for predicting outcomes of the disease but did not offer reliable methods for the early diagnosis of AD [
4,
5,
6]. At the same time, some forms of mild cognitive impairment (MCI) do not evolve into overt dementia, whereas other forms of MCI represent a very mild form of AD [
7]. In view of this, advanced computer techniques may represent a tool for the early diagnosis of AD and for predicting the evolution of prodromal forms of the disease or MCI into dementia.
Magnetic resonance imaging (MRI) techniques are becoming a relevant tool for prodromal AD and MCI evaluation [
8]. A few studies based on the comparative analysis of cognitive testing and neuroimaging have hypothesized that AD neuroimaging may be enough to predict disease [
8,
9,
10]. On the other hand, dementia forecasting with machine learning (ML) is becoming a more diffused approach in clinical practice [
11]. In spite of the practical interest to quantify AD evolutions based on MRI data, only a few studies have calculated AD incidence rates based on MRI.
Neuroimaging and primarily MRI provide essential information for AD dementia classification and prediction [
12,
13,
14]. ML models, coupled with MRI information, can provide high diagnostic accuracy of age-related cognitive decline (ARCD) in dementia subjects [
15]. It has been hypothesized that ML-supervised methods generate the knowledge of features necessary to correlate AD sample data [
16]. It is also reported that logistic regression, coupled with cross-validation, can enhance the accuracy of AD prediction by speech amalgamation [
17]. On the other hand, support vectors, along with feature reduction techniques, were able to classify dementia subjects with 70% accuracy [
4].
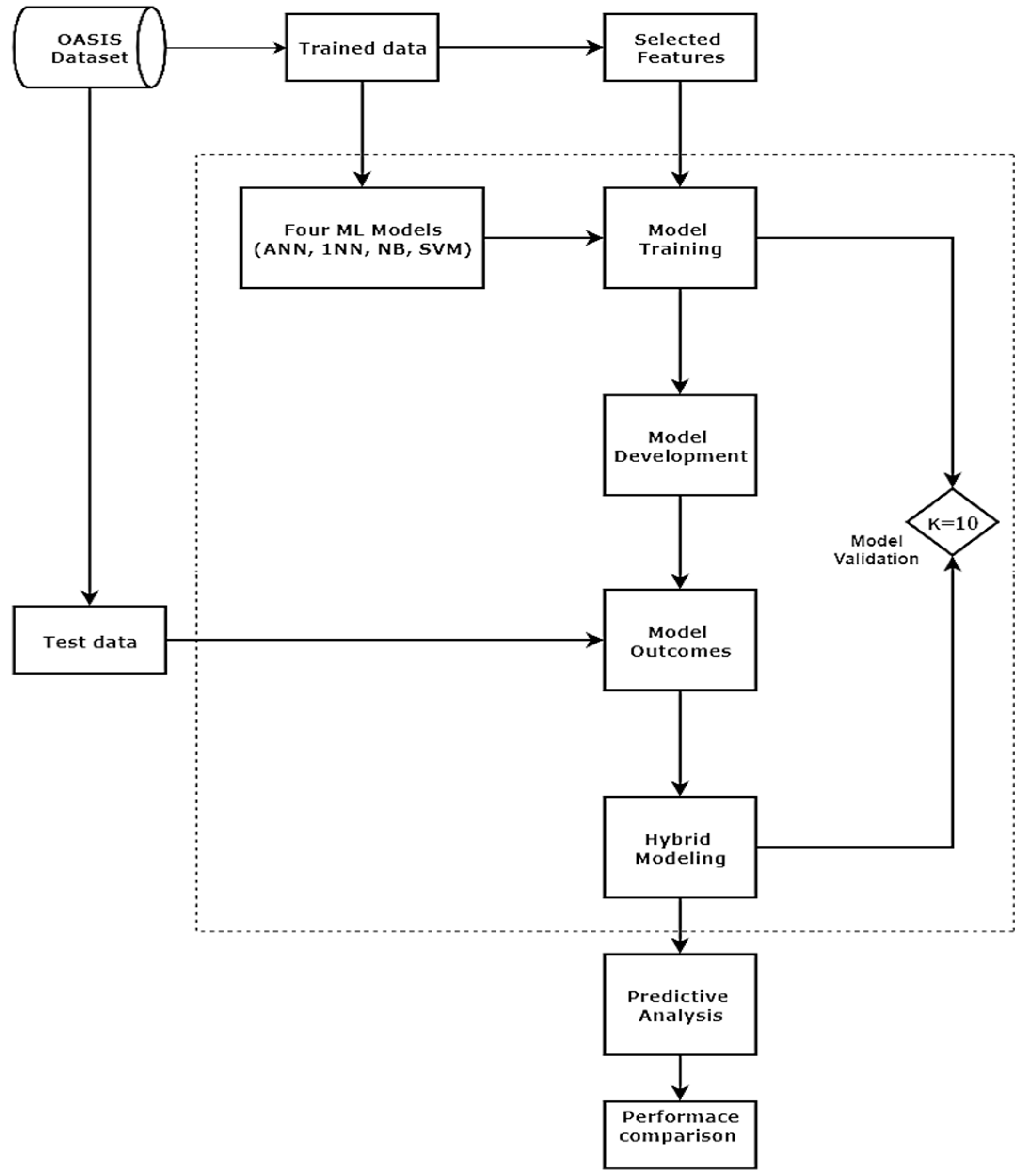
The present study was designed to detect AD based on MRI findings along with the use of four ML models, such as naive Bayes, neural networks, k-nearest neighbor, and support vectors. Each model was validated separately by tenfold cross validation (CV). The receiver operating characteristic (ROC) curve value was used to evaluate the model accuracy. Three individual experiments were designed to test the model, and model performance was separately evaluated with given MRI characteristic information. The experiments that were done included
Models with manual selection of MRI features,
Models with automatic feature selection, and
A single model with ensemble learning or hybrid modeling.
The subsequent part of this paper is organized as follows. In
Section 2, subject information of MRI features, feature selection techniques, and adopted models of AD prediction are analyzed. In
Section 3, the experimental results of the four models are presented. In
Section 4, each model is discussed and compared by accuracy and ROC parameters. Finally,
Section 5 summarizes the main results of the present work.
4. Discussion
ML models are highly acknowledged in real-time clinical practice and also in diagnosis and AD treatment selection [
41]. Several MRI works have been integrated into ML models to make AD predictions [
12,
17,
42], but there has been no comprehensive model to amplify model accuracy. In view of this, we introduced a hybrid model to enhance the precise detection of AD based on the analysis of MRIs.
In this paper, the significance of joint ML modeling for AD-onset prediction in elderly people has been demonstrated. Three different experiments were conducted, including manual and automatic feature selection techniques. Fourteen independent MRI features were used to identify the AD group using standard diagnostic approaches. Four supervised predictive models (NB, ANN, KNN, and SVM) were used, and the obtained results indicate the prediction accuracy of each model, constantly increasing between experiments.
Figure 6 compares the prediction accuracy of the three experiments. 1NN generated 91.32% accuracy by manual feature selection; SVM had a high 96.12% accuracy by automatic feature selection, whereas joint or hybrid modeling enabled 98% accuracy in predicting AD in older adults. The outcomes suggest that joint modeling, with limited features, is a best practice to assess AD-onset by subject prediction.
In the first experiment, all the designed classifiers revealed enough performance values in terms of true-positive rates (sensitivity). ANN and 1NN produced the highest sensitivity (89.92%), followed by SVM (89.24%) and NB (82.43%). As mentioned, ROC curve values between 0.5 and 0.7 indicate low prediction accuracy, between 0.7 and 0.9 indicate moderate prediction accuracy, and between 0.9 and 1 indicate high prediction accuracy [
43]. From
Table 7, it is obvious that the four adopted models produce moderate prediction accuracy when checking with manual feature selection.
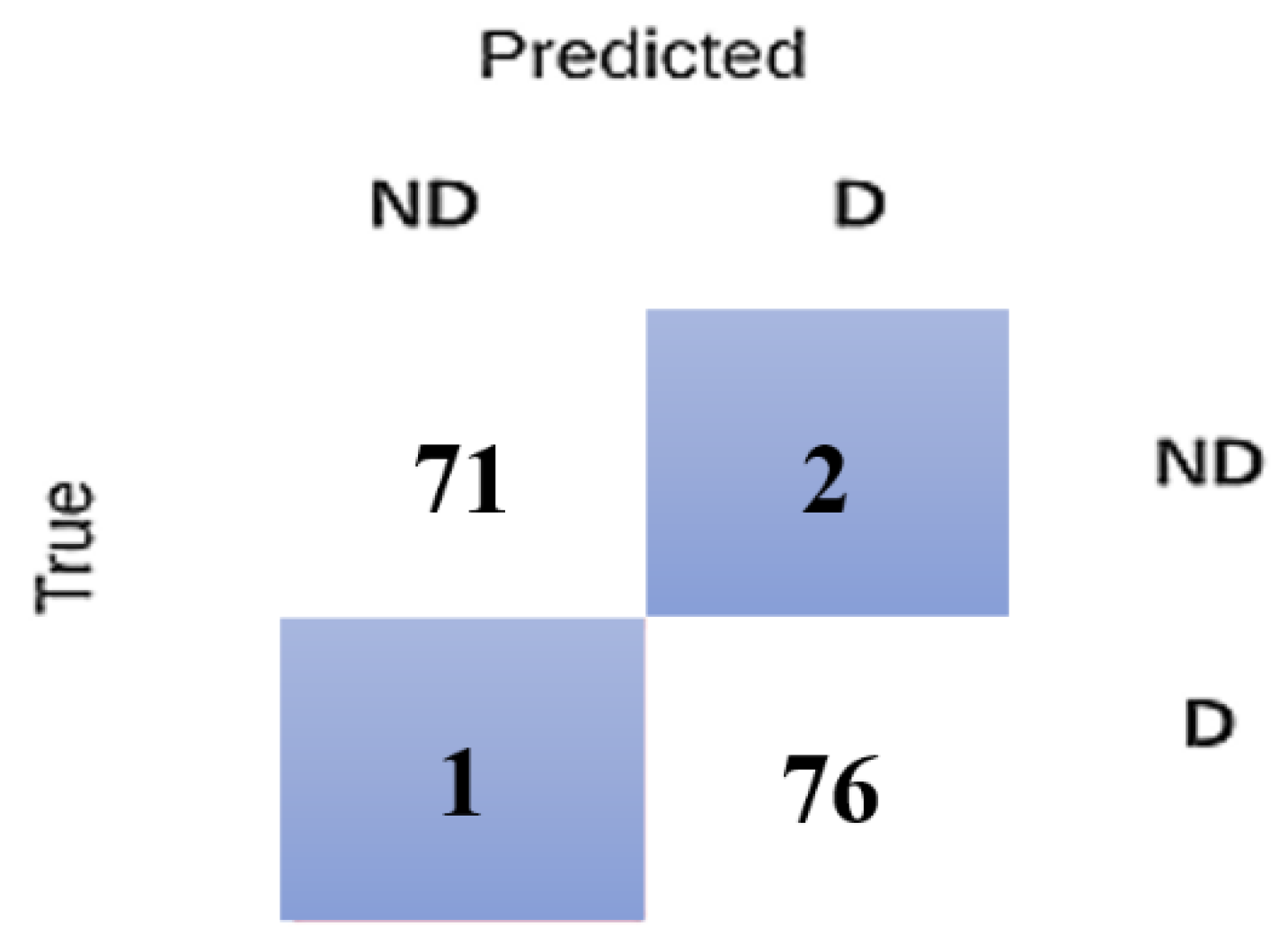
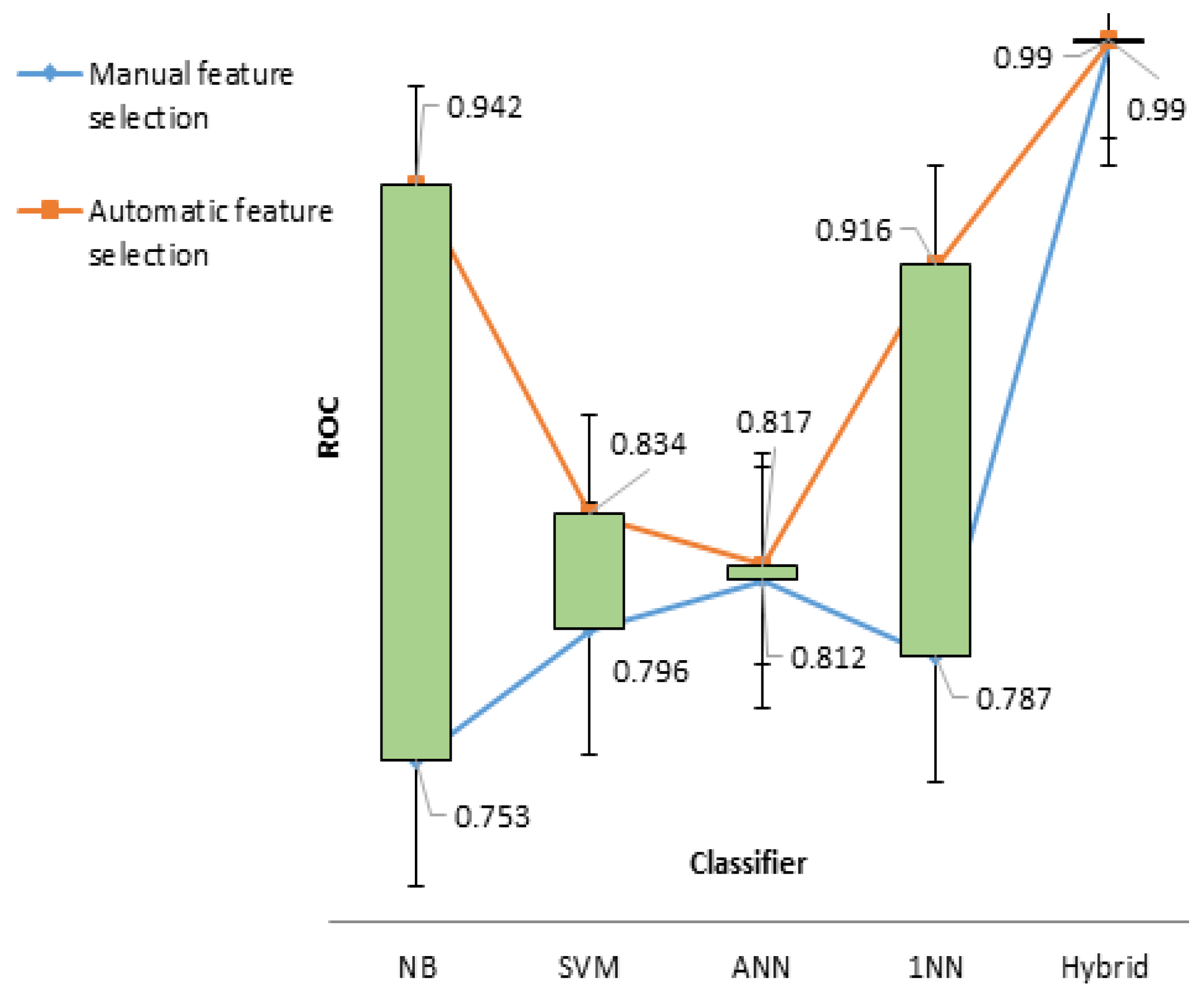
To amplify model performances, the second experiment was conducted with selective features after wrapping. This resulted in NB of 98.21% sensitivity, followed in descending order by SVM (94.94%), ANN (94.92%), and 1NN (89.92%). Both NB and 1NN predict subject class in a comparatively better manner, with ROC of 0.942 and 0.916, respectively. However, we argued that there could be other possibilities for enhancing prediction accuracy to values higher than those identified in the above two experiments. To support this claim, a hybrid model was developed by combining the four investigated models. A simulation of four recruited models was then performed, and thanks to this approach, the sensitivity of the model attained the highest predicted value of 97.4%, and its ROC was nearly equal to one (
Figure 7).
The developed model produced better accuracy than other conventional models, but the present study has some limitations. First, the limited number of subjects investigated could hamper the final dementia subject prediction to the overall AD subjects; second, the outcome of the integration of three experiments may have influenced the results. The use of external MRI information does not guarantee data quality and can affect the significance of the study as a whole.
Brain studies corroborated with artificial intelligence analysis may offer relatively faster investigation methods to modern neurological research. However, it would be preferable to avoid data limitations and, therefore, to enlarge as much as possible the size of the sample investigated in future studies. At the same time, it is also recommended to apply hybrid modeling to younger subjects or subjects with mild AD and to anticipate prediction accuracy with other biological tests like cerebrospinal fluid (CSF) or blood markers.
5. Conclusions
Adult-onset dementia disorders are serious brain pathologies caused by the loss of neuron functions and to progressive atrophy. AD is the most common of these pathologies. It affects primarily elderly people and has a tremendous impact on the lives of people suffering from it. In view of the long time passing between brain lesions bringing about dementia and the onset of clinical symptomatology, early identification of the preclinical and prodromal forms of the disease represents a challenge for medicine. This will reduce medical costs and could contribute to undertaking therapeutic approaches for delaying the conversion of the disease into overt dementia.
Unfortunately, the identification of AD at very early stages is extremely difficult, and there are no tools for its simple detection. We have developed different ML models to predict dementia in the elderly based on MRI findings. The hybrid model with selective features was found to enhance the accuracy of dementia prediction. Experiments with manual feature selection prior to automatic feature selection with 1NN produced 91.32% of accuracy, and the experiment of automatic feature selection generated 96.12% accuracy by SVM. This value significantly increased using multi modeling and produced 98% accuracy. The predictive models developed in this study forecast early AD diagnosis and the associated risk of developing dementia. Although it is difficult to develop longitudinal projection models in older adults as compared to the younger population, future research in the field should consider addressing both genetic and nongenetic features of multifactorial hazards.