Oral Iron for IBD Patients: Lessons Learned at Time of COVID-19 Pandemic
Abstract
1. Introduction
2. Experimental Section
3. Results
3.1. Ferrous Oral Iron
3.2. Ferric Oral Iron
3.3. Ferric Maltol
3.4. Sucrosomial Iron
4. Discussion
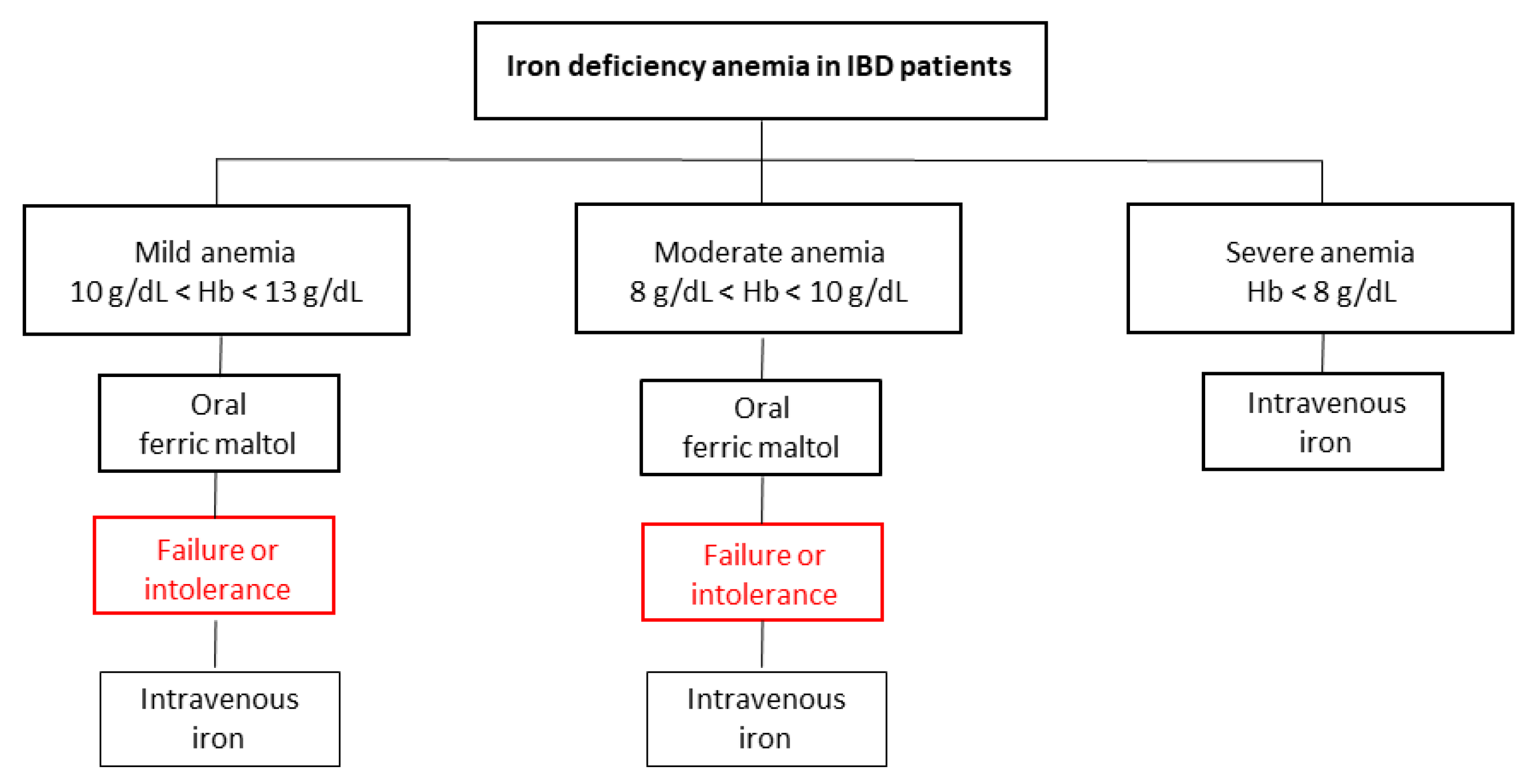
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Torres, J.; Mehandru, S.; Colombel, J.-F.; Peyrin-Biroulet, L. Crohn’s disease. Lancet 2017, 389, 1741–1755. [Google Scholar] [CrossRef]
- Ungaro, R.; Mehandru, S.; Allen, P.B.; Peyrin-Biroulet, L.; Colombel, J.-F. Ulcerative colitis. Lancet 2017, 389, 1756–1770. [Google Scholar] [CrossRef]
- Harbord, M.; Annese, V.; Vavricka, S.R.; Allez, M.; Barreiro-de Acosta, M.; Boberg, K.M.; Burisch, J.; De Vos, M.; De Vries, A.-M.; Dick, A.D.; et al. The First European Evidence-based Consensus on Extra-intestinal Manifestations in Inflammatory Bowel Disease. J. Crohns Colitis 2016, 10, 239–254. [Google Scholar] [CrossRef] [PubMed]
- Bonovas, S.; Fiorino, G.; Allocca, M.; Lytras, T.; Tsantes, A.; Peyrin-Biroulet, L.; Danese, S. Intravenous Versus Oral Iron for the Treatment of Anemia in Inflammatory Bowel Disease: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Medicine 2016, 95, e2308. [Google Scholar] [CrossRef] [PubMed]
- Dignass, A.U.; Gasche, C.; Bettenworth, D.; Birgegård, G.; Danese, S.; Gisbert, J.P.; Gomollon, F.; Iqbal, T.; Katsanos, K.; Koutroubakis, I.; et al. European consensus on the diagnosis and management of iron deficiency and anaemia in inflammatory bowel diseases. J. Crohns Colitis 2015, 9, 211–222. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Archived: Iron Deficiency Anaemia: Assessment, Prevention and Control. Available online: http://www.who.int/nutrition/publications/micronutrients/anaemia_iron_deficiency/WHO_NHD_01.3/en/ (accessed on 24 April 2020).
- Gasche, C.; Lomer, M.C.E.; Cavill, I.; Weiss, G. Iron, anaemia, and inflammatory bowel diseases. Gut 2004, 53, 1190–1197. [Google Scholar] [CrossRef]
- Wells, C.W.; Lewis, S.; Barton, J.R.; Corbett, S. Effects of changes in hemoglobin level on quality of life and cognitive function in inflammatory bowel disease patients. Inflamm. Bowel Dis. 2006, 12, 123–130. [Google Scholar] [CrossRef]
- Vegh, Z.; Kurti, Z.; Gonczi, L.; Golovics, P.A.; Lovasz, B.D.; Szita, I.; Balogh, M.; Pandur, T.; Vavricka, S.R.; Rogler, G.; et al. Association of extraintestinal manifestations and anaemia with disease outcomes in patients with inflammatory bowel disease. Scand. J. Gastroenterol. 2016, 51, 848–854. [Google Scholar] [CrossRef]
- Blumenstein, I.; Dignass, A.; Vollmer, S.; Klemm, W.; Weber-Mangal, S.; Stein, J. Current practice in the diagnosis and management of IBD-associated anaemia and iron deficiency in Germany: The German AnaemIBD Study. J. Crohns Colitis 2014, 8, 1308–1314. [Google Scholar] [CrossRef]
- Stein, J.; Bager, P.; Befrits, R.; Gasche, C.; Gudehus, M.; Lerebours, E.; Magro, F.; Mearin, F.; Mitchell, D.; Oldenburg, B.; et al. Anaemia management in patients with inflammatory bowel disease: Routine practice across nine European countries. Eur. J. Gastroenterol. Hepatol. 2013, 25, 1456–1463. [Google Scholar] [CrossRef]
- Abhyankar, A.; Moss, A.C. Iron Replacement in Patients with Inflammatory Bowel Disease: A Systematic Review and Meta-analysis. Inflamm. Bowel Dis. 2015, 21, 1976–1981. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, O.H.; Soendergaard, C.; Vikner, M.E.; Weiss, G. Rational Management of Iron-Deficiency Anaemia in Inflammatory Bowel Disease. Nutrients 2018, 10, 82. [Google Scholar] [CrossRef] [PubMed]
- Lee, T.W.; Kolber, M.R.; Fedorak, R.N.; van Zanten, S.V. Iron replacement therapy in inflammatory bowel disease patients with iron deficiency anemia: A systematic review and meta-analysis. J Crohns Colitis 2012, 6, 267–275. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, O.H.; Ainsworth, M.; Coskun, M.; Weiss, G. Management of Iron-Deficiency Anemia in Inflammatory Bowel Disease: A Systematic Review. Medicine (Baltimore) 2015, 94, e963. [Google Scholar] [CrossRef]
- Reinisch, W.; Staun, M.; Tandon, R.K.; Altorjay, I.; Thillainayagam, A.V.; Gratzer, C.; Nijhawan, S.; Thomsen, L.L. A randomized, open-label, non-inferiority study of intravenous iron isomaltoside 1,000 (Monofer) compared with oral iron for treatment of anemia in IBD (PROCEED). Am. J. Gastroenterol. 2013, 108, 1877–1888. [Google Scholar] [CrossRef]
- Tolkien, Z.; Stecher, L.; Mander, A.P.; Pereira, D.I.A.; Powell, J.J. Ferrous sulfate supplementation causes significant gastrointestinal side-effects in adults: A systematic review and meta-analysis. PLoS ONE 2015, 10, e0117383. [Google Scholar] [CrossRef]
- Danese, S.; Hoffman, C.; Vel, S.; Greco, M.; Szabo, H.; Wilson, B.; Avedano, L. Anaemia from a patient perspective in inflammatory bowel disease: Results from the European Federation of Crohn’s and Ulcerative Colitis Association’s online survey. Eur. J. Gastroenterol. Hepatol. 2014, 26, 1385–1391. [Google Scholar] [CrossRef]
- Lugg, S.; Beal, F.; Nightingale, P.; Bhala, N.; Iqbal, T. Iron treatment and inflammatory bowel disease: What happens in real practice? J. Crohns Colitis 2014, 8, 876–880. [Google Scholar] [CrossRef]
- Gasche, C.; Ahmad, T.; Tulassay, Z.; Baumgart, D.C.; Bokemeyer, B.; Büning, C.; Howaldt, S.; Stallmach, A. AEGIS Study Group Ferric maltol is effective in correcting iron deficiency anemia in patients with inflammatory bowel disease: Results from a phase-3 clinical trial program. Inflamm. Bowel Dis. 2015, 21, 579–588. [Google Scholar] [CrossRef]
- Schmidt, C.; Ahmad, T.; Tulassay, Z.; Baumgart, D.C.; Bokemeyer, B.; Howaldt, S.; Stallmach, A.; Büning, C. AEGIS Study Group Ferric maltol therapy for iron deficiency anaemia in patients with inflammatory bowel disease: Long-term extension data from a Phase 3 study. Aliment. Pharmacol. Ther. 2016, 44, 259–270. [Google Scholar] [CrossRef]
- Farrell, D.; Artom, M.; Czuber-Dochan, W.; Jelsness-Jørgensen, L.P.; Norton, C.; Savage, E. Interventions for fatigue in inflammatory bowel disease. Cochrane Database Syst. Rev. 2020, 4, CD012005. [Google Scholar] [CrossRef] [PubMed]
- Cummings, F.; Singfield, C.; Jones, L.; Hickey, J.; Beales, I.; Fraser, A.; Sebastian, S.; Stansfield, C.; Hoque, S. PWE-013 Feraccru® real world effectiveness study in hospital practice (fresh): An interim analysis. Gut 2018, 67, A74. [Google Scholar] [CrossRef]
- Oppong, P.; Lovato, S.; Akbar, A. PTU-124 Real world tolerability & efficacy of oral ferric maltol (feraccru) in IBD associated anaemia. Gut 2018, 67, A252–A253. [Google Scholar] [CrossRef]
- Howaldt, S.; Jacob, I.; Sampson, M.; Akriche, F. P331 Productivity loss in patients with inflammatory bowel disease receiving treatment for iron deficiency anaemia: A comparison of ferric maltol and IV iron. J. Crohns Colitis 2020, 14, S319–S320. [Google Scholar] [CrossRef]
- Howaldt, S.; Jacob, I.; Sampson, M.; Akriche, F. P567 Impact of oral ferric maltol and IV iron on health-related quality of life in patients with iron deficiency anaemia and inflammatory bowel disease, and relationship with haemoglobin and serum iron. J. Crohns Colitis 2020, 14, S478–S479. [Google Scholar] [CrossRef]
- Howaldt, S.; Jacob, I.; Sampson, M.; Akriche, F. P685 Healthcare resource use associated with ferric maltol and IV iron treatment for iron deficiency anaemia in patients with inflammatory bowel disease. J. Crohns Colitis 2020, 14, S558. [Google Scholar] [CrossRef]
- Abbati, G.; Incerti, F.; Boarini, C.; Pileri, F.; Bocchi, D.; Ventura, P.; Buzzetti, E.; Pietrangelo, A. Safety and efficacy of sucrosomial iron in inflammatory bowel disease patients with iron deficiency anemia. Intern. Emerg. Med. 2019, 14, 423–431. [Google Scholar] [CrossRef]
- Stallmach, A.; Büning, C. Ferric maltol (ST10): A novel oral iron supplement for the treatment of iron deficiency anemia in inflammatory bowel disease. Expert Opin. Pharmacother. 2015, 16, 2859–2867. [Google Scholar] [CrossRef]
- Guan, W.-J.; Ni, Z.-Y.; Hu, Y.; Liang, W.-H.; Ou, C.-Q.; He, J.-X.; Liu, L.; Shan, H.; Lei, C.-L.; Hui, D.S.C.; et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N. Engl. J. Med. 2020. [CrossRef]
- COVID-19 situation reports. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports (accessed on 27 April 2020).
- Danese, S.; Cecconi, M.; Spinelli, A. Management of IBD during the COVID-19 outbreak: Resetting clinical priorities. Nat. Rev. Gastroenterol. Hepatol. 2020, 17, 253–255. [Google Scholar] [CrossRef]
- Danese, S.; Ran, Z.H.; Repici, A.; Tong, J.; Omodei, P.; Aghemo, A.; Malesci, A. Gastroenterology department operational reorganisation at the time of covid-19 outbreak: An Italian and Chinese experience. Gut 2020, 69, 981–983. [Google Scholar] [CrossRef] [PubMed]
- Kulnigg, S.; Teischinger, L.; Dejaco, C.; Waldhör, T.; Gasche, C. Rapid recurrence of IBD-associated anemia and iron deficiency after intravenous iron sucrose and erythropoietin treatment. Am. J. Gastroenterol. 2009, 104, 1460–1467. [Google Scholar] [CrossRef] [PubMed]
- Q&A on Coronaviruses (COVID-19). Available online: https://www.who.int/news-room/q-a-detail/q-a-coronaviruses (accessed on 25 April 2020).
| First Author | Study Design | Study Population | No. of Patients | Treatment | Results | Adverse Events |
|---|---|---|---|---|---|---|
| Lee [14] | Systematic review and meta-analysis | IBD | 333 | Oral ferrous iron IV iron | IV iron showed a higher improvement in Hb levels compared to oral iron | IV iron led to a lower rate of therapy discontinuation due to AEs compared to oral iron |
| Nielsen [15] | Systematic review | IBD | 2906 | Oral ferrous iron Oral ferric maltol IV iron | No difference between IV and oral iron in Hb increase in mild anemia | Milder AEs occurred more frequently in oral group than in IV group |
| Abhyankar [12] | Systematic review and meta-analysis | IBD | 694 | Oral ferrous iron IV iron | No difference between IV and oral iron in Hb response (Hb rise > 2 g/dL) | IV iron led to a lower rate of therapy discontinuation due to AEs compared to oral iron |
| Bonovas [4] | Systematic review and meta-analysis | IBD | 694 | Oral ferrous iron IV iron | IV iron showed a higher Hb response (Hb rise > 2 g/dL) compared to oral iron | GI AEs occurred more frequently in oral group than in IV arm |
| Reinisch [16] | Randomized open-label trial | IBD | 338 | Oral ferrous iron IV iron | Non-inferiority in Hb change between IV and oral iron was not proven | No difference in term of AEs was found between the study groups |
| Tolkien [17] | Systematic review and meta-analysis | Adult subjects | 6831 | Oral ferrous iron IV iron Placebo | / | More GI AEs occurred in oral group than in IV and placebo arms |
| Lugg [19] | Cross-sectional study | IBD | 87 | Oral ferrous iron IV iron | Median Hb change after oral iron was 7 g/L in CD patients and 4 g/L in UC patients | AEs occurred in 51% of the patients treated with oral iron |
| First Author | Study Design | Study Population | No. of Patients | Treatment | Results | Adverse Events |
|---|---|---|---|---|---|---|
| Gasche [20] | RCT | IBD | 128 | Ferric maltol Placebo | A mean Hb increase of 2.25 g/dL was found in the ferric maltol group vs. placebo arm | AEs were comparable between ferric maltol and placebo groups (58% vs. 72%) |
| Schmidt [21] | Prospective cohort study | IBD | 97 | Ferric maltol | 86% of patients achieved normal Hb values after 64 weeks | Drug-related AEs were detected in 24% of patients |
| Farrell [22] | Systematic review | IBD | / | Ferric maltol Placebo | / | Fewer AEs (51% vs. 71%) and serious AEs (8% vs. 13%) occurred with ferric maltol compared to placebo |
| Cummings [23] | Prospective cohort study | IBD | 30 | Ferric maltol | 62% of patients achieved normalized Hb levels after 3 months of therapy | / |
| Oppong [24] | Prospective cohort study | IBD | 28 | Ferric maltol | Ferric maltol was well-tolerated in 14/21 patients (66%) | The most common AEs was abdominal pain, no serious AE occurred |
| Howaldt [25] | RCT | IBD | 250 | Ferric maltol IV iron | Ferric maltol was not inferior to IV iron to achieve normalization or increase in Hb values of ≥2 g/dL | / |
| Howaldt [26] | RCT | IBD | 250 | Ferric maltol IV iron | Improvements in SF-36 and MCS scores were numerically higher with ferric maltol than IV iron | / |
| Howaldt [27] | RCT | IBD | 250 | Ferric maltol IV iron | Total costs per patient were lower in ferric maltol group than in IV arm | / |
| Abbati [28] | Prospective cohort study | IBD | 30 | Sucrosomial iron | Hb increased in 86% of patients after 3 months | 44 AEs were recorded, but no AE was certainly related to the drug |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
D’Amico, F.; Peyrin-Biroulet, L.; Danese, S. Oral Iron for IBD Patients: Lessons Learned at Time of COVID-19 Pandemic. J. Clin. Med. 2020, 9, 1536. https://doi.org/10.3390/jcm9051536
D’Amico F, Peyrin-Biroulet L, Danese S. Oral Iron for IBD Patients: Lessons Learned at Time of COVID-19 Pandemic. Journal of Clinical Medicine. 2020; 9(5):1536. https://doi.org/10.3390/jcm9051536
Chicago/Turabian StyleD’Amico, Ferdinando, Laurent Peyrin-Biroulet, and Silvio Danese. 2020. "Oral Iron for IBD Patients: Lessons Learned at Time of COVID-19 Pandemic" Journal of Clinical Medicine 9, no. 5: 1536. https://doi.org/10.3390/jcm9051536
APA StyleD’Amico, F., Peyrin-Biroulet, L., & Danese, S. (2020). Oral Iron for IBD Patients: Lessons Learned at Time of COVID-19 Pandemic. Journal of Clinical Medicine, 9(5), 1536. https://doi.org/10.3390/jcm9051536






