Differences in Brain Volume between Metabolically Healthy and Unhealthy Overweight and Obese Children: The Role of Fitness
Abstract
1. Introduction
2. Material and Methods
2.1. Design
2.2. Participants
2.3. Measurements
2.3.1. Anthropometric Variables
2.3.2. Blood Analyses and Blood Pressure
2.3.3. MHO and MUO’s Categorization
2.3.4. Global and Regional Brain Volume
2.3.5. Academic Achievement
2.3.6. Cardiorespiratory Fitness
2.3.7. Other Covariates
2.4. Statistical Analyses
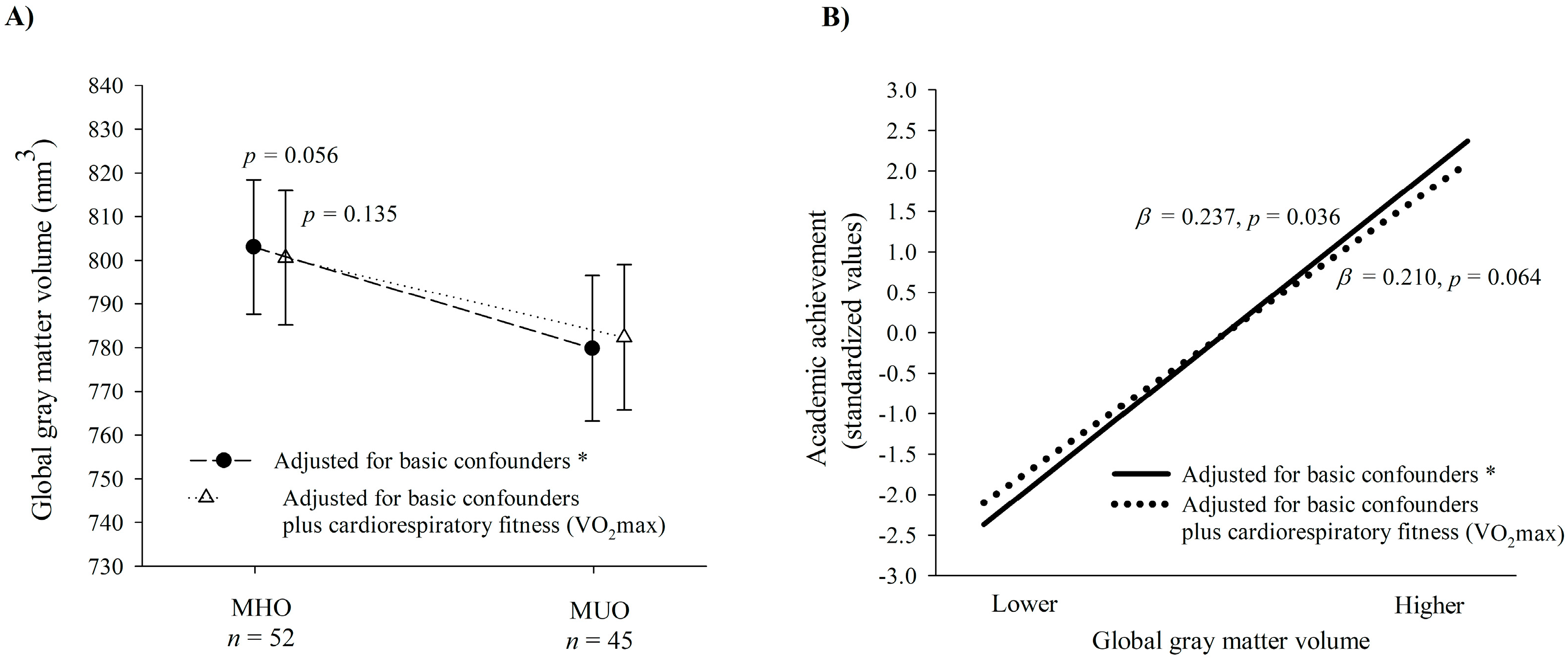
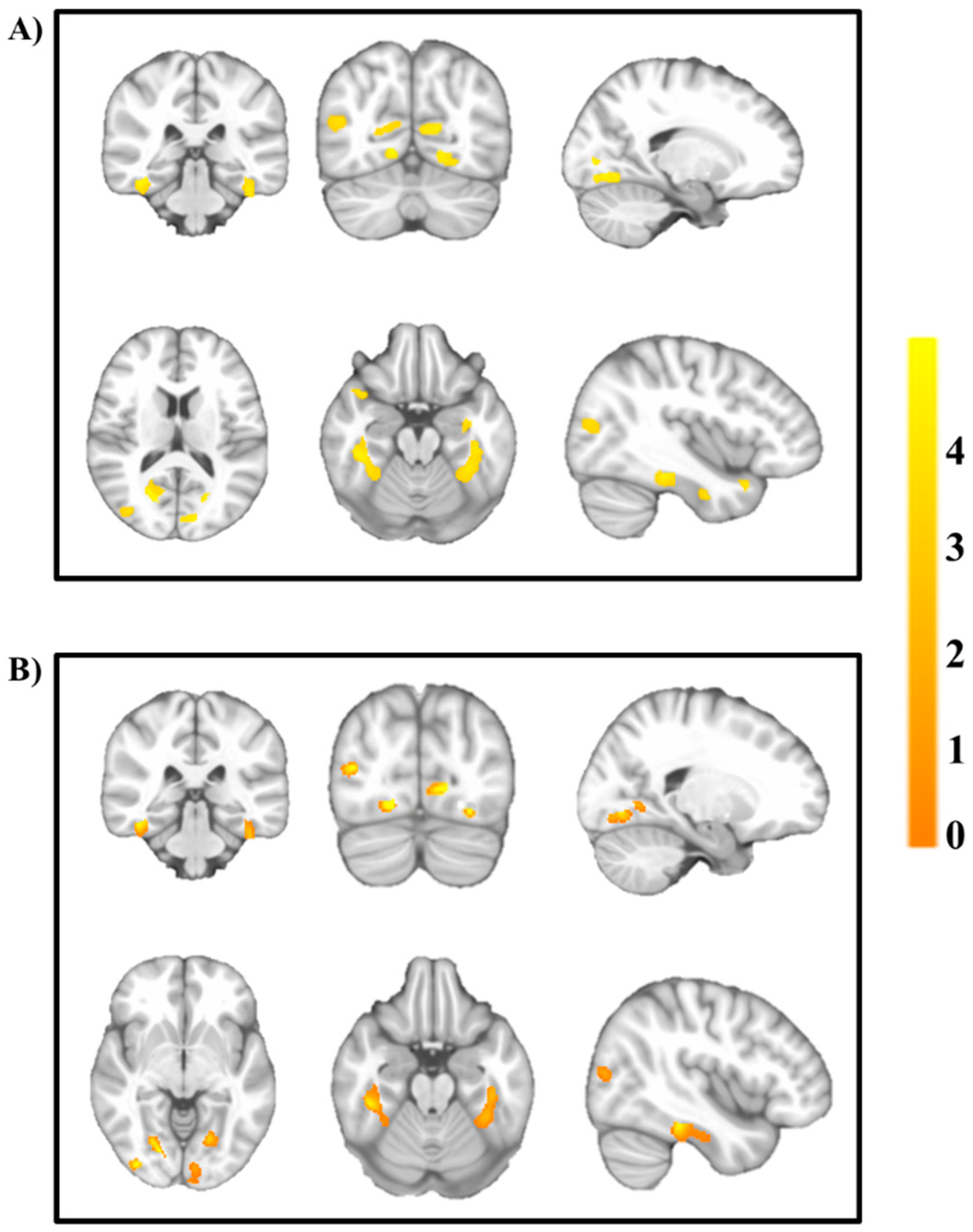
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F.; et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014, 384, 766–781. [Google Scholar] [CrossRef]
- Ortega, F.B.; Lavie, C.J.; Blair, S.N. Obesity and Cardiovascular Disease. Circ. Res. 2016, 118, 1752–1770. [Google Scholar] [CrossRef] [PubMed]
- Umer, A.; Kelley, G.A.; Cottrell, L.E.; Giacobbi, P., Jr.; Innes, K.E.; Lilly, C.L. Childhood obesity and adult cardiovascular disease risk factors: A systematic review with meta-analysis. BMC Public Health 2017, 17, 683. [Google Scholar] [CrossRef] [PubMed]
- Medic, N.; Ziauddeen, H.; Ersche, K.D.; Farooqi, I.S.; Bullmore, E.T.; Nathan, P.J.; Ronan, L.; Fletcher, P.C. Increased body mass index is associated with specific regional alterations in brain structure. Int. J. Obes. 2016, 40, 1177–1182. [Google Scholar] [CrossRef]
- Brooks, S.J.; Benedict, C.; Burgos, J.; Kempton, M.J.; Kullberg, J.; Nordenskjold, R.; Kilander, L.; Nylander, R.; Larsson, E.M.; Johansson, L.; et al. Late-life obesity is associated with smaller global and regional gray matter volumes: A voxel-based morphometric study. Int. J. Obes. 2013, 37, 230–236. [Google Scholar] [CrossRef] [PubMed]
- Kamijo, K.; Khan, N.A.; Pontifex, M.B.; Scudder, M.R.; Drollette, E.S.; Raine, L.B.; Evans, E.M.; Castelli, D.M.; Hillman, C.H. The relation of adiposity to cognitive control and scholastic achievement in preadolescent children. Obesity 2012, 20, 2406–2411. [Google Scholar] [CrossRef]
- O’Brien, P.D.; Hinder, L.M.; Callaghan, B.C.; Feldman, E.L. Neurological consequences of obesity. Lancet Neurol. 2017, 16, 465–477. [Google Scholar] [CrossRef]
- Garcia-Garcia, I.; Michaud, A.; Dadar, M.; Zeighami, Y.; Neseliler, S.; Collins, D.L.; Evans, A.C.; Dagher, A. Neuroanatomical differences in obesity: Meta-analytic findings and their validation in an independent dataset. Int. J. Obes. 2019, 43, 943–951. [Google Scholar] [CrossRef]
- Gracia-Marco, L.; Esteban-Cornejo, I.; Ubago-Guisado, E.; Rodriguez-Ayllon, M.; Mora-Gonzalez, J.; Solis-Urra, P.; Cadenas-Sanchez, C.; Verdejo-Roman, J.; Catena, A.; Erickson, K.I.; et al. Lean mass index is positively associated with white matter volumes in several brain regions in children with overweight/obesity. Ped. Obes. 2020, e12604. [Google Scholar] [CrossRef]
- Jolliffe, C.J.; Janssen, I. Development of age-specific adolescent metabolic syndrome criteria that are linked to the Adult Treatment Panel III and International Diabetes Federation criteria. J. Am. Coll. Cardiol. 2007, 49, 891–898. [Google Scholar] [CrossRef]
- Fan, J.; Song, Y.; Chen, Y.; Hui, R.; Zhang, W. Combined effect of obesity and cardio-metabolic abnormality on the risk of cardiovascular disease: A meta-analysis of prospective cohort studies. Int. J. Cardiol. 2013, 168, 4761–4768. [Google Scholar] [CrossRef] [PubMed]
- Kramer, C.K.; Zinman, B.; Retnakaran, R. Are metabolically healthy overweight and obesity benign conditions? A systematic review and meta-analysis. Ann. Intern. Med. 2013, 159, 758–769. [Google Scholar] [CrossRef] [PubMed]
- Roberson, L.L.; Aneni, E.C.; Maziak, W.; Agatston, A.; Feldman, T.; Rouseff, M.; Tran, T.; Blaha, M.J.; Santos, R.D.; Sposito, A.; et al. Beyond BMI: The “Metabolically healthy obese” phenotype & its association with clinical/subclinical cardiovascular disease and all-cause mortality—A systematic review. BMC Public Health 2014, 14, 14. [Google Scholar]
- Zheng, R.; Zhou, D.; Zhu, Y. The long-term prognosis of cardiovascular disease and all-cause mortality for metabolically healthy obesity: A systematic review and meta-analysis. J. Epidemiol. Community Health 2016, 70, 1024–1031. [Google Scholar] [CrossRef] [PubMed]
- Eckel, N.; Meidtner, K.; Kalle-Uhlmann, T.; Stefan, N.; Schulze, M.B. Metabolically healthy obesity and cardiovascular events: A systematic review and meta-analysis. Eur. J. Prev. Cardiol. 2016, 23, 956–966. [Google Scholar] [CrossRef]
- Ortega, F.B.; Cadenas-Sanchez, C.; Sui, X.; Blair, S.N.; Lavie, C.J. Role of Fitness in the Metabolically Healthy but Obese Phenotype: A Review and Update. Prog. Cardiovasc. Dis. 2015, 58, 76–86. [Google Scholar] [CrossRef]
- Lavie, C.J.; Kokkinos, P.F.; Ortega, F.B. Impact of Physical Activity and Fitness in Metabolically Health Obesity. J. Am. Coll. Cardiol. 2018, 71, 812–813. [Google Scholar] [CrossRef]
- Bluher, S.; Schwarz, P. Metabolically healthy obesity from childhood to adulthood—Does weight status alone matter? Metabolism 2014, 63, 1084–1092. [Google Scholar] [CrossRef]
- Cadenas-Sanchez, C.; Ruiz, J.R.; Labayen, I.; Huybrechts, I.; Manios, Y.; Gonzalez-Gross, M.; Breidenassel, C.; Kafatos, A.; De Henauw, S.; Vanhelst, J.; et al. Prevalence of Metabolically Healthy but Overweight/Obese Phenotype and Its Association With Sedentary Time, Physical Activity, and Fitness. J. Adolesc. Health 2017, 61, 107–114. [Google Scholar] [CrossRef]
- Ortega, F.B.; Cadenas-Sanchez, C.; Migueles, J.H.; Labayen, I.; Ruiz, J.R.; Sui, X.; Blair, S.N.; Martínez-Vizcaino, V.; Lavie, C.J. Role of Physical Activity and Fitness in the Characterization and Prognosis of the Metabolically Healthy Obesity Phenotype: A Systematic Review and Meta-analysis. Prog. Cardiovasc. Dis. 2018, 61, 190–205. [Google Scholar] [CrossRef]
- Ortega, F.B.; Lee, D.C.; Katzmarzyk, P.T.; Ruiz, J.R.; Sui, X.; Church, T.S.; Blair, S.N. The intriguing metabolically healthy but obese phenotype: Cardiovascular prognosis and role of fitness. Eur. Heart J. 2013, 34, 389–397. [Google Scholar] [CrossRef] [PubMed]
- Esteban-Cornejo, I.; Cadenas-Sanchez, C.; Contreras-Rodriguez, O.; Verdejo-Roman, J.; Mora-Gonzalez, J.; Migueles, J.H.; Henriksson, P.; Davis, C.L.; Verdejo-Garcia, A.; Catena, A.; et al. A whole brain volumetric approach in overweight/obese children: Examining the association with different physical fitness components and academic performance. The ActiveBrains project. Neuroimage 2017, 159, 346–354. [Google Scholar] [CrossRef] [PubMed]
- Cadenas-Sanchez, C.; Mora-Gonzalez, J.; Migueles, J.H.; Martin-Matillas, M.; Gomez-Vida, J.; Escolano-Margarit, M.V.; Maldonado, J.; Enriquez, G.M.; Pastor-Villaescusa, B.; de Teresa, C.; et al. An exercise-based randomized controlled trial on brain, cognition, physical health and mental health in overweight/obese children (ActiveBrains project): Rationale, design and methods. Contemp. Clin. Trials 2016, 47, 315–324. [Google Scholar] [CrossRef] [PubMed]
- Bervoets, L.; Massa, G. Defining morbid obesity in children based on BMI 40 at age 18 using the extended international (IOTF) cut-offs. Pediatr. Obes. 2014, 9, 94–98. [Google Scholar] [CrossRef] [PubMed]
- Cole, T.J.; Lobstein, T. Extended international (IOTF) body mass index cut-offs for thinness, overweight and obesity. Pediatr. Obes. 2012, 7, 284–294. [Google Scholar] [CrossRef] [PubMed]
- Ashburner, J.; Friston, K.J. Unified segmentation. Neuroimage 2005, 26, 839–851. [Google Scholar] [CrossRef] [PubMed]
- Ashburner, J. A fast diffeomorphic image registration algorithm. Neuroimage 2007, 38, 95–113. [Google Scholar] [CrossRef]
- Ashburner, J.; Friston, K.J. Voxel-based morphometry--the methods. Neuroimage 2000, 11, 805–821. [Google Scholar] [CrossRef]
- Schrank, F.A.; McGrew, K.S.; Woodcock, R.W. Woodcock-Johnson® III. Available online: https://www.hmhco.com/~/media/sites/home/hmh-assessments/clinical/woodcock-johnson/pdf/wjiii/wjiii_asb2.pdf?la=en (accessed on 30 May 2018).
- Leger, L.A.; Mercier, D.; Gadoury, C.; Lambert, J. The multistage 20 metre shuttle run test for aerobic fitness. J. Sports Sci. 1988, 6, 93–101. [Google Scholar] [CrossRef]
- Mirwald, R.L.; Baxter-Jones, A.D.; Bailey, D.A.; Beunen, G.P. An assessment of maturity from anthropometric measurements. Med. Sci. Sports Exerc. 2002, 34, 689–694. [Google Scholar]
- Song, X.-W.; Dong, Z.-Y.; Long, X.-Y.; Li, S.-F.; Zuo, X.-N.; Zhu, C.-Z.; He, Y.; Yan, C.-G.; Zang, Y.-F. REST: A Toolkit for Resting-State Functional Magnetic Resonance Imaging Data Processing. PLoS ONE 2011, 6, e25031. [Google Scholar] [CrossRef] [PubMed]
- Hayasaka, S.; Phan, K.L.; Liberzon, I.; Worsley, K.J.; Nichols, T.E. Nonstationary cluster-size inference with random field and permutation methods. Neuroimage 2004, 22, 676–687. [Google Scholar] [CrossRef] [PubMed]
- Bruehl, H.; Sweat, V.; Tirsi, A.; Shah, B.; Convit, A. Obese Adolescents with Type 2 Diabetes Mellitus Have Hippocampal and Frontal Lobe Volume Reductions. Neurosci. Med. 2011, 2, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Nouwen, A.; Chambers, A.; Chechlacz, M.; Higgs, S.; Blissett, J.; Barrett, T.G.; Allen, H.A. Microstructural abnormalities in white and gray matter in obese adolescents with and without type 2 diabetes. Neuroimage 2017, 16, 43–51. [Google Scholar] [CrossRef]
- Perlaki, G.; Molnar, D.; Smeets, P.A.M.; Ahrens, W.; Wolters, M.; Eiben, G.; Lissner, L.; Erhard, P.; Meer, F.v.; Herrmann, M.; et al. Volumetric gray matter measures of amygdala and accumbens in childhood overweight/obesity. PLoS ONE 2018, 13, e0205331. [Google Scholar] [CrossRef]
- Firat, R.B. Opening the “Black Box”: Functions of the Frontal Lobes and Their Implications for Sociology. Front. Sociol 2019, 4. [Google Scholar] [CrossRef]
- Primeau, V.; Coderre, L.; Karelis, A.D.; Brochu, M.; Lavoie, M.E.; Messier, V.; Sladek, R.; Rabasa-Lhoret, R. Characterizing the profile of obese patients who are metabolically healthy. Int. J. Obes. 2011, 35, 971–981. [Google Scholar] [CrossRef] [PubMed]
- Bluher, M. Are metabolically healthy obese individuals really healthy? Eur. J. End. 2014, 171, 209–219. [Google Scholar] [CrossRef]
- Cotman, C.W.; Berchtold, N.C.; Christie, L.A. Exercise builds brain health: Key roles of growth factor cascades and inflammation. Trends Neurosci. 2007, 30, 464–472. [Google Scholar] [CrossRef]
- Ortega, F.B.; Ruiz, J.R.; Labayen, I.; Lavie, C.J.; Blair, S.N. The Fat but Fit paradox: What we know and don’t know about it. Br. J. Sports Med. 2017, 52, 151–153. [Google Scholar] [CrossRef]
- Opel, N.; Martin, S.; Meinert, S.; Redlich, R.; Enneking, V.; Richter, M.; Goltermann, J.; Johnen, A.; Dannlowski, U.; Repple, J. White matter microstructure mediates the association between physical fitness and cognition in healthy, young adults. Sci. Rep. 2019, 9, 12885. [Google Scholar] [CrossRef] [PubMed]

| All (n = 97) | MHO (n = 52) | MUO (n = 45) | p | |
|---|---|---|---|---|
| Mean ± SD | Mean ± SD | Mean ± SD | ||
| Descriptive characteristics: | ||||
| Age (years) | 10.0 ± 1.2 | 9.9 ± 1.1 | 10.1 ± 1.2 | 0.473 |
| Peak height velocity (years) | −2.0 ± 1.0 | −2.2 ± 1.0 | −1.7 ± 0.9 | 0.031 |
| Weight (kg) | 56.0 ± 11.1 | 53.4 ± 11.2 | 59.0 ± 10.1 | 0.011 |
| Height (cm) | 144.1 ± 8.3 | 143.3 ± 8.4 | 144.9 ± 8.2 | 0.325 |
| Body mass index (kg/m2) | 26.8 ± 3.7 | 25.7 ± 3.5 | 28.0 ± 3.5 | 0.003 |
| Weight status (n, (%)) *: | 0.016 | |||
| Overweight | 24 (24.7) | 19, (36.5) | 5, (11.1) | |
| Obesity type I | 42 (43.3) | 21, (40.4) | 21, (46.7) | |
| Obesity type II | 19 (19.6) | 6, (11.5) | 13, (28.9) | |
| Obesity type III | 12 (12.4) | 6, (11.5) | 6, (13.3) | |
| Parental education (n (%)): | 0.248 | |||
| None with university studies | 65 (67.0) | 31 (59.6) | 34 (75.6) | |
| Only one with university studies | 17 (17.5) | 11 (21.2) | 6 (13.3) | |
| Both of them with university studies | 15 (15.5) | 10 (19.2) | 5 (11.1) | |
| Cardiorespiratory fitness: | ||||
| Cardiorespiratory fitness (VO2max) † | 40.8 ± 2.7 | 41.6 ± 2.6 | 39.8 ± 2.6 | 0.001 |
| Metabolic risk factors: | ||||
| Triglycerides (mg/dL) | 98.6 ± 57.7 | 73.3 ± 23.7 | 128.6 ± 72.8 | <0.001 |
| Glucose (mg/dL) | 86.3 ± 6.6 | 86.4 ± 5.8 | 86.4 ± 7.5 | 0.987 |
| High-Density Lipoprotein (mg/dL) | 50.3 ± 11.2 | 56.7 ± 9.7 | 42.6 ± 9.6 | <0.001 |
| Systolic blood pressure (mmHg) | 99.6 ± 12.9 | 98.9 ± 10.7 | 100.9 ± 15.2 | 0.458 |
| Diastolic blood pressure (mmHg) | 56.0 ± 12.3 | 55.2 ± 10.4 | 57.4 ± 14.1 | 0.383 |
| Academic achievement: | ||||
| Total achievement | 108.8 ± 12.4 | 111.38 ± 12.9 | 105.9 ± 11.2 | 0.028 |
| MHO (n = 52) > MUO (n = 45) | ||||||||
|---|---|---|---|---|---|---|---|---|
| Brain Regions | x | y | z | t | Cluster Size | Hemisphere | Effect Size | |
| Cohen’s d | 95% CI | |||||||
| Model 1: | ||||||||
| Fusiform gyrus | 44 | −33 | −20 | 4.33 | 2008 | Right | 0.82 | 0.23, 1.05 |
| −41 | −30 | −27 | 4.35 | 1581 | Left | 0.57 | 0.16, 0.98 | |
| Calcarine | −12 | −83 | 2 | 4.33 | 948 | Left | 0.72 | 0.31, 1.13 |
| 18 | −66 | 14 | 3.69 | 662 | Right | 0.61 | 0.20, 1.01 | |
| Lingual gyrus | −20 | −68 | −5 | 4.42 | 893 | Left | 0.67 | 0.26, 1.08 |
| 20 | −77 | −6 | 4.85 | 386 | Right | 0.80 | 0.38, 1.21 | |
| Middle occipital gyrus | 41 | −80 | 14 | 3.72 | 120 | Right | 0.57 | 0.17, 0.98 |
| Superior temporal gyrus | 36 | 20 | −33 | 3.99 | 93 | Right | 0.64 | 0.23, 1.05 |
| Inferior temporal gyrus | −38 | −6 | −35 | 3.74 | 76 | Left | 0.53 | 0.12, 0.93 |
| Model 2: | ||||||||
| Fusiform gyrus | −41 | −30 | −27 | 4.08 | 700 | Left | 0.39 | 0.06, 0.79 |
| 44 | −33 | −20 | 4.64 | 427 | Right | 0.68 | 0.27, 1.09 | |
| Calcarine | −12 | −83 | 2 | 4.19 | 487 | Left | 0.58 | 0.17, 0.98 |
| Lingual gyrus | −20 | −68 | −5 | 4.15 | 388 | Left | 0.50 | 0.09, 0.90 |
| 20 | −75 | −6 | 4.62 | 256 | Right | 0.62 | 0.20, 1.02 | |
| Middle occipital gyrus | 41 | −78 | 12 | 3.67 | 94 | Right | 0.47 | 0.06, 0.87 |
| Superior temporal gyrus | ns | ns | ns | ns | ns | ns | ns | ns |
| Inferior temporal gyrus | ns | ns | ns | ns | ns | ns | ns | ns |
| Model 1 | Model 2 | ||||||
|---|---|---|---|---|---|---|---|
| Coordinates (x, y, z) | β | p | β | p | |||
| Regional gray matter: | |||||||
| Fusiform gyrus | 44 | −33 | −20 | 0.171 | 0.065 | −0.080 | 0.395 |
| −41 | −30 | −27 | 0.034 | 0.713 | 0.062 | 0.514 | |
| Calcarine | −12 | −83 | 2 | 0.006 | 0.959 | 0.104 | 0.275 |
| 18 | −66 | 14 | −0.012 | 0.901 | - | - | |
| Lingual gyrus | −20 | −68 | −5 | −0.188 | 0.052 | 0.076 | 0.433 |
| 20 | −77 | −6 | 0.042 | 0.672 | 0.028 | 0.772 | |
| Middle occipital gyrus | 41 | −80 | 14 | 0.030 | 0.751 | −0.071 | 0.473 |
| Superior temporal gyrus | 36 | 20 | −33 | 0.094 | 0.350 | - | - |
| Inferior temporal gyrus | −38 | −6 | −35 | 0.139 | 0.167 | - | - |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cadenas-Sanchez, C.; Esteban-Cornejo, I.; Migueles, J.H.; Labayen, I.; Verdejo-Román, J.; Mora-Gonzalez, J.; Henriksson, P.; Maldonado, J.; Gómez-Vida, J.; Hillman, C.H.; et al. Differences in Brain Volume between Metabolically Healthy and Unhealthy Overweight and Obese Children: The Role of Fitness. J. Clin. Med. 2020, 9, 1059. https://doi.org/10.3390/jcm9041059
Cadenas-Sanchez C, Esteban-Cornejo I, Migueles JH, Labayen I, Verdejo-Román J, Mora-Gonzalez J, Henriksson P, Maldonado J, Gómez-Vida J, Hillman CH, et al. Differences in Brain Volume between Metabolically Healthy and Unhealthy Overweight and Obese Children: The Role of Fitness. Journal of Clinical Medicine. 2020; 9(4):1059. https://doi.org/10.3390/jcm9041059
Chicago/Turabian StyleCadenas-Sanchez, Cristina, Irene Esteban-Cornejo, Jairo H. Migueles, Idoia Labayen, Juan Verdejo-Román, Jose Mora-Gonzalez, Pontus Henriksson, José Maldonado, José Gómez-Vida, Charles H. Hillman, and et al. 2020. "Differences in Brain Volume between Metabolically Healthy and Unhealthy Overweight and Obese Children: The Role of Fitness" Journal of Clinical Medicine 9, no. 4: 1059. https://doi.org/10.3390/jcm9041059
APA StyleCadenas-Sanchez, C., Esteban-Cornejo, I., Migueles, J. H., Labayen, I., Verdejo-Román, J., Mora-Gonzalez, J., Henriksson, P., Maldonado, J., Gómez-Vida, J., Hillman, C. H., Erickson, K. I., Kramer, A. F., Catena, A., & Ortega, F. B. (2020). Differences in Brain Volume between Metabolically Healthy and Unhealthy Overweight and Obese Children: The Role of Fitness. Journal of Clinical Medicine, 9(4), 1059. https://doi.org/10.3390/jcm9041059






