Working Alliance in Blended Versus Face-to-Face Cognitive Behavioral Treatment for Patients with Depression in Specialized Mental Health Care
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants
2.3. Procedures
2.4. Random Allocation
2.5. Interventions
2.6. Therapists
2.7. Measures
2.8. Statistical Analyses
3. Results
3.1. Patients
3.2. Study Dropout
3.3. Treatment Received
3.4. Working Alliance
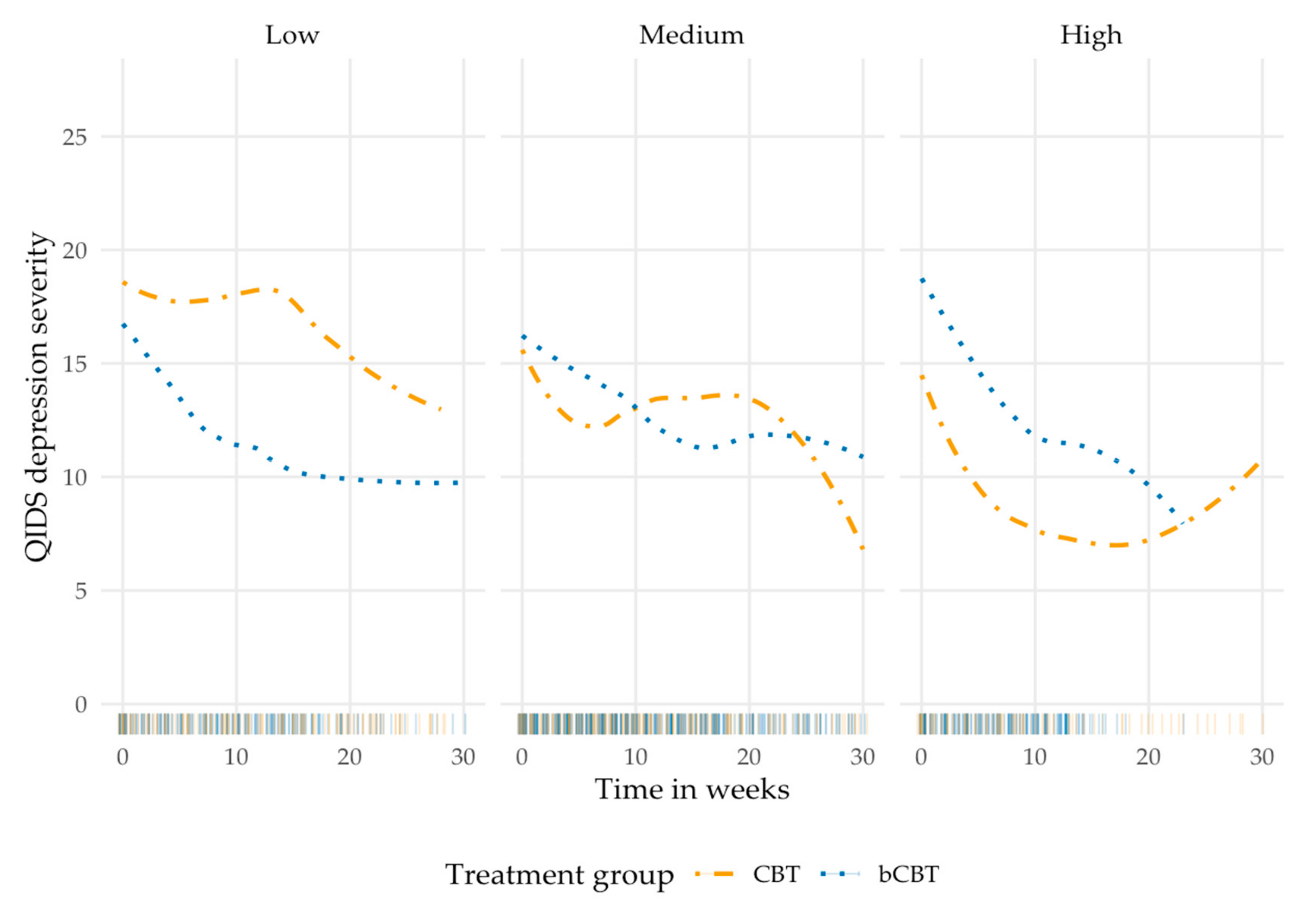
3.5. Working Alliance and Depression Severity
4. Discussion
4.1. Working Alliance between Patients and Therapists
4.2. Association between Working Alliance and Depressive Symptoms
4.3. Change in Depressive Symptoms
4.4. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Kessler, R.C.; Chiu, W.T.; Demler, O.; Merikangas, K.R.; Walters, E.E. Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch. Gen. Psychiatry 2005, 62, 617–627. [Google Scholar] [CrossRef]
- Kohn, R.; Saxena, S.; Levav, I.; Saraceno, B. The treatment gap in mental health care. Bull. World Health Organ. 2004, 82, 858–866. [Google Scholar] [PubMed]
- Demyttenaere, K.; Bruffaerts, R.; Posada-Villa, J.; Gasquet, I.; Kovess, V.; Lepine, J.P.; Angermeyer, M.C.; Bernert, S.; de Girolamo, G.; Morosini, P.; et al. Prevalence, severity, and unmet need for treatment of mental disorders in the World Health Organization World Mental Health Surveys. JAMA 2004, 291, 2581–2590. [Google Scholar] [PubMed]
- Bremmer, F.; van Es, M. Een Analyse van de Verwachte Kosten en Baten Van Ehealth: Blended Behandelen en Begeleiden; GGZ Nederland: Amersfoort, The Netherlands, 2013. [Google Scholar]
- Van’t Hof, E.; Cuijpers, P.; Stein, D.J. Self-help and Internet-guided interventions in depression and anxiety disorders: A systematic review of meta-analyses. CNS Spectr. 2009, 14, 34–40. [Google Scholar] [PubMed]
- Cuijpers, P.; Donker, T.; van Straten, A.; Li, J.; Andersson, G. Is guided self-help as effective as face-to-face psychotherapy for depression and anxiety disorders? A systematic review and meta-analysis of comparative outcome studies. Psychol. Med. 2010, 40, 1943–1957. [Google Scholar] [CrossRef]
- Mohr, D.C.; Lyon, A.R.; Lattie, E.G.; Reddy, M.; Schueller, S.M. Accelerating digital mental health research from early design and creation to successful implementation and sustainment. J. Med. Internet Res. 2017, 19, e153. [Google Scholar] [CrossRef]
- Schröder, J.; Berger, T.; Westermann, S.; Klein, J.P.; Moritz, S. Internet interventions for depression: New developments. Dialogues Clin. Neurosci. 2016, 18, 203–212. [Google Scholar]
- Andersson, G.; Cuijpers, P.; Carlbring, P.; Riper, H.; Hedman, E. Guided Internet-based vs. face-to-face cognitive behavior therapy for psychiatric and somatic disorders: A systematic review and meta-analysis. World Psychiatry 2014, 13, 288–295. [Google Scholar] [CrossRef]
- Cuijpers, P.; Riper, H. Internet Interventions for depressive disorders: An overview. Revista de Psicopatología y Psicol. Clínica 2014, 19, 209–216. [Google Scholar] [CrossRef]
- Richards, D.; Richardson, T. Computer-based psychological treatments for depression: A systematic review and meta-analysis. Clin. Psychol. Rev. 2012, 32, 329–342. [Google Scholar] [CrossRef]
- Andrews, G.; Basu, A.; Cuijpers, P.; Craske, M.G.; McEvoy, P.; English, C.L.; Newby, J.M. Computer therapy for the anxiety and depression disorders is effective, acceptable and practical health care: An updated meta-analysis. J. Anxiety Disord. 2018, 55, 70–78. [Google Scholar] [CrossRef] [PubMed]
- Carlbring, P.; Andersson, G.; Cuijpers, P.; Riper, H.; Hedman-Lagerlöf, E. Internet-based vs. face-to-face cognitive behavior therapy for psychiatric and somatic disorders: An updated systematic review and meta-analysis. Cogn. Behav. Ther. 2018, 47, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Cuijpers, P.; Donker, T.; Johansson, R.; Mohr, D.C.; van Straten, A.; Andersson, G. Self-guided psychological treatment for depressive symptoms: A meta-analysis. PLoS ONE 2011, 6, e21274. [Google Scholar] [CrossRef] [PubMed]
- Andersson, G.; Rozental, A.; Shafran, R.; Carlbring, P. Long-term effects of internet-supported cognitive behaviour therapy. Expert Rev. Neurother. 2017, 18, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Kleiboer, A.; Smit, J.; Bosmans, J.; Ruwaard, J.; Andersson, G.; Topooco, N.; Berger, T.; Krieger, T.; Botella, C.; Baños, R.; et al. European COMPARative Effectiveness research on blended Depression treatment versus treatment-as-usual (E-COMPARED): Study protocol for a randomized controlled, non-inferiority trial in eight European countries. Trials 2016, 17, 387. [Google Scholar] [CrossRef]
- Høifødt, R.S.; Lillevoll, K.R.; Griffiths, K.M.; Wilsgaard, T.; Eisemann, M.; Waterloo, K.; Kolstrup, N. The clinical effectiveness of web-based cognitive behavioral therapy with face-to-face therapist support for depressed primary care patients: Randomized controlled trial. J. Med. Internet Res. 2013, 15, e153. [Google Scholar] [CrossRef]
- Van der Vaart, R.; Witting, M.; Riper, H.; Kooistra, L.; Bohlmeijer, E.T.; van Gemert-Pijnen, L.J.E.W.C. Blending online therapy into regular face-to-face therapy for depression: Content, ratio and preconditions according to patients and therapists using a Delphi study. BMC Psychiatry 2014, 14, 355. [Google Scholar] [CrossRef]
- Kenter, R.M.F.; van de Ven, P.M.; Cuijpers, P.; Koole, G.; Niamat, S.; Gerrits, R.S.; Willems, M.; van Straten, A. Costs and effects of Internet cognitive behavioral treatment blended with face-to-face treatment: Results from a naturalistic study. Internet Interv. 2015, 2, 77–83. [Google Scholar] [CrossRef]
- Kooistra, L.C.; Ruwaard, J.; Wiersma, J.E.; van Oppen, P.; van der Vaart, R.; van Gemert-Pijnen, J.E.W.C.; Riper, H. Development and initial evaluation of blended cognitive behavioural treatment for major depression in routine specialized mental health care. Internet Interv. 2016, 4, 61–71. [Google Scholar] [CrossRef]
- Erbe, D.; Eichert, H.-C.; Riper, H.; Ebert, D.D. Blending face-to-face and Internet-based interventions for the treatment of mental disorders in adults: Systematic review. J. Med. Internet Res. 2017, 19, e306. [Google Scholar] [CrossRef]
- Thase, M.E.; Wright, J.H.; Eells, T.D.; Barrett, M.S.; Wisniewski, S.R.; Balasubramani, G.K.; McCrone, P.; Brown, G.K. Improving the efficiency of psychotherapy for depression: Computer-assisted versus standard CBT. Am. J. Psychiatry 2018, 175, 242–250. [Google Scholar] [CrossRef] [PubMed]
- Berger, T.; Krieger, T.; Sude, K.; Meyer, B.; Maercker, A. Evaluating an e-mental health program (“deprexis”) as adjunctive treatment tool in psychotherapy for depression: Results of a pragmatic randomized controlled trial. J. Affect. Disord. 2018, 227, 455–462. [Google Scholar] [CrossRef] [PubMed]
- Kooistra, L.C.; Wiersma, J.E.; Ruwaard, J.; Neijenhuijs, K.; Lokkerbol, J.; van Oppen, P.; Smit, F.; Riper, H. Costs and effectiveness of blended versus standard cognitive behavioral therapy for depressed outpatients in routine specialized mental health care: Pilot randomized controlled trial. J. Med. Internet Res. 2019, 21, e14261. [Google Scholar] [CrossRef] [PubMed]
- Wampold, B.E. How important are the common factors in psychotherapy? An update. World Psychiatry 2015, 14, 270–277. [Google Scholar] [CrossRef] [PubMed]
- Horvath, A.O.; Del Re, A.C.; Flückiger, C.; Symonds, D. Alliance in individual psychotherapy. Psychotherapy 2011, 48, 9–16. [Google Scholar] [CrossRef]
- Zilcha-Mano, S. Is the alliance really therapeutic? Revisiting this question in light of recent methodological advances. Am. Psychol. 2017, 72, 311–325. [Google Scholar] [CrossRef]
- Flückiger, C.; Del, A.C.; Wampold, B.E.; Horvath, A.O. The alliance in adult psychotherapy: A meta-analytic synthesis. Psychotherapy 2018, 55, 316–340. [Google Scholar] [CrossRef]
- Cameron, S.K.; Rodgers, J.; Dagnan, D. The relationship between the therapeutic alliance and clinical outcomes in cognitive behaviour therapy for adults with depression: A meta-analytic review. Clin. Psychol. Psychother. 2018, 25, 446–456. [Google Scholar] [CrossRef]
- Laws, H.B.; Constantino, M.J.; Sayer, A.G.; Klein, D.N.; Kocsis, J.H.; Manber, R.; Markowitz, J.C.; Rothbaum, B.O.; Steidtmann, D.; Thase, M.E.; et al. Convergence in patient-therapist therapeutic alliance ratings and its relation to outcome in chronic depression treatment. Psychother. Res. 2017, 27, 410–424. [Google Scholar] [CrossRef]
- Lorenzo-Luaces, L.; Driessen, E.; DeRubeis, R.J.; Van, H.L.; Keefe, J.R.; Hendriksen, M.; Dekker, J. Moderation of the alliance-outcome association by prior depressive episodes: Differential ffects in cognitive-behavioral therapy and short-term psychodynamic supportive psychotherapy. Behav. Ther. 2017, 48, 581–595. [Google Scholar] [CrossRef]
- Berger, T. The therapeutic alliance in internet interventions: A narrative review and suggestions for future research. Psychother. Res. 2017, 27, 511–524. [Google Scholar] [CrossRef] [PubMed]
- Preschl, B.; Maercker, A.; Wagner, B. The working alliance in a randomized controlled trial comparing online with face-to-face cognitive-behavioral therapy for depression. BMC Psychiatry 2011, 11, 189. [Google Scholar] [CrossRef] [PubMed]
- Vernmark, K.; Hesser, H.; Topooco, N.; Berger, T.; Riper, H.; Luuk, L.; Backlund, L.; Carlbring, P.; Andersson, G. Working alliance as a predictor of change in depression during blended cognitive behaviour therapy. Cogn. Behav. Ther. 2019, 48, 285–299. [Google Scholar] [CrossRef] [PubMed]
- Kooistra, L.C.; Wiersma, J.E.; Ruwaard, J.; van Oppen, P.; Smit, F.; Lokkerbol, J.; Cuijpers, P.; Riper, H. Blended vs. face-to-face cognitive behavioural treatment for major depression in specialized mental health care: Study protocol of a randomized controlled cost-effectiveness trial. BMC Psychiatry 2014, 14, 290. [Google Scholar] [CrossRef] [PubMed]
- Sheehan, D.V.; Lecrubier, Y.; Sheehan, K.H.; Amorim, P.; Janavs, J.; Weiller, E.; Hergueta, T.; Baker, R.; Dunbar, G.C. The Mini-International Neuropsychiatric Interview (M.I.N.I.): The development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J. Clin. Psychiatry 1998, 59 (Suppl. 2), 22–33, quiz 34–57. [Google Scholar] [PubMed]
- Van Vliet, I.M.; De Beurs, E. Het Mini Internationaal Neuropsychiatrisch Interview (MINI). Een kort gestructureerd diagnostisch psychiatrisch interview voor DSM-IV en ICD-10-stoornissen. Tijdschr. Psychiatr. 2007, 49, 393–397. [Google Scholar]
- Bockting, C.L.H.; Huibers, M.J.H. Protocollaire Behandeling Van Patienten Met Een Depressieve Stoornis. In Protocollaire Behandelingen Voor Volwassenen Met Psychische Klachten 1; Keijsers, G.P.J., van Minnen, A., Hoogduin, C.A.L., Eds.; Uitgeverij Boom: Amsterdam, The Netherlands, 2011; pp. 251–288. ISBN 9789461057723. [Google Scholar]
- Beck, A.T.; Rush, A.J.; Shaw, B.F.; Emery, G. Cognitive Therapy of Depression; Guilford: New York, NY, USA, 1979; ISBN 0898620007. [Google Scholar]
- Rush, A.J.; Trivedi, M.H.; Ibrahim, H.M.; Carmody, T.J.; Arnow, B.; Klein, D.N.; Markowitz, J.C.; Ninan, P.T.; Kornstein, S.; Manber, R.; et al. The 16-Item Quick Inventory of Depressive Symptomatology (QIDS), clinician rating (QIDS-C), and self-report (QIDS-SR): A psychometric evaluation in patients with chronic major depression. Biol. Psychiatry 2003, 54, 573–583. [Google Scholar] [CrossRef]
- Bordin, E.S. The generalizability of the psychoanalytic concept of the working alliance. Psychother. Theory, Res. Pract. 1979, 16, 252–260. [Google Scholar] [CrossRef]
- Horvath, A.O.; Greenberg, L.S. Development and validation of the Working Alliance Inventory. J. Couns. Psychol. 1989, 36, 223–233. [Google Scholar] [CrossRef]
- Hatcher, R.L.; Gillaspy, J.A. Development and validation of a revised short version of the working alliance inventory. Psychother. Res. 2006, 16, 12–25. [Google Scholar] [CrossRef]
- Stinckens, N.; Ulburghs, A.; Claes, L. De werkalliantie als sleutelelement in het therapiegebeuren: Meting met behulp van de WAV-12, de Nederlandstalige versie. Tijdschr. Klin. Psychol. 2009, 39, 44–60. [Google Scholar]
- Munder, T.; Wilmers, F.; Leonhart, R.; Linster, H.W.; Barth, J. Working alliance inventory-short revised (WAI-SR): Psychometric properties in outpatients and inpatients. Clin. Psychol. Psychother. 2010, 17, 231–239. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, S.S.; Wilk, M.B. An analysis of variance test for normality (complete samples). Biometrika 1965, 52, 591–611. [Google Scholar] [CrossRef]
- Revelle, W. Psych: Procedures for Psychological, Psychometric and Personality Research; Northwestern University: Evanston, IL, USA, 2018. [Google Scholar]
- R Core Team. R: A Language and Environment for Statistical Computing; R Core Team: Vienna, Austria, 2017. [Google Scholar]
- Hesser, H. Modeling individual differences in randomized experiments using growth models: Recommendations for design, statistical analysis and reporting of results of internet interventions. Internet Interv. 2015, 2, 110–120. [Google Scholar] [CrossRef]
- White, I.R.; Carpenter, J.; Horton, N.J. Including all individuals is not enough: Lessons for intention-to-treat analysis. Clin. Trials 2012, 9, 396–407. [Google Scholar] [CrossRef]
- Holm, S. A simple sequentially rejective multiple test procedure. Scand. J. Stat. 1979, 6, 65–70. [Google Scholar]
- Bates, D.; Maechler, M.; Bolker, B.; Walker, S.; Christensen, R.H.B.; Singmann, H.; Dai, B.; Eigen, C. Linear Mixed-Effects Models using “Eigen” and S4; R package, version 1-1.21; 2017. [Google Scholar]
- Cuijpers, P.; Huibers, M.; Ebert, D.D.; Koole, S.L.; Andersson, G. How much psychotherapy is needed to treat depression? A metaregression analysis. J. Affect. Disord. 2013, 149, 1–13. [Google Scholar] [CrossRef]
| bCBT n = 47 | CBT n = 45 | Total n = 92 | |
|---|---|---|---|
| Demographic | |||
| Gender, female (n, %) | 30 (63.8) | 25 (55.6) | 43 (59.8) |
| Age (mean, SD) | 39.5 (11.4) | 37.7 (10.5) | 38.6 (11.0) |
| In a relationship (n, %) | 26 (55.3) | 27 (60.0) | 53 (57.6) |
| Education (n, %) | |||
| Low | 6 (12.8) | 1 (2.2) | 7 (7.6) |
| Middle | 24 (51.1) | 31 (68.9) | 55 (59.8) |
| High | 17 (36.2) | 13 (28.9) | 30 (32.6) |
| Employed (n, %) | 27 (57.5) | 26 (57.8) | 53 (57.6) |
| Nationality, Dutch (n, %) | 42 (89.4) | 44 (97.8) | 68 (93.5) |
| Clinical | |||
| Treatment preference, bCBT (n, %) | 30 (63.8) | 30 (66.7) | 60 (65.2) |
| Co-morbid disorder(s) (n, %) | 31 (66.0) | 30 (66.7) | 61 (66.3) |
| QIDS-SR (mean, SD) | 16.6 (4.9) | 15.9 (4.1) | 16.3 (4.6) |
| Antidepressant medication (n, %) | 32 (68.0) | 27 (60.0) | 59 (64.1) |
| bCBT n = 47 | CBT n = 45 | Total n = 92 | |
|---|---|---|---|
| Treatment received before assessment of working alliance: mean (SD) | |||
| Face-to-face sessions | 7.1 (2.1) | 6.6 (2.2) | 6.7 (2.2) |
| Online sessions | 7.9 (2.4) | - | - |
| Online feedback messages | 6.9 (2.5) | - | - |
| Therapist time in minutes | 636 (187) | 395 (132) | 518 (203) |
| Treatment received after assessment of working alliance: mean (SD) | |||
| Face-to-face sessions | 4.0 (2.7) | 7.5 (4.8) | 5.7 (4.3) |
| Online sessions | 2.7 (2.8) | - | - |
| Online feedback messages | 2.4 (2.6) | - | - |
| Therapist time in minutes | 308 (208) | 449 (289) | 377 (258) |
| Treatment received during the full study period: mean (SD) | |||
| Face-to-face sessions | 11.1 (3.5) | 14.1 (5.8) | 12.5 (5.0) |
| Online sessions | 10.3 (2.9) | - | - |
| Online feedback messages | 9.3 (3.5) | - | - |
| Therapist time in minutes | 944 (274) | 844 (348) | 895 (315) |
| Patients | Therapists | |||||||
|---|---|---|---|---|---|---|---|---|
| Mean difference | Mean difference | |||||||
| (95% CI) | (95% CI) | |||||||
| Outcome 1 | bCBT | CBT | Total | bCBT vs. CBT | bCBT | CBT | Total | bCBT vs. CBT |
| n = 39 | n = 34 | n = 73 | n = 46 | n = 44 | n = 90 | |||
| Goal | 16.3 (3.1) | 16.1 (3.2) | 16.2 (3.1) | 0.25 (−1.22; 1.71) | 12.4 (1.9) | 11.7 (1.8) | 12.1 (1.9) | 0.73 (0.04; 1.50) a |
| Scaled | 4.1 (0.8) | 4.0 (0.8) | 4.1 (0.8) | 4.1 (0.6) | 3.9 (0.6) | 4.0 (0.6) | ||
| Task | 12.4 (4.1) | 11.9 (4.2) | 12.2 (4.1) | 0.47 (−1.45; 2.40) | 12.1 (2.0) | 11.2 (1.6) | 11.7 (1.9) | 0.93 (0.17; 1.68) b |
| Scaled | 3.1 (1.0) | 3.0 (1.1) | 3.0 (1.0) | 4.0 (0.7) | 3.7 (0.5) | 3.9 (0.6) | ||
| Bond | 15.6 (3.3) | 14.7 (3.6) | 15.2 (3.4) | 0.97 (−0.64; 2.57) | 17.9 (1.9) | 17.6 (2.1) | 17.7 (2.0) | 0.28 (−0.52; 1.17) |
| Scaled | 3.9 (0.8) | 3.7 (0.9) | 3.8 (0.9) | 4.6 (0.5) | 4.4 (0.5) | 4.4 (0.5) | ||
| Composite | 3.7 (0.7) | 3.6 (0.8) | 3.6 (0.8) | 0.14 (−0.22; 0.50) | 4.2 (0.5) | 4.0 (0.4) | 4.1 (0.5) | 0.20 (0.00; 0.40) c |
| Dependent Variable | |||||
|---|---|---|---|---|---|
| Predictors | Estimates | SE | 95% CI | Statistic | p-value |
| (Intercept) | 14.96 | 0.88 | 13.25; 16.68 | 17.08 | <0.001 |
| Time × group × working alliance | 0.61 | 0.14 | 0.33; 0.89 | 4.25 | <0.001 |
| Quadratic time × group × working alliance | −0.03 | 0.00 | −0.04; −0.02 | −5.34 | <0.001 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kooistra, L.; Ruwaard, J.; Wiersma, J.; van Oppen, P.; Riper, H. Working Alliance in Blended Versus Face-to-Face Cognitive Behavioral Treatment for Patients with Depression in Specialized Mental Health Care. J. Clin. Med. 2020, 9, 347. https://doi.org/10.3390/jcm9020347
Kooistra L, Ruwaard J, Wiersma J, van Oppen P, Riper H. Working Alliance in Blended Versus Face-to-Face Cognitive Behavioral Treatment for Patients with Depression in Specialized Mental Health Care. Journal of Clinical Medicine. 2020; 9(2):347. https://doi.org/10.3390/jcm9020347
Chicago/Turabian StyleKooistra, Lisa, Jeroen Ruwaard, Jenneke Wiersma, Patricia van Oppen, and Heleen Riper. 2020. "Working Alliance in Blended Versus Face-to-Face Cognitive Behavioral Treatment for Patients with Depression in Specialized Mental Health Care" Journal of Clinical Medicine 9, no. 2: 347. https://doi.org/10.3390/jcm9020347
APA StyleKooistra, L., Ruwaard, J., Wiersma, J., van Oppen, P., & Riper, H. (2020). Working Alliance in Blended Versus Face-to-Face Cognitive Behavioral Treatment for Patients with Depression in Specialized Mental Health Care. Journal of Clinical Medicine, 9(2), 347. https://doi.org/10.3390/jcm9020347




