Using the Personalized Advantage Index for Individual Treatment Allocation to Blended Treatment or Treatment as Usual for Depression in Secondary Care
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample
2.2. Interventions
2.3. Measures
2.3.1. Primary Outcome
2.3.2. Predictor Variables
2.4. Data Analytical Strategy
2.4.1. Missing Data
2.4.2. Bayesian Model Averaging (BMA)
2.4.3. Personalized Advantage Index (PAI)
3. Results
3.1. Variables Predicting Outcome in TAU
3.2. Variables Predicting Outcome in the Nlended Treatment
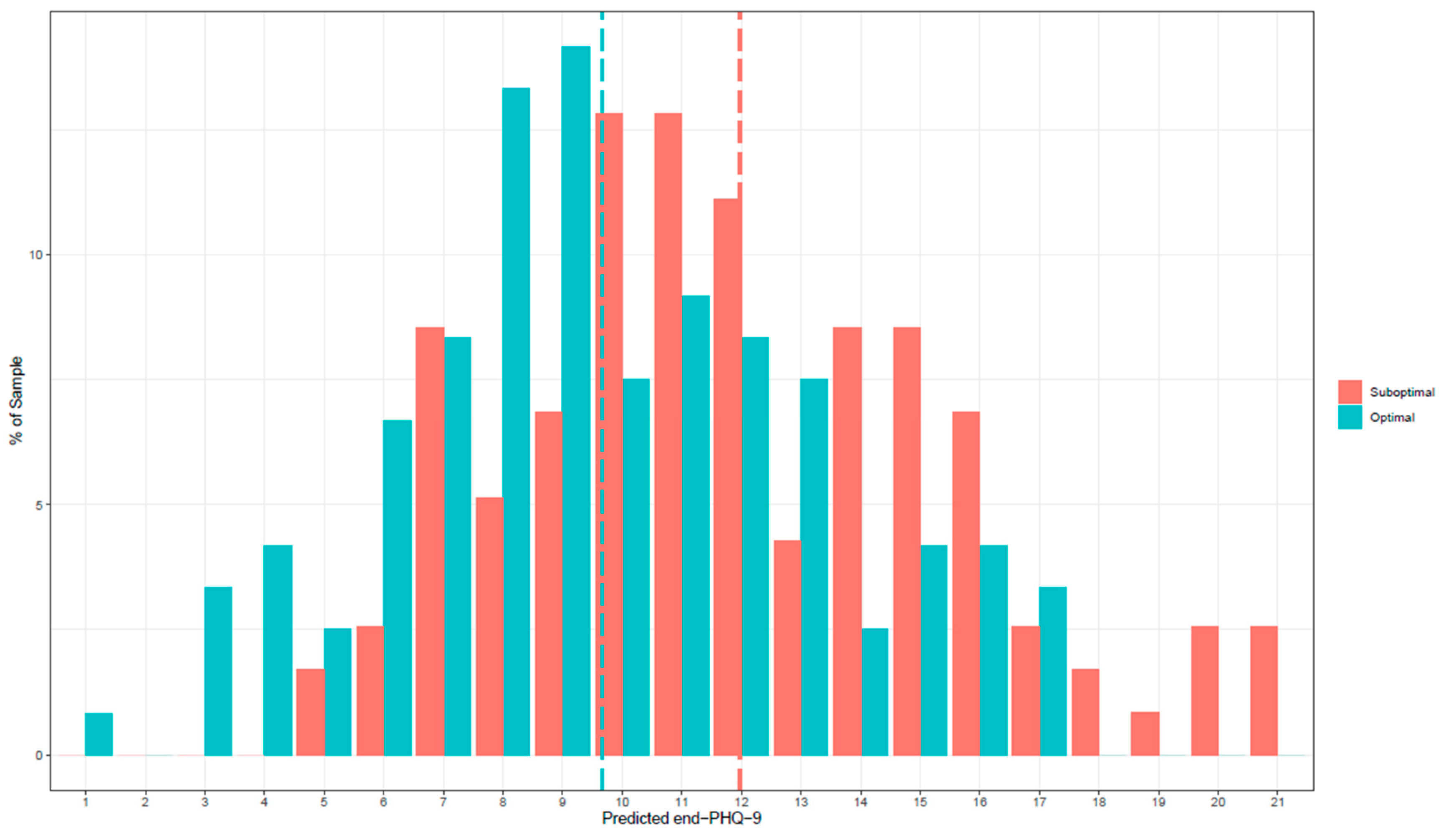
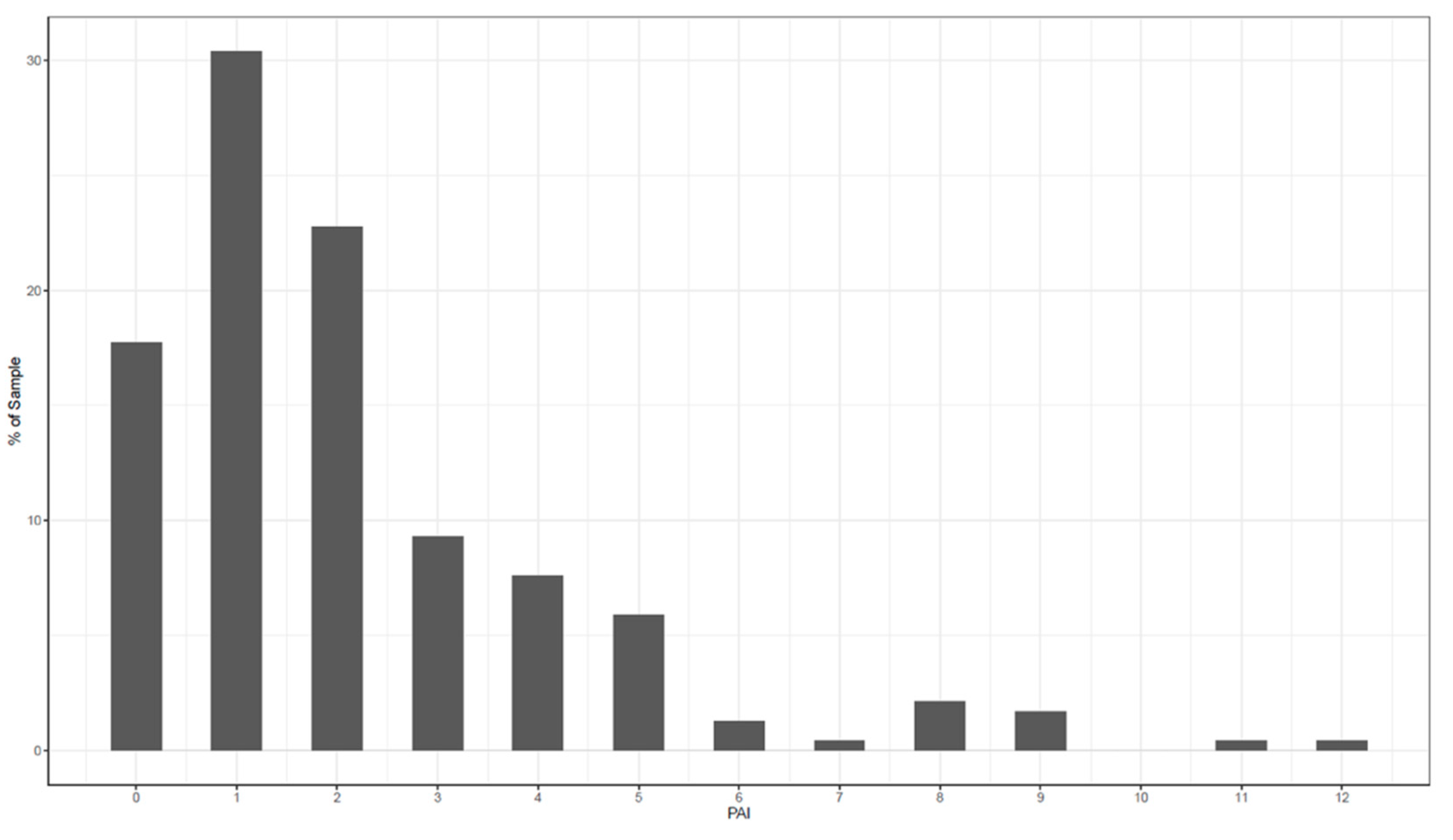
3.3. Personalized Advantage Index
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- World Health Organization. Depression. 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/depression (accessed on 21 November 2019).
- World Health Organization. The Global Burden of Disease: 2004 Update. 2008. Available online: https://www.who.int/healthinfo/global_burden_disease/2004_report_update/en/ (accessed on 3 October 2019).
- Kemmeren, L.; Van Schaik, D.J.; Riper, H.; Kleiboer, A.M.; Bosmans, J.E.; Smit, J.H. Effectiveness of blended depression treatment for adults in specialised mental healthcare: Study protocol for a randomised controlled trial. BMC Psychiatry 2016, 16, 113. [Google Scholar] [CrossRef] [PubMed]
- Karasu, T.B.; Gelenberg, A.; Merriam, A.; Wang, P. Treatment of patients with major depressive disorder. In American Psychiatric Association Practice Guidelines for the Treatment of Psychiatric Disorders Compendium; American Psychiatric Publishing: Washington, DC, USA, 2000; pp. 413–495. [Google Scholar]
- Cuijpers, P. Psychotherapies for adult depression: Recent developments. Curr. Opin. Psychiatry 2015, 28, 24–29. [Google Scholar] [CrossRef] [PubMed]
- Carlbring, P.; Andersson, G.; Cuijpers, P.; Riper, H.; Hedman-Lagerlöf, E. Internet-based vs. face-to-face cognitive behavior therapy for psychiatric and somatic disorders: An updated systematic review and meta-analysis. Cognit. Behav. Ther. 2018, 47, 1–18. [Google Scholar] [CrossRef]
- Arnberg, F.K.; Linton, S.J.; Hultcrantz, M.; Heintz, E.; Jonsson, U. Internet-delivered psychological treatments for mood and anxiety disorders: A systematic review of their efficacy, safety, and cost-effectiveness. PLoS ONE 2014, 9, e98118. [Google Scholar] [CrossRef]
- Gerhards, S.; De Graaf, L.; Jacobs, L.; Severens, J.; Huibers, M.; Arntz, A.; Riper, H.; Widdershoven, G.; Metsemakers, J.F.M.; Evers, S.M.A.A. Economic evaluation of online computerised cognitive–behavioural therapy without support for depression in primary care: Randomised trial. Br. J. Psychiatry 2010, 196, 310–318. [Google Scholar] [CrossRef]
- Richards, D.; Richardson, T. Computer-based psychological treatments for depression: A systematic review and meta-analysis. Clin. Psychol. Rev. 2012, 32, 329–342. [Google Scholar] [CrossRef]
- Krieger, T.; Meyer, B.; Sude, K.; Urech, A.; Maercker, A.; Berger, T. Evaluating an e-mental health program (“deprexis”) as adjunctive treatment tool in psychotherapy for depression: Design of a pragmatic randomized controlled trial. BMC Psychiatry 2014, 14, 285. [Google Scholar] [CrossRef]
- Hickie, I.B.; Davenport, T.A.; Luscombe, G.M.; Moore, M.; Griffiths, K.M.; Christensen, H. Practitioner-supported delivery of internet-based cognitive behaviour therapy: Evaluation of the feasibility of conducting a cluster randomised trial. Med. J. Aust. 2010, 192, S31–S35. [Google Scholar] [CrossRef]
- Høifødt, R.S.; Lillevoll, K.R.; Griffiths, K.M.; Wilsgaard, T.; Eisenmann, M.; Waterloo, K.; Kolstrup, N. The clinical effectiveness of web-based cognitive behavioral therapy with face-to-face therapist support for depressed primary care patients: Randomized controlled trial. J. Med. Int. Res. 2013, 15, e153. [Google Scholar]
- Kessler, D.; Lewis, G.; Kaur, S.; Wiles, N.; King, M.; Weich, S.; Sharp, D.J.; Araya, R.; Hollinghurst, S.; Peters, T.J. Therapist-delivered Internet psychotherapy for depression in primary care: A randomised controlled trial. Lancet 2009, 374, 628–634. [Google Scholar] [CrossRef]
- Kooistra, L.C.; Wiersma, J.E.; Ruwaard, J.; van Oppen, P.; Smit, F.; Lokkerbol, J.; Cuijpers, P.; Riper, H. Blended vs. face-to-face cognitive behavioural treatment for major depression in specialized mental health care: Study protocol of a randomized controlled cost-effectiveness trial. BMC Psychiatry 2014, 14, 290. [Google Scholar] [CrossRef]
- Robertson, L.; Smith, M.; Castle, D.; Tannenbaum, D. Using the Internet to enhance the treatment of depression. Aust. Psychiatry 2006, 14, 413–417. [Google Scholar] [CrossRef]
- Berger, T.; Krieger, T.; Sude, K.; Meyer, B.; Maercker, A. Evaluating an e-mental health program (“deprexis”) as adjunctive treatment tool in psychotherapy for depression: Results of a pragmatic randomized controlled trial. J. Affect. Disord. 2018, 227, 455–462. [Google Scholar] [CrossRef] [PubMed]
- Thase, M.E.; Wright, J.H.; Eells, T.D.; Barrett, M.S.; Wisniewski, S.R.; Balasubramani, G.K.; McCrone, P.; Brown, G.K. Improving the efficiency of psychotherapy for depression: Computer-assisted versus standard CBT. Am. J. Psychiatry 2017, 175, 242–250. [Google Scholar] [CrossRef] [PubMed]
- Zwerenz, R.; Becker, J.; Knickenberg, R.J.; Siepmann, M.; Hagen, K.; Beutel, M.E. Online Self-Help as an Add-On to Inpatient Psychotherapy: Efficacy of a New Blended Treatment Approach. Psychother. Psychosom. 2017, 86, 341–350. [Google Scholar] [CrossRef] [PubMed]
- Erbe, D.; Eichert, H.-C.; Riper, H.; Ebert, D.D. Blending face-to-face and internet-based interventions for the treatment of mental disorders in adults: Systematic review. J. Med. Int. Res. 2017, 19, e306. [Google Scholar] [CrossRef] [PubMed]
- Wright, J.H.; Wright, A.S.; Albano, A.M.; Basco, M.R.; Goldsmith, L.J.; Raffield, T.; Otto, M.W. Computer-assisted cognitive therapy for depression: Maintaining efficacy while reducing therapist time. Am. J. Psychiatry 2005, 162, 1158–1164. [Google Scholar] [CrossRef]
- Clough, B.A.; Casey, L.M. Technological adjuncts to increase adherence to therapy: A review. Clin. Psychol. Rev. 2011, 31, 697–710. [Google Scholar] [CrossRef]
- Riper, H.; Van Ballegooijen, W.; Kooistra, L.; De Wit, J.; Donker, T. Preventie & eMental-Health-Prevention & eMental-Health; Vrije Universiteit Commissioned by ZonMw: Amsterdam, The Netherlands, 2013. [Google Scholar]
- Van der Vaart, R.; Witting, M.; Riper, H.; Kooistra, L.; Bohlmeijer, E.T.; van Gemert-Pijnen, L.J. Blending online therapy into regular face-to-face therapy for depression: Content, ratio and preconditions according to patients and therapists using a Delphi study. BMC Psychiatry 2014, 14, 355. [Google Scholar] [CrossRef]
- Wentzel, J.; van der Vaart, R.; Bohlmeijer, E.T.; van Gemert-Pijnen, J.E. Mixing online and face-to-face therapy: How to benefit from blended care in mental health care. JMIR Mental Health 2016, 3, e9. [Google Scholar] [CrossRef]
- Ruwaard, J.; Kok, R. Wild West eHealth: Time to hold our horses? Eur. Health Psychol. 2015, 17, 45–49. [Google Scholar]
- Zilcha-Mano, S. Major developments in methods addressing for whom psychotherapy may work and why. Psychother. Res. 2018, 29, 693–708. [Google Scholar] [CrossRef] [PubMed]
- Kazdin, A.E. Evidence-based treatment and practice: New opportunities to bridge clinical research and practice, enhance the knowledge base, and improve patient care. Am. Psychol. 2008, 63, 146. [Google Scholar] [CrossRef] [PubMed]
- Cuijpers, P.; Van Straten, A.; Bohlmeijer, E.; Hollon, S.D.; Andersson, G. The effects of psychotherapy for adult depression are overestimated: A meta-analysis of study quality and effect size. Psychol. Med. 2010, 40, 211–223. [Google Scholar] [CrossRef]
- Fournier, J.C.; DeRubeis, R.J.; Shelton, R.C.; Hollon, S.D.; Amsterdam, J.D.; Gallop, R. Prediction of response to medication and cognitive therapy in the treatment of moderate to severe depression. J. Consult. Clin. Psychol. 2009, 77, 775. [Google Scholar] [CrossRef]
- Cohen, Z.D.; DeRubeis, R.J. Treatment selection in depression. Ann. Rev. Clin. Psychol. 2018, 14, 209–236. [Google Scholar] [CrossRef]
- Fisher, A.J.; Boswell, J.F. Enhancing the personalization of psychotherapy with dynamic assessment and modeling. Assessment 2016, 23, 496–506. [Google Scholar] [CrossRef]
- Hollon, S.D.; Cohne, Z.D.; Singla, D.R.; Andrews, P. Recent Developments in the Treatment of Depression. Behav. Ther. 2019, 50, 257–269. [Google Scholar] [CrossRef]
- Hamburg, M.A.; Collins, F.S. The path to personalized medicine. N. Engl. J. Med. 2010, 363, 301–304. [Google Scholar] [CrossRef]
- Van Bronswijk, S.C.; Lemmens, L.H.; Keefe, J.R.; Huibers, M.J.; DeRubeis, R.J.; Peeters, F.P. A prognostic index for long-term outcome after successful acute phase cognitive therapy and interpersonal psychotherapy for major depressive disorder. Depress. Anxiety 2018, 36, 252–261. [Google Scholar] [CrossRef]
- Becker, D.; van Breda, W.; Funk, B.; Hoogendoorn, M.; Ruwaard, J.; Riper, H. Predictive modeling in e-mental health: A common language framework. Internet Interv. 2018, 12, 57–67. [Google Scholar] [CrossRef] [PubMed]
- DeRubeis, R.J.; Cohen, Z.D.; Forand, N.R.; Fournier, J.C.; Gelfand, L.A.; Lorenzo-Luaces, L. The Personalized Advantage Index: Translating research on prediction into individualized treatment recommendations. A demonstration. PLoS ONE 2014, 9, e83875. [Google Scholar] [CrossRef] [PubMed]
- Cohen, Z.D.; Kim, T.; Van, H.; Dekker, J.; Driessen, E. Recommending Cognitive-Behavioral Versus Psychodynamic Therapy for Mild to Moderate Adult Depression. Psychother. Res. 2017, 30, 137–150. [Google Scholar] [CrossRef] [PubMed]
- Friedl, N.; Berger, T.; Krieger, T.; Caspar, F.; Grosse Holtforth, M. Using the Personalized Advantage Index for individual treatment allocation to cognitive behavioral therapy (CBT) or a CBT with integrated exposure and emotion-focused elements (CBT-EE). Psychother. Res. 2019. [Google Scholar] [CrossRef]
- DeRubeis, R.J.; Hollon, S.D.; Amsterdam, J.D.; Shelton, R.C.; Young, P.R.; Salomon, R.M.; O’Reardon, J.P.; Lovett, M.L.; Gladis, M.M.; Brown, L.L. Cognitive therapy vs. medications in the treatment of moderate to severe depression. Arch. Gen. Psychiatry 2005, 62, 409–416. [Google Scholar] [CrossRef]
- Huibers, M.J.; Cohen, Z.D.; Lemmens, L.H.; Arntz, A.; Peeters, F.P.; Cuijpers, P.; DeRubeis, R.J. Predicting optimal outcomes in cognitive therapy or interpersonal psychotherapy for depressed individuals using the personalized advantage index approach. PLoS ONE 2015, 10, e0140771. [Google Scholar] [CrossRef]
- Van Breda, W.; Bremer, V.; Becker, D.; Hoogendoorn, M.; Funk, B.; Ruwaard, J.; Riper, H. Predicting therapy success for treatment as usual and blended treatment in the domain of depression. Internet Interv. 2018, 12, 100–104. [Google Scholar] [CrossRef]
- Bremer, V.; Becker, D.; Kolovos, S.; Funk, B.; Van Breda, W.; Hoogendoorn, M.; Riper, H. Predicting therapy success and costs for personalized treatment recommendations using baseline characteristics: Data-driven analysis. J. Med. Internet Res. 2018, 20, e10275. [Google Scholar] [CrossRef]
- Kleiboer, A.; Smit, J.; Bosmans, J.; Ruwaard, J.; Andersson, G.; Topooco, N.; Berger, T.; Krieger, T.; Botella, C.; Banos, R. European COMPARative Effectiveness research on blended Depression treatment versus treatment-as-usual (E-COMPARED): Study protocol for a randomized controlled, non-inferiority trial in eight European countries. Trials 2016, 17, 387. [Google Scholar] [CrossRef]
- Sheehan, D.V.; Lecrubier, Y.; Sheehan, K.H.; Amorim, P.; Janavs, J.; Weiller, E.; Hergueta, T.; Baker, R.; Dunbar, G.C. The Mini-International Neuropsychiatric Interview (MINI): The development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J. Clin. Psychiatry 1998, 59, 22–33. [Google Scholar]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef] [PubMed]
- Meyer, B.; Berger, T.; Caspar, F.; Beevers, C.G.; Andersson, G.; Weiss, M. Effectiveness of a Novel Integrative Online Treatment for Depression (Deprexis): Randomized Controlled Trial. J. Med. Internet Res. 2009, 11, e15. [Google Scholar] [CrossRef] [PubMed]
- Mathiasen, K.; Andersen, T.E.; Riper, H.; Kleiboer, A.A.; Roessler, K.K. Blended CBT versus face-to-face CBT: A randomised non-inferiority trial. BMC Psychiatry 2016, 16, 432. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K. Enhancing the clinical utility of depression screening. CMAJ Can. Med. Assoc. J. 2012, 184, 281–282. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K.; Spitzer, R.L. The PHQ-9: A new depression diagnostic and severity measure. Psychiatr. Ann. 2002, 32, 509–515. [Google Scholar] [CrossRef]
- Manea, L.; Gilbody, S.; McMillan, D. Optimal cut-off score for diagnosing depression with the Patient Health Questionnaire (PHQ-9): A meta-analysis. Can. Med. Assoc. J. 2012, 184, E191–E196. [Google Scholar] [CrossRef]
- EuroQol. EuroQol—A new facility for the measurement of health-related quality of life. Health Policy 1990, 16, 199–208. [Google Scholar]
- Bouwmans, C.; De Jong, K.; Timman, R.; Zijlstra-Vlasveld, M.; Van der Feltz-Cornelis, C.; Tan, S.S.; Hakkaart-van Roijen, L. Feasibility, reliability and validity of a questionnaire on healthcare consumption and productivity loss in patients with a psychiatric disorder (TiC-P). BMC Health Serv. Res. 2013, 13, 217. [Google Scholar] [CrossRef] [PubMed]
- Devilly, G.J.; Borkovec, T.D. Psychometric properties of the credibility/expectancy questionnaire. J. Behav. Ther. Exp. Psychiatry 2000, 31, 73–86. [Google Scholar] [CrossRef]
- Stekhoven, D.J. Missforest: Nonparametric Missing Value Imputation Using Random Forest; R Package Version, 1; Astrophysics Source Code Library: Leicester, UK, 2013. [Google Scholar]
- Stekhoven, D.J.; Buhlmann, P. MissForest: Non-parametric missing value imputation for mixed-type data. Bioinformatics 2012, 28, 112–118. [Google Scholar] [CrossRef]
- Waljee, A.K.; Mukherjee, A.; Singal, A.G.; Zhang, Y.; Warren, J.; Balis, U.; Marrero, J.; Zhu, J.; Higgins, P.D. Comparison of imputation methods for missing laboratory data in medicine. BMJ Open 2013, 3, e002847. [Google Scholar] [CrossRef]
- Peduzzi, P.; Concato, J.; Feinstein, A.R.; Holford, T.R. Importance of events per independent variable in proportional hazards regression analysis II. Accuracy and precision of regression estimates. J. Clin. Epidemiol. 1995, 48, 1503–1510. [Google Scholar] [CrossRef]
- Vittinghoff, E.; McCulloch, C.E. Relaxing the rule of ten events per variable in logistic and Cox regression. Am. J. Epidemiol. 2007, 165, 710–718. [Google Scholar] [CrossRef] [PubMed]
- Raftery, A.E.; Madigan, D.; Hoeting, J.A. Bayesian model averaging for linear regression models. J. Am. Stat. Assoc. 1997, 92, 179–191. [Google Scholar] [CrossRef]
- Stock, E.M.; Kimbrel, N.A.; Meyer, E.C.; Copeland, L.A.; Monte, R.; Zeber, J.E.; Gulliver, S.B.; Morissette, S.B. A Bayesian model averaging approach to examining changes in quality of life among returning Iraq and Afghanistan Veterans. Int. J. Methods Psychiatry Res. 2014, 23, 345–358. [Google Scholar] [CrossRef] [PubMed]
- Babyak, M.A. What you see may not be what you get: A brief, nontechnical introduction to overfitting in regression-type models. Psychosom. Med. 2004, 66, 411–421. [Google Scholar]
- Fragoso, T.M.; Bertoli, W.; Louzada, F. Bayesian model averaging: A systematic review and conceptual classification. Int. Stat. Rev. 2018, 86, 1–28. [Google Scholar] [CrossRef]
- Fernandez, C.; Ley, E.; Steel, M.F. Benchmark priors for Bayesian model averaging. J. Econom. 2001, 100, 381–427. [Google Scholar] [CrossRef]
- Fernandez, C.; Ley, E.; Steel, M.F. Model uncertainty in cross-country growth regressions. J. Appl. Econom. 2001, 16, 563–576. [Google Scholar] [CrossRef]
- Ley, E.; Steel, M.F.J. On the effect of prior assumptions in Bayesian model averaging with applications to growth regression. J. Appl. Econom. 2009, 24, 651–674. [Google Scholar] [CrossRef]
- Steel, M.F. Bayesian model averaging and forecasting. Bull. Inflat. Macroecon. Anal. 2011, 200, 30–41. [Google Scholar]
- Clyde, M.A. BAS: Bayesian Variable Selection and Model Averaging using Bayesian. In Adaptive Sampling; 2018; R Package Version 1.5.3; Available online: https://cran.r-project.org/web/packages/BAS/BAS.pdf (accessed on 15 September 2019).
- Clyde, M.A.; Ghosh, J.; Littman, M.L. Bayesian adaptive sampling for variable selection and model averaging. J. Comput. Gr. Stat. 2011, 20, 80–101. [Google Scholar] [CrossRef]
- Efron, B.; Gong, G. A leisurely look at the bootstrap, the jackknife, and cross-validation. Am. Stat. 1983, 37, 36–48. [Google Scholar]
- Deisenhofer, A.K.; Delgadillo, J.; Rubel, J.A.; Böhnke, J.R.; Zimmermann, D.; Schwartz, B.; Lutz, W. Individual treatment selection for patients with posttraumatic stress disorder. Depress. Anxiety 2018, 35, 541–550. [Google Scholar] [CrossRef]
- Lowe, B.; Unutzer, J.; Callahan, C.M.; Perkins, A.J.; Kroenke, K. Monitoring depression treatment outcomes with the patient health questionnaire-9. Med. Care 2004, 42, 1194–1201. [Google Scholar]
- Dinga, R.; Marquand, A.F.; Veltman, D.J.; Beekman, A.T.F.; Schoevers, R.A.; van Hemert, A.M.; Penninx, B.; Schmaal, L. Predicting the naturalistic course of depression from a wide range of clinical, psychological, and biological data: A machine learning approach. Transl. Psychiatry 2018, 8, 241. [Google Scholar] [CrossRef]
- Hamilton, K.E.; Dobson, K.S. Cognitive therapy of depression: Pretreatment patient predictors of outcome. Clin. Psychol. Rev. 2002, 22, 875–893. [Google Scholar] [CrossRef]
- Constantino, M.J.; Arnkoff, D.B.; Glass, C.R.; Ametrano, R.M.; Smith, J.Z. Expectations. J. Clin. Psychol. 2011, 67, 184–192. [Google Scholar] [CrossRef]
- Greenberg, R.P.; Constantino, M.J.; Bruce, N. Are patient expectations still relevant for psychotherapy process and outcome? Clin. Psychol. Rev. 2006, 26, 657–678. [Google Scholar] [CrossRef]
- Spek, V.; Nyklíček, I.; Cuijpers, P.; Pop, V. Predictors of outcome of group and internet-based cognitive behavior therapy. J. Affect. Disord. 2008, 105, 137–145. [Google Scholar] [CrossRef]
- Andersson, G.; Hedman, E. Effectiveness of guided internet-based cognitive behavior therapy in regular clinical settings. Verhaltenstherapie 2013, 23, 140–148. [Google Scholar] [CrossRef]
- Bower, P.; Kontopantelis, E.; Sutton, A.; Kendrick, T.; Richards, D.A.; Gillbody, S.; Knowles, S.; Cuijpers, P.; Andersson, G.; Christensen, H.; et al. Influence of initial severity of depression on effectiveness of low intensity interventions: Meta-analysis of individual patient data. BMJ (Clin. Res.) 2013, 346, f540. [Google Scholar] [CrossRef]
- Thase, M.E.; Reynolds, C.F.; Frank, E.; Simons, A.D. Response to cognitive-behavioral therapy in chronic depression. J. Psychother. Pract. Res. 1994, 3, 304–314. [Google Scholar]
- Blom, M.B.; Spinhoven, P.; Hoffman, T.; Jonker, K.; Hoencamp, E.; Haffmans, P.J.; van Dyck, R. Severity and duration of depression, not personality factors, predict short term outcome in the treatment of major depression. J. Affect. Disord. 2007, 104, 119–126. [Google Scholar] [CrossRef]
- Delgadillo, J.; Huey, D.; Bennett, H.; McMillan, D. Case complexity as a guide for psychological treatment selection. J. Consult. Clin. Psychol. 2017, 85, 835–853. [Google Scholar] [CrossRef]
- Luedtke, A.; Sadikova, E.; Kessler, R.C. Sample Size Requirements for Multivariate Models to Predict Between-Patient Differences in Best Treatments of Major Depressive Disorder. Clin. Psychol. Sci. 2019, 7, 445–461. [Google Scholar] [CrossRef]
- Van Bronswijk, S.C.; DeRubeis, R.J.; Lemmens, L.H.; Peeters, F.P.; Keefe, J.R.; Cohen, Z.D.; Huibers, M. Precision medicine for long-term depression outcomes using the Personalized Advantage Index approach: Cognitive therapy or interpersonal psychotherapy? Psychol. Med. 2019, 1–11. [Google Scholar] [CrossRef]
- Gillan, C.M.; Whelan, D.R. What big data can do for treatment in psychiatry. Curr. Opin. Behav. Sci. 2017, 18, 34–42. [Google Scholar] [CrossRef]
- Urech, A.; Krieger, T.; Möseneder, L.; Biaggi, A.; Vincent, A.; Poppe, C.; Meyer, B.; Riper, H.; Berger, T. A patient post hoc perspective on advantages and disadvantages of blended cognitive behaviour therapy for depression: A qualitative content analysis. Psychother. Res. 2019, 29, 986–998. [Google Scholar] [CrossRef]
| “How many times did you consult a general practitioner?” “How many times did you consult a psychologist?” “How many times did you consult a psychotherapist?”, “How many times did you consult a psychiatrist?”, and “How many times did you consult a professional from an ambulatory mental health institution?” “How many times did you consult a professional from a clinic for alcohol or drugs?” and “How many times did you consult self-help groups?” | “How many days did you spend in a day-time treatment program in a regular hospital?” “How many days did you spend in a day-time treatment program in a psychiatric hospital?” and “How many days did you use outpatient psychotherapeutic services in addition to your psychotherapy?” | “How many admissions to a regular hospital did you have?” and “How many admissions to a psychiatric hospital did you have?” “How many admissions to a rehabilitation clinic did you have?” “Do you have a paid job?” “Did health problems oblige you to call in sick from work at any time?” |
| Fit Indices | Model 1 | Model 2 | Model 3 | Model 4 | Model 5 |
|---|---|---|---|---|---|
| Bayes Factor | 1 | 0.934 | 0.597 | 0.572 | 0.510 |
| Number of Variables | 6 | 6 | 6 | 5 | 6 |
| R2 | 0.428 | 0.445 | 0.441 | 0.440 | 0.439 |
| Log Marginal Likelihood | 22.729 | 22.659 | 22.213 | 22.170 | 22.056 |
| Posterior Probabilities | 0.021 | 0.019 | 0.012 | 0.012 | 0.011 |
| Fit Indices | Model 1 | Model 2 | Model 3 | Model 4 | Model 5 |
|---|---|---|---|---|---|
| Bayes Factor | 1 | 0.887 | 0.577 | 0.525 | 0.516 |
| Number of Variables | 6 | 5 | 4 | 6 | 6 |
| R2 | 0.398 | 0.416 | 0.392 | 0.429 | 0.446 |
| Log Marginal Likelihood | 19.852 | 19.731 | 19.301 | 19.207 | 19.190 |
| Posterior Probabilities | 0.012 | 0.011 | 0.007 | 0.006 | 0.006 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Friedl, N.; Krieger, T.; Chevreul, K.; Hazo, J.B.; Holtzmann, J.; Hoogendoorn, M.; Kleiboer, A.; Mathiasen, K.; Urech, A.; Riper, H.; et al. Using the Personalized Advantage Index for Individual Treatment Allocation to Blended Treatment or Treatment as Usual for Depression in Secondary Care. J. Clin. Med. 2020, 9, 490. https://doi.org/10.3390/jcm9020490
Friedl N, Krieger T, Chevreul K, Hazo JB, Holtzmann J, Hoogendoorn M, Kleiboer A, Mathiasen K, Urech A, Riper H, et al. Using the Personalized Advantage Index for Individual Treatment Allocation to Blended Treatment or Treatment as Usual for Depression in Secondary Care. Journal of Clinical Medicine. 2020; 9(2):490. https://doi.org/10.3390/jcm9020490
Chicago/Turabian StyleFriedl, Nadine, Tobias Krieger, Karine Chevreul, Jean Baptiste Hazo, Jérôme Holtzmann, Mark Hoogendoorn, Annet Kleiboer, Kim Mathiasen, Antoine Urech, Heleen Riper, and et al. 2020. "Using the Personalized Advantage Index for Individual Treatment Allocation to Blended Treatment or Treatment as Usual for Depression in Secondary Care" Journal of Clinical Medicine 9, no. 2: 490. https://doi.org/10.3390/jcm9020490
APA StyleFriedl, N., Krieger, T., Chevreul, K., Hazo, J. B., Holtzmann, J., Hoogendoorn, M., Kleiboer, A., Mathiasen, K., Urech, A., Riper, H., & Berger, T. (2020). Using the Personalized Advantage Index for Individual Treatment Allocation to Blended Treatment or Treatment as Usual for Depression in Secondary Care. Journal of Clinical Medicine, 9(2), 490. https://doi.org/10.3390/jcm9020490





