Handling of Doubtful WBC Scintigraphies in Patients with Suspected Prosthetic Joint Infections
Abstract
1. Introduction
2. Experimental Section
2.1. Materials and Methods
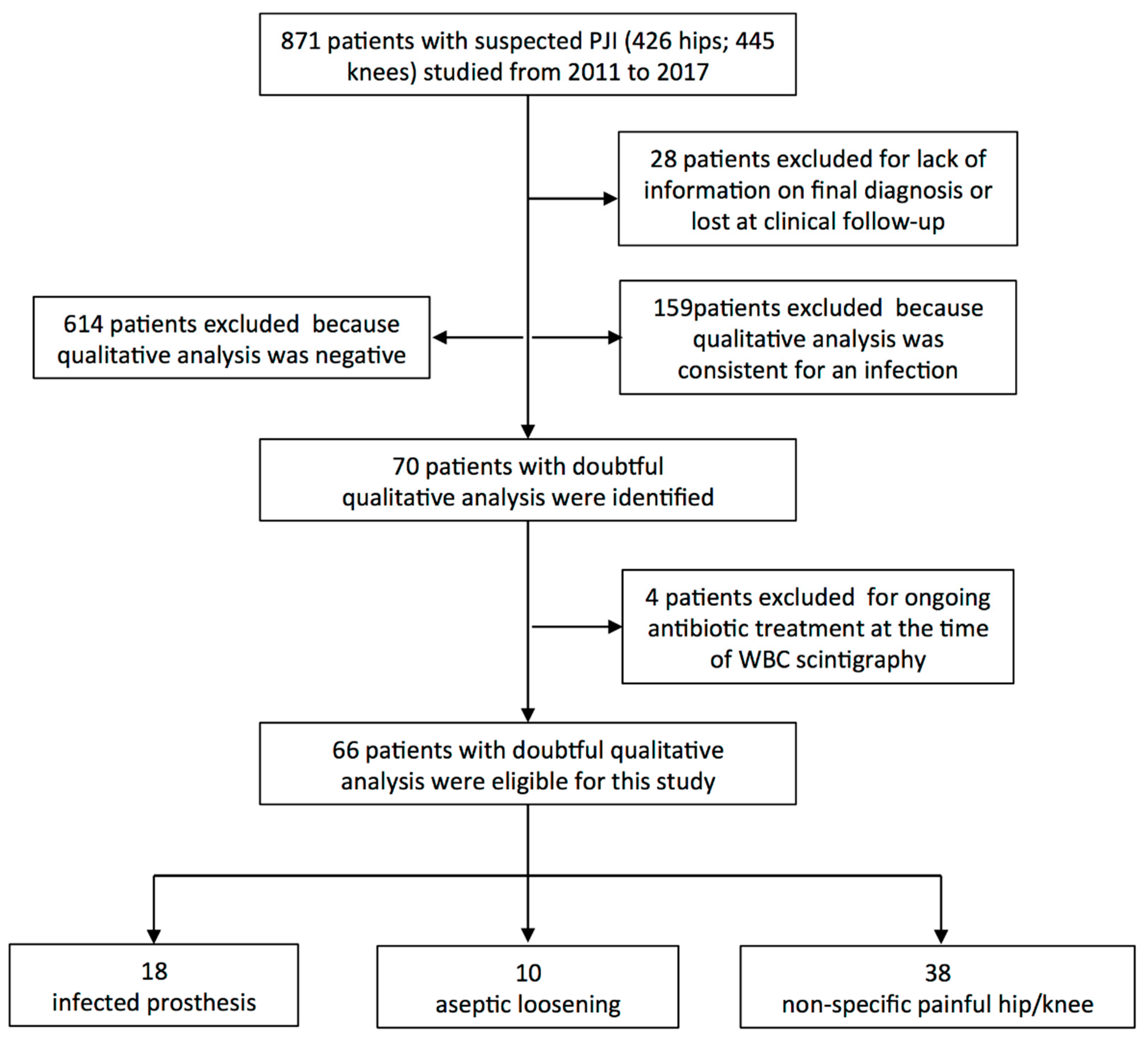
2.1.1. Patients
- Suspected mono-lateral PJI of hip or knee, according to IDSA criteria [22];
- Final diagnosis provided by gold standard;
- Equivocal WBC scintigraphy at visual analysis;
- BMS, if available;
- Raised inflammatory markers, if available.
- Clearly positive or negative scintigraphy at qualitative analysis;
- Lack of information on final diagnosis;
- Patients lost at clinical follow-up;
- Patients with suspected bilateral prosthesis;
- Ongoing antibiotic treatment at the time of WBC scintigraphy.
2.1.2. Acquisition Protocol and Image Display of WBC Scintigraphy
- early planar images (30 min: 1 h p.i.) were acquired for 100 s;
- delayed planar images (3 h p.i) were acquired for 141 s;
- late planar images (20 h p.i.) were acquired for 1007 s.
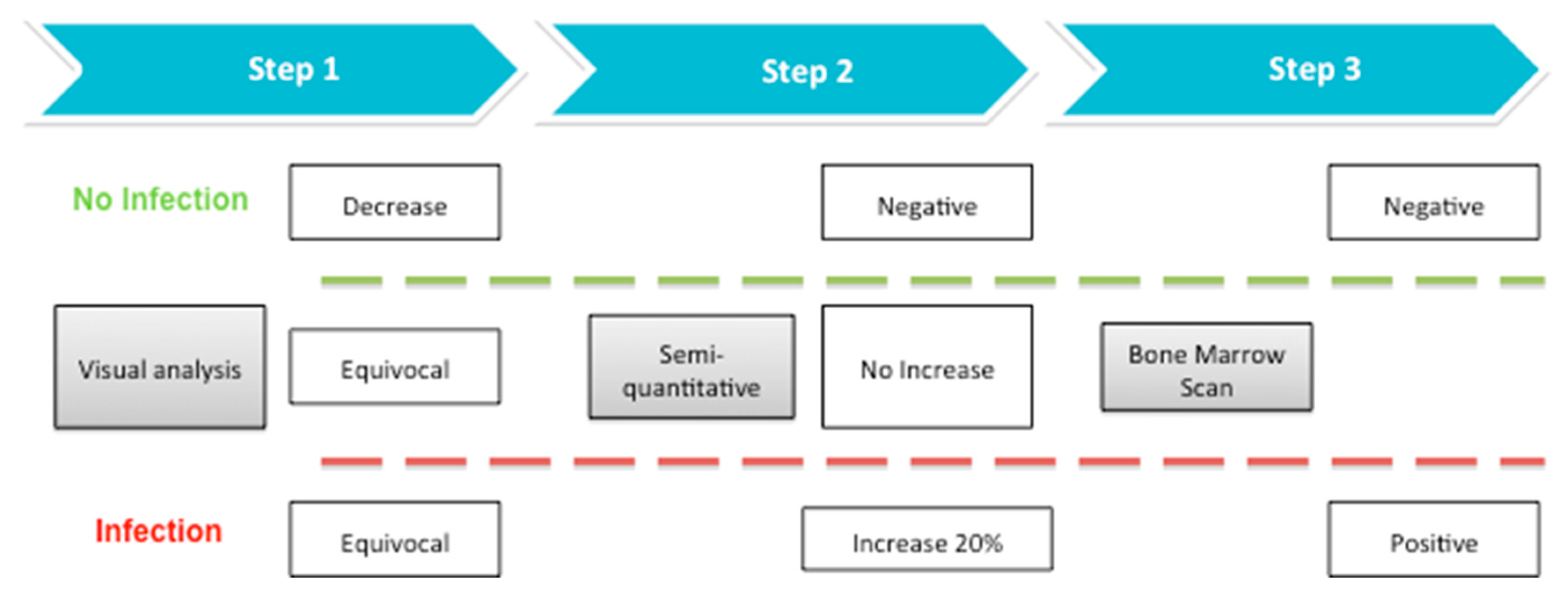
2.1.3. Image Interpretation and Definition of Doubtful Cases
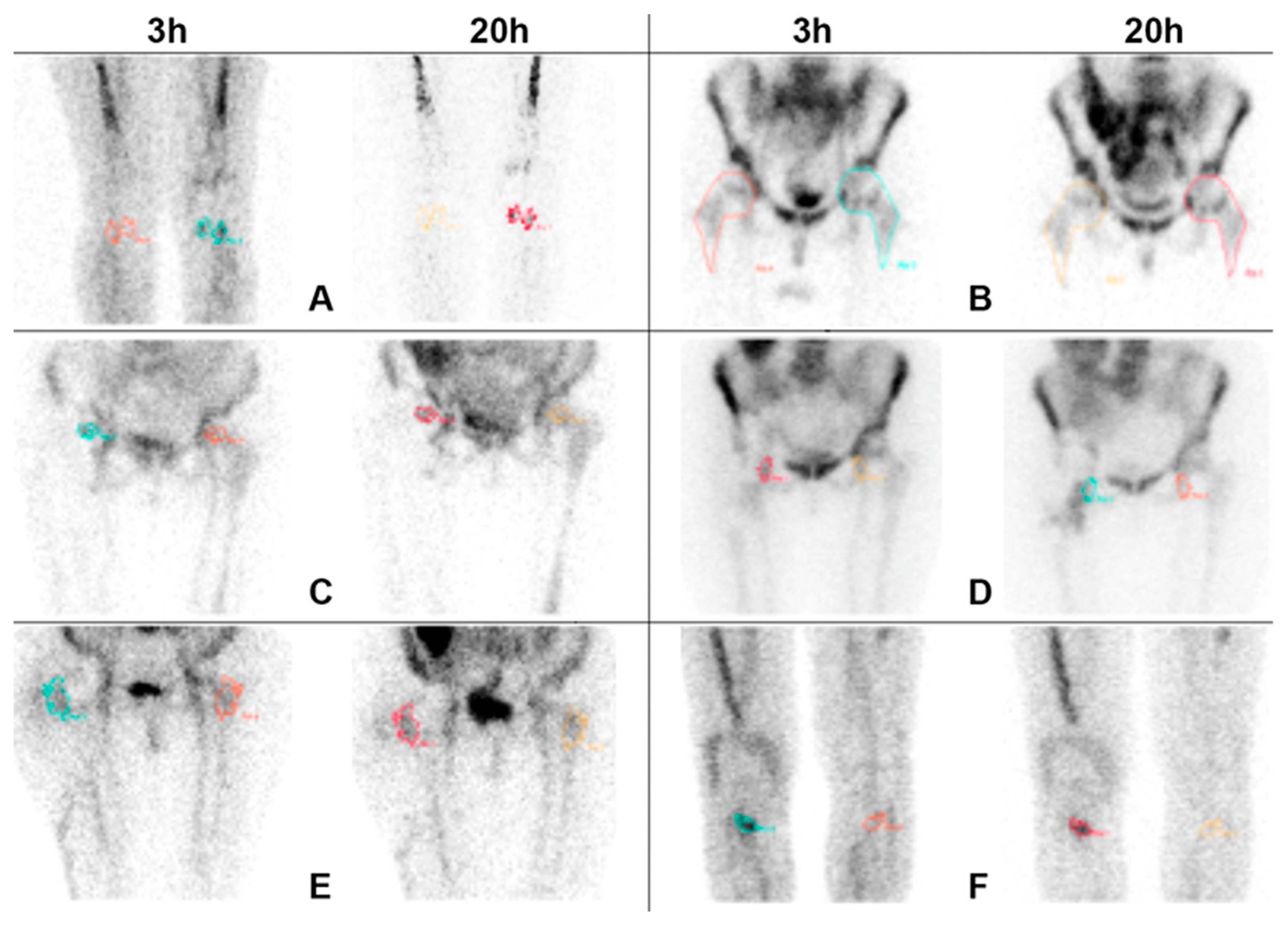
- Small increase of extent of uptake in the suspected region, at late images, without significant increase of activity;
- Soft tissue infection that does not allow to clearly evaluate the bone;
- Small increase of activity over time, in the suspected region, but similar increase also in BM;
- Unmodified activity over time, in the suspected region, but with clear decrease of BM and background activity.
2.1.4. Semi-Quantitative Analysis of Doubtful Cases
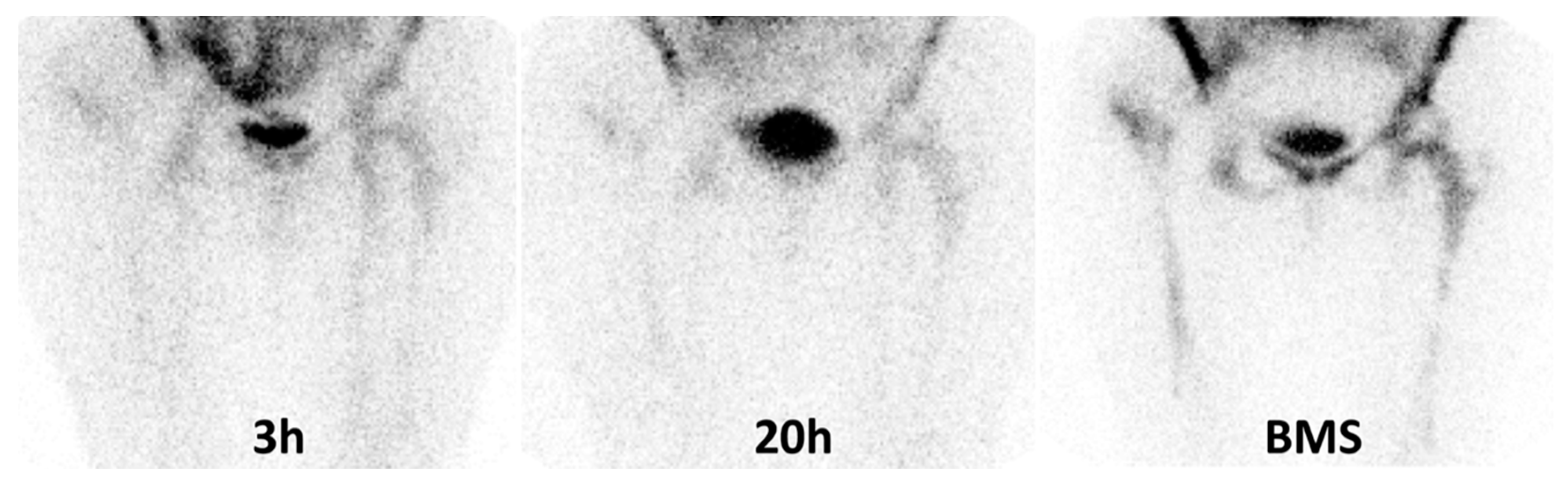
2.1.5. Bone Marrow Scintigraphy (BMS)
2.1.6. Gold Standard
2.1.7. Statistical Analysis
3. Results
3.1. Patients
3.2. WBC Scintigraphy
3.3. Semi-Quantitative Analysis
3.4. Bone Marrow Scintigraphy (BMS)
3.5. Comparison between Semi-Quantitative Analysis and BMS according to Final Diagnosis
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Brunenberg, D.E.; van Steyn, M.J.; Sluimer, J.C.; Bekebrede, L.L.; Bulstra, S.K.; Joore, M.A. Joint recovery programme versus usual care: An economic evaluation of a clinical pathway for joint replacement surgery. Med. Care 2005, 43, 1018–1026. [Google Scholar] [CrossRef] [PubMed]
- Kurtz, S.M.; Lau, E.; Watson, H.; Schmier, J.K.; Parvizi, J. Economic burden of periprosthetic joint infection in the United States. J. Arthroplast. 2012, 27, 61–65. [Google Scholar] [CrossRef] [PubMed]
- Trampuz, A.; Zimmerli, W. Prosthetic joint infections: Update in diagnosis and treatment. Swiss Med. Wkly. 2005, 135, 243–251. [Google Scholar] [PubMed]
- Signore, A.; Sconfienza, L.M.; Borens, O.; Glaudemans, A.W.J.M.; Cassar-Pullicino, V.; Trampuz, A.; Winkler, H.; Gheysens, O.; Vanhoenacker, F.M.H.M.; Petrosillo, N.; et al. Consensus document for the diagnosis of prosthetic joint infections: A joint paper by the EANM, EBJIS, and ESR (with ESCMID endorsement). Eur. J. Nucl. Med. Mol. Imaging 2019, 46, 971–988. [Google Scholar] [CrossRef]
- Trampuz, A.; Hanssen, A.D.; Osmon, D.R.; Mandrekar, J.; Steckelberg, J.M.; Patel, R. Synovial fluid leukocyte count and differential for the diagnosis of prosthetic knee infection. Am. J. Med. 2004, 117, 556–562. [Google Scholar] [CrossRef]
- Spangehl, M.J.; Masri, B.A.; O’Connell, J.X.; Duncan, C.P. Prospective analysis of preoperative and intraoperative investigations for the diagnosis of infection at the sites of two hundred and two revision total hip arthroplasties. J. Bone Jt. Surg. Am. 1999, 81, 672–683. [Google Scholar] [CrossRef]
- Fink, B.; Makowiak, C.; Fuerst, M.; Berger, I.; Schäfer, P.; Frommelt, L. The value of synovial biopsy, joint aspiration and C-reactive protein in the diagnosis of late peri-prosthetic infection of total knee replacements. J. Bone Jt. Surg. Br. 2008, 90, 874–878. [Google Scholar] [CrossRef]
- Fink, B.; Gebhard, A.; Fuerst, M.; Berger, I.; Schäfer, P. High diagnostic value of synovial biopsy in periprosthetic joint infection of the hip. Clin. Orthop. Relat. Res. 2013, 471, 956–964. [Google Scholar] [CrossRef]
- Glaudemans, A.W.; Prandini, N.; Di Girolamo, M.; Argento, G.; Lauri, C.; Lazzeri, E.; Muto, M.; Sconfienza, L.M.; Signore, A. Hybrid imaging of musculoskeletal infections. Q. J. Nucl. Med. Mol. Imaging 2018, 62, 3–13. [Google Scholar] [CrossRef]
- Signore, A.; Lauri, C.; Galli, F. Radiolabelled Probes Targeting Infection and Inflammation for Personalized Medicine. Curr. Pharm. Des. 2014, 20, 2338–2345. [Google Scholar] [CrossRef]
- Sollini, M.; Lauri, C.; Boni, R.; Lazzeri, E.; Erba, P.A.; Signore, A. Current status of molecular imaging in infections. Curr. Pharm. Des. 2018, 24, 754–771. [Google Scholar] [CrossRef] [PubMed]
- Glaudemans, A.W.; Galli, F.; Pacilio, M.; Signore, A. Leukocyte and bacteria imaging in prosthetic joint infection. Eur. Cell Mater. 2013, 25, 61–77. [Google Scholar] [CrossRef] [PubMed]
- Roca, M.; De Vries, E.F.J.; Jamar, F.; Israel, O.; Signore, A. Guidelines for the labelling of leucocytes with 111In-oxine. Eur. J. Nucl. Med. Mol. Imaging 2010, 37, 835–841. [Google Scholar] [CrossRef] [PubMed]
- De Vries, E.F.; Roca, M.; Jamar, F.; Israel, O.; Signore, A. Guidelines fort the labelling of leucocytes with (99m)Tc-HMPAO. Inflammation/Infection Taskgroup of the European Association of Nuclear Medicine. Eur. J. Nucl. Med. Mol. Imaging 2010, 37, 842–848. [Google Scholar] [CrossRef]
- Signore, A.; Jamar, F.; Israel, O.; Buscombe, J.; Martin-Comin, J.; Lazzeri, E. Clinical indications, image acquisition and data interpretation for white blood cells and anti-granulocyte monoclonal antibody scintigraphy: An EANM procedural guideline. Eur. J. Nucl. Med. Mol. Imaging 2018, 45, 1816–1831. [Google Scholar] [CrossRef]
- Erba, P.A.; Glaudemans, A.W.; Veltman, N.C.; Sollini, M.; Pacilio, M.; Galli, F.; Dierckx, R.A.; Signore, A. Image acquisition and interpretation criteria for 99mTc-HMPAO-labelled white blood cell scintigraphy: Results of a multicentre study. Eur. J. Nucl. Med. Mol. Imaging 2014, 41, 615–623. [Google Scholar] [CrossRef]
- Glaudemans, A.W.; de Vries, E.F.; Vermeulen, L.E.; Slart, R.H.; Dierckx, R.A.; Signore, A. A large retrospective single-centre study to define the best image acquisition protocols and interpretation criteria for white blood cell scintigraphy with 99mTc-HMPAO-labelled leucocytes in musculoskeletal infections. Eur. J. Nucl. Med. Mol. Imaging 2013, 40, 1760–1769. [Google Scholar] [CrossRef]
- Pelosi, E.; Baiocco, C.; Pennone, M.; Migliaretti, G.; Varetto, T.; Maiello, A.; Bellò, M.; Bisi, G. 99mTc-HMPAO-leukocyte scintigraphy in patients with symptomatic total hip or knee arthroplasty: Improved diagnostic accuracy by means of semiquantitative evaluation. J. Nucl. Med. 2004, 45, 438–444. [Google Scholar]
- Palestro, C.J.; Love, C.; Tronco, G.G.; Tomas, M.B.; Rini, J.N. Combined labeled leukocyte and technetium 99m sulfur colloid bone marrow imaging for diagnosing musculoskeletal infection. Radiographics 2006, 26, 859–870. [Google Scholar] [CrossRef]
- Gemmel, F.; van den Wyngaert, H.; Love, C.; Welling, M.M.; Gemmel, P.; Palestro, C.J. Prosthetic joint infections: Radionuclide state-of-the-art imaging. Eur. J. Nucl. Med. Mol. Imaging 2012, 39, 892–909. [Google Scholar] [CrossRef]
- Palestro, C.J.; Kim, C.K.; Swyer, A.J.; Capozzi, J.D.; Solomon, R.W.; Goldsmith, S.J. Total-hip arthroplasty: Periprosthetic indium-111- labeled leukocyte activity and complementary technetium-99msulfur colloid imaging in suspected infection. J. Nucl. Med. 1990, 31, 1950–1955. [Google Scholar] [PubMed]
- Osmon, D.R.; Berbari, E.F.; Berendt, A.R.; Lew, D.; Zimmerli, W.; Steckelberg, J.M.; Rao, N.; Hanssen, A.; Wilson, W.R.; Infectious Diseases Society of America. Diagnosis and management of prosthetic joint infection: Clinical practice guidelines by the Infectious Diseases Society of America. Clin. Infect. Dis. 2013, 56, e1–e25. [Google Scholar] [CrossRef] [PubMed]
- Romanò, C.L.; Petrosillo, N.; Argento, G.; Sconfienza, L.M.; Treglia, G.; Alavi, A.; Glaudemans, A.W.J.M.; Gheysens, O.; Maes, A.; Lauri, C.; et al. The Role of Imaging Techniques to Define a Peri-Prosthetic Hip and Knee Joint Infection: Multidisciplinary Consensus Statements. J. Clin. Med. 2020, 9, 2548. [Google Scholar] [CrossRef] [PubMed]
- Lauri, C.; Glaudemans, A.W.J.M.; Campagna, G.; Keidar, Z.; Muchnik Kurash, M.; Georga, S.; Arsos, G.; Noriega-Álvarez, E.; Argento, G.; Kwee, T.C.; et al. Comparison of White Blood Cell Scintigraphy, FDG PET/CT and MRI in Suspected Diabetic Foot Infection: Results of a Large Retrospective Multicenter Study. J. Clin. Med. 2020, 9, 1645. [Google Scholar] [CrossRef]
- Love, C.; Marwin, S.E.; Tomas, M.B.; Krauss, E.S.; Tronco, G.G.; Bhargava, K.K.; Nichols, K.J.; Palestro, C.J. Diagnosing infection in the failed joint replacement: A comparison of coincidence detection 18F-FDG and 111In-labeled leukocyte/99mTc-sulfur colloid marrow imaging. J. Nucl. Med. 2004, 45, 1864–1871. [Google Scholar]
- Simonsen, L.; Buhl, A.; Oersnes, T.; Duus, B. White blood cell scintigraphy for differentiation of infection and aseptic loosening: A retrospective study of 76 painful hip prostheses. Acta Orthop. 2007, 78, 640–647. [Google Scholar] [CrossRef]
- Mulamba, L.; Ferrant, A.; Leners, N.; de Nayer, P.; Rombouts, J.J.; Vincent, A. Indium-111 leucocyte scanning in the evaluation of painful hip arthroplasty. Acta Orthop. Scand. 1983, 54, 695–697. [Google Scholar] [CrossRef]
- Palestro, C.J.; Swyer, A.J.; Kim, C.K.; Goldsmith, S.J. Infected knee prosthesis: Diagnosis with in-111 leukocyte, Tc-99m sulfur colloid, and Tc-99m MDP imaging. Radiology 1991, 179, 645–648. [Google Scholar] [CrossRef]
- El Espera, I.; Blondet, C.; Moullart, V.; Saïdi, L.; Havet, E.; Mertl, P.; Canarelli, B.; Schmit, J.L.; Meyer, M.E. The usefulness of 99mTc sulfur colloid bone marrow scintigraphy combined with 111In leucocyte scintigraphy in prosthetic joint infection. Nucl. Med. Commun. 2004, 25, 171–175. [Google Scholar] [CrossRef]
- Joseph, T.N.; Mujtaba, M.; Chen, A.L.; Maurer, S.L.; Zuckerman, J.D.; Maldjian, C.; Di Cesare, P.E. Efficacy of combined technetium-99m sulfur colloid/indium-111 leukocyte scans to detect infected total hip and knee arthroplasties. J. Arthroplast. 2001, 16, 753–758. [Google Scholar] [CrossRef]
- Thang, S.P.; Tong, A.K.; Lam, W.W.; Ng, D.C. SPECT/CT in musculoskeletal infections. Semin. Musculoskelet. Radiol. 2014, 18, 194–202. [Google Scholar] [CrossRef] [PubMed]
- Tam, H.H.; Bhaludin, B.; Rahman, F.; Weller, A.; Ejindu, V.; Parthipun, A. SPECT-CT in total hip arthroplasty. Clin. Radiol. 2014, 69, 82–95. [Google Scholar] [CrossRef] [PubMed]
- Mariani, G.; Bruselli, L.; Kuwert, T.; Kim, E.E.; Flotats, A.; Israel, O.; Dondi, M.; Watanabe, N. A review on the clinical uses of SPECT/CT. Eur. J. Nucl. Med. Mol. Imaging 2010, 37, 1959–1985. [Google Scholar] [CrossRef] [PubMed]
- Scharf, S. SPECT/CT imaging in general orthopedic practice. Semin. Nucl. Med. 2009, 39, 293–307. [Google Scholar] [CrossRef] [PubMed]
| All Patients (66) | Infected (18) | Non Infected (48) | |
|---|---|---|---|
| Age (years) | 72.24 ± 10.42 | 71.56 ± 10.33 | 72.4 ± 10.4 |
| Gender (F-M) * | 69.7%–30.3% | 61.1%–38.9% | 72.9%–27.1% |
| Time after surgery (years) | 4.28 ± 4.19 | 2.67 ± 1.37 | 4.8 ± 4.6 |
| Type of prosthesis (Hip-Knee) * | 51.5%–48.5% | 50.0%–50.0% | 50.0%–50.0% |
| T/B3h | 1.67 ± 0.67 | 1.60 ± 0.56 | 1.69 ± 0.71 |
| T/B20h | 1.85 ± 0.74 | 2.00 ± 0.68 | 1.79 ± 0.75 |
| Criteria for Doubtful Interpretation | n. of Patients | Patients with BMS |
|---|---|---|
| A. Small, not significant increase of activity in the suspected region at late images | 36 | 30 |
| B. Increase of bone marrow activity over time, that does not allow easy visualization of peri-prosthetic or bone activity | 11 | 9 |
| C. Small increase of extent of uptake in the suspected region at late images, without significant increase of activity | 4 | 4 |
| D. Soft tissue infection that does not allow to clearly evaluate the bone | 6 | 5 |
| E. Small increase of activity over time, in the suspected region, but similar increase also in bone marrow | 2 | 2 |
| F. Unmodified activity over time in the suspected region with clear decrease of bone marrow and background activity | 7 | 6 |
| tot: 66 | tot: 56 |
| n. TP | n. FP | n. TN | n. FN | |
|---|---|---|---|---|
| T/B20h > T/B3h 5% | 14 | 27 | 21 | 4 |
| T/B20h > T/B3h 10% | 13 | 16 | 32 | 5 |
| T/B20h > T/B3h 15% | 12 | 12 | 36 | 6 |
| T/B20h > T/B3h 20% | 12 | 7 | 41 | 6 |
| T/B20h > T/B3h 30% | 6 | 3 | 45 | 12 |
| BMS | 11 | 3 | 40 | 2 |
| Sensitivity (%) (95% CI) | Specificity (%) (95% CI) | Accuracy (%) (95% CI) | |
|---|---|---|---|
| T/B20h > T/B3h 5% | 77.8 (58.6–97.0) | 43.8 (29.7–57.8) | 53.0 (41.0–65.1) |
| T/B20h > T/B3h 10% | 72.2 (51.5–92.9) | 66.7 (53.3–80.0) | 68.2 (56.2–79.4) |
| T/B20h > T/B3h 15% | 66.7 (44.9–88.4) | 75.0 (62.8–87.3) | 72.7 (62.0–83.5) |
| T/B20h > T/B3h 20% | 66.7 (44.9–88.4) | 85.4 (75.4–95.4) | 80.3 (70.7–89.9) |
| T/B20h > T/B3h 30% | 33.3 (11.6–55.1) | 93.8 (86.9–100) | 77.3 (67.2–87.4) |
| BMS | 84.6 (65.0–100) | 93.0 (85.4–100) | 91.1 (83.6–98.5) |
| Sensitivity (p) | Specificity (p) | Accuracy (p) | |
|---|---|---|---|
| T/B20h > T/B3h 5% vs. BMS | 0.63 | <0.0001 | <0.0001 |
| T/B20h > T/B3h 10% vs. BMS | 0.51 | 0.005 | 0.005 |
| T/B20h > T/B3h 15% vs. BMS | 0.43 | 0.035 | 0.016 |
| T/B20h > T/B3h 20% vs. BMS | 0.43 | 0.31 | 0.09 |
| T/B20h > T/B3h 30% vs. BMS | 0.023 | 0.89 | 0.06 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lauri, C.; Lauretti, G.; Galli, F.; Campagna, G.; Tetti, S.; Riolo, D.; Signore, A. Handling of Doubtful WBC Scintigraphies in Patients with Suspected Prosthetic Joint Infections. J. Clin. Med. 2020, 9, 4031. https://doi.org/10.3390/jcm9124031
Lauri C, Lauretti G, Galli F, Campagna G, Tetti S, Riolo D, Signore A. Handling of Doubtful WBC Scintigraphies in Patients with Suspected Prosthetic Joint Infections. Journal of Clinical Medicine. 2020; 9(12):4031. https://doi.org/10.3390/jcm9124031
Chicago/Turabian StyleLauri, Chiara, Giancarlo Lauretti, Filippo Galli, Giuseppe Campagna, Simone Tetti, Donatella Riolo, and Alberto Signore. 2020. "Handling of Doubtful WBC Scintigraphies in Patients with Suspected Prosthetic Joint Infections" Journal of Clinical Medicine 9, no. 12: 4031. https://doi.org/10.3390/jcm9124031
APA StyleLauri, C., Lauretti, G., Galli, F., Campagna, G., Tetti, S., Riolo, D., & Signore, A. (2020). Handling of Doubtful WBC Scintigraphies in Patients with Suspected Prosthetic Joint Infections. Journal of Clinical Medicine, 9(12), 4031. https://doi.org/10.3390/jcm9124031






