Familial Hypercholesterolemia in Premature Acute Coronary Syndrome. Insights from CholeSTEMI Registry
Abstract
1. Introduction
2. Materials and Methods
2.1. General Definitions
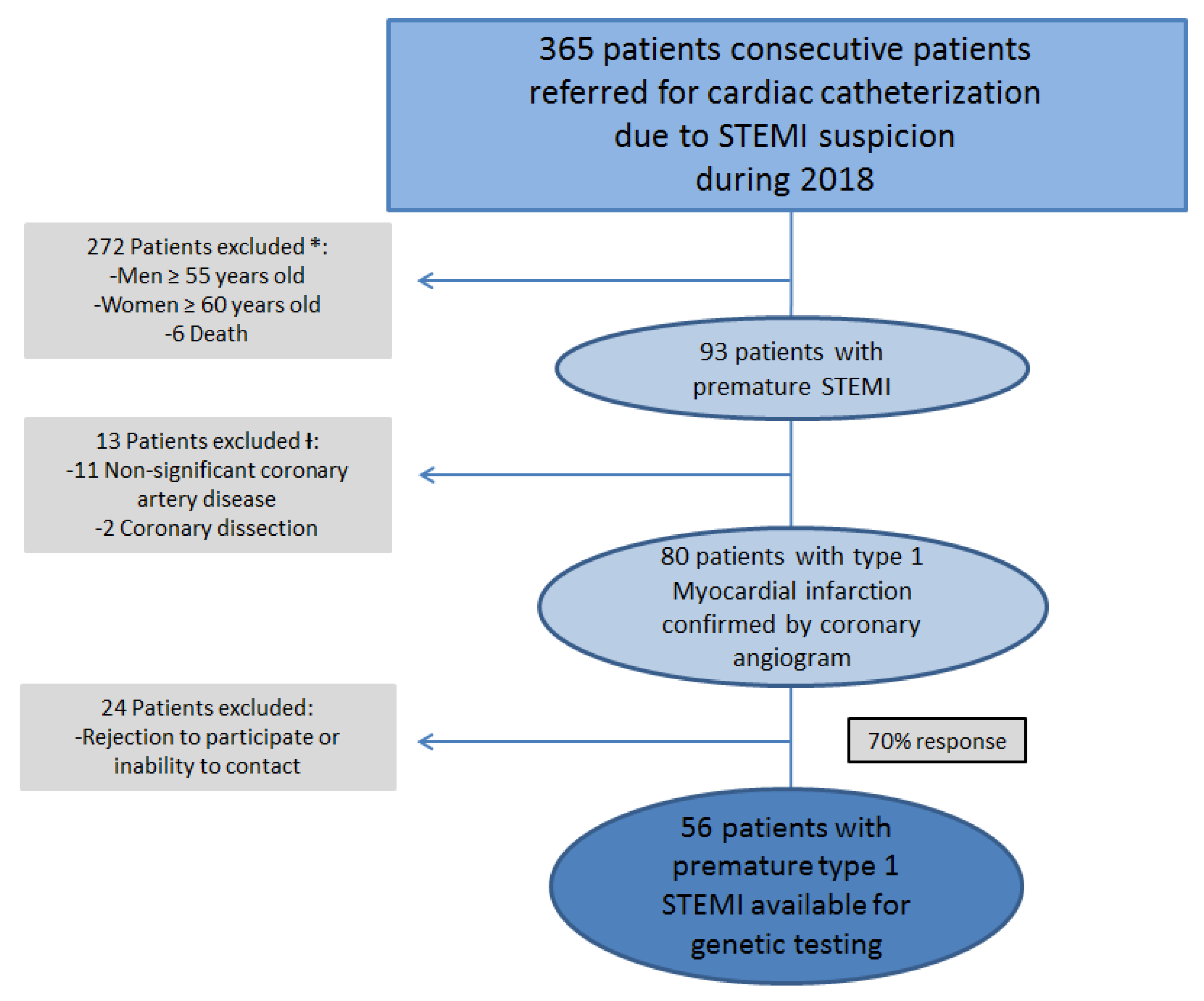
2.2. Study Population
2.3. Clinical Evaluation
2.4. Genetic Testing
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Ibáñez, B.; James, S.; Agewall, S.; Antunes, M.J.; Bucciarelli-Ducci, C.; Bueno, H.; Caforio, A.L.P.; Crea, F.; Goudevenos, J.A.; Halvorsen, S.; et al. Guía ESC 2017 sobre el tratamiento del infarto agudo de miocardio en pacientes con elevación del segmento ST. Rev. Esp. Cardiol. 2017, 70, 1082.e1–1082.e61. [Google Scholar] [CrossRef]
- Fernández de Larrea-Baz, N.; Morant-Ginestar, C.; Catalá-López, F.; Gènova-Maleras, R.; Álvarez-Martín, E. Años de vida ajustados por discapacidad perdidos por cardiopatía isquémica en España. Rev. Esp. Cardiol. 2015, 68, 968–975. [Google Scholar] [CrossRef]
- Schnohr, P. Coronary heart disease risk factors ranked by importance for the individual and community. A 21 year follow-up of 12,000 men and women from The Copenhagen City Heart Study. Eur. Heart J. 2002, 23, 620–626. [Google Scholar] [CrossRef]
- Ruiz García, A.; Mata, P.; Alonso, R.; González-Juanatey, J.; Badimon, L.; Díaz, D.; Muñoz, M.T.; Muñiz, O.; Dalmau, J.; Fuentes, F.; et al. Diagnóstico y Tratamiento de la Hipercolesterolemia Familiar en España: Documento de Consenso; Fundación Hipercolesterolemia Familiar: Madrid, Spain, 2014. [Google Scholar]
- Kramer, A.I.; Trinder, M.; Brunham, L.R. Estimating the Prevalence of Familial Hypercholesterolemia in Acute Coronary Syndrome: A Systematic Review and Meta-analysis. Can. J. Cardiol. 2019, 35, 1322–1331. [Google Scholar] [CrossRef]
- Vogt, A. The genetics of familial hypercholesterolemia and emerging therapies. Appl. Clin. Genet. 2015, 28, 27–36. [Google Scholar] [CrossRef]
- Civeira, F. Guidelines for the diagnosis and management of heterozygous familial hypercholesterolemia. Atherosclerosis 2004, 173, 55–68. [Google Scholar] [CrossRef]
- WHO Human Genetics Programme. Familial Hypercholesterolaemia (FH): Report of a Second WHO Consultation, Geneva, 4 September 1998; World Health Organization: Geneva, Switzerland, 1998. [Google Scholar]
- Sturm, A.C.; Knowles, J.W.; Gidding, S.S.; Ahmad, Z.S.; Ahmed, C.D.; Ballantyne, C.M.; Baum, S.J.; Bourbon, M.; Carrié, A.; Cuchel, M.; et al. Clinical Genetic Testing for Familial Hypercholesterolemia. J. Am. Coll. Cardiol. 2018, 72, 662–680. [Google Scholar] [CrossRef]
- Mach, F.; Baigent, C.; Catapano, A.L.; Koskinas, K.C.; Casula, M.; Badimon, L.; Chapman, M.J.; De Backer, G.G.; Delgado, V.; Ference, B.A.; et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: Lipid modification to reduce cardiovascular risk. Eur. Heart J. 2020, 41, 111–188. [Google Scholar] [CrossRef]
- Ascaso, J.F.; Civeira, F.; Guijarro, C.; López Miranda, J.; Masana, L.; Mostaza, J.M.; Pedro-Botet, J.; Pintó, X.; Valdivielso, P. Indicaciones de los inhibidores de PCSK9 en la práctica clínica. Recomendaciones de la Sociedad Española de Arteriosclerosis (SEA), 2019. Clínica Investig. Arterioscler. 2019, 31, 128–139. [Google Scholar] [CrossRef]
- Akioyamen, L.E.; Genest, J.; Shan, S.D.; Reel, R.L.; Albaum, J.M.; Chu, A.; Tu, J.V. Estimating the prevalence of heterozygous familial hypercholesterolaemia: A systematic review and meta-analysis. BMJ Open 2017, 7, e016461. [Google Scholar] [CrossRef]
- Nordestgaard, B.G.; Chapman, M.J.; Humphries, S.E.; Ginsberg, H.N.; Masana, L.; Descamps, O.S.; Wiklund, O.; Hegele, R.A.; Raal, F.J.; Defesche, J.C.; et al. Familial hypercholesterolaemia is underdiagnosed and undertreated in the general population: Guidance for clinicians to prevent coronary heart disease: Consensus Statement of the European Atherosclerosis Society. Eur. Heart J. 2013, 34, 3478–3490. [Google Scholar] [CrossRef]
- Benn, M.; Watts, G.F.; Tybjærg-Hansen, A.; Nordestgaard, B.G. Mutations causative of familial hypercholesterolaemia: Screening of 98 098 individuals from the Copenhagen General Population Study estimated a prevalence of 1 in 217. Eur. Heart J. 2016, 37, 1384–1394. [Google Scholar] [CrossRef]
- Do, R.; Stitziel, N.O.; Won, H.-H.; Jørgensen, A.B.; Duga, S.; Angelica Merlini, P.; Kiezun, A.; Farrall, M.; Goel, A.; Zuk, O.; et al. Exome sequencing identifies rare LDLR and APOA5 alleles conferring risk for myocardial infarction. Nature 2015, 518, 102–106. [Google Scholar] [CrossRef]
- Beheshti, S.O.; Madsen, C.M.; Varbo, A.; Nordestgaard, B.G. Worldwide Prevalence of Familial Hypercholesterolemia. J. Am. Coll. Cardiol. 2020, 75, 2553–2566. [Google Scholar] [CrossRef]
- Thygesen, K.; Alpert, J.S.; Jaffe, A.S.; Chaitman, B.R.; Bax, J.J.; Morrow, D.A.; White, H.D.; ESC Scientific Document Group; Thygesen, K.; Alpert, J.S.; et al. Fourth universal definition of myocardial infarction (2018). Eur. Heart J. 2019, 40, 237–269. [Google Scholar] [CrossRef]
- Collet, J.-P.; Thiele, H.; Barbato, E.; Barthélémy, O.; Bauersachs, J.; Bhatt, D.L.; Dendale, P.; Dorobantu, M.; Edvardsen, T.; Folliguet, T.; et al. 2020 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur. Heart J. 2020, ehaa575. [Google Scholar] [CrossRef]
- Cannon, R.O. Chest Pain with Normal Coronary Angiograms. N. Engl. J. Med. 1993, 328, 1706–1708. [Google Scholar] [CrossRef]
- Besseling, J.; Kindt, I.; Hof, M.; Kastelein, J.J.P.; Hutten, B.A.; Hovingh, G.K. Severe heterozygous familial hypercholesterolemia and risk for cardiovascular disease: A study of a cohort of 14,000 mutation carriers. Atherosclerosis 2014, 233, 219–223. [Google Scholar] [CrossRef]
- Gómez, J.; Reguero, J.R.; Morís, C.; Martín, M.; Alvarez, V.; Alonso, B.; Iglesias, S.; Coto, E. Mutation Analysis of the Main Hypertrophic Cardiomyopathy Genes Using Multiplex Amplification and Semiconductor Next-Generation Sequencing. Circ. J. 2014, 78, 2963–2971. [Google Scholar] [CrossRef]
- Gómez, J.; Lorca, R.; Reguero, J.R.; Morís, C.; Martín, M.; Tranche, S.; Alonso, B.; Iglesias, S.; Alvarez, V.; Díaz-Molina, B.; et al. Screening of the Filamin C Gene in a Large Cohort of Hypertrophic Cardiomyopathy Patients. Circ. Cardiovasc. Genet. 2017, 10, e001584. [Google Scholar] [CrossRef]
- On behalf of the ACMG Laboratory Quality Assurance Committee; Richards, S.; Aziz, N.; Bale, S.; Bick, D.; Das, S.; Gastier-Foster, J.; Grody, W.W.; Hegde, M.; Lyon, E.; et al. Standards and guidelines for the interpretation of sequence variants: A joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet. Med. 2015, 17, 405–423. [Google Scholar]
- Hopkins, P.N. Genotype-guided diagnosis in familial hypercholesterolemia: Population burden and cascade screening. Curr. Opin. Lipidol. 2017, 28, 136–143. [Google Scholar] [CrossRef]
- Khera, A.V.; Won, H.-H.; Peloso, G.M.; Lawson, K.S.; Bartz, T.M.; Deng, X.; van Leeuwen, E.M.; Natarajan, P.; Emdin, C.A.; Bick, A.G.; et al. Diagnostic Yield and Clinical Utility of Sequencing Familial Hypercholesterolemia Genes in Patients With Severe Hypercholesterolemia. J. Am. Coll. Cardiol. 2016, 67, 2578–2589. [Google Scholar] [CrossRef]
- Robinson, J.G.; Goldberg, A.C. Treatment of adults with Familial Hypercholesterolemia and evidence for treatment: Recommendations from the National Lipid Association Expert Panel on Familial Hypercholesterolemia. J. Clin. Lipidol. 2011, 5, S18–S29. [Google Scholar] [CrossRef]
- Pirazzi, C.; Håkansson, L.; Gustafsson, C.; Omerovic, E.; Wiklund, O.; Mancina, R.M. High prevalence of genetic determined familial hypercholesterolemia in premature coronary artery disease. Appl. Clin. Genet. 2019, 12, 71–78. [Google Scholar] [CrossRef]
- Nanchen, D.; Gencer, B.; Auer, R.; Räber, L.; Stefanini, G.G.; Klingenberg, R.; Schmied, C.M.; Cornuz, J.; Muller, O.; Vogt, P.; et al. Prevalence and management of familial hypercholesterolaemia in patients with acute coronary syndromes. Eur. Heart J. 2015, 36, 2438–2445. [Google Scholar] [CrossRef]
- Amor-Salamanca, A.; Castillo, S.; Gonzalez-Vioque, E.; Dominguez, F.; Quintana, L.; Lluís-Ganella, C.; Escudier, J.M.; Ortega, J.; Lara-Pezzi, E.; Alonso-Pulpon, L.; et al. Genetically Confirmed Familial Hypercholesterolemia in Patients With Acute Coronary Syndrome. J. Am. Coll. Cardiol. 2017, 70, 1732–1740. [Google Scholar] [CrossRef]
- Cui, Y.; Li, S.; Zhang, F.; Song, J.; Lee, C.; Wu, M.; Chen, H. Prevalence of familial hypercholesterolemia in patients with premature myocardial infarction. Clin. Cardiol. 2019, 42, 385–390. [Google Scholar]
- De Backer, G.; Besseling, J.; Chapman, J.; Hovingh, G.K.; Kastelein, J.J.P.; Kotseva, K.; Ray, K.; Reiner, Ž.; Wood, D.; De Bacquer, D.; et al. Prevalence and management of familial hypercholesterolaemia in coronary patients: An analysis of EUROASPIRE IV, a study of the European Society of Cardiology. Atherosclerosis 2015, 241, 169–175. [Google Scholar] [CrossRef]
- Koivisto, U.M.; Hämäläinen, L.; Taskinen, M.R.; Kettunen, K.; Kontula, K. Prevalence of familial hypercholesterolemia among young north Karelian patients with coronary heart disease: A study based on diagnosis by polymerase chain reaction. J. Lipid Res. 1993, 34, 269–277. [Google Scholar]
- Li, S.; Zhang, Y.; Zhu, C.-G.; Guo, Y.-L.; Wu, N.-Q.; Gao, Y.; Qing, P.; Li, X.-L.; Sun, J.; Liu, G.; et al. Identification of familial hypercholesterolemia in patients with myocardial infarction: A Chinese cohort study. J. Clin. Lipidol. 2016, 10, 1344–1352. [Google Scholar] [CrossRef]
- Pang, J.; Poulter, E.B.; Bell, D.A.; Bates, T.R.; Jefferson, V.-L.; Hillis, G.S.; Schultz, C.J.; Watts, G.F. Frequency of familial hypercholesterolemia in patients with early-onset coronary artery disease admitted to a coronary care unit. J. Clin. Lipidol. 2015, 9, 703–708. [Google Scholar] [CrossRef] [PubMed]
- Wald, D.S.; Bangash, F.A.; Bestwick, J.P. Prevalence of DNA-confirmed familial hypercholesterolaemia in young patients with myocardial infarction. Eur. J. Intern. Med. 2015, 26, 127–130. [Google Scholar] [CrossRef]
- Yudi, M.; Omera, L.; McCubbery, N.; Dick, S.; Jayasinghe, R.; Hamilton-Craig, I. Suboptimal consideration and management of potential familial hypercholesterolaemia in patients with suspected premature coronary artery disease. Singap. Med. J. 2012, 53, 174–178. [Google Scholar]
- Gidding, S.S.; Champagne, M.A.; de Ferranti, S.D.; Defesche, J.; Ito, M.K.; Knowles, J.W.; McCrindle, B.; Raal, F.; Rader, D.; Santos, R.D.; et al. The Agenda for Familial Hypercholesterolemia: A Scientific Statement from the American Heart Association. Circulation 2015, 132, 2167–2192. [Google Scholar] [CrossRef]
- Thygesen, K.; Alpert, J.S.; Jaffe, A.S.; Simoons, M.L.; Chaitman, B.R.; White, H.D. Third universal definition of myocardial infarction. Eur. Heart J. 2012, 33, 2551–2567. [Google Scholar] [CrossRef]
| Whole Cohort (n = 56) | Women (n = 8) | Men (n = 48) | p | |
|---|---|---|---|---|
| Smoking | 85.7% | 100% | 83.3% | 0.21 |
| Dyslipidemia | 42.9% | 37.5% | 43.8% | 0.74 |
| Hypertension | 28.6% | 25% | 29.2% | 0.81 |
| Diabetes | 10.7% | 12.5% | 10.4% | 0.86 |
| Average BMI | 28.9 ± 3.8 SD | 28.5± 4.7 SD | 29 ± 3.6 SD | 0.7 |
| Cohort at STEMI (n = 56) | Women at STEMI (n = 8) | Men at STEMI (n = 48) | Cohort at Control | p | Women at Control (n = 8) | Men at Control (n = 48) | p | |
|---|---|---|---|---|---|---|---|---|
| Total cholesterol (mg/dL) | 179.8 ± 39.3 SD | 168.4 ± 29.4 SD | 181.7 ± 40.6 SD | 138.6 ± 50.4 SD | p > 0.05 | 137.4 ± 37.1 SD | 138.8 ± 52.6 SD | p > 0.05 |
| LDLc (mg/dL) | 110.4 ± 39.3 SD | 94.75 ± 29.2 SD | 112.9 ± 36.9 SD | 65.3 ± 31.5 SD | p > 0.05 | 68.6 ± 31.2 SD | 64.7 ± 31.9 SD | p > 0.05 |
| HDLc (mg/dL) | 39.2 ± 12.2 SD | 48.6 ± 18.6 SD | 37.6 ± 10.3 SD | 43.5 ± 16.8 SD | p > 0.05 | 44 ± 15.3 SD | 43.1 ± 17.2 SD | p > 0.05 |
| Triglycerides (mg/dL) | 176.9 ± 117.8 SD | 144.5 ± 104.2 SD | 182.3 ± 120.1 SD | 190.6 ± 393.5 SD | p > 0.05 | 140.9 ± 89.1 SD | 199.2 ± 423.7 SD | p > 0.05 |
| N | Inclusion Criteria | Clinical Presentation of CAD | Clinical Diagnosis (DLCN Probable-Definite) (%) | Genetic Diagnosis (%) | |
|---|---|---|---|---|---|
| Amor-Salamanca et al. [29] | 103 | ≤65 years old and LDLc ≥160 mg/dL | STEMI, NSTEMI and unstable angina | 27.2% | 8.7% |
| Cui et al. [30] | 225 | ≤55 years old in men and ≤60 in women | Myocardial infarction (STEMI and NSTEMI) | 5.3% | 4.4% |
| De Backer et al. [31], Subanalysis of premature CAD | 2212 | <60 years old | ACS, acute myocardial ischemia or procedure: coronary artery bypass grafting or percutaneous coronary intervention) | 15.4% | Not evaluated |
| Koivisto et al. [32] | 90 | ≤45 years old | Symptomatic CAD (myocardial infarction and effort-induced angina pectoris) | Not evaluated | 9% |
| Li et al. [33], Subanalysis of premature CAD | 889 | ≤55 years old in men and ≤60 in women | Myocardial infarction (STEMI and NSTEMI) | 7.1% | Not evaluated |
| Nanchen et al. [28] Subanalysis of premature CAD | 1451 | <55 years old in men and <60 in women | ACS (not specified whether STEMI, NSTEMI or unstable angina) | 4.8% | Not evaluated |
| Pang et al. [34] | 175 | <60 years old | ACS, myocardial revascularization and angina pectoris | 14.3% | Not evaluated |
| Pirazzi et al. [27] | 49 | <50 years old in men and <55 in women | Myocardial infarction (STEMI or NSTEMI), unstable angina, stable angina or atherosclerosis, spasm angina and other diagnosis (non- atherosclerotic) | 16.7% | 6.1% |
| Wald et al. [35] | 231 | ≤50 years old | STEMI and NSTEMI | Not evaluated | 1.3% |
| Yudi et al. [36] | 210 | ≤55 years old in men and ≤60 in women | ACS, angina, unstable angina, STEMI and NSTEMI | 1.4% | Not evaluated |
| Lorca et al. (this study). | 56 | <55 years old in men and <60 females in women | STEMIConfirmed by coronary angiogram | 1.8% | 1.8% |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lorca, R.; Aparicio, A.; Cuesta-Llavona, E.; Pascual, I.; Junco, A.; Hevia, S.; Villazón, F.; Hernandez-Vaquero, D.; Rodríguez Reguero, J.J.; Moris, C.; et al. Familial Hypercholesterolemia in Premature Acute Coronary Syndrome. Insights from CholeSTEMI Registry. J. Clin. Med. 2020, 9, 3489. https://doi.org/10.3390/jcm9113489
Lorca R, Aparicio A, Cuesta-Llavona E, Pascual I, Junco A, Hevia S, Villazón F, Hernandez-Vaquero D, Rodríguez Reguero JJ, Moris C, et al. Familial Hypercholesterolemia in Premature Acute Coronary Syndrome. Insights from CholeSTEMI Registry. Journal of Clinical Medicine. 2020; 9(11):3489. https://doi.org/10.3390/jcm9113489
Chicago/Turabian StyleLorca, Rebeca, Andrea Aparicio, Elias Cuesta-Llavona, Isaac Pascual, Alejandro Junco, Sergio Hevia, Francisco Villazón, Daniel Hernandez-Vaquero, Jose Julian Rodríguez Reguero, Cesar Moris, and et al. 2020. "Familial Hypercholesterolemia in Premature Acute Coronary Syndrome. Insights from CholeSTEMI Registry" Journal of Clinical Medicine 9, no. 11: 3489. https://doi.org/10.3390/jcm9113489
APA StyleLorca, R., Aparicio, A., Cuesta-Llavona, E., Pascual, I., Junco, A., Hevia, S., Villazón, F., Hernandez-Vaquero, D., Rodríguez Reguero, J. J., Moris, C., Coto, E., Gómez, J., & Avanzas, P. (2020). Familial Hypercholesterolemia in Premature Acute Coronary Syndrome. Insights from CholeSTEMI Registry. Journal of Clinical Medicine, 9(11), 3489. https://doi.org/10.3390/jcm9113489






