Nutritional Management of Medical Inpatients
Abstract
:1. Introduction
2. Today’s Clinical Evidence Level
3. Nutritional Therapy
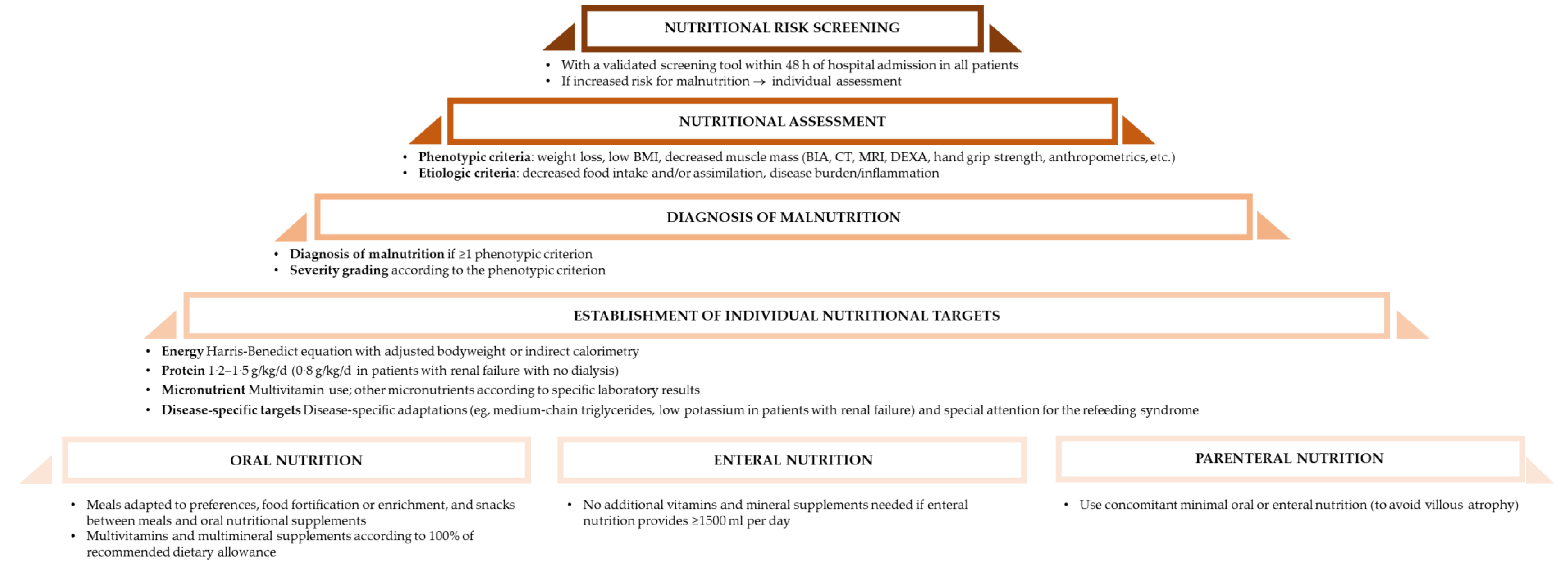
3.1. Organization of Nutritional Support
3.2. Screening and Assessment
3.3. Nutritional Targets
3.3.1. Energy
3.3.2. Proteins
3.3.3. Micronutrients
3.4. Nutritional Route
3.5. Nutrition for Specific Medical Conditions
3.6. Timing
3.7. Monitoring
4. Barriers to the Adequate Provision of Nutritional Support
5. Conclusions and Outlook
Author Contributions
Funding
Conflicts of Interest
References
- Sprengell, C. Hippocrates: The Aphorisms of Hippocrates, and The Sentences of Celsus; with Explanations and References to the Most Considerable Writers, 2nd ed.; Wilkin, F., Bonwick, F., Eds.; Gale Ecco: London, UK, 1735. [Google Scholar]
- Studley, H.O. Percentage of weight loss: A basic indicator of surgical risk in patients with chronic peptic ulcer. J. Am. Med. Assoc. 1936, 106, 458–460. [Google Scholar] [CrossRef]
- McWhirter, J.P.; Pennington, C.P. Incidence and recognition of malnutrition in hospital. Br. Med. J. 1994, 308, 945–948. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hill, G.L.; Pickford, I.; Young, G.A.; Schorah, C.J.; Blackett, R.L.; Burkinshaw, L.; Warren, J.V.; Morgan, D.B. Malnutrition in surgical patients: An unrecognised problem. Lancet 1977, 309, 689–692. [Google Scholar] [CrossRef]
- Bistrian, B.R.; Blackburn, G.L.; Vitale, J.; Cochran, D.; Naylor, J. Prevalence of malnutrition in general medical patients. JAMA 1976, 235, 1567–1570. [Google Scholar] [CrossRef] [PubMed]
- Kubrak, C.; Jensen, L. Malnutrition in acute care patients: A narrative review. Int. J. Nurs. Stud. 2007, 44, 1036–1054. [Google Scholar] [CrossRef]
- Schutz, P.; Bally, M.; Stanga, Z.; Keller, U. Loss of appetite in acutely ill medical inpatients: Physiological response or therapeutic target? Swiss Med. Wkly. 2014, 144, w13957. [Google Scholar] [CrossRef]
- Casaer, M.P.; Hermans, G.; Wilmer, A.; Van den Berghe, G. Impact of early parenteral nutrition completing enteral nutrition in adult critically ill patients (EPaNIC trial): A study protocol and statistical analysis plan for a randomized controlled trial. Trials 2011, 12, 21. [Google Scholar] [CrossRef]
- Felder, S.; Lechtenboehmer, C.; Bally, M.; Fehr, R.; Deiss, M.; Faessler, L.; Kutz, A.; Steiner, D.; Rast, A.C.; Laukemann, S.; et al. Association of nutritional risk and adverse medical outcomes across different medical inpatient populations. Nutrition 2015, 31, 1385–1393. [Google Scholar] [CrossRef]
- Villet, S.; Chiolero, R.L.; Bollmann, M.D.; Revelly, J.P.; Cayeux, M.C.; Delarue, J.; Berger, M.M. Negative impact of hypocaloric feeding and energy balance on clinical outcome in ICU patients. Clin. Nutr. 2005, 24, 502–509. [Google Scholar] [CrossRef]
- Sorensen, J.; Kondrup, J.; Prokopowicz, J.; Schiesser, M.; Krahenbuhl, L.; Meier, R.; Liberda, M. EuroOOPS: An international, multicentre study to implement nutritional risk screening and evaluate clinical outcome. Clin. Nutr. 2008, 27, 340–349. [Google Scholar] [CrossRef]
- Barton, A.D.; Beigg, C.L.; Macdonald, I.A.; Allison, S.P. High food wastage and low nutritional intakes in hospital patients. Clin. Nutr. 2000, 19, 445–449. [Google Scholar] [CrossRef] [PubMed]
- Gomes, F.; Schuetz, P.; Bounoure, L.; Austin, P.; Ballesteros-Pomar, M.; Cederholm, T.; Fletcher, J.; Laviano, A.; Norman, K.; Poulia, K.A.; et al. ESPEN guidelines on nutritional support for polymorbid internal medicine patients. Clin. Nutr. 2018, 37, 336–353. [Google Scholar] [CrossRef] [PubMed]
- Casaer, M.P.; Van den Berghe, G. Nutrition in the acute phase of critical illness. N. Engl. J. Med. 2014, 370, 1227–1236. [Google Scholar] [CrossRef] [PubMed]
- Felder, S.; Braun, N.; Stanga, Z.; Kulkarni, P.; Faessler, L.; Kutz, A.; Steiner, D.; Laukemann, S.; Haubitz, S.; Huber, A.; et al. Unraveling the Link between Malnutrition and Adverse Clinical Outcomes: Association of Acute and Chronic Malnutrition Measures with Blood Biomarkers from Different Pathophysiological States. Ann. Nutr. Metab. 2016, 68, 164–172. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tribolet, P.; Fehr, R.; Bächli, V.; Geiser, M.; Toplak, H.; Stanga, Z.; Schuetz, P. What are Barriers of Nutritional Therapy in Malnourished Medical Inpatients? An Observational Study. Aktuel Ernahr. 2017, 42, 167–179. [Google Scholar]
- Schetz, M.; Casaer, M.P.; Van den Berghe, G. Does artificial nutrition improve outcome of critical illness? Crit. Care 2013, 17, 302. [Google Scholar] [CrossRef]
- Russell, R.C.; Yuan, H.X.; Guan, K.L. Autophagy regulation by nutrient signaling. Cell Res. 2014, 24, 42–57. [Google Scholar] [CrossRef] [PubMed]
- Fujishima, I.; Fujiu-Kurachi, M.; Arai, H.; Hyodo, M.; Kagaya, H.; Maeda, K.; Mori, T.; Nishioka, S.; Oshima, F.; Ogawa, S.; et al. Sarcopenia and dysphagia: Position paper by four professional organizations. Geriatr. Gerontol. Int. 2019, 19, 91–97. [Google Scholar] [CrossRef] [Green Version]
- Morley, J.E. Defining Undernutrition (Malnutrition) in Older Persons. J. Nutr. Health Aging 2018, 22, 308–310. [Google Scholar] [CrossRef]
- Ortega, O.; Martin, A.; Clave, P. Diagnosis and Management of Oropharyngeal Dysphagia Among Older Persons, State of the Art. J. Am. Med. Direct. Assoc. 2017, 18, 576–582. [Google Scholar] [CrossRef]
- Arends, J.; Bachmann, P.; Baracos, V.; Barthelemy, N.; Bertz, H.; Bozzetti, F.; Fearon, K.; Hutterer, E.; Isenring, E.; Kaasa, S.; et al. ESPEN guidelines on nutrition in cancer patients. Clin. Nutr. 2017, 36, 11–48. [Google Scholar] [CrossRef] [PubMed]
- Forbes, A.; Escher, J.; Hebuterne, X.; Klek, S.; Krznaric, Z.; Schneider, S.; Shamir, R.; Stardelova, K.; Wierdsma, N.; Wiskin, A.E.; et al. ESPEN guideline: Clinical nutrition in inflammatory bowel disease. Clin. Nutr. 2017, 36, 321–347. [Google Scholar] [CrossRef] [PubMed]
- Meier, R.; Beglinger, C.; Layer, P.; Gullo, L.; Keim, V.; Laugier, R.; Friess, H.; Schweitzer, M.; Macfie, J. ESPEN guidelines on nutrition in acute pancreatitis. European Society of Parenteral and Enteral Nutrition. Clin. Nutr. 2002, 21, 173–183. [Google Scholar] [CrossRef] [PubMed]
- Plauth, M.; Bernal, W.; Dasarathy, S.; Merli, M.; Plank, L.D.; Schutz, T.; Bischoff, S.C. ESPEN guideline on clinical nutrition in liver disease. Clin. Nutr. 2019, 38, 485–521. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Turck, D.; Braegger, C.P.; Colombo, C.; Declercq, D.; Morton, A.; Pancheva, R.; Robberecht, E.; Stern, M.; Strandvik, B.; Wolfe, S.; et al. ESPEN-ESPGHAN-ECFS guidelines on nutrition care for infants, children, and adults with cystic fibrosis. Clin. Nutr. 2016, 35, 557–577. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bally, M.R.; Blaser Yildirim, P.Z.; Bounoure, L.; Gloy, V.L.; Mueller, B.; Briel, M.; Schuetz, P. Nutritional Support and Outcomes in Malnourished Medical Inpatients: A Systematic Review and Meta-analysis. JAMA Intern. Med. 2016, 176, 43–53. [Google Scholar] [CrossRef] [PubMed]
- Feinberg, J.; Nielsen, E.E.; Korang, S.K.; Halberg Engell, K.; Nielsen, M.S.; Zhang, K.; Didriksen, M.; Lund, L.; Lindahl, N.; Hallum, S.; et al. Nutrition support in hospitalised adults at nutritional risk. Cochrane Database Syst. Rev. 2017, 5, Cd011598. [Google Scholar] [CrossRef]
- Deutz, N.E.; Matheson, E.M.; Matarese, L.E.; Luo, M.; Baggs, G.E.; Nelson, J.L.; Hegazi, R.A.; Tappenden, K.A.; Ziegler, T.R. Readmission and mortality in malnourished, older, hospitalized adults treated with a specialized oral nutritional supplement: A randomized clinical trial. Clin. Nutr. 2016, 35, 18–26. [Google Scholar] [CrossRef] [Green Version]
- Schuetz, P.; Fehr, R.; Baechli, V.; Geiser, M.; Gomes, F.; Kutz, A.; Tribolet, P.; Bregenzer, T.; Hoess, C.; Pavlicek, V.; et al. Individualized nutritional support in medical inpatients at nutritional risk: A randomized clinical trial. Lancet 2019, 393, 2312–2321. [Google Scholar] [CrossRef]
- Cederholm, T.; Jensen, G.L.; Correia, M.; Gonzalez, M.C.; Fukushima, R.; Higashiguchi, T.; Baptista, G.; Barazzoni, R.; Blaauw, R.; Coats, A.J.S.; et al. GLIM criteria for the diagnosis of malnutrition—A consensus report from the global clinical nutrition community. J. Cachexia Sarcopenia Muscle 2019, 10, 207–217. [Google Scholar] [CrossRef]
- Ten Dam, S.; Droop, A.; Arjaans, W.; de Groot, S.; van Bokhorst-de van der Schueren, M. Module 11.1 Organisation of a Nutritional Support Team. In ESPEN LLL, Organisation of Nutritional Care Ethical and Legal Aspects: ESPEN; 2012; Available online: https://lllnutrition.com/mod/page/view.php?id=3422, (accessed on 29 July 2019).
- National Institute for Health and Clinical Excellence. Nutrition Support for Adults: Oral Nutrition Support, Enteral Tube Feeding and Parenteral Nutrition (Clinical Guidance 32) London: National Collaborating Centre for Acute Care (UK); National Institute for Health and Clinical Excellence: London, UK, 2006. [Google Scholar]
- Donini, L.M.; Savina, C.; Rosano, A.; Cannella, C. Systematic review of nutritional status evaluation and screening tools in the elderly. J. Nutr. Health Aging 2007, 11, 421–432. [Google Scholar] [PubMed]
- Foley, N.C.; Salter, K.L.; Robertson, J.; Teasell, R.W.; Woodbury, M.G. Which Reported Estimate of the Prevalence of Malnutrition After Stroke Is Valid? Stroke 2009, 40, E66–E74. [Google Scholar] [CrossRef] [PubMed]
- Bauer, J.M.; Kaiser, M.J.; Sieber, C.C. Evaluation of nutritional status in older persons: Nutritional screening and assessment. Curr. Opin. Clin. Nutr. Metab. Care 2010, 13, 8–13. [Google Scholar] [CrossRef] [PubMed]
- Weekes, C.E.; Elia, M.; Emery, P.W. The development, validation and reliability of a nutrition screening tool based on the recommendations of the British Association for Parenteral and Enteral Nutrition (BAPEN). Clin. Nutr. 2004, 23, 1104–1112. [Google Scholar] [PubMed]
- Power, L.; Mullally, D.; Gibney, E.R.; Clarke, M.; Visser, M.; Volkert, D.; Bardon, L.; de van der Schueren, M.A.E.; Corish, C.A. A review of the validity of malnutrition screening tools used in older adults in community and healthcare settings—A MaNuEL study. Clin. Nutr. ESPEN 2018, 24, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Van Bokhorst-de van der Schueren, M.A.; Guaitoli, P.R.; Jansma, E.P.; de Vet, H.C. Nutrition screening tools: Does one size fit all? A systematic review of screening tools for the hospital setting. Clin. Nutr. 2014, 33, 39–58. [Google Scholar] [CrossRef] [PubMed]
- Charney, P. Nutrition screening vs. nutrition assessment: How do they differ? Nutr. Clin. Pract. 2008, 23, 366–372. [Google Scholar] [CrossRef] [PubMed]
- Elia, M. Guidelines for Detection and Management of Malnutrition; British Association for Parenteral and Enteral Nutrition: Redditch, UK, 2000. [Google Scholar]
- Friedli, N.; Stanga, Z.; Culkin, A.; Crook, M.; Laviano, A.; Sobotka, L.; Kressig, R.W.; Kondrup, J.; Mueller, B.; Schuetz, P. Management and prevention of refeeding syndrome in medical inpatients: An evidence-based and consensus-supported algorithm. Nutrition 2018, 47, 13–20. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Deutz, N.E.; Bauer, J.M.; Barazzoni, R.; Biolo, G.; Boirie, Y.; Bosy-Westphal, A.; Cederholm, T.; Cruz-Jentoft, A.; Krznaric, Z.; Nair, K.S.; et al. Protein intake and exercise for optimal muscle function with aging: Recommendations from the ESPEN Expert Group. Clin. Nutr. 2014, 33, 929–936. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Volkert, D.; Beck, A.M.; Cederholm, T.; Cruz-Jentoft, A.; Goisser, S.; Hooper, L.; Kiesswetter, E.; Maggio, M.; Raynaud-Simon, A.; Sieber, C.C.; et al. ESPEN guideline on clinical nutrition and hydration in geriatrics. Clin. Nutr. 2019, 38, 10–47. [Google Scholar] [CrossRef] [PubMed]
- Gariballa, S.; Forster, S.; Walters, S.; Powers, H. A randomized, double-blind, placebo-controlled trial of nutritional supplementation during acute illness. Am. J. Med. 2006, 119, 693–699. [Google Scholar] [CrossRef] [PubMed]
- Hegerova, P.; Dedkova, Z.; Sobotka, L. Early nutritional support and physiotherapy improved long-term self-sufficiency in acutely ill older patients. Nutrition 2015, 31, 166–170. [Google Scholar] [CrossRef] [PubMed]
- Starke, J.; Schneider, H.; Alteheld, B.; Stehle, P.; Meier, R. Short-term individual nutritional care as part of routine clinical setting improves outcome and quality of life in malnourished medical patients. Clin. Nutr. 2011, 30, 194–201. [Google Scholar] [CrossRef] [PubMed]
- Volkert, D.; Hubsch, S.; Oster, P.; Schlierf, G. Nutritional support and functional status in undernourished geriatric patients during hospitalization and 6-month follow-up. Aging Clin. Exp. Res. 1996, 8, 386–395. [Google Scholar] [CrossRef]
- Bounoure, L.; Gomes, F.; Stanga, Z.; Keller, U.; Meier, R.; Ballmer, P.; Fehr, R.; Mueller, B.; Genton, L.; Bertrand, P.C.; et al. Detection and treatment of medical inpatients with or at-risk of malnutrition: Suggested procedures based on validated guidelines. Nutrition 2016, 32, 790–798. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wong, A.; Chew, A.; Wang, C.M.; Ong, L.; Zhang, S.H.; Young, S. The use of a specialised amino acid mixture for pressure ulcers: A placebo-controlled trial. J. Wound Care 2014, 23, 259–260. [Google Scholar] [CrossRef] [PubMed]
- Vandewoude, M.F.; Paridaens, K.M.; Suy, R.A.; Boone, M.A.; Strobbe, H. Fibre-supplemented tube feeding in the hospitalised elderly. Age Ageing 2005, 34, 120–124. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.M.; Holst, M.; Rasmussen, H.H. Oral nutritional support of older (65 years+) medical and surgical patients after discharge from hospital: Systematic review and meta-analysis of randomized controlled trials. Clin. Rehabil. 2013, 27, 19–27. [Google Scholar] [CrossRef] [PubMed]
- Munk, T.; Tolstrup, U.; Beck, A.M.; Holst, M.; Rasmussen, H.H.; Hovhannisyan, K.; Thomsen, T. Individualised dietary counselling for nutritionally at-risk older patients following discharge from acute hospital to home: A systematic review and meta-analysis. J. Hum. Nutr. Diet. 2016, 29, 196–208. [Google Scholar] [CrossRef] [PubMed]
- Aubry, E.; Mareschal, J.; Gschweitl, M.; Zvingelis, M.; Schuetz, P.; Stanga, Z. Facts zum Management der Klinischen Ernährung—Eine Online-Befragung. Aktuel Ernahr. 2018, 42, 452–460. [Google Scholar] [CrossRef]
- Lobo, D.N. Improving outcomes with a little EFFORT. Lancet 2019, 393, 2278–2280. [Google Scholar] [CrossRef]
| Country | Number of Participating Centers | Percentage of Hospitals with NST Present on Site | Percentage of Screening at Hospital Admission |
|---|---|---|---|
| Australia | 1 | 100 | 100 |
| Austria | 4 | 100 | 45.5 |
| Belgium | 52 | 88 | 77.3 |
| Brazil | 12 | 100 | 80.0 |
| Bulgaria | 1 | 66.7 | 0 |
| China | 9 | 100 | 56.5 |
| Colombia | 35 | 69.1 | 56.6 |
| Croatia | 3 | 55.6 | 20.0 |
| Germany | 36 | 60.9 | 49.5 |
| Greece | 3 | 100 | 0 |
| India | 13 | 7.7 | 50.1 |
| Japan | 9 | 100 | 50 |
| Netherlands | 1 | 100 | 0 |
| Poland | 4 | 0 | 60 |
| Portugal | 4 | 100 | 66.7 |
| Singapore | 1 | 0 | 82.6 |
| Spain | 5 | 100 | 50.0 |
| Sweden | 2 | 100 | 100 |
| Switzerland | 1 | 66.7 | 16.7 |
| Thailand | 1 | 100 | 66.7 |
| United States of America | 16 | 62.5 | 96.0 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Reber, E.; Gomes, F.; Bally, L.; Schuetz, P.; Stanga, Z. Nutritional Management of Medical Inpatients. J. Clin. Med. 2019, 8, 1130. https://doi.org/10.3390/jcm8081130
Reber E, Gomes F, Bally L, Schuetz P, Stanga Z. Nutritional Management of Medical Inpatients. Journal of Clinical Medicine. 2019; 8(8):1130. https://doi.org/10.3390/jcm8081130
Chicago/Turabian StyleReber, Emilie, Filomena Gomes, Lia Bally, Philipp Schuetz, and Zeno Stanga. 2019. "Nutritional Management of Medical Inpatients" Journal of Clinical Medicine 8, no. 8: 1130. https://doi.org/10.3390/jcm8081130






