Gastroparesis and Dumping Syndrome: Current Concepts and Management
Abstract
1. Introduction
2. Definitions and Epidemiology
2.1. Gastroparesis
2.2. Dumping Syndrome
3. Pathophysiology and Clinical Presentation
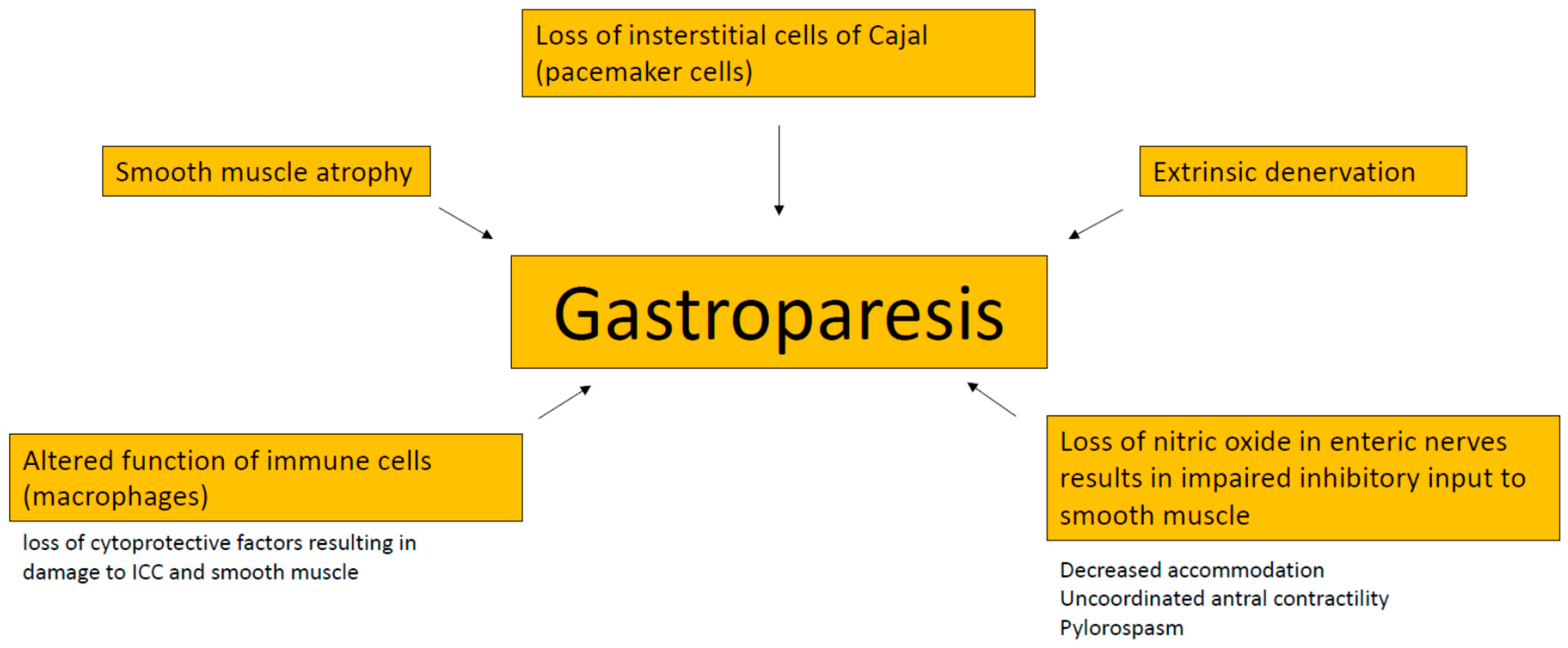
3.1. Gastroparesis
3.2. Dumping Syndrome
4. Diagnostic Evaluations
4.1. Gastroparesis
4.2. Dumping Syndrome
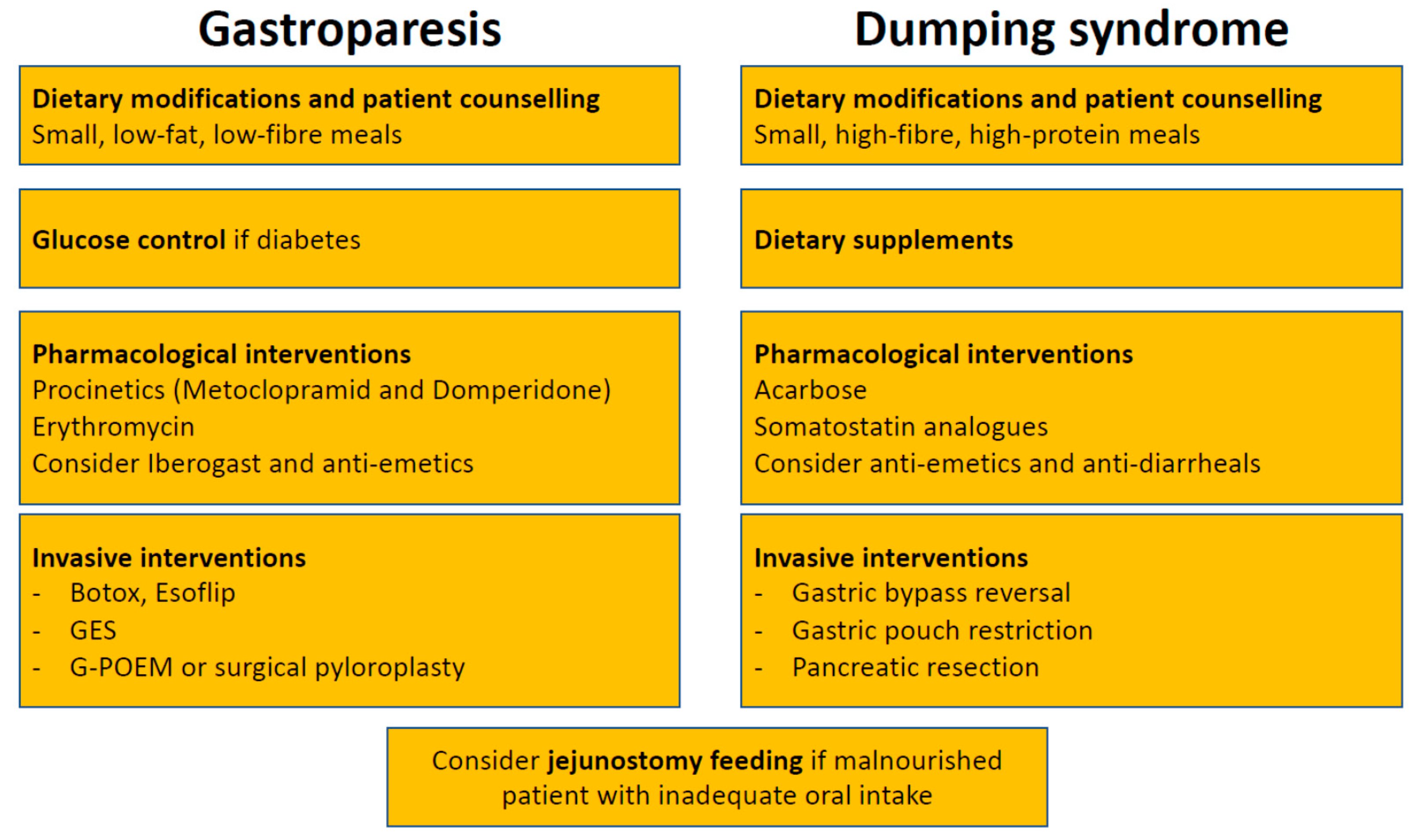
5. Treatment of Gastroparesis
6. Treatment of Dumping Syndrome
7. Conclusions
Author Contributions
Conflicts of Interest
References
- Camilleri, M.; Bharucha, A.E.; Farrugia, G. Epidemiology, mechanisms, and management of diabetic gastroparesis. Clin. Gastroenterol. Hepatol. 2011, 9, 5–12. [Google Scholar] [CrossRef] [PubMed]
- van Beek, A.P.; Emous, M.; Laville, M.; Tack, J. Dumping syndrome after esophageal, gastric or bariatric surgery: Pathophysiology, diagnosis, and management. Obes. Rev. 2017, 18, 68–85. [Google Scholar] [CrossRef] [PubMed]
- Talley, N.J.; Vakil, N.B.; Moayyedi, P. American gastroenterological association technical review on the evaluation of dyspepsia. Gastroenterology 2005, 129, 1756–1780. [Google Scholar] [CrossRef] [PubMed]
- Mulla, C.M.; Storino, A.; Yee, E.U.; Lautz, D.; Sawnhey, M.S.; Moser, A.J.; Patti, M.E. Insulinoma After Bariatric Surgery: Diagnostic Dilemma and Therapeutic Approaches. Obes. Surg. 2016, 26, 874–881. [Google Scholar] [CrossRef] [PubMed]
- Mathur, A.; Gorden, P.; Libutti, S.K. Insulinoma. Surg. Clin. N. Am. 2009, 89, 1105–1121. [Google Scholar] [CrossRef] [PubMed]
- Bharucha, A.E. Epidemiology and natural history of gastroparesis. Gastroenterol. Clin. N. Am. 2015, 44, 9–19. [Google Scholar] [CrossRef] [PubMed]
- Jung, H.K.; Choung, R.S.; Locke, G.R.; Schleck, C.D.; Zinsmeister, A.R.; Szarka, L.A.; Mullan, B.; Talley, N.J. The incidence, prevalence, and outcomes of patients with gastroparesis in Olmsted County, Minnesota, from 1996 to 2006. Gastroenterology 2009, 136, 1225–1233. [Google Scholar] [CrossRef] [PubMed]
- Rey, E.; Choung, R.S.; Schleck, C.D.; Zinsmeister, A.R.; Talley, N.J.; Locke, G.R. Prevalence of hidden gastroparesis in the community: The gastroparesis “iceberg”. J. Neurogastroenterol. Motil. 2012, 18, 34–42. [Google Scholar] [CrossRef]
- Choung, R.S.; Locke, G.R.; Schleck, C.D.; Zinsmeister, A.R.; Melton, L.J.; Talley, N.J. Risk of gastroparesis in subjects with type 1 and 2 diabetes in the general population. Am. J. Gastroenterol. 2012, 107, 82–88. [Google Scholar] [CrossRef]
- Horowitz, M.; Harding, P.E.; Maddox, A.F.; Wishart, J.M.; Akkermans, L.M.; Chatterton, B.E.; Shearman, D.J. Gastric and oesophageal emptying in patients with type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia 1989, 32, 151–159. [Google Scholar] [CrossRef]
- Horowitz, M.; Maddox, A.F.; Wishart, J.M.; Harding, P.E.; Chatterton, B.E.; Shearman, D.J. Relationships between oesophageal transit and solid and liquid gastric emptying in diabetes mellitus. Eur. J. Nucl. Med. 1991, 18, 229–234. [Google Scholar] [CrossRef] [PubMed]
- Dong, K.; Yu, X.J.; Li, B.; Wen, E.G.; Xiong, W.; Guan, Q.L. Advances in mechanisms of postsurgical gastroparesis syndrome and its diagnosis and treatment. Chin. J. Dig. Dis. 2006, 7, 76–82. [Google Scholar] [CrossRef] [PubMed]
- Dong, K.; Li, B.; Guan, Q.L.; Huang, T. Analysis of multiple factors of postsurgical gastroparesis syndrome after pancreaticoduodenectomy and cryotherapy for pancreatic cancer. World J. Gastroenterol. 2004, 10, 2434–2438. [Google Scholar] [CrossRef] [PubMed]
- Nusrat, S.; Bielefeldt, K. Gastroparesis on the rise: Incidence vs awareness? Neurogastroenterol. Motil. 2013, 25, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Tack, J.; Arts, J.; Caenepeel, P.; De Wulf, D.; Bisschops, R. Pathophysiology, diagnosis and management of postoperative dumping syndrome. Nat. Rev. Gastroenterol. Hepatol. 2009, 6, 583–590. [Google Scholar] [CrossRef]
- Tack, J.; Deloose, E. Complications of bariatric surgery: Dumping syndrome, reflux and vitamin deficiencies. Best Pract. Res. Clin. Gastroenterol. 2014, 28, 741–749. [Google Scholar] [CrossRef] [PubMed]
- Eagon, J.C.; Miedema, B.W.; Kelly, K.A. Postgastrectomy syndromes. Surg. Clin. N. Am. 1992, 72, 445–465. [Google Scholar] [CrossRef]
- Vecht, J.; Masclee, A.A.; Lamers, C.B. The dumping syndrome. Current insights into pathophysiology, diagnosis and treatment. Scand. J. Gastroenterol. Suppl. 1997, 223, 21–27. [Google Scholar]
- McLarty, A.J.; Deschamps, C.; Trastek, V.F.; Allen, M.S.; Pairolero, P.C.; Harmsen, W.S. Esophageal resection for cancer of the esophagus: Long-term function and quality of life. Ann. Thorac. Surg. 1997, 63, 1568–1572. [Google Scholar] [CrossRef]
- Banerjee, A.; Ding, Y.; Mikami, D.J.; Needleman, B.J. The role of dumping syndrome in weight loss after gastric bypass surgery. Surg. Endosc. 2013, 27, 1573–1578. [Google Scholar] [CrossRef]
- Papamargaritis, D.; Koukoulis, G.; Sioka, E.; Zachari, E.; Bargiota, A.; Zacharoulis, D.; Tzovaras, G. Dumping symptoms and incidence of hypoglycaemia after provocation test at 6 and 12 months after laparoscopic sleeve gastrectomy. Obes. Surg. 2012, 22, 1600–1606. [Google Scholar] [CrossRef] [PubMed]
- Tzovaras, G.; Papamargaritis, D.; Sioka, E.; Zachari, E.; Baloyiannis, I.; Zacharoulis, D.; Koukoulis, G. Symptoms suggestive of dumping syndrome after provocation in patients after laparoscopic sleeve gastrectomy. Obes. Surg. 2012, 22, 23–28. [Google Scholar] [CrossRef] [PubMed]
- Berg, P.; McCallum, R. Dumping Syndrome: A Review of the Current Concepts of Pathophysiology, Diagnosis, and Treatment. Dig. Dis. Sci. 2016, 61, 11–18. [Google Scholar] [CrossRef]
- O’Grady, G.; Angeli, T.R.; Du, P.; Lahr, C.; Lammers, W.J.E.P.; Windsor, J.A.; Abell, T.L.; Farrugia, G.; Pullan, A.J.; Cheng, L.K. Abnormal initiation and conduction of slow-wave activity in gastroparesis, defined by high-resolution electrical mapping. Gastroenterology 2012, 143, 589–598.e583. [Google Scholar] [CrossRef] [PubMed]
- Hyett, B.; Martinez, F.J.; Gill, B.M.; Mehra, S.; Lembo, A.; Kelly, C.P.; Leffler, D.A. Delayed radionucleotide gastric emptying studies predict morbidity in diabetics with symptoms of gastroparesis. Gastroenterology 2009, 137, 445–452. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.D.; Lin, Z.; Pan, J.; McCallum, R.W. Abnormal gastric myoelectrical activity and delayed gastric emptying in patients with symptoms suggestive of gastroparesis. Dig. Dis. Sci. 1996, 41, 1538–1545. [Google Scholar] [CrossRef] [PubMed]
- Oh, J.J.; Kim, C.H. Gastroparesis after a presumed viral illness: Clinical and laboratory features and natural history. Mayo Clin. Proc. 1990, 65, 636–642. [Google Scholar] [CrossRef]
- Bityutskiy, L.P.; Soykan, I.; McCallum, R.W. Viral gastroparesis: A subgroup of idiopathic gastroparesis--clinical characteristics and long-term outcomes. Am. J. Gastroenterol. 1997, 92, 1501–1504. [Google Scholar]
- Camilleri, M.; Parkman, H.P.; Shafi, M.A.; Abell, T.L.; Gerson, L. Clinical guideline: Management of gastroparesis. Am. J. Gastroenterol. 2013, 108, 18–37. [Google Scholar] [CrossRef]
- Mittal, R.K.; Frank, E.B.; Lange, R.C.; McCallum, R.W. Effects of morphine and naloxone on esophageal motility and gastric emptying in man. Dig. Dis. Sci. 1986, 31, 936–942. [Google Scholar] [CrossRef]
- Salehi, M.; Aulinger, B.A.; D’Alessio, D.A. Targeting beta-cell mass in type 2 diabetes: Promise and limitations of new drugs based on incretins. Endocr. Rev. 2008, 29, 367–379. [Google Scholar] [CrossRef] [PubMed]
- Maes, B.D.; Vanwalleghem, J.; Kuypers, D.; Ghoos, Y.; Rutgeerts, P.J.; Vanrenterghem, Y.F. Differences in gastric motor activity in renal transplant recipients treated with FK-506 versus cyclosporine. Transplantation 1999, 68, 1482–1485. [Google Scholar] [CrossRef] [PubMed]
- Samsom, M.; Vermeijden, J.R.; Smout, A.J.; Van Doorn, E.; Roelofs, J.; Van Dam, P.S.; Martens, E.P.; Eelkman-Rooda, S.J.; Van Berge-Henegouwen, G.P. Prevalence of delayed gastric emptying in diabetic patients and relationship to dyspeptic symptoms: A prospective study in unselected diabetic patients. Diabetes Care 2003, 26, 3116–3122. [Google Scholar] [CrossRef]
- Jones, K.L.; Russo, A.; Stevens, J.E.; Wishart, J.M.; Berry, M.K.; Horowitz, M. Predictors of delayed gastric emptying in diabetes. Diabetes Care 2001, 24, 1264–1269. [Google Scholar] [CrossRef] [PubMed]
- Horváth, V.J.; Izbéki, F.; Lengyel, C.; Kempler, P.; Várkonyi, T. Diabetic gastroparesis: Functional/morphologic background, diagnosis, and treatment options. Curr. Diabetes Rep. 2014, 14, 527. [Google Scholar] [CrossRef] [PubMed]
- Woodhouse, S.; Hebbard, G.; Knowles, S.R. Psychological controversies in gastroparesis: A systematic review. World J. Gastroenterol. 2017, 23, 1298–1309. [Google Scholar] [CrossRef] [PubMed]
- Bielefeldt, K. Gastroparesis: Concepts, controversies, and challenges. Scientifica (Cairo) 2012, 2012, 424802. [Google Scholar] [CrossRef]
- Liu, N.; Abell, T. Gastroparesis Updates on Pathogenesis and Management. Gut Liver 2017, 11, 579–589. [Google Scholar] [CrossRef]
- Cherian, D.; Sachdeva, P.; Fisher, R.S.; Parkman, H.P. Abdominal pain is a frequent symptom of gastroparesis. Clin. Gastroenterol. Hepatol. 2010, 8, 676–681. [Google Scholar] [CrossRef]
- Cherian, D.; Parkman, H.P. Nausea and vomiting in diabetic and idiopathic gastroparesis. Neurogastroenterol. Motil. 2012, 24, 217–222. [Google Scholar] [CrossRef]
- Tack, J. Gastric motor disorders. Best Pract. Res. Clin. Gastroenterol. 2007, 21, 633–644. [Google Scholar] [CrossRef] [PubMed]
- Mayer, E.A.; Thompson, J.B.; Jehn, D.; Reedy, T.; Elashoff, J.; Meyer, J.H. Gastric emptying and sieving of solid food and pancreatic and biliary secretion after solid meals in patients with truncal vagotomy and antrectomy. Gastroenterology 1982, 83 Pt 2, 184–192. [Google Scholar]
- Lawaetz, O.; Blackburn, A.M.; Bloom, S.R.; Aritas, Y.; Ralphs, D.N. Gut hormone profile and gastric emptying in the dumping syndrome. A hypothesis concerning the pathogenesis. Scand. J. Gastroenterol. 1983, 18, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Salehi, M.; Gastaldelli, A.; D’Alessio, D.A. Blockade of glucagon-like peptide 1 receptor corrects postprandial hypoglycemia after gastric bypass. Gastroenterology 2014, 146, 669–680. [Google Scholar] [CrossRef] [PubMed]
- Toft-Nielsen, M.; Madsbad, S.; Holst, J.J. Exaggerated secretion of glucagon-like peptide-1 (GLP-1) could cause reactive hypoglycaemia. Diabetologia 1998, 41, 1180–1186. [Google Scholar] [CrossRef] [PubMed]
- Eloy, R.; Garaud, J.C.; Moody, A.; Jaeck, D.; Grenier, J.F. Jejunal factor stimulating insulin release in the isolated perfused canine pancreas and jejunum. Horm. Metab. Res. 1975, 7, 461–467. [Google Scholar] [CrossRef]
- Mehagnoul-Schipper, D.J.; Lenders, J.W.; Willemsen, J.J.; Hopman, W.P. Sympathoadrenal activation and the dumping syndrome after gastric surgery. Clin. Auton. Res. 2000, 10, 301–308. [Google Scholar] [CrossRef]
- Holdsworth, C.D.; Turner, D.; McIntyre, N. Pathophysiology of post-gastrectomy hypoglycaemia. Br. Med. J. 1969, 4, 257–259. [Google Scholar] [CrossRef]
- Hejazi, R.A.; Patil, H.; McCallum, R.W. Dumping syndrome: Establishing criteria for diagnosis and identifying new etiologies. Dig. Dis. Sci. 2010, 55, 117–123. [Google Scholar] [CrossRef]
- Berg, P.; McCallum, R.; Hall, M.; Sarosiek, I. Dumping Syndrome: Updated Perspectives on Etiologies and Diagnosis. Pract. Gastroenterol. 2014, 38, 30–38. [Google Scholar]
- Arts, J.; Caenepeel, P.; Bisschops, R.; Dewulf, D.; Holvoet, L.; Piessevaux, H.; Bourgeois, S.; Sifrim, D.; Janssens, J.; Tack, J. Efficacy of the long-acting repeatable formulation of the somatostatin analogue octreotide in postoperative dumping. Clin. Gastroenterol. Hepatol. 2009, 7, 432–437. [Google Scholar] [CrossRef] [PubMed]
- Marsk, R.; Jonas, E.; Rasmussen, F.; Näslund, E. Nationwide cohort study of post-gastric bypass hypoglycaemia including 5,040 patients undergoing surgery for obesity in 1986–2006 in Sweden. Diabetologia 2010, 53, 2307–2311. [Google Scholar] [CrossRef] [PubMed]
- Tack, J.; Bisschops, R.; Sarnelli, G. Pathophysiology and treatment of functional dyspepsia. Gastroenterology 2004, 127, 1239–1255. [Google Scholar] [CrossRef] [PubMed]
- Bredenoord, A.J.; Chial, H.J.; Camilleri, M.; Mullan, B.P.; Murray, J.A. Gastric accommodation and emptying in evaluation of patients with upper gastrointestinal symptoms. Clin. Gastroenterol. Hepatol. 2003, 1, 264–272. [Google Scholar] [CrossRef]
- Abell, T.L.; Camilleri, M.; Donohoe, K.; Hasler, W.L.; Lin, H.C.; Maurer, A.H.; McCallum, R.W.; Nowak, T.; Nusynowitz, M.L.; Parman, H.P.; et al. Consensus recommendations for gastric emptying scintigraphy: A joint report of the American Neurogastroenterology and Motility Society and the Society of Nuclear Medicine. Am. J. Gastroenterol. 2008, 103, 753–763. [Google Scholar] [CrossRef] [PubMed]
- Tougas, G.; Eaker, E.Y.; Abell, T.L.; Abrahamsson, H.; Boivin, M.; Chen, J.; Hocking, M.P.; Quigley, E.M.; Koch, K.L.; Tokayer, A.Z.; et al. Assessment of gastric emptying using a low fat meal: Establishment of international control values. Am. J. Gastroenterol. 2000, 95, 1456–1462. [Google Scholar] [CrossRef] [PubMed]
- Keller, J.; Bassotti, G.; Clarke, J.; Dinning, P.; Fox, M.; Grover, M.; Hellström, P.M.; Ke, M.; Layer, P.; Malagelada, C.; et al. Expert consensus document: Advances in the diagnosis and classification of gastric and intestinal motility disorders. Nat. Rev. Gastroenterol. Hepatol. 2018, 15, 291–308. [Google Scholar] [CrossRef]
- Camilleri, M. Clinical practice. Diabetic gastroparesis. N. Engl. J. Med. 2007, 356, 820–829. [Google Scholar] [CrossRef]
- de Zwart, I.M.; de Roos, A. MRI for the evaluation of gastric physiology. Eur. Radiol. 2010, 20, 2609–2616. [Google Scholar] [CrossRef][Green Version]
- Bradshaw, L.A.; Cheng, L.K.; Chung, E.; Obioha, C.B.; Erickson, J.C.; Gorman, B.L.; Somarajan, S.; Richars, W.O. Diabetic gastroparesis alters the biomagnetic signature of the gastric slow wave. Neurogastroenterol. Motil. 2016, 28, 837–848. [Google Scholar] [CrossRef]
- Mine, S.; Sano, T.; Tsutsumi, K.; Murakami, Y.; Ehara, K.; Saka, M.; Hara, K.; Fukagawa, T.; Udagawa, H.; Katai, H. Large-scale investigation into dumping syndrome after gastrectomy for gastric cancer. J. Am. Coll. Surg. 2010, 211, 628–636. [Google Scholar] [CrossRef] [PubMed]
- Ritz, P.; Hanaire, H. Post-bypass hypoglycaemia: A review of current findings. Diabetes Metab. 2011, 37, 274–281. [Google Scholar] [CrossRef] [PubMed]
- van der Kleij, F.G.; Vecht, J.; Lamers, C.B.; Masclee, A.A. Diagnostic value of dumping provocation in patients after gastric surgery. Scand. J. Gastroenterol. 1996, 31, 1162–1166. [Google Scholar] [CrossRef] [PubMed]
- Khoo, C.M.; Muehlbauer, M.J.; Stevens, R.D.; Pamuklar, Z.; Chen, J.; Newgard, C.B.; Torquati, A. Postprandial metabolite profiles reveal differential nutrient handling after bariatric surgery compared with matched caloric restriction. Ann. Surg. 2014, 259, 687–693. [Google Scholar] [CrossRef] [PubMed]
- Emous, M.; Ubels, F.L.; van Beek, A.P. Diagnostic tools for post-gastric bypass hypoglycaemia. Obes. Rev. 2015, 16, 843–856. [Google Scholar] [CrossRef] [PubMed]
- Waseem, S.; Moshiree, B.; Draganov, P.V. Gastroparesis: Current diagnostic challenges and management considerations. World J. Gastroenterol. 2009, 15, 25–37. [Google Scholar] [CrossRef]
- Ogorek, C.P.; Davidson, L.; Fisher, R.S.; Krevsky, B. Idiopathic gastroparesis is associated with a multiplicity of severe dietary deficiencies. Am. J. Gastroenterol. 1991, 86, 423–428. [Google Scholar]
- Parkman, H.P.; Yates, K.P.; Hasler, W.L.; Nguyan, L.; Pasricha, P.J.; Snape, W.J.; Farrugia, G.; Calles, J.; Koch, K.L.; Abell, T.L.; et al. Dietary intake and nutritional deficiencies in patients with diabetic or idiopathic gastroparesis. Gastroenterology 2011, 141, 486–498. [Google Scholar] [CrossRef]
- Bytzer, P.; Talley, N.J.; Hammer, J.; Young, L.J.; Jones, M.P.; Horowitz, M. GI symptoms in diabetes mellitus are associated with both poor glycemic control and diabetic complications. Am. J. Gastroenterol. 2002, 97, 604–611. [Google Scholar] [CrossRef]
- Quigley, E.M. Pharmacotherapy of gastroparesis. Expert Opin. Pharmacother. 2000, 1, 881–887. [Google Scholar] [CrossRef]
- Patterson, D.; Abell, T.; Rothstein, R.; Koch, K.; Barnett, J. A double-blind multicenter comparison of domperidone and metoclopramide in the treatment of diabetic patients with symptoms of gastroparesis. Am. J. Gastroenterol. 1999, 94, 1230–1234. [Google Scholar] [PubMed]
- McCallum, R.W.; Ricci, D.A.; Rakatansky, H.; Behar, J.; Rhodes, J.B.; Salen, G.; Deren, J.; Ippoliti, A.; Olsen, H.W.; Falchuk, K.; et al. A multicenter placebo-controlled clinical trial of oral metoclopramide in diabetic gastroparesis. Diabetes Care 1983, 6, 463–467. [Google Scholar] [CrossRef] [PubMed]
- Janssen, P.; Harris, M.S.; Jones, M.; Masaoka, T.; Farre, R.; Törnblom, H.; Van Oudenhove, L.; Simren, M.; Tack, J. The relation between symptom improvement and gastric emptying in the treatment of diabetic and idiopathic gastroparesis. Am. J. Gastroenterol. 2013, 108, 1382–1391. [Google Scholar] [CrossRef] [PubMed]
- Stanghellini, V.; Tack, J. Gastroparesis: Separate entity or just a part of dyspepsia? Gut 2014, 63, 1972–1978. [Google Scholar] [CrossRef] [PubMed]
- Rao, A.S.; Camilleri, M. Review article: Metoclopramide and tardive dyskinesia. Aliment. Pharmacol. Ther. 2010, 31, 11–19. [Google Scholar] [CrossRef] [PubMed]
- Richards, R.D.; Davenport, K.; McCallum, R.W. The treatment of idiopathic and diabetic gastroparesis with acute intravenous and chronic oral erythromycin. Am. J. Gastroenterol. 1993, 88, 203–207. [Google Scholar] [PubMed]
- Pasricha, P.J.; Yates, K.P.; Sarosiek, I.; McCallum, R.W.; Abell, T.L.; Koch, K.L.; Nguyen, L.A.B.; Snape, W.J.; Hasler, W.L.; Clarke, J.O.; et al. Aprepitant Has Mixed Effects on Nausea and Reduces Other Symptoms in Patients With Gastroparesis and Related Disorders. Gastroenterology 2018, 154, 65–76. [Google Scholar] [CrossRef] [PubMed]
- Braden, B.; Caspary, W.; Börner, N.; Vinson, B.; Schneider, A.R. Clinical effects of STW 5 (Iberogast) are not based on acceleration of gastric emptying in patients with functional dyspepsia and gastroparesis. Neurogastroenterol. Motil. 2009, 21, 632–638. [Google Scholar] [CrossRef] [PubMed]
- Friedenberg, F.; Gollamudi, S.; Parkman, H.P. The use of botulinum toxin for the treatment of gastrointestinal motility disorders. Dig. Dis. Sci. 2004, 49, 165–175. [Google Scholar] [CrossRef] [PubMed]
- Ezzeddine, D.; Jit, R.; Katz, N.; Gopalswamy, N.; Bhutani, M.S. Pyloric injection of botulinum toxin for treatment of diabetic gastroparesis. Gastrointest. Endosc. 2002, 55, 920–923. [Google Scholar] [CrossRef] [PubMed]
- Lacy, B.E.; Zayat, E.N.; Crowell, M.D.; Schuster, M.M. Botulinum toxin for the treatment of gastroparesis: A preliminary report. Am. J. Gastroenterol. 2002, 97, 1548–1552. [Google Scholar] [CrossRef] [PubMed]
- Miller, L.S.; Szych, G.A.; Kantor, S.B.; Bromer, M.Q.; Knight, L.C.; Maurer, A.H.; Fisher, R.S.; Parkman, H.P. Treatment of idiopathic gastroparesis with injection of botulinum toxin into the pyloric sphincter muscle. Am. J. Gastroenterol. 2002, 97, 1653–1660. [Google Scholar] [CrossRef] [PubMed]
- Arts, J.; Holvoet, L.; Caenepeel, P.; Bisschops, R.; Sifrim, D.; Verbeke, K.; Janssens, J.; Tack, J. Clinical trial: A randomized-controlled crossover study of intrapyloric injection of botulinum toxin in gastroparesis. Aliment. Pharmacol. Ther. 2007, 26, 1251–1258. [Google Scholar] [CrossRef] [PubMed]
- Friedenberg, F.K.; Palit, A.; Parkman, H.P.; Hanlon, A.; Nelson, D.B. Botulinum toxin A for the treatment of delayed gastric emptying. Am. J. Gastroenterol. 2008, 103, 416–423. [Google Scholar] [CrossRef] [PubMed]
- Angeli, T.R.; Du, P.; Midgley, D.; Paskaranandavadivel, N.; Sathar, S.; Lahr, C.; Abell, T.L.; Cheng, L.K.; O’Grady, G. Acute Slow Wave Responses to High-Frequency Gastric Electrical Stimulation in Patients With Gastroparesis Defined by High-Resolution Mapping. Neuromodulation 2016, 19, 864–871. [Google Scholar] [CrossRef] [PubMed]
- Abell, T.; McCallum, R.; Hocking, M.; Koch, K.; Abrahamsson, H.; Leblanc, I.; Lindberg, G.; Konturek, J.; Nowak, T.; Quigley, E.M.; et al. Gastric electrical stimulation for medically refractory gastroparesis. Gastroenterology 2003, 125, 421–428. [Google Scholar] [CrossRef]
- Chu, H.; Lin, Z.; Zhong, L.; McCallum, R.W.; Hou, X. Treatment of high-frequency gastric electrical stimulation for gastroparesis. J. Gastroenterol. Hepatol. 2012, 27, 1017–1026. [Google Scholar] [CrossRef]
- Khashab, M.A.; Ngamruengphong, S.; Carr-Locke, D.; Bapaye, A.; Benias, P.C.; Serouya, S.; Dorwat, S.; Chaves, D.M.; Artifon, E.; de Moura, E.G.; et al. Gastric per-oral endoscopic myotomy for refractory gastroparesis: Results from the first multicenter study on endoscopic pyloromyotomy (with video). Gastrointest. Endosc. 2017, 85, 123–128. [Google Scholar] [CrossRef]
- Khashab, M.A.; Stein, E.; Clarke, J.O.; Saxena, P.; Kumbhari, V.; Chander Roland, B.; Kalloo, A.N.; Stavropoulos, S.; Pasricha, P.; Inoue, H. Gastric peroral endoscopic myotomy for refractory gastroparesis: First human endoscopic pyloromyotomy (with video). Gastrointest. Endosc. 2013, 78, 764–768. [Google Scholar] [CrossRef]
- Dacha, S.; Mekaroonkamol, P.; Li, L.; Shahnavaz, N.; Sakaria, S.; Keilin, S.; Willingham, F.; Christie, J.; Cai, Q. Outcomes and quality-of-life assessment after gastric per-oral endoscopic pyloromyotomy (with video). Gastrointest. Endosc. 2017, 86, 282–289. [Google Scholar] [CrossRef]
- Gonzalez, J.M.; Benezech, A.; Vitton, V.; Barthet, M. G-POEM with antro-pyloromyotomy for the treatment of refractory gastroparesis: Mid-term follow-up and factors predicting outcome. Aliment. Pharmacol. Ther. 2017, 46, 364–370. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez, J.M.; Lestelle, V.; Benezech, A.; Cohen, J.; Vitton, V.; Grimaud, J.C.; Barthet, M. Gastric per-oral endoscopic myotomy with antropyloromyotomy in the treatment of refractory gastroparesis: Clinical experience with follow-up and scintigraphic evaluation (with video). Gastrointest. Endosc. 2017, 85, 132–139. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez, J.H.; Haskins, I.N.; Strong, A.T.; Plescia, R.L.; Allemang, M.T.; Butler, R.S.; Cline, M.S.; El-Hayek, K.; Ponsky, J.L.; Kroh, M.D. Per oral endoscopic pyloromyotomy for refractory gastroparesis: Initial results from a single institution. Surg. Endosc. 2017, 31, 5381–5388. [Google Scholar] [CrossRef] [PubMed]
- Gourcerol, G.; Tissier, F.; Melchior, C.; Touchais, J.Y.; Huet, E.; Prevost, G.; Leroi, A.M.; Ducrotte, P. Impaired fasting pyloric compliance in gastroparesis and the therapeutic response to pyloric dilatation. Aliment. Pharmacol. Ther. 2015, 41, 360–367. [Google Scholar] [CrossRef]
- Hibbard, M.L.; Dunst, C.M.; Swanström, L.L. Laparoscopic and endoscopic pyloroplasty for gastroparesis results in sustained symptom improvement. J. Gastrointest. Surg. 2011, 15, 1513–1519. [Google Scholar] [CrossRef]
- Felsher, J.; Chand, B.; Ponsky, J. Decompressive percutaneous endoscopic gastrostomy in nonmalignant disease. Am. J. Surg. 2004, 187, 254–256. [Google Scholar] [CrossRef]
- Pittman, A.C.; Robinson, F.W. Dietary management of the “dumping” syndrome. Long-term follow-up. J. Am. Diet. Assoc. 1962, 40, 108–110. [Google Scholar]
- Robinson, F.W.; Pittman, A.C. Dietary management of postgastrectomy dumping syndrome. Surg. Gynecol. Obstet. 1957, 104, 529–534. [Google Scholar]
- Khoshoo, V.; Reifen, R.M.; Gold, B.D.; Sherman, P.M.; Pencharz, P.B. Nutritional manipulation in the management of dumping syndrome. Arch. Dis. Child. 1991, 66, 1447–1448. [Google Scholar] [CrossRef]
- Kellogg, T.A.; Bantle, J.P.; Leslie, D.B.; Redmond, J.B.; Slusarek, B.; Swan, T.; Buchwald, H.; Ikramuddin, S. Postgastric bypass hyperinsulinemic hypoglycemia syndrome: Characterization and response to a modified diet. Surg. Obes. Relat. Dis. 2008, 4, 492–499. [Google Scholar] [CrossRef]
- Ukleja, A. Dumping syndrome: Pathophysiology and treatment. Nutr. Clin. Pract. 2005, 20, 517–525. [Google Scholar] [CrossRef] [PubMed]
- Jenkins, D.J.; Gassull, M.A.; Leeds, A.R.; Metz, G.; Dilawari, J.B.; Slavin, B.; Blendis, L.M. Effect of dietary fiber on complications of gastric surgery: Prevention of postprandial hypoglycemia by pectin. Gastroenterology 1977, 73, 215–217. [Google Scholar] [CrossRef]
- Harju, E.; Larmi, T.K. Efficacy of guar gum in preventing the dumping syndrome. JPEN J. Parenter. Enter. Nutr. 1983, 7, 470–472. [Google Scholar] [CrossRef] [PubMed]
- Kneepkens, C.M.; Fernandes, J.; Vonk, R.J. Dumping syndrome in children. Diagnosis and effect of glucomannan on glucose tolerance and absorption. Acta Paediatr. Scand. 1988, 77, 279–286. [Google Scholar] [CrossRef] [PubMed]
- Ng, D.D.; Ferry, R.J.; Kelly, A.; Weinzimer, S.A.; Stanley, C.A.; Katz, L.E. Acarbose treatment of postprandial hypoglycemia in children after Nissen fundoplication. J. Pediatr. 2001, 139, 877–879. [Google Scholar] [CrossRef] [PubMed]
- Ritz, P.; Vaurs, C.; Bertrand, M.; Anduze, Y.; Guillaume, E.; Hanaire, H. Usefulness of acarbose and dietary modifications to limit glycemic variability following Roux-en-Y gastric bypass as assessed by continuous glucose monitoring. Diabetes Technol. Ther. 2012, 14, 736–740. [Google Scholar] [CrossRef] [PubMed]
- Speth, P.A.; Jansen, J.B.; Lamers, C.B. Effect of acarbose, pectin, a combination of acarbose with pectin, and placebo on postprandial reactive hypoglycaemia after gastric surgery. Gut 1983, 24, 798–802. [Google Scholar] [CrossRef] [PubMed]
- McLoughlin, J.C.; Buchanan, K.D.; Alam, M.J. A glycoside-hydrolase inhibitor in treatment of dumping syndrome. Lancet 1979, 2, 603–605. [Google Scholar] [CrossRef]
- Hasegawa, T.; Yoneda, M.; Nakamura, K.; Ohnishi, K.; Harada, H.; Kyouda, T.; Yoshida, Y.; Makino, I. Long-term effect of alpha-glucosidase inhibitor on late dumping syndrome. J. Gastroenterol. Hepatol. 1998, 13, 1201–1206. [Google Scholar] [CrossRef] [PubMed]
- Didden, P.; Penning, C.; Masclee, A.A. Octreotide therapy in dumping syndrome: Analysis of long-term results. Aliment. Pharmacol. Ther. 2006, 24, 1367–1375. [Google Scholar] [CrossRef] [PubMed]
- Penning, C.; Vecht, J.; Masclee, A.A. Efficacy of depot long-acting release octreotide therapy in severe dumping syndrome. Aliment. Pharmacol. Ther. 2005, 22, 963–969. [Google Scholar] [CrossRef] [PubMed]
- Deloose, E.; Bisschops, R.; Holvoet, L.; Arts, J.; De Wulf, D.; Caenepeel, P.; Lannoo, M.; Vanuytsel, T.; Andrews, C.; Tack, J. A pilot study of the effects of the somatostatin analog pasireotide in postoperative dumping syndrome. Neurogastroenterol. Motil. 2014, 26, 803–809. [Google Scholar] [CrossRef] [PubMed]
- Vilarrasa, N.; Goday, A.; Rubio, M.A.; Caixas, A.; Pellitero, S.; Ciudin, A.; Calanas, A.; Botella, J.I.; Breton, I.; Morales, M.J.; et al. Hyperinsulinemic Hypoglycemia after Bariatric Surgery: Diagnosis and Management Experience from a Spanish Multicenter Registry. Obes. Facts 2016, 9, 41–51. [Google Scholar] [CrossRef] [PubMed]
| Symptoms and Causes of Gastroparesis |
|---|
| Symptoms: |
| Postprandial fullness, early satiety, bloating, abdominal distension, nausea, and vomiting, abdominal pain, and dysphagia |
| Causes: |
| Diabetes Non-diabetic causes Surgery (such as gastrectomy with vagotomy, vagal nerve injury, Roux-en-Y, pancreatectomy, anti-reflux operations, lung transplant) Gastrointestinal disorders: gastroesophageal reflux, gastric ulcer disease, gastritis, atrophic gastritis, pancreatitis Diseases of the nervous system (such as parkinsonism) Connective tissue diseases (such as scleroderma) Unknown (“idiopathic gastroparesis”) Paraneoplastic Mesenteric ischemia Viral infections: e.g., CMV Side effect of medications Metabolic and endocrine disorders: hypothyroidism, pregnancy, uremia |
| Symptoms and Causes of Dumping Syndrome |
|---|
| Symptoms: |
| Early dumping syndrome (within 1 h after meal ingestion) Gastrointestinal symptoms: Abdominal pain, epigastric fullness, diarrhea, nausea, vomiting, borborygmi, and bloating Vasomotor symptoms: desire to lie down, palpitations and tachycardia, fatigue, faintness, syncope, perspiration, headache, light-headedness, hypotension, flushing, and pallor |
| Late dumping syndrome (1–3 h after meal ingestion) Neuroglycopenia: fatigue, weakness, confusion, hunger and syncope Autonomic reactivity: perspiration, palpitations, tremor and irritability |
| Causes: |
| Surgery: gastrojejunostomy, antrectomy, pylorectomy, pyloroplasty, esophagectomy, vagotomy, Roux-en Y bypass, Nissen fundoplication Not-surgery related: diabetes mellitus, viral illness, unkown (“idiopathic”) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vavricka, S.R.; Greuter, T. Gastroparesis and Dumping Syndrome: Current Concepts and Management. J. Clin. Med. 2019, 8, 1127. https://doi.org/10.3390/jcm8081127
Vavricka SR, Greuter T. Gastroparesis and Dumping Syndrome: Current Concepts and Management. Journal of Clinical Medicine. 2019; 8(8):1127. https://doi.org/10.3390/jcm8081127
Chicago/Turabian StyleVavricka, Stephan R., and Thomas Greuter. 2019. "Gastroparesis and Dumping Syndrome: Current Concepts and Management" Journal of Clinical Medicine 8, no. 8: 1127. https://doi.org/10.3390/jcm8081127
APA StyleVavricka, S. R., & Greuter, T. (2019). Gastroparesis and Dumping Syndrome: Current Concepts and Management. Journal of Clinical Medicine, 8(8), 1127. https://doi.org/10.3390/jcm8081127




