The Use of Yoga to Manage Stress and Burnout in Healthcare Workers: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
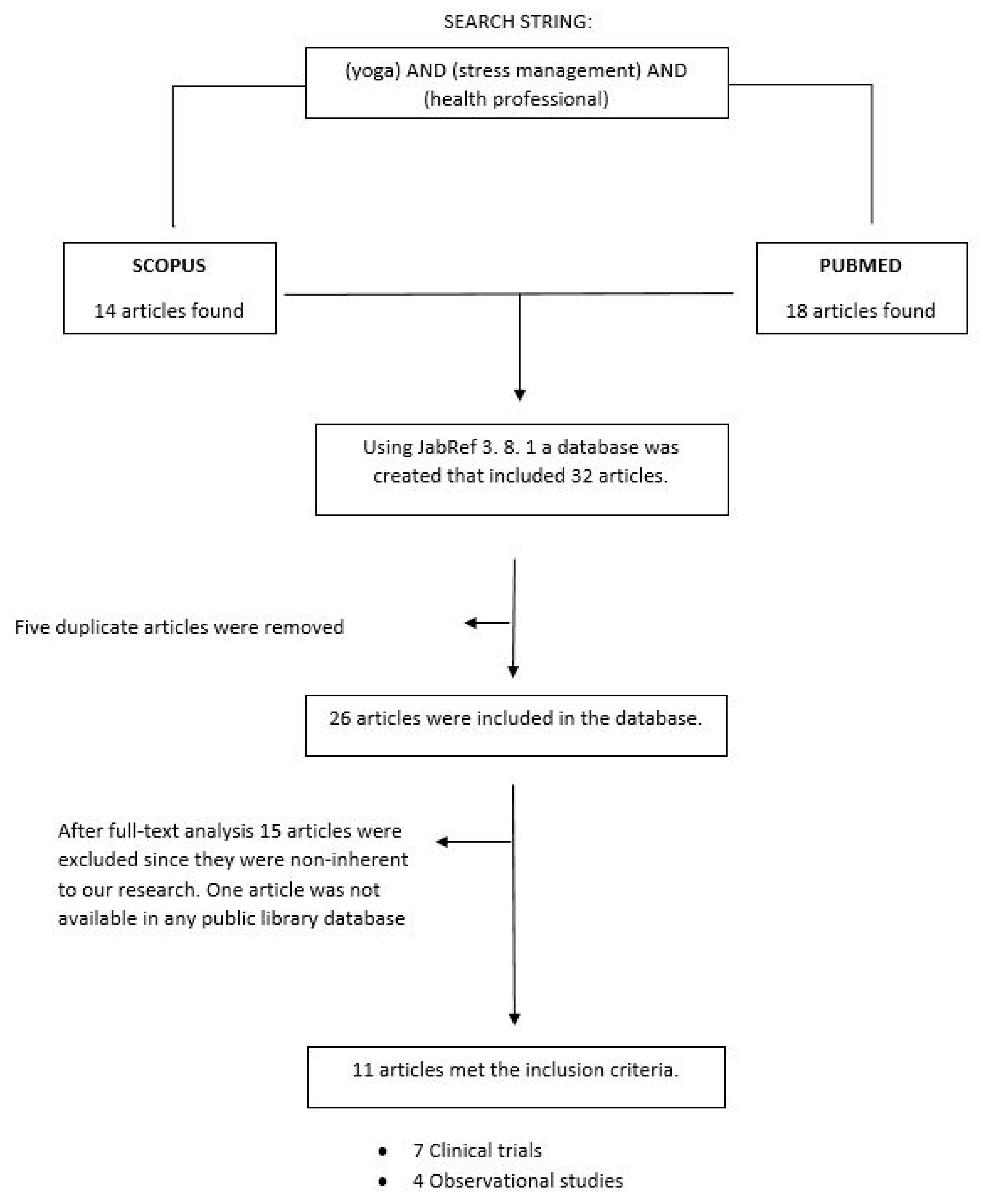
2.1. Identification of Relevant Studies
2.2. Study Selection and Eligibility Criteria
2.3. Data Extraction
2.4. Quality Assessment
3. Results
3.1. Physical Problems in Healthcare Professionals
3.2. Psycho-Emotional Problems in Healthcare Professionals
3.3. The Use of Yoga as a Tool for the Welfare of the Healthcare Worker
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Bond, A.R.; Mason, H.F.; Lemaster, C.M.; Shaw, S.E.; Mullin, C.S.; Hplick, E.A.; Saper, R.B. Embodied health: the effects of a mind-body course for medical students. Med. Educ. Online 2013, 18, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Shirey, M.R. An evidence based solution for minimizing stress and anger in nursing students. J. Nurs. Educ. 2007, 46, 568–571. [Google Scholar] [PubMed]
- Perez, G.K.; Haime, V.; Jackson, V.; Chittenden, E.; Mehta, D.H.; Park, E.R. Promoting resiliency among palliative care clinicians: Stressors, coping strategies, and training needs. J. Palliat Med. 2015, 18, 332–337. [Google Scholar] [CrossRef] [PubMed]
- Wiederhold, B.K.; Cipresso, P.; Pizzioli, D.; Wiederhold, M.; Riva, G. Intervention for Physician Burnout: A Systematic Review. Open Med. 2018, 13, 253–263. [Google Scholar] [CrossRef] [PubMed]
- Alexander, G.K.; Rollins, K.; Walker, D.; Wong, L.; Pennings, J. Yoga for Self-Care and Burnout Prevention Among Nurses. Workplace Health Saf. 2015, 63, 462–470. [Google Scholar] [CrossRef] [PubMed]
- Fang, R.; Li, X. A regular yoga intervention for staff nurse sleep quality and work stress: A randomised controlled trial. J. Clin. Nurs. 2015, 24, 3374–3379. [Google Scholar] [CrossRef] [PubMed]
- Repar, P.A.; Patton, D. Stress reduction for nurses through Arts-in-Medicine at the University of New Mexico Hospitals. Holist Nurs. Pract. 2007, 21, 182–186. [Google Scholar] [CrossRef] [PubMed]
- Chismark, A.M.; Asher, G.; Stein, M.; Tavoc, T.; Curran, A. Use of complementary and alternative medicine for work-related pain correlates with career satisfaction among dental hygienists. J. Dent. Hyg. 2011, 85, 273–284. [Google Scholar] [PubMed]
- Benson, H.; Casey, A. Stress Management: Approaches for Preventing and Reducing Stress; Harvard Health Publications: Boston, MA, USA, 2013. [Google Scholar]
- Wu, S.; Li, H.; Zhu, W.; Lin, S.; Chai, W.; Wang, X. Effect of work stressors, personal strain, and coping resources on burnout in Chinese medical professionals: A structural equation model. Ind. Health 2012, 50, 279–287. [Google Scholar] [CrossRef] [PubMed]
- Nieuwenhuijsen, K.; Bruinvels, D.; Frings Dresen, M. Psychosocial work environment and stress related disorders, a systematic review. Occup. Med. 2010, 60, 277–286. [Google Scholar] [CrossRef] [PubMed]
- LeBlanc, V.R. The effects of acute stress on performance: Implications for health professions education. Acad. Med 2009, 84, S25–S33. [Google Scholar] [CrossRef] [PubMed]
- Mathad, M.D.; Pradhan, B.; Sasidharan, R.K. Effect of Yoga on Psychological Functioning of Nursing Students: A Randomized Wait List Control Trial. J. Clin. Diagn Res. 2017, 11, KC01–KC05. [Google Scholar] [CrossRef] [PubMed]
- Axén, I.; Follin, G. Medical yoga in the workplace setting—Perceived stress and work ability—A feasibility study. Complement. Ther. Med. 2017, 30, 61–66. [Google Scholar] [CrossRef] [PubMed]
- Klatt, M.; Steinberg, B.; Duchemin, A.M. Mindfulness in Motion (MIM): an onsite Mindfulness Based Intervention (MBI) for chronically high stress work environments to increase resiliency and work engagement. J. Vis. Exp. 2015, 101, e52359. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Jadad, A.R.; Moore, R.A.; Carroll, D.; Jenkinson, C.; Reynolds, D.J.; Gavaghan, D.J.; McQuay, H.J. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control. Clin. Trials 1996, 17, 1–12. [Google Scholar] [CrossRef]
- Wells, G.A.; Shea, B.; O’Connell, D.; Peterson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle-Ottawa Scale (NOS) for assessing the quality of non randomised studies in meta-analyses. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 1 August 2017).
- Riley, K.E.; Park, C.L.; Wilson, A.; Sabo, A.N.; Antoni, M.H.; Braun, T.D.; Harrington, J.; Reiss, J.; Harris, A.D.; Cope, S.; et al. Improving physical and mental health in frontline mental health care providers: yoga-based stress management versus cognitive behavioral stress management. J. Workplace Behav. Health 2017, 32. [Google Scholar] [CrossRef]
- Kemper, K.; Bulla, S.; Krueger, D.; Ott, M.J.; McCool, J.A.; Gardiner, P. Nurses’ experiences, expectations, and preferences for mind-body practices to reduce stress. BMC Complement. Altern. Med. 2011, 11, 26. [Google Scholar] [CrossRef] [PubMed]
- Sulenses, K.; Freitas, J.; Colgan, D.D. Underuse of yoga as a referral resource by health professions students. J. Altern. Complement. Med. 2015, 21, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Koinis, A.; Giannou, V.; Drantaki, V.; Angelaina, S.; Stratou, E.; Saridi, M. The Impact of Healthcare Workers Job Environment on Their Mental-emotional Health. Coping Strategies: The Case of a Local General Hospital. Health Psychol. Res. 2015, 3, 1984. [Google Scholar] [CrossRef] [PubMed]
- Portoghese, I.; Galletta, M.; Coppola, R.C.; Finco, G.; Campagna, M. Burnout and workload among health care workers: the moderating role of job control. Saf. Health Work 2014, 5, 152–157. [Google Scholar] [CrossRef] [PubMed]
- Ruotsalainen, J.H.; Verbeek, J.H.; Mariné, A.; Serra, C. Preventing occupational stress in healthcare workers. Cochrane Database Syst. Rev. 2015. [Google Scholar] [CrossRef] [PubMed]
- Awosan, K.J.; Yikawe, S.S.; Oche, O.M.; Oboirien, M. Prevalence, perception and correlates of low back pain among healthcare workers in tertiary health institutions in Sokoto, Nigeria. Ghana Med. J. 2017, 51, 164–174. [Google Scholar] [PubMed]
- Abdollahzade, F.; Mohammadi, F.; Dianat, I.; Asghari, E.; Asghari-Jafarabadi, M.; Sokhanvar, Z. Working posture and its predictors in hospital operating room nurses. Health Promot. Perspect. 2016, 6, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Soylar, P.; Ozer, A. Evaluation of the prevalence of musculoskeletal disorders in nurses: A systematic review. Med. Sci. 2018, 7, 479–485. [Google Scholar] [CrossRef]
- Memon, A.G.; Naeem, Z.; Zaman, A.; Zahid, F. Occupational health related concerns among surgeons. Int. J. Health Sci. 2016, 10, 279–291. [Google Scholar] [CrossRef]
- Gaowgzeh, R.A.; Chevidikunnan, M.F.; Al Saif, A.; El-Gendy, S.; Karrouf, G.; Al Senany, S. Prevalence of and risk factors for low back pain among dentists. J. Phys. Ther. Sci. 2015, 27, 2803–2806. [Google Scholar] [CrossRef] [PubMed]
- de Paiva, L.C.; Canário, A.C.G.; de Paiva China, E.L.C.; Gonçalves, A.K. Burnout syndrome in health-care professionals in a university hospital. Clinics 2017, 72, 305–309. [Google Scholar] [CrossRef] [PubMed]
- Freudenberger, H.J. Staff burn-out. J. Soc. Issues 1974, 30, 159–165. [Google Scholar] [CrossRef]
- Kumar, S. Burnout and Doctors: Prevalence, Prevention and Intervention. Healthcare 2016, 4, 37. [Google Scholar] [CrossRef] [PubMed]
- Maslach, C.; Schaufeli, W.B.; Leiter, M.P. Job Burnout. Annu. Rev. Psychol. 2001, 52, 397–422. [Google Scholar] [CrossRef] [PubMed]
- Maslach, C.; Jackson, S.E.; Leiter, M.P. Maslach Burnout Inventory Manual, 3rd ed.; Consulting Psychologist Press: Palo Alto, CA, USA, 1996. [Google Scholar]
- Salam, A.; Yousuf, R.; Bakar, S.M.A.; Haque, M. Stress among medical students in Malaysia: A systematic review of literatures. IMJ 2013, 20, 649–655. [Google Scholar]
- Iqbal, S.; Gupta, S.; Venkatarao, E. Stress, anxiety and depression among medical undergraduate students and their socio-demographic correlates. Indian J. Med. Res. 2015, 141, 354–357. [Google Scholar] [PubMed]
- Roberts, R.K.; Grubb, P.L. The consequences of nursing stress and need for integrated solutions. Rehabil. Nurs. 2013, 39, 62–69. [Google Scholar] [CrossRef] [PubMed]
- Büssing, A.; Michalsen, A.; Khalsa, S.B.S.; Telles, S.; Sherman, K.J. Effects of Yoga on Mental and Physical Health: A Short Summary of Reviews. Evid. Based Complement. Altern Med. 2012, 2012, 165410. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, S.; Mondal, S. Effect of regular yogic training on growth hormone and dehydroepiandrosterone sulfate as an endocrine marker of aging. Evid. Based Complement. Altern. Med. 2014, 2014, 240581. [Google Scholar] [CrossRef] [PubMed]
- Wolff, M.; Sundquist, K.; Larsson Lönn, S.; Midlöv, P. Impact of yoga on blood pressure and quality of life patients with hypertension—A controlled trial in primary care, matched for systolic blood pressure. BMC Cardiovasc. Disord. 2013, 13, 111. [Google Scholar] [CrossRef] [PubMed]
- Naik, D.; Thomas, N. Yoga- a potential solution for diabetes & metabolic syndrome. Indian J. Med. Res. 2015, 141, 753–756. [Google Scholar] [PubMed]
- Chou, C.C.; Huang, C.J. Effects of an 8-week yoga program on sustained attention and discrimination function in children with attention deficit hyperactivity disorder. PeerJ 2017, 5, e2883. [Google Scholar] [CrossRef] [PubMed]
- Akhtar, P.; Yardi, S.; Akhtar, M. Effects of yoga on functional capacity and well-being. Int. J. Yoga 2013, 6, 76–79. [Google Scholar] [CrossRef] [PubMed]
- Stonerock, G.L.; Hoffman, B.M.; Smith, P.J.; Blumenthal, J.A. Exercise as Treatment for Anxiety: Systematic Review and Analysis. Ann. Behav. Med. 2015, 49, 542–556. [Google Scholar] [CrossRef] [PubMed]
- Dwivedi, U.C.; Kumari, S.; Nagendra, H.R. Model of yoga intervention in industrial organizational psychology for counterproductive work behavior. Ind. Psychiatry J. 2015, 24, 119–124. [Google Scholar] [CrossRef] [PubMed]
- Ferri, P.; Guadi, M.; Marcheselli, L.; Balduzzi, S.; Magnani, D.; Di Lorenzo, R. The impact of shift work on the psychological and physical health of nurses in a general hospital: A comparison between rotating night shifts and day shifts. Risk Manag. Healthc. Policy 2016, 9, 203–211. [Google Scholar] [CrossRef] [PubMed]
- De Bruin, E.I.; Formsma, A.R.; Frijstein, G.; Bögels, S.M. Mindful2Work: Effects of Combined Physical Exercise, Yoga, and Mindfulness Meditations for Stress Relieve in Employees. A Proof of Concept Study. Mindfulness 2017, 8, 204. [Google Scholar] [CrossRef] [PubMed]
| Authors | Country | Year | Results | Jadad Score |
|---|---|---|---|---|
| Alexander et al. [5] | USA | 2015 | Yoga should be used to improve physical and mental health, to promote self-care and preventing burnout among nurses. Yoga intervention in this clinical trial lasted 8 weeks and was intended to develop self-reflection, self-care and self-discovery. Mind–body practices are useful in managing stress and building emotional resilience. To evaluate lifestyles, the authors used Health Promoting Lifestyle Profile II (HPLP-II); curiosity, acceptance and feasibility were evaluated with the Freiburg Mindfulness Inventory (FMI) while burnout was measured with the Maslach Burnout Inventory (MBI). | 1 |
| Bond et al. [1] | USA | 2013 | Medical students were evaluated for Jefferson’s Scale of Physician Empathy, Cohen’s Perceived Stress Scale, Self-Regulation Questionnaire and Self-Compassion Scale. The intervention consisted of an 11-week program of yoga and meditation and of a post-intervention evaluation. Statistically significant improvements in self-regulation and self-compassion of students were recorded. Changes in empathy and perceived stress were also recorded, although these values did not reach statistical significance. | 3 |
| Fang and Li [6] | China | 2015 | Yoga techniques were offered to nurses to improve sleep quality and reduce stress after work shifts. The group who received the intervention followed the yoga sessions twice a week (50/60 min per session) and demonstrated better sleep quality and reduced work stress. Yoga can improve back pain and quality of life. Sleep quality was evaluated using the Pittsburgh Quality Index (C-PSQI) while for work pressure, the authors used the Questionnaire on Medical Worker’s Stress (QMWS). | 5 |
| Klatt et al. [15] | USA | 2015 | This clinical trial was structured on an 8-week yoga program associated with a day-to-day work of 20 min of meditative awareness. The program was called MIM (Mindfulness In Motion) and consisted of a less time-invasive method to be administered in the work environment, based on meditation awareness, yoga stretching, relaxing music, and daily individual meditation practice. Resilience was measured with the Connor-Davidson Resiliency Scale (CD-RISC). The work commitment was evaluated through the Utrecht Work Engagement Scale (UWES). This study was designed for stressed workers, such as health care professionals of intensive care units. | 1 |
| Repar and Patton [7] | USA | 2007 | This Arts In Medicine (AIM) Program aimed to resolve compassion, fatigue, and chronic pain among nurses. Massages, poetry, listening to live music and visual arts, in combination, helped to improve the quality of life. | 1 |
| Riley et al. [19] | USA | 2017 | This large randomized clinical trial included two studies to compare the impact of Cognitive Behavioral Stress Management (CBSM) and Yoga-Based Stress Management (YBSM). Stress was associated with high levels of blood pressure, weight gain, anger, depression, anxiety, and reduced quality of life with worse health behaviors (diet, exercise, alcohol use). This trial, which included an 8-week yoga program, also focused on the consequences of stress, such as suicide and costs associated with tournaments and absenteeism. Among the questionnaires included in the study there were Depression, Anxiety and Stress Scale (DASS-21), SF12 and Self-Compassion Scale-Short Form (SCS). | 2 |
| Shirey [2] | USA | 2007 | The goal of this study was to investigate evidence-based solutions to reduce anger and stress. Consciousness-based interventions have shown a reduction in stress. The instrument used to evaluate empathy, considering mood changes, was the Interpersonal Reactivity Index (IRI). | 1 |
| Authors | Country | Year | Results | NOS |
|---|---|---|---|---|
| Chismark et al. [8] | USA | 2011 | This survey conducted on dental hygienists concerned the use of complementary medicine, including yoga and meditation to manage muscle-skeletal pain and obtain a better overall health and career satisfaction. | 8 |
| Kemper et al. [20] | USA | 2011 | This study reported the results of an online survey administered to nurses to evaluate their experience with meditation, prayer and mind–body practices. Expectations about the benefits of physical, emotional, mental and spiritual health and preferences on the type and structure of meditation training were also investigated. | 5 |
| Perez et al. [3] | USA | 2015 | The target population of this study was represented by palliative care clinicians. Factors of interest in the interviewed population were the challenges of managing a heavy workload (establishing skills and recognizing limitations); patient-related factors (patient management and case intensity); emotional and professional limits (limited resources, conflicting needs and expectations). | 5 |
| Sulenses et al. [21] | USA | 2015 | This survey was structured in 22 questions to evaluate the commitment to yoga practice, barriers to yoga practice, acceptability as additional treatment for physical and mental health and the characteristics of the participants. The aim was to demonstrate the under-utilization of yoga as a complementary alternative medicine resource (CAM). | 8 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cocchiara, R.A.; Peruzzo, M.; Mannocci, A.; Ottolenghi, L.; Villari, P.; Polimeni, A.; Guerra, F.; La Torre, G. The Use of Yoga to Manage Stress and Burnout in Healthcare Workers: A Systematic Review. J. Clin. Med. 2019, 8, 284. https://doi.org/10.3390/jcm8030284
Cocchiara RA, Peruzzo M, Mannocci A, Ottolenghi L, Villari P, Polimeni A, Guerra F, La Torre G. The Use of Yoga to Manage Stress and Burnout in Healthcare Workers: A Systematic Review. Journal of Clinical Medicine. 2019; 8(3):284. https://doi.org/10.3390/jcm8030284
Chicago/Turabian StyleCocchiara, Rosario Andrea, Margherita Peruzzo, Alice Mannocci, Livia Ottolenghi, Paolo Villari, Antonella Polimeni, Fabrizio Guerra, and Giuseppe La Torre. 2019. "The Use of Yoga to Manage Stress and Burnout in Healthcare Workers: A Systematic Review" Journal of Clinical Medicine 8, no. 3: 284. https://doi.org/10.3390/jcm8030284
APA StyleCocchiara, R. A., Peruzzo, M., Mannocci, A., Ottolenghi, L., Villari, P., Polimeni, A., Guerra, F., & La Torre, G. (2019). The Use of Yoga to Manage Stress and Burnout in Healthcare Workers: A Systematic Review. Journal of Clinical Medicine, 8(3), 284. https://doi.org/10.3390/jcm8030284








