A General Pathway Model for Improving Health Disparities: Lessons from Community and Cultural Involvement in Improving Cervical Cancer Screening in Vietnamese Women
Abstract
1. Introduction
2. Background
- a)
- What are the modifiable predisposing factors for these observations?
- b)
- What are the barriers, facilitators, feasibilities, and interventions with their success rates?
- c)
- Can these techniques be generalized to delivering other health messages to Vietnamese women, and possibly to other populations?
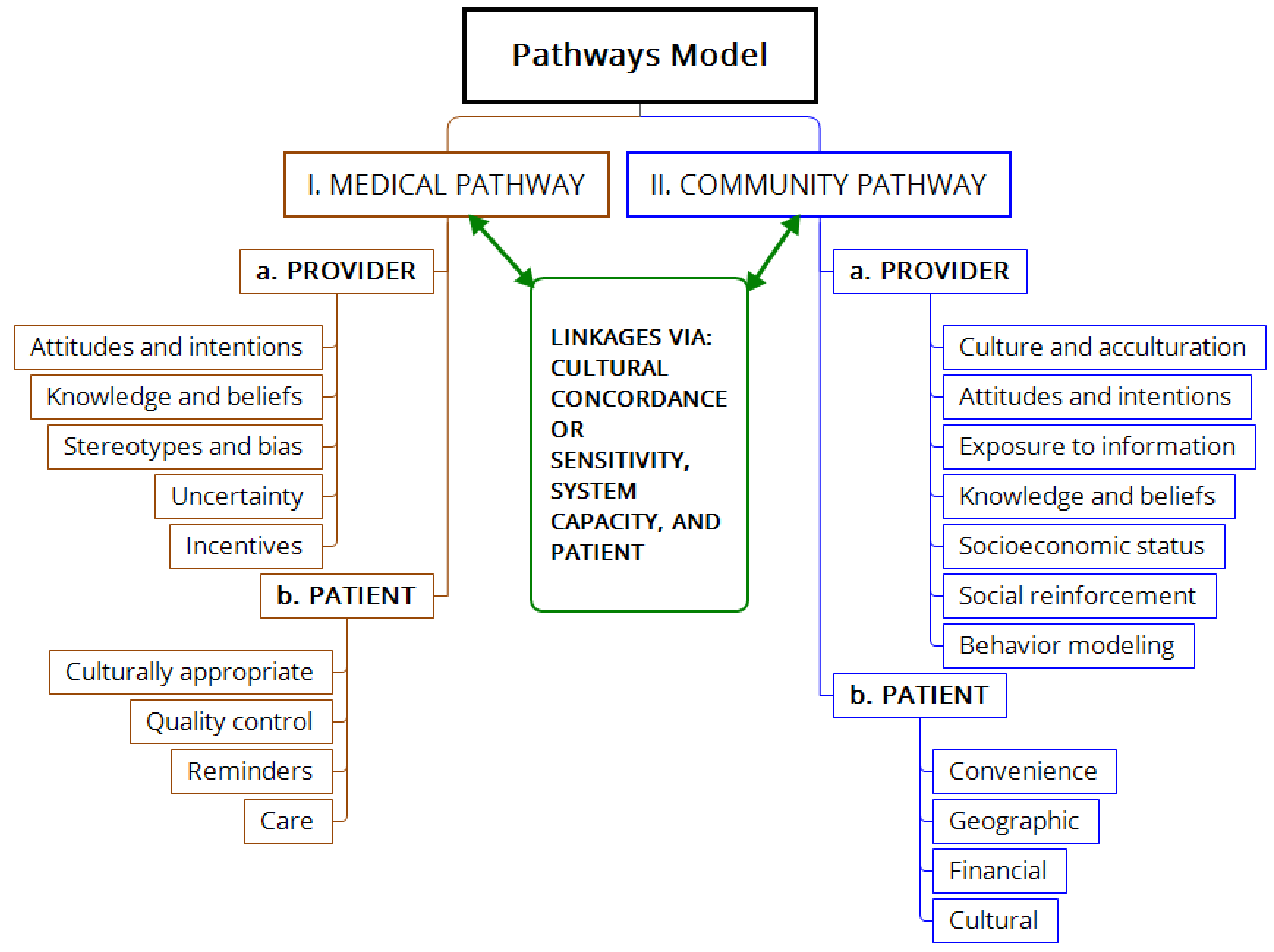
3. Genesis of a Community Action Plan based upon a Pathways Model
4. Components of the Program
5. Results of the Model
6. Discussion
7. Conclusions
- a)
- Predisposing factors contributing to the prevalence of low Pap tests initially included participant misinformation concerning the disease, testing, and effects upon outcomes, but also concerning cultural beliefs, awareness and attitudes, all of which were modifiable.
- b)
- Individual participants identified important perceived barriers listed in Table 2. Those assigned to the community were addressed by lay health workers, educational and nonmedical staff individually. One of the most important conduits of transformation was a bond formed by the staff that spoke Vietnamese and could relate with their culture.
- c)
- Techniques used in the pathway model can be used to deliver other health messages to Vietnamese women. However, specific data from each application, health delivery system, new population and location will be required in each instance.
Author Contributions
Conflicts of Interest
Compliance with Ethical Standards
References
- Kones, R.; Rumana, U. Cultural primer for cardiometabolic health. Health disparities, structural factors, community, and pathways to improvement. Postgrad. Med. 2018, 130, 200–221. [Google Scholar] [CrossRef] [PubMed]
- Heiman, H.J.; Artiga, S. Beyond Health Care: The Role of Social Determinants in Promoting Health and Health Equity; Kaiser Family Foundation: Menlo Park, CA, USA, 2015; Available online: http://www.kff.org/disparities-policy/issue-brief/beyond-health-care-the-role-of-social-determinants-in-promoting-health-and-health-equity/ (accessed on 1 January 2019).
- Wilkinson, R.; Marmot, M. (Eds.) Social Determinants of Health: The Solid Facts, 2nd ed.; International Centre for Health & Society; World Health Organization: Copenhagen, Denmark, 2003. [Google Scholar]
- 2016 National Healthcare Quality & Disparities Report; AHRQ Pub. No. 17-0001; Agency for Healthcare Research and Quality: Rockville, MD, USA, July 2017. Available online: https://www.ahrq.gov/research/findings/nhqrdr/nhqdr16/index.html (accessed on 1 January 2019).
- Kilbourne, A.M.; Switzer, G.; Hyman, K.; Crowley-Matoka, M.; Fine, M.J. Advancing Health Disparities Research Within the Health Care System: A Conceptual Framework. Am. J. Public Health 2006, 96, 2113–2121. [Google Scholar] [CrossRef] [PubMed]
- McGovern, L.; Miller, G.; Hugher-Cromwick, P. Health Policy Brief: The Relative Contribution of Multiple Determinants to Health Outcomes. Health Aff. 2014. Available online: http://www.healthaffairs.org/healthpolicybriefs/brief.php?brief_id=123 (accessed on 1 January 2019).
- World Health Organization. The World Health Report 2002: Reducing Risks, Promoting Healthy Life; World Health Organization: Geneva, Switzerland, 2002; Available online: www.who.int/whr/2002/en/ (accessed on 1 January 2019).
- Friel, S.; Marmot, M.G. Action on the social determinants of health and health inequities goes global. Annu. Rev. Public Health 2011, 32, 225–236. [Google Scholar] [CrossRef] [PubMed]
- Davis, R.S.; Savannah, S.; Harding, M.; Macaysa, A.; Parks, L. Countering the Production of Inequities: An Emerging Systems Framework to Achieve an Equitable Culture of Health; The Prevention Institute: Oakland, CA, USA, 2016; Available online: http://media.wix.com/ugd/b49d47_3c56f7659645462b8b8962299deb9bd9.pdf (accessed on 1 January 2019).
- Social Determinants of Health. Healthy People 2020; HealthyPeople.gov. Office of Disease Prevention and Health Promotion: Rockville, MD, USA, 2017. Available online: https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-of-health (accessed on 1 January 2019).
- Program Planning. Health People 2020; HealthyPeople.gov. Office of Disease Prevention and Health Promotion: Rockville, MD, USA, 2017. Available online: https://www.healthypeople.gov/2020/tools-and-resources/Program-Planning (accessed on 1 January 2019).
- Ahnquist, J.; Wamalal, S.; Lindstrom, M. Social determinants of health—A question of social or economic capital? Interaction effects of socioeconomic factors on health outcomes. Soc. Sci. Med. 2012, 74, 930–939. [Google Scholar] [CrossRef] [PubMed]
- Robert Wood Johnson Foundation (RWJF). How We Work Building a Culture of Health; RWJF: Princeton, NJ, USA, 2017; Available online: http://www.rwjf.org/en/how-we-work/building-a-culture-of-health.html (accessed on 1 January 2019).
- Chang, W.C.; Fraser, J.H. Cooperate! A paradigm shift for health equity. Int. J. Equity Health 2017, 16, 12. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine. The Future of the Public’s Health in the 21st Century; The National Academies Press: Washington, DC, USA, 2003; Available online: https://doi.org/10.17226/10548 (accessed on 1 January 2019).
- Schroeder, S.A. Shattuck Lecture. We can do better—Improving the health of the American people. N. Engl. J. Med. 2007, 357, 1221–1228. [Google Scholar] [CrossRef] [PubMed]
- Braveman, P.; Gottlieb, L. The Social Determinants of Health: It’s Time to Consider the Causes of the Causes. Public Health Rep. 2014, 129 (Suppl. 2), 19–31. [Google Scholar] [CrossRef]
- World Health Organization. A Conceptual Framework for Action on the Social Determinants of Health; WHO International: Geneva, Switzerland, 2010; Available online: www.who.int/sdhconference/resources/ConceptualframeworkforactiononSDH_eng.pdf (accessed on 1 January 2019).
- Thomas, S.B.; Quinn, S.C.; Butler, J.; Fryer, C.S.; Garza, M.A. Toward a fourth generation of disparities research to achieve health equity. Annu. Rev. Public Health 2011, 32, 399–416. [Google Scholar] [CrossRef]
- Wilson, L. Finding Answers: Disparities Research for Change Progress Report; Robert Wood Johnson Foundation: Princeton, NJ, USA, 2013; Available online: http://www.rwjf.org/en/library/research/2013/10/finding-answers--disparities-research-for-change.html (accessed on 1 January 2019).
- Cockerham, W.C.; Hamby, B.W.; Oates, G.R. The Social Determinants of Chronic Disease. Am. J. Prev. Med. 2017, 52 (Suppl. 1), S5–S12. [Google Scholar] [CrossRef]
- Taylor, L.A.; Tan, A.X.; Coyle, C.E.; Ndumele, C.; Rogan, E.; Canavan, M.; Curry, L.A.; Bradley, E.H. Leveraging the Social Determinants of Health: What Works? PLoS ONE 2016, 11, e0160217. [Google Scholar] [CrossRef]
- Scribner, R.A.; Simonsen, N.R.; Leonardi, C. The Social Determinants of Health Core: Taking a Place-Based Approach. Am. J. Prev. Med. 2017, 52 (Suppl. 1), S13–S19. [Google Scholar] [CrossRef] [PubMed]
- Healthy People 2020. Access to Health Services; U.S. Department of Health and Human Services: Washington, DC, USA, 2017. Available online: https://www.healthypeople.gov/2020/topics-objectives/topic/Access-to-Health-Services (accessed on 1 January 2019).
- Hassan, A.; Scherer, E.A.; Pikcilingis, A.; Krull, E.; McNickles, L.; Marmon, G.; Woods, E.R.; Fleegler, E.W. Improving Social Determinants of Health: Effectiveness of a Web-Based Intervention. Am. J. Prev. Med. 2015, 49, 822–831. [Google Scholar] [CrossRef] [PubMed]
- Smith, M.D.; Institute of Medicine (US). Committee on the Learning Health Care System in America. Best Care at Lower Cost: The Path to Continuously Learning Health Care in America; National Academies Press: Washington, DC, USA, 2013; Available online: https://www.nap.edu/catalog/13444/best-care-at-lower-cost-the-path-to-continuously-learning (accessed on 1 January 2019).
- Ayanian, J.Z.; Markel, H. Donabedian’s Lasting Framework for Health Care Quality. N. Engl. J. Med. 2016, 375, 205–207. [Google Scholar] [CrossRef]
- Robert Wood Johnson Foundation, Johns Hopkins Bloomberg School of Public Health. Chronic Care: Making the Case for Ongoing Care. 2010. Available online: https://www.rwjf.org/content/dam/farm/reports/reports/2010/rwjf54583 (accessed on 1 January 2019).
- Knapper, J.T.; Ghasemzadeh, N.; Khayata, M.; Patel, S.; Quyyumi, A.; Mendis, S.; Mensah, G.A.; Taubert, K.; Sperling, L. Time to Change Our Focus. Defining, Promoting, and Impacting Cardiovascular Population Health. J. Am. Coll. Cardiol. 2015, 66, 960–971. [Google Scholar] [CrossRef]
- Kones, R.; Rumana, U. Cardiometabolic diseases of civilization: History and maturation of an evolving global threat. An update and call for action. Ann. Med. 2017, 49, 260–274. [Google Scholar] [PubMed]
- Center for Advanced Research on Language Acquisition; University of Minnesota: Minneapolis, MN, USA, 2014; Available online: http://carla.umn.edu/culture/definitions.html (accessed on 1 January 2019).
- Verma, A.; Griffin, A.; Dacre, J.; Elder, A. Exploring cultural and linguistic influences on clinical communication skills: A qualitative study of International Medical Graduates. BMC Med. Educ. 2016, 16, 162. [Google Scholar] [CrossRef] [PubMed]
- Pew Research Center. Vietnamese Americans. 2013. Available online: http://www.pewsocialtrends.org/asianamericans-graphics/vietnamese/ (accessed on 1 January 2019).
- Mock, J.; McPhee, S.J.; Nguyen, T.; Wong, C.; Doan, H.; Lai, K.Q.; Nguyen, K.H.; Nguyen, T.T.; Bui-Tong, N. Effective lay health worker outreach and media-based education for promoting cervical cancer screening among Vietnamese American women. Am. J. Public Health 2007, 97, 1693–1700. [Google Scholar] [CrossRef]
- Taylor, V.M.; Schwartz, S.M.; Yasui, Y.; Burke, N.; Shu, J.; Lam, D.H.; Jackson, J.C. Pap testing among Vietnamese women: Health care system and physician factors. J. Community Health 2004, 29, 437–450. [Google Scholar] [CrossRef]
- Do, H.H.; Taylor, V.M.; Burke, N.; Yutaka, Y.; Schwartz, S.M.; Jackson, J.C. Knowledge about cervical cancer risk factors, traditional health beliefs, and Pap testing among Vietnamese American women. J. Immigr. Minor. Health 2007, 9, 109–114. [Google Scholar] [CrossRef]
- Nguyen, T.T.; McPhee, S.J.; Bui-Tong, N.; Luong, T.N.; Ha-Iaconis, T.; Nguyen, T.; Wong, C.; Lai, K.Q.; Lam, H. Community-based participatory research increases cervical cancer screening among Vietnamese-Americans. J. Health Care Poor Underserved 2006, 17, 31–54. [Google Scholar] [CrossRef]
- American Cancer Society (ACS). History of ACS Recommendations for the Early Detection of Cancer in People Without Symptoms. Available online: https://www.cancer.org/healthy/find-cancer-early/cancer-screening-guidelines/chronological-history-of-acs-recommendations.html (accessed on 1 January 2019).
- Houston, H.R. Health care and the silent language of Vietnamese immigrant consumers. Bus. Prof. Commun. Q. 2002, 65, 37. [Google Scholar] [CrossRef]
- Baciu, A.; Negussie, Y.; Geller, A.; Weinstein, J.N. (Eds.) Communities in Action: Pathways to Health Equity; National Academies of Sciences, Engineering, and Medicine, Health and Medicine Division, Committee on Community-Based Solutions to Promote Health Equity in the United States; National Academies Press: Washington, DC, USA, 2017; Available online: https://www.ncbi.nlm.nih.gov/books/n/nap24624/pdf/ (accessed on 1 January 2019).
- Centers for Disease Control and Prevention (CDC). CDC Community Health Improvement Navigator, 2015. Available online: http://www.cdc.gov/chinav/ (accessed on 1 January 2019).
- Centers for Disease Control and Prevention. The Community Guide. What Works to Promote Health. 2017. Available online: https://www.thecommunityguide.org/ (accessed on 1 January 2019).
- Community Tool Box. Chapter 1. Section 7. Working Together for Healthier Communities: A Framework for Collaboration among Community Partnership, Support Organizations, and Funders; Work Group for Community Health and Development, University of Kansa: Lawrence, KS, USA, 2016; Available online: http://ctb.ku.edu/en/table-of-contents/overview/model-for-community-change-and-improvement/framework-for-collaboration/main (accessed on 1 January 2019).
- Do, M. Predictors of cervical cancer screening among Vietnamese American women. J. Immigr. Minor. Health 2015, 17, 756–764. [Google Scholar] [CrossRef] [PubMed]
- Ma, G.X.; Fang, C.Y.; Feng, Z.; Tan, Y.; Gao, W.; Ge, S.; Nguyen, C. Correlates of Cervical Cancer Screening among Vietnamese-American Women. Infect. Dis. Obstet. Gynecol. 2012, 2012, 617234. [Google Scholar] [CrossRef] [PubMed]
- Taylor, V.M.; Jackson, J.C.; Yasui, Y.; Nguyen, T.T.; Woodall, E.; Acorda, E.; Li, L.; Ramsey, S. Evaluation of a cervical cancer control intervention using lay health workers for Vietnamese American women. Am. J. Public Health 2010, 100, 1924–1929. [Google Scholar] [CrossRef] [PubMed]
- National Cancer Institute. Research-tested Intervention Programs. Vietnamese Women’s Health Project. 2013. Available online: https://rtips.cancer.gov/rtips/programDetails.do?programId=1427816 (accessed on 28 January 2019).
- Scoggins, J.F.; Ramsey, S.D.; Jackson, J.C.; Taylor, V.M. Cost effectiveness of a program to promote screening for cervical cancer in the Vietnamese-American population. Asian Pac. J. Cancer Prev. 2010, 11, 717–722. [Google Scholar] [PubMed]
- Fr, C.E.; Nikpay, S.S.; Leslie, E.; Buntin, M.B. Evaluating Community-Based Health Improvement Programs. Health Aff. 2018, 37, 22–29. [Google Scholar] [CrossRef] [PubMed]
- Kones, R.; Rumana, U.; Merino, J. Exclusion of ‘nonRCT evidence’ in guidelines for chronic diseases—Is it always appropriate? The Look AHEAD study. Curr. Med. Res. Opin. 2014, 30, 2009–2019. [Google Scholar] [CrossRef]
| Period (years) | Test | Age Range(s) | Recommendation |
|---|---|---|---|
| 1987–2002 | Pap test | 18 and over or sexually active | Yearly, but after 3 consecutive normal exams, less frequently at the discretion of the doctor |
| 2003–2012 | Pap test | Start 3 years after first vaginal intercourse but no later than 21 | Yearly with conventional Pap test or every 2 years with liquid-based Pap test |
| 30 and over | After 3 normal results in a row, screening can be every 2 to 3 years. An alternative is a Pap test plus HPV DNA testing every 3 years. | ||
| 70 and over | After 3 normal Pap tests in a row within the past 10 years, women may choose to stop screening. |
| Barrier | % |
|---|---|
| Feeling well | 3.8 |
| No insurance | 5.5 |
| Not suggested by physician | 5.5 |
| High cost | 8.6 |
| Lack of time | 5.2 |
| Shame/embarrassment | 4.8 |
| Lack of knowledge | 3.5 |
| No physician | 3.5 |
| Did not know where to go | 2.8 |
| Physician not speaking Vietnamese | 1.4 |
| Uncertain insurance covered Pap | 1.4 |
| No female physician | 0.7 |
| Other | 2.1 |
| Barrier, as Defined by Patient | Pathway Chosen for Resolution |
|---|---|
| Poor physician recommendations | Medical |
| Cultural incompetence by physician, e.g., insensitivity | Medical |
| Lack of health insurance | Medical |
| Cost | Medical |
| Poor resources for follow-up treatment | Medical |
| Excessive paperwork load by staff, decreasing face-to-face time | Medical |
| Lack of knowledge within the community | Community |
| Social stigma of cancer as an STD | Community |
| Child, elder, or sick care during appointment time | Community |
| Concern about the diagnosis of cancer | Community |
| Directions and appointment for a Pap test | Both Medical and Community |
| Excessive patient paperwork | Both Medical and Community |
| Language barrier | Both Medical and Community |
| Transportation need | Both Medical and Community |
| Desire for female physician | Both Medical and Community |
| Excessive appointment waiting time | Both Medical and Community |
| Need for different appointment time frame (unstructured) | Both Medical and Community |
| Modesty and other special needs | Both Medical and Community |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kones, R.; Rumana, U.; Arain, F. A General Pathway Model for Improving Health Disparities: Lessons from Community and Cultural Involvement in Improving Cervical Cancer Screening in Vietnamese Women. J. Clin. Med. 2019, 8, 154. https://doi.org/10.3390/jcm8020154
Kones R, Rumana U, Arain F. A General Pathway Model for Improving Health Disparities: Lessons from Community and Cultural Involvement in Improving Cervical Cancer Screening in Vietnamese Women. Journal of Clinical Medicine. 2019; 8(2):154. https://doi.org/10.3390/jcm8020154
Chicago/Turabian StyleKones, Richard, Umme Rumana, and Fauzia Arain. 2019. "A General Pathway Model for Improving Health Disparities: Lessons from Community and Cultural Involvement in Improving Cervical Cancer Screening in Vietnamese Women" Journal of Clinical Medicine 8, no. 2: 154. https://doi.org/10.3390/jcm8020154
APA StyleKones, R., Rumana, U., & Arain, F. (2019). A General Pathway Model for Improving Health Disparities: Lessons from Community and Cultural Involvement in Improving Cervical Cancer Screening in Vietnamese Women. Journal of Clinical Medicine, 8(2), 154. https://doi.org/10.3390/jcm8020154





