Online Porn Addiction: What We Know and What We Don’t—A Systematic Review
Abstract
1. Introduction
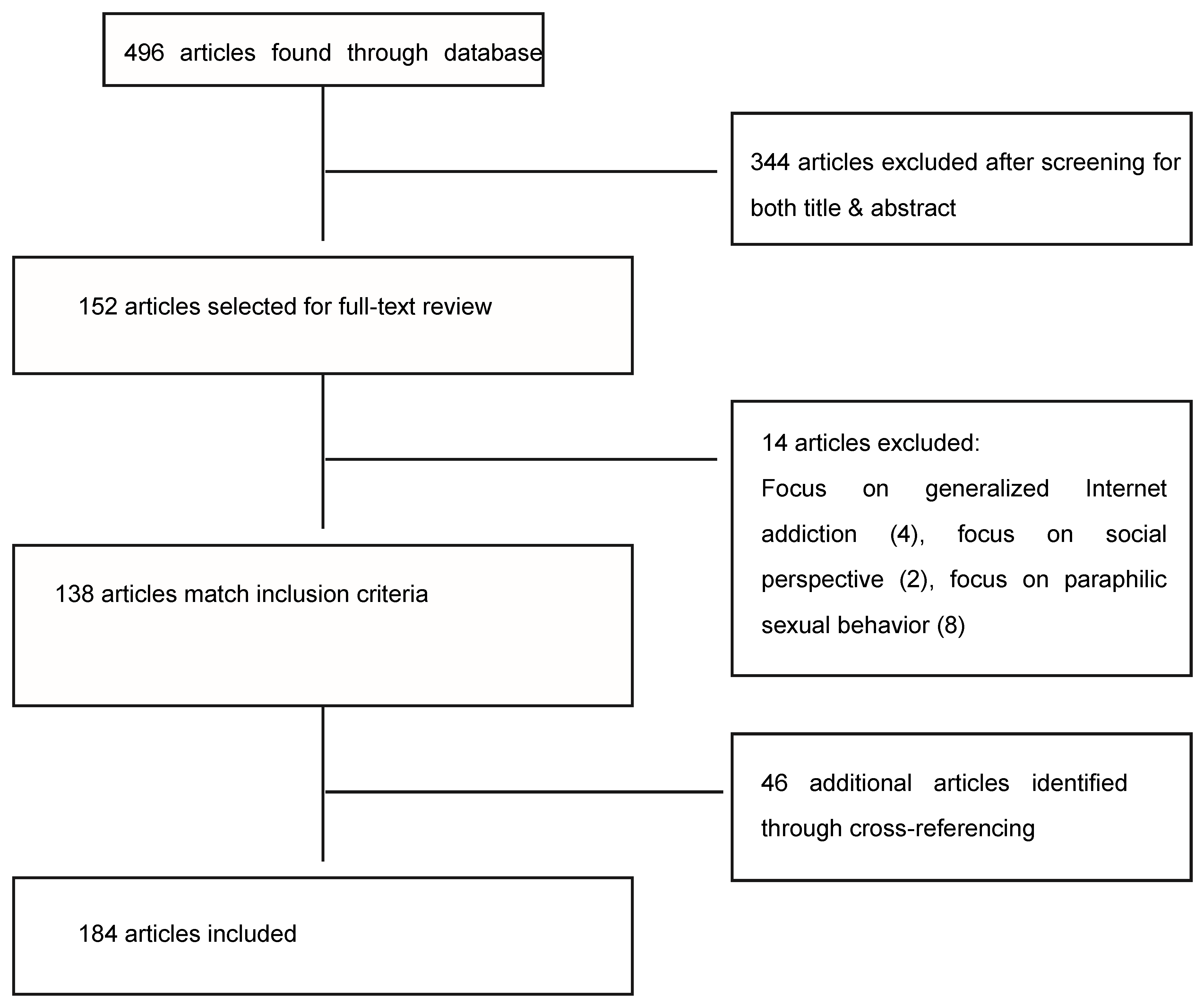
2. Methods
3. Results
3.1. Epidemiology
- (1)
- A study assessing behavioral addictions among substance users, found that only 9.80% out of 51 participants considered they had an addiction to sex or pornography [36].
- (2)
- A Swedish study that recruited a sample of 1913 participants through a web questionnaire, 7.6% reported some Internet sexual problem and 4.5% indicated feeling ‘addicted’ to Internet for love and sexual purposes, and that this was a ‘big problem’ [17].
- (3)
- A Spanish study with a sample of 1557 college students found that 8.6% was in a potential risk of developing a pathological usage of online pornography, but that the actual pathological user prevalence was 0.7% [37].
3.2. Ethiopathogenical and Diagnostic Conceptualization
3.3. Clinical Manifestations
- Erectile dysfunction: while some studies have found little evidence of the association between pornography use and sexual dysfunction [33], others propose that the rise in pornography use may be the key factor explaining the sharp rise in erectile dysfunction among young people [80]. In one study, 60% of patients who suffered sexual dysfunction with a real partner, characteristically did not have this problem with pornography [8]. Some argue that causation between pornography use and sexual dysfunction is difficult to establish, since true controls not exposed to pornography are rare to find [81] and have proposed a possible research design in this regard.
- Psychosexual dissatisfaction: pornography use has been associated with sexual dissatisfaction and sexual dysfunction, for both males and females [82], being more critical of one’s body or their partner’s, increased performance pressure and less actual sex [83], having more sexual partners and engaging in paid sex behavior [34]. This impact is especially noted in relationships when it is one sided [84], in a very similar way to marijuana use, sharing key factors like higher secrecy [85]. These studies are based on regular non-pathological pornography use, but online pornography may not have harmful effects by itself, only when it has become an addiction [24]. This can explain the relationship between the use of female-centric pornography and more positive outcomes for women [86].
- Comorbidities: hypersexual behavior has been associated with anxiety disorder, followed by mood disorder, substance use disorder and sexual dysfunction [87]. These findings also apply to POPU [88], also being associated with smoking, drinking alcohol or coffee, substance abuse [41] and problematic video-game use [89,90].
3.4. Neurobiological Evidence Supporting Addiction Model
3.5. Neuropsychological Evidence
3.6. Prognosis
3.7. Assessment Tools
3.8. Treatment
3.8.1. Pharmacological Approaches
3.8.2. Psychotherapeutic Approaches
4. Discussion
Funding
Conflicts of Interest
References
- American Psychiatry Association. Manual Diagnóstico y Estadístico de los Trastornos Mentales, 5th ed.; Panamericana: Madrid, España, 2014; pp. 585–589. ISBN 978-84-9835-810-0. [Google Scholar]
- Love, T.; Laier, C.; Brand, M.; Hatch, L.; Hajela, R. Neuroscience of Internet Pornography Addiction: A Review and Update. Behav. Sci. (Basel) 2015, 5, 388–433. [Google Scholar] [CrossRef] [PubMed]
- Elmquist, J.; Shorey, R.C.; Anderson, S.; Stuart, G.L. A preliminary investigation of the relationship between early maladaptive schemas and compulsive sexual behaviors in a substance-dependent population. J. Subst. Use 2016, 21, 349–354. [Google Scholar] [CrossRef] [PubMed]
- Chamberlain, S.R.; Lochner, C.; Stein, D.J.; Goudriaan, A.E.; van Holst, R.J.; Zohar, J.; Grant, J.E. Behavioural addiction-A rising tide? Eur. Neuropsychopharmacol. 2016, 26, 841–855. [Google Scholar] [CrossRef] [PubMed]
- Blum, K.; Badgaiyan, R.D.; Gold, M.S. Hypersexuality Addiction and Withdrawal: Phenomenology, Neurogenetics and Epigenetics. Cureus 2015, 7, e348. [Google Scholar] [CrossRef] [PubMed]
- Duffy, A.; Dawson, D.L.; Nair, R. das Pornography Addiction in Adults: A Systematic Review of Definitions and Reported Impact. J. Sex. Med. 2016, 13, 760–777. [Google Scholar] [CrossRef] [PubMed]
- Karila, L.; Wéry, A.; Weinstein, A.; Cottencin, O.; Petit, A.; Reynaud, M.; Billieux, J. Sexual addiction or hypersexual disorder: Different terms for the same problem? A review of the literature. Curr. Pharm. Des. 2014, 20, 4012–4020. [Google Scholar] [CrossRef] [PubMed]
- Voon, V.; Mole, T.B.; Banca, P.; Porter, L.; Morris, L.; Mitchell, S.; Lapa, T.R.; Karr, J.; Harrison, N.A.; Potenza, M.N.; et al. Neural correlates of sexual cue reactivity in individuals with and without compulsive sexual behaviours. PLoS ONE 2014, 9, e102419. [Google Scholar] [CrossRef]
- Wéry, A.; Billieux, J. Problematic cybersex: Conceptualization, assessment, and treatment. Addict. Behav. 2017, 64, 238–246. [Google Scholar] [CrossRef]
- Garcia, F.D.; Thibaut, F. Sexual addictions. Am. J. Drug Alcohol Abuse 2010, 36, 254–260. [Google Scholar] [CrossRef]
- Davis, R.A. A cognitive-behavioral model of pathological Internet use. Comput. Hum. Behav. 2001, 17, 187–195. [Google Scholar] [CrossRef]
- Ioannidis, K.; Treder, M.S.; Chamberlain, S.R.; Kiraly, F.; Redden, S.A.; Stein, D.J.; Lochner, C.; Grant, J.E. Problematic internet use as an age-related multifaceted problem: Evidence from a two-site survey. Addict. Behav. 2018, 81, 157–166. [Google Scholar] [CrossRef] [PubMed]
- Cooper, A.; Delmonico, D.L.; Griffin-Shelley, E.; Mathy, R.M. Online Sexual Activity: An Examination of Potentially Problematic Behaviors. Sex. Addict. Compuls. 2004, 11, 129–143. [Google Scholar] [CrossRef]
- Döring, N.M. The internet’s impact on sexuality: A critical review of 15 years of research. Comput. Hum. Behav. 2009, 25, 1089–1101. [Google Scholar] [CrossRef]
- Fisher, W.A.; Barak, A. Internet Pornography: A Social Psychological Perspective on Internet Sexuality. J. Sex. Res. 2001, 38, 312–323. [Google Scholar] [CrossRef]
- Janssen, E.; Carpenter, D.; Graham, C.A. Selecting films for sex research: Gender differences in erotic film preference. Arch. Sex. Behav. 2003, 32, 243–251. [Google Scholar] [CrossRef] [PubMed]
- Ross, M.W.; Månsson, S.-A.; Daneback, K. Prevalence, severity, and correlates of problematic sexual Internet use in Swedish men and women. Arch. Sex. Behav. 2012, 41, 459–466. [Google Scholar] [CrossRef] [PubMed]
- Riemersma, J.; Sytsma, M. A New Generation of Sexual Addiction. Sex. Addict. Compuls. 2013, 20, 306–322. [Google Scholar] [CrossRef]
- Beyens, I.; Eggermont, S. Prevalence and Predictors of Text-Based and Visually Explicit Cybersex among Adolescents. Young 2014, 22, 43–65. [Google Scholar] [CrossRef]
- Rosenberg, H.; Kraus, S. The relationship of “passionate attachment” for pornography with sexual compulsivity, frequency of use, and craving for pornography. Addict. Behav. 2014, 39, 1012–1017. [Google Scholar] [CrossRef]
- Keane, H. Technological change and sexual disorder. Addiction 2016, 111, 2108–2109. [Google Scholar] [CrossRef]
- Cooper, A. Sexuality and the Internet: Surfing into the New Millennium. CyberPsychol. Behav. 1998, 1, 187–193. [Google Scholar] [CrossRef]
- Cooper, A.; Scherer, C.R.; Boies, S.C.; Gordon, B.L. Sexuality on the Internet: From sexual exploration to pathological expression. Prof. Psychol. Res. Pract. 1999, 30, 154–164. [Google Scholar] [CrossRef]
- Harper, C.; Hodgins, D.C. Examining Correlates of Problematic Internet Pornography Use Among University Students. J. Behav. Addict. 2016, 5, 179–191. [Google Scholar] [CrossRef] [PubMed]
- Pornhub Insights: 2017 Year in Review. Available online: https://www.pornhub.com/insights/2017-year-in-review (accessed on 15 April 2018).
- Litras, A.; Latreille, S.; Temple-Smith, M. Dr Google, porn and friend-of-a-friend: Where are young men really getting their sexual health information? Sex. Health 2015, 12, 488–494. [Google Scholar] [CrossRef] [PubMed]
- Zimbardo, P.; Wilson, G.; Coulombe, N. How Porn Is Messing with Your Manhood. Available online: https://www.skeptic.com/reading_room/how-porn-is-messing-with-your-manhood/ (accessed on 25 March 2018).
- Pizzol, D.; Bertoldo, A.; Foresta, C. Adolescents and web porn: A new era of sexuality. Int. J. Adolesc. Med. Health 2016, 28, 169–173. [Google Scholar] [CrossRef] [PubMed]
- Prins, J.; Blanker, M.H.; Bohnen, A.M.; Thomas, S.; Bosch, J.L.H.R. Prevalence of erectile dysfunction: A systematic review of population-based studies. Int. J. Impot. Res. 2002, 14, 422–432. [Google Scholar] [CrossRef] [PubMed]
- Mialon, A.; Berchtold, A.; Michaud, P.-A.; Gmel, G.; Suris, J.-C. Sexual dysfunctions among young men: Prevalence and associated factors. J. Adolesc. Health 2012, 51, 25–31. [Google Scholar] [CrossRef]
- O’Sullivan, L.F.; Brotto, L.A.; Byers, E.S.; Majerovich, J.A.; Wuest, J.A. Prevalence and characteristics of sexual functioning among sexually experienced middle to late adolescents. J. Sex. Med. 2014, 11, 630–641. [Google Scholar] [CrossRef]
- Wilcox, S.L.; Redmond, S.; Hassan, A.M. Sexual functioning in military personnel: Preliminary estimates and predictors. J. Sex. Med. 2014, 11, 2537–2545. [Google Scholar] [CrossRef]
- Landripet, I.; Štulhofer, A. Is Pornography Use Associated with Sexual Difficulties and Dysfunctions among Younger Heterosexual Men? J. Sex. Med. 2015, 12, 1136–1139. [Google Scholar] [CrossRef]
- Wright, P.J. U.S. males and pornography, 1973–2010: Consumption, predictors, correlates. J. Sex. Res. 2013, 50, 60–71. [Google Scholar] [CrossRef] [PubMed]
- Price, J.; Patterson, R.; Regnerus, M.; Walley, J. How Much More XXX is Generation X Consuming? Evidence of Changing Attitudes and Behaviors Related to Pornography Since 1973. J. Sex Res. 2015, 53, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Najavits, L.; Lung, J.; Froias, A.; Paull, N.; Bailey, G. A study of multiple behavioral addictions in a substance abuse sample. Subst. Use Misuse 2014, 49, 479–484. [Google Scholar] [CrossRef] [PubMed]
- Ballester-Arnal, R.; Castro Calvo, J.; Gil-Llario, M.D.; Gil-Julia, B. Cybersex Addiction: A Study on Spanish College Students. J. Sex. Marital Ther. 2017, 43, 567–585. [Google Scholar] [CrossRef] [PubMed]
- Rissel, C.; Richters, J.; de Visser, R.O.; McKee, A.; Yeung, A.; Caruana, T. A Profile of Pornography Users in Australia: Findings From the Second Australian Study of Health and Relationships. J. Sex. Res. 2017, 54, 227–240. [Google Scholar] [CrossRef] [PubMed]
- Skegg, K.; Nada-Raja, S.; Dickson, N.; Paul, C. Perceived “Out of Control” Sexual Behavior in a Cohort of Young Adults from the Dunedin Multidisciplinary Health and Development Study. Arch. Sex. Behav. 2010, 39, 968–978. [Google Scholar] [CrossRef] [PubMed]
- Štulhofer, A.; Jurin, T.; Briken, P. Is High Sexual Desire a Facet of Male Hypersexuality? Results from an Online Study. J. Sex. Marital Ther. 2016, 42, 665–680. [Google Scholar] [CrossRef]
- Frangos, C.C.; Frangos, C.C.; Sotiropoulos, I. Problematic Internet Use among Greek university students: An ordinal logistic regression with risk factors of negative psychological beliefs, pornographic sites, and online games. Cyberpsychol. Behav. Soc. Netw. 2011, 14, 51–58. [Google Scholar] [CrossRef]
- Farré, J.M.; Fernández-Aranda, F.; Granero, R.; Aragay, N.; Mallorquí-Bague, N.; Ferrer, V.; More, A.; Bouman, W.P.; Arcelus, J.; Savvidou, L.G.; et al. Sex addiction and gambling disorder: Similarities and differences. Compr. Psychiatry 2015, 56, 59–68. [Google Scholar] [CrossRef]
- Kafka, M.P. Hypersexual disorder: A proposed diagnosis for DSM-V. Arch. Sex. Behav. 2010, 39, 377–400. [Google Scholar] [CrossRef]
- Kaplan, M.S.; Krueger, R.B. Diagnosis, assessment, and treatment of hypersexuality. J. Sex. Res. 2010, 47, 181–198. [Google Scholar] [CrossRef] [PubMed]
- Reid, R.C. Additional challenges and issues in classifying compulsive sexual behavior as an addiction. Addiction 2016, 111, 2111–2113. [Google Scholar] [CrossRef] [PubMed]
- Gola, M.; Lewczuk, K.; Skorko, M. What Matters: Quantity or Quality of Pornography Use? Psychological and Behavioral Factors of Seeking Treatment for Problematic Pornography Use. J. Sex. Med. 2016, 13, 815–824. [Google Scholar] [CrossRef] [PubMed]
- Reid, R.C.; Carpenter, B.N.; Hook, J.N.; Garos, S.; Manning, J.C.; Gilliland, R.; Cooper, E.B.; McKittrick, H.; Davtian, M.; Fong, T. Report of findings in a DSM-5 field trial for hypersexual disorder. J. Sex. Med. 2012, 9, 2868–2877. [Google Scholar] [CrossRef] [PubMed]
- Bancroft, J.; Vukadinovic, Z. Sexual addiction, sexual compulsivity, sexual impulsivity, or what? Toward a theoretical model. J. Sex. Res. 2004, 41, 225–234. [Google Scholar] [CrossRef]
- Bancroft, J. Sexual behavior that is “out of control”: A theoretical conceptual approach. Psychiatr. Clin. N. Am. 2008, 31, 593–601. [Google Scholar] [CrossRef]
- Stein, D.J.; Black, D.W.; Pienaar, W. Sexual disorders not otherwise specified: Compulsive, addictive, or impulsive? CNS Spectr. 2000, 5, 60–64. [Google Scholar] [CrossRef]
- Kafka, M.P.; Prentky, R.A. Compulsive sexual behavior characteristics. Am. J. Psychiatry 1997, 154, 1632. [Google Scholar] [CrossRef]
- Kafka, M.P. What happened to hypersexual disorder? Arch. Sex. Behav. 2014, 43, 1259–1261. [Google Scholar] [CrossRef]
- Krueger, R.B. Diagnosis of hypersexual or compulsive sexual behavior can be made using ICD-10 and DSM-5 despite rejection of this diagnosis by the American Psychiatric Association. Addiction 2016, 111, 2110–2111. [Google Scholar] [CrossRef]
- Reid, R.; Kafka, M. Controversies about Hypersexual Disorder and the DSM-5. Curr. Sex. Health Rep. 2014, 6, 259–264. [Google Scholar] [CrossRef]
- Kor, A.; Fogel, Y.; Reid, R.C.; Potenza, M.N. Should Hypersexual Disorder be Classified as an Addiction? Sex. Addict. Compuls. 2013, 20, 27–47. [Google Scholar] [CrossRef]
- Coleman, E. Is Your Patient Suffering from Compulsive Sexual Behavior? Psychiatr. Ann. 1992, 22, 320–325. [Google Scholar] [CrossRef]
- Coleman, E.; Raymond, N.; McBean, A. Assessment and treatment of compulsive sexual behavior. Minn. Med. 2003, 86, 42–47. [Google Scholar] [PubMed]
- Kafka, M.P.; Prentky, R. A comparative study of nonparaphilic sexual addictions and paraphilias in men. J. Clin. Psychiatry 1992, 53, 345–350. [Google Scholar] [PubMed]
- Derbyshire, K.L.; Grant, J.E. Compulsive sexual behavior: A review of the literature. J. Behav. Addict. 2015, 4, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Kafka, M.P.; Hennen, J. The paraphilia-related disorders: An empirical investigation of nonparaphilic hypersexuality disorders in outpatient males. J. Sex. Marital Ther. 1999, 25, 305–319. [Google Scholar] [CrossRef]
- Stein, D.J. Classifying hypersexual disorders: Compulsive, impulsive, and addictive models. Psychiatr. Clin. N. Am. 2008, 31, 587–591. [Google Scholar] [CrossRef]
- Lochner, C.; Stein, D.J. Does work on obsessive-compulsive spectrum disorders contribute to understanding the heterogeneity of obsessive-compulsive disorder? Prog. Neuropsychopharmacol. Biol. Psychiatry 2006, 30, 353–361. [Google Scholar] [CrossRef]
- Barth, R.J.; Kinder, B.N. The mislabeling of sexual impulsivity. J. Sex. Marital Ther. 1987, 13, 15–23. [Google Scholar] [CrossRef]
- Stein, D.J.; Chamberlain, S.R.; Fineberg, N. An A-B-C model of habit disorders: Hair-pulling, skin-picking, and other stereotypic conditions. CNS Spectr. 2006, 11, 824–827. [Google Scholar] [CrossRef] [PubMed]
- Goodman, A. Addictive Disorders: An Integrated Approach: Part One-An Integrated Understanding. J. Minist. Addict. Recover. 1995, 2, 33–76. [Google Scholar] [CrossRef]
- Carnes, P.J. Sexual addiction and compulsion: Recognition, treatment, and recovery. CNS Spectr. 2000, 5, 63–72. [Google Scholar] [CrossRef] [PubMed]
- Potenza, M.N. The neurobiology of pathological gambling and drug addiction: An overview and new findings. Philos. Trans. R. Soc. Lond. B Biol. Sci. 2008, 363, 3181–3189. [Google Scholar] [CrossRef] [PubMed]
- Orzack, M.H.; Ross, C.J. Should Virtual Sex Be Treated Like Other Sex Addictions? Sex. Addict. Compuls. 2000, 7, 113–125. [Google Scholar] [CrossRef]
- Zitzman, S.T.; Butler, M.H. Wives’ Experience of Husbands’ Pornography Use and Concomitant Deception as an Attachment Threat in the Adult Pair-Bond Relationship. Sex. Addict. Compuls. 2009, 16, 210–240. [Google Scholar] [CrossRef]
- Rosenberg, K.P.; O’Connor, S.; Carnes, P. Chapter 9—Sex Addiction: An Overview∗. In Behavioral Addictions; Rosenberg, K.P., Feder, L.C., Eds.; Academic Press: San Diego, CA, USA, 2014; pp. 215–236. ISBN 978-0-12-407724-9. [Google Scholar]
- Kraus, S.W.; Voon, V.; Kor, A.; Potenza, M.N. Searching for clarity in muddy water: Future considerations for classifying compulsive sexual behavior as an addiction. Addiction 2016, 111, 2113–2114. [Google Scholar] [CrossRef]
- Grant, J.E.; Chamberlain, S.R. Expanding the definition of addiction: DSM-5 vs. ICD-11. CNS Spectr. 2016, 21, 300–303. [Google Scholar] [CrossRef]
- Wéry, A.; Karila, L.; De Sutter, P.; Billieux, J. Conceptualisation, évaluation et traitement de la dépendance cybersexuelle: Une revue de la littérature. Can. Psychol. 2014, 55, 266–281. [Google Scholar] [CrossRef]
- Chaney, M.P.; Dew, B.J. Online Experiences of Sexually Compulsive Men Who Have Sex with Men. Sex. Addict. Compuls. 2003, 10, 259–274. [Google Scholar] [CrossRef]
- Schimmenti, A.; Caretti, V. Psychic retreats or psychic pits? Unbearable states of mind and technological addiction. Psychoanal. Psychol. 2010, 27, 115–132. [Google Scholar] [CrossRef]
- Griffiths, M.D. Internet sex addiction: A review of empirical research. Addict. Res. Theory 2012, 20, 111–124. [Google Scholar] [CrossRef]
- Navarro-Cremades, F.; Simonelli, C.; Montejo, A.L. Sexual disorders beyond DSM-5: The unfinished affaire. Curr. Opin. Psychiatry 2017, 30, 417–422. [Google Scholar] [CrossRef]
- Kraus, S.W.; Krueger, R.B.; Briken, P.; First, M.B.; Stein, D.J.; Kaplan, M.S.; Voon, V.; Abdo, C.H.N.; Grant, J.E.; Atalla, E.; et al. Compulsive sexual behaviour disorder in the ICD-11. World Psychiatry 2018, 17, 109–110. [Google Scholar] [CrossRef]
- Hyman, S.E.; Andrews, G.; Ayuso-Mateos, J.L.; Gaebel, W.; Goldberg, D.; Gureje, O.; Jablensky, A.; Khoury, B.; Lovell, A.; Medina Mora, M.E.; et al. A conceptual framework for the revision of the ICD-10 classification of mental and behavioural disorders. World Psychiatry 2011, 10, 86–92. [Google Scholar]
- Park, B.Y.; Wilson, G.; Berger, J.; Christman, M.; Reina, B.; Bishop, F.; Klam, W.P.; Doan, A.P. Is Internet Pornography Causing Sexual Dysfunctions? A Review with Clinical Reports. Behav. Sci. (Basel) 2016, 6, 17. [Google Scholar] [CrossRef] [PubMed]
- Wilson, G. Eliminate Chronic Internet Pornography Use to Reveal Its Effects. Addicta Turkish J. Addict. 2016, 3, 209–221. [Google Scholar] [CrossRef]
- Blais-Lecours, S.; Vaillancourt-Morel, M.-P.; Sabourin, S.; Godbout, N. Cyberpornography: Time Use, Perceived Addiction, Sexual Functioning, and Sexual Satisfaction. Cyberpsychol. Behav. Soc. Netw. 2016, 19, 649–655. [Google Scholar] [CrossRef] [PubMed]
- Albright, J.M. Sex in America online: An exploration of sex, marital status, and sexual identity in internet sex seeking and its impacts. J. Sex. Res. 2008, 45, 175–186. [Google Scholar] [CrossRef] [PubMed]
- Minarcik, J.; Wetterneck, C.T.; Short, M.B. The effects of sexually explicit material use on romantic relationship dynamics. J. Behav. Addict. 2016, 5, 700–707. [Google Scholar] [CrossRef]
- Pyle, T.M.; Bridges, A.J. Perceptions of relationship satisfaction and addictive behavior: Comparing pornography and marijuana use. J. Behav. Addict. 2012, 1, 171–179. [Google Scholar] [CrossRef] [PubMed]
- French, I.M.; Hamilton, L.D. Male-Centric and Female-Centric Pornography Consumption: Relationship With Sex Life and Attitudes in Young Adults. J. Sex. Marital Ther. 2018, 44, 73–86. [Google Scholar] [CrossRef] [PubMed]
- Starcevic, V.; Khazaal, Y. Relationships between Behavioural Addictions and Psychiatric Disorders: What Is Known and What Is Yet to Be Learned? Front. Psychiatry 2017, 8, 53. [Google Scholar] [CrossRef] [PubMed]
- Mitra, M.; Rath, P. Effect of internet on the psychosomatic health of adolescent school children in Rourkela—A cross-sectional study. Indian J. Child Health 2017, 4, 289–293. [Google Scholar]
- Voss, A.; Cash, H.; Hurdiss, S.; Bishop, F.; Klam, W.P.; Doan, A.P. Case Report: Internet Gaming Disorder Associated With Pornography Use. Yale J. Biol. Med. 2015, 88, 319–324. [Google Scholar]
- Stockdale, L.; Coyne, S.M. Video game addiction in emerging adulthood: Cross-sectional evidence of pathology in video game addicts as compared to matched healthy controls. J. Affect. Disord. 2018, 225, 265–272. [Google Scholar] [CrossRef]
- Grubbs, J.B.; Wilt, J.A.; Exline, J.J.; Pargament, K.I. Predicting pornography use over time: Does self-reported “addiction” matter? Addict. Behav. 2018, 82, 57–64. [Google Scholar] [CrossRef]
- Vilas, D.; Pont-Sunyer, C.; Tolosa, E. Impulse control disorders in Parkinson’s disease. Parkinsonism Relat. Disord. 2012, 18, S80–S84. [Google Scholar] [CrossRef]
- Poletti, M.; Bonuccelli, U. Impulse control disorders in Parkinson’s disease: The role of personality and cognitive status. J. Neurol. 2012, 259, 2269–2277. [Google Scholar] [CrossRef]
- Hilton, D.L. Pornography addiction—A supranormal stimulus considered in the context of neuroplasticity. Socioaffect. Neurosci. Psychol. 2013, 3, 20767. [Google Scholar] [CrossRef]
- Volkow, N.D.; Koob, G.F.; McLellan, A.T. Neurobiologic Advances from the Brain Disease Model of Addiction. N. Engl. J. Med. 2016, 374, 363–371. [Google Scholar] [CrossRef] [PubMed]
- Vanderschuren, L.J.M.J.; Pierce, R.C. Sensitization processes in drug addiction. Curr. Top. Behav. Neurosci. 2010, 3, 179–195. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.-J.; Fowler, J.S.; Tomasi, D.; Telang, F.; Baler, R. Addiction: Decreased reward sensitivity and increased expectation sensitivity conspire to overwhelm the brain’s control circuit. Bioessays 2010, 32, 748–755. [Google Scholar] [CrossRef]
- Goldstein, R.Z.; Volkow, N.D. Dysfunction of the prefrontal cortex in addiction: Neuroimaging findings and clinical implications. Nat. Rev. Neurosci. 2011, 12, 652–669. [Google Scholar] [CrossRef]
- Koob, G.F. Addiction is a Reward Deficit and Stress Surfeit Disorder. Front. Psychiatry 2013, 4, 72. [Google Scholar] [CrossRef] [PubMed]
- Mechelmans, D.J.; Irvine, M.; Banca, P.; Porter, L.; Mitchell, S.; Mole, T.B.; Lapa, T.R.; Harrison, N.A.; Potenza, M.N.; Voon, V. Enhanced attentional bias towards sexually explicit cues in individuals with and without compulsive sexual behaviours. PLoS ONE 2014, 9, e105476. [Google Scholar] [CrossRef] [PubMed]
- Seok, J.-W.; Sohn, J.-H. Neural Substrates of Sexual Desire in Individuals with Problematic Hypersexual Behavior. Front. Behav. Neurosci. 2015, 9, 321. [Google Scholar] [CrossRef] [PubMed]
- Hamann, S. Sex differences in the responses of the human amygdala. Neuroscientist 2005, 11, 288–293. [Google Scholar] [CrossRef]
- Klucken, T.; Wehrum-Osinsky, S.; Schweckendiek, J.; Kruse, O.; Stark, R. Altered Appetitive Conditioning and Neural Connectivity in Subjects with Compulsive Sexual Behavior. J. Sex. Med. 2016, 13, 627–636. [Google Scholar] [CrossRef]
- Sescousse, G.; Caldú, X.; Segura, B.; Dreher, J.-C. Processing of primary and secondary rewards: A quantitative meta-analysis and review of human functional neuroimaging studies. Neurosci. Biobehav. Rev. 2013, 37, 681–696. [Google Scholar] [CrossRef]
- Steele, V.R.; Staley, C.; Fong, T.; Prause, N. Sexual desire, not hypersexuality, is related to neurophysiological responses elicited by sexual images. Socioaffect. Neurosci. Psychol. 2013, 3, 20770. [Google Scholar] [CrossRef] [PubMed]
- Hilton, D.L. ‘High desire’, or ‘merely’ an addiction? A response to Steele et al. Socioaffect. Neurosci. Psychol. 2014, 4. [Google Scholar] [CrossRef] [PubMed]
- Prause, N.; Steele, V.R.; Staley, C.; Sabatinelli, D.; Hajcak, G. Modulation of late positive potentials by sexual images in problem users and controls inconsistent with “porn addiction”. Biol. Psychol. 2015, 109, 192–199. [Google Scholar] [CrossRef] [PubMed]
- Laier, C.; Pekal, J.; Brand, M. Cybersex addiction in heterosexual female users of internet pornography can be explained by gratification hypothesis. Cyberpsychol. Behav. Soc. Netw. 2014, 17, 505–511. [Google Scholar] [CrossRef] [PubMed]
- Laier, C.; Pekal, J.; Brand, M. Sexual Excitability and Dysfunctional Coping Determine Cybersex Addiction in Homosexual Males. Cyberpsychol. Behav. Soc. Netw. 2015, 18, 575–580. [Google Scholar] [CrossRef] [PubMed]
- Stark, R.; Klucken, T. Neuroscientific Approaches to (Online) Pornography Addiction. In Internet Addiction; Studies in Neuroscience, Psychology and Behavioral Economics; Springer: Cham, Switzerland, 2017; pp. 109–124. ISBN 978-3-319-46275-2. [Google Scholar]
- Albery, I.P.; Lowry, J.; Frings, D.; Johnson, H.L.; Hogan, C.; Moss, A.C. Exploring the Relationship between Sexual Compulsivity and Attentional Bias to Sex-Related Words in a Cohort of Sexually Active Individuals. Eur. Addict. Res. 2017, 23, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Kunaharan, S.; Halpin, S.; Sitharthan, T.; Bosshard, S.; Walla, P. Conscious and Non-Conscious Measures of Emotion: Do They Vary with Frequency of Pornography Use? Appl. Sci. 2017, 7, 493. [Google Scholar] [CrossRef]
- Kühn, S.; Gallinat, J. Brain Structure and Functional Connectivity Associated with Pornography Consumption: The Brain on Porn. JAMA Psychiatry 2014, 71, 827–834. [Google Scholar] [CrossRef]
- Banca, P.; Morris, L.S.; Mitchell, S.; Harrison, N.A.; Potenza, M.N.; Voon, V. Novelty, conditioning and attentional bias to sexual rewards. J. Psychiatr. Res. 2016, 72, 91–101. [Google Scholar] [CrossRef]
- Banca, P.; Harrison, N.A.; Voon, V. Compulsivity Across the Pathological Misuse of Drug and Non-Drug Rewards. Front. Behav. Neurosci. 2016, 10, 154. [Google Scholar] [CrossRef]
- Gola, M.; Wordecha, M.; Sescousse, G.; Lew-Starowicz, M.; Kossowski, B.; Wypych, M.; Makeig, S.; Potenza, M.N.; Marchewka, A. Can Pornography be Addictive? An fMRI Study of Men Seeking Treatment for Problematic Pornography Use. Neuropsychopharmacology 2017, 42, 2021–2031. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, C.; Morris, L.S.; Kvamme, T.L.; Hall, P.; Birchard, T.; Voon, V. Compulsive sexual behavior: Prefrontal and limbic volume and interactions. Hum. Brain Mapp. 2017, 38, 1182–1190. [Google Scholar] [CrossRef] [PubMed]
- Brand, M.; Snagowski, J.; Laier, C.; Maderwald, S. Ventral striatum activity when watching preferred pornographic pictures is correlated with symptoms of Internet pornography addiction. Neuroimage 2016, 129, 224–232. [Google Scholar] [CrossRef] [PubMed]
- Balodis, I.M.; Potenza, M.N. Anticipatory reward processing in addicted populations: A focus on the monetary incentive delay task. Biol. Psychiatry 2015, 77, 434–444. [Google Scholar] [CrossRef] [PubMed]
- Seok, J.-W.; Sohn, J.-H. Gray matter deficits and altered resting-state connectivity in the superior temporal gyrus among individuals with problematic hypersexual behavior. Brain Res. 2018, 1684, 30–39. [Google Scholar] [CrossRef] [PubMed]
- Taki, Y.; Kinomura, S.; Sato, K.; Goto, R.; Inoue, K.; Okada, K.; Ono, S.; Kawashima, R.; Fukuda, H. Both global gray matter volume and regional gray matter volume negatively correlate with lifetime alcohol intake in non-alcohol-dependent Japanese men: A volumetric analysis and a voxel-based morphometry. Alcohol. Clin. Exp. Res. 2006, 30, 1045–1050. [Google Scholar] [CrossRef] [PubMed]
- Chatzittofis, A.; Arver, S.; Öberg, K.; Hallberg, J.; Nordström, P.; Jokinen, J. HPA axis dysregulation in men with hypersexual disorder. Psychoneuroendocrinology 2016, 63, 247–253. [Google Scholar] [CrossRef]
- Jokinen, J.; Boström, A.E.; Chatzittofis, A.; Ciuculete, D.M.; Öberg, K.G.; Flanagan, J.N.; Arver, S.; Schiöth, H.B. Methylation of HPA axis related genes in men with hypersexual disorder. Psychoneuroendocrinology 2017, 80, 67–73. [Google Scholar] [CrossRef]
- Blum, K.; Werner, T.; Carnes, S.; Carnes, P.; Bowirrat, A.; Giordano, J.; Oscar-Berman, M.; Gold, M. Sex, drugs, and rock “n” roll: Hypothesizing common mesolimbic activation as a function of reward gene polymorphisms. J. Psychoact. Drugs 2012, 44, 38–55. [Google Scholar] [CrossRef]
- Jokinen, J.; Chatzittofis, A.; Nordstrom, P.; Arver, S. The role of neuroinflammation in the pathophysiology of hypersexual disorder. Psychoneuroendocrinology 2016, 71, 55. [Google Scholar] [CrossRef]
- Reid, R.C.; Karim, R.; McCrory, E.; Carpenter, B.N. Self-reported differences on measures of executive function and hypersexual behavior in a patient and community sample of men. Int. J. Neurosci. 2010, 120, 120–127. [Google Scholar] [CrossRef] [PubMed]
- Leppink, E.; Chamberlain, S.; Redden, S.; Grant, J. Problematic sexual behavior in young adults: Associations across clinical, behavioral, and neurocognitive variables. Psychiatry Res. 2016, 246, 230–235. [Google Scholar] [CrossRef] [PubMed]
- Kamaruddin, N.; Rahman, A.W.A.; Handiyani, D. Pornography Addiction Detection based on Neurophysiological Computational Approach. Indones. J. Electr. Eng. Comput. Sci. 2018, 10, 138–145. [Google Scholar] [CrossRef]
- Brand, M.; Laier, C.; Pawlikowski, M.; Schächtle, U.; Schöler, T.; Altstötter-Gleich, C. Watching pornographic pictures on the Internet: Role of sexual arousal ratings and psychological-psychiatric symptoms for using Internet sex sites excessively. Cyberpsychol. Behav. Soc. Netw. 2011, 14, 371–377. [Google Scholar] [CrossRef] [PubMed]
- Laier, C.; Schulte, F.P.; Brand, M. Pornographic picture processing interferes with working memory performance. J. Sex. Res. 2013, 50, 642–652. [Google Scholar] [CrossRef] [PubMed]
- Miner, M.H.; Raymond, N.; Mueller, B.A.; Lloyd, M.; Lim, K.O. Preliminary investigation of the impulsive and neuroanatomical characteristics of compulsive sexual behavior. Psychiatry Res. 2009, 174, 146–151. [Google Scholar] [CrossRef] [PubMed]
- Cheng, W.; Chiou, W.-B. Exposure to Sexual Stimuli Induces Greater Discounting Leading to Increased Involvement in Cyber Delinquency Among Men. Cyberpsychol. Behav. Soc. Netw. 2017, 21, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Messina, B.; Fuentes, D.; Tavares, H.; Abdo, C.H.N.; Scanavino, M.d.T. Executive Functioning of Sexually Compulsive and Non-Sexually Compulsive Men Before and After Watching an Erotic Video. J. Sex. Med. 2017, 14, 347–354. [Google Scholar] [CrossRef]
- Negash, S.; Sheppard, N.V.N.; Lambert, N.M.; Fincham, F.D. Trading Later Rewards for Current Pleasure: Pornography Consumption and Delay Discounting. J. Sex. Res. 2016, 53, 689–700. [Google Scholar] [CrossRef]
- Sirianni, J.M.; Vishwanath, A. Problematic Online Pornography Use: A Media Attendance Perspective. J. Sex. Res. 2016, 53, 21–34. [Google Scholar] [CrossRef]
- Laier, C.; Pawlikowski, M.; Pekal, J.; Schulte, F.P.; Brand, M. Cybersex addiction: Experienced sexual arousal when watching pornography and not real-life sexual contacts makes the difference. J. Behav. Addict. 2013, 2, 100–107. [Google Scholar] [CrossRef] [PubMed]
- Brand, M.; Young, K.S.; Laier, C. Prefrontal control and internet addiction: A theoretical model and review of neuropsychological and neuroimaging findings. Front. Hum. Neurosci. 2014, 8, 375. [Google Scholar] [CrossRef]
- Snagowski, J.; Wegmann, E.; Pekal, J.; Laier, C.; Brand, M. Implicit associations in cybersex addiction: Adaption of an Implicit Association Test with pornographic pictures. Addict. Behav. 2015, 49, 7–12. [Google Scholar] [CrossRef]
- Snagowski, J.; Laier, C.; Duka, T.; Brand, M. Subjective Craving for Pornography and Associative Learning Predict Tendencies Towards Cybersex Addiction in a Sample of Regular Cybersex Users. Sex. Addict. Compuls. 2016, 23, 342–360. [Google Scholar] [CrossRef]
- Walton, M.T.; Cantor, J.M.; Lykins, A.D. An Online Assessment of Personality, Psychological, and Sexuality Trait Variables Associated with Self-Reported Hypersexual Behavior. Arch. Sex. Behav. 2017, 46, 721–733. [Google Scholar] [CrossRef]
- Parsons, J.T.; Kelly, B.C.; Bimbi, D.S.; Muench, F.; Morgenstern, J. Accounting for the social triggers of sexual compulsivity. J. Addict. Dis. 2007, 26, 5–16. [Google Scholar] [CrossRef] [PubMed]
- Laier, C.; Brand, M. Mood changes after watching pornography on the Internet are linked to tendencies towards Internet-pornography-viewing disorder. Addict. Behav. Rep. 2017, 5, 9–13. [Google Scholar] [CrossRef]
- Laier, C.; Brand, M. Empirical Evidence and Theoretical Considerations on Factors Contributing to Cybersex Addiction from a Cognitive-Behavioral View. Sex. Addict. Compuls. 2014, 21, 305–321. [Google Scholar] [CrossRef]
- Antons, S.; Brand, M. Trait and state impulsivity in males with tendency towards Internet-pornography-use disorder. Addict. Behav. 2018, 79, 171–177. [Google Scholar] [CrossRef] [PubMed]
- Egan, V.; Parmar, R. Dirty habits? Online pornography use, personality, obsessionality, and compulsivity. J. Sex. Marital Ther. 2013, 39, 394–409. [Google Scholar] [CrossRef] [PubMed]
- Werner, M.; Štulhofer, A.; Waldorp, L.; Jurin, T. A Network Approach to Hypersexuality: Insights and Clinical Implications. J. Sex. Med. 2018, 15, 373–386. [Google Scholar] [CrossRef]
- Snagowski, J.; Brand, M. Symptoms of cybersex addiction can be linked to both approaching and avoiding pornographic stimuli: Results from an analog sample of regular cybersex users. Front. Psychol. 2015, 6, 653. [Google Scholar] [CrossRef]
- Schiebener, J.; Laier, C.; Brand, M. Getting stuck with pornography? Overuse or neglect of cybersex cues in a multitasking situation is related to symptoms of cybersex addiction. J. Behav. Addict. 2015, 4, 14–21. [Google Scholar] [CrossRef] [PubMed]
- Brem, M.J.; Shorey, R.C.; Anderson, S.; Stuart, G.L. Depression, anxiety, and compulsive sexual behaviour among men in residential treatment for substance use disorders: The role of experiential avoidance. Clin. Psychol. Psychother. 2017, 24, 1246–1253. [Google Scholar] [CrossRef] [PubMed]
- Carnes, P. Sexual addiction screening test. Tenn. Nurse 1991, 54, 29. [Google Scholar]
- Montgomery-Graham, S. Conceptualization and Assessment of Hypersexual Disorder: A Systematic Review of the Literature. Sex. Med. Rev. 2017, 5, 146–162. [Google Scholar] [CrossRef] [PubMed]
- Miner, M.H.; Coleman, E.; Center, B.A.; Ross, M.; Rosser, B.R.S. The compulsive sexual behavior inventory: Psychometric properties. Arch. Sex. Behav. 2007, 36, 579–587. [Google Scholar] [CrossRef] [PubMed]
- Miner, M.H.; Raymond, N.; Coleman, E.; Swinburne Romine, R. Investigating Clinically and Scientifically Useful Cut Points on the Compulsive Sexual Behavior Inventory. J. Sex. Med. 2017, 14, 715–720. [Google Scholar] [CrossRef]
- Öberg, K.G.; Hallberg, J.; Kaldo, V.; Dhejne, C.; Arver, S. Hypersexual Disorder According to the Hypersexual Disorder Screening Inventory in Help-Seeking Swedish Men and Women With Self-Identified Hypersexual Behavior. Sex. Med. 2017, 5, e229–e236. [Google Scholar] [CrossRef]
- Delmonico, D.; Miller, J. The Internet Sex Screening Test: A comparison of sexual compulsives versus non-sexual compulsives. Sex. Relatsh. Ther. 2003, 18, 261–276. [Google Scholar] [CrossRef]
- Ballester Arnal, R.; Gil Llario, M.D.; Gómez Martínez, S.; Gil Juliá, B. Psychometric properties of an instrument for assessing cyber-sex addiction. Psicothema 2010, 22, 1048–1053. [Google Scholar]
- Beutel, M.E.; Giralt, S.; Wölfling, K.; Stöbel-Richter, Y.; Subic-Wrana, C.; Reiner, I.; Tibubos, A.N.; Brähler, E. Prevalence and determinants of online-sex use in the German population. PLoS ONE 2017, 12, e0176449. [Google Scholar] [CrossRef] [PubMed]
- Kor, A.; Zilcha-Mano, S.; Fogel, Y.A.; Mikulincer, M.; Reid, R.C.; Potenza, M.N. Psychometric development of the Problematic Pornography Use Scale. Addict. Behav. 2014, 39, 861–868. [Google Scholar] [CrossRef] [PubMed]
- Wéry, A.; Burnay, J.; Karila, L.; Billieux, J. The Short French Internet Addiction Test Adapted to Online Sexual Activities: Validation and Links With Online Sexual Preferences and Addiction Symptoms. J. Sex. Res. 2016, 53, 701–710. [Google Scholar] [CrossRef] [PubMed]
- Grubbs, J.B.; Volk, F.; Exline, J.J.; Pargament, K.I. Internet pornography use: Perceived addiction, psychological distress, and the validation of a brief measure. J. Sex. Marital Ther. 2015, 41, 83–106. [Google Scholar] [CrossRef] [PubMed]
- Fernandez, D.P.; Tee, E.Y.J.; Fernandez, E.F. Do Cyber Pornography Use Inventory-9 Scores Reflect Actual Compulsivity in Internet Pornography Use? Exploring the Role of Abstinence Effort. Sex. Addict. Compuls. 2017, 24, 156–179. [Google Scholar] [CrossRef]
- Bőthe, B.; Tóth-Király, I.; Zsila, Á.; Griffiths, M.D.; Demetrovics, Z.; Orosz, G. The Development of the Problematic Pornography Consumption Scale (PPCS). J. Sex. Res. 2018, 55, 395–406. [Google Scholar] [CrossRef] [PubMed]
- Griffiths, M. A “Components” Model of Addiction within a Biopsychosocial Framework. J. Subst. Use 2009, 10, 191–197. [Google Scholar] [CrossRef]
- Reid, R.C.; Li, D.S.; Gilliland, R.; Stein, J.A.; Fong, T. Reliability, validity, and psychometric development of the pornography consumption inventory in a sample of hypersexual men. J. Sex. Marital Ther. 2011, 37, 359–385. [Google Scholar] [CrossRef]
- Baltieri, D.A.; Aguiar, A.S.J.; de Oliveira, V.H.; de Souza Gatti, A.L.; de Souza Aranha E Silva, R.A. Validation of the Pornography Consumption Inventory in a Sample of Male Brazilian University Students. J. Sex. Marital Ther. 2015, 41, 649–660. [Google Scholar] [CrossRef]
- Noor, S.W.; Simon Rosser, B.R.; Erickson, D.J. A Brief Scale to Measure Problematic Sexually Explicit Media Consumption: Psychometric Properties of the Compulsive Pornography Consumption (CPC) Scale among Men who have Sex with Men. Sex. Addict. Compuls. 2014, 21, 240–261. [Google Scholar] [CrossRef] [PubMed]
- Kraus, S.; Rosenberg, H. The pornography craving questionnaire: Psychometric properties. Arch. Sex. Behav. 2014, 43, 451–462. [Google Scholar] [CrossRef] [PubMed]
- Kraus, S.W.; Rosenberg, H.; Tompsett, C.J. Assessment of self-efficacy to employ self-initiated pornography use-reduction strategies. Addict. Behav. 2015, 40, 115–118. [Google Scholar] [CrossRef] [PubMed]
- Kraus, S.W.; Rosenberg, H.; Martino, S.; Nich, C.; Potenza, M.N. The development and initial evaluation of the Pornography-Use Avoidance Self-Efficacy Scale. J. Behav. Addict. 2017, 6, 354–363. [Google Scholar] [CrossRef] [PubMed]
- Sniewski, L.; Farvid, P.; Carter, P. The assessment and treatment of adult heterosexual men with self-perceived problematic pornography use: A review. Addict. Behav. 2018, 77, 217–224. [Google Scholar] [CrossRef] [PubMed]
- Gola, M.; Potenza, M.N. Paroxetine Treatment of Problematic Pornography Use: A Case Series. J. Behav. Addict. 2016, 5, 529–532. [Google Scholar] [CrossRef] [PubMed]
- Fong, T.W. Understanding and managing compulsive sexual behaviors. Psychiatry (Edgmont) 2006, 3, 51–58. [Google Scholar]
- Aboujaoude, E.; Salame, W.O. Naltrexone: A Pan-Addiction Treatment? CNS Drugs 2016, 30, 719–733. [Google Scholar] [CrossRef]
- Raymond, N.C.; Grant, J.E.; Coleman, E. Augmentation with naltrexone to treat compulsive sexual behavior: A case series. Ann. Clin. Psychiatry 2010, 22, 56–62. [Google Scholar]
- Kraus, S.W.; Meshberg-Cohen, S.; Martino, S.; Quinones, L.J.; Potenza, M.N. Treatment of Compulsive Pornography Use with Naltrexone: A Case Report. Am. J. Psychiatry 2015, 172, 1260–1261. [Google Scholar] [CrossRef]
- Bostwick, J.M.; Bucci, J.A. Internet sex addiction treated with naltrexone. Mayo Clin. Proc. 2008, 83, 226–230. [Google Scholar] [CrossRef]
- Camacho, M.; Moura, A.R.; Oliveira-Maia, A.J. Compulsive Sexual Behaviors Treated With Naltrexone Monotherapy. Prim. Care Companion CNS Disord. 2018, 20. [Google Scholar] [CrossRef] [PubMed]
- Capurso, N.A. Naltrexone for the treatment of comorbid tobacco and pornography addiction. Am. J. Addict. 2017, 26, 115–117. [Google Scholar] [CrossRef] [PubMed]
- Short, M.B.; Wetterneck, C.T.; Bistricky, S.L.; Shutter, T.; Chase, T.E. Clinicians’ Beliefs, Observations, and Treatment Effectiveness Regarding Clients’ Sexual Addiction and Internet Pornography Use. Commun. Ment. Health J. 2016, 52, 1070–1081. [Google Scholar] [CrossRef] [PubMed]
- Orzack, M.H.; Voluse, A.C.; Wolf, D.; Hennen, J. An ongoing study of group treatment for men involved in problematic Internet-enabled sexual behavior. Cyberpsychol. Behav. 2006, 9, 348–360. [Google Scholar] [CrossRef] [PubMed]
- Young, K.S. Cognitive behavior therapy with Internet addicts: Treatment outcomes and implications. Cyberpsychol. Behav. 2007, 10, 671–679. [Google Scholar] [CrossRef] [PubMed]
- Hardy, S.A.; Ruchty, J.; Hull, T.; Hyde, R. A Preliminary Study of an Online Psychoeducational Program for Hypersexuality. Sex. Addict. Compuls. 2010, 17, 247–269. [Google Scholar] [CrossRef]
- Crosby, J.M.; Twohig, M.P. Acceptance and Commitment Therapy for Problematic Internet Pornography Use: A Randomized Trial. Behav. Ther. 2016, 47, 355–366. [Google Scholar] [CrossRef]
- Twohig, M.P.; Crosby, J.M. Acceptance and commitment therapy as a treatment for problematic internet pornography viewing. Behav. Ther. 2010, 41, 285–295. [Google Scholar] [CrossRef]
| DSM-5 | ICD-11 | |
|---|---|---|
| Goal | Provide common research and clinical language for mental health problems | Reflect issues of clinical utility in a broad range of settings, global applicability, and scientific validity [79] |
| Conceptualization of hypersexual disorder | Addiction model | Impulse control model |
| Available diagnosis | No current hypersexual disorder diagnosis, due to insufficient evidence to categorize it as addiction | Compulsive sexual behavior disorder |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
de Alarcón, R.; de la Iglesia, J.I.; Casado, N.M.; Montejo, A.L. Online Porn Addiction: What We Know and What We Don’t—A Systematic Review. J. Clin. Med. 2019, 8, 91. https://doi.org/10.3390/jcm8010091
de Alarcón R, de la Iglesia JI, Casado NM, Montejo AL. Online Porn Addiction: What We Know and What We Don’t—A Systematic Review. Journal of Clinical Medicine. 2019; 8(1):91. https://doi.org/10.3390/jcm8010091
Chicago/Turabian Stylede Alarcón, Rubén, Javier I. de la Iglesia, Nerea M. Casado, and Angel L. Montejo. 2019. "Online Porn Addiction: What We Know and What We Don’t—A Systematic Review" Journal of Clinical Medicine 8, no. 1: 91. https://doi.org/10.3390/jcm8010091
APA Stylede Alarcón, R., de la Iglesia, J. I., Casado, N. M., & Montejo, A. L. (2019). Online Porn Addiction: What We Know and What We Don’t—A Systematic Review. Journal of Clinical Medicine, 8(1), 91. https://doi.org/10.3390/jcm8010091






