Use of Linagliptin for the Management of Medicine Department Inpatients with Type 2 Diabetes in Real-World Clinical Practice (Lina-Real-World Study)
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Hospital Antihyperglycemic Protocol
2.2. Study Outcomes
2.3. Statistical Analysis
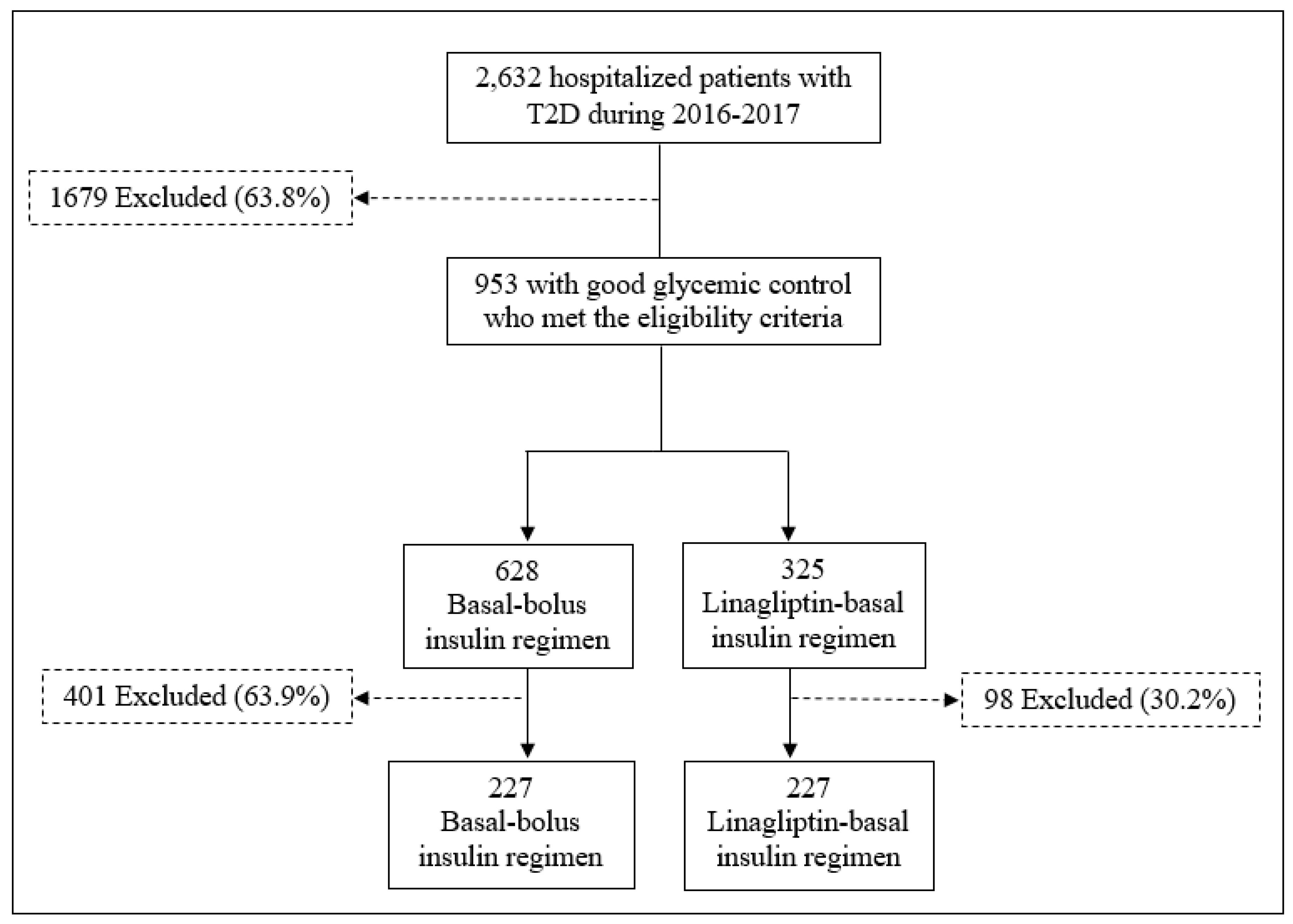
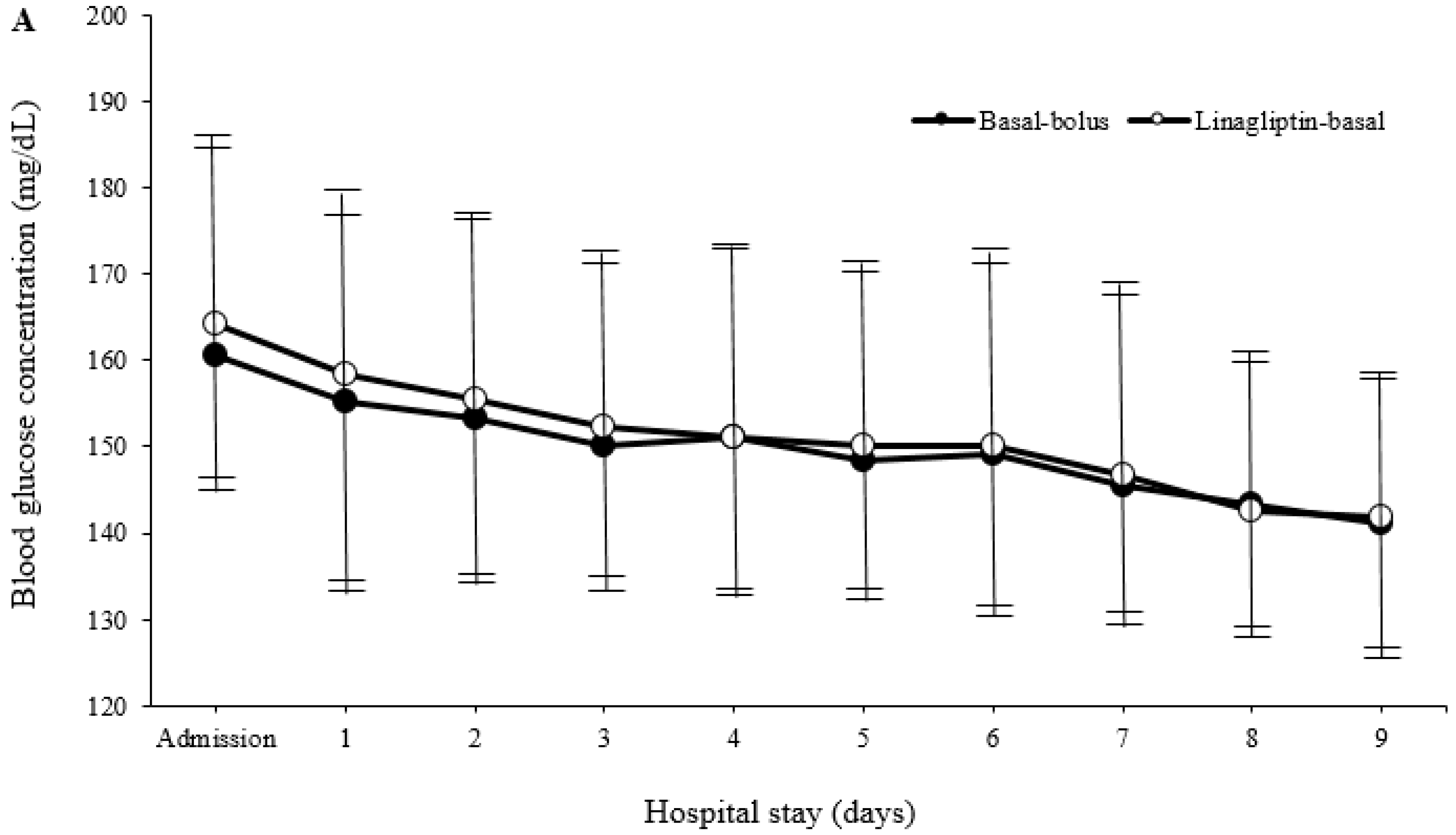
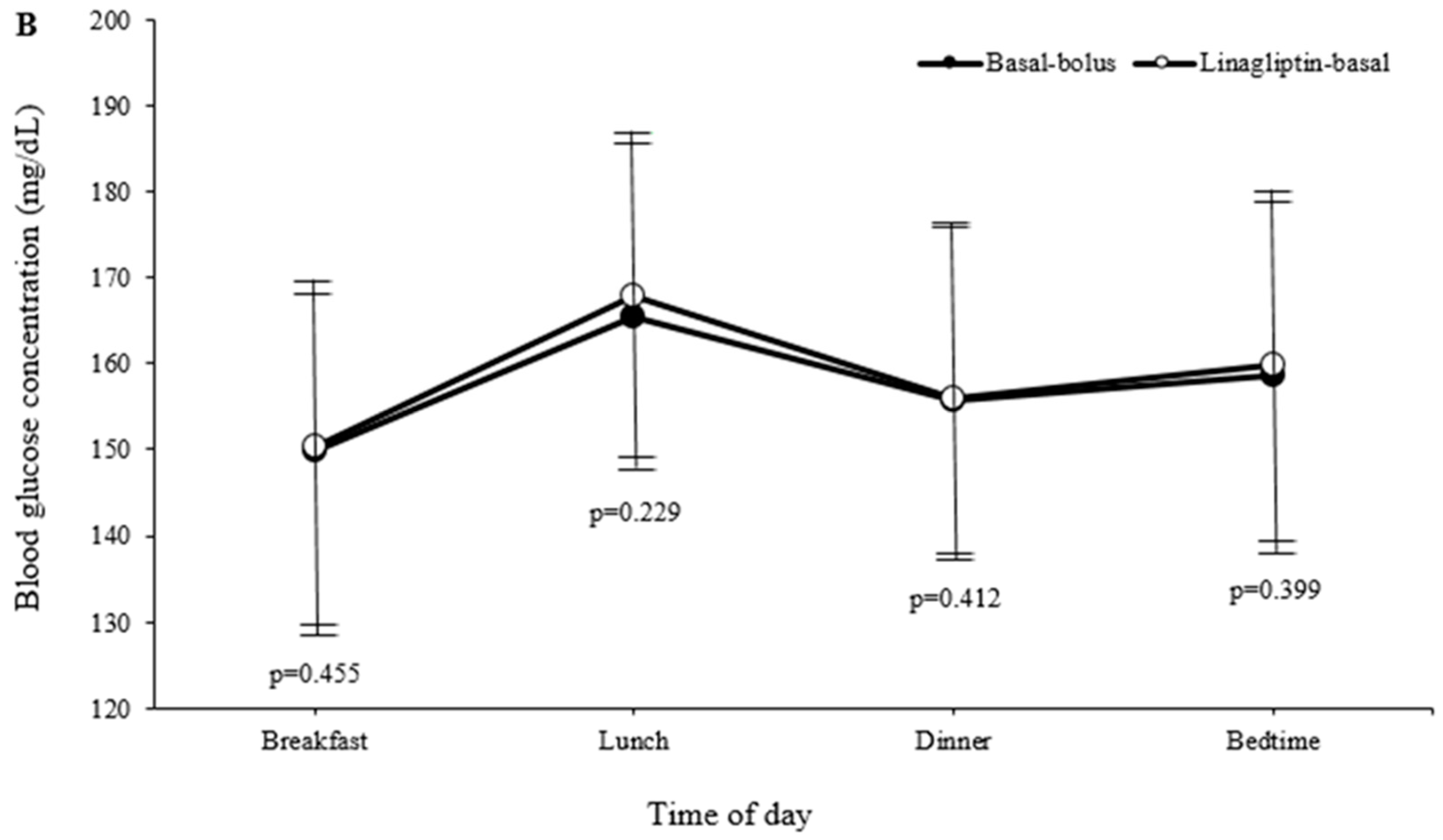
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Gregori, D.; Pagano, E.; Rosato, R.; Bo, S.; Zigon, G.; Merletti, F. Evaluating hospital costs in type 2 diabetes care: Does the choice of the model matter? Curr. Med. Res. Opin. 2006, 22, 1965–1971. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Belmonte, L.M.; Lara-Rojas, C.M.; López-Carmona, M.D.; Guijarro-Merino, R.; Bernal-López, M.R.; Gómez-Huelgas, R. National trends in heart failure hospitalization rates in patients with diabetes mellitus: 1997–2010. Rev. Esp. Cardiol. 2018, 71, 408–410. [Google Scholar] [CrossRef] [PubMed]
- Lara-Rojas, C.M.; Pérez-Belmonte, L.M.; López-Carmona, M.D.; Guijarro-Merino, R.; Bernal-López, M.R.; Gómez-Huelgas, R. National trends in diabetes mellitus hospitalization in Spain 1997–2010: Analysis of over 5.4 millions of admissions. Eur. J. Intern. Med. 2018, in press. [Google Scholar] [CrossRef] [PubMed]
- Sarwar, N.; Gao, P.; Seshasai, S.R.; Gobin, R.; Kaptoge, S.; Di Angelantonio, E.; Ingelsson, E.; Lawlor, D.A.; Selvin, E.; Stampfer, M.; et al. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: A collaborative meta-analysis of 102 prospective studies. Lancet 2010, 375, 2215–2222. [Google Scholar] [CrossRef] [PubMed]
- Moss, S.E.; Klein, R.; Klein, B.E. Risk factors for hospitalization in people with diabetes. Arch. Intern. Med. 1999, 159, 2053–2057. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, G.E.; Hellman, R.; Korytkowski, M.T.; Kosiborod, M.; Maynard, G.A.; Montori, V.M.; Seley, J.J.; Van den Berghe, G. Management of hyperglycemia in hospitalized patients in non-critical care setting: An endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 2012, 97, 16–38. [Google Scholar] [CrossRef] [PubMed]
- Inzucchi, S.E. Management of hyperglycemia in the hospital setting. N. Engl. J. Med. 2006, 355, 1903–1911. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. Diabetes Care in the Hospital: Standards of Medical Care in Diabetes—2018. Diabetes Care 2018, 41, S144–S151. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, G.E.; Smiley, D.; Zisman, A.; Prieto, L.M.; Palacio, A.; Ceron, M.; Puig, A.; Mejia, R. Randomized study of basal-bolus insulin therapy in the inpatient management of patients with type 2 diabetes (RABBIT 2 trial). Diabetes Care 2007, 30, 2181–2186. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, GE.; Smiley, D.; Jacobs, S.; Peng, L.; Temponi, A.; Mulligan, P.; Umpierrez, D.; Newton, C.; Olson, D.; Rizzo, M. Randomized study of basal-bolus insulin therapy in the inpatient management of patients with type 2 diabetes undergoing general surgery (RABBIT 2 surgery). Diabetes Care 2011, 34, 256–261. [Google Scholar] [CrossRef] [PubMed]
- Boucai, L.; Southern, W.N.; Zonszein, J. Hypoglycemia-associated mortality is not drug-associated but linked to comorbidities. Am. J. Med. 2011, 124, 1028–1035. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Huelgas, R.; López-Carmona, M.D.; Jansen-Chaparro, S.; Sobrino, B.; Chaves, M.; Martín-Gallardo, P.; García-Fernández, C.; Bernal-López, M.R. Assessment of an educational intervention in the management of non-critical inpatient glycemic control. Acta Diabetol. 2014, 51, 377–383. [Google Scholar] [CrossRef] [PubMed]
- Donner, T.W.; Flammer, K.M. Diabetes management in the hospital. Med. Clin. N. Am. 2008, 92, 407–425. [Google Scholar] [CrossRef] [PubMed]
- Moghissi, E.S.; Korytkowski, M.T.; DiNardo, M.; Einhorn, D.; Hellman, R.; Hirsch, I.B.; Inzucchi, S.E.; Ismail-Beigi, F.; Kirkman, M.S.; Umpierrez, G.E. American Association of Clinical Endocrinologists and American Diabetes Association consensus statement on inpatient glycemic control. Diabetes Care 2009, 32, 1119–1131. [Google Scholar] [CrossRef] [PubMed]
- Mendez, C.E.; Umpierrez, G.E. Pharmacotherapy for hyperglycemia in noncritically ill hospitalized patients. Diabetes Spectr. 2014, 27, 180–188. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, G.E.; Korytkowski, M. Is incretin based therapy ready for the care of hospitalized patients with type 2 diabetes?: Insulin therapy has proven itself and is considered the mainstay of treatment. Diabetes Care 2013, 36, 2112–2117. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, G.E.; Gianchandani, R.; Smiley, D.; Jacobs, S.; Wesorick, D.H.; Newton, C.; Farrokhi, F.; Peng, L.; Reyes, D.; Lathkar-Pradhan, S.; et al. Safety and efficacy of sitagliptin therapy for the inpatient management of general medicine and surgery patients with type 2 diabetes: A pilot, randomized, controlled study. Diabetes Care 2013, 36, 3430–3435. [Google Scholar] [CrossRef] [PubMed]
- Pasquel, F.J.; Gianchandani, R.; Rubin, D.J.; Dungan, K.M.; Anzola, I.; Gomez, P.C.; Peng, L.; Hodish, I.; Bodnar, T.; Wesorick, D.; et al. Efficacy of sitagliptin for the hospital management of general medicine and surgery patients with type 2 diabetes (Sita-Hospital): A multicentre, prospective, open-label, non-inferiority randomized trial. Lancet Diabetes Endocrinol. 2017, 5, 125–133. [Google Scholar] [CrossRef]
- Garg, R.; Schuman, B.; Hurwitz, S.; Metzger, C.; Bhandari, S. Safety and efficacy of saxagliptin for glycemic control in non-critically ill hospitalized patients. BMJ Open Diabetes Res. Care 2017, 5, e000394. [Google Scholar] [CrossRef] [PubMed]
- Radhakutty, A.; Stranks, J.L.; Mangelsdorf, B.L.; Drake, S.M.; Roberts, G.W.; Zimmermann, A.T.; Stranks, S.N.; Thompson, C.H.; Burt, M.G. Treatment of prednisolone-induced hyperglycaemia in hospitalized patients: Insights from a randomized, controlled study. Diabetes Obes. Metab. 2017, 19, 571–578. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, G.E.; Hor, T.; Smiley, D.; Temponi, A.; Umpierrez, D.; Ceron, M.; Munoz, C.; Newton, C.; Peng, L.; Baldwin, D. Comparison of impatient insulin regiments with determir plus aspart versus neutral protamine hagedorn plus regular in medical patients with type 2 diabetes. J. Clin. Endocrinol. Metab. 2009, 97, 564–569. [Google Scholar] [CrossRef] [PubMed]
- Pasquel, F.J.; Gomez-Huelgas, R.; Anzola, I.; Oyedokun, F.; Haw, J.S.; Vellanki, P.; Peng, L.; Umpierrez, G.E. Predictive value of admission hemoglobin A1c on inpatient glycemic control and response to insulin therapy in medicine and surgery patients with type 2 diabetes. Diabetes Care 2015, 38, 202–203. [Google Scholar] [CrossRef] [PubMed]
- Nauck, M.A.; Meier, J.J. Sitagliptin plus basal insulin: Simplifying in-hospital diabetes treatment? Lancet Diabetes Endocrinol. 2017, 5, 83–85. [Google Scholar] [CrossRef]
- Ena, J.; Gaviria, A.Z.; Romero-Sánchez, M.; Carretero-Gómez, J.; Carrasco-Sánchez, F.J.; Segura-Heras, J.V.; Porto-Perez, A.B.; Vázquez-Rodriguez, P.; González-Becerra, C.; Gómez-Huelgas, R. Derivation and validation model for hospital hypoglycemia. Eur. J. Intern. Med. 2018, 47, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Huelgas, R.; Guijarro-Merino, R.; Zapatero, A.; Barba, R.; Guijarro-Contreras, A.; Tinahones, F.; Bernal-López, R. The frequency and impact of hypoglycemia among hospitalized patients with diabetes: A population-based study. J. Diabetes Complicat. 2015, 29, 1050–1055. [Google Scholar] [CrossRef] [PubMed]
- Farrokhi, F.; Klindukhova, O.; Chandra, P.; Peng, L.; Smiley, D.; Newton, C.; Pasquel, F.; Fereira, M.E.; Umpierrez, G. Risk factors for inpatient hypoglycemia during subcutaneous insulin therapy in non-critically ill patients with type 2 diabetes. J. Diabetes Sci. Technol. 2012, 6, 1022–1029. [Google Scholar] [CrossRef] [PubMed]
- D’Ancona, G.; Bertuzzi, F.; Sacchi, L.; Pirone, F.; Stringi, V.; Arcadipane, A.; Bellazzi, R.; Pilato, M. Iatrogenic hypoglycemia secondary to tight glucose control is an independent determinant for mortality and cardiac morbidity. Eur. J. Cardiothorac. Surg. 2011, 40, 360–366. [Google Scholar] [CrossRef] [PubMed]
- Morales, J.; Assumpcao-Morales, M. The 2018 update of the American College of Physicians glycaemic management recommendations: An invitation to continued inertia? Diabetes Obes. Metab. 2018, 20, 1809–18011. [Google Scholar] [CrossRef] [PubMed]
- Garg, R.; Chaudhuri, A.; Munschauer, F.; Dandona, P. Hyperglycemia, insulin, and acute ischemic stroke: A mechanistic justification for a trial of insulin infusion therapy. Stroke 2006, 37, 267–273. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, G.E.; Schawartz, S. Use of incretin-based therapy in hospitalized patients with hyperglycemia. Endocr. Pract. 2014, 20, 933–944. [Google Scholar] [CrossRef] [PubMed]
- Deacon, C.F.; Holst, J.J. Linagliptin, a xanthine-based dipeptidyl peptidase-4 inhibitor with an unusual profile for the treatment of type 2 diabetes. Expert Opin. Investig. Drugs 2010, 19, 133–140. [Google Scholar] [CrossRef] [PubMed]
| Blood Glucose Concentration | Option A (TDI < 40 U/d or BW < 60 kg) | Option B (TDI 40–80 U/d or BW 60–90 kg) | Option C (TDI > 80 U/d or BW > 90 kg) |
|---|---|---|---|
| <80 mg/dL | −1 | −1 | −2 |
| 80–129 mg/dL | 0 | 0 | 0 |
| 130–149 mg/dL | 0 | 1 | 1 |
| 150–199 mg/dL | 1 | 1 | 2 |
| 200–249 mg/dL | 2 | 3 | 4 |
| 250–299 mg/dL | 3 | 5 | 7 |
| 300–349 mg/dL | 4 | 7 | 10 |
| >349 mg/dL | 5 | 8 | 12 |
| Pre-Propensity Matching | Post-Propensity Matching | |||||||
|---|---|---|---|---|---|---|---|---|
| Basal-Bolus (n = 628) | Linagliptin-Basal (n = 325) | Standardized Difference | p-Value | Basal-Bolus (n = 227) | Linagliptin-Basal (n = 227) | Standardized Difference | p-Value | |
| Age (years) | 70.2 ± 7.3 | 75.1 ± 9.2 | 0.160 | 0.022 | 71.5 ± 8.1 | 72.9 ± 8.3 | 0.024 | 0.074 |
| Male gender | 311 (49.5%) | 146 (44.9%) | 0.084 | 0.102 | 112 (49.3%) | 103 (45.4%) | 0.016 | 0.226 |
| Caucasic ethnic origin | 604 (96.2%) | 305 (93.8%) | 0.021 | 0.213 | 218 (96%) | 213 (93.8%) | 0.014 | 0.254 |
| Bodyweight (kg) | 92.3 ± 9.4 | 86.6 ± 8.2 | 0.122 | 0.031 | 89 ± 8.3 | 88.6 ± 9.5 | 0.006 | 0.108 |
| Body Mass Index (kg/m2) | 29.9 ± 1.8 | 28.4 ± 2.1 | 0.097 | 0.039 | 29.3 ± 1.6 | 29 ± 2.1 | 0.002 | 0.079 |
| Body Mass Index ≥30 | 264 (42%) | 116 (35.7%) | 0.178 | 0.028 | 84 (37%) | 82 (36.1%) | 0.002 | 0.487 |
| Abdominal circumference (cm) | 99.8 ± 8.8 | 95.1 ± 8.2 | 0.122 | 0.041 | 95.8 ± 8.3 | 96.4 ± 9.2 | 0.002 | 0.448 |
| Home diabetes treatment | 0.302 | 0.018 | 0.021 | 0.220 | ||||
| Diet alone | 12 (1.9%) | 13 (4.0%) | 4 (1.8%) | 6 (2.6%) | ||||
| Monotherapy | 288 (45.9%) | 193 (59.4%) | 118 (51.9%) | 128 (56.4%) | ||||
| Combination of oral antidiabetic drugs | 328 (52.2%) | 119 (36.6%) | 105 (46.3%) | 93 (41%) | ||||
| Diabetes duration (years) | 8.3 ± 3.2 | 9.1 ± 3.6 | 0.023 | 0.069 | 8.4 ± 3.2 | 8.9 ± 3.5 | 0.003 | 0.087 |
| Admission glycated haemoglobin (%) | 7.2 ± 0.6 | 7.6 ± 0.7 | 0.026 | 0.101 | 7.1 ± 0.6 | 7.2 ± 0.6 | 0.001 | 0.105 |
| Admission blood glucose concentration (mg/dL) | 158.3 ± 20.3 | 165.6 ± 24.9 | 0.111 | 0.042 | 160.5 ± 21.6 | 164.1 ± 24.7 | 0.002 | 0.098 |
| History of smoking | 356 (56.7%) | 201 (61.3%) | 0.189 | 0.030 | 134 (59%) | 137 (60.4%) | 0.010 | 0.424 |
| History of alcohol abuse | 283 (45.1%) | 110 (33.8%) | 0.231 | 0.029 | 92 (40.5%) | 80 (35.4%) | 0.019 | 0.246 |
| Hypertension | 410 (65.2%) | 203 (62.4%) | 0.081 | 0.206 | 146 (64.3%) | 143 (63%) | 0.004 | 0.423 |
| Dyslipidaemia | 383 (61.0%) | 217 (66.7%) | 0.075 | 0.165 | 142 (62.6%) | 149 (65.6%) | 0.005 | 0.279 |
| Chronic kidney disease | 176 (28.0%) | 52 (16.0%) | 0.336 | 0.027 | 46 (20.3%) | 44 (19.4%) | 0.002 | 0.453 |
| Cerebrovascular disease | 94 (15.0%) | 26 (8.0%) | 0.329 | 0.039 | 26 (11.5%) | 18 (7.9%) | 0.029 | 0.133 |
| Chronic obstructive pulmonary disease | 267 (42.5%) | 123 (37.8%) | 0.113 | 0.041 | 91 (40.1%) | 88 (38.8%) | 0.012 | 0.424 |
| Atrial fibrillation | 208 (33.1%) | 52 (16.0%) | 0.342 | 0.033 | 61 (26.9%) | 42 (18.5%) | 0.031 | 0.067 |
| Ischemic heart disease | 189 (30.1%) | 137 (42.2%) | 0.301 | 0.017 | 73 (32.2%) | 92 (40.5%) | 0.022 | 0.079 |
| Heart failure | 414 (65.9%) | 238 (73.2%) | 0.191 | 0.024 | 153 (67.4%) | 163 (71.8%) | 0.014 | 0.179 |
| Admission principal diagnosis | 0.189 | 0.036 | 0.017 | 0.141 | ||||
| Cardiovascular | 330 (52.5%) | 202 (62.2%) | 124 (54.6%) | 140 (61.7%) | ||||
| Infectious | 148 (23.6%) | 67 (20.6%) | 53 (23.3%) | 49 (21.6%) | ||||
| Pulmonary | 90 (14.3%) | 38 (11.7%) | 30 (13.2%) | 27 (11.9%) | ||||
| Neurologic | 44 (7.1%) | 13 (4.0%) | 12 (5.3%) | 10 (4.4%) | ||||
| Other | 16 (2.5%) | 5 (1.5%) | 8 (3.5%) | 1 (0.04%) | ||||
| Length of hospital stay (days) | 6.6 ± 1.8 | 7.1 ± 1.8 | 0.032 | 0.186 | 6.7 ± 1.9 | 6.9 ± 1.7 | 0.003 | 0.134 |
| Pre-Propensity Matching | Post-Propensity Matching | |||||||
|---|---|---|---|---|---|---|---|---|
| Basal-Bolus (n = 628) | Linagliptin-Basal (n = 325) | Standardized Difference | p-Value | Basal-Bolus (n = 227) | Linagliptin-Basal (n = 227) | Standardized Difference | p-Value | |
| Blood glucose concentration after admission (mg/dL) | 145.6 ± 12.2 | 158.6 ± 14.7 | 0.122 | 0.036 | 149.8 ± 13.5 | 151.2 ± 14.3 | 0.011 | 0.177 |
| Patients with mean blood glucose reading 100–140 mg/dL | 79 (12.6%) | 52 (16.0%) | 0.134 | 0.044 | 31 (13.7%) | 35 (15.4%) | 0.017 | 0.201 |
| Patients with mean blood glucose reading >200 mg/dL | 35 (5.6%) | 36 (11.1%) | 0.156 | 0.035 | 14 (6.2%) | 24 (10.6%) | 0.021 | 0.090 |
| Number of treatment failures | 110 (17.5%) | 72 (22.2%) | 0.131 | 0.040 | 43 (18.9%) | 47 (20.7%) | 0.011 | 0.362 |
| Day of treatment failure | 2.4 ± 1.2 | 2.0 ± 1.1 | 0.099 | 0.444 | 2.3 ± 1.1 | 2.1 ± 1.3 | 0.009 | 0.411 |
| Total insulin dose (Units per day) | 32.2 ± 5.5 | 22.7 ± 7.3 | 0.304 | <0.001 | 30.4 ± 5.4 | 24.6 ± 7.9 | 0.298 | <0.001 |
| Total basal insulin (Units per day) | 17.4 ± 2.7 | 14.7 ± 2.6 | 0.087 | 0.252 | 15.3 ± 2.7 | 15.6 ± 2.7 | 0.003 | 0.768 |
| Total prandial rapid-acting insulin (Units per day) | 9.6 ± 2.8 | - | - | - | 9.2 ± 2.6 | - | - | - |
| Total supplemental rapid-acting insulin (Units per day) | 5.2 ± 1.1 | 7.0 ± 1.8 | 0.139 | 0.038 | 5.9 ± 1.1 | 6.8 ± 1.7 | 0.012 | 0.126 |
| Number of injections per day during hospital stay | 4.0 ± 0.0 | 2.6 ± 0.8 | 0.309 | <0.001 | 4.0 ± 0.0 | 2.7 ± 0.8 | 0.301 | <0.001 |
| Patients with any blood glucose reading <70 mg/dL | 72 (11.5%) | 22 (6.8%) | 0.239 | 0.029 | 21 (9.3%) | 16 (7%) | 0.018 | 0.247 |
| Patients with any blood glucose reading <54 mg/dL | 22 (3.5%) | 7 (2.2%) | 0.137 | 0.043 | 7 (3.1%) | 5 (2.2%) | 0.013 | 0.199 |
| Patients with any blood glucose reading <40 mg/dL | 7 (1.1%) | 0 | 0.202 | 0.041 | 2 (0.09%) | 0 | 0.011 | 0.249 |
| Total number of hospital complications | 107 (17.0%) | 41 (12.6%) | 0.177 | 0.039 | 36 (15.9%) | 29 (12.8%) | 0.01 | 0.106 |
| Infection | 18 | 12 | 0.129 | 0.044 | 7 | 6 | 0.004 | 0.577 |
| Acute respiratory failure | 19 | 12 | 0.138 | 0.043 | 7 | 7 | 0.002 | 0.601 |
| Acute kidney failure | 32 | 14 | 0.248 | 0.038 | 13 | 9 | 0.014 | 0.201 |
| Acute coronary event | 6 | 0 | 0.211 | 0.036 | 3 | 0 | 0.011 | 0.103 |
| Bleeding | 6 | 3 | 0.188 | 0.041 | 2 | 2 | 0.002 | 0.613 |
| Thromboembolism | 5 | 3 | 0.176 | 0.044 | 2 | 2 | 0.002 | 0.622 |
| Other | 6 | 4 | 0.125 | 0.044 | 2 | 3 | 0.004 | 0.598 |
| Requiring admission to an intensive care unit | 23 | 7 | 0.284 | 0.036 | 8 | 3 | 0.014 | 0.107 |
| Hospital deaths | 11 | 7 | 0.138 | 0.042 | 3 | 2 | 0.004 | 0.315 |
| Pre-Propensity Matching (n = 108) | Post-Propensity Matching (n = 71) | |
|---|---|---|
| Age (years) | 76.2 ± 9.3 | 74.4 ± 8.4 |
| Male gender | 71 (65.7%) | 47 (66.2%) |
| Caucasic ethnic origin | 101 (93.5%) | 65 (91.5%) |
| Bodyweight (kg) | 89.2 ± 8.7 | 90.8 ± 9.7 |
| Body Mass Index (kg/m2) | 29.1 ± 2.0 | 29.5 ± 2.1 |
| Body Mass Index ≥30 | 55 (50.9%) | 39 (54.9%) |
| Abdominal circumference (cm) | 98.1 ± 9.3 | 99.0 ± 11.7 |
| Home diabetes treatment | ||
| Diet alone | 0 | 0 |
| Monotherapy | 46 (42.6%) | 29 (40.8%) |
| Combination of oral antidiabetic drugs | 62 (57.4%) | 42 (59.2%) |
| Diabetes duration (years) | 9.2 ± 3.7 | 8.9 ± 2.5 |
| Admission glycated haemoglobin (%) | 7.7 ± 0.7 | 7.5 ± 0.5 |
| Admission blood glucose concentration (mg/dL) | 178.5 ± 20.8 | 173.7 ± 18.9 |
| History of smoking | 59 (54.6%) | 39 (54.9%) |
| History of alcohol abuse | 36 (33.3%) | 25 (35.1%) |
| Hypertension | 75 (69.4%) | 50 (70.4%) |
| Dyslipidaemia | 71 (65.7%) | 47 (66.2%) |
| Chronic kidney disease | 15 (13.9%) | 9 (12.7%) |
| Cerebrovascular disease | 10 (9.3%) | 7 (9.9%) |
| Chronic obstructive pulmonary disease | 49 (45.4%) | 34 (47.9%) |
| Atrial fibrillation | 27 (25.0%) | 15 (21.1%) |
| Ischemic heart disease | 49 (45.4%) | 33 (46.5%) |
| Heart failure | 84 (77.8%) | 57 (80.3%) |
| Admission principal diagnosis | ||
| Cardiovascular | 81 (75.0%) | 54 (76.1%) |
| Infectious | 18 (16.7%) | 11 (15.5%) |
| Pulmonary | 7 (6.4%) | 5 (7.0%) |
| Neurologic | 2 (1.9%) | 1 (1.4%) |
| Other | 0 | 0 |
| Length of hospital stay (days) | 7.0 ± 1.4 | 7.1 ± 1.4 |
| Blood glucose concentration after admission (mg/dL) | 186.7 ± 14.2 | 183.4 ± 13.1 |
| Patients with any blood glucose reading <70 mg/dL | 10 (9.3%) | 6 (8.5%) |
| Patients with any blood glucose reading <54 mg/dL | 4 (3.7%) | 2 (2.8%) |
| Patients with any blood glucose reading <40 mg/dL | 0 | 0 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pérez-Belmonte, L.M.; Gómez-Doblas, J.J.; Millán-Gómez, M.; López-Carmona, M.D.; Guijarro-Merino, R.; Carrasco-Chinchilla, F.; De Teresa-Galván, E.; Jiménez-Navarro, M.; Bernal-López, M.R.; Gómez-Huelgas, R. Use of Linagliptin for the Management of Medicine Department Inpatients with Type 2 Diabetes in Real-World Clinical Practice (Lina-Real-World Study). J. Clin. Med. 2018, 7, 271. https://doi.org/10.3390/jcm7090271
Pérez-Belmonte LM, Gómez-Doblas JJ, Millán-Gómez M, López-Carmona MD, Guijarro-Merino R, Carrasco-Chinchilla F, De Teresa-Galván E, Jiménez-Navarro M, Bernal-López MR, Gómez-Huelgas R. Use of Linagliptin for the Management of Medicine Department Inpatients with Type 2 Diabetes in Real-World Clinical Practice (Lina-Real-World Study). Journal of Clinical Medicine. 2018; 7(9):271. https://doi.org/10.3390/jcm7090271
Chicago/Turabian StylePérez-Belmonte, Luis M., Juan J. Gómez-Doblas, Mercedes Millán-Gómez, María D. López-Carmona, Ricardo Guijarro-Merino, Fernando Carrasco-Chinchilla, Eduardo De Teresa-Galván, Manuel Jiménez-Navarro, M. Rosa Bernal-López, and Ricardo Gómez-Huelgas. 2018. "Use of Linagliptin for the Management of Medicine Department Inpatients with Type 2 Diabetes in Real-World Clinical Practice (Lina-Real-World Study)" Journal of Clinical Medicine 7, no. 9: 271. https://doi.org/10.3390/jcm7090271
APA StylePérez-Belmonte, L. M., Gómez-Doblas, J. J., Millán-Gómez, M., López-Carmona, M. D., Guijarro-Merino, R., Carrasco-Chinchilla, F., De Teresa-Galván, E., Jiménez-Navarro, M., Bernal-López, M. R., & Gómez-Huelgas, R. (2018). Use of Linagliptin for the Management of Medicine Department Inpatients with Type 2 Diabetes in Real-World Clinical Practice (Lina-Real-World Study). Journal of Clinical Medicine, 7(9), 271. https://doi.org/10.3390/jcm7090271






