The Therapeutic Effects of Traditional Chinese Medicine for Poor Semen Quality in Infertile Males
Abstract
1. Introduction
2. Materials and Methods
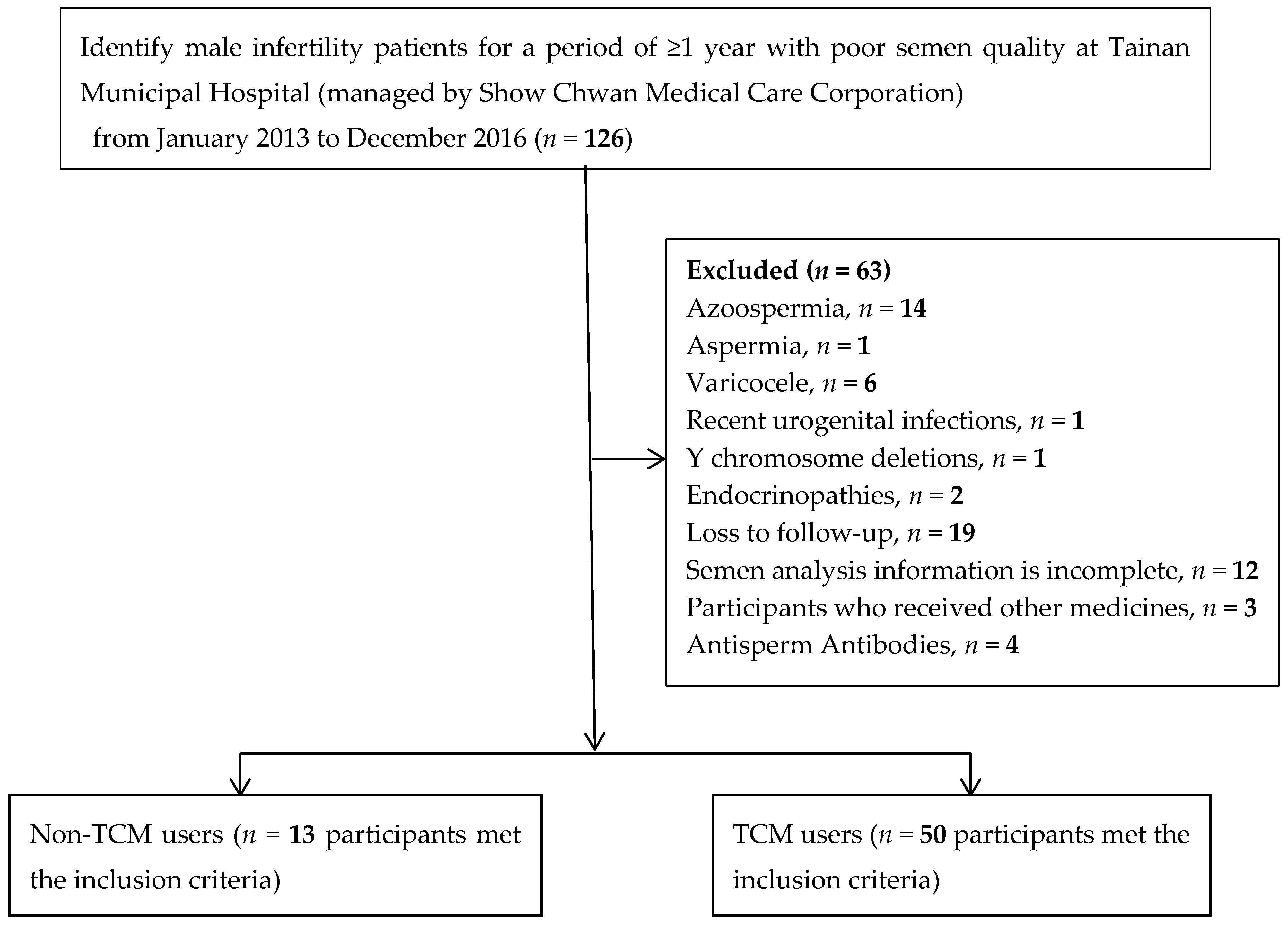
2.1. Data Source and Study Design
2.2. Semen Analysis
2.3. Statistical Analysis
2.4. Ethics
3. Results
4. Discussion
4.1. Summary of Evidence
4.2. Mechanism of Traditional Chinese Herbs for the Treatment of Poor Semen Quality in Male Infertility
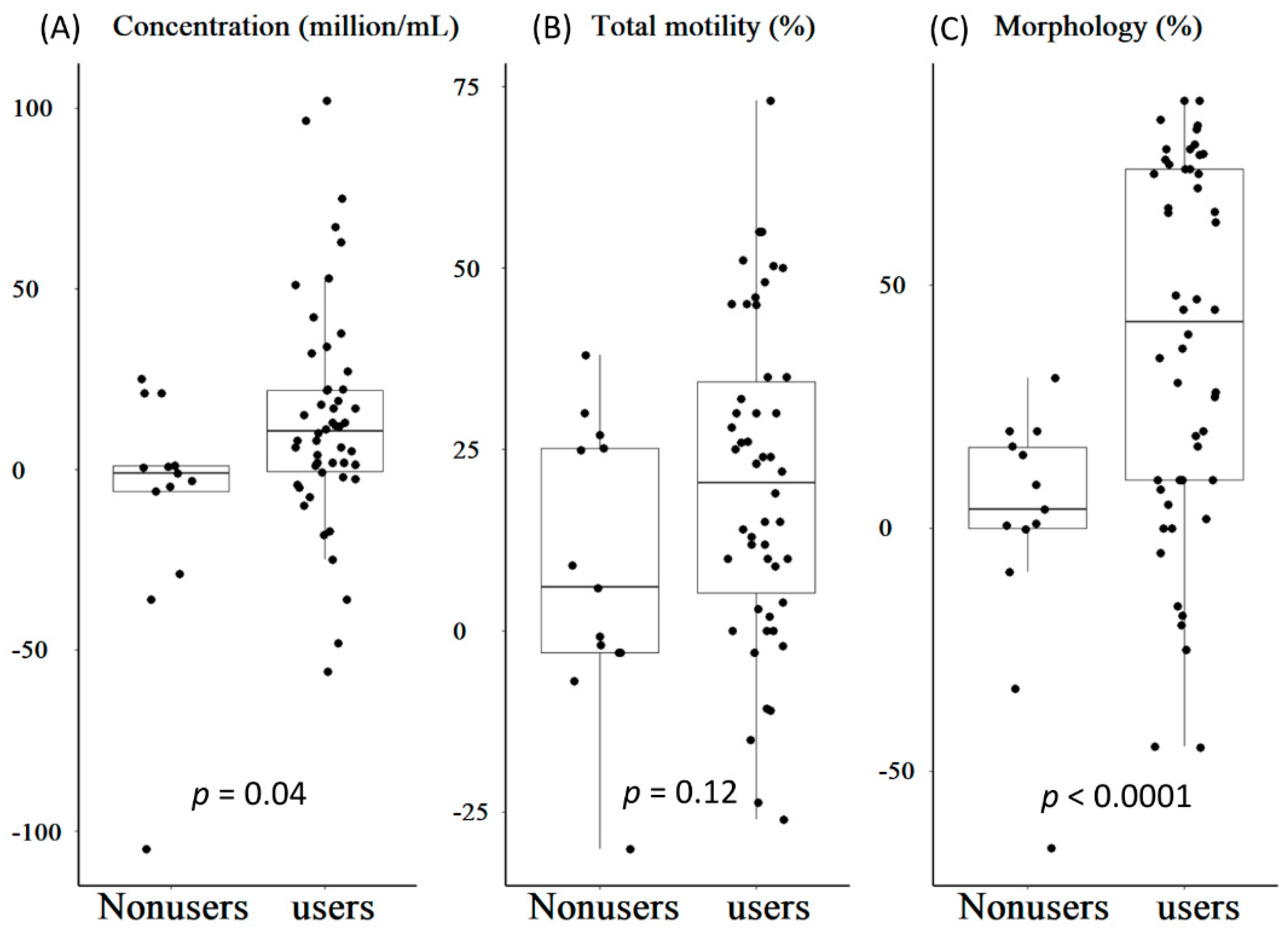
4.3. Changes in Semen Parameters Values
4.4. Adverse Effects
5. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Zegers-Hochschild, F.; Adamson, G.D.; de Mouzon, J.; Ishihara, O.; Mansour, R.; Nygren, K.; Sullivan, E.; van der Poel, S. The International Committee for Monitoring Assisted Reproductive Technology (ICMART) and the World Health Organization (WHO) Revised Glossary on ART Terminology, 2009. Hum. Reprod. 2009, 24, 2683–2687. [Google Scholar] [CrossRef] [PubMed]
- Mascarenhas, M.N.; Flaxman, S.R.; Boerma, T.; Vanderpoel, S.; Stevens, G.A. National, regional, and global trends in infertility prevalence since 1990: a systematic analysis of 277 health surveys. PLoS Med. 2012, 9, e1001356. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, A.; Mulgund, A.; Hamada, A.; Chyatte, M.R. A unique view on male infertility around the globe. Reprod. Biol. Endocrinol. 2015, 13, 37. [Google Scholar] [CrossRef] [PubMed]
- Ferlin, A.; Arredi, B.; Foresta, C. Genetic causes of male infertility. Reprod. Toxicol. 2006, 22, 133–141. [Google Scholar] [CrossRef] [PubMed]
- Singh, P.; Singh, M.; Cugati, G.; Singh, A.K. Hyperprolactinemia: An often missed cause of male infertility. J. Hum. Reprod. Sci. 2011, 4, 102–103. [Google Scholar] [CrossRef] [PubMed]
- Jarow, J.P. Effects of varicocele on male fertility. Hum. Reprod. Update 2001, 7, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Harlev, A.; Agarwal, A.; Gunes, S.O.; Shetty, A.; du Plessis, S.S. Smoking and Male Infertility: An Evidence-Based Review. World J. Men Health 2015, 33, 143–160. [Google Scholar] [CrossRef] [PubMed]
- Kumar, P.; Kumar, N.; Thakur, D.S.; Patidar, A. Male hypogonadism: Symptoms and treatment. J. Adv. Pharm. Technol. Res. 2010, 1, 297–301. [Google Scholar] [CrossRef] [PubMed]
- Chang, W.H.; Li, S.S.; Wu, M.H.; Pan, H.A.; Lee, C.C. Phthalates might interfere with testicular function by reducing testosterone and insulin-like factor 3 levels. Hum. Reprod. 2015, 30, 2658–2670. [Google Scholar] [CrossRef] [PubMed]
- Hamada, A.; Esteves, S.C.; Nizza, M.; Agarwal, A. Unexplained male infertility: diagnosis and management. Int. Braz. J. Urol. 2012, 38, 576–594. [Google Scholar] [CrossRef] [PubMed]
- Yao, D.F.; Mills, J.N. Male infertility: Lifestyle factors and holistic, complementary, and alternative therapies. Asian. J. Androl. 2016, 18, 410–418. [Google Scholar] [PubMed]
- Dabaja, A.A.; Schlegel, P.N. Medical treatment of male infertility. Transl. Androl. Urol. 2014, 3, 9–16. [Google Scholar] [PubMed]
- Ross, C.; Morriss, A.; Khairy, M.; Khalaf, Y.; Braude, P.; Coomarasamy, A.; El-Toukhy, T. A systematic review of the effect of oral antioxidants on male infertility. Reprod. Biomed. Online 2010, 20, 711–723. [Google Scholar] [CrossRef] [PubMed]
- Professional Committee of Andrology. Clinical guidelines of integrative medicine for male infertility (trial edition). Chin. Assoc. Integr. Med. 2015, 35, 1034–1038. [Google Scholar]
- Chua, M.E.; Escusa, K.G.; Luna, S.; Tapia, L.C.; Dofitas, B.; Morales, M. Revisiting oestrogen antagonists (clomiphene or tamoxifen) as medical empiric therapy for idiopathic male infertility: A meta-analysis. Andrology 2013, 1, 749–757. [Google Scholar] [CrossRef] [PubMed]
- Zini, A.; Fischer, M.A.; Nam, R.K.; Jarvi, K. Use of alternative and hormonal therapies in male infertility. Urology 2004, 63, 141–143. [Google Scholar] [CrossRef] [PubMed]
- Bardaweel, S.K. Alternative and antioxidant therapies used by a sample of infertile males in Jordan: A cross-sectional survey. BMC Complement. Altern. Med. 2014, 14, 244. [Google Scholar] [CrossRef] [PubMed]
- Leung, K.W.; Wong, A.S. Ginseng and male reproductive function. Spermatogenesis 2013, 3, e26391. [Google Scholar] [CrossRef] [PubMed]
- Yun, S.J.; Bae, G.S.; Park, J.H.; Song, T.H.; Choi, A.; Ryu, B.Y.; Pang, M.G.; Kim, E.J.; Yoon, M.; Chang, M.B. Antioxidant effects of cultured wild ginseng root extracts on the male reproductive function of boars and guinea pigs. Anim. Reprod. Sci. 2016, 170, 51–60. [Google Scholar] [CrossRef] [PubMed]
- Niu, S.; Chen, J.; Duan, F.; Song, Q.; Qin, M.; Wang, Z.; Liu, J. Possible mechanism underlying the effect of Heshouwuyin, a tonifying kidney herb, on sperm quality in aging rats. BMC Complement. Altern. Med. 2014, 14, 250. [Google Scholar] [CrossRef] [PubMed]
- Bahmanpour, S.; Vojdani, Z.; Panjehshahin, M.R.; Hoballah, H.; Kassas, H. Effects of carthamus tinctorius on semen quality and gonadal hormone levels in partially sterile male rats. Korean J. Urol. 2012, 53, 705–710. [Google Scholar] [CrossRef] [PubMed]
- Park, H.J.; Choe, S.; Park, N.C. Effects of Korean red ginseng on semen parameters in male infertility patients: A randomized, placebo-controlled, double-blind clinical study. Chin. J. Integr. Med. 2016, 22, 490–495. [Google Scholar] [CrossRef] [PubMed]
- Tempest, H.G.; Homa, S.T.; Routledge, E.J.; Garner, A.; Zhai, X.P.; Griffin, D.K. Plants used in Chinese medicine for the treatment of male infertility possess antioxidant and anti-oestrogenic activity. Syst. Biol. Reprod. Med. 2008, 54, 185–195. [Google Scholar] [CrossRef] [PubMed]
- Lu, W.H.; Gu, Y.Q. Insights into semen analysis: A Chinese perspective on the fifth edition of the WHO laboratory manual for the examination and processing of human semen. Asian J. Androl. 2010, 12, 605–606. [Google Scholar] [CrossRef] [PubMed]
- Cooper, T.G.; Noonan, E.; von Eckardstein, S.; Auger, J.; Baker, H.W.; Behre, H.M.; Haugen, T.B.; Kruger, T.; Wang, C.; Mbizvo, M.T.; et al. World Health Organization reference values for human semen characteristics. Hum. Reprod. Update 2010, 16, 231–245. [Google Scholar] [CrossRef] [PubMed]
- Zhao, M.P.; Shi, X.; Kong, G.W.S.; Wang, C.C.; Wu, J.C.Y.; Lin, Z.X.; Li, T.C.; Chan, D.Y.L. The therapeutic effects of a traditional chinese medicine formula wuzi yanzong pill for the treatment of oligoasthenozoospermia: A meta-analysis of randomized controlled trials. Evid.-Based Complement. Altern. Med. eCAM 2018, 2018, 2968025. [Google Scholar] [CrossRef] [PubMed]
- Jo, J.; Kang, M.J.; Lee, J.M.; Kim, H.; Jerng, U.M. Effects of traditional Korean medicine on anti-Mullerian hormone in patients with diminished ovarian reserve: A retrospective study. Complement. Ther. Med. 2016, 24, 118–122. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, A.; Saleh, R.A. Role of oxidants in male infertility: Rationale, significance, and treatment. Urol. Clin. N. Am. 2002, 29, 817–827. [Google Scholar] [CrossRef]
- Sikka, S.C. Relative impact of oxidative stress on male reproductive function. Curr. Med. Chem. 2001, 8, 851–862. [Google Scholar] [CrossRef] [PubMed]
- Sanocka, D.; Kurpisz, M. Reactive oxygen species and sperm cells. Reprod. Biol. Endocrinol. 2004, 2, 12. [Google Scholar] [CrossRef] [PubMed]
- de Lamirande, E.; Gagnon, C. Impact of reactive oxygen species on spermatozoa: A balancing act between beneficial and detrimental effects. Hum. Reprod. 1995, 10, 15–21. [Google Scholar] [CrossRef] [PubMed]
- Aziz, N.; Saleh, R.A.; Sharma, R.K.; Lewis-Jones, I.; Esfandiari, N.; Thomas, A.J., Jr.; Agarwal, A. Novel association between sperm reactive oxygen species production, sperm morphological defects, and the sperm deformity index. Fertil. Steril. 2004, 81, 349–354. [Google Scholar] [CrossRef] [PubMed]
- Aitken, R.J.; Baker, M.A. Oxidative stress, sperm survival and fertility control. Mol. Cell Endocrinol. 2006, 250, 66–69. [Google Scholar] [CrossRef] [PubMed]
- Ahmadi, S.; Bashiri, R.; Ghadiri-Anari, A.; Nadjarzadeh, A. Antioxidant supplements and semen parameters: An evidence based review. Int. J. Reprod. Biomed. (Yazd) 2016, 14, 729–736. [Google Scholar] [CrossRef]
- Kim, S.J.; Kim, M.R.; Hwang, S.Y.; Bae, W.J.; Kim, S.; Hong, S.H.; Lee, J.Y.; Hwang, T.K.; Wang, Z.; Kim, S.W. Preliminary report on the safety of a new herbal formula and its effect on sperm quality. World J. Men Health 2013, 31, 254–261. [Google Scholar] [CrossRef] [PubMed]
- Qian, L.; Yu, S. Protective effect of polysaccharides from Lycium barbarum on spermatogenesis of mice with impaired reproduction system induced by cyclophosphamide. Am. J. Reprod. Immunol. 2016, 76, 383–385. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.M.; Fu, H.; Liu, G.X. Clinical and experimental study on effect of Wu-Zi-Yan-Zong pill on oxidative damage of mitochondrial DNA in aging. Chin. J. Integr. Tradit. West. Med. 2002, 22, 3. [Google Scholar]
- Chen, M.L.; Tsai, S.H.; Ip, S.P.; Ko, K.M.; Che, C.T. Long-term treatment with a “Yang-invigorating” Chinese herbal formula, Wu-Zi-Yan-Zong-Wan, reduces mortality and liver oxidative damage in chronic alcohol-intoxicated rats. Rejuvenation Res. 2010, 13, 459–467. [Google Scholar] [CrossRef] [PubMed]
- Ji, H.J.; Wang, D.M.; Wu, Y.P.; Niu, Y.Y.; Jia, L.L.; Liu, B.W.; Feng, Q.J.; Feng, M.L. Wuzi Yanzong pill, a Chinese polyherbal formula, alleviates testicular damage in mice induced by ionizing radiation. BMC Complement. Altern. Med. 2016, 16, 509. [Google Scholar] [CrossRef] [PubMed]
- Omirinde, J.O.; Ozegbe, P.C.; Oyeyemi, M.O. Comparative evaluation of the sperm characteristics and morphology of adult Wistar rats fed either low or normal protein-energy diets and orally dosed with aqueous Cuscuta australis extracts. Niger. J. Physiol. Sci. 2014, 29, 55–61. [Google Scholar] [PubMed]
- Travison, T.G.; Araujo, A.B.; O’Donnell, A.B.; Kupelian, V.; McKinlay, J.B. A population-level decline in serum testosterone levels in American men. J. Clin. Endocrinol. Metab. 2007, 92, 196–202. [Google Scholar] [CrossRef] [PubMed]
- Crosnoe, L.E.; Grober, E.; Ohl, D.; Kim, E.D. Exogenous testosterone: A preventable cause of male infertility. Transl. Androl. Urol. 2013, 2, 106–113. [Google Scholar] [PubMed]
- Chen, J.C.; Chen, L.D.; Tsauer, W.; Tsai, C.C.; Chen, B.C.; Chen, Y.J. Effects of Ginsenoside Rb2 and Rc on inferior human sperm motility in vitro. Am. J. Chin. Med. 2001, 29, 155–160. [Google Scholar] [CrossRef] [PubMed]
- Tamler, R.; Mechanick, J.I. Dietary supplements and nutraceuticals in the management of andrologic disorders. Endocrinol. Metab. Clin. North. Am. 2007, 36, 533–552. [Google Scholar] [CrossRef] [PubMed]
- Wu, Z.Q.; Chen, D.L.; Lin, F.H.; Lin, L.; Shuai, O.; Wang, J.Y.; Qi, L.K.; Zhang, P. Effect of bajijiasu isolated from Morinda officinalis F.C. how on sexual function in male mice and its antioxidant protection of human sperm. J. Ethnopharmacol. 2015, 164, 283–292. [Google Scholar] [CrossRef] [PubMed]
- Colagar, A.H.; Marzony, E.T.; Chaichi, M.J. Zinc levels in seminal plasma are associated with sperm quality in fertile and infertile men. Nutr. Res. 2009, 29, 82–88. [Google Scholar] [CrossRef] [PubMed]
- Zhang, M.; Wang, J.; Zhang, S. Study on the composition of Lycium barbarum polysaccharides and its effects on the growth of weanling mice. J. Hyg. Res. 2002, 31, 118–119. [Google Scholar]
- Zhu, M.Y.; Wang, C.J.; Zhang, H.S.; Pei, X.W.; Fen, J.M. Protective effect of polysaccharides from morinda officinalis on bone loss in ovariectomized rats. Int. J. Biol. Macromol. 2008, 43, 276–278. [Google Scholar]
- Sharpe, R.M. Sperm counts and fertility in men: a rocky road ahead. Science & Society Series on Sex and Science. EMBO Rep. 2012, 13, 398–403. [Google Scholar] [PubMed]
- Nan, Y.; Zhang, X.; Yang, G.; Xie, J.; Lu, Z.; Wang, W.; Ni, X.; Cao, X.; Ma, J.; Wang, Z. Icariin stimulates the proliferation of rat Sertoli cells in an ERK1/2-dependent manner in vitro. Andrologia 2014, 46, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Yang, B.; Zhang, C.; Du, L.; Shan, X.; Zou, P.; Dang, Q. Clinical study on the treatment of male immune infertility with sheng jing zhong zi tang. J. Tradit. Chin. Med. 2002, 22, 102–103. [Google Scholar] [PubMed]
- Pan, M.H.; Chiou, Y.S.; Tsai, M.L.; Ho, C.T. Anti-inflammatory activity of traditional Chinese medicinal herbs. J. Tradit. Complement. Med. 2011, 1, 8–24. [Google Scholar] [CrossRef]
- Wang, W. What kinds of external therapies can be adopted for chronic prostatitis? J. Tradit. Chin. Med. 2007, 27, 238–240. [Google Scholar] [PubMed]
| Variable | TCM Nonusers | TCM Users | p-Value |
|---|---|---|---|
| N = 13 (%) | N = 50 (%) | ||
| Age, years (SD) * | 37.6 (3.75) | 37.7 (6.31) | 0.97 |
| Duration of infertility, year (SD) * | 2.77 (1.30) | 4.43 (3.46) | 0.009 |
| Body mass index, mean (SD) * | 25.7 (4.42) | 25.5 (3.39) | 0.84 |
| Smokers | 2 (15.4) | 7 (14.0) | 0.90 |
| Alcohol use | 0 (0) | 3 (6.0) | 0.37 |
| Infertility type | 0.46 | ||
| Primary | 13 (100) | 48 (96.0) | |
| Secondary | 0 (0) | 2 (4.00) |
| Variable | Semen Improvement | Crude OR (95% CI) | Adjusted OR (95% CI) | |
|---|---|---|---|---|
| No N = 23 (%) | Yes N = 40 (%) | |||
| TCM | ||||
| No | 10 (43.5) | 3 (7.50) | ref | ref |
| Yes | 13 (56.5) | 37 (92.5) | 9.49 (2.26–39.9) | 10.7 (2.28–50.4) |
| Age group, years | ||||
| <40 | 14 (60.9) | 32 (80.0) | ref | ref |
| ≥40 | 9 (39.1) | 8 (20.0) | 0.39 (0.12–1.22) | 0.37 (0.10–1.40) |
| Duration of infertility, yeas | ||||
| <3 | 9 (39.1) | 16 (40.0) | ref | ref |
| ≥3 | 14 (60.9) | 24 (60.0) | 0.96 (0.34–2.75) | 1.04 (0.27–4.02) |
| BMI | ||||
| <24 | 7 (30.4) | 14 (35.0) | ref | ref |
| ≥24 | 16 (69.6) | 26 (65.0) | 0.81 (0.27–2.44) | 0.84 (0.22–3.16) |
| Smokers (ref: non-smokers) | 5 (21.7) | 4 (10.0) | 0.40 (0.10–1.67) | 0.27 (0.04–1.72) |
| Alcohol use (ref: nonusers) | 1 (4.35) | 2 (5.00) | 1.16 (0.10–13.5) | 1.44 (0.09–22.1) |
| Infertility type | ||||
| Primary | 22 (95.7) | 39 (97.5) | ref | ref |
| Secondary | 1 (4.35) | 1 (2.50) | 0.56 (0.03–9.47) | 0.21 (0.01–4.30) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wang, S.-C.; Wang, S.-C.; Li, C.-J.; Lin, C.-H.; Huang, H.-L.; Tsai, L.-M.; Chang, C.-H. The Therapeutic Effects of Traditional Chinese Medicine for Poor Semen Quality in Infertile Males. J. Clin. Med. 2018, 7, 239. https://doi.org/10.3390/jcm7090239
Wang S-C, Wang S-C, Li C-J, Lin C-H, Huang H-L, Tsai L-M, Chang C-H. The Therapeutic Effects of Traditional Chinese Medicine for Poor Semen Quality in Infertile Males. Journal of Clinical Medicine. 2018; 7(9):239. https://doi.org/10.3390/jcm7090239
Chicago/Turabian StyleWang, Shu-Chiu, Shu-Chen Wang, Chia-Jung Li, Ching-Heng Lin, Hsiao-Lin Huang, Liang-Miin Tsai, and Chiung-Hung Chang. 2018. "The Therapeutic Effects of Traditional Chinese Medicine for Poor Semen Quality in Infertile Males" Journal of Clinical Medicine 7, no. 9: 239. https://doi.org/10.3390/jcm7090239
APA StyleWang, S.-C., Wang, S.-C., Li, C.-J., Lin, C.-H., Huang, H.-L., Tsai, L.-M., & Chang, C.-H. (2018). The Therapeutic Effects of Traditional Chinese Medicine for Poor Semen Quality in Infertile Males. Journal of Clinical Medicine, 7(9), 239. https://doi.org/10.3390/jcm7090239






