The Role of Insulin Resistance/Hyperinsulinism on the Rising Trend of Thyroid and Adrenal Nodular Disease in the Current Environment
Abstract
1. Introduction
2. The Rising Prevalence of Thyroid and Adrenal Nodular Disease in the Current Environment
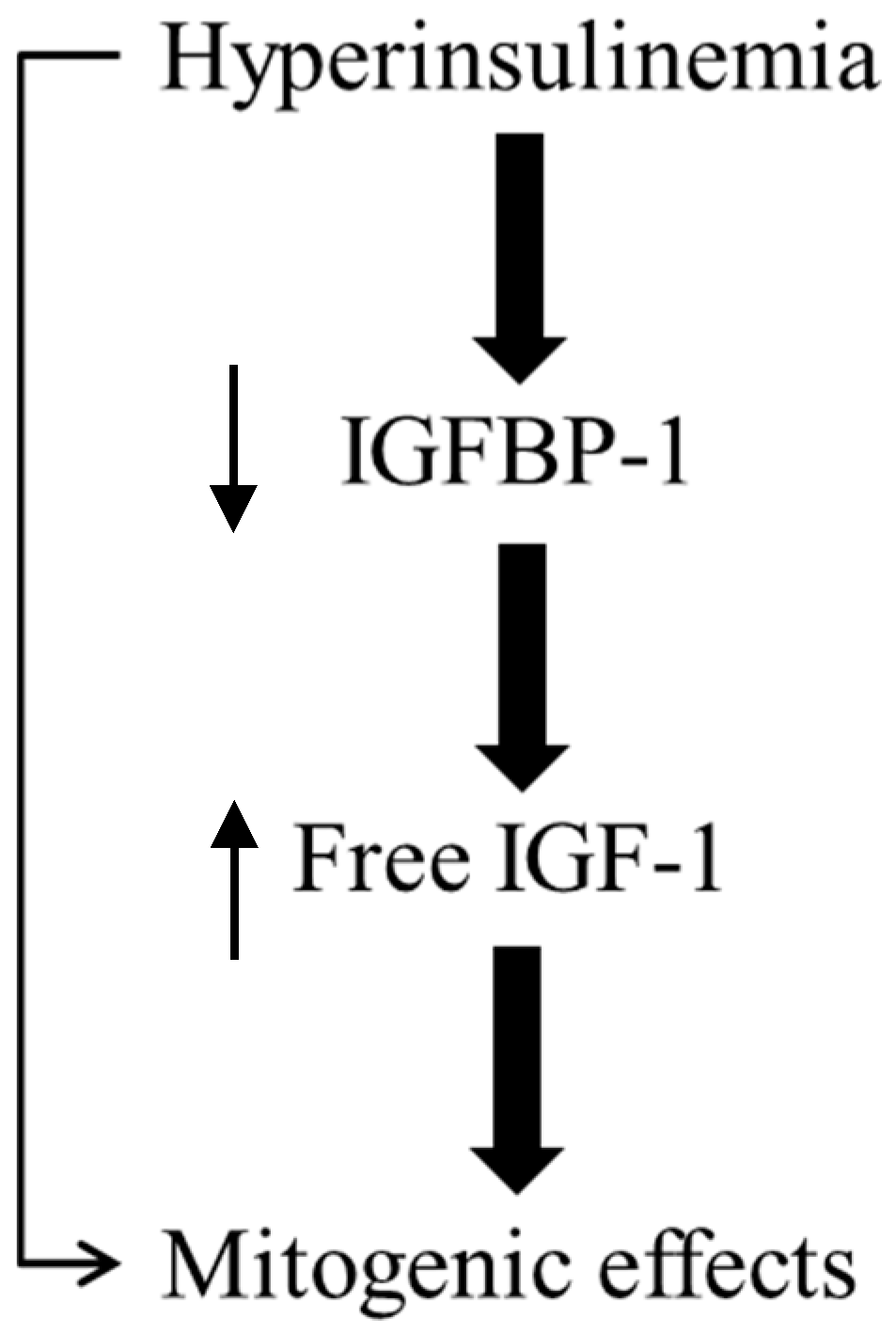
3. Metabolic/Insulin Resistance Syndrome and Compensatory Hyperinsulinism—Mitogenic Effects
4. Association of Insulin Resistance/Hyperinsulinism with Increased Risk of Thyroid and Adrenal Nodular Disease—Clinical Evidence
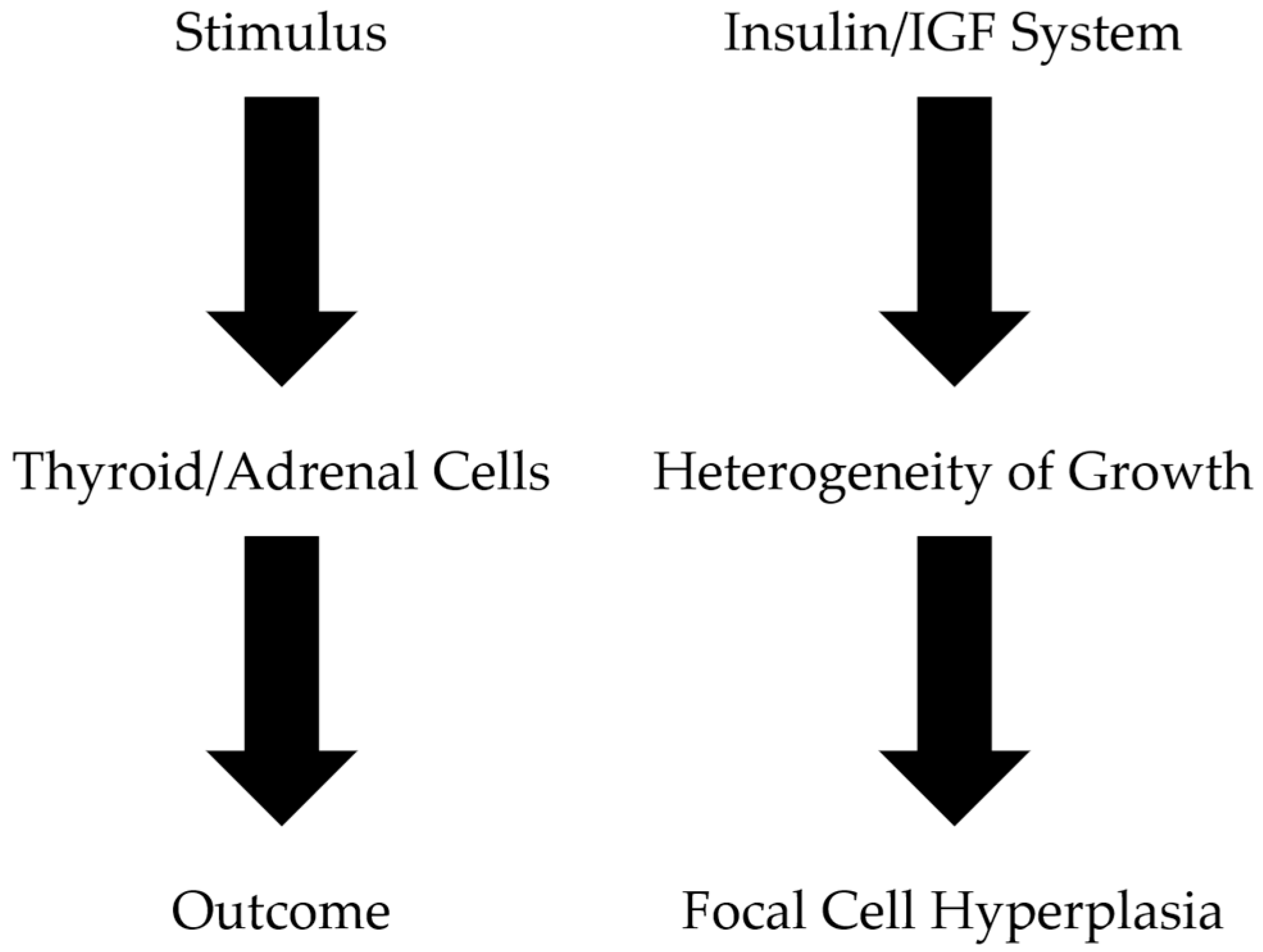
5. The Insulin/IGF System and Its Involvement in Thyroid and Adrenal Cell Hyperplasia
6. Conclusions and Future Perspectives
Conflicts of Interest
References
- Gharib, H.; Papini, E. Thyroid nodules: Clinical importance, assessment, and treatment. Endocrinol. Metab. Clin. N. Am. 2007, 36, 707–773. [Google Scholar] [CrossRef] [PubMed]
- Medeios-Neto, G.; Rubio, I.G.S. Multinodular Goiter. 2016. Available online: http://www.thyroidmanager.org/chapter/multinodular-goiter (accessed on 18 February 2018).
- Kloos, R.T.; Gross, M.D.; Francis, I.R.; Korobkin, M.; Shapiro, B. Incidentally discovered adrenal masses. Endocr. Rev. 1995, 16, 460–484. [Google Scholar] [PubMed]
- Studer, H.; Derwhal, M. Mechanisms of non-neoplastic endocrine hyperplasia—A changing concept: A review focused on the thyroid gland. Endocr. Rev. 1995, 16, 411–426. [Google Scholar] [PubMed]
- Derwahl, M. Molecular aspects of the pathogenesis of nodular goiters, thyroid nodules and adenomas. Exp. Clin. Endocrinol. Diab. 1996, 104 (Suppl. 4), 32–35. [Google Scholar] [CrossRef] [PubMed]
- Kimura, T.; Van Keymeulen, A.; Golstein, J.; Fusco, A.; Dumont, J.E.; Roger, P.P. Regulation of thyroid cell proliferation by TSH and other factors: A critical evaluation of in vitro models. Endocr. Rev. 2001, 22, 631–656. [Google Scholar] [CrossRef] [PubMed]
- Bidey, S.P.; Hill, D.J.; Eggo, M.C. Growth factors and goitrogenesis. J. Endocrinol. 1999, 160, 321–332. [Google Scholar] [CrossRef] [PubMed]
- Ribeiro, T.C.; Latronico, A.C. Insulin-like growth factor system on adrenocortical tumorigenesis. Mol. Cel. Endoctrinol. 2012, 351, 96–100. [Google Scholar] [CrossRef] [PubMed]
- Rezzonico, J.; Rezzonico, M.; Pusiol, E.; Pitoia, F.; Niepomniszcze, H. High prevalence of thyroid nodules in patients with acrochordons (skin tags). Possible role of insulin-resistance. Medicina 2009, 69, 302–304. [Google Scholar] [PubMed]
- Arduc, A.; Isik, S.; Ozuguz, U.; Tutuncu, Y.A.; Kucukler, F.K.; Ozcan, H.N. Relationship between thyroid nodules and non-functioning adrenal incidentalomas and their association with insulin resistance. Endocr. Res. 2014, 39, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Nilsson, M. Iodine handling by the thyroid epithelial cell. Exp. Clin. Endocrinol. Diabetes 2001, 109, 13–18. [Google Scholar] [CrossRef] [PubMed]
- Laurberg, P.; Pedesren, K.M.; Vestergaard, H.; Sigurdsson, G. High incidence of multinodular goiter in the elderly population in a low iodine intake area vs. high incidence of Graves’ disease in the young in a high iodine intake area. J. Int. Med. 1991, 229, 415–420. [Google Scholar] [CrossRef]
- Tsatsoulis, A.; Johnson, E.O.; Andricula, M.; Kalogera, C.; Svarna, E.; Spyroy, P.; Seferiadis, K.; Tsolas, O. Thyroid autoimmunity is associated with higher urinary iodine concentrations in an iodine-deficient area of Northwestern Greece. Thyroid 1999, 9, 279–283. [Google Scholar] [CrossRef] [PubMed]
- Zois, C.; Stavrou, I.; Kalogera, C.; Svarna, E.; Dimoliatis, I.; Seferiadis, K.; Tsatsoulis, A. High prevalence of autoimmune thyroiditis in school children after elimination of iodine deficiency in Northwestern Greece. Thyroid 2003, 13, 485–489. [Google Scholar] [CrossRef] [PubMed]
- Ayturk, S.; Gursoy, A.; Kut, A.; Anil, C.; Nar A Tutuncu, N.B. Metabolic syndrome and its components are associated with increased thyroid volume and nodule prevalence in a mild-to-moderate iodine-deficient area. Eur. J. Endocrinol. 2009, 61, 599–605. [Google Scholar] [CrossRef] [PubMed]
- Reincke, M.; Fassnacht, M.; Väth, S.; Mora, P.; Allolio, B. Adrenal incidentalomas: A manifestation of the metabolic syndrome? Enocr. Res. 1996, 22, 757–761. [Google Scholar] [CrossRef]
- Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z. The metabolic syndrome. Lancet 2005, 365, 1415–1418. [Google Scholar] [CrossRef]
- Wilcox, G. Insulin and insulin resistance. Clin. Biochem. Rev. 2005, 26, 19–39. [Google Scholar] [PubMed]
- Tsatsoulis, A.; Mantzaris, M.D.; Bellou, S.; Andrikoula, M. Insulin resistance: An adaptive mechanism becomes maladaptive in the current environment—An evolutionary perspective. Metabolism 2013, 65, 622–633. [Google Scholar] [CrossRef] [PubMed]
- Heidari, Z.; Mashhadi, A.; Nosratzehi, S. Insulin resistance in patients with benign thyroid nodules. Arch. Iran Med. 2015, 18, 572–576. [Google Scholar] [PubMed]
- El Saghier, E.O.A.; Hassan, Z.A.B.; Shawky, A.M.A. Euthyroid nodular disease in relation to insulin resistance. Int. J. Diabetes Res. 2015, 4, 49–57. [Google Scholar]
- Reszzonico, J.; Rezzonico, M.; Pusiol, E.; Pitoia, F.; Nieomnisszcze, H. Introducing the thyroid gland as another victim of the insulin resistance syndrome. Thyroid 2008, 18, 461–464. [Google Scholar] [CrossRef] [PubMed]
- Yasar, H.Y.; Ertugrul, O.; Ertugrul, B.; Ertugrul, D.; Sahim, M. Insulin resistance in nodular thyroid disease. Endocr. Res. 2011, 36, 167–174. [Google Scholar] [CrossRef] [PubMed]
- Sousa, P.A.; Vaisman, M.; Carneiro, J.R.; Guimarães, L.; Freitas, H.; Pinheiro, M.F.; Liechocki, S.; Monteiro, C.M.; Teixeira Pde, F. Prevalence of goiter and thyroid nodular disease in patients with class III obesity. Arq. Bras. Endocrinol. 2013, 57, 120–124. [Google Scholar] [CrossRef]
- Anil, C.; Akkurt, S.; Kut, A.; Gursoy, A. Impaired glucose metabolism is a risk factor for increased thyroid volume and nodule prevalence in a mild-to-moderate iodine deficient area. Metabolism 2013, 62, 970–975. [Google Scholar] [CrossRef] [PubMed]
- Javier, C.; Ricardo, P.; Hugo, C. To assess the relationship between hyper-insulinism and thyroid nodules in children with overweight and obesity. Endocrinol. Metab. Synd. 2015, 4. [Google Scholar] [CrossRef]
- Cheng, N.W.; Boyages, S.C. The thyroid gland in acromegaly: An ultrasonographic study. Clin. Endocrinol. 1997, 46, 545–549. [Google Scholar] [CrossRef]
- Tuna, M.M.; Imga, N.N.; Dogan, B.A.; Yilmaz, F.M.T.; Topcuoglu, C.; Akbaba, G.; Berker, D.; Gule, S. Non-functioning adrenal incidentalomas are associated with higher hypertension prevalence and higher risk of atherosclerosis. J. Endocrinol. Investig. 2014, 37, 765–768. [Google Scholar] [CrossRef] [PubMed]
- Peppa, M.; Boutati, E.; Koliaki, C.; Papaefstathiou, N.; Garoflos, E.; Economopoulos, T.; Hadjidakis, D.; Raptis, S.A. Insulin resistance and metabolic syndrome in patients with nonfunctioning adrenal incidentalomas: A cause-effect relationship? Metab. Clin. Exp. 2010, 59, 1435–1441. [Google Scholar] [CrossRef] [PubMed]
- Hiroi, N.; Sue, M.; Yoshihara, A.; Ichijo, T.; Yoshida-Hiroi, M.; Higa, M.; Yoshino, G. Prevalence of adrenal massess in Japanese patients with type 2 diabetes mellitus. Diabetol. Metb. Syvndr. 2010, 2, 71. [Google Scholar] [CrossRef] [PubMed]
- Hedeland, H.; Osterg, G.; Hokfelt, B. On the prevalence of adrenocortical adenomas in an autopsy material in relation to hypertension and diabetes. Acta Med. Scand. 1968, 184, 211–214. [Google Scholar] [CrossRef] [PubMed]
- Muscogiuri, G.; Sorice, G.P.; Prioletta, A.; Mezza, T.; Cipolla, C.; Salomone, E.; Giaccari, A.; Pontecorvi, A.; Della Casa, S. The size of adrenal incidentalomas correlates with insulin resistance. Is there a cause-effect relationship? Clin. Endocrinol. 2011, 74, 300–305. [Google Scholar] [CrossRef] [PubMed]
- Altieri, B.; Tirabassi, G.; Della Casa, S.; Ronchi, C.L.; Balercia, G.; Orio, F.; Pontecorvi, A.; Colao, A.; Muscogiuri, G. Adrenocortical tumors and insulin resistance: What is the first step? Int. J. Cancer 2015, 138, 2785–2794. [Google Scholar] [CrossRef] [PubMed]
- Muscogiuri, G.; De Martino, M.C.; Negri, M.R.; Pivonello, C.; Simeoli, C.; Orio, F.; Pivonello, R.; Colao, A. Adrenal mass: Insight into pathogenesis and a common link with insulin resistance. Endocrinology 2017, 158, 1527–1532. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Peppa, M.; Koliaki, C.; Raptis, S.A. Adrenal incidentalomas and cardiometabolic morbidity: An emerging association with serious clinical implications. J. Intern. Med. 2010, 268, 555–556. [Google Scholar] [CrossRef] [PubMed]
- Kotłowska, A.; Maliński, E.; Sworczak, K.; Kumirska, J.; Stepnowski, P. Urinary steroid profile in patients diagnosed with adrenal incidentalomas. Clin. Biochem. 2009, 42, 448–454. [Google Scholar] [CrossRef] [PubMed]
- Brossaud, J.; Ducint, D.; Corcuff, J.B. Urinary glucocorticoid metabolites: Biomarkers to classify adrenal incidentalomas? Clin. Endocrinol. 2015, 84, 236–243. [Google Scholar] [CrossRef] [PubMed]
- Midorikawa, S.; Sanada, H.; Hashimoto, S. The improvement of insulin resistance in patients with adrenal incidentaloma by surgical resection. Clin. Endocrinol. 2001, 54, 797–804. [Google Scholar] [CrossRef]
- Bernini, G.; Moretti, A.; Iacconi, P.; Miccoli, P.; Nami, R.; Lucani, B.; Salvetti, A. Anthropometric, haemodynamic, humoral and hormonal evaluation in patients with incidental adrenocortical adenomas before and after surgery. Eur. J. Endocrinol. 2003, 148, 213–219. [Google Scholar] [CrossRef] [PubMed]
- Sereg, M.; Szappanos, A.; Toke, J.; Karlinger, K.; Feldman, K.; Kaszper, E.; Varga, I.; Glaz, E.; Racz, K.; Toth, M. Atherosclerotic risk factors and complications in patients with non-functioning adrenal adenomas treated with or without adrenalectomy: A long-term follow-up study. Eur. J. Endocrinol. 2009, 160, 647–655. [Google Scholar] [CrossRef] [PubMed]
- Belfiore, A.; Frasca, F.; Pandini, G.; Sciacca, L.; Vigneri, R. Insulin receptor isoforms and insulin receptor/insulin-like growth factor receptor hybrids in physiology and disease. Endocr. Rev. 2009, 30, 586–623. [Google Scholar] [CrossRef] [PubMed]
- Malaquarnera, R.; Morcavallo, A.; Belfiore, A. The insulin and IGF-I pathway in endocrine glands carcinogenesis. J. Oncol. 2012, 2012. [Google Scholar] [CrossRef] [PubMed]
- Malaguarnera, R.; Frasca, F.; Garozzo, A.; Gianì, F.; Pandini, G.; Vella, V.; Vigneri, R.; Belfiore, A. Insulin receptor isoforms and insulin-like growth factor receptor in human follicular cell precursors from papillary thyroid cancer and normal thyroid. J. Clin. Endocrinol. Metab. 2011, 96, 766–774. [Google Scholar] [CrossRef] [PubMed]
- Jaffe, R.B. Mitogenic action, regulation, and localization of insulin-like growth factors in the human fetal adrenal gland. J. Clin. Endocrinol. Metab. 1993, 76, 968–976. [Google Scholar]
- Baxter, R.C.; Dayson, J.M.; Turtle, J.R. Somatogenic receptors of rat liver: Regulation by insulin. Endocrinology 1984, 14, 1176–1181. [Google Scholar] [CrossRef] [PubMed]
- Ittermann, T.; Markus, M.R.; Schipf, S.; Derwahl, M.; Meisinger, C.; Völzke, H. Metformin inhibits goitrogenous effects of type 2 diabetes. Eur. J. Endocrinol. 2013, 169, 9–15. [Google Scholar] [CrossRef] [PubMed][Green Version]
© 2018 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tsatsoulis, A. The Role of Insulin Resistance/Hyperinsulinism on the Rising Trend of Thyroid and Adrenal Nodular Disease in the Current Environment. J. Clin. Med. 2018, 7, 37. https://doi.org/10.3390/jcm7030037
Tsatsoulis A. The Role of Insulin Resistance/Hyperinsulinism on the Rising Trend of Thyroid and Adrenal Nodular Disease in the Current Environment. Journal of Clinical Medicine. 2018; 7(3):37. https://doi.org/10.3390/jcm7030037
Chicago/Turabian StyleTsatsoulis, Agathocles. 2018. "The Role of Insulin Resistance/Hyperinsulinism on the Rising Trend of Thyroid and Adrenal Nodular Disease in the Current Environment" Journal of Clinical Medicine 7, no. 3: 37. https://doi.org/10.3390/jcm7030037
APA StyleTsatsoulis, A. (2018). The Role of Insulin Resistance/Hyperinsulinism on the Rising Trend of Thyroid and Adrenal Nodular Disease in the Current Environment. Journal of Clinical Medicine, 7(3), 37. https://doi.org/10.3390/jcm7030037



