Management Strategies for Zenker’s Diverticulum: A Comprehensive Review
Abstract
1. Introduction
2. Methods
3. Discussion
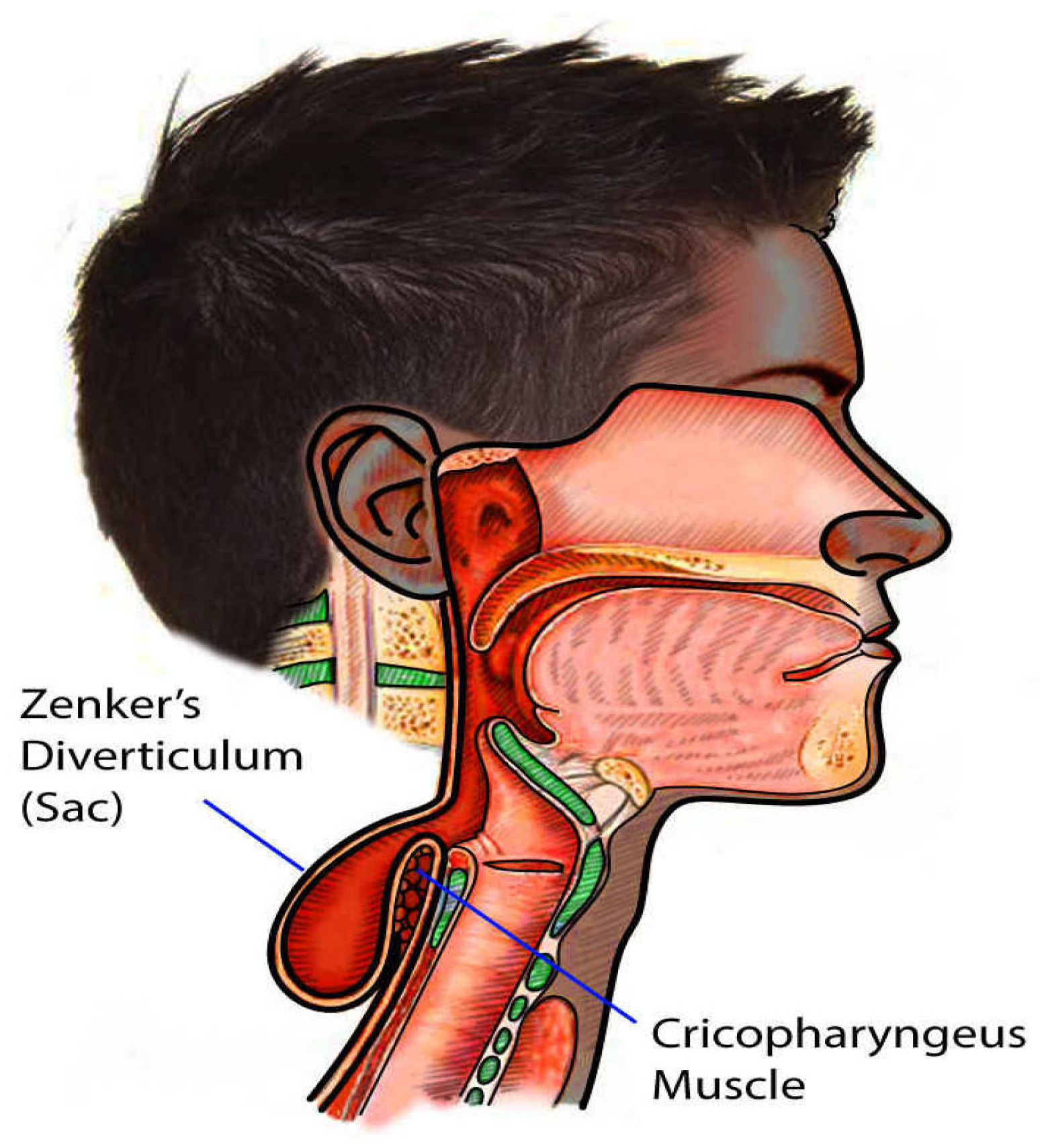
3.1. Anatomy and Pathophysiology
- Small—Diverticulum size less than 2 cm.
- Intermediate—Diverticulum size between 2 and 4 cm.
- Large—Diverticulum size greater than 4 cm.
- Grade I—Diverticulum less than 2 cm.
- Grade II—Diverticulum between 2 and 5 cm.
- Grade III—Diverticulum greater than 5 cm.
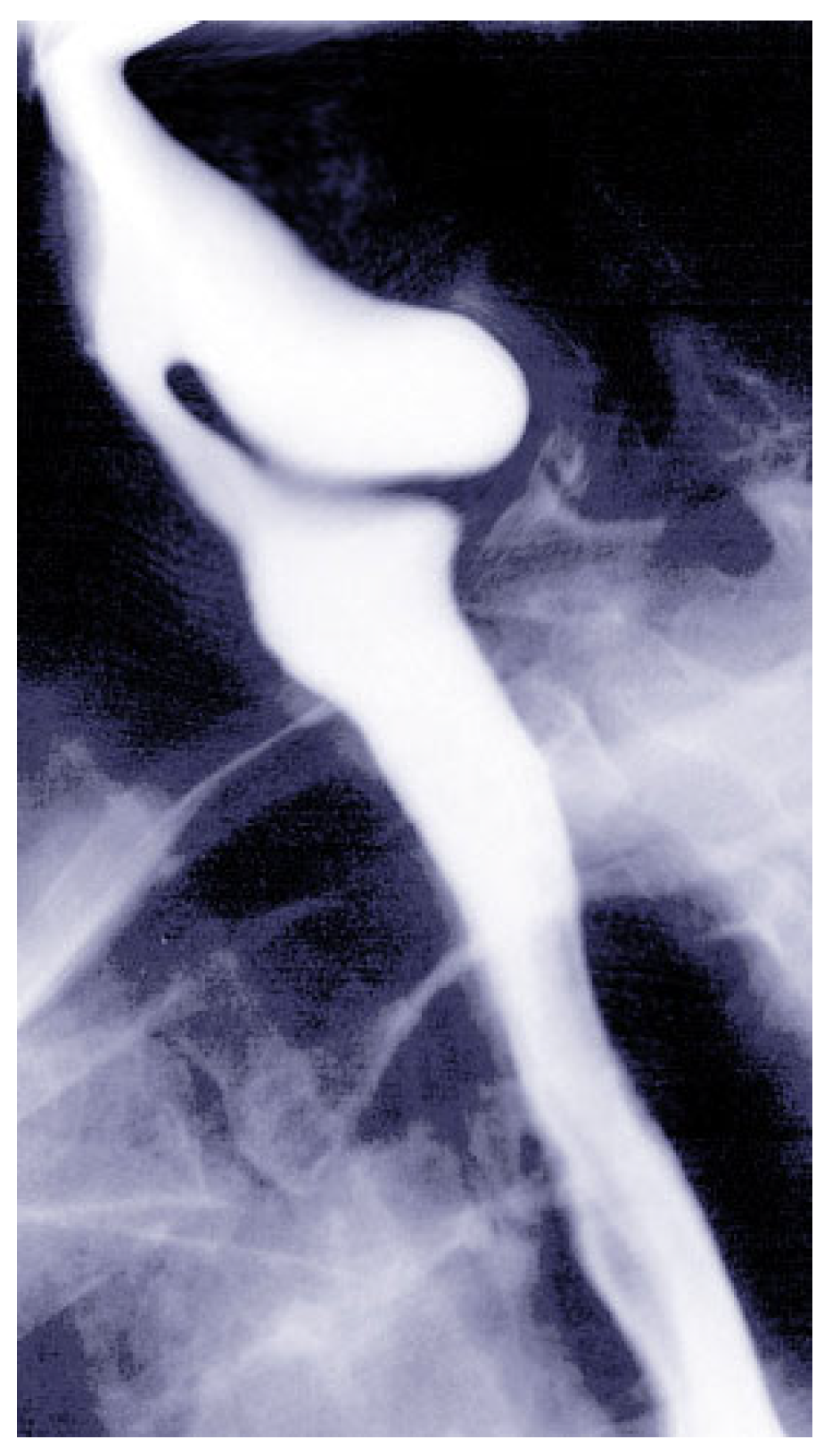
3.2. Diagnosis of Zenker’s Diverticulum
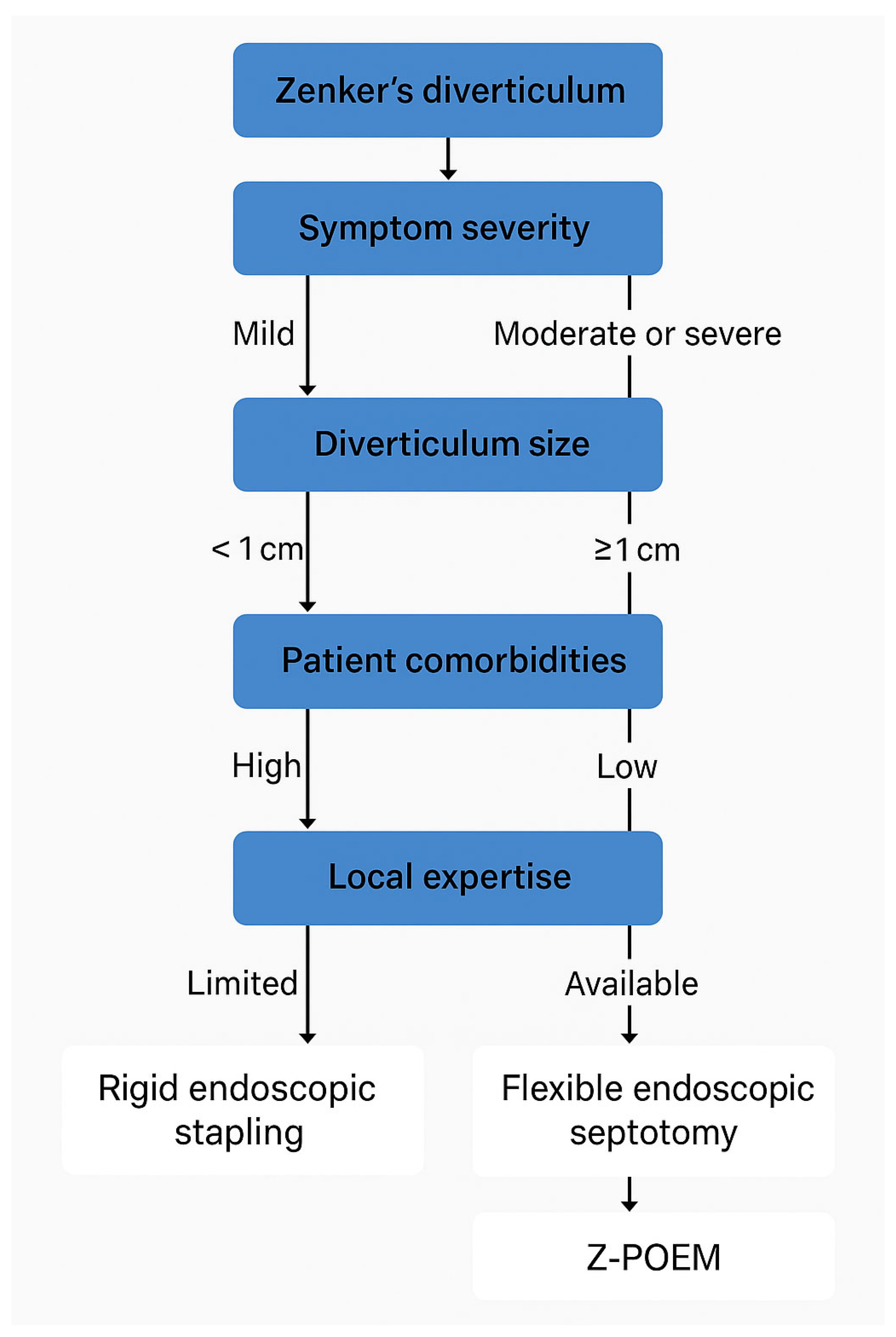
3.3. Management of Zenker’s Diverticulum
3.3.1. Open Surgery
3.3.2. Endoscopic Modalities of Treatment for Zenker’s Diverticulum
Rigid Endoscopic Stapling
Flexible Endoscopic Techniques (Z-POEM)
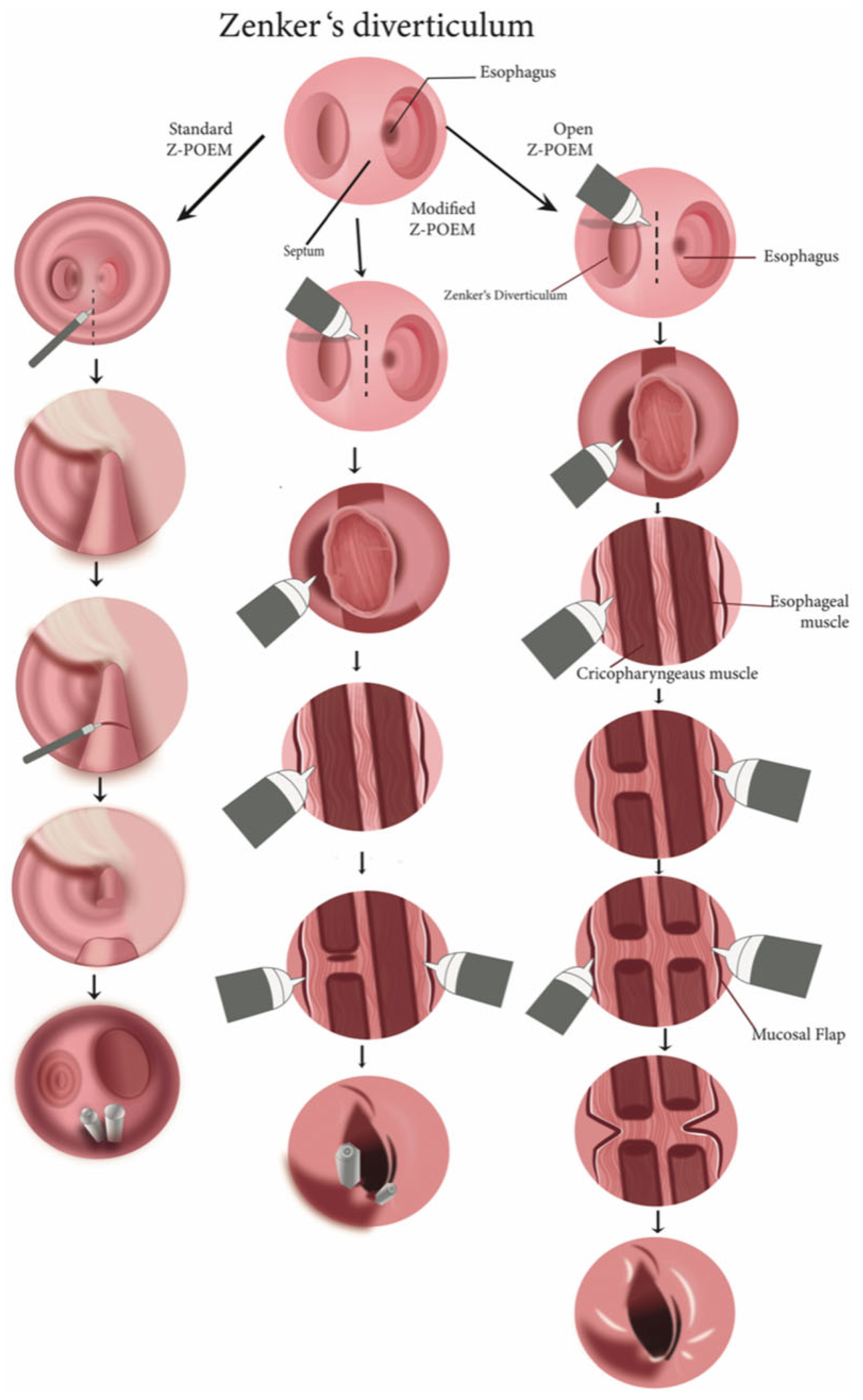
3.4. Techniques of Zenker’s Peroral Endoscopic Myotomy (Z-POEM)
3.5. Special Considerations and Techniques
3.5.1. Role of EndoFLIP in Z-POEM
3.5.2. Role of Endoscopic Sutures in Z-POEM
3.5.3. Detailed Summary of Results Comparing Different Treatment Modalities for Zenker’s Diverticulum
- Z-POEM vs. Flexible Endoscopic Septotomy (FES):
- Clinical and Technical Success: Both Z-POEM and FES demonstrated high technical success (100%) and clinical success rates (92.8%). Z-POEM showed a reduction in procedure time with experience, highlighting a learning curve. Both methods had comparable safety profiles over a 2-year follow-up, but Z-POEM’s submucosal tunneling technique offered better adaptability to complex cases [21].
- Z-POEM vs. Rigid Endoscopic Stapling (RES):
- Clinical Outcomes: Z-POEM and RES both achieved high clinical success rates, but Z-POEM is more versatile, accommodating various diverticulum sizes and anatomical challenges. RES is quicker but limited by anatomical constraints that Z-POEM overcomes by not requiring rigid diverticuloscope positioning [35].
- Procedure Time and Recovery: RES typically has shorter procedure times than Z-POEM; however, Z-POEM times can improve with experience. Both have similar hospital stays, reflecting their minimally invasive approaches [35].
- Additionally, a multicenter experience found Z-POEM to have a comparable clinical success rate (92.7%) with lower complication rates than flexible septotomy and rigid endoscopy [37].
- Z-POEM vs. Open Surgery:
- Clinical Success and Safety: Z-POEM and open surgery are effective, but Z-POEM has a lower complication rate and quicker recovery. Open surgery remains effective for larger or complex diverticula but has higher risks, such as nerve injury and infections. Z-POEM is favored due to its minimally invasive nature and suitability for high-risk patients [28].
4. Expert Synthesis and Future Directions
Limitations
5. Conclusions
Funding
Institutional Review Board Statement
Acknowledgments
Conflicts of Interest
References
- Yang, J.; Novak, S.; Ujiki, M.; Hernández, Ó.; Desai, P.; Benias, P.; Lee, D.; Chang, K.; Brieau, B.; Barret, M.; et al. An international study on the use of peroral endoscopic myotomy in the management of Zenker’s diverticulum. Gastrointest. Endosc. 2020, 91, 163–168. [Google Scholar] [CrossRef]
- Law, R.; Katzka, D.A.; Baron, T.H. Zenker’s Diverticulum. Clin. Gastroenterol. Hepatol. 2014, 12, 1773–1782. [Google Scholar] [CrossRef]
- Veenker, E.; Cohen, J.I. Current trends in management of Zenker diverticulum. Curr. Opin. Otolaryngol. Head Neck Surg. 2003, 11, 160–165. [Google Scholar] [CrossRef]
- van Overbeek, J.J. Pathogenesis and methods of treatment of Zenker’s diverticulum. Ann. Otol. Rhinol. Laryngol. 2003, 112, 583–593. [Google Scholar] [CrossRef] [PubMed]
- Achkar, E. Zenker’s diverticulum. Dig. Dis. 1998, 16, 144–151. [Google Scholar] [CrossRef]
- Cook, I.J.; Gabb, M.; Panagopoulos, V.; Jamieson, G.G.; Dodds, W.J.; Dent, J.; Shearman, D.J. Pharyngeal (Zenker’s) diverticulum is a disorder of upper esophageal sphincter opening. Gastroenterology 1992, 103, 1229–1235. [Google Scholar] [CrossRef]
- Ferreira, L.; Simmons, D.T.; Baron, T.H. Zenker’s diverticula: Pathophysiology, clinical presentation, and flexible endoscopic management. Dis. Esophagus 2008, 21, 1–8. [Google Scholar] [CrossRef]
- Bhimji, S.T.; Dulebohn, S.C. Zenker Diverticulum. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2025. Available online: https://www.ncbi.nlm.nih.gov/books/NBK499996/ (accessed on 22 June 2025).
- Yuan, Y.; Zhao, Y.F.; Hu, Y.; Chen, L.Q. Surgical treatment of Zenker’s diverticulum. Dig. Surg. 2013, 30, 207–218. [Google Scholar] [CrossRef] [PubMed]
- Greene, C.L.; McFadden, P.M.; Oh, D.S.; Chang, E.J.; Hagen, J.A. Long-term outcome of the treatment of Zenker’s diverticulum. Ann. Thorac. Surg. 2015, 100, 975–978. [Google Scholar] [CrossRef]
- Nuño-Guzmán, C.M.; García-Carrasco, D.; Haro, M.; Arróniz-Jáuregui, J.; Corona, J.L.; Salcido, M. Zenker’s diverticulum: Diagnostic approach and surgical management. Case Rep. Gastroenterol. 2014, 8, 346–352. [Google Scholar] [CrossRef] [PubMed]
- Feeley, M.A.; Righi, P.D.; Weisberger, E.C.; Hamaker, R.C.; Spahn, T.J.; Radpour, S.; Wynne, M.K. Zenker’s diverticulum: Analysis of surgical complications from diverticulectomy and cricopharyngeal myotomy. Laryngoscope 1999, 109, 858–861. [Google Scholar] [CrossRef]
- Zbären, P.; Schär, P.; Tschopp, L. Surgical treatment of Zenker’s diverticulum: Transcutaneous diverticulectomy versus microendoscopic myotomy of the cricopharyngeal muscle with CO2 laser. Otolaryngol. Head Neck Surg. 1999, 121, 482–487. [Google Scholar] [CrossRef] [PubMed]
- Shahawy, S.; Janisiewicz, A.M.; Annino, D.; Shapiro, J. A comparative study of outcomes for endoscopic diverticulotomy versus external diverticulectomy. Otolaryngol. Head. Neck Surg. 2014, 151, 646–651. [Google Scholar] [CrossRef]
- Keck, T.; Rozsasi, A.; Grün, P.M. Surgical treatment of hypopharyngeal diverticulum (Zenker’s diverticulum). Eur. Arch. Otorhinolaryngol. 2010, 267, 587–592. [Google Scholar] [CrossRef]
- Verdonck, J.; Morton, R.P. Systematic review on treatment of Zenker’s diverticulum. Eur. Arch. Otorhinolaryngol. 2015, 272, 3095–3107. [Google Scholar] [CrossRef] [PubMed]
- Witterick, I.J.; Gullane, P.J.; Yeung, E. Outcome analysis of Zenker’s diverticulectomy and cricopharyngeal myotomy. Head. Neck 1995, 17, 382–388. [Google Scholar] [CrossRef]
- Konowitz, P.M.; Biller, H.F. Diverticulopexy and cricopharyngeal myotomy: Treatment for the high-risk patient with a pharyngoesophageal (Zenker’s) diverticulum. Otolaryngol. Head. Neck Surg. 1989, 100, 146–153. [Google Scholar] [CrossRef]
- Colombo-Benkmann, M.; Unruh, V.; Krieglstein, C.; Senninger, N. Cricopharyngeal myotomy in the treatment of Zenker’s diverticulum. J. Am. Coll. Surg. 2003, 196, 370–377. [Google Scholar] [CrossRef] [PubMed]
- Tsuchiya, Y.; Suzuki, S.; Sakaguchi, T.; Kojima, Y.; Okamoto, K.; Kurachi, K.; Konno, H.; Baba, S.; Nakamura, S. Lymphoepithelial Cyst of the Pancreas: Report of a Case. Surg. Today 2000, 30, 856–860. [Google Scholar] [CrossRef]
- Swei, E.; Pokala, S.K.; Menard-Katcher, P.; Wagh, M.S. Comparison of Zenker’s per-oral endoscopic myotomy (Z-POEM) with standard flexible endoscopic septotomy for Zenker’s diverticulum: A prospective study with 2-year follow-up. Surgical Endoscopy. Surg. Endosc. 2023, 37, 6818–6823. [Google Scholar] [CrossRef] [PubMed]
- Dell’Anna, G.; Fasulo, E.; Fanizza, J.; Barà, R.; Vespa, E.; Barchi, A.; Cecinato, P.; Fuccio, L.; Annese, V.; Malesci, A.; et al. The endoscopic management of Zenker’s diverticulum: A comprehensive review. Diagnostics 2023, 14, 2155. [Google Scholar] [CrossRef]
- Hillel, A.T.; Flint, P.W. Evolution of endoscopic surgical therapy for Zenker’s diverticulum. Laryngoscope 2009, 119, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Koch, M.; Mantsopoulos, K.; Velegrakis, S.; Iro, H.; Zenk, J. Endoscopic laser-assisted diverticulotomy versus open surgical approach in the treatment of Zenker’s diverticulum. Laryngoscope 2011, 121, 2090–2094. [Google Scholar] [CrossRef] [PubMed]
- Avasarala, J. Inadequacy of clinical trial designs and data to control for the confounding impact of race/ethnicity in response to treatment in multiple sclerosis. JAMA Neurol. 2014, 71, 943–944. [Google Scholar] [CrossRef] [PubMed]
- Restrepo-Rodas, G.; Barajas-Gamboa, J.S.; Dang, J.T.; Piechowska-Jóźwiak, M.I.; Khan, M.; Diaz Del Gobbo, G.; Abdallah, M.; Moreno, C.; Abril, C.; Pantoja, J.P.; et al. Seven-Year Experience of Intramural Surgery in the Middle East: A Safety and Feasibility Analysis. J. Clin. Med. 2024, 13, 3989. [Google Scholar] [CrossRef]
- Zhang, L.Y.; Hernández-Mondragón, O.; Pioche, M.; Steinway, S.N.; Nieto, J.; Ujiki, M.B.; VanDruff, V.N.; Kim, R.E.; Canakis, A.; Tantau, M.; et al. Zenker’s peroral endoscopic myotomy for management of large Zenker’s diverticulum. Endoscopy 2023, 55, 501–507. [Google Scholar] [CrossRef]
- Norton, B.; Siggens, K.; Papaefthymiou, A.; Telese, A.; Duku, M.; Murino, A.; Johnson, G.; Murray, C.; Mohammadi, B.; Mughal, M.; et al. The safety and efficacy of endoscopic approaches for the management of Zenker’s diverticulum: A multicentre retrospective study. Surg. Endosc. 2024, 38, 5842–5850. [Google Scholar] [CrossRef]
- Perbtani, Y.B.; Mramba, L.K.; Yang, D.; Suarez, J.; Draganov, P.V. Life after per-oral endoscopic myotomy: Long-term outcomes of quality of life and their association with Eckardt scores. Gastrointest. Endosc. 2018, 87, 1415–1420.e1. [Google Scholar] [CrossRef]
- Montali, A.; Reverberi, V.; Pelagatti, A.; Vecchi, A.; Rossi, M.; Doselli, S.; Farina, B.; Olivani, A.; Economopoulos, G.; Dalla Valle, R.; et al. Metabolic and Functional Characterization of CD8+ T-Cell Subpopulations in Hepatocellular Carcinoma: Implications of Tumor Microenvironment on T-Cell Dysfunction. Dig. Liver Dis. 2025, 57, S1–S2. [Google Scholar] [CrossRef]
- Shapiro, J.M.; Suarez, M.G.; Turner, T.L. Cracking the clinician educator code in gastroenterology. Clin. Gastroenterol. Hepatol. 2017, 15, 1828–1832. [Google Scholar] [CrossRef]
- Kurian, A.A.; Dunst, C.M.; Sharata, A.; Bhayani, N.H.; Reavis, K.M.; Swanström, L.L. Peroral endoscopic esophageal myotomy: Defining the learning curve. Gastrointest. Endosc. 2013, 77, 719–725. [Google Scholar] [CrossRef]
- Puli, S.R.; Wagh, M.S.; Forcione, D.; Gopakumar, H. Learning curve for esophageal peroral endoscopic myotomy: A systematic review and meta-analysis. Endoscopy 2023, 55, 355–360. [Google Scholar] [CrossRef]
- Kahaleh, M.; Tyberg, A.; Suresh, S.; Lambroza, A.; Casas, F.R.; Rey, M.; Nieto, J.; Martínez, G.M.; Zamarripa, F.; Arantes, V.; et al. The learning curve for peroral endoscopic myotomy in Latin America: A slide to the right? Clin. Endosc. 2021, 54, 701–705. [Google Scholar] [CrossRef]
- Cerchione, R.; Parise, P.; Olivari, G.; Cossu, A.; Barbieri, L.; Palucci, M.; Cinelli, L.; Puccetti, F.; Rosati, R. Endoscopic management of Zenker’s diverticulum: Stapling vs. Z-POEM. Shanghai Chest 2020, 4, 43. [Google Scholar] [CrossRef]
- Che, S.Y.W.; Joseph, S.; Kuchta, K.; Amundson, J.R.; VanDruff, V.N.; Ishii, S.; Zimmermann, C.J.; Hedberg, H.M.; Ujiki, M.B. Outcomes after per-oral endoscopic myotomy for Zenker’s diverticula (Z-POEM) and correlation with impedance planimetry (FLIP). Surg. Endosc. 2024, 38, 957–963. [Google Scholar] [CrossRef] [PubMed]
- Al Ghamdi, S.S.; Farha, J.; Moran, R.A.; Pioche, M.; Moll, F.; Yang, D.J.; Mondragón, O.V.H.; Ujiki, M.; Wong, H.; Tantau, A.; et al. Zenker’s peroral endoscopic myotomy, or flexible or rigid septotomy for Zenker’s diverticulum: A multicenter retrospective comparison. Endoscopy 2022, 54, 345–351. [Google Scholar] [CrossRef] [PubMed]
- Steinway, S.; Zhang, L.; Amundson, J.; Nieto, J.; Desai, P.; Jacques, J.; Bejjani, M.; Pioche, M.; Kumta, N.; Hernández-Mondragón, O.; et al. Long-term outcomes of Zenker’s peroral endoscopic myotomy (Z-POEM) for treatment of Zenker’s diverticulum: An international multicenter study. Endosc. Int. Open 2023, 11, E607–E612. [Google Scholar] [CrossRef]
| Treatment Approach | Indications | Advantages | Disadvantages | Potential Complications |
|---|---|---|---|---|
| Flexible Endoscopic Techniques (Z-POEM) | - Broad range of patients, including those not suited for rigid endoscopy or general anesthesia. - Complex anatomy or larger diverticula. - High-risk patients needing minimally invasive treatment. | - Minimally invasive, often performed under conscious sedation. - Suitable for outpatient procedures. - High clinical success rate (~92%). - Reduced risk of infection and bleeding due to precision. | - Technically challenging, requires advanced endoscopic skills and specialized equipment. - Limited availability to specialized centers. - Long-term efficacy data still evolving. | - Incomplete myotomy or submucosal fibrosis. - Recurrence of symptoms. - Potential for difficulty in future interventions due to fibrosis. |
| Rigid Endoscopic Stapling | - Patients with favorable neck anatomy and good mobility. - Moderate-sized diverticula. - Patients who are poor candidates for open surgery. | - Minimally invasive compared to open surgery. - Shorter hospital stays. - Symptom resolution in ~90% of cases. - Lower risk of major complications than open surgery. | - Limited by anatomical factors (e.g., poor neck extension or significant dental issues). - Requires general anesthesia. | - Dental injury. - Perforation. - Incomplete septotomy, particularly in smaller or deeper diverticula. |
| Open Surgery (Diverticulectomy, Diverticulopexy) | - Large or complex diverticula. - Not suitable for endoscopic treatment. - Symptomatic patients with significant comorbidities. | - Highly effective for large/complex diverticula. - Symptom resolution in 90–95% of cases. - Precise management of the diverticulum. | - Higher morbidity than endoscopic techniques. - Longer recovery time. - Requires general anesthesia. - Not ideal for frail or elderly patients. | - Nerve injury (recurrent laryngeal nerve), infection, fistula, hematoma. - Longer operative and recovery times. |
| Conservative Management | - Asymptomatic patients or diverticula < 1 cm. - Regular monitoring, treating symptoms only if they arise or progress. | - Non-invasive, avoids unnecessary intervention. - Low risk. | - Requires continuous monitoring. - May miss progression of symptoms until severe. | - No immediate complications, but risk of diverticulum enlargement or symptom worsening. |
| Technique | Operative Time | Recovery Time |
|---|---|---|
| Rigid Endoscopic Stapling | Typically, 30–60 min | Shorter recovery time than open surgery, usually 1–2 days in hospital, with faster return to normal activities. |
| Z-POEM (Flexible Endoscopy) | Typically, 45–90 min (can vary based on complexity) | Very short recovery time, often performed as an outpatient procedure with same-day discharge or 1-day hospital stay. |
| Open Surgery | Typically, 1–2 h | Longer recovery time, with hospital stays of 3–7 days and a few weeks for full recovery. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ramamurthy, S.; Ahuja, P.; Dahiya, D.S.; Hayat, U.; Ahuja, N.; Bharadwaj, H.R.; Gangwani, M.K.; Inamdar, S. Management Strategies for Zenker’s Diverticulum: A Comprehensive Review. J. Clin. Med. 2025, 14, 6141. https://doi.org/10.3390/jcm14176141
Ramamurthy S, Ahuja P, Dahiya DS, Hayat U, Ahuja N, Bharadwaj HR, Gangwani MK, Inamdar S. Management Strategies for Zenker’s Diverticulum: A Comprehensive Review. Journal of Clinical Medicine. 2025; 14(17):6141. https://doi.org/10.3390/jcm14176141
Chicago/Turabian StyleRamamurthy, Suhaas, Priyanka Ahuja, Dushyant Singh Dahiya, Umar Hayat, Neha Ahuja, Hareesha Rishab Bharadwaj, Manesh Kumar Gangwani, and Sumant Inamdar. 2025. "Management Strategies for Zenker’s Diverticulum: A Comprehensive Review" Journal of Clinical Medicine 14, no. 17: 6141. https://doi.org/10.3390/jcm14176141
APA StyleRamamurthy, S., Ahuja, P., Dahiya, D. S., Hayat, U., Ahuja, N., Bharadwaj, H. R., Gangwani, M. K., & Inamdar, S. (2025). Management Strategies for Zenker’s Diverticulum: A Comprehensive Review. Journal of Clinical Medicine, 14(17), 6141. https://doi.org/10.3390/jcm14176141







