Cervical Regeneration Following Monopolar Electrosurgical Conization: A Prospective Evaluation of Volume, Length, and Transformation Zone Reformation
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Papoutsis, D.; Rodolakis, A.; Mesogitis, S.; Sotiropoulou, M.; Antsaklis, A. Regeneration of uterine cervix at 6 months after large loop excision of the transformation zone for cervical intraepithelial neoplasia. BJOG Int. J. Obstet. Gynaecol. 2012, 119, 678–684. [Google Scholar] [CrossRef]
- MacLean, A.B. Healing of cervical epithelium after laser treatment of cervical intraepithelial neoplasia. BJOG Int. J. Obstet. Gynaecol. 1984, 91, 697–706. [Google Scholar] [CrossRef] [PubMed]
- Perkins, R.B.; Guido, R.S.; Castle, P.E.; Chelmow, D.; Einstein, M.H.; Garcia, F.; Huh, W.K.; Kim, J.J.; Moscicki, A.-B.; Nayar, R. 2019 ASCCP risk-based management consensus guidelines: Updates through 2023. J. Low. Genit. Tract Dis. 2024, 28, 3–6. [Google Scholar] [CrossRef] [PubMed]
- Isono, W.; Tsuchiya, A.; Okamura, A.; Honda, M.; Saito, A.; Tsuchiya, H.; Matsuyama, R.; Fujimoto, A.; Nishii, O. Effectiveness of Oxidized Regenerated Cellulose-Based Haemostat (Surgicel®) for Monopolar Electrosurgical Conization and Its Risk Factors for Postoperative Rebleeding: An Observational Study. Clin. Exp. Obstet. Gynecol. 2022, 49, 208. [Google Scholar] [CrossRef]
- Ding, J.; Xu, H.; Xia, L.; Cao, S.; Wu, Q. Comparison of monopolar electrosurgical conization and the loop electrosurgical excision procedure in the management of high-grade squamous intraepithelial lesion. Front. Surg. 2021, 8, 721545. [Google Scholar] [CrossRef]
- Bostofte, E.; Berget, A.; Larsen, J.F.; Pedersen, P.H.; Rank, F. Conization by carbon dioxide laser or cold knife in the treatment of cervical intra-epithelial neoplasia. Acta Obstet. Gynecol. Scand. 1986, 65, 199–202. [Google Scholar] [CrossRef]
- Song, T.; Seong, S.J.; Kim, B.-G. Regeneration process after cervical conization for cervical intraepithelial neoplasia. Obstet. Gynecol. 2016, 128, 1258–1264. [Google Scholar] [CrossRef]
- Ciavattini, A.; Carpini, G.D.; Moriconi, L.; Clemente, N.; Montik, N.; De Vincenzo, R.; Del Fabro, A.; Buttignol, M.; Ricci, C.; Moro, F. Effect of age and cone dimensions on cervical regeneration: An Italian multicentric prospective observational study. BMJ Open 2018, 8, e020675. [Google Scholar] [CrossRef]
- Paraskevaidis, E.; Bilirakis, E.; Koliopoulos, G.; Lolis, E.D.; Kalantaridou, S.; Paschopoulos, M.; Plachouras, N.; Malamou-Mitsi, V.; Kitchener, H.C. Cervical regeneration after diathermy excision of cervical intraepithelial neoplasia as assessed by transvaginal sonography. Eur. J. Obstet. Gynecol. Reprod. Biol. 2002, 102, 88–91. [Google Scholar] [CrossRef]
- Kyrgiou, M.; Athanasiou, A.; Arbyn, M.; Lax, S.F.; Raspollini, M.R.; Nieminen, P.; Carcopino, X.; Bornstein, J.; Gultekin, M.; Paraskevaidis, E. Terminology for cone dimensions after local conservative treatment for cervical intraepithelial neoplasia and early invasive cervical cancer: 2022 consensus recommendations from ESGO, EFC, IFCPC, and ESP. Lancet Oncol. 2022, 23, e385–e392. [Google Scholar] [CrossRef]
- Wang, X.; Li, L.; Bi, Y.; Wu, H.; Wu, M.; Lang, J. The effects of different instruments and suture methods of conization for cervical lesions. Sci. Rep. 2019, 9, 19114. [Google Scholar] [CrossRef]
- Castanon, A.; Landy, R.; Brocklehurst, P.; Evans, H.; Peebles, D.; Singh, N.; Walker, P.; Patnick, J.; Sasieni, P. Risk of preterm delivery with increasing depth of excision for cervical intraepithelial neoplasia in England: Nested case-control study. BMJ 2014, 349, g6223. [Google Scholar] [CrossRef]
- Founta, C.; Arbyn, M.; Valasoulis, G.; Kyrgiou, M.; Tsili, A.; Martin-Hirsch, P.; Dalkalitsis, N.; Karakitsos, P.; Kassanos, D.; Prendiville, W. Proportion of excision and cervical healing after large loop excision of the transformation zone for cervical intraepithelial neoplasia. BJOG Int. J. Obstet. Gynaecol. 2010, 117, 1468–1474. [Google Scholar] [CrossRef]
- Pinto, V.; Dellino, M.; Santarsiero, C.M.; Cormio, G.; Loizzi, V.; Griseta, V.; Vimercati, A.; Cazzato, G.; Cascardi, E.; Cicinelli, E. Ultrasound control of cervical regeneration after large loop excision of the transformation zone: Results of an innovative measurement technique. Diagnostics 2023, 13, 791. [Google Scholar] [CrossRef]
- Lūse, L.; Urtāne, A.Ķ.; Lisovaja, I.; Jermakova, I.; Donders, G.G.; Vedmedovska, N. Literature Review of Cervical Regeneration after Loop Electrosurgical Excision Procedure, and Study Project (CeVaLEP) Proposal. J. Clin. Med. 2022, 11, 2096. [Google Scholar] [CrossRef] [PubMed]
- Gentry, D.J.; Baggish, M.S.; Brady, K.; Walsh, P.M.; Hungler, M.S. The effects of loop excision of the transformation zone on cervical length: Implications for pregnancy. Am. J. Obstet. Gynecol. 2000, 182, 516–520. [Google Scholar] [CrossRef] [PubMed]
- Dückelmann, A.M.; Wordell, J.; Richter, R.; Sehouli, J. 3D ultrasound as a surgical quality control of conization in patients with severe dysplasia: A prospective study. Arch. Gynecol. Obstet. 2020, 302, 1189–1196. [Google Scholar] [CrossRef]
- Sharp, G.; Cordiner, J.; Murray, E.L.; More, I. Healing of cervical epithelium after laser ablation of cervical intraepithelial neoplasia. J. Clin. Pathol. 1984, 37, 611–615. [Google Scholar] [CrossRef]
- Kashimura, M. Reparative process of benign erosion of the uterine cervix following cryosurgery. Gynecol. Oncol. 1980, 9, 334–350. [Google Scholar] [CrossRef] [PubMed]
- Miyako, J.; Iwanari, O.; Kitao, M. Studies on repair of the uterine cervix after CO2 laser conization with anti-keratin monoclonal antibodies. Gynecol. Obstet. Investig. 1993, 35, 179–184. [Google Scholar] [CrossRef]
- Prendiville, W.; Sankaranarayanan, R. Colposcopy and Treatment of Cervical Precancer; International Agency for Research on Cancer, World Health Organization: Lyon, France, 2017. [Google Scholar]
- Anderson, M.; Hartley, R. Cervical crypt involvement by intraepithelial neoplasia. Obstet. Gynecol. 1980, 55, 546–550. [Google Scholar] [CrossRef] [PubMed]
- Panna, S.; Luanratanakorn, S. Positive margin prevalence and risk factors with cervical specimens obtained from loop electrosurgical excision procedures and cold knife conization. Asian Pac. J. Cancer Prev. 2009, 10, 637–640. [Google Scholar] [PubMed]
| Variable | n = 28 |
|---|---|
| Age (years), Mean ± SD | 43.57 ± 9.14 |
| Cytology Indications, n (%) | |
| • LSIL | 4 (14.8%) |
| • HSIL | 19 (70.4%) |
| • ASC-H | 4 (14.8%) |
| Histology Indications, n (%) | |
| • CIN1 | 4 (36.4%) |
| • CIN2–3 | 7 (63.6%) |
| Conization Pathology, n (%) | |
| • CIN1 | 13 (46.4%) |
| • CIN2–3 | 11 (39.3%) |
| • Chronic cervicitis | 4 (14.3%) |
| Parity, n (%) | |
| • Nulliparous | 1 (3.6%) |
| • Multiparous | 27 (96.4%) |
| HPV Status, n (%) | |
| • Low-risk | 1 (5.6%) |
| • High-risk | 17 (94.4%) |
| Diabetes Mellitus, n (%) | |
| • No | 27 (96.4%) |
| • Yes | 1 (3.6%) |
| Smoking Status, n (%) | |
| • Non-smoker | 22 (78.6%) |
| • Smoker | 6 (21.4%) |
| 3. month Biopsy, n (%) | |
| • TZ negative | 19 (67.9%) |
| • TZ positive | 9 (32.1%) |
| 6. month Cytology-TZ Status, n (%) | |
| • TZ negative | 6 (20.7%) |
| • TZ positive | 22 (75.9%) |
| 6. month Cytology Results, n (%) | |
| • NILM | 25 (86.2%) |
| • ASC-US | 1 (3.4%) |
| • LSIL | 2 (6.9%) |
| Post-MESC Surgical Margin, n (%) | |
| • Negative | 27 (93.1%) |
| • Positive | 1 (3.4%) |
| Variable | Mean ± SD |
|---|---|
| Preoperative cervical dimensions | |
| Cervical volume (cm3) | 34.09 ± 3.35 |
| Cervical length (mm) | 33.77 ± 3.13 |
| Excised cone dimensions | |
| Cone volume (cm3) | 2.75 ± 1.08 |
| Cone length (mm) | 13.24 ± 3.10 |
| Proportion Excised | |
| Proportion of volume excised (%) | 8.45 ± 4.10 |
| Proportion of length excised (%) | 40.31 ± 12.87 |
| Volume regeneration (%) | 84.61 ± 5.64 |
| Length regeneration (%) | 86.36 ± 3.33 |
| Variable | Preoperative | 1. Month | 6. Month | p-Value |
|---|---|---|---|---|
| Cervical volume (cm3) | 34.09 ± 3.35 | 31.34 ± 4.42 | 33.61 ± 3.67 | <0.001 |
| % of baseline volume | 100 | 91.55 ± 4.10 | 98.48 ± 1.15 | <0.001 |
| Deficit volume (cm3) | 0 | 2.75 ± 1.08 | 0.48 ± 0.32 | <0.001 |
| Cervical length (mm) | 33.77 ± 3.13 | 20.53 ± 6.17 | 31.86 ± 3.98 | <0.001 |
| % of baseline length | 100 | 59.69 ± 12.87 | 94.09 ± 3.26 | <0.001 |
| Deficit length (mm) | 0 | 13.24 ± 3.1 | 1.90 ± 0.89 | <0.001 |
| Variables | r (Volume Regeneration) | p-Value | r (Length Regeneration) | p-Value |
|---|---|---|---|---|
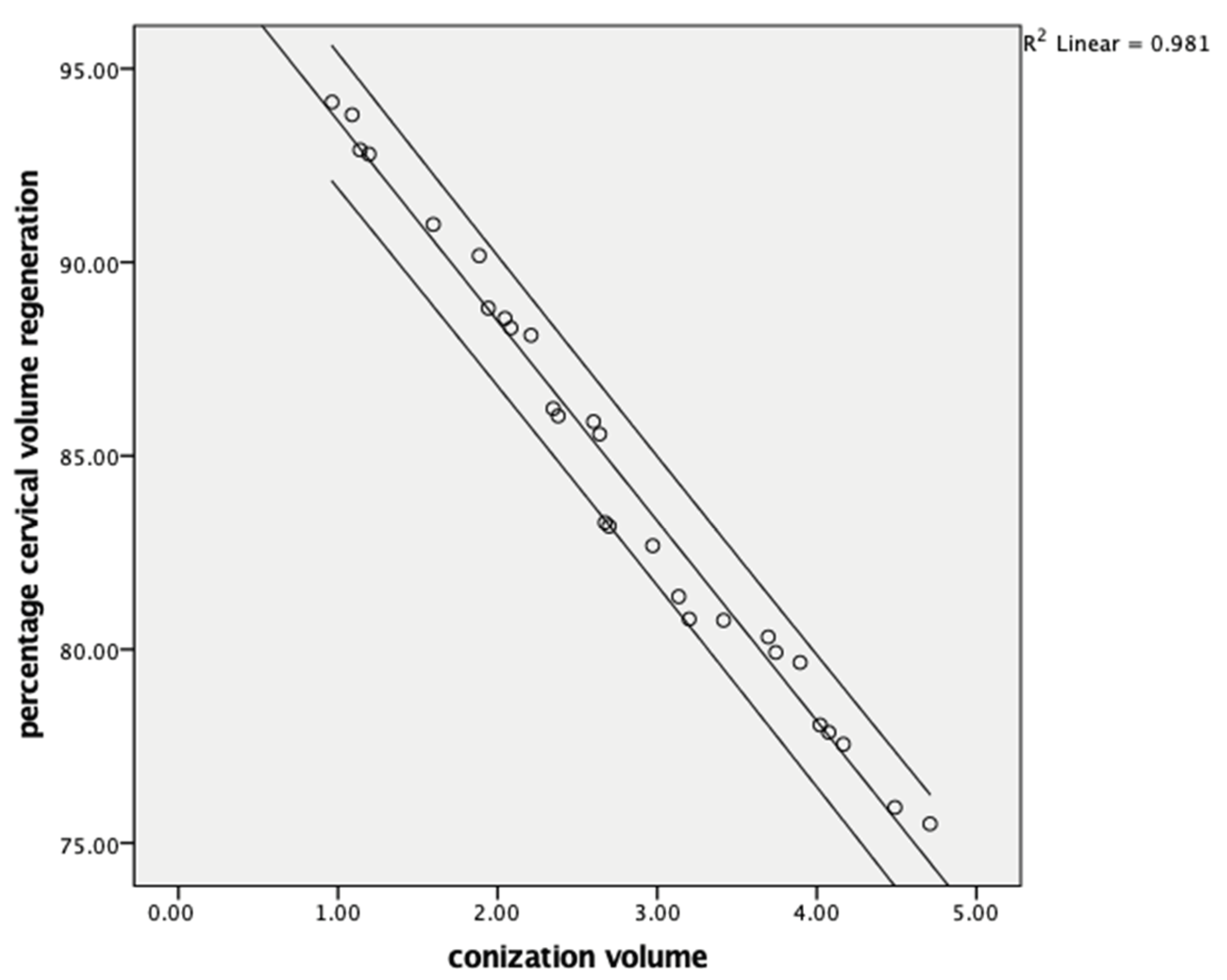
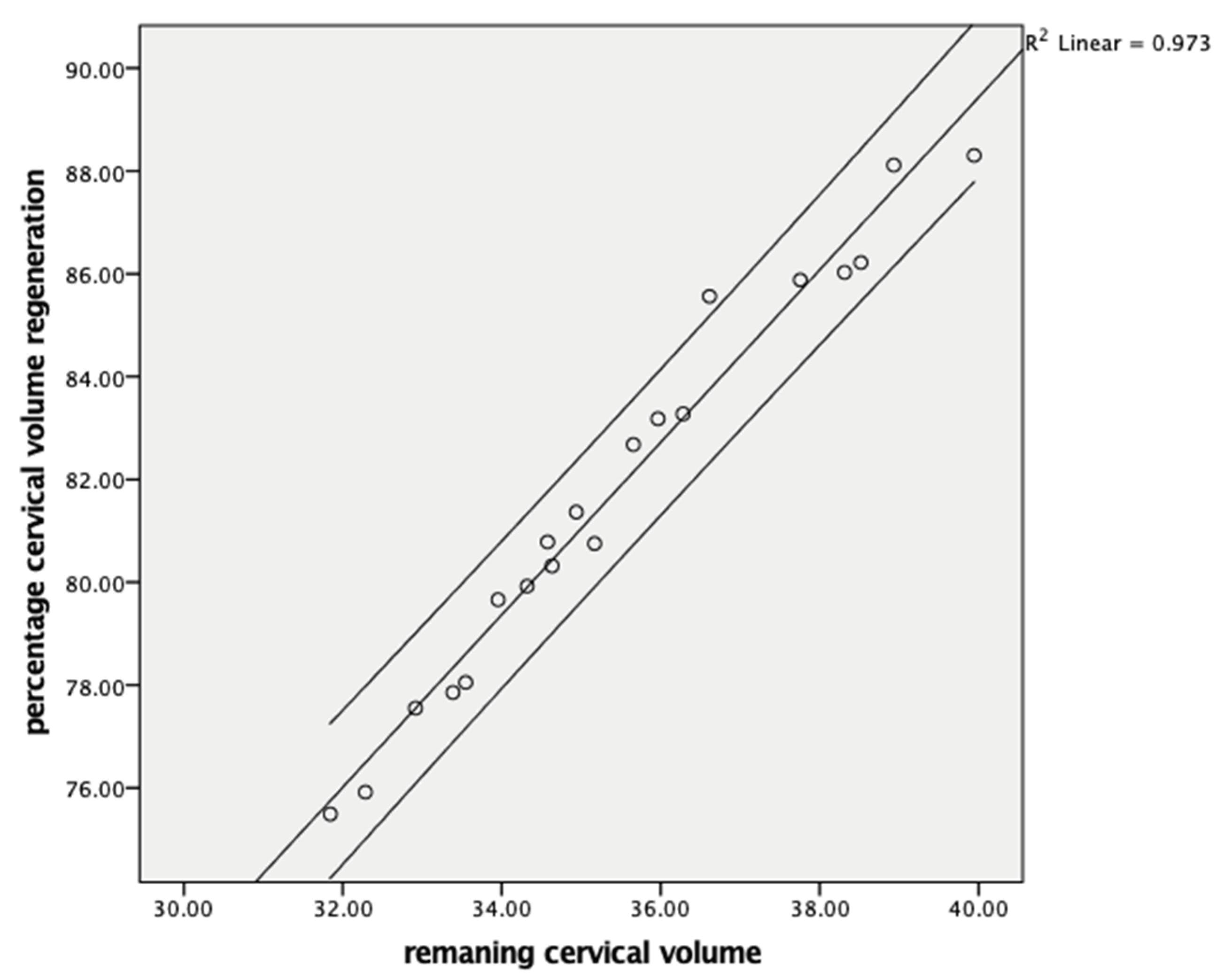
| Cone volume (cm3) | −0.990 | <0.001 | ||
| Remaining cervical volume (post. MESC at 1. month) | 0.998 | <0.001 | ||
| Cone length (cm) | −0.977 | <0.001 | ||
| Remaining cervical length (post. MESC at 1. month) | 0.473 | 0.018 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gül Aydın, Ş.; Baş, S.; Özmen, F.; Yaşar, Ş.; Taş, Z.A.; Nessar, A.Z.; Seyfettinoğlu, S.; Narin, M.A. Cervical Regeneration Following Monopolar Electrosurgical Conization: A Prospective Evaluation of Volume, Length, and Transformation Zone Reformation. J. Clin. Med. 2025, 14, 5918. https://doi.org/10.3390/jcm14165918
Gül Aydın Ş, Baş S, Özmen F, Yaşar Ş, Taş ZA, Nessar AZ, Seyfettinoğlu S, Narin MA. Cervical Regeneration Following Monopolar Electrosurgical Conization: A Prospective Evaluation of Volume, Length, and Transformation Zone Reformation. Journal of Clinical Medicine. 2025; 14(16):5918. https://doi.org/10.3390/jcm14165918
Chicago/Turabian StyleGül Aydın, Şule, Sevda Baş, Fatma Özmen, Şeyma Yaşar, Zeynel Abidin Taş, Ahmet Zeki Nessar, Sevtap Seyfettinoğlu, and Mehmet Ali Narin. 2025. "Cervical Regeneration Following Monopolar Electrosurgical Conization: A Prospective Evaluation of Volume, Length, and Transformation Zone Reformation" Journal of Clinical Medicine 14, no. 16: 5918. https://doi.org/10.3390/jcm14165918
APA StyleGül Aydın, Ş., Baş, S., Özmen, F., Yaşar, Ş., Taş, Z. A., Nessar, A. Z., Seyfettinoğlu, S., & Narin, M. A. (2025). Cervical Regeneration Following Monopolar Electrosurgical Conization: A Prospective Evaluation of Volume, Length, and Transformation Zone Reformation. Journal of Clinical Medicine, 14(16), 5918. https://doi.org/10.3390/jcm14165918







