Reporting of Magnetic Resonance Enterography in Inflammatory Bowel Disease: Results of an Italian Survey
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Procedures
3. Results
3.1. General Questions, Experience in IBD, Characteristics of the Centers
3.2. Reporting Details
3.3. Structured Report, Scores of Disease Activity, and Multidisciplinary Meetings
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Roda, G.; Chien Ng, S.; Kotze, P.G.; Argollo, M.; Panaccione, R.; Spinelli, A.; Kaser, A.; Peyrin-Biroulet, L.; Danese, S. Crohn’s Disease. Nat. Rev. Dis. Primers 2020, 6, 22. [Google Scholar] [CrossRef] [PubMed]
- Alatab, S.; Sepanlou, S.G.; Ikuta, K.; Vahedi, H.; Bisignano, C.; Safiri, S.; Sadeghi, A.; Nixon, M.R.; Abdoli, A.; Abolhassani, H.; et al. The Global, Regional, and National Burden of Inflammatory Bowel Disease in 195 Countries and Territories, 1990–2017: A Systematic Analysis for the Global Burden of Disease Study 2017. Lancet Gastroenterol. Hepatol. 2020, 5, 17–30. [Google Scholar] [CrossRef] [PubMed]
- Torres, J.; Bonovas, S.; Doherty, G.; Kucharzik, T.; Gisbert, J.P.; Raine, T.; Adamina, M.; Armuzzi, A.; Bachmann, O.; Bager, P.; et al. ECCO Guidelines on Therapeutics in Crohn’s Disease: Medical Treatment. J. Crohn’s Colitis 2020, 14, 4–22. [Google Scholar] [CrossRef] [PubMed]
- Turner, D.; Ricciuto, A.; Lewis, A.; D’Amico, F.; Dhaliwal, J.; Griffiths, A.M.; Bettenworth, D.; Sandborn, W.J.; Sands, B.E.; Reinisch, W.; et al. STRIDE-II: An Update on the Selecting Therapeutic Targets in Inflammatory Bowel Disease (STRIDE) Initiative of the International Organization for the Study of IBD (IOIBD): Determining Therapeutic Goals for Treat-to-Target Strategies in IBD. Gastroenterology 2021, 160, 1570–1583. [Google Scholar] [CrossRef] [PubMed]
- Bettenworth, D.; Bokemeyer, A.; Baker, M.; Mao, R.; Parker, C.E.; Nguyen, T.; Ma, C.; Panés, J.; Rimola, J.; Fletcher, J.G.; et al. Assessment of Crohn’s Disease-Associated Small Bowel Strictures and Fibrosis on Cross-Sectional Imaging: A Systematic Review. Gut 2019, 68, 1115–1126. [Google Scholar] [CrossRef] [PubMed]
- Rimola, J.; Torres, J.; Kumar, S.; Taylor, S.A.; Kucharzik, T. Recent Advances in Clinical Practice: Advances in Cross-Sectional Imaging in Inflammatory Bowel Disease. Gut 2022, 71, 2587–2597. [Google Scholar] [CrossRef]
- Panés, J.; Bouzas, R.; Chaparro, M.; García-Sánchez, V.; Gisbert, J.P.; Martínez De Guereñu, B.; Mendoza, J.L.; Paredes, J.M.; Quiroga, S.; Ripollés, T.; et al. Systematic Review: The Use of Ultrasonography, Computed Tomography and Magnetic Resonance Imaging for the Diagnosis, Assessment of Activity and Abdominal Complications of Crohn’s Disease. Aliment. Pharmacol. Ther. 2011, 34, 125–145. [Google Scholar] [CrossRef]
- Fernandes, S.R.; Serrazina, J.; Botto, I.A.; Leal, T.; Guimarães, A.; Garcia, J.L.; Rosa, I.; Prata, R.; Carvalho, D.; Neves, J.; et al. Transmural Remission Improves Clinical Outcomes up to 5 Years in Crohn’s Disease. United Eur. Gastroenterol. J. 2023, 11, 51–59. [Google Scholar] [CrossRef]
- Deepak, P.; Fletcher, J.G.; Fidler, J.L.; Barlow, J.M.; Sheedy, S.P.; Kolbe, A.B.; Harmsen, W.S.; Loftus, E.V.; Hansel, S.L.; Becker, B.D.; et al. Radiological Response Is Associated With Better Long-Term Outcomes and Is a Potential Treatment Target in Patients With Small Bowel Crohn’s Disease. Am. J. Gastroenterol. 2016, 111, 997–1006. [Google Scholar] [CrossRef]
- Castiglione, F.; Imperatore, N.; Testa, A.; De Palma, G.D.; Nardone, O.M.; Pellegrini, L.; Caporaso, N.; Rispo, A. One-Year Clinical Outcomes with Biologics in Crohn’s Disease: Transmural Healing Compared with Mucosal or No Healing. Aliment. Pharmacol. Ther. 2019, 49, 1026–1039. [Google Scholar] [CrossRef]
- Bruining, D.H.; Zimmermann, E.M.; Loftus, E.V.; Sandborn, W.J.; Sauer, C.G.; Strong, S.A.; Fletcher, J.G. Consensus Recommendations for Evaluation, Interpretation, and Utilization of Computed Tomography and Magnetic Resonance Enterography in Patients With Small Bowel Crohn’s Disease. Radiology 2018, 286, 776–799. [Google Scholar] [CrossRef]
- Maaser, C.; Sturm, A.; Vavricka, S.R.; Kucharzik, T.; Fiorino, G.; Annese, V.; Calabrese, E.; Baumgart, D.C.; Bettenworth, D.; Borralho Nunes, P.; et al. ECCO-ESGAR Guideline for Diagnostic Assessment in IBD Part 1: Initial Diagnosis, Monitoring of Known IBD, Detection of Complications. J. Crohns Colitis 2019, 13, 144–164. [Google Scholar] [CrossRef]
- Sturm, A.; Maaser, C.; Calabrese, E.; Annese, V.; Fiorino, G.; Kucharzik, T.; Vavricka, S.R.; Verstockt, B.; Van Rheenen, P.; Tolan, D.; et al. ECCO-ESGAR Guideline for Diagnostic Assessment in IBD Part 2: IBD Scores and General Principles and Technical Aspects. J. Crohns Colitis 2019, 13, 273–284E. [Google Scholar] [CrossRef]
- Deepak, P.; Axelrad, J.E.; Ananthakrishnan, A.N. The Role of the Radiologist in Determining Disease Severity in Inflammatory Bowel Diseases. Gastrointest. Endosc. Clin. N. Am. 2019, 29, 447–470. [Google Scholar] [CrossRef]
- Buisson, A.; Pereira, B.; Goutte, M.; Reymond, M.; Allimant, C.; Obritin-Guilhen, H.; Bommelaer, G.; Hordonneau, C. Magnetic resonance index of activity (MaRIA) and Clermont score are highly and equally effective MRI indices in detecting mucosal healing in Crohn’s disease. Dig. Liver Dis. 2017, 49, 1211–1217. [Google Scholar] [CrossRef]
- Ordás, I.; Rimola, J.; Rodríguez, S.; Paredes, J.M.; Martínez-Pérez, M.J.; Blanc, E.; Arévalo, J.A.; Aduna, M.; Andreu, M.; Radosevic, A.; et al. Accuracy of Magnetic Resonance Enterography in Assessing Response to Therapy and Mucosal Healing in Patients with Crohn’s Disease. Gastroenterology 2014, 146, 374–382.e1. [Google Scholar] [CrossRef]
- Park, S.H.; Park, S.H. Simplified Magnetic Resonance Index of Activity for Crohn’s Disease—Let’s Try to Kick It Up a Notch. Gastroenterology 2020, 158, 281–282.e1. [Google Scholar] [CrossRef]
- Williet, N.; Jardin, S.; Roblin, X. The Simplified Magnetic Resonance Index of Activity (MARIA) for Crohn’s Disease Is Strongly Correlated with the MARIA and Clermont Score: An External Validation. Gastroenterology 2020, 158, 282–283. [Google Scholar] [CrossRef]
- Roseira, J.; Ventosa, A.R.; de Sousa, H.T.; Brito, J. The New Simplified MARIA Score Applies beyond Clinical Trials: A Suitable Clinical Practice Tool for Crohn’s Disease That Parallels a Simple Endoscopic Index and Fecal Calprotectin. United Eur. Gastroenterol. J. 2020, 8, 1208–1216. [Google Scholar] [CrossRef]
- Ferman, M.; Lim, A.H.; Hossain, M.; Siow, G.W.; Andrews, J.M. Multidisciplinary Team Meetings Appear to Be Effective in Inflammatory Bowel Disease Management: An Audit of Process and Outcomes. Intern. Med. J. 2018, 48, 1102–1108. [Google Scholar] [CrossRef]
- Fiorino, G.; Lytras, T.; Younge, L.; Fidalgo, C.; Coenen, S.; Chaparro, M.; Allocca, M.; Arnott, I.; Bossuyt, P.; Burisch, J.; et al. Quality of Care Standards in Inflammatory Bowel Diseases: A European Crohn’s and Colitis Organisation [ECCO] Position Paper. J. Crohn’s Colitis 2020, 14, 1037–1048. [Google Scholar] [CrossRef] [PubMed]
- “Role of Radiology in a Multidisciplinary Approach to Patient Care”: Summary of the ESR International Forum 2022|Enhanced Reader. Available online: https://insightsimaging.springeropen.com/articles/10.1186/s13244-023-01377-x (accessed on 12 December 2023).
- Gandhi, N.S.; Dillman, J.R.; Grand, D.J.; Huang, C.; Fletcher, J.G.; Al-Hawary, M.M.; Anupindi, S.A.; Baker, M.E.; Bruining, D.H.; Chatterji, M.; et al. Computed tomography and magnetic resonance enterography protocols and techniques: Survey of the Society of Abdominal Radiology Crohn’s Disease Disease-Focused Panel. Abdom. Radiol. 2020, 45, 1011–1017. [Google Scholar] [CrossRef] [PubMed]
- Fiorino, G.; Bonifacio, C.; Padrenostro, M.; Mrakic Sposta, F.; Spinelli, A.; Malesci, A.; Balzarini, L.; Peyrin-Biroulet, L.; Danese, S. Comparison Between 1.5 and 3.0 Tesla Magnetic Resonance Enterography for the Assessment of Disease Activity and Complications in Ileo-Colonic Crohn’s Disease. Dig. Dis. Sci. 2013, 58, 3246–3255. [Google Scholar] [CrossRef]
| Q1 | Where do you work? |
|
| Q2 | How old are you? |
|
| Q3 | What is your qualification? |
|
| Q4 | In what type of facility do you work? |
|
| Q5 | How many patients with IBD are treated at your Center annually? |
|
| Q6 | How many MRE are performed at your Center weekly (only for patients with IBD)? |
|
| Q7 | Which magnetic field is used in your Center for enteric MRI? |
|
| Q8 | Do you have experience in IBD? |
|
| Q9 | If yes, how many years have you been involved in IBD? |
|
| Q10 | Do you usually use a structured report for MRE of patients with IBD? |
|
| Q11 | Among general findings, what is included in your Center’s reports for MRE of patients with IBD (multiple answers possible)? |
|
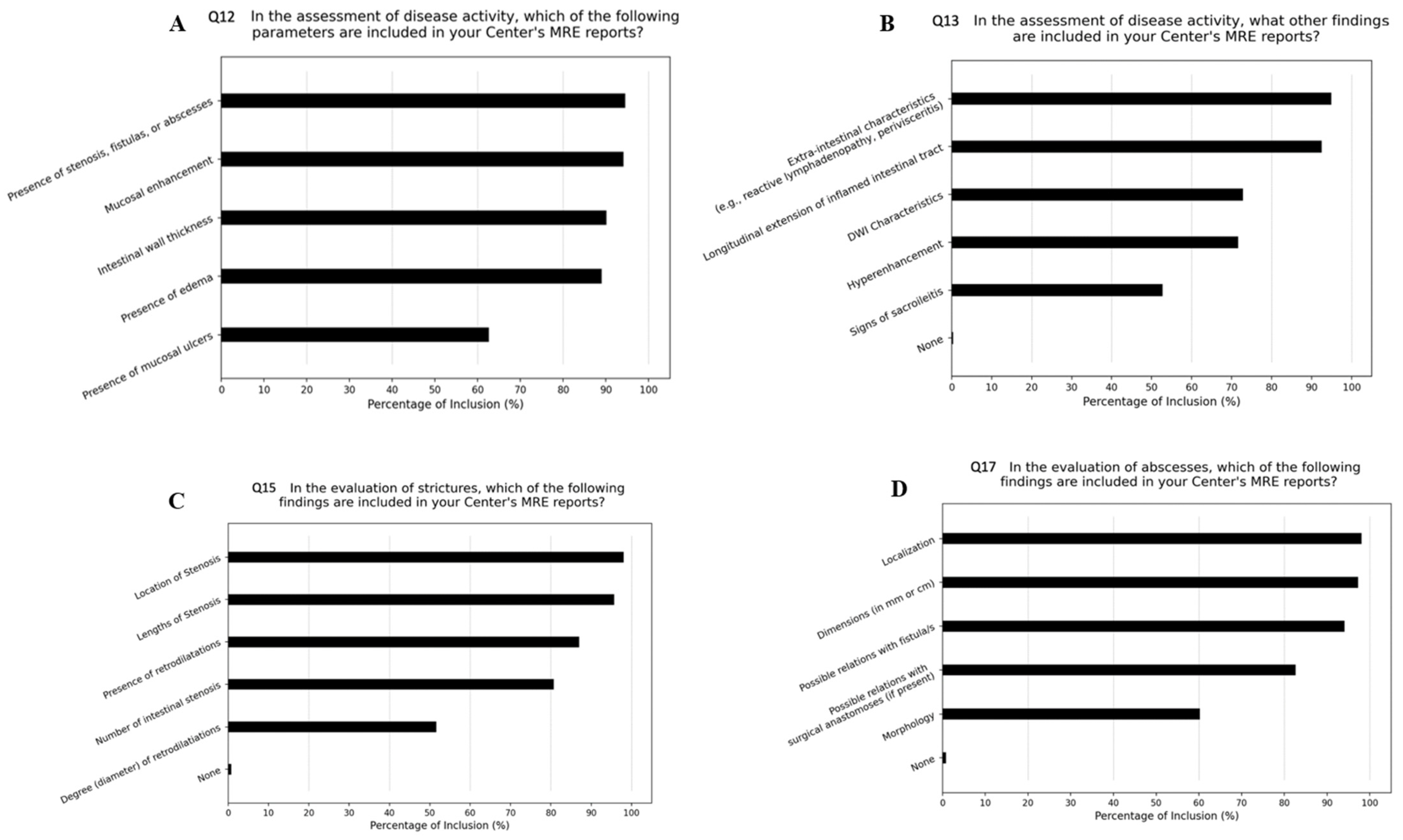
| Q12 | In the assessment of disease activity, which of the following parameters are included in your Center in the reports of MRE of patients with IBD (multiple answers possible)? |
|
| Q13 | In the assessment of disease activity, what other findings are included in your Center in the reports of MRE of patients with IBD (multiple answers possible)? |
|
| Q14 | Do you usually quantify numerically the wall thickness (in mm)? |
|
| Q15 | In the evaluation of stenosis, which of the following findings are included in your Center in the reports of MRE of patients with IBD (multiple answers possible)? |
|
| Q16 | In the evaluation of stenosis, which of the following findings are included in the reports of MRE of patients with IBD at your Center (multiple answers possible)? |
|
| Q17 | In the evaluation of abscesses, which of the following findings are included in the reports of MRE of patients with IBD at your Center (multiple answers possible)? |
|
| Q18 | Do you use scores in the assessment of IBD at your Center? |
|
| Q19 | If yes, which scores are usually included (multiple possible)? |
|
| Q20 | How confident do you feel with MaRIA or MaRIAs? |
|
| Q21 | Do you participate as a radiologist in multidisciplinary IBD meetings? |
|
| Characteristics | n = 253 n (%) | |
|---|---|---|
| Age class | ||
| <35 years | 79 (31.1) | |
| 35–50 years | 115 (45.3) | |
| >50 years | 59 (23.6) | |
| Professional qualification | ||
| Radiologist Hospital doctor Independent practitioner | 191 (75.5) 166 (86.9) 25 (13.1) | |
| Radiology resident | 62 (24.5) | |
| Site of employment | ||
| Public hospital | 119 (47.1) | |
| University hospital | 92 (36.3) | |
| Private hospital or clinic | 34 (13.4) | |
| Non-hospital structure | 8 (3.2) | |
| Geographic area of work | ||
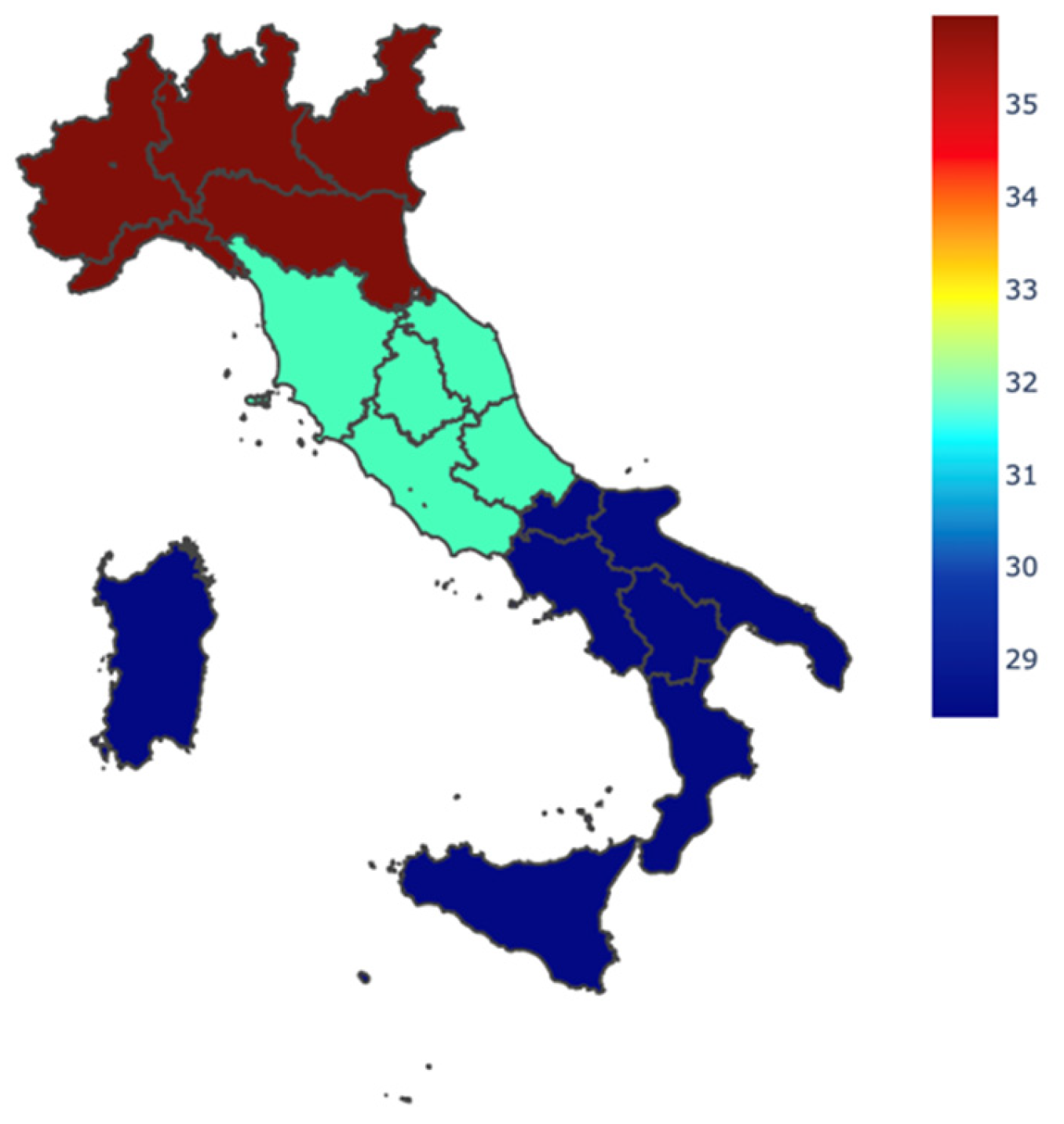
| Northern Italy | 113 (44.9) | |
| Central Italy | 66 (26.0) | |
| Southern Italy or islands | 74 (31.1) | |
| Experience with IBD | ||
| Yes | 188 (74.3) | |
| No | 65 (25.7) | |
| Duration of IBD experience, years | ||
| <5 | 68 (36.2) | |
| 5–10 | 59 (31.4) | |
| >10 | 61 (32.4) | |
| Hospital case load of patients with IBD, number per year | ||
| <100 | 97 (38.3) | |
| 100–500 | 80 (31.6) | |
| 500–1000 | 47 (18.6) | |
| >1000 | 29 (11.5) | |
| Hospital case load of MRE examinations for IBD, number per week | ||
| ≤1 | 74 (29.2) | |
| 2–3 | 95 (37.6) | |
| 4–5 | 35 (13.8) | |
| >5 | 49 (19.4) | |
| Participation in multidisciplinary IBD meetings | ||
| Yes, always | 25 (9.9) | |
| Mainly for complex cases and when invited by colleagues | 29 (11.5) | |
| I’m interested, but I’m not involved | 43 (17.0) | |
| I’m not interested in participating, although there is a multidisciplinary IBD meeting in my center | 24 (9.5) | |
| No, because multidisciplinary IBD meetings are not held in my center | 132 (52.1) | |
| MRI scanner’s magnetic field | ||
| 1.5 Tesla | 189 (74.7) | |
| 3 Tesla | 26 (10.3) | |
| 1.5 and 3 Tesla | 38 (15.0) | |
| Adoption of Structured MRE Report | Adoption of Disease Activity Scores | |
|---|---|---|
| Geographical Location | χ2 = 1.20, p-value = 0.55 1 | χ2 = 15.28, p-value = 0.004 1 |
| Responder’s Age | χ2 = 3.17, p-value = 0.21 1 | χ2 = 15.70, p-value = 0.003 1 |
| Type of Hospital | p-value = 0.606 2 | p-value = 0.005 2 |
| Working Occupation | p-value = 0.442 2 | p-value = 0.004 2 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bonifacio, C.; Dal Buono, A.; Levi, R.; Gabbiadini, R.; Reca, C.; Bezzio, C.; Francone, M.; Armuzzi, A.; Balzarini, L. Reporting of Magnetic Resonance Enterography in Inflammatory Bowel Disease: Results of an Italian Survey. J. Clin. Med. 2024, 13, 3953. https://doi.org/10.3390/jcm13133953
Bonifacio C, Dal Buono A, Levi R, Gabbiadini R, Reca C, Bezzio C, Francone M, Armuzzi A, Balzarini L. Reporting of Magnetic Resonance Enterography in Inflammatory Bowel Disease: Results of an Italian Survey. Journal of Clinical Medicine. 2024; 13(13):3953. https://doi.org/10.3390/jcm13133953
Chicago/Turabian StyleBonifacio, Cristiana, Arianna Dal Buono, Riccardo Levi, Roberto Gabbiadini, Christian Reca, Cristina Bezzio, Marco Francone, Alessandro Armuzzi, and Luca Balzarini. 2024. "Reporting of Magnetic Resonance Enterography in Inflammatory Bowel Disease: Results of an Italian Survey" Journal of Clinical Medicine 13, no. 13: 3953. https://doi.org/10.3390/jcm13133953
APA StyleBonifacio, C., Dal Buono, A., Levi, R., Gabbiadini, R., Reca, C., Bezzio, C., Francone, M., Armuzzi, A., & Balzarini, L. (2024). Reporting of Magnetic Resonance Enterography in Inflammatory Bowel Disease: Results of an Italian Survey. Journal of Clinical Medicine, 13(13), 3953. https://doi.org/10.3390/jcm13133953







