Mild Water-Filtered Infrared-A Whole-Body Hyperthermia Reduces Pain in Patients with Fibromyalgia Syndrome—A Randomized Sham-Controlled Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Design and Procedure
2.2. Participants
2.3. Randomization
2.4. Intervention Group
2.5. Control Group
2.6. Outcomes
2.6.1. Primary Outcome
2.6.2. Secondary Outcomes
2.6.3. Blood Parameters
2.6.4. Safety
2.7. Statistical Analysis
2.8. Sample Size
3. Results
3.1. Participants
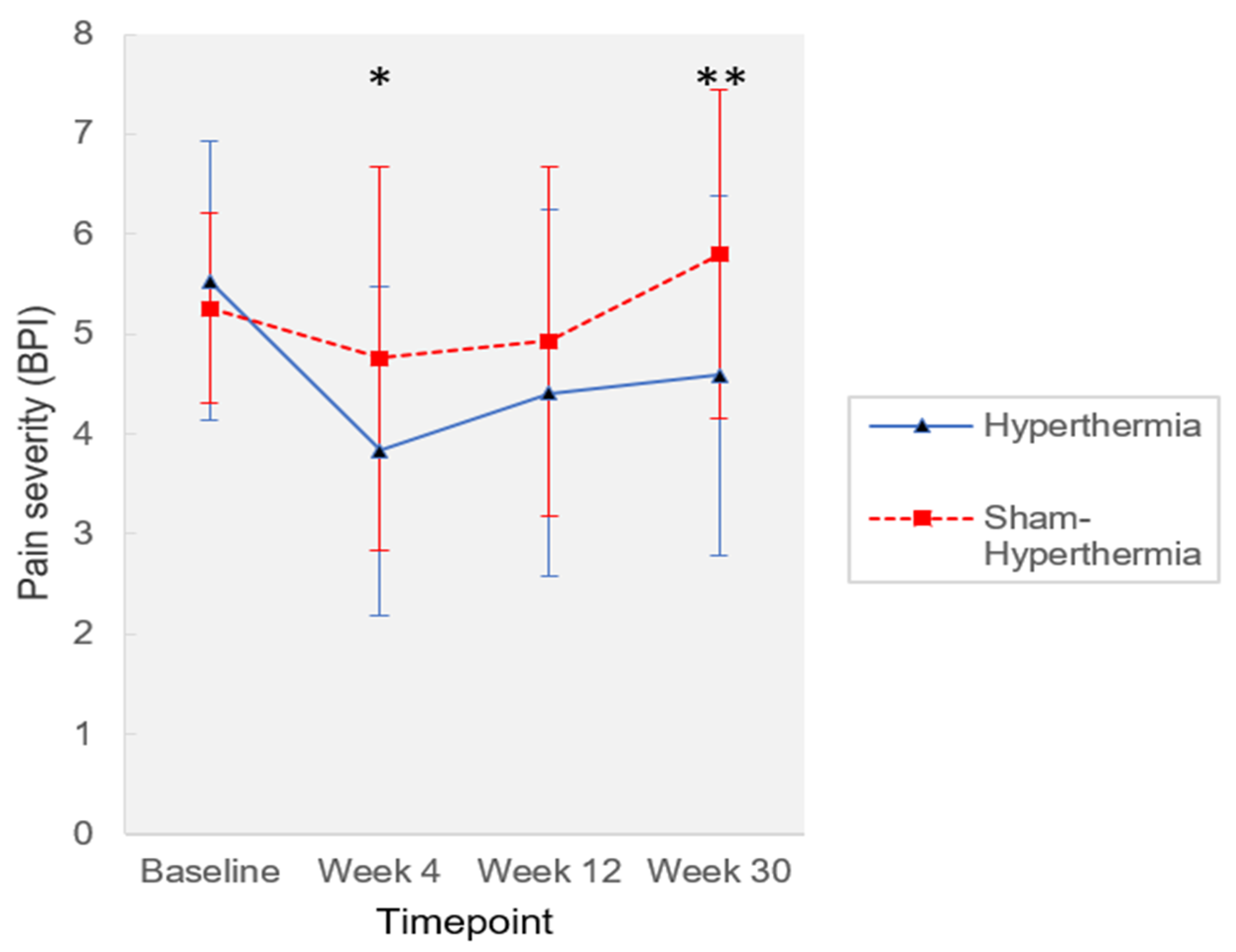
3.2. Primary Outcome
3.3. Secondary Outcomes
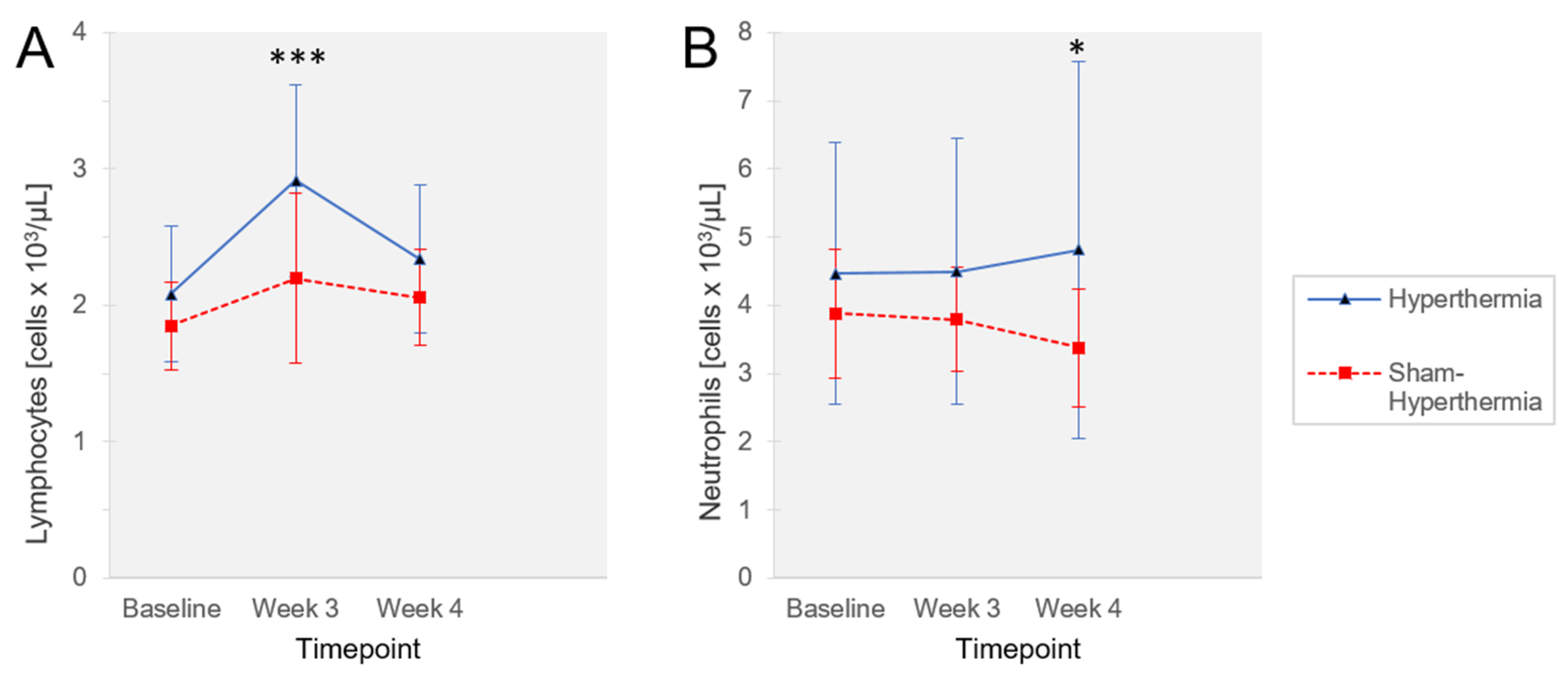
3.4. Immunological Changes
3.5. Physiologic Responses
3.6. Credibility Check
3.7. Safety
4. Discussion
4.1. Summary of Main Results
4.2. Comparison to Previous Studies
4.3. Strengths and Weaknesses
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Marques, A.P.; Santo, A.d.S.d.E.; Berssaneti, A.A.; Matsutani, L.A.; Yuan, S.L.K. Prevalence of fibromyalgia: Literature review update. Rev. Bras. De Reumatol. (Engl. Ed.) 2017, 57, 356–363. [Google Scholar] [CrossRef]
- Creed, F. A review of the incidence and risk factors for fibromyalgia and chronic widespread pain in population-based studies. Pain 2020, 161, 1169–1176. [Google Scholar] [CrossRef] [PubMed]
- Cagnie, B.; Coppieters, I.; Denecker, S.; Six, J.; Danneels, L.; Meeus, M. Central sensitization in fibromyalgia? A systematic review on structural and functional brain MRI. Semin. Arthritis Rheum. 2014, 44, 68–75. [Google Scholar] [CrossRef] [PubMed]
- Becker, S.; Schweinhardt, P. Dysfunctional Neurotransmitter Systems in Fibromyalgia, Their Role in Central Stress Circuitry and Pharmacological Actions on These Systems. Pain Res. Treat. 2012, 2012, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Martínez, L.-A.; Mora, T.; Vargas, A.; Fuentes-Iniestra, M.; Martínez-Lavín, M. Sympathetic Nervous System Dysfunction in Fibromyalgia, Chronic Fatigue Syndrome, Irritable Bowel Syndrome, and Interstitial Cystitis. JCR J. Clin. Rheumatol. 2014, 20, 146–150. [Google Scholar] [CrossRef]
- Üçeyler, N.; Zeller, D.; Kahn, A.-K.; Kewenig, S.; Kittel-Schneider, S.; Schmid, A.; Casanova-Molla, J.; Reiners, K.; Sommer, C. Small fibre pathology in patients with fibromyalgia syndrome. Brain 2013, 136, 1857–1867. [Google Scholar] [CrossRef]
- Üçeyler, N.; Burgmer, M.; Friedel, E.; Greiner, W.; Petzke, F.; Sarholz, M.; Schiltenwolf, M.; Winkelmann, A.; Sommer, C.; Häuser, W. Ätiologie und Pathophysiologie des Fibromyalgiesyndroms. Schmerz 2017, 31, 239–245. [Google Scholar] [CrossRef]
- Morf, S.; Amann-Vesti, B.; Forster, A.; Franzeck, U.K.; Koppensteiner, R.; Uebelhart, D.; Sprott, H. Microcirculation abnormalities in patients with fibromyalgia - measured by capillary microscopy and laser fluxmetry. Arthritis Res. Ther. 2005, 7, R209. [Google Scholar] [CrossRef]
- Häuser, W.; Ablin, J.; Fitzcharles, M.-A.; Littlejohn, G.; Luciano, J.V.; Usui, C.; Walitt, B. Fibromyalgia. Nat. Rev. Dis. Prim. 2015, 1, 15022. [Google Scholar] [CrossRef]
- Marschall, U.; Arnold, B.; Häuser, W. Behandlung und Krankheitskosten des Fibromyalgiesyndroms in Deutschland. Schmerz 2011, 25, 402–410. [Google Scholar] [CrossRef]
- Sommer, C.; Alten, R.; Bär, K.J.; Bernateck, M.; Brückle, W.; Friedel, E.; Henningsen, P.; Petzke, F.; Tölle, T.; Üçeyler, N.; et al. Medikamentöse Therapie des Fibromyalgiesyndroms. Schmerz 2017, 31, 274–284. [Google Scholar] [CrossRef] [PubMed]
- Okifuji, A.; Gao, J.; Bokat, C.; Hare, B.D. Management of fibromyalgia syndrome in 2016. Pain Manag. 2016, 6, 383–400. [Google Scholar] [CrossRef] [PubMed]
- Häuser, W.; Bernardy, K.; Arnold, B.; Offenbächer, M.; Schiltenwolf, M. Efficacy of multicomponent treatment in fibromyalgia syndrome: A meta-analysis of randomized controlled clinical trials. Arthritis Rheum. 2009, 61, 216–224. [Google Scholar] [CrossRef] [PubMed]
- Thieme, K.; Mathys, M.; Turk, D.C. Evidenced-Based Guidelines on the Treatment of Fibromyalgia Patients: Are They Consistent and If Not, Why Not? Have Effective Psychological Treatments Been Overlooked? J. Pain 2017, 18, 747–756. [Google Scholar] [CrossRef]
- Crofford, L.J.; Appleton, B.E. Complementary and alternative therapies for fibromyalgia. Curr. Rheumatol. Rep. 2001, 3, 147–156. [Google Scholar] [CrossRef]
- Petzke, F.; Brückle, W.; Eidmann, U.; Heldmann, P.; Köllner, V.; Kühn, T.; Kühn-Becker, H.; Strunk-Richter, M.; Schiltenwolf, M.; Settan, M.; et al. Allgemeine Behandlungsgrundsätze, Versorgungskoordination und Patientenschulung beim Fibromyalgiesyndrom. Schmerz 2017, 31, 246–254. [Google Scholar] [CrossRef]
- Brockow, T.; Wagner, A.; Franke, A.; Offenbächer, M.; Resch, K.L. A Randomized Controlled Trial on the Effectiveness of Mild Water-filtered Near Infrared Whole-body Hyperthermia as an Adjunct to a Standard Multimodal Rehabilitation in the Treatment of Fibromyalgia. Clin. J. Pain 2007, 23, 67–75. [Google Scholar] [CrossRef]
- Romeyke, T.; Scheuer, H.; Stummer, H. Fibromyalgia with severe forms of progression in a multidisciplinary therapy setting with emphasis on hyperthermia therapy—A prospective controlled study. Clin. Interv. Aging 2014, 69–79. [Google Scholar] [CrossRef]
- Romeyke, T.; Stummer, H. Multi-Modal Pain Therapy of Fibromyalgia Syndrome with Integration of Systemic Whole-Body Hyperthermia—Effects on Pain Intensity and Mental State: A Non-Randomised Controlled Study. J. Musculoskelet. Pain 2014, 22, 341–355. [Google Scholar] [CrossRef]
- Schleenbecker, H.; Schmidt, K. Zur Wirkung einer iterativen milden Ganzkörperhyperthermie auf den Fibromyalgieschmerz - Pilotstudie. Phys. Med. Rehabil. Kurortmed. 1998, 8, 113–117. [Google Scholar] [CrossRef]
- Schwedtke, C. Evaluierung von Kurzzeit- und Serieneffekten von milder Infrarot A-Hyperthermie auf die Schmerzempfindung bei Patienten mit Fibromyalgie. 2010. Available online: https://refubium.fu-berlin.de/bitstream/handle/fub188/1718/DissOnline.pdf?sequence=1&isAllowed=y (accessed on 13 February 2023).
- Walz, J.; Hinzmann, J.; Haase, I.; Witte, T. Ganzkörperhyperthermie in der Schmerztherapie. Schmerz 2013, 27, 38–45. [Google Scholar] [CrossRef] [PubMed]
- Heckel, M. Ganzkörperhyperthermie und Fiebertherapie: Grundlagen und Praxis; Hippokrates-Verlag: Stuttgart, Germany, 1990. [Google Scholar]
- Schmidt, K.L.H. Fieber. Wirkungen bei Mensch und Tier. Klinik, Pathologie, Immunologie, Wirkungen auf Entzündungen. 2. überarb. Auflage. Stuttgart. In Hippokrates; Georg Thieme Verlag KG: Stuttgart, Germany, 1987. [Google Scholar]
- Schmidt, K.L. Zur Wirkung einer Ganzkörperhyperthermie auf Entzündungen und Immunreaktionen: Experimentelle Grundlagen. Phys. Med. Rehabil. Kurortmed. 2004, 14, 227–235. [Google Scholar] [CrossRef]
- Laukkanen, T.; Lipponen, J.; Kunutsor, S.K.; Zaccardi, F.; Araújo, C.G.S.; Mäkikallio, T.H.; Khan, H.; Willeit, P.; Lee, E.; Poikonen, S.; et al. Recovery from sauna bathing favorably modulates cardiac autonomic nervous system. Complement. Ther. Med. 2019, 45, 190–197. [Google Scholar] [CrossRef] [PubMed]
- Tracy, L.M.; Ioannou, L.; Baker, K.S.; Gibson, S.J.; Georgiou-Karistianis, N.; Giummarra, M.J. Meta-analytic evidence for decreased heart rate variability in chronic pain implicating parasympathetic nervous system dysregulation. Pain 2016, 157, 7–29. [Google Scholar] [CrossRef] [PubMed]
- Alen, N.V.; Parenteau, A.M.; Sloan, R.P.; Hostinar, C.E. Heart rate variability and circulating inflammatory markers in midlife. Brain Behav. Immun. Health 2021, 15, 100273. [Google Scholar] [CrossRef]
- Kuwahata, S.; Miyata, M.; Fujita, S.; Kubozono, T.; Shinsato, T.; Ikeda, Y.; Hamasaki, S.; Kuwaki, T.; Tei, C. Improvement of autonomic nervous activity by Waon therapy in patients with chronic heart failure. J. Cardiol. 2011, 57, 100–106. [Google Scholar] [CrossRef]
- Tarner, I.H.; Müller-Ladner, U.; Uhlemann, C.; Lange, U. The effect of mild whole-body hyperthermia on systemic levels of TNF-alpha, IL-1beta, and IL-6 in patients with ankylosing spondylitis. Clin. Rheumatol. 2009, 28, 397–402. [Google Scholar] [CrossRef]
- Lange, U.; Dischereit, G. Wirkeffekte differenter iterativer Ganzkörper-Hyperthermie-Verfahren auf Schmerzen und Zytokine bei rheumatischen Erkrankungen – eine aktuelle Literaturübersicht. Aktuelle Rheumatol. 2018, 57, 479–483. [Google Scholar] [CrossRef]
- Wallace, D. Is There a Role for Cytokine Based Therapies in Fibromyalgia. Curr. Pharm. Des. 2006, 12, 17–22. [Google Scholar] [CrossRef]
- Bazzichi, L.; Rossi, A.; Massimetti, G.; Giannaccini, G.; Giuliano, T.; De Feo, F.; Ciapparelli, A.; Dell’Osso, L.; Bombardieri, S. Cytokine patterns in fibromyalgia and their correlation with clinical manifestations. Clin. Exp. Rheumatol. 2007, 25, 225–230. [Google Scholar]
- Menzies, V.; Lyon, D.E. Integrated Review of the Association of Cytokines with Fibromyalgia and Fibromyalgia Core Symptoms. Biol. Res. Nurs. 2010, 11, 387–394. [Google Scholar] [CrossRef] [PubMed]
- Mendieta, D.; la Cruz-Aguilera, D.L.D.; Barrera-Villalpando, M.I.; Becerril-Villanueva, E.; Arreola, R.; Hernández-Ferreira, E.; Pérez-Tapia, S.M.; Pérez-Sánchez, G.; Garcés-Alvarez, M.E.; Aguirre-Cruz, L.; et al. IL-8 and IL-6 primarily mediate the inflammatory response in fibromyalgia patients. J. Neuroimmunol. 2016, 290, 22–25. [Google Scholar] [CrossRef] [PubMed]
- Kumbhare, D.; Hassan, S.; Diep, D.; Duarte, F.C.K.; Hung, J.; Damodara, S.; West, D.W.D.; Selvaganapathy, P.R. Potential role of blood biomarkers in patients with fibromyalgia: A systematic review with meta-analysis. Pain 2022, 163, 1232–1253. [Google Scholar] [CrossRef]
- Cleeland, C.S.; Ryan, K. The brief pain inventory. Pain Res. Group 1991, 20, 143–147. [Google Scholar]
- Radbruch, L.; Loick, G.; Kiencke, P.; Lindena, G.; Sabatowski, R.; Grond, S.; Lehmann, K.A.; Cleeland, C.S. Validation of the German Version of the Brief Pain Inventory. J. Pain Symptom Manag. 1999, 18, 180–187. [Google Scholar] [CrossRef] [PubMed]
- Arnold, L.M.; Williams, D.A.; Hudson, J.I.; Martin, S.A.; Clauw, D.J.; Crofford, L.J.; Wang, F.; Emir, B.; Lai, C.; Zablocki, R.; et al. Development of responder definitions for fibromyalgia clinical trials. Arthritis Rheum. 2012, 64, 885–894. [Google Scholar] [CrossRef] [PubMed]
- Burckhardt, C.S.; Clark, S.R.; Bennett, R.M. The fibromyalgia impact questionnaire: Development and validation. J. Rheumatol. 1991, 18, 728–733. [Google Scholar]
- Offenbächer, M.; Waltz, M.; Schoeps, P. Validation of a German Version of the Fibromyalgia Impact Questionnaire (FIQ-G). J. Rheumatol. 2000, 27, 1984–1988. [Google Scholar]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B.W. The PHQ-9. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Radbruch, L.; Sabatowski, R.; Elsner, F.; Everts, J.; Mendoza, T.; Cleeland, C. Validation of the German Version of the Brief Fatigue Inventory. J. Pain Symptom Manag. 2003, 25, 449–458. [Google Scholar] [CrossRef]
- Smets, E.M.A.; Garssen, B.; Bonke, B.; De Haes, J.C.J.M. The multidimensional Fatigue Inventory (MFI) psychometric qualities of an instrument to assess fatigue. J. Psychosom. Res. 1995, 39, 315–325. [Google Scholar] [CrossRef] [PubMed]
- Buysse, D.J.; Reynolds, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh sleep quality index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef] [PubMed]
- Hinz, A.; Glaesmer, H.; Brähler, E.; Löffler, M.; Engel, C.; Enzenbach, C.; Hegerl, U.; Sander, C. Sleep quality in the general population: Psychometric properties of the Pittsburgh Sleep Quality Index, derived from a German community sample of 9284 people. Sleep Med. 2017, 30, 57–63. [Google Scholar] [CrossRef] [PubMed]
- Ware, J.J.E.; Gandek, B. The SF-36 Health Survey: Development and Use in Mental Health Research and the IQOLA Project. Int. J. Ment. Health 1994, 23, 49–73. [Google Scholar] [CrossRef]
- Bullinger, M. German translation and psychometric testing of the SF-36 Health Survey: Preliminary results from the IQOLA project. Soc. Sci. Med. 1995, 41, 1359–1366. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Löwe, B. A Brief Measure for Assessing Generalized Anxiety Disorder: The GAD-7. Arch. Intern. Med. 2006, 166, 1092–1097. [Google Scholar] [CrossRef] [PubMed]
- Melzack, R. The short-form McGill pain questionnaire. Pain 1987, 30, 191–197. [Google Scholar] [CrossRef]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B.W. The PHQ-15: Validity of a New Measure for Evaluating the Severity of Somatic Symptoms. Psychosom. Med. 2002, 64, 258–266. [Google Scholar] [CrossRef]
- Üçeyler, N.; Häuser, W.; Sommer, C. Systematic review with meta-analysis: Cytokines in fibromyalgia syndrome. BMC Musculoskelet. Disord. 2011, 12, 245. [Google Scholar] [CrossRef]
- Zhou, Y.-Q.; Liu, Z.; Liu, Z.-H.; Chen, S.-P.; Li, M.; Shahveranov, A.; Ye, D.-W.; Tian, Y.-K. Interleukin-6: An emerging regulator of pathological pain. J. Neuroinflamm. 2016, 13, 141. [Google Scholar] [CrossRef]
- Totsch, S.K.; Sorge, R.E. Immune system involvement in specific pain conditions. Mol. Pain 2017, 13, 1744806917724559. [Google Scholar] [CrossRef] [PubMed]

| Mild WBH (n = 21) | Sham Hyperthermia (n = 20) | |
|---|---|---|
| Sex (female/male) | 19/2 | 20/0 |
| Age, M (SD), years | 54.61 (7.65) | 56.40 (4.86) |
| BMI, M (SD), kg/m2 | 28.61 (6.70) | 27.47 (7.05) |
| Education, n (%) | ||
| Primary school graduation | 9 (42.9) | 3 (15) |
| Secondary school certificate | 7 (33.3) | 14 (70) |
| Qualification for university entrance | 3 (9.5) | 3 (15) |
| University degree | 2 (9.5) | 0 (0) |
| Marital status, n (%) | ||
| Single | 2 (9.5) | 3 (15) |
| Married/partner | 15 (71.4) | 14 (70) |
| Divorced, separated, widowed | 4 (19) | 3 (15) |
| Employment status, n (%) | ||
| Employed | 15 (71.4) | 14 (70) |
| Employed, but sick leave | 1 (4.8) | 3 (15) |
| Unemployed | 0 (0) | 0 (0) |
| Retired, housework, apprentice | 6 (28.6) | 6 (30) |
| Comorbidities, n (%) | ||
| Metabolic | 7 (33.3) | 8 (40) |
| Psychiatric | 8 (38.1) | 5 (25) |
| Nervous system | 13 (61.9) | 9 (45) |
| Cardiovascular | 5 (23.8) | 3 (15) |
| Gastrointestinal | 5 (23.8) | 1 (5) |
| Musculoskeletal | 12 (57.1) | 10 (50) |
| Other | 7 (33.3) | 7 (35) |
| Medication, n (%) | ||
| Opioid Analgesics | 3 (14.3) | 0 (0) |
| Non-opioid Analgesics | 8 (38.1) | 7 (35) |
| NSAID | 11 (52.4) | 14 (70) |
| Muscle relaxants | 0 (0) | 0 (0) |
| Anticonvulsants | 3 (14.3) | 0 (0) |
| Antidepressants | 8 (38.1) | 7 (35) |
| Glucocorticoids | 0 (0) | 1 (5) |
| Other | 15 (71.4) | 12 (60) |
| Pain intensity (1–10), M (SD) | 5.53 (1.40) | 5.26 (0.95) |
| Outcome | Group | T0/Baseline (Week 0) | T1 (End of Treatment) | T2 (Week 4) |
|---|---|---|---|---|
| TNF | Hyperthermia | 0.88 ± 0.25 | 0.93 ± 0.24 | 0.99 ± 0.32 |
| Sham Hyperthermia | 0.84 ± 0.16 | 0.88 ± 0.25 | 0.95 ± 0.26 | |
| IL-6 | Hyperthermia | 2.00 ± 1.35 | 3.04 ± 1.91 | 2.31 ± 1.45 |
| Sham Hyperthermia | 2.01 ± 1.68 | 2.52 ± 2.20 | 2.18 ± 1.67 | |
| IL-8 | Hyperthermia | 6.56 ± 2.92 | 7.35 ± 3.55 | 6.32 ± 1.56 |
| Sham Hyperthermia | 6.24 ± 1.88 | 6.90 ± 2.03 | 6.47 ± 1.65 | |
| IL-10 | Hyperthermia | 1.52 ± 1.64 | 1.56 ± 1.81 | 2.24 ± 2.03 |
| Sham Hyperthermia | 1.01 ± 1.15 | 1.15 ± 1.07 | 1.79 ± 3.42 | |
| Neutrophils | Hyperthermia | 4.47 ± 1.92 | 4.50 ± 1.95 | 4.82 ± 2.77 |
| Sham Hyperthermia | 3.88 ± 0.95 | 3.79 ± 0.76 | 3.38 ± 0.86 | |
| Leukocytes | Hyperthermia | 7.33 ± 2.25 | 8.60 ± 2.95 | 8.04 ± 3.23 |
| Sham Hyperthermia | 6.31 ± 1.21 | 6.75 ± 1.36 | 6.26 ± 1.08 | |
| Lymphocytes | Hyperthermia | 2.08 ± 0.49 | 2.91 ± 0.71 | 2.34 ± 0.54 |
| Sham Hyperthermia | 1.85 ± 0.32 | 2.20 ± 0.62 | 2.06 ± 0.35 | |
| Monocytes | Hyperthermia | 0.54 ± 0.15 | 0.53 ± 0.36 | 0.57 ± 0.38 |
| Sham Hyperthermia | 0.48 ± 0.20 | 0.51 ± 0.26 | 0.51 ± 0.21 | |
| Thrombocytes | Hyperthermia | 282.95 ± 49.14 | 294.99 ± 53.78 | 282.42 ± 41.28 |
| Sham Hyperthermia | 263.60 ± 43.64 | 256.01 ± 34.32 | 263.81 ± 36.83 | |
| CRP | Hyperthermia | 0.31 ± 0.39 | 0.22 ± 0.33 | 0.23 ± 0.39 |
| Sham Hyperthermia | 0.29 ± 0.28 | 0.20 ± 0.23 | 0.18 ± 0.20 | |
| ESR | Hyperthermia | 9.95 ± 6.52 | 8.68 ± 4.59 | 8.97 ± 4.85 |
| Sham Hyperthermia | 10.20 ± 6.14 | 11.43 ± 7.68 | 10.57 ± 4.51 |
| Mild WBH M ± SD | Sham Hyperthermia M ± SD | |
|---|---|---|
| Heating phase (min) a | 45.30 ± 6.69 | - |
| Retention phase (min) a | 14.69 ± 6.64 | - |
| Maximum Temperature (°C) a | 38.74 ± 0.17 | 37.52 ± 0.25 |
| Side effects during interventions, n (%) b | ||
| Burning sensation on skin (calf, buttocks, shoulder, back) | 15 (71.4) | 0 |
| Physical stress (feeling of heat/palpitations/throbbing/restlessness) | 8 (38.1) | 0 |
| Headache | 5 (23.8) | 4 (20) |
| Severe circulatory problems | 2 (9.5) | 0 |
| Dizziness | 2 (9.5) | 0 |
| Poor general condition | 1 (4.8) | 0 |
| Tingling/shaking | 1 (4.8) | 0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Langhorst, J.; Koch, A.K.; Kehm, C.; Öznur, Ö.; Engler, H.; Häuser, W. Mild Water-Filtered Infrared-A Whole-Body Hyperthermia Reduces Pain in Patients with Fibromyalgia Syndrome—A Randomized Sham-Controlled Trial. J. Clin. Med. 2023, 12, 2945. https://doi.org/10.3390/jcm12082945
Langhorst J, Koch AK, Kehm C, Öznur Ö, Engler H, Häuser W. Mild Water-Filtered Infrared-A Whole-Body Hyperthermia Reduces Pain in Patients with Fibromyalgia Syndrome—A Randomized Sham-Controlled Trial. Journal of Clinical Medicine. 2023; 12(8):2945. https://doi.org/10.3390/jcm12082945
Chicago/Turabian StyleLanghorst, Jost, Anna K. Koch, Christina Kehm, Özlem Öznur, Harald Engler, and Winfried Häuser. 2023. "Mild Water-Filtered Infrared-A Whole-Body Hyperthermia Reduces Pain in Patients with Fibromyalgia Syndrome—A Randomized Sham-Controlled Trial" Journal of Clinical Medicine 12, no. 8: 2945. https://doi.org/10.3390/jcm12082945
APA StyleLanghorst, J., Koch, A. K., Kehm, C., Öznur, Ö., Engler, H., & Häuser, W. (2023). Mild Water-Filtered Infrared-A Whole-Body Hyperthermia Reduces Pain in Patients with Fibromyalgia Syndrome—A Randomized Sham-Controlled Trial. Journal of Clinical Medicine, 12(8), 2945. https://doi.org/10.3390/jcm12082945





