Mobile Apps to Improve Brace-Wearing Compliance in Patients with Idiopathic Scoliosis: A Quality Analysis, Functionality Review and Future Directions
Abstract
1. Introduction
2. Materials and Methods
2.1. Search and Selection Strategy
2.2. In-Depth Analysis and Procedure
3. Results
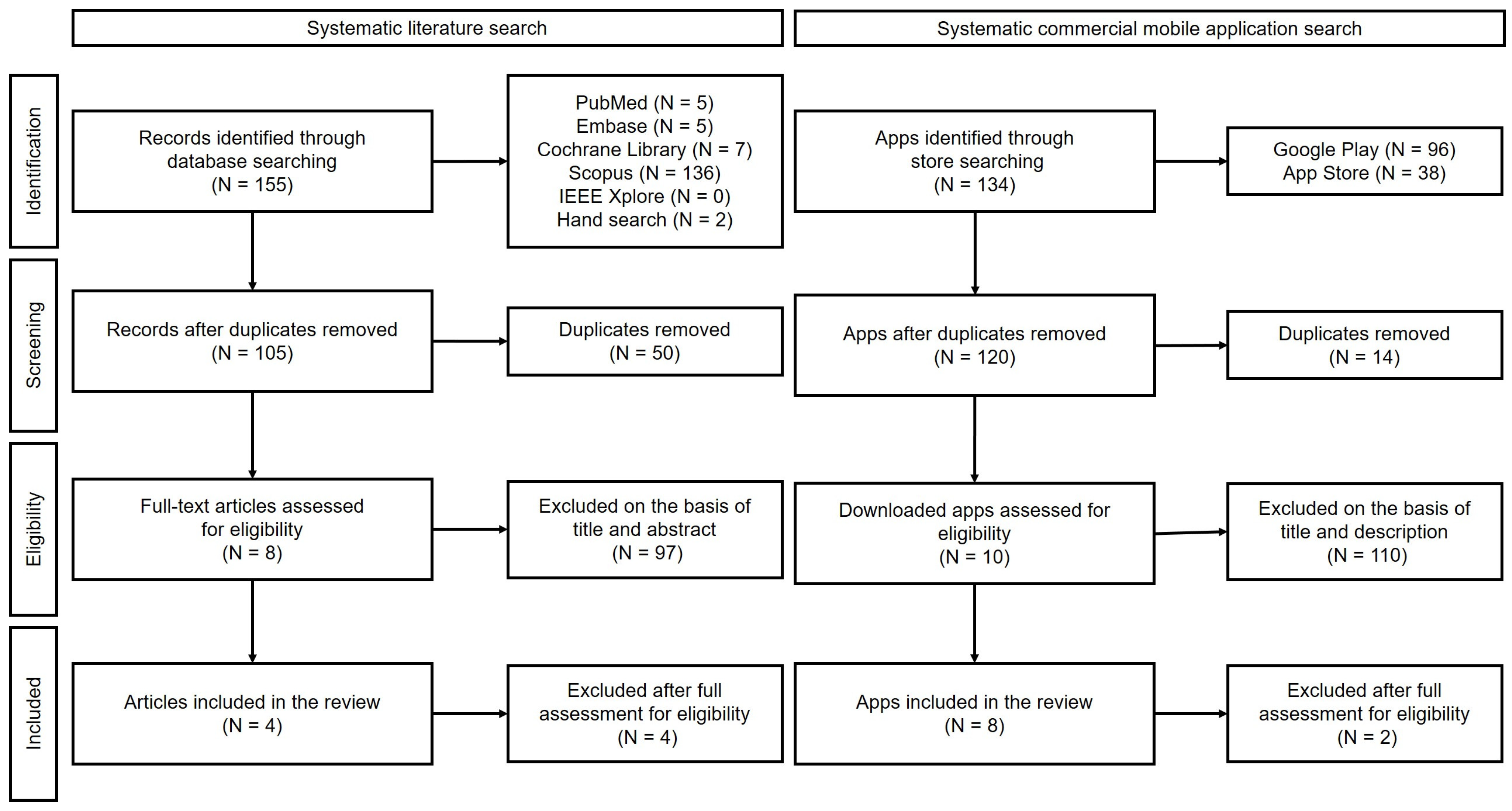
3.1. Search Results
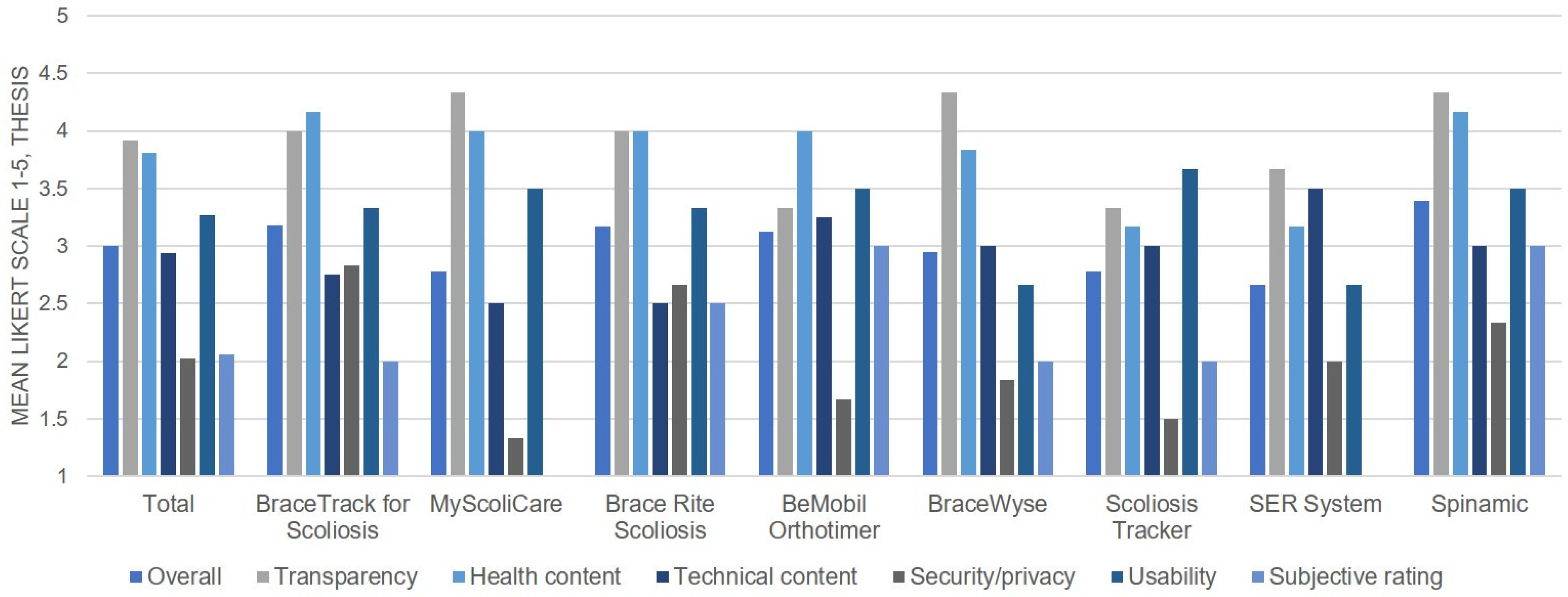
3.2. Quality by the THESIS
3.3. Functionality
3.3.1. Data Acquisition
3.3.2. Compliance Enhancement
3.3.3. Educational Components
3.3.4. Additional Functionalities
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Konieczny, M.R.; Senyurt, H.; Krauspe, R. Epidemiology of adolescent idiopathic scoliosis. J. Child Orthop. 2013, 7, 3–9. [Google Scholar] [CrossRef]
- Cheng, J.C.; Castelein, R.M.; Chu, W.C.; Danielsson, A.J.; Dobbs, M.B.; Grivas, T.B.; Gurnett, C.A.; Luk, K.D.; Moreau, A.; Newton, P.O. Adolescent idiopathic scoliosis. Nat. Rev. Dis. Prim. 2015, 1, 15030. [Google Scholar] [CrossRef]
- Janicki, J.A.; Alman, B. Scoliosis: Review of diagnosis and treatment. Paediatr. Child Health 2007, 12, 771–776. [Google Scholar] [CrossRef] [PubMed]
- Lonstein, J.E. Scoliosis: Surgical versus nonsurgical treatment. Clin. Orthop. Relat. Res. 2006, 443, 248–259. [Google Scholar] [CrossRef]
- Weinstein, S.L.; Dolan, L.A.; Cheng, J.C.; Danielsson, A.; Morcuende, J.A. Adolescent idiopathic scoliosis. Lancet 2008, 371, 1527–1537. [Google Scholar] [CrossRef]
- Negrini, S.; Donzelli, S.; Aulisa, A.G.; Czaprowski, D.; Schreiber, S.; de Mauroy, J.C.; Diers, H.; Grivas, T.B.; Knott, P.; Kotwicki, T.; et al. 2016 sosort guidelines: Orthopaedic and rehabilitation treatment of idiopathic scoliosis during growth. Scoliosis Spinal Disord. 2018, 13, 3. [Google Scholar] [CrossRef]
- de Kleuver, M.; Lewis, S.J.; Germscheid, N.M.; Kamper, S.J.; Alanay, A.; Berven, S.H.; Cheung, K.M.; Ito, M.; Lenke, L.G.; Polly, D.W.; et al. Optimal surgical care for adolescent idiopathic scoliosis: An international consensus. Eur. Spine J. 2014, 23, 2603–2618. [Google Scholar] [CrossRef]
- Weinstein, S.L.; Dolan, L.A.; Wright, J.G.; Dobbs, M.B. Effects of bracing in adolescents with idiopathic scoliosis. N. Engl. J. Med. 2013, 369, 1512–1521. [Google Scholar] [CrossRef] [PubMed]
- Dolan, L.A.; Donzelli, S.; Zaina, F.; Weinstein, S.L.; Negrini, S. Adolescent idiopathic scoliosis bracing success is influenced by time in brace: Comparative effectiveness analysis of braist and isico cohorts. Spine 2020, 45, 1193–1199. [Google Scholar] [CrossRef]
- Takemitsu, M.; Bowen, J.R.; Rahman, T.; Glutting, J.J.; Scott, C.B. Compliance monitoring of brace treatment for patients with idiopathic scoliosis. Spine 2004, 29, 2070–2074; discussion in 2074. [Google Scholar] [CrossRef]
- Nicholson, G.P.; Ferguson-Pell, M.W.; Smith, K.; Edgar, M.; Morley, T. The objective measurement of spinal orthosis use for the treatment of adolescent idiopathic scoliosis. Spine 2003, 28, 2243–2250; discussion in 2250–2241. [Google Scholar] [CrossRef]
- Lou, E.; Hill, D.; Hedden, D.; Mahood, J.; Moreau, M.; Raso, J. An objective measurement of brace usage for the treatment of adolescent idiopathic scoliosis. Med. Eng. Phys. 2011, 33, 290–294. [Google Scholar] [CrossRef] [PubMed]
- Miller, D.J.; Franzone, J.M.; Matsumoto, H.; Gomez, J.A.; Avendaño, J.; Hyman, J.E.; Roye, D.P., Jr.; Vitale, M.G. Electronic monitoring improves brace-wearing compliance in patients with adolescent idiopathic scoliosis: A randomized clinical trial. Spine 2012, 37, 717–721. [Google Scholar] [CrossRef]
- World Health Organization. Mhealth: New Horizons for Health through Mobile Technologies. 2011. Available online: https://scholarworks.iupui.edu/bitstream/handle/1805/11987/faiola_2016_consumer.pdf?sequence=1&isAllowed=y (accessed on 23 February 2023).
- Kao, C.K.; Liebovitz, D.M. Consumer mobile health apps: Current state, barriers, and future directions. PM&R 2017, 9, S106–S115. [Google Scholar]
- Aitken, M.; Lyle, J. Patient Adoption of mhealth: Use, Evidence and Remaining Barriers to Mainstream Acceptance; IMS Institute for Healthcare Informatics: Parsippany, NJ, USA, 2015. [Google Scholar]
- Martínez-Pérez, B.; de la Torre-Díez, I.; López-Coronado, M. Mobile health applications for the most prevalent conditions by the World Health Organization: Review and analysis. J. Med. Internet Res. 2013, 15, e120. [Google Scholar] [CrossRef] [PubMed]
- Tabi, K.; Randhawa, A.S.; Choi, F.; Mithani, Z.; Albers, F.; Schnieder, M.; Nikoo, M.; Vigo, D.; Jang, K.; Demlova, R.; et al. Mobile apps for medication management: Review and analysis. JMIR Mhealth Uhealth 2019, 7, e13608. [Google Scholar] [CrossRef]
- Timmers, T.; Janssen, L.; Kool, R.B.; Kremer, J.A. Educating patients by providing timely information using smartphone and tablet apps: Systematic review. J. Med. Internet Res. 2020, 22, e17342. [Google Scholar] [CrossRef]
- Levine, D.M.; Co, Z.; Newmark, L.P.; Groisser, A.R.; Holmgren, A.J.; Haas, J.S.; Bates, D.W. Design and testing of a mobile health application rating tool. NPJ Digit. Med. 2020, 3, 74. [Google Scholar] [CrossRef]
- Dannehl, S.; Seiboth, D.; Doria, L.; Minge, M.; Lorenz, K.; Thüring, M.; Kraft, M. A smartphone-based system to improve adherence in scoliosis therapy. i-com 2016, 15, 313–319. [Google Scholar] [CrossRef]
- Minge, M.; Lorenz, K.; Dannehl, S.; Jankowski, N.; Klausner, M. Developing a mobile system for children and teenagers with scoliosis to improve therapy adherence. In Proceedings of the Extended Abstracts of the 2018 CHI Conference on Human Factors in Computing Systems, Montreal, QC, Canada, 20 April 2018; pp. 1–8. [Google Scholar]
- Martínez-Borba, V.; Suso-Ribera, C.; Díaz-García, A.; Salat-Batlle, J.; Castilla, D.; Zaragoza, I.; García-Palacios, A.; Sánchez-Raya, J. Mhealth for the monitoring of brace compliance and wellbeing in adolescents with idiopathic scoliosis: Study protocol for a feasibility study. Int. J. Environ. Res. Public Health 2021, 18, 7767. [Google Scholar] [CrossRef]
- Zhu, C.; Wu, Q.; Xiao, B.; Wang, J.; Luo, C.; Yu, Q.; Liu, L.; Song, Y. A compliance real-time monitoring system for the management of the brace usage in adolescent idiopathic scoliosis patients: A pilot study. BMC Musculoskelet. Disord. 2021, 22, 152. [Google Scholar] [CrossRef]
- Katz, D.E.; Herring, J.A.; Browne, R.H.; Kelly, D.M.; Birch, J.G. Brace wear control of curve progression in adolescent idiopathic scoliosis. J. Bone Jt. Surg. Am. 2010, 92, 1343–1352. [Google Scholar] [CrossRef] [PubMed]
- Aulisa, A.G.; Giordano, M.; Falciglia, F.; Marzetti, E.; Poscia, A.; Guzzanti, V. Correlation between compliance and brace treatment in juvenile and adolescent idiopathic scoliosis: Sosort 2014 award winner. Scoliosis 2014, 9, 6. [Google Scholar] [CrossRef]
- Morton, A.; Riddle, R.; Buchanan, R.; Katz, D.; Birch, J. Accuracy in the prediction and estimation of adherence to bracewear before and during treatment of adolescent idiopathic scoliosis. J. Pediatr. Orthop. 2008, 28, 336–341. [Google Scholar] [CrossRef]
- Zang, Y.; Zhang, F.; Di, C.-A.; Zhu, D. Advances of flexible pressure sensors toward artificial intelligence and health care applications. Mater. Horiz. 2015, 2, 140–156. [Google Scholar] [CrossRef]
- Huang, Y.; Fan, X.; Chen, S.C.; Zhao, N. Emerging technologies of flexible pressure sensors: Materials, modeling, devices, and manufacturing. Adv. Funct. Mater. 2019, 29, 1808509. [Google Scholar] [CrossRef]
- Karol, L.A.; Virostek, D.; Felton, K.; Wheeler, L. Effect of compliance counseling on brace use and success in patients with adolescent idiopathic scoliosis. J. Bone Jt. Surg. Am. 2016, 98, 9–14. [Google Scholar] [CrossRef]
- Rahimi, S.; Kiaghadi, A.; Fallahian, N. Effective factors on brace compliance in idiopathic scoliosis: A literature review. Disabil. Rehabil. Assist. Technol. 2020, 15, 917–923. [Google Scholar] [CrossRef]
- Naziri, Q.; Detolla, J.; Hayes, W.; Burekhovich, S.A.; Merola, A.; Akamnanu, C.; Paulino, C.B. A systematic review of all smart phone applications specifically aimed for use as a scoliosis screening tool. J. Long-Term Eff. Med. Implant. 2018, 28, 25–30. [Google Scholar] [CrossRef]
- Monticone, M.; Ambrosini, E.; Cazzaniga, D.; Rocca, B.; Ferrante, S. Active self-correction and task-oriented exercises reduce spinal deformity and improve quality of life in subjects with mild adolescent idiopathic scoliosis. Results of a randomised controlled trial. Eur. Spine J. 2014, 23, 1204–1214. [Google Scholar] [CrossRef]
- Schreiber, S.; Parent, E.C.; Moez, E.K.; Hedden, D.M.; Hill, D.; Moreau, M.J.; Lou, E.; Watkins, E.M.; Southon, S.C. The effect of schroth exercises added to the standard of care on the quality of life and muscle endurance in adolescents with idiopathic scoliosis-an assessor and statistician blinded randomized controlled trial: “Sosort 2015 award winner”. Scoliosis 2015, 10, 24. [Google Scholar] [CrossRef] [PubMed]
- Williams, M.A.; Heine, P.J.; Williamson, E.M.; Toye, F.; Dritsaki, M.; Petrou, S.; Crossman, R.; Lall, R.; Barker, K.L.; Fairbank, J.; et al. Active treatment for idiopathic adolescent scoliosis (activates): A feasibility study. Health Technol. Assess. 2015, 19, 1–242. [Google Scholar] [CrossRef] [PubMed]
- Kuru, T.; Yeldan, İ.; Dereli, E.E.; Özdinçler, A.R.; Dikici, F.; Çolak, İ. The efficacy of three-dimensional schroth exercises in adolescent idiopathic scoliosis: A randomised controlled clinical trial. Clin. Rehabil. 2016, 30, 181–190. [Google Scholar] [CrossRef]
- Park, J.; Chung, S.Y.; Park, J.H. Real-time exercise feedback through a convolutional neural network: A machine learning-based motion-detecting mobile exercise coaching application. Yonsei Med. J. 2022, 63, S34–S42. [Google Scholar] [CrossRef] [PubMed]
| Mobile Application Market Review | |
| Inclusion Criteria | Exclusion Criteria |
| Available to the public (with or without payment) Self-contained product Centered on supporting brace treatments for patients with scoliosis | Irrelevant to scoliosis Only provided general information about scoliosis Focused only on the diagnosis or surgical treatment of scoliosis Developed for healthcare professionals |
| Literature Review | |
| Inclusion Criteria | Exclusion Criteria |
| Available in full text Address patients with scoliosis Refer to the development and use of mobile apps as tools specific to monitoring brace wearing compliance | Not available in full text Not centered on patients with scoliosis Did not involve any types of digital tools Refer to digital tools in different contexts, such as developing sensors, using as digital scoliometers, and designing braces, which were not directly related to the monitoring of brace compliance Ongoing research |
| App Name | BeMobil Orthotimer | BraceTrack for Scoliosis | BraceWyse | Brace Rite Scoliosis | MyScoliCare | Scoliosis Tracker | SER System | Spinamic | Pain Monitor | WeChat Mini Program |
|---|---|---|---|---|---|---|---|---|---|---|
| Data acquisition | ||||||||||
| Scoliosis severity check | . | . | . | . | . | V | . | V | . | . |
| Brace wearing time import | Automatic | Manual | Automatic | Automatic | Manual | Manual | Automatic | Manual | . | Manual |
| Brace connection with sensors | NFC 1 | . | NFC 2 | Bluetooth 2 | . | . | Bluetooth 2 | . | . | Bluetooth 3 |
| Compliance enhancement | ||||||||||
| Goal setting | . | V | . | V | . | . | . | . | . | . |
| Data visualization | V(graph) | V(graph + calender) | V(graphs) | V(graphs) | V(text) | . | V(graph) | V(graph) | . | V |
| Motivation | . | V(text) | . | V(text) | V(point) | V(text) | . | V(point,notify) | V(notify) | . |
| Testimonial and practical tips | V | . | . | . | . | V | . | . | . | . |
| Educational components | ||||||||||
| General information of scoliosis | V(quiz) | . | . | V | . | V | . | . | . | . |
| PSSE | . | . | . | . | V(Schroth) | . | V | . | . | . |
| Additional functionalities | ||||||||||
| Brace wearing time export | V(CSV) | V(PDF) | V(CSV) | . | . | . | . | . | . | . |
| Direct communication | . | V | V | . | . | V | . | Unknown | . | V |
| Appointment reminder | V | . | . | . | V | V | . | . | . | . |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cho, H.E.; Jang, C.W.; Cho, S.R.; Choi, W.A.; Park, J.H. Mobile Apps to Improve Brace-Wearing Compliance in Patients with Idiopathic Scoliosis: A Quality Analysis, Functionality Review and Future Directions. J. Clin. Med. 2023, 12, 1972. https://doi.org/10.3390/jcm12051972
Cho HE, Jang CW, Cho SR, Choi WA, Park JH. Mobile Apps to Improve Brace-Wearing Compliance in Patients with Idiopathic Scoliosis: A Quality Analysis, Functionality Review and Future Directions. Journal of Clinical Medicine. 2023; 12(5):1972. https://doi.org/10.3390/jcm12051972
Chicago/Turabian StyleCho, Han Eol, Chan Woong Jang, Sung Rae Cho, Won Ah Choi, and Jung Hyun Park. 2023. "Mobile Apps to Improve Brace-Wearing Compliance in Patients with Idiopathic Scoliosis: A Quality Analysis, Functionality Review and Future Directions" Journal of Clinical Medicine 12, no. 5: 1972. https://doi.org/10.3390/jcm12051972
APA StyleCho, H. E., Jang, C. W., Cho, S. R., Choi, W. A., & Park, J. H. (2023). Mobile Apps to Improve Brace-Wearing Compliance in Patients with Idiopathic Scoliosis: A Quality Analysis, Functionality Review and Future Directions. Journal of Clinical Medicine, 12(5), 1972. https://doi.org/10.3390/jcm12051972






