Improving Adherence to a Home Rehabilitation Plan for Chronic Neck Pain through Immersive Virtual Reality: A Case Report
Abstract
1. Introduction
2. Methods
3. Case Presentation
3.1. Past and Present Medical History
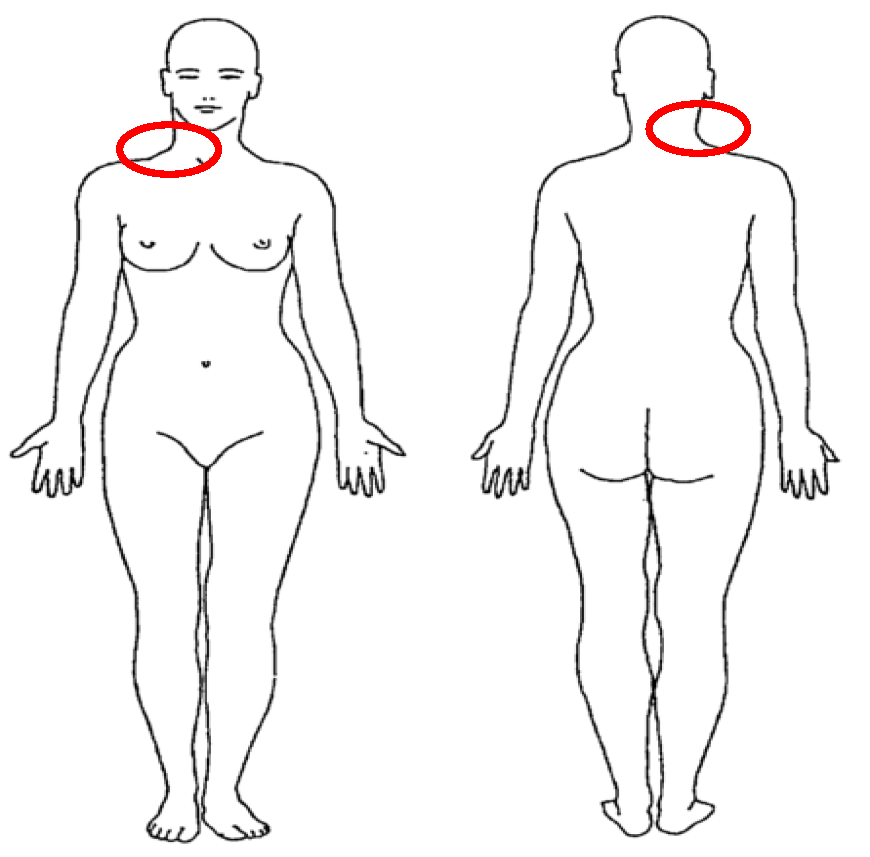
3.2. Objective Exam
3.3. Diagnostic Evaluation
4. Timeline
5. Intervention
5.1. First Follow-Up
5.2. Second Follow-Up
5.3. Third and Fourth Follow-Ups
6. Discussion
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hogg-Johnson, S.; Van Der Velde, G.; Carroll, L.; Holm, L.W.; Cassidy, J.D.; Guzman, J.; Côté, P.; Haldeman, S.; Ammendolia, C.; Carragee, E.J.; et al. The Burden and Determinants of Neck Pain in the General Population Results of the Bone and Joint Decade 2000–2010 Task Force on Neck Pain and Its Associated Disorders. Eur. Spine J. 2008, 17 (Suppl. 1), 39–51. [Google Scholar] [CrossRef]
- Thompson, D.P.; Urmston, M.; Oldham, J.A.; Woby, S.R. The association between cognitive factors, pain and disability in patients with idiopathic chronic neck pain. Disabil. Rehabil. 2010, 32, 1758–1767. [Google Scholar] [CrossRef]
- Côté, P.; Van Der Velde, G.; Cassidy, J.D.; Carroll, L.; Hogg-Johnson, S.; Holm, L.W.; Carragee, E.J.; Haldeman, S.; Nordin, M.; Hurwitz, E.L.; et al. Bone and Joint Decade 2000-2010 Task Force on Neck Pain and Its Associated Disorders The burden and determinants of neck pain in workers: Results of the Bone and Joint Decade 2000-2010 Task Force on Neck Pain and Its Associated Disorders. Spine 2008, 33 (Suppl. 4), S60–S74. [Google Scholar] [CrossRef] [PubMed]
- Raja, S.N.; Carr, D.B.; Cohen, M.; Finnerup, N.B.; Flor, H.; Gibson, S.; Keefe, F.J.; Mogil, J.S.; Ringkamp, M.; Sluka, K.A.; et al. The revised International Association for the Study of Pain definition of pain: Concepts, challenges, and compromises. Pain 2020, 161, 1976–1982. [Google Scholar] [CrossRef] [PubMed]
- Weigl, M.; Letzel, J.; Angst, F. Prognostic factors for the improvement of pain and disability following multidisciplinary rehabilitation in patients with chronic neck pain. BMC Musculoskelet. Disord. 2021, 22, 330. [Google Scholar] [CrossRef] [PubMed]
- Kori, S.M.R.; Miller, R.P.; Todd, D.D. Kinesiophobia: A new view of chronic pain behavior. Pain Manag. 1990, 3, 35–43. [Google Scholar]
- Dimitriadis, Z.; Kapreli, E.; Strimpakos, N.; Oldham, J. Do psychological states associate with pain and disability inchronic neck pain patients? Back Musculoskelet. Rehabil. 2015, 28, 797–802. [Google Scholar] [CrossRef] [PubMed]
- Pool, J.M.; Ostelo, R.W.J.G.; Knol, D.; Bouter, L.M.; de Vet, H.C.W. Are psychological factors prognostic indicators of outcome in patients with sub-acute neck pain? Man. Ther. 2010, 15, 111–116. [Google Scholar] [CrossRef]
- Asiri, F.; Reddy, R.S.; Tedla, J.S.; Almohiza, M.A.; Alshahrani, M.S.; Govindappa, S.C.; Sangadala, D.R. Kinesiophobia and its correlations with pain, proprioception, and functional performance among individuals with chronic neck pain. PLoS ONE 2021, 16, e0254262. [Google Scholar] [CrossRef] [PubMed]
- Xu, Y.; Song, Y.; Sun, D.; Fekete, G.; Gu, Y. Effect of Multi-Modal Therapies for Kinesiophobia Caused by Musculoskeletal Disorders: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2020, 17, 9439. [Google Scholar] [CrossRef] [PubMed]
- Blanpied, P.R.; Gross, A.R.; Elliott, J.M.; Devaney, L.L.; Clewley, D.; Walton, D.M.; Sparks, C.; Robertson, E.K.; Altman, R.D.; Beattie, P.; et al. Neck Pain: Revision 2017: Clinical Practice Guidelines Linked to the International Classification of Functioning, Disability and Health From the Orthopaedic Section of the American Physical Therapy Association. J. Orthop. Sports Phys. Ther. 2017, 47, A1–A83. [Google Scholar] [CrossRef] [PubMed]
- Bier, J.D.; Scholten-Peeters, W.J.M.; Staal, J.B.; Pool, J.; van Tulder, M.W.; Beekman, E.; Knoop, J.; Meerhoff, G.; Verhagen, A.P. Clinical Practice Guideline for Physical Therapy Assessment and Treatment in Patients with Nonspecific Neck Pain. Phys. Ther. 2018, 98, 162–171. [Google Scholar] [CrossRef] [PubMed]
- Monticone, M.; Ambrosini, E.; Cedraschi, C.; Rocca, B.; Fiorentini, R.; Restelli, M.; Gianola, S.; Ferrante, S.; Zanoli, G.; Moja, L. Cognitive Behavioral Treatment for Subacute and Chronic Neck Pain: A Cochrane Review. Spine 2015, 40, 1495–1504. [Google Scholar] [CrossRef]
- Gumaa, M.; Youssef, A.R. Is Virtual Reality Effective in Orthopedic Rehabilitation? A Systematic Review and Meta-Analysis. Phys. Ther. 2019, 99, 1304–1325. [Google Scholar] [CrossRef] [PubMed]
- Ahern, M.M.; Dean, L.V.; Stoddard, C.C.; Agrawal, A.; Kim, K.; Cook, C.E.; Garcia, A.G. The Effectiveness of Virtual Reality in Patients with Spinal Pain: A Systematic Review and Meta-Analysis. Pain Pract. 2020, 20, 656–675. [Google Scholar] [CrossRef]
- Pournajaf, S.; Goffredo, M.; Pellicciari, L.; Piscitelli, D.; Criscuolo, S.; Le Pera, D.; Damiani, C.; Franceschini, M. Effect of balance training using virtual reality-based serious games in individuals with total knee replacement: A randomized controlled trial. Ann. Phys. Rehabil. Med. 2022, 65, 10160917. [Google Scholar] [CrossRef]
- Nusser, M.; Knapp, S.; Kramer, M.; Krischak, G. Effects of virtual reality-based neckspecific sensorimotor training in patients with chronic neck pain: A randomized controlled pilot trial. J. Rehabil. Med. 2021, 53, jrm00151. [Google Scholar] [CrossRef]
- Tejera, D.M.; Beltran-Alacreu, H.; Canode- la-Cuerda, R.; Hernández, J.V.L.; Martín-Pintado-Zugasti, A.; Calvo-Lobo, C.; Gil-Martínez, A.; Fernández-Carnero, J. Effects of Virtual Reality versus Exercise on Pain, Functional, Somatosensory and Psychosocial Outcomes in Patients with Non-specific Chronic Neck Pain: A Randomized Clinical Trial. Int. J. Environ. Res. Public Health 2020, 17, 5950. [Google Scholar] [CrossRef]
- Meichenbaum, D.; Turk, D.C. Facilitating Treatment Adherence: A Practitioner’s Guidebook; Plenum Press: New York, NY, USA, 1987. [Google Scholar]
- Hutting, N.; Caneiro, J.P.; Ong’wen, O.M.; Miciak, M.; Roberts, L. Patient centered care in musculoskeletal practice: Key elements to support clinicians to focus on the person. Musculoskelet. Sci. Pract. 2022, 57, 102434. [Google Scholar] [CrossRef] [PubMed]
- Gagnier, J.J.; Kienle, G.; Altman, D.G.; Moher, D.; Sox, H.; Riley, D. The CARE guidelines: Consensus-based clinical case reporting guideline development CARE Group Collaborators. BMJ Case Rep. 2013, 2, 38–43. [Google Scholar] [CrossRef]
- Williamson, A.; Hoggart, B. Pain: A review of three commonly used pain rating scales. J. Clin. Nurs. 2005, 14, 798–804. [Google Scholar] [CrossRef] [PubMed]
- Finucane, L.M.; Downie, A.; Mercer, C.; Greenhalgh, S.M.; Boissonnault, W.G.; Pool- Goudzwaard, A.L.; Beneciuk, J.M.; Leech, R.L.; Selfe, J. International Framework for Red Flags for Potential Serious Spinal Pathologies. J. Orthop. Sports Phys. Ther. 2020, 50, 350–372. [Google Scholar] [CrossRef] [PubMed]
- Satpute, K.; Nalband, S.; Hall, T. The C0-C2 axial rotation test: Normal values, intra- and inter-rater reliability and correlation with the flexion rotation test in normal subjects. J. Man. Manip. Ther. 2019, 27, 92–98. [Google Scholar] [CrossRef] [PubMed]
- Rey-Eiriz, G.; Alburquerque-Sendín, F.; Barrera-Mellado, I.; Vallejo, F.J.M.; Fernández-De-Las-Peñas, C. Validity of the posterior-anterior middle cervical spine gliding test for the examination of intervertebral joint hypomobility in mechanical neck pain. J. Manip. Physiol. Ther. 2010, 33, 279–285. [Google Scholar] [CrossRef] [PubMed]
- Lindfren, K.A.; Leino, E.; Hakola, M.; Hamberg, J. Cervical spine rotation and lateral flexion combined motion in the examination of the thoracic outlet. Arch. Phys. Med. Rehabil. 1990, 71, 343–344. [Google Scholar] [PubMed]
- Paternostro-Sluga, T.; Grim-Stieger, M.; Posch, M.; Schuhfried, O.; Vacariu, G.; Mittermaier, C.; Bittner, C.; Fialka-Moser, V. Reliability and validity of the Medical Research Council (MRC) scale and a modified scale for testing muscle strength in patients with radial palsy. J. Rehabil. Med. 2008, 40, 665–671. [Google Scholar] [CrossRef]
- Domenech, M.A.; Sizer, P.S.; Dedrick, G.S.; McGalliard, M.K.; Brismee, J.M. The Deep Neck Flexor Endurance Test: Normative data scores in healthy adults. PMR 2011, 3, 105–110. [Google Scholar] [CrossRef]
- Monticone, M.; Ferrante, S.; Vernon, H.; Rocca, B.; Dal Farra, F.; Foti, C. Development of the Italian Version of the Neck Disability Index: Cross-cultural adaptation, factor analysis, reliability, validity, and sensitivity to change. Spine 2012, 37, E1038–E1044. [Google Scholar] [CrossRef]
- Monticone, M.; Giorgi, I.; Baiardi, P.; Barbieri, M.; Rocca, B.; Bonezzi, C. Development of the Italian version of the Tampa Scale of Kinesiophobia (TSK-I): Cross-cultural adaptation, factor analysis, reliability, and validity. Spine 2010, 35, 1241–1246. [Google Scholar] [CrossRef] [PubMed]
- Fordyce, W.E.; Company, M.C. Behavioral Methods for Chronic Pain and Illness. Pain 1977, 3, 291–292. [Google Scholar] [CrossRef]
- Engel, G.L. The need for a new medical model: A challenge for biomedicine. Science 1977, 196, 129–136. [Google Scholar] [CrossRef] [PubMed]
- Wade, D.T. Rehabilitation—A new approach. Part two: The underlying theories. Clin. Rehabil. 2015, 29, 1145–1154. [Google Scholar] [CrossRef] [PubMed]
- Garcia, L.M.; Birckhead, B.J.; Krishnamurthy, P.; Sackman, J.; Mackey, I.G.; Louis, R.G.; Salmasi, V.; Maddox, T.; Darnall, B.D. An 8-Week Self-Administered At-Home Behavioral Skills-Based Virtual Reality Program for Chronic Low Back Pain: Double-Blind, Randomized, Placebo-Controlled Trial Conducted During COVID-19. J. Med. Internet Res. 2021, 23, e26292. [Google Scholar] [CrossRef] [PubMed]
- Price, J.; Rushton, A.; Tyros, I.; Tyros, V.; Heneghan, N.R. Effectiveness and optimal dosage of exercise training for chronic non-specific neck pain: A systematic review with a narrative synthesis. PLoS ONE 2020, 15, e0234511. [Google Scholar] [CrossRef]
- Baker, N.A.; Polhemus, A.H.; Ospina, E.H.; Feller, H.; Zenni, M.; Deacon, M.; DeGrado, G.; Basnet, S.; Driscoll, M. The State of Science in the Use of Virtual Reality in the Treatment of Acute and Chronic Pain: A Systematic Scoping Review. Clin. J. Pain 2022, 38, 424–441. [Google Scholar] [CrossRef] [PubMed]
- Malloy, K.M.; Milling, L.S. The effectiveness of virtual reality distraction for pain reduction: A systematic review. Clin. Psychol. Rev. 2010, 30, 1011–1018. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, H.G.; Richards, T.L.; Bills, A.R.; Van Oostrom, T.; Magula, J.; Seibel, E.J.; Sharar, S.R. Using fMRI to study the neural correlates of virtual reality analgesia. CNS Spectr. 2006, 11, 45–51. [Google Scholar] [CrossRef] [PubMed]
- Valet, M.; Sprenger, T.; Boecker, H.; Willoch, F.; Rummeny, E.; Conrad, B.; Erhard, P.; Tolle, T.R. Distraction modulates connectivity of the cingulofrontal cortex and the midbrain during pain—An fMRI analysis. Pain 2004, 109, 399–408. [Google Scholar] [CrossRef]
- Rossettini, G.; Carlino, E.; Testa, M. Clinical relevance of contextual factors as triggers of placebo and nocebo effects in musculoskeletal pain. BMC Musculoskelet. Disord. 2018, 19, 27. [Google Scholar] [CrossRef]
- Gallego-Sendarrubias, G.M.; Voogt, L.; Arias-Buría, J.L.; Bialosky, J.; Fernández-de-Las-Peñas, C. Can Patient Expectations Modulate the Short-Term Effects of Dry Needling on Sensitivity Outcomes Patients with Mechanical Neck Pain? A Randomized Clinical Trial. Pain Med. 2022, 23, 965–976. [Google Scholar] [CrossRef]



| Movement | Degrees (°) |
|---|---|
| Flexion | 40 |
| Extension | 70 |
| Right rotation | 35 |
| Left rotation | 75 |
| Right lateral flexion | 35 |
| Left lateral flexion | 35 |
| Day | Repetition (n°) | Repetition Length (s) | Rest between Repetition (s) |
|---|---|---|---|
| 1 | 3 | 120 | 60 |
| 2 | 3 | 120 | 60 |
| 3 | 3 | 150 | 60 |
| 4 | 4 | 150 | 60 |
| 5 | 4 | 180 | 60 |
| Day | Repetition (n°) | Repetition Length (s) | Rest between Repetition (s) |
|---|---|---|---|
| 1 | 3 | 210 | 60 |
| 2 | 4 | 210 | 60 |
| 3 | 3 | 240 | 60 |
| 4 | 4 | 240 | 60 |
| 5 | 3 | 270 | 60 |
| Day | Repetition (n°) | Repetition Length (s) | Rest between Repetition (s) |
|---|---|---|---|
| 1 | 4 | 270 | 60 |
| 2 | 4 | 300 | 60 |
| 3 | 4 | 330 | 60 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cioeta, M.; Pournajaf, S.; Goffredo, M.; Giovannico, G.; Franceschini, M. Improving Adherence to a Home Rehabilitation Plan for Chronic Neck Pain through Immersive Virtual Reality: A Case Report. J. Clin. Med. 2023, 12, 1926. https://doi.org/10.3390/jcm12051926
Cioeta M, Pournajaf S, Goffredo M, Giovannico G, Franceschini M. Improving Adherence to a Home Rehabilitation Plan for Chronic Neck Pain through Immersive Virtual Reality: A Case Report. Journal of Clinical Medicine. 2023; 12(5):1926. https://doi.org/10.3390/jcm12051926
Chicago/Turabian StyleCioeta, Matteo, Sanaz Pournajaf, Michela Goffredo, Giuseppe Giovannico, and Marco Franceschini. 2023. "Improving Adherence to a Home Rehabilitation Plan for Chronic Neck Pain through Immersive Virtual Reality: A Case Report" Journal of Clinical Medicine 12, no. 5: 1926. https://doi.org/10.3390/jcm12051926
APA StyleCioeta, M., Pournajaf, S., Goffredo, M., Giovannico, G., & Franceschini, M. (2023). Improving Adherence to a Home Rehabilitation Plan for Chronic Neck Pain through Immersive Virtual Reality: A Case Report. Journal of Clinical Medicine, 12(5), 1926. https://doi.org/10.3390/jcm12051926









