Cerclage Wiring Improves Biomechanical Stability in Distal Tibia Spiral Fractures Treated by Intramedullary Nailing
Abstract
1. Introduction
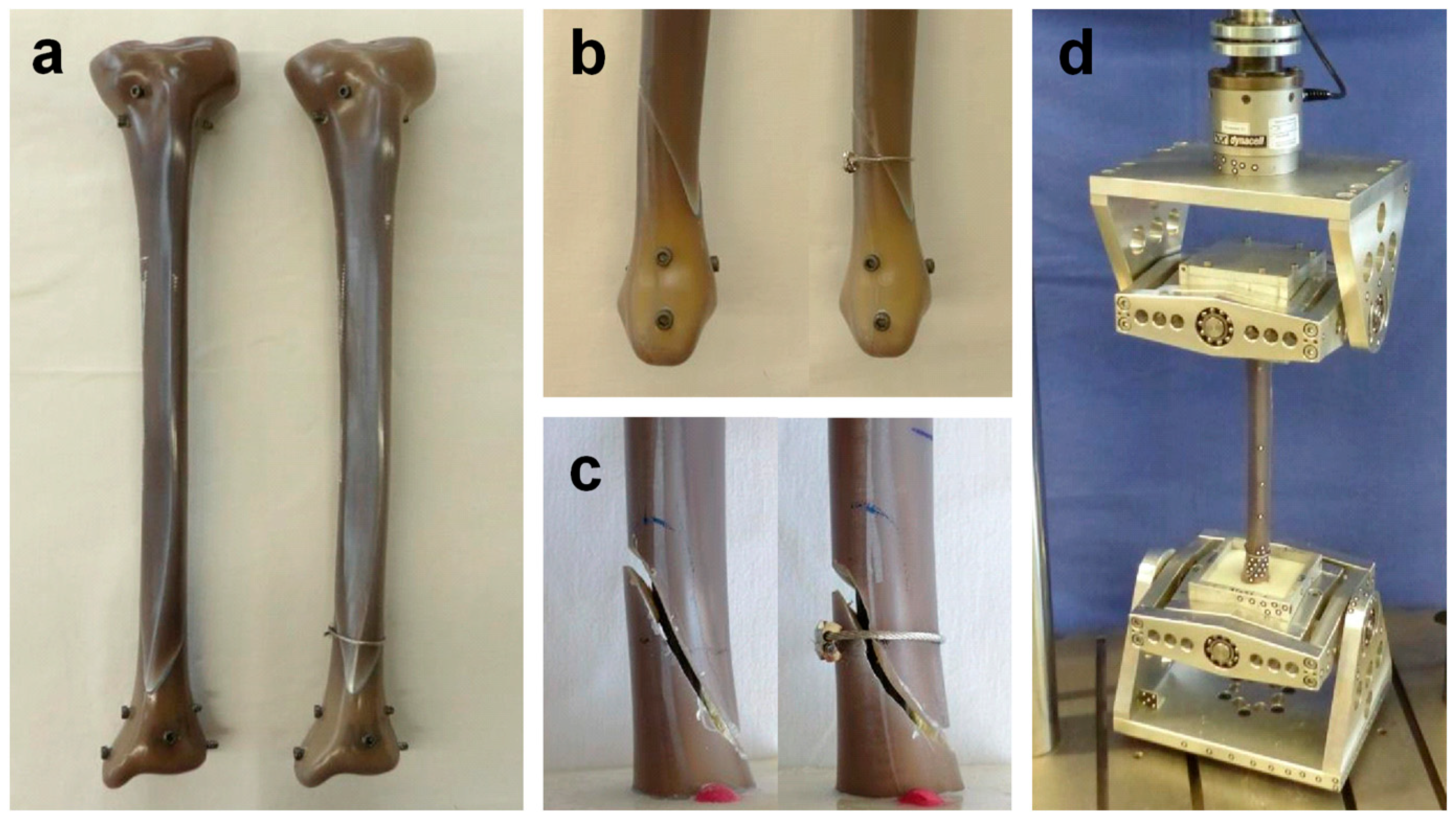
2. Materials and Methods
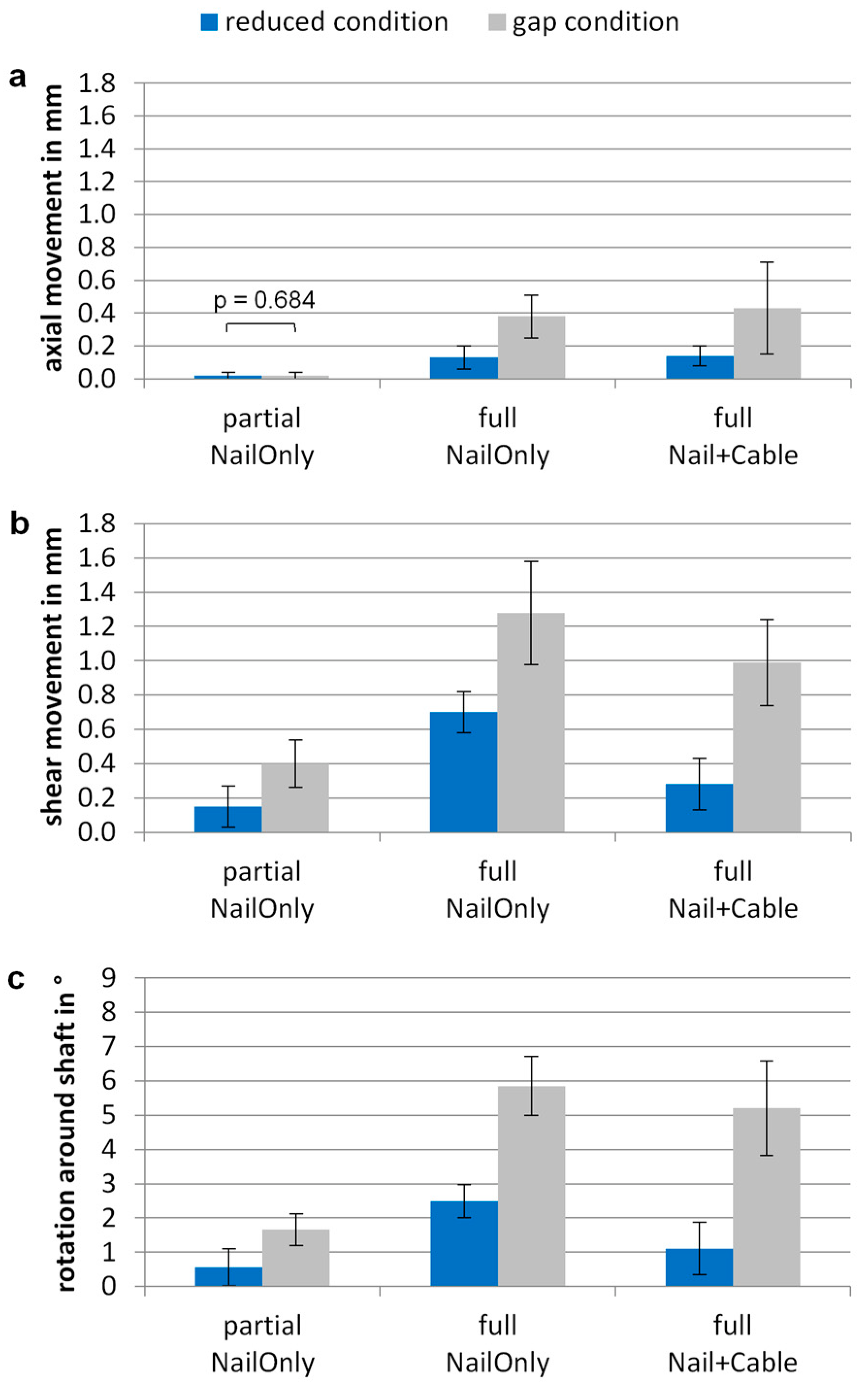
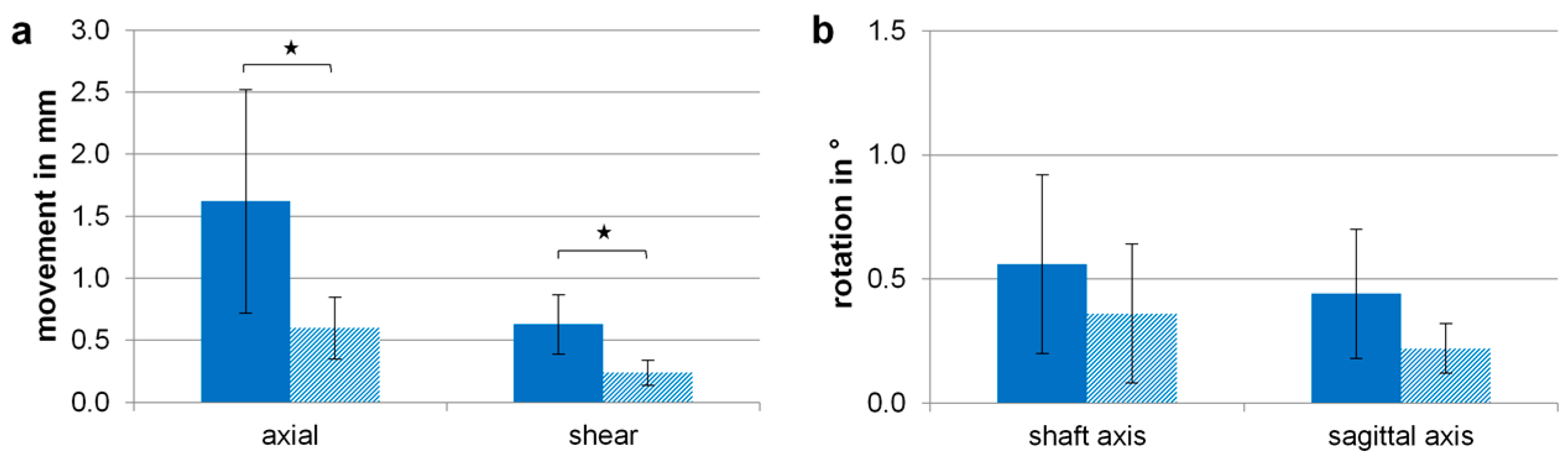
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Larsen, P.; Elsoe, R.; Hansen, S.H.; Graven-Nielsen, T.; Laessoe, U.; Rasmussen, S. Incidence and epidemiology of tibial shaft fractures. Injury 2015, 46, 746–750. [Google Scholar] [CrossRef] [PubMed]
- White, R.; Camuso, M. AO Surgery Reference-Intramedullary Nailing. Available online: https://surgeryreference.aofoundation.org/orthopedic-trauma/adult-trauma/tibial-shaft/simple-fracture-spiral/intramedullary-nailing#aftercare (accessed on 6 February 2023).
- Baer, M.; Neuhaus, V.; Pape, H.C.; Ciritsis, B. Influence of mobilization and weight bearing on in-hospital outcome in geriatric patients with hip fractures. SICOT J. 2019, 5, 4. [Google Scholar] [CrossRef] [PubMed]
- Consigliere, P.; Iliopoulos, E.; Ads, T.; Trompeter, A. Early versus delayed weight bearing after surgical fixation of distal femur fractures: A non-randomized comparative study. Eur. J. Orthop. Surg. Traumatol. 2019, 29, 1789–1794. [Google Scholar] [CrossRef] [PubMed]
- Kammerlander, C.; Pfeufer, D.; Lisitano, L.A.; Mehaffey, S.; Bocker, W.; Neuerburg, C. Inability of Older Adult Patients with Hip Fracture to Maintain Postoperative Weight-Bearing Restrictions. J. Bone Joint Surg. Am. 2018, 100, 936–941. [Google Scholar] [CrossRef]
- Sandriesser, S.; Förch, S.; Mayr, E.; Schrödl, F.; von Rüden, C.; Augat, P. Supplemental cerclage wiring in angle stable plate fixation of distal tibial spiral fractures enables immediate post-operative full weight-bearing: A biomechanical analysis. Eur. J. Trauma Emerg. Surg. 2020, 48, 621–628. [Google Scholar] [CrossRef]
- Förch, S.; Sandriesser, S.; Mayr, E.; Schrödl, F.; von Rüden, C.; Augat, P. Biomechanical comparison of different cerclage types in addition to an angle stable plate osteosynthesis of distal tibial fractures. Injury 2021, 52, 2126–2130. [Google Scholar] [CrossRef]
- Förch, S.; Reuter, J.; von der Helm, F.; Lisitano, L.; Hartwig, C.; Sandriesser, S.; Nuber, S.; Mayr, E. A minimally invasive cerclage of the tibia in a modified Goetze technique: Operative technique and first clinical results. Eur. J. Trauma Emerg. Surg. 2021, 48, 3115–3122. [Google Scholar] [CrossRef]
- Förch, S.; Sandriesser, S.; Fenwick, A.; Mayr, E. Impairment of the blood supply by cerclages: Myth or reality? An overview of the experimental study situation. Unfallchirurg 2020, 124, 231–240. [Google Scholar] [CrossRef]
- Bleeker, N.J.; van de Wall, B.J.M.; FFA, I.J.; Doornberg, J.N.; Kerkhoffs, G.; Jaarsma, R.L.; Knobe, M.; Link, B.C.; Babst, R.; Beeres, F.J.P. Plate vs. nail for extra-articular distal tibia fractures: How should we personalize surgical treatment? A meta-analysis of 1332 patients. Injury 2021, 52, 345–357. [Google Scholar] [CrossRef]
- Ekman, E.; Lehtimäki, K.; Syvänen, J.; Saltychev, M. Comparison Between Nailing and Plating in the Treatment of Distal Tibial Fractures: A Meta-Analysis. Scand. J. Surg. 2021, 110, 115–122. [Google Scholar] [CrossRef]
- Habernek, H. Percutaneous cerclage wiring and interlocking nailing for treatment of torsional fractures of the tibia. Clin. Orthop. Relat. Res. 1991, 267, 164–168. [Google Scholar] [CrossRef]
- Huang, M.T.; Lin, C.J. Percutaneous cerclage wiring-assisted interlocking nailing for torsional tibia fractures: A modification with improved safety and simplicity. J. Trauma 2011, 71, 1054–1058. [Google Scholar] [CrossRef]
- Augat, P.; Burger, J.; Schorlemmer, S.; Henke, T.; Peraus, M.; Claes, L. Shear movement at the fracture site delays healing in a diaphyseal fracture model. J. Orthop. Res. 2003, 21, 1011–1017. [Google Scholar] [CrossRef]
- Bliemel, C.; Anrich, D.; Knauf, T.; Oberkircher, L.; Eschbach, D.; Klasan, A.; Debus, F.; Ruchholtz, S.; Baumlein, M. More than a reposition tool: Additional wire cerclage leads to increased load to failure in plate osteosynthesis for supracondylar femoral shaft fractures. Arch. Orthop. Trauma Surg. 2020, 141, 1197–1205. [Google Scholar] [CrossRef]
- Perren, S.M.; Fernandez Dell’oca, A.; Regazzoni, P. Fracture Fixation Using Cerclage, Research Applied to Surgery. Acta Chir. Orthop. Traumatol. Cech. 2015, 82, 389–397. [Google Scholar]
- Gordon, K.; Winkler, M.; Hofstadter, T.; Dorn, U.; Augat, P. Managing Vancouver B1 fractures by cerclage system compared to locking plate fixation-a biomechanical study. Injury 2016, 47 (Suppl. S2), S51–S57. [Google Scholar] [CrossRef]
- Apivatthakakul, T.; Siripipattanamongkol, P.; Oh, C.W.; Sananpanich, K.; Phornphutkul, C. Safe zones and a technical guide for cerclage wiring of the femur: A computed topographic angiogram (CTA) study. Arch. Orthop. Trauma Surg. 2018, 138, 43–50. [Google Scholar] [CrossRef]
- Codesido, P.; Mejia, A.; Riego, J.; Ojeda-Thies, C. Subtrochanteric fractures in elderly people treated with intramedullary fixation: Quality of life and complications following open reduction and cerclage wiring versus closed reduction. Arch. Orthop. Trauma Surg. 2017, 137, 1077–1085. [Google Scholar] [CrossRef]
- Hoskins, W.; Bingham, R.; Joseph, S.; Liew, D.; Love, D.; Bucknill, A.; Oppy, A.; Griffin, X. Subtrochanteric fracture: The effect of cerclage wire on fracture reduction and outcome. Injury 2015, 46, 1992–1995. [Google Scholar] [CrossRef]
- Ottesen, T.D.; McLynn, R.P.; Galivanche, A.R.; Bagi, P.S.; Zogg, C.K.; Rubin, L.E.; Grauer, J.N. Increased complications in geriatric patients with a fracture of the hip whose postoperative weight-bearing is restricted: An analysis of 4918 patients. Bone Joint J. 2018, 100-B, 1377–1384. [Google Scholar] [CrossRef]
- Pfeufer, D.; Zeller, A.; Mehaffey, S.; Bocker, W.; Kammerlander, C.; Neuerburg, C. Weight-bearing restrictions reduce postoperative mobility in elderly hip fracture patients. Arch. Orthop. Trauma Surg. 2019, 139, 1253–1259. [Google Scholar] [CrossRef] [PubMed]
- Paulsson, M.; Ekholm, C.; Jonsson, E.; Geijer, M.; Rolfson, O. Immediate Full Weight-Bearing Versus Partial Weight-Bearing After Plate Fixation of Distal Femur Fractures in Elderly Patients. A Randomized Controlled Trial. Geriatr. Orthop. Surg. Rehabil. 2021, 12, 21514593211055889. [Google Scholar] [CrossRef] [PubMed]
- Smeeing, D.P.J.; Houwert, R.M.; Briet, J.P.; Groenwold, R.H.H.; Lansink, K.W.W.; Leenen, L.P.H.; van der Zwaal, P.; Hoogendoorn, J.M.; van Heijl, M.; Verleisdonk, E.J.; et al. Weight-bearing or non-weight-bearing after surgical treatment of ankle fractures: A multicenter randomized controlled trial. Eur. J. Trauma Emerg. Surg. 2020, 46, 121–130. [Google Scholar] [CrossRef] [PubMed]
- Gross, S.C.; Galos, D.K.; Taormina, D.P.; Crespo, A.; Egol, K.A.; Tejwani, N.C. Can Tibial Shaft Fractures Bear Weight After Intramedullary Nailing? A Randomized Controlled Trial. J. Orthop. Trauma 2016, 30, 370–375. [Google Scholar] [CrossRef] [PubMed]
- Hoegel, F.W.; Hoffmann, S.; Weninger, P.; Bühren, V.; Augat, P. Biomechanical comparison of locked plate osteosynthesis, reamed and unreamed nailing in conventional interlocking technique, and unreamed angle stable nailing in distal tibia fractures. J. Trauma Acute Care Surg. 2012, 73, 933–938. [Google Scholar] [CrossRef]
- Claes, L. Mechanobiology of fracture healing part 2:Relevance for internal fixation of fractures. Unfallchirurg 2017, 120, 23–31. [Google Scholar] [CrossRef]
- Claes, L. Mechanobiology of fracture healing part 1:Principles. Unfallchirurg 2017, 120, 14–22. [Google Scholar] [CrossRef]
- Epari, D.R.; Kassi, J.P.; Schell, H.; Duda, G.N. Timely fracture-healing requires optimization of axial fixation stability. J. Bone Joint Surg. Am. 2007, 89, 1575–1585. [Google Scholar] [CrossRef]
- Högel, F.; Gerber, C.; Bühren, V.; Augat, P. Reamed intramedullary nailing of diaphyseal tibial fractures: Comparison of compression and non-compression nailing. Eur. J. Trauma Emerg. Surg. 2013, 39, 73–77. [Google Scholar] [CrossRef]
- Gonschorek, O.; Hofmann, G.O.; Bühren, V. Interlocking compression nailing: A report on 402 applications. Arch. Orthop. Trauma Surg. 1998, 117, 430–437. [Google Scholar] [CrossRef]
- Bisaccia, M.; Cappiello, A.; Meccariello, L.; Rinonapoli, G.; Falzarano, G.; Medici, A.; Vicente, C.I.; Piscitelli, L.; Stano, V.; Bisaccia, O.; et al. Nail or plate in the management of distal extra-articular tibial fracture, what is better? Valutation of outcomes. SICOT J. 2018, 4, 2. [Google Scholar] [CrossRef]
- Hu, L.; Xiong, Y.; Mi, B.; Panayi, A.C.; Zhou, W.; Liu, Y.; Liu, J.; Xue, H.; Yan, C.; Abududilibaier, A.; et al. Comparison of intramedullary nailing and plate fixation in distal tibial fractures with metaphyseal damage: A meta-analysis of randomized controlled trials. J. Orthop. Surg. Res. 2019, 14, 30. [Google Scholar] [CrossRef]
- Casstevens, C.; Le, T.; Archdeacon, M.T.; Wyrick, J.D. Management of extra-articular fractures of the distal tibia: Intramedullary nailing versus plate fixation. J. Am. Acad. Orthop. Surg. 2012, 20, 675–683. [Google Scholar] [CrossRef]
- Mao, Z.; Wang, G.; Zhang, L.; Zhang, L.; Chen, S.; Du, H.; Zhao, Y.; Tang, P. Intramedullary nailing versus plating for distal tibia fractures without articular involvement: A meta-analysis. J. Orthop. Surg. Res. 2015, 10, 95. [Google Scholar] [CrossRef]
- Augat, P.; Penzkofer, R.; Nolte, A.; Maier, M.; Panzer, S.; v Oldenburg, G.; Pueschl, K.; Simon, U.; Buhren, V. Interfragmentary movement in diaphyseal tibia fractures fixed with locked intramedullary nails. J. Orthop. Trauma 2008, 22, 30–36. [Google Scholar] [CrossRef]
- Claes, L.; Eckert-Hubner, K.; Augat, P. The fracture gap size influences the local vascularization and tissue differentiation in callus healing. Langenbecks Arch. Surg. 2003, 388, 316–322. [Google Scholar] [CrossRef]
- Gardner, M.J.; Silva, M.J.; Krieg, J.C. Biomechanical testing of fracture fixation constructs: Variability, validity, and clinical applicability. J. Am. Acad. Orthop. Surg. 2012, 20, 86–93. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Förch, S.; Sandriesser, S.; von Rüden, C.; Mayr, E.; Augat, P. Cerclage Wiring Improves Biomechanical Stability in Distal Tibia Spiral Fractures Treated by Intramedullary Nailing. J. Clin. Med. 2023, 12, 1770. https://doi.org/10.3390/jcm12051770
Förch S, Sandriesser S, von Rüden C, Mayr E, Augat P. Cerclage Wiring Improves Biomechanical Stability in Distal Tibia Spiral Fractures Treated by Intramedullary Nailing. Journal of Clinical Medicine. 2023; 12(5):1770. https://doi.org/10.3390/jcm12051770
Chicago/Turabian StyleFörch, Stefan, Sabrina Sandriesser, Christian von Rüden, Edgar Mayr, and Peter Augat. 2023. "Cerclage Wiring Improves Biomechanical Stability in Distal Tibia Spiral Fractures Treated by Intramedullary Nailing" Journal of Clinical Medicine 12, no. 5: 1770. https://doi.org/10.3390/jcm12051770
APA StyleFörch, S., Sandriesser, S., von Rüden, C., Mayr, E., & Augat, P. (2023). Cerclage Wiring Improves Biomechanical Stability in Distal Tibia Spiral Fractures Treated by Intramedullary Nailing. Journal of Clinical Medicine, 12(5), 1770. https://doi.org/10.3390/jcm12051770






