Cranial Shape in Infants Aged One Month Can Predict the Severity of Deformational Plagiocephaly at the Age of Six Months
Abstract
:1. Introduction
2. Materials and Methods
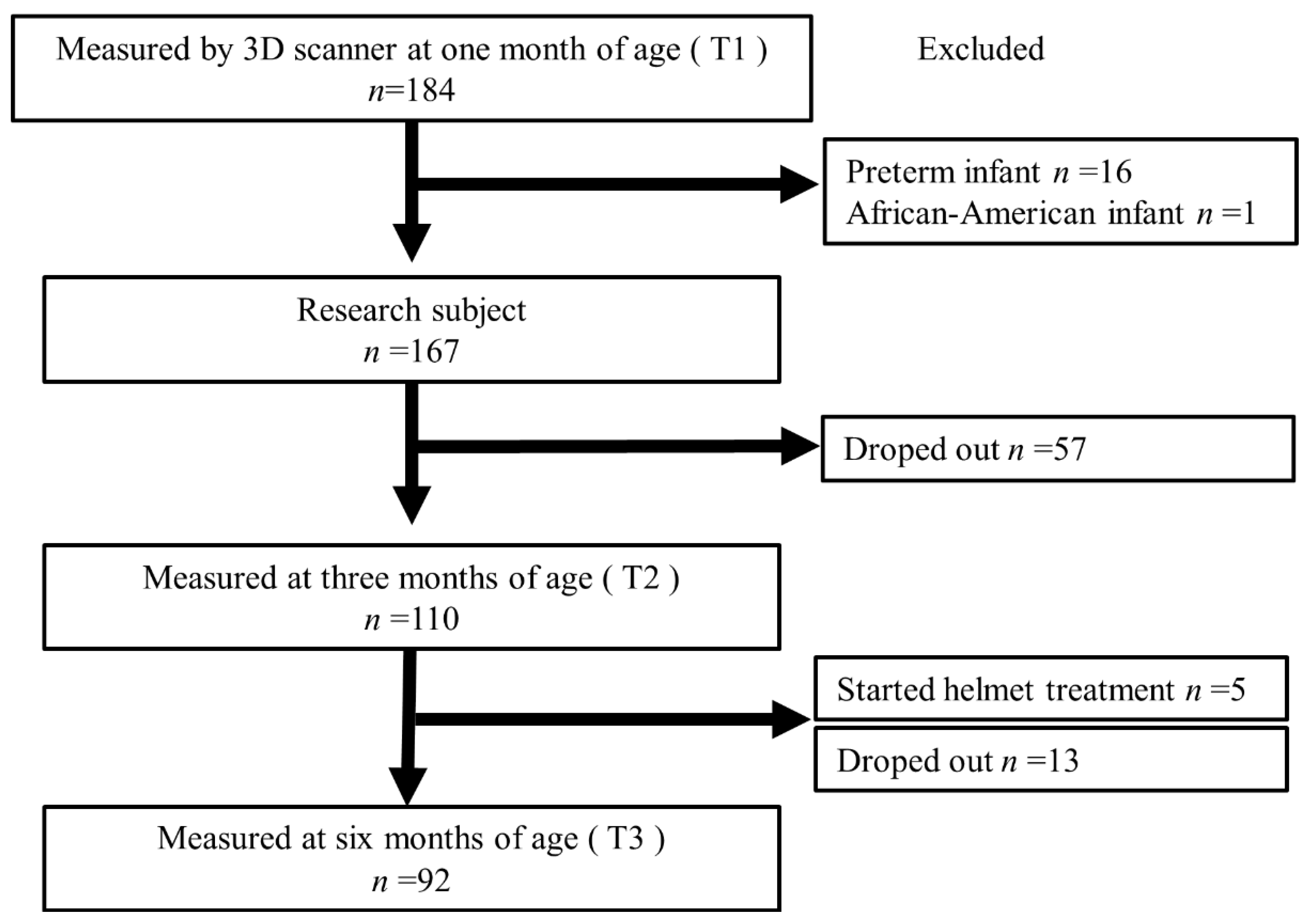
2.1. Study Population
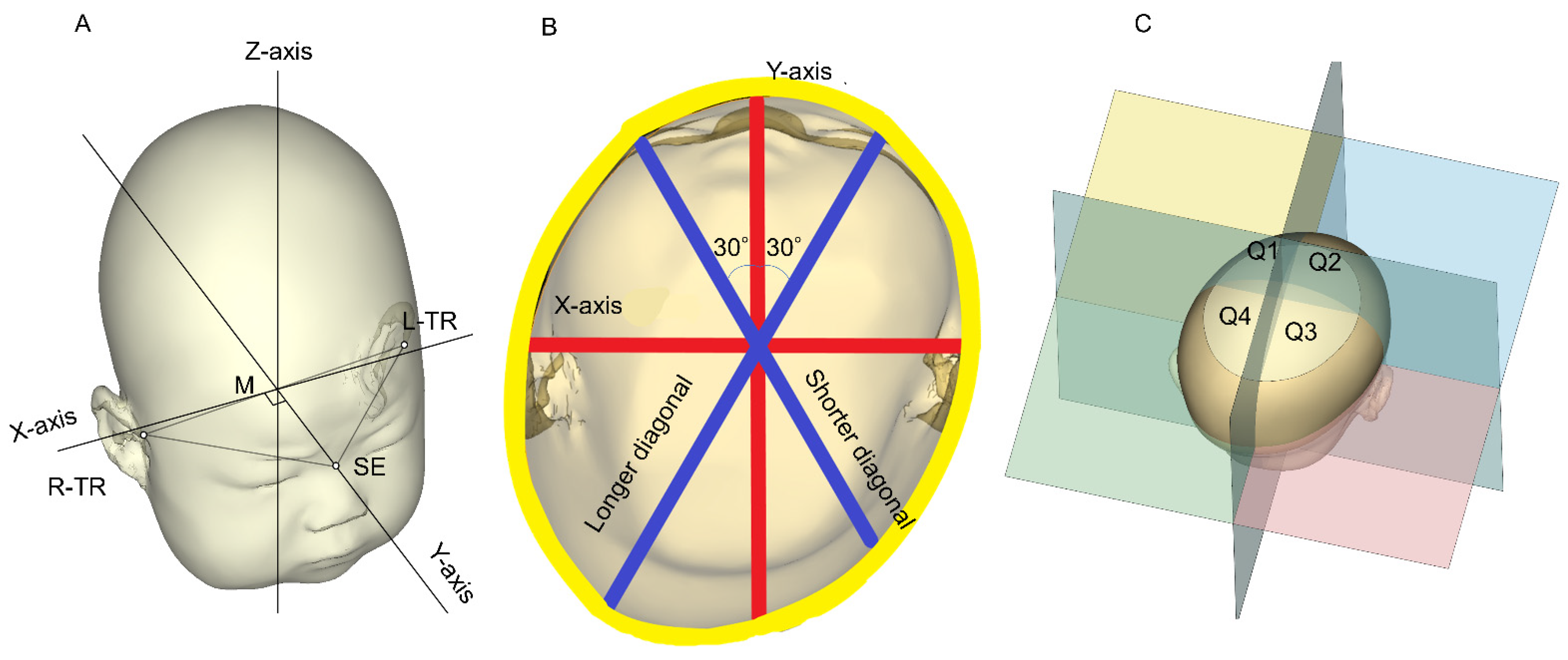
2.2. Data Acquisition
2.3. Data Analysis
2.4. Study Design and Statistical Analyses
3. Results
3.1. Background Characteristics
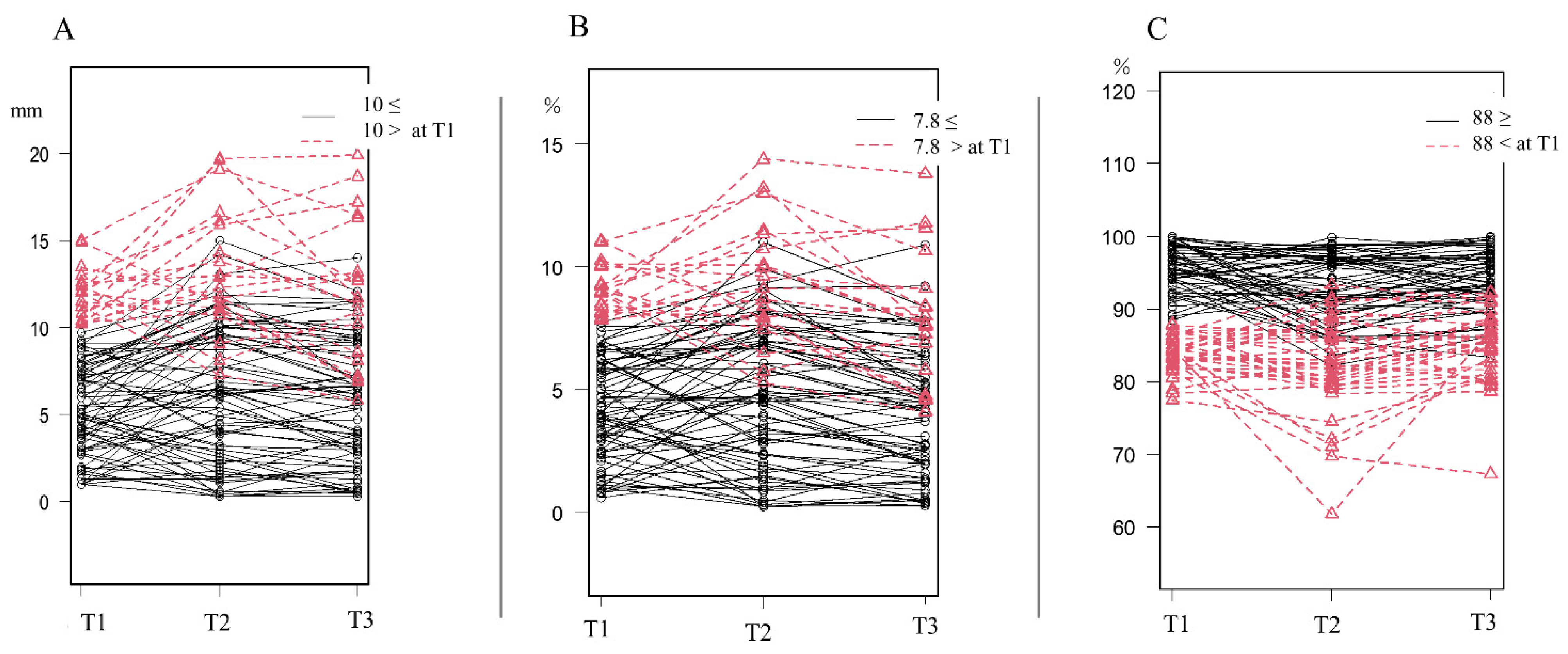
3.2. Changes in Symmetry-Related Cranial Parameters
3.3. Prevalence and Severity of DP
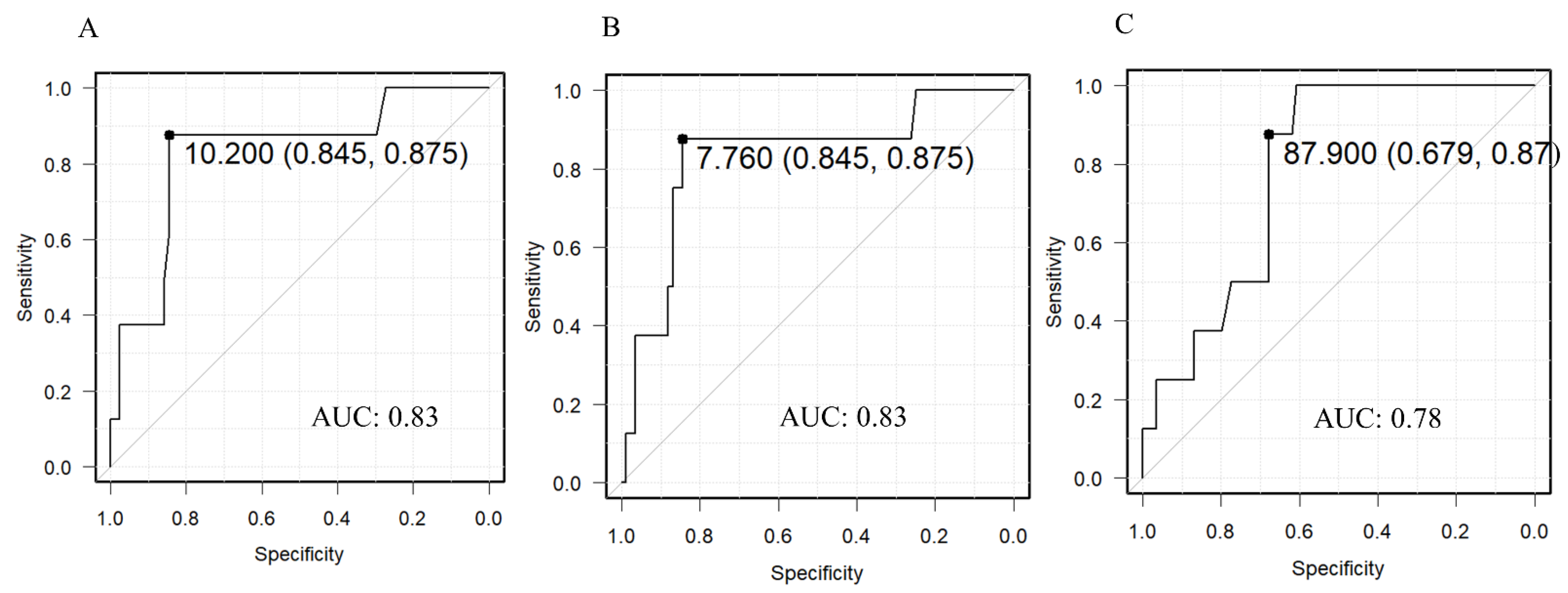
3.4. Predictive Threshold of Severity at T1
4. Discussion
4.1. Characteristics of the Infants
4.2. Natural Course and Prediction of DP
4.3. Initiation of CHT
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Mawji, A.; Vollman, A.R.; Hatfield, J.; McNeil, D.A.; Sauvé, R. The incidence of positional plagiocephaly: A cohort study. Pediatrics 2013, 132, 298–304. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dec, W.; Warren, S.M. Current concepts in deformational plagiocephaly. J. Craniofac. Surg. 2011, 22, 6–8. [Google Scholar] [CrossRef] [PubMed]
- Argenta, L.; David, L.; Thompson, J. Clinical classification of positional plagiocephaly. J. Craniofac. Surg. 2004, 15, 368–372. [Google Scholar] [CrossRef] [PubMed]
- Aihara, Y.; Komatsu, K.; Dairoku, H.; Kubo, O.; Hori, T.; Okada, Y. Cranial molding helmet therapy and establishment of practical criteria for management in asian infant positional head deformity. Childs Nerv. Syst. 2014, 30, 1499–1509. [Google Scholar] [CrossRef]
- Takamatsu, A.; Hikosaka, M.; Kaneko, T.; Mikami, M.; Kaneko, A. Evaluation of the molding helmet therapy for Japanese infants with deformational plagiocephaly. JMA J. 2021, 4, 50–60. [Google Scholar] [CrossRef]
- Noto, T.; Nagano, N.; Kato, R.; Hashimoto, S.; Saito, K.; Miyabayashi, H.; Sasano, M.; Sumi, K.; Yoshino, A.; Morioka, I. Natural-course evaluation of infants with positional severe plagiocephaly using a three-dimensional scanner in Japan: Comparison with those who received cranial helmet therapy. J. Clin. Med. 2021, 10, 3531. [Google Scholar] [CrossRef]
- Graham, T.; Adams-Huet, B.; Gilbert, N.; Witthoff, K.; Gregory, T.; Walsh, M. Effects of Initial Age and Severity on Cranial Remolding Orthotic Treatment for Infants with Deformational Plagiocephaly. J. Clin. Med. 2019, 8, 1097. [Google Scholar] [CrossRef] [Green Version]
- Kluba, S.; Kraut, W.; Reinert, S.; Krimmel, M. what is the optimal time to start helmet therapy in positional plagiocephaly? Plast. Reconstr. Surg. 2011, 128, 492–498. [Google Scholar] [CrossRef] [Green Version]
- Freudlsperger, C.; Steinmacher, S.; Saure, D.; Bodem, J.P.; Kühle, R.; Hoffmann, J.; Engel, M. Impact of severity and therapy onset on helmet therapy in positional plagiocephaly. J. Craniomaxillofac. Surg. 2016, 44, 110–115. [Google Scholar] [CrossRef]
- Aarnivala, H.; Vuollo, V.; Harila, V.; Heikkinen, T.; Pirttiniemi, P.; Holmström, L.; Valkama, A.M. The course of positional cranial deformation from 3 to 12 months of age and associated risk factors: A follow-up with 3D imaging. Eur. J. Pediatr. 2016, 175, 1893–1903. [Google Scholar] [CrossRef]
- Meyer-Marcotty, P.; Kunz, F.; Schweitzer, T.; Wachter, B.; Böhm, H.; Waßmuth, N.; Linz, C. Cranial growth in infants─a longitudinal three-dimensional analysis of the first months of life. J. Craniomaxillofac. Surg. 2018, 46, 987–993. [Google Scholar] [CrossRef] [PubMed]
- Plank, L.H.; Giavedoni, B.; Lombardo, J.R.; Geil, M.D.; Reisner, A. Comparison of infant head shape changes in deformational plagiocephaly following treatment with a cranial remolding orthosis using a noninvasive laser shape digitizer. J. Craniofac. Surg. 2006, 17, 1084–1091. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ifflaender, S.; Rüdiger, M.; Konstantelos, D.; Wahls, K.; Burkhardt, W. Prevalence of head deformities in preterm infants at term equivalent age. Early Hum. Dev. 2013, 89, 1041–1047. [Google Scholar] [CrossRef] [PubMed]
- Ifflaender, S.; Rüdiger, M.; Koch, A.; Burkhardt, W. Three-dimensional digital capture of head size in neonates—A method evaluation. PLoS ONE 2013, 8, e61274. [Google Scholar] [CrossRef] [Green Version]
- Loveday, B.P.; de Chalain, T.B. Active counterpositioning or orthotic device to treat positional plagiocephaly? J. Craniofac. Surg. 2001, 12, 308–313. [Google Scholar] [CrossRef]
- Kunz, F.; Schweitzer, T.; Große, S.; Waßmuth, N.; Stellzig-Eisenhauer, A.; Böhm, H.; Meyer-Marcotty, P.; Linz, C. Head orthosis therapy in positional plagiocephaly: Longitudinal 3D-investigation of long-term outcomes, compared with untreated infants and with a control group. Eur. J. Orthod. 2019, 41, 29–37. [Google Scholar] [CrossRef]
- Holowka, M.A.; Reisner, A.; Giavedoni, B.; Lombardo, J.R.; Coulter, C. Plagiocephaly Severity Scale to Aid in Clinical Treatment Recommendations. J. Craniofac. Surg. 2017, 28, 717–722. [Google Scholar] [CrossRef]
- Kanda, Y. Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transplant. 2013, 48, 452–458. [Google Scholar] [CrossRef] [Green Version]
- Hutchison, B.L.; Hutchison, L.A.; Thompson, J.M.; Mitchell, E.A. Plagiocephaly and brachycephaly in the first two years of life: A prospective cohort study. Pediatrics 2004, 114, 970–980. [Google Scholar] [CrossRef] [Green Version]
- Aarnivala, H.E.; Valkama, A.M.; Pirttiniemi, P.M. Cranial shape, size and cervical motion in normal newborns. Early Hum. Dev. 2014, 90, 425–430. [Google Scholar] [CrossRef]
- Boere-Boonekamp, M.M.; van der Linden-Kuiper, L.T. Positional preference: Prevalence in infants and follow-up after two years. Pediatrics 2001, 107, 339–343. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, E.; Majnemer, A.; Farmer, J.P.; Barr, R.G.; Platt, R.W. Motor development of infants with positional plagiocephaly. Phys. Occup. Ther. Pediatr. 2009, 29, 222–235. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nuysink, J.; Eijsermans, M.J.; van Haastert, I.C.; Koopman-Esseboom, C.; Helders, P.J.; de Vries, L.S.; van der Net, J. Clinical course of asymmetric motor performance and deformational plagiocephaly in very preterm infants. J. Pediatr. 2013, 163, 658–665.e1. [Google Scholar] [CrossRef] [PubMed]
- van Vlimmeren, L.A.; van der Graaf, Y.; Boere-Boonekamp, M.M.; L’Hoir, M.P.; Helders, P.J.; Engelbert, R.H. Risk factors for deformational plagiocephaly at birth and at 7 weeks of age: A prospective cohort study. Pediatrics 2007, 119, e408–e418. [Google Scholar] [CrossRef] [Green Version]
- De Bock, F.; Braun, V.; Renz-Polster, H. Deformational plagiocephaly in normal infants: A systematic review of causes and hypotheses. Arch. Dis. Child. 2017, 102, 535–542. [Google Scholar] [CrossRef]
- Foster, J.; Ahluwalia, R.; Sherburn, M.; Kelly, K.; Sellyn, G.E.; Kiely, C.; Wiseman, A.L.; Gannon, S.; Shannon, C.N.; Bonfield, C.M. Pediatric cranial deformations: Demographic associations. J. Neurosurg. Pediatr. 2020, 26, 415–420. [Google Scholar] [CrossRef]
- Aarnivala, H.; Vuollo, V.; Harila, V.; Heikkinen, T.; Pirttiniemi, P.; Valkama, A.M. Preventing deformational plagiocephaly through parent guidance: A randomized, controlled trial. Eur. J. Pediatr. 2015, 174, 1197–1208. [Google Scholar] [CrossRef]
- Bialocerkowski, A.E.; Vladusic, S.L.; Wei Ng, C.W.W. Prevalence, risk factors, and natural history of positional plagiocephaly: A systematic review. Dev. Med. Child Neurol. 2008, 50, 577–586. [Google Scholar] [CrossRef]
- van Vlimmeren, L.A.; Engelbert, R.H.; Pelsma, M.; Groenewoud, H.M.; Boere-Boonekamp, M.M.; der Sanden, M.W. The course of skull deformation from birth to 5 years of age: A prospective cohort study. Eur. J. Pediatr. 2017, 176, 11–21. [Google Scholar] [CrossRef] [Green Version]
- Hewitt, L.; Stephens, S.; Spencer, A.; Stanley, R.M.; Okely, A.D. Weekly group tummy time classes are feasible and acceptable to mothers with infants: A pilot cluster randomized controlled trial. Pilot Feasibility Stud. 2020, 6, 155. [Google Scholar] [CrossRef]
- Ellwood, J.; Draper-Rodi, J.; Carnes, D. The effectiveness and safety of conservative interventions for positional plagiocephaly and congenital muscular torticollis: A synthesis of systematic reviews and guidance. Chiropr. Man. Therap. 2020, 28, 31. [Google Scholar] [CrossRef] [PubMed]
- Koban, K.C.; Perko, P.; Etzel, L.; Li, Z.; Schenck, T.L.; Giunta, R.E. Validation of two handheld devices against a non-portable three-dimensional surface scanner and assessment of potential use for intraoperative facial imaging. J. Plast. Reconstr. Aesthet. Surg. 2020, 73, 141–148. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Verhulst, A.; Hol, M.; Vreeken, R.; Becking, A.; Ulrich, D.; Maal, T. Three-dimensional imaging of the face: A comparison between three different imaging modalities. Aesthet. Surg. J. 2018, 38, 579–585. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Choi, H.; Lim, S.H.; Kim, J.S.; Hong, B.Y. Outcome analysis of the effects of helmet therapy in infants with brachycephaly. J. Clin. Med. 2020, 9, 1171. [Google Scholar] [CrossRef] [Green Version]
| Maternal Age, Years | 34.0 ± 5.3 |
| Maternal BMI, kg/m2 | 21.8 ± 3.5 |
| First birth/previous birth | 44 (47.8)/48 (52.2) |
| Single pregnancy/multiple pregnancies | 86 (93.5)/6 (6.5) |
| Infertility treatment | 13 (14.1) |
| Hypertensive disorders of pregnancy | 8 (8.7) |
| Gestational diabetes mellitus | 13 (14.1) |
| Smoking history | 17 (18.5) |
| Delivery method: | |
| Vaginal | 46 (50.0) |
| Cesarean | 36 (39.1) |
| Vacuum or forceps | 10 (10.9) |
| Cephalic fetal presentation/other fetal presentation | 85 (92.4)/7 (7.6) |
| Sex, male/female | 48 (52.2)/44 (47.8) |
| Gestational age, weeks | 38.5 ± 1.3 |
| Birth weight, g | 3016 ± 324 |
| 5 min Apgar score | 9 ± 0.4 |
| Breastfeeding only/formula mix | 20 (21.7)/72 (78.3) |
| Not concerned/concerned | 81 (88.0)/11 (12.0) |
| T1 | T2 | T3 | p-Value | |||
|---|---|---|---|---|---|---|
| T1–T2 | T2–T3 | T1–T3 | ||||
| Cranial asymmetry, mm | 6.4 (4.0–9.0) | 8.0 (4.1–11.3) | 6.8 (3.5–10.1) | <0.01 | <0.01 | 0.76 |
| Cranial vault asymmetry index, % | 5.0 (3.1–7.0) | 5.8 (3.0–8.0) | 4.7 (2.5–7.1) | 0.10 | <0.01 | 0.56 |
| Anterior symmetry ratio, % | 93.8 (89.5–96.7) | 94.2 (90.8–97.1) | 95.9 (92.5–98.0) | 0.13 | <0.01 | <0.01 |
| Posterior symmetry ratio, % | 92.8 (84.6–95.5) | 90.2 (84.4–96.1) | 91.4 (86.2–95.5) | <0.01 | <0.01 | 1.00 |
| Prevalence of deformational plagiocephaly, % | 50.0 | 56.5 | 44.6 | 0.63 | 0.03 | 1.00 |
| T3 | |||
|---|---|---|---|
| CVAI ≤ 6.25% | CVAI > 6.25% | ||
| T1 | CVAI ≤ 6.25% | 49 (53.2%) | 12 (13.0%) |
| CVAI > 6.25% | 12 (13.0%) | 19 (20.7%) |
| CVAI ≤ 8.75% at T3 | CVAI > 8.75% at T3 | p-Value | ||
|---|---|---|---|---|
| n | 84 | 8 | ||
| T1 | Cranial asymmetry, mm | 6.0 (3.8–8.3) | 10.4 (10.2–12.7) | <0.01 |
| Cranial vault asymmetry index, % | 4.7 (3.0–6.6) | 8.3 (7.9–9.5) | <0.01 | |
| Anterior symmetry ratio, % | 93.9 (89.6–97.0) | 90.3 (88.8–92.1) | 0.19 | |
| Posterior symmetry ratio, % | 94.1 (84.9–97.1) | 86.1 (82.7–87.8) | <0.01 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Miyabayashi, H.; Nagano, N.; Kato, R.; Noto, T.; Hashimoto, S.; Saito, K.; Morioka, I. Cranial Shape in Infants Aged One Month Can Predict the Severity of Deformational Plagiocephaly at the Age of Six Months. J. Clin. Med. 2022, 11, 1797. https://doi.org/10.3390/jcm11071797
Miyabayashi H, Nagano N, Kato R, Noto T, Hashimoto S, Saito K, Morioka I. Cranial Shape in Infants Aged One Month Can Predict the Severity of Deformational Plagiocephaly at the Age of Six Months. Journal of Clinical Medicine. 2022; 11(7):1797. https://doi.org/10.3390/jcm11071797
Chicago/Turabian StyleMiyabayashi, Hiroshi, Nobuhiko Nagano, Risa Kato, Takanori Noto, Shin Hashimoto, Katsuya Saito, and Ichiro Morioka. 2022. "Cranial Shape in Infants Aged One Month Can Predict the Severity of Deformational Plagiocephaly at the Age of Six Months" Journal of Clinical Medicine 11, no. 7: 1797. https://doi.org/10.3390/jcm11071797
APA StyleMiyabayashi, H., Nagano, N., Kato, R., Noto, T., Hashimoto, S., Saito, K., & Morioka, I. (2022). Cranial Shape in Infants Aged One Month Can Predict the Severity of Deformational Plagiocephaly at the Age of Six Months. Journal of Clinical Medicine, 11(7), 1797. https://doi.org/10.3390/jcm11071797






