Clinical Evidence of Cannabinoids in Migraine: A Narrative Review
Abstract
:1. Introduction
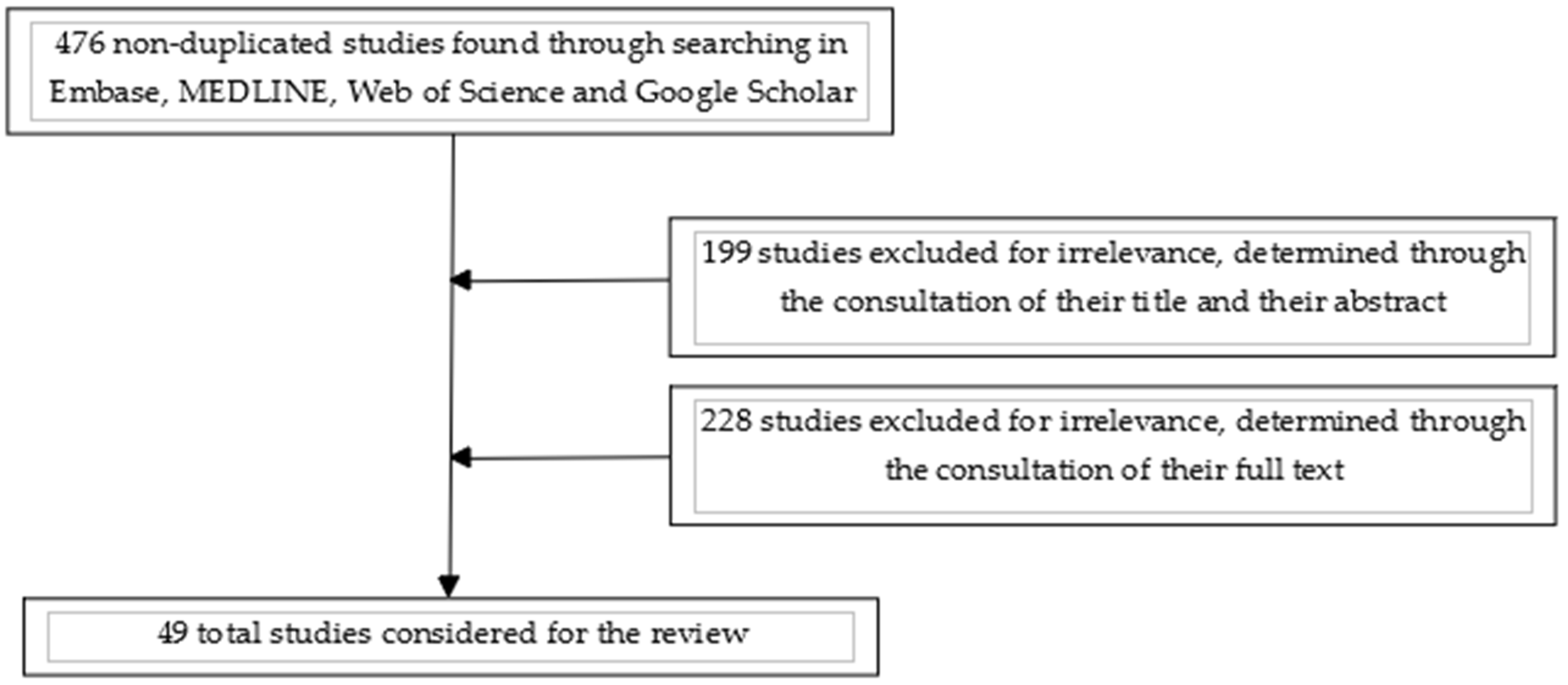
2. Materials and Methods
3. Results
3.1. Endocannabinoid System and Migraine
3.2. Phytocannabinoids
3.3. Synthetic Cannabinoids
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Burch, R.C.; Buse, D.C.; Lipton, R.B. Migraine: Epidemiology, burden, and comorbidity. Neurol. Clin. 2019, 37, 631–649. [Google Scholar] [CrossRef] [PubMed]
- Burch, R.; Rizzoli, P.; Loder, E. The prevalence and impact of migraine and severe headache in the United States: Updated age, sex, and socioeconomic-specific estimates from government health surveys. Headache 2021, 61, 60–68. [Google Scholar] [CrossRef] [PubMed]
- Steiner, T.J.; Stovner, L.J.; Jensen, R.; Uluduz, D.; Katsarava, Z. Lifting the Burden: The Global Campaign against Headache. Migraine remains second among the world’s causes of disability, and first among young women: Findings from GBD2019. J. Headache Pain 2020, 21, 137. [Google Scholar] [CrossRef] [PubMed]
- Miller, S.; Matharu, M.S. Migraine is underdiagnosed and undertreated. Practitioner 2014, 258, 19–24. [Google Scholar] [PubMed]
- Viana, M.; Genazzani, A.A.; Terrazzino, S.; Nappi, G.; Goadsby, P.J. Triptan nonresponders: Do they exist and who are they? Cephalalgia 2013, 33, 891–896. [Google Scholar] [CrossRef]
- Hepp, Z.; Bloudek, L.M.; Varon, S.F. Systematic review of migraine prophylaxis adherence and persistence. J. Manag. Care Pharm. 2014, 20, 22–33. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baron, E.P. Medicinal properties of cannabinoids, terpenes, and flavonoids in cannabis, and benefits in migraine, headache, and pain: An update on current evidence and cannabis science. Headache 2018, 58, 1139–1186. [Google Scholar] [CrossRef]
- Bramer, W.M.; Rethlefsen, M.L.; Kleijnen, J.; Franco, O.H. Optimal database combination for literature searches in systematic reviews: A prospective exploratory study. Syst. Rev. 2017, 6, 245. [Google Scholar] [CrossRef]
- Guindon, J.; Hohmann, A. The Endocannabinoid System and Pain. CNS Neurol. Disord. Drug Targets 2012, 8, 403–421. [Google Scholar] [CrossRef]
- Matsuda, L.A.; Lolait, S.J.; Brownstein, M.J.; Young, A.C.; Bonner, T.I. Structure of a cannabinoid receptor and functional expression of the cloned cDNA. Nature 1990, 346, 561–564. [Google Scholar] [CrossRef]
- Munro, S.; Thomas, K.L.; Abu-Shaar, M. Molecular characterization of a peripheral receptor for cannabinoids. Nature 1993, 365, 61–65. [Google Scholar] [CrossRef] [PubMed]
- Pertwee, R.G.; Ross, R.A. Cannabinoid receptors and their ligands. Prostaglandins Leukot. Essent. Fat. Acids 2002, 66, 101–121. [Google Scholar] [CrossRef] [PubMed]
- Cantarella, G.; Scollo, M.; Lempereur, L.; Saccani-Jotti, G.; Basile, F.; Bernardini, R. Endocannabinoids inhibit release of nerve growth factor by inflammation-activated mast cells. Biochem. Pharmacol. 2011, 82, 380–388. [Google Scholar] [CrossRef] [Green Version]
- Starowicz, K.; Makuch, W.; Osikowicz, M.; Piscitelli, F.; Petrosino, S.; Di Marzo, V.; Przewlocka, B. Spinal anandamide produces analgesia in neuropathic rats: Possible CB(1)- and TRPV1-mediated mechanisms. Neuropharmacology 2012, 62, 1746–1755. [Google Scholar] [CrossRef] [PubMed]
- Glass, M.; Northup, J.K. Agonist selective regulation of G proteins by cannabinoid CB(1) and CB(2) receptors. Mol. Pharmacol. 1999, 56, 1362–1369. [Google Scholar] [CrossRef] [Green Version]
- Mechoulam, R.; Ben-Shabat, S.; Hanus, L.; Ligumsky, M.; Kaminski, N.E.; Schatz, A.R.; Gopher, A.; Almog, S.; Martin, B.R.; Compton, D.R.; et al. Identification of an endogenous 2-monoglyceride, present in canine gut, that binds to cannabinoid receptors. Biochem. Pharmacol. 1995, 50, 83–90. [Google Scholar] [CrossRef]
- Marsicano, G.; Goodenough, S.; Monory, K.; Hermann, H.; Eder, M.; Cannich, A.; Azad, S.C.; Cascio, M.G.; Gutiérrez, S.O.; van der Stelt, M.; et al. CB1 cannabinoid receptors and on-demand defense against excitotoxicity. Science 2003, 302, 84–88. [Google Scholar] [CrossRef] [Green Version]
- Ueda, N.; Okamoto, Y.; Morishita, J. N-acylphosphatidylethanolamine-hydrolyzing phospholipase D: A novel enzyme of the beta-lactamase fold family releasing anandamide and other N-acylethanolamines. Life Sci. 2005, 77, 1750–1758. [Google Scholar] [CrossRef]
- Bisogno, T.; Howell, F.; Williams, G.; Minassi, A.; Cascio, M.G.; Ligresti, A.; Matias, I.; Schiano-Moriello, A.; Paul, P.; Williams, E.J.; et al. Cloning of the first sn1-DAG lipases points to the spatial and temporal regulation of endocannabinoid signaling in the brain. J. Cell Biol. 2003, 163, 463–468. [Google Scholar] [CrossRef]
- Zou, S.; Kumar, U. Cannabinoid receptors and the endocannabinoid system: Signaling and function in the central nervous system. Int. J. Mol. Sci. 2018, 19, 833. [Google Scholar] [CrossRef] [Green Version]
- Russo, E.B. Clinical Endocannabinoid Deficiency Reconsidered: Current Research Supports the Theory in Migraine, Fibromyalgia, Irritable Bowel, and Other Treatment-Resistant Syndromes. Cannabis Cannabinoid Res. 2016, 1, 154–165. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Akerman, S.; Kaube, H.; Goadsby, P.J. Anandamide is able to inhibit trigeminal neurons using an in vivo model of trigeminovascular-mediated nociception. J. Pharmacol. Exp. Ther. 2004, 309, 56–63. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tassorelli, C.; Greco, R.; Silberstein, S.D. The endocannabinoid system in migraine: From bench to pharmacy and back. Curr. Opin. Neurol. 2019, 32, 405–412. [Google Scholar] [CrossRef] [PubMed]
- Leimuranta, P.; Khiroug, L.; Giniatulli, R. Emerging Role of (Endo)Cannabinoids in Migraine. Front. Pharmacol. 2018, 9, 420. [Google Scholar] [CrossRef] [PubMed]
- Greco, R.; Demartini, C.; Zanaboni, A.M.; Piomelli, D.; Tassorelli, C. Endocannabinoid System and Migraine Pain: An Update. Front. Neurosci. 2018, 12, 172. [Google Scholar] [CrossRef]
- Cupini, L.M.; Bari, M.; Battista, N.; Argirò, G.; Finazzi-Agrò, A.; Calabresi, P.; Maccarrone, M. Biochemical changes in endocannabinoid system are expressed in platelets of female but not male migraineurs. Cephalalgia 2006, 26, 277–281. [Google Scholar] [CrossRef]
- Cupini, L.M.; Costa, C.; Sarchielli, P.; Bari, M.; Battista, N.; Eusebi, P.; Calabresi, P.; Maccarrone, M. Degradation of endocannabinoids in chronic migraine and medication overuse headache. Neurobiol. Dis. 2008, 30, 186–189. [Google Scholar] [CrossRef]
- Rossi, C.; Pini, L.A.; Cupini, M.L.; Calabresi, P.; Sarchielli, P. Endocannabinoids in platelets of chronic migraine patients and medication-overuse headache patients: Relation with serotonin levels. Eur. J. Clin. Pharmacol. 2008, 64, 1–8. [Google Scholar] [CrossRef]
- Gouveia-Figueira, S.; Goldin, K.; Hashemian, S.A.; Lindberg, A.; Persson, M.; Nording, M.L.; Laurell, K.; Fowler, C.J. Plasma levels of the endocannabinoid anandamide, related N-acylethanolamines and linoleic acid-derived oxylipins in patients with migraine. Prostaglandins Leukot. Essent. Fat. Acids 2017, 120, 15–24. [Google Scholar] [CrossRef]
- Sarchielli, P.; Pini, L.A.; Coppola, F.; Rossi, C.; Baldi, A.; Mancini, M.L.; Calabresi, P. Endocannabinoids in chronic migraine: CSF findings suggest a system failure. Neuropsychopharmacology 2007, 32, 1384–1390. [Google Scholar] [CrossRef]
- Van der Schueren, B.J.; Van Laere, K.; Gérard, N.; Bormans, G.; De Hoon, J.N. Interictal type 1 cannabinoid receptor binding is increased in female migraine patients. Headache 2012, 52, 433–440. [Google Scholar] [CrossRef] [PubMed]
- Perrotta, A.; Arce-Leal, N.; Tassorelli, C.; Gasperi, V.; Sances, G.; Blandini, F.; Serrao, M.; Bolla, M.; Pierelli, F.; Nappi, G.; et al. Acute reduction of anandamide-hydrolase (FAAH) activity is coupled with a reduction of nociceptive pathways facilitation in medication-overuse headache subjects after withdrawal treatment. Headache 2012, 52, 1350–1361. [Google Scholar] [CrossRef] [PubMed]
- Anttila, V.; Winsvold, B.S.; Gormley, P.; Kurth, T.; Bettella, F.; McMahon, G.; Kallela, M.; Malik, R.; de Vries, B.; Terwindt, G.; et al. Genome-wide meta-analysis identifies new susceptibility loci for migraine. Nat. Genet. 2013, 45, 912–917. [Google Scholar] [CrossRef] [PubMed]
- Gormley, P.; Anttila, V.; Winsvold, B.S.; Palta, P.; Esko, T.; Pers, T.H.; Farh, K.H.; Cuenca-Leon, E.; Muona, M.; Furlotte, N.A.; et al. Meta-analysis of 375,000 individuals identifies 38 susceptibility loci for migraine. Nat. Genet. 2016, 48, 856–866. [Google Scholar] [CrossRef] [Green Version]
- Juhasz, G.; Csepany, E.; Magyar, M.; Edes, A.E.; Eszlari, N.; Hullam, G.; Antal, P.; Kokonyei, G.; Anderson, I.M.; Deakin, J.F.; et al. Variants in the CNR1 gene predispose to headache with nausea in the presence of life stress. Genes Brain Behav. 2017, 16, 384–393. [Google Scholar] [CrossRef] [Green Version]
- Greco, R.; Demartini, C.; Zanaboni, A.M.; Tumelero, E.; Icco, R.; Sances, G.; Allena, M.; Tassorelli, C. Peripheral changes of endocannabinoid system components in episodic and chronic migraine patients: A pilot study. Cephalalgia 2021, 41, 185–196. [Google Scholar] [CrossRef]
- De Icco, R.; Greco, R.; Demartini, C.; Vergobbi, P.; Zanaboni, A.; Tumelero, E.; Reggiani, A.; Realini, N.; Sances, G.; Grillo, V.; et al. Spinal nociceptive sensitization and plasma palmitoylethanolamide levels during experimentally induced migraine attacks. Pain 2021, 162, 2376–2385. [Google Scholar] [CrossRef]
- Salazar, C.A.; Tomko, R.L.; Akbar, S.A.; Squeglia, L.M.; McClure, E.A. Medical cannabis use among adults on the southeastern United States. Cannabis 2019, 2, 53–65. [Google Scholar] [CrossRef]
- Azcarate, P.M.; Zhang, A.J.; Keyhani, S.; Steigerwald, S.; Ishida, J.H.; Cohen, B.E. Medical reasons for marijuana use, forms of use, and patient perception of physician attitudes among the US population. J. Gen. Intern. Med. 2020, 35, 1979–1986. [Google Scholar] [CrossRef]
- Aviram, J.; Vysotski, Y.; Berman, P.; Lewitus, G.M.; Eisenberg, E.; Meiri, D. Migraine frequency decrease following prolonged medical cannabis treatment: A cross-sectional study. Brain Sci. 2020, 10, 360. [Google Scholar] [CrossRef]
- Gibson, L.P.; Hitchcock, L.N.; Bryan, A.D.; Cinnamon Bidwell, L. Experience of migraine, its severity, and perceived efficacy of treatments among cannabis users. Complement. Ther. Med. 2021, 56, 102619. [Google Scholar] [CrossRef] [PubMed]
- Rhyne, D.N.; Anderson, S.L.; Gedde, M.; Borgelt, L.M. Effects of Medical Marijuana on Migraine Headache Frequency in an Adult Population. Pharmacotherapy 2016, 36, 505–510. [Google Scholar] [CrossRef] [PubMed]
- Baraldi, C.; Lo Castro, F.; Negro, A.; Ferrari, A.; Cainazzo, M.M.; Pani, L.; Guerzoni, S. Oral cannabinoid preparations for the treatment of chronic migraine: A retrospective study. Pain Med. 2021, 23, 396–402. [Google Scholar] [CrossRef] [PubMed]
- Sexton, M.; Cuttler, C.; Finnell, J.S.; Mischley, L.K. A cross-sectional survey of medical cannabis users: Patterns of use and perceived efficacy. Cannabis Cannabinoid Res. 2016, 1, 131–138. [Google Scholar] [CrossRef]
- Stith, S.S.; Diviant, J.P.; Brockelman, F.; Keeling, K.; Hall, B.; Lucern, S.; Vigil, J.M. Alleviative effects of cannabis flower on migraine and headache. J. Integr. Med. 2020, 18, 416–424. [Google Scholar] [CrossRef]
- Pellesi, L.; Licata, M.; Verri, P.; Vandelli, P.; Palazzoli, F.; Marchesi, F.; Cainazzo, M.M.; Pini, L.A.; Guerzoni, S. Pharmacokinetics and tolerability of oral cannabis preparations in patients with medication overuse headache (MOH)- a pilot study. Eur. J. Clin. Pharmacol. 2018, 74, 1427–1436. [Google Scholar] [CrossRef]
- Cuttler, C.; Spradlin, A.; Cleveland, M.J.; Craft, R.M. Short and long-term effects of cannabis on headache and migraine. J. Pain 2020, 21, 722–730. [Google Scholar] [CrossRef]
- Kopruszinski, C.M.; Navratilova, E.; Vagnerova, B.; Swiokla, J.; Patwardhan, A.; Dodick, D.; Porreca, F. Cannabinoids induce latent sensitization in a preclinical model of medication overuse headache. Cephalalgia 2020, 40, 68–78. [Google Scholar] [CrossRef]
- Zhang, N.; Woldeamanuel, Y.W. Medication overuse headache in patients with chronic migraine using cannabis: A case-referent study. Headache 2021, 61, 1234–1244. [Google Scholar] [CrossRef]
- National Library of Medicine (U.S.). Cannabis for the Prophylactic Treatment of Migraine. Identifier: NCT03972124. 2019. Available online: https://clinicaltrials.gov/ct2/show/NCT03972124 (accessed on 30 November 2021).
- National Library of Medicine (U.S.). Efficacy of Inhaled Cannabis for Acute Migraine Treatment. Identifier: NCT04360044. 2020. Available online: https://clinicaltrials.gov/ct2/show/NCT04360044 (accessed on 30 November 2021).
- Riboulet-Zemouli, K. ‘Cannabis’ ontologies I: Conceptual issues with cannabis and cannabinoids terminology. Drug Sci. Policy Law 2020, 6, 1–37. [Google Scholar] [CrossRef]
- Pini, L.A.; Guerzoni, S.; Cainazzo, M.M.; Ferrari, A.; Sarchielli, P.; Tiraferri, I.; Ciccarese, M.; Zappaterra, M. Nabilone for the treatment of medication overuse headache: Results of a preliminary double-blind, active-controlled, randomized trial. J. Headache Pain 2012, 13, 677–684. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mikuriya, T.H. Chronic Migraine Headache: Five Cases Successfully Treated with Marinol and/or Illicit Cannabis; Schaffer Library: Berkeley, CA, USA, 1991. [Google Scholar]
- National Library of Medicine (U.S.). Study to Evaluate the Efficacy and Safety of Dronabinol Metered Dose Inhaler (MDI) in Acute Treatment of Migraine Headache. Identifier: NCT00123201. 2005–2015. Available online: https://clinicaltrials.gov/ct2/show/NCT00123201 (accessed on 15 December 2021).
- Edvinsson, L. CGRP and migraine: From bench to bedside. Rev. Neurol. 2021, 177, 785–790. [Google Scholar] [CrossRef] [PubMed]
- Sacco, S.; Braschinsky, M.; Ducros, A.; Lampl, C.; Little, P.; van den Brink, A.M.; Pozo-Rosich, P.; Reuter, U.; de la Torre, E.R.; Sanchez Del Rio, M.; et al. European headache federation consensus on the definition of resistant and refractory migraine: Developed with the endorsement of the European Migraine & Headache Alliance (EMHA). J. Headache Pain 2020, 21, 76. [Google Scholar] [PubMed]
- Poudel, S.; Quinonez, J.; Choudhari, J.; Au, Z.T.; Paesani, S.; Thiess, A.K.; Ruxmohan, S.; Hosameddin, M.; Ferrer, G.F.; Michel, J. Medical cannabis, headaches, and migraines: A review of the current literature. Cureus 2021, 13, 17407. [Google Scholar] [CrossRef] [PubMed]
- Della Pietra, A.; Giniatullin, R.; Savinainen, J.R. Distinct activity of endocannabinoid-hydrolyzing enzymes MAGL and FAAH in key regions of peripheral and central nervous system implicated in migraine. Int. J. Mol. Sci. 2021, 22, 1204. [Google Scholar] [CrossRef] [PubMed]
- Kaur, R.; Ambwani, S.R.; Singh, S. Endocannabinoid system: A multi-facet therapeutic target. Curr. Clin. Pharmacol. 2016, 11, 110–117. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Reference | Study Design | Number of Patients | Cannabinoid Studied | Route of Administration | Principal Results |
|---|---|---|---|---|---|
| Phytocannabinoids | |||||
| [39] | Retrospective | 9003 | Marijuana | Various (inhaled, oral, vaporized, topical) | 121 patients used marijuana for migraine self-treatment |
| [40] | Retrospective, cross-sectional | 145 | Marijuana | Various (inhaled, oral, vaporized) | >60% patients reported a long-term reduction in migraine frequency |
| [41] | Retrospective | 589 | Marijuana | Various (inhaled, oral, vaporized) | 86 patients used cannabis for migraine relief; Cannabis was more effective than other painkillers in determining migraine relief |
| [43] | Retrospective | 121 | Marijuana | Various (inhaled, oral, vaporized, topical) | Significant decrease in migraine frequency |
| [43] | Retrospective | 32 | Bediol®, Bedrocan®, FM2® | Oral | Significant decrease in pain intensity and analgesic consumption after 3 and 6 months of treatment compared to the baseline |
| [44] | Retrospective | 1429 | Marijuana | Various (inhaled, oral, vaporized, topical) | 35.5% of patients used marijuana to treat their migraines |
| [45] | Prospective | 699 | Marijuana | Various (inhaled, oral, vaporized, topical) | 94% of patients experienced two-hour migraine relief |
| [46] | Prospective, crossover | 13 | Cannabis decoction and cannabis oil | Oral | THC bioavailability is higher for cannabis oil than cannabis decoction |
| [47] | Prospective | 653 | Cannabis (both concentrated and flowers) | Inhaled | Self-reported headache and migraine severity were reduced by approximately 50%. Reduction in effectiveness across time |
| [49] | Retrospective | 212 | Marijuana | Various (inhaled, oral, vaporized, topical) | Cannabis use significantly decreased migraine frequency |
| Synthetic cannabinoids | |||||
| [51] | Prospective | 30 | Nabilone 0.5 mg/die | Oral | Nabilone significantly reduced pain intensity and analgesic consumption compared to ibuprofen. Side effects were mild. |
| [52] | Retrospective | 5 | Dronabinol 5 mg/die | Oral | Dronabinol significantly reduced migraine frequency compared to the baseline |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lo Castro, F.; Baraldi, C.; Pellesi, L.; Guerzoni, S. Clinical Evidence of Cannabinoids in Migraine: A Narrative Review. J. Clin. Med. 2022, 11, 1479. https://doi.org/10.3390/jcm11061479
Lo Castro F, Baraldi C, Pellesi L, Guerzoni S. Clinical Evidence of Cannabinoids in Migraine: A Narrative Review. Journal of Clinical Medicine. 2022; 11(6):1479. https://doi.org/10.3390/jcm11061479
Chicago/Turabian StyleLo Castro, Flavia, Carlo Baraldi, Lanfranco Pellesi, and Simona Guerzoni. 2022. "Clinical Evidence of Cannabinoids in Migraine: A Narrative Review" Journal of Clinical Medicine 11, no. 6: 1479. https://doi.org/10.3390/jcm11061479
APA StyleLo Castro, F., Baraldi, C., Pellesi, L., & Guerzoni, S. (2022). Clinical Evidence of Cannabinoids in Migraine: A Narrative Review. Journal of Clinical Medicine, 11(6), 1479. https://doi.org/10.3390/jcm11061479






