Music Intervention for Pain Control in the Pediatric Population: A Systematic Review and Meta-Analysis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Search Strategy and Selection Criteria
2.2. Data Extraction
2.3. Assessment of Risk of Bias in the Included Studies
2.4. Statistical Analysis
2.5. Subgroup Analysis
3. Results
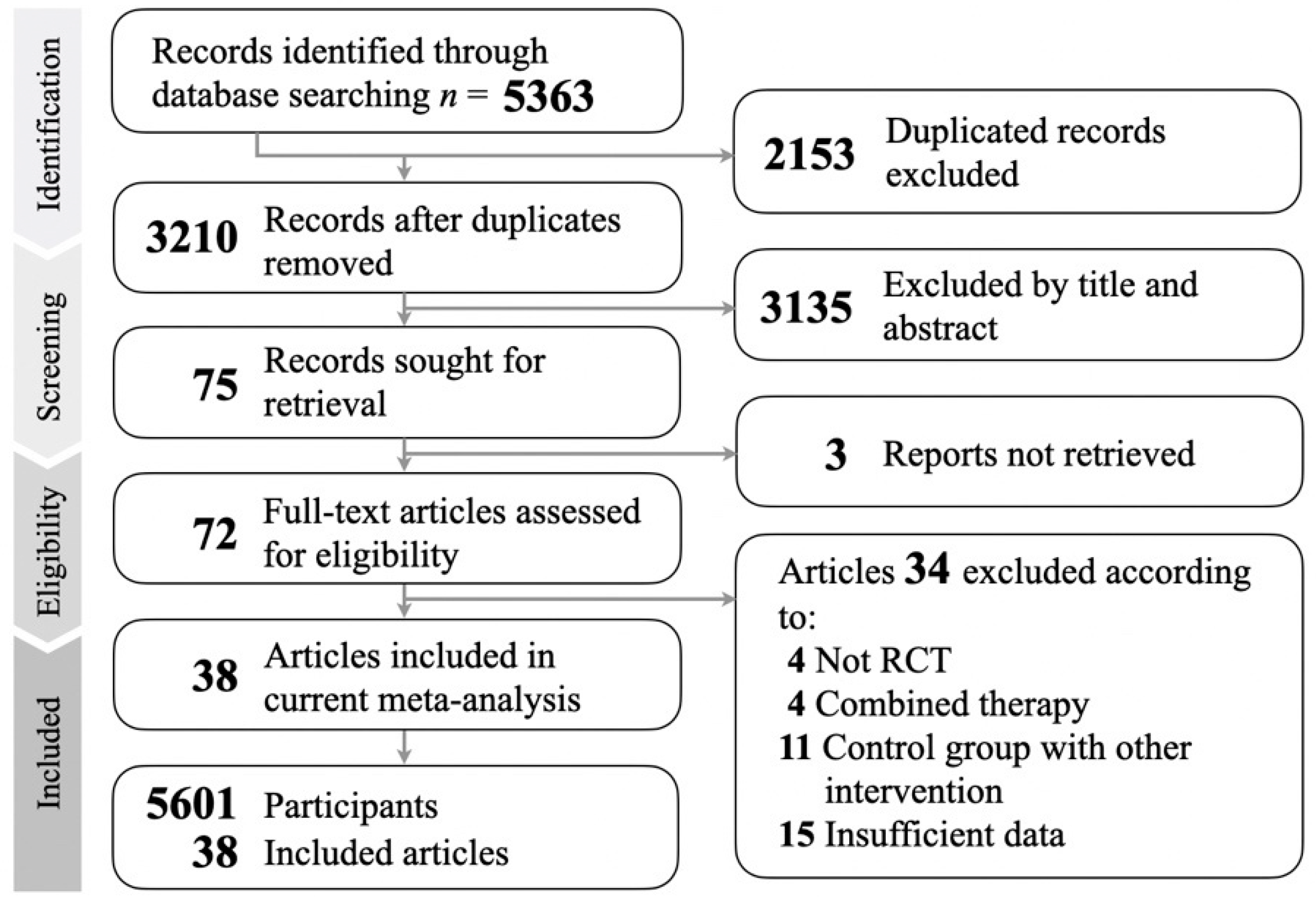
3.1. Identification of Eligible Studies
3.2. Study Characteristics and Patient Populations
3.3. Quality of the Included Articles
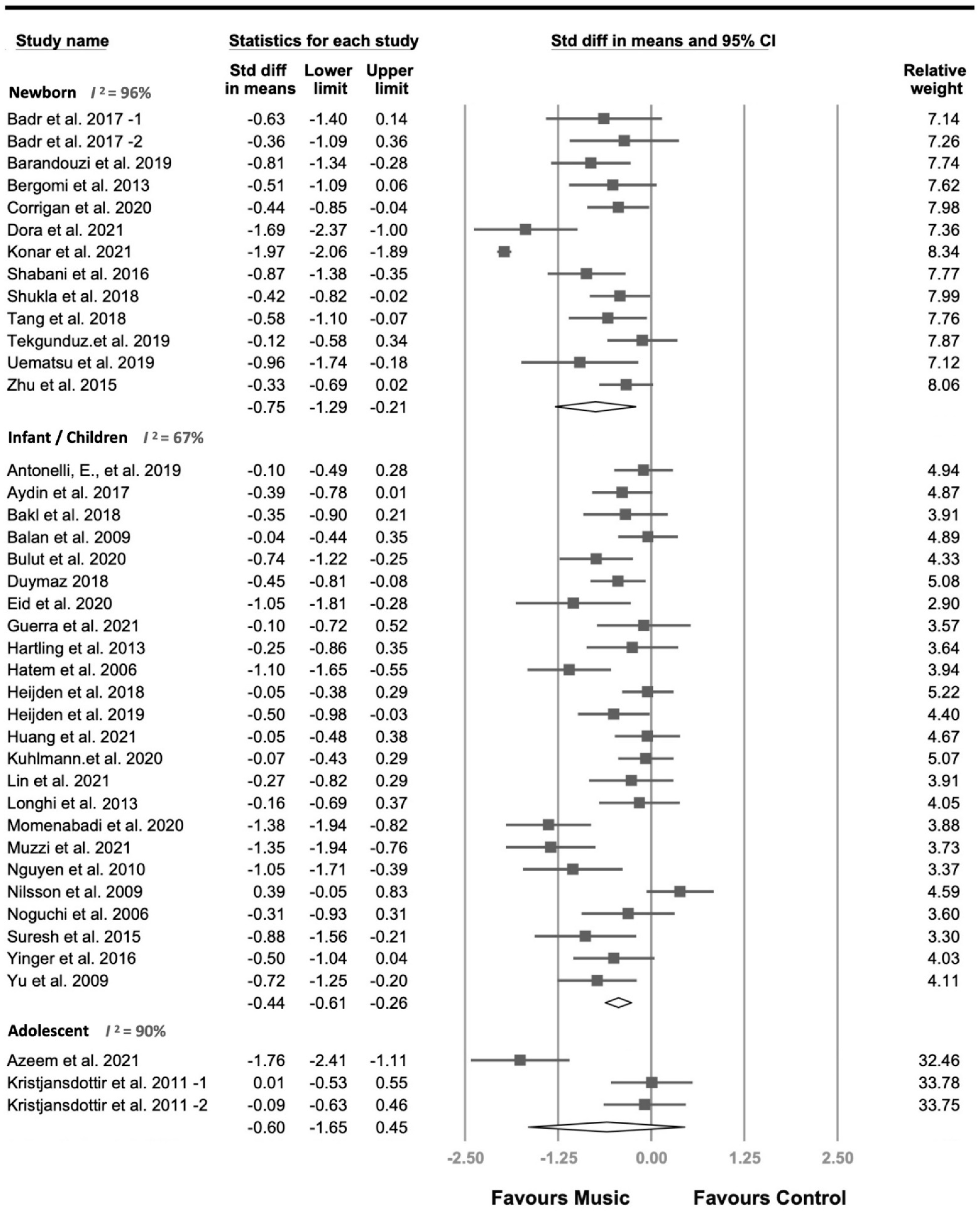
3.4. Primary Outcome of MI
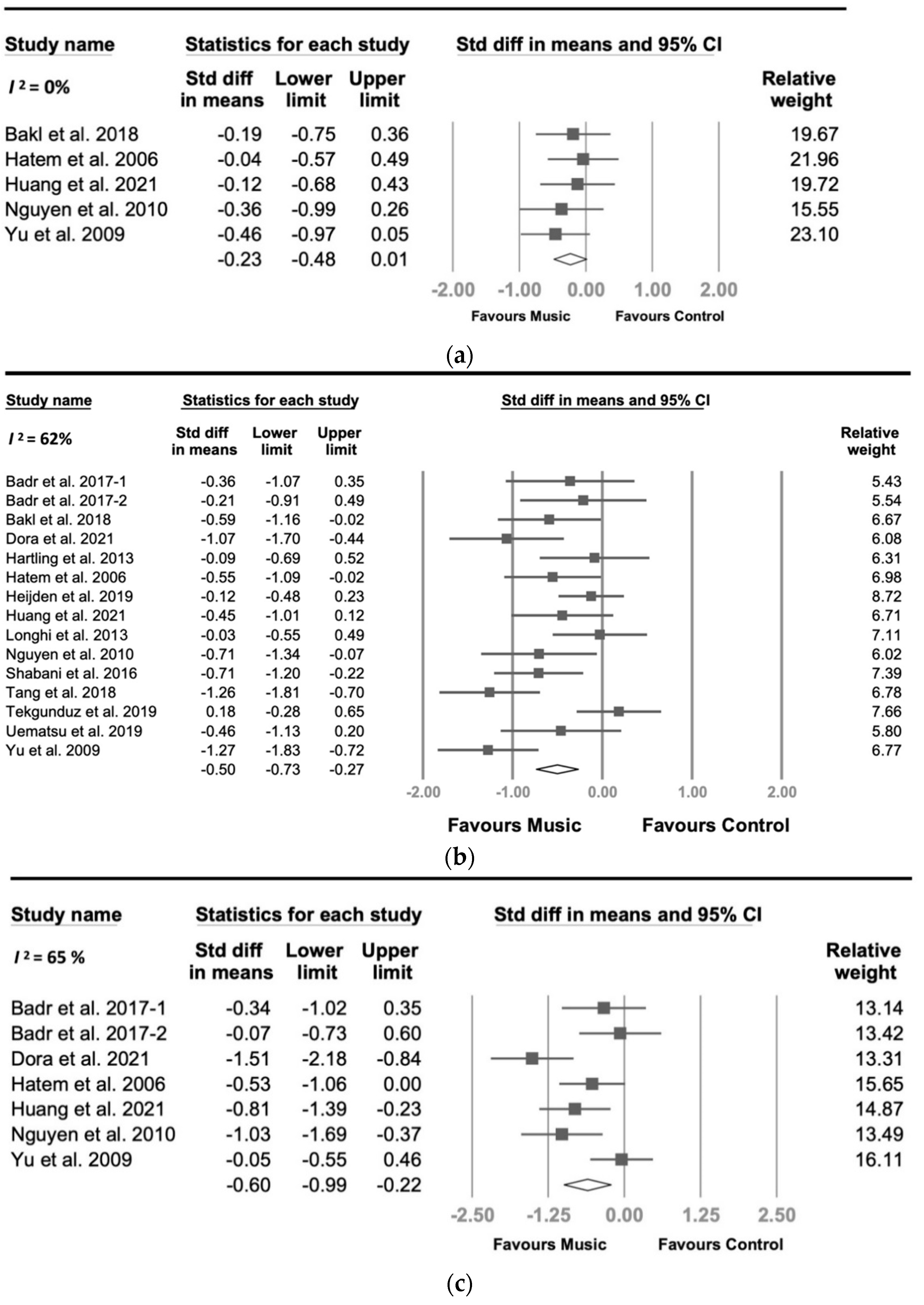
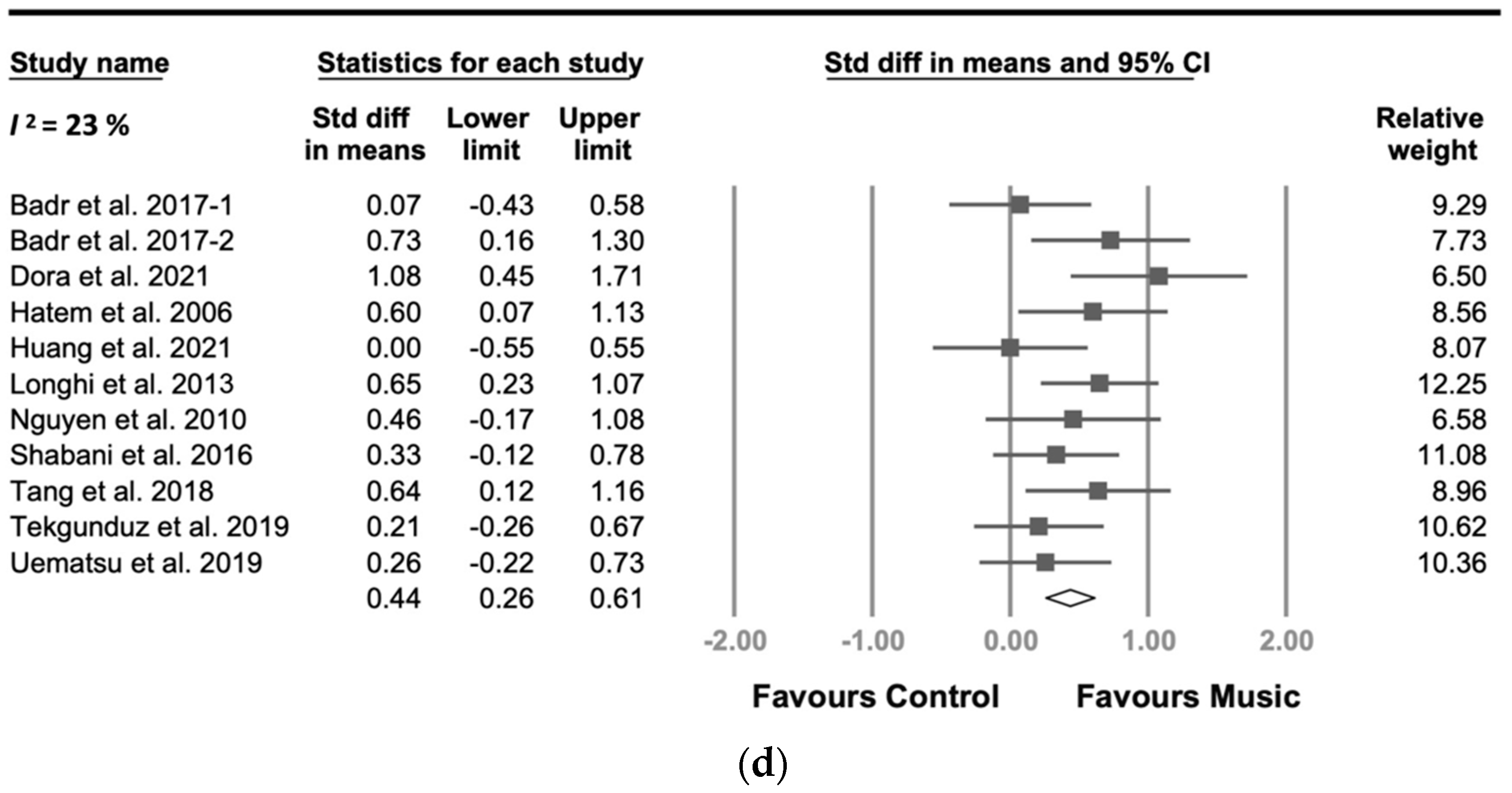
3.5. Secondary Outcome of MI
3.6. Subgroup Analyses
3.7. Sensitivity Analysis
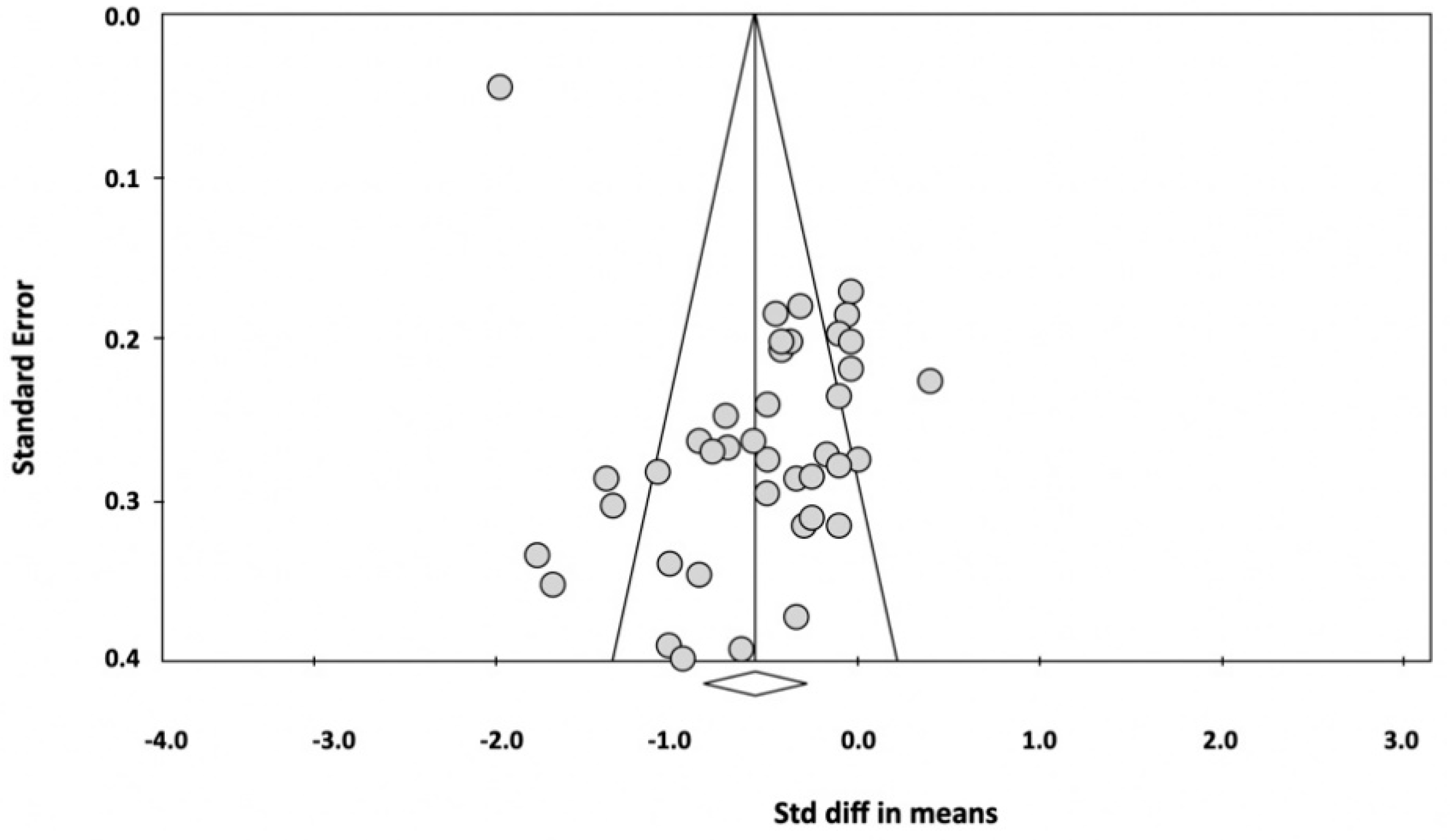
3.8. Evaluation of Publication Bias
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Inal, S.; Şahiner, N.C. Using of distraction methods on procedural pain management of pediatric patients. Sağlık Bilimleri Ve Mesl. Derg. 2015, 2, 372–378. [Google Scholar] [CrossRef] [Green Version]
- Lago, P.; Garetti, E.; Merazzi, D.; Pieragostini, L.; Ancora, G.; Pirelli, A.; Bellieni, C.V. Guidelines for procedural pain in the newborn. Acta Paediatr. 2009, 98, 932–939. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bonutti, P.D.; Daré, M.F.; Castral, T.C.; Leite, A.M.; Vici-Maia, J.A.; Scochi, C.G.S. Dimensioning of painful procedures and interventions for acute pain relief in premature infants. Rev. Lat. Am. De Enferm. 2017, 25. [Google Scholar] [CrossRef] [Green Version]
- Friedrichsdorf, J.S.; Sidman, J.; Krane, E.J. Prevention and treatment of pain in children: Toward a paradigm shift. Otolaryngol. Head Neck Surg. 2016, 154, 804–805. [Google Scholar] [CrossRef] [PubMed]
- Rosen, A.D.; Dower, J. Pediatric pain management. Pediatr. Ann. 2011, 40, 243–252. [Google Scholar] [CrossRef]
- Su, P.K.; Matsuoka, Y.; Pae, C.U. Omega-3 polyunsaturated fatty acids in prevention of mood and anxiety disorders. Clin. Psychopharmacol. Neurosci. 2015, 13, 129–137. [Google Scholar] [CrossRef] [Green Version]
- Lee, J.H. The effects of music on pain: A meta-analysis. J. Music Ther. 2016, 53, 430–477. [Google Scholar] [CrossRef]
- Henry, L.L. Music therapy: A nursing intervention for the control of pain and anxiety in the icu: A review of the research literature. Dimens. Crit. Care Nurs 1995, 14, 295–304. [Google Scholar] [CrossRef]
- Colwell, M.C.; Edwards, R.; Hernandez, E.; Brees, K. Impact of music therapy interventions (listening, composition, orff-based) on the physiological and psychosocial behaviors of hospitalized children: A feasibility study. J. Pediatr. Nurs. 2013, 28, 249–257. [Google Scholar] [CrossRef]
- Kleiber, C.; Adamek, M.S. Adolescents’ perceptions of music therapy following spinal fusion surgery. J. Clin. Nurs. 2013, 22, 414–422. [Google Scholar] [CrossRef]
- van der Heijden, M.J.E.; Mevius, H.; van der Heijde, N.; van Rosmalen, J.; van As, S.; van Dijk, M. Children listening to music or watching cartoons during er procedures: A RCT. J. Pediatr. Psychol. 2019, 44, 1151–1162. [Google Scholar] [CrossRef] [PubMed]
- Avers, L.; Mathur, A.; Kamat, D. Music therapy in pediatrics. Clin. Pediatr. 2007, 46, 575–579. [Google Scholar] [CrossRef] [PubMed]
- Bruscia, K. Defining Music Therapy, 3rd ed.; Barcelona Publishers: Gilsum, NH, USA, 2014. [Google Scholar]
- Cepeda, M.S.; Carr, D.B.; Lau, J.; Alvarez, H. Music for pain relief. Cochrane Database Syst. Rev. 2006, 2, Cd004843. [Google Scholar] [CrossRef]
- Cheng, J.; Zhang, H.; Bao, H.; Hong, H. Music-based interventions for pain relief in patients undergoing hemodialysis: A prisma-compliant systematic review and meta-analysis. Medicine 2021, 100, e24102. [Google Scholar] [CrossRef]
- Chuang, C.H.; Chen, P.C.; Lee, C.S.; Chen, C.H.; Tu, Y.K.; Wu, S.C. Music intervention for pain and anxiety management of the primiparous women during labour: A systematic review and meta-analysis. J. Adv. Nurs. 2019, 75, 723–733. [Google Scholar] [CrossRef] [Green Version]
- García-Perdomo, H.A.; Cardona, L.M.M.; Cordoba-Wagner, M.J.; Zapata-Copete, J.A. Music to reduce pain and anxiety in cystoscopy: A systematic review and meta-analysis. J. Complement. Integr. Med. 2018, 16. [Google Scholar] [CrossRef]
- Garza-Villarreal, E.A.; Pando, V.; Vuust, P.; Parsons, C. Music-induced analgesia in chronic pain conditions: A systematic review and meta-analysis. Pain Physician 2017, 20, 597–610. [Google Scholar] [CrossRef]
- Hung, T.T.; Liu, Y.C.; Tsai, P.C.; Lin, M.F. The pain-relief efficacy of passive music-based interventions in cancer patients undergoing diagnostic biopsies and surgery: A systematic review and meta-analysis. Hu Li Za Zhi J. Nurs. 2018, 65, 70–82. [Google Scholar] [CrossRef]
- Lin, C.L.; Hwang, S.L.; Jiang, P.; Hsiung, N.H. Effect of music therapy on pain after orthopedic surgery-a systematic review and meta-analysis. Pain Pract. 2020, 20, 422–436. [Google Scholar] [CrossRef]
- Martin-Saavedra, J.S.; Vergara-Mendez, L.D.; Talero-Gutiérrez, C. Music is an effective intervention for the management of pain: An umbrella review. Complement. Ther. Clin. Pract. 2018, 32, 103–114. [Google Scholar] [CrossRef]
- Wang, M.C.; Zhang, L.Y.; Zhang, Y.L.; Zhang, Y.W.; Xu, X.D.; Zhang, Y.C. Effect of music in endoscopy procedures: Systematic review and meta-analysis of randomized controlled trials. Pain Med. 2014, 15, 1786–1794. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Wei, J.; Guan, X.; Zhang, Y.; Zhang, Y.; Zhang, N.; Mao, M.; Du, W.; Ren, Y.; Shen, H.; et al. Music intervention in pain relief of cardiovascular patients in cardiac procedures: A systematic review and meta-analysis. Pain Med. 2020, 21, 3055–3065. [Google Scholar] [CrossRef] [PubMed]
- Wu, Q.; Liu, Z.; Pang, X.; Cheng, L. Efficacy of five-element music interventions in perinatal mental health and labor pain: A meta-analysis. Complement. Ther. Clin. Pract. 2020, 40, 101217. [Google Scholar] [CrossRef] [PubMed]
- Yu, R.; Zhuo, Y.; Feng, E.; Wang, W.; Lin, W.; Lin, F.; Li, Z.; Lin, L.; Xiao, L.; Wang, H.; et al. The effect of musical interventions in improving short-term pain outcomes following total knee replacement: A meta-analysis and systematic review. J. Orthop. Surg. Res. 2020, 15, 465. [Google Scholar] [CrossRef]
- Higgins, J.P.; Altman, D.G.; Gøtzsche, P.C.; Jüni, P.; Moher, D.; Oxman, A.D.; Savovic, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A. The cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, d5928. [Google Scholar] [CrossRef] [Green Version]
- Higgins, J.; Thomas, J.; Chandler, J.; Cumpston, M.; Li, T.; Page, M.; Welch, V. Cochrane Handbook for Systematic Reviews of Interventions Version 6.2; Cochrane: London, UK, 2021. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Academic Press: Cambridge, MA, USA, 2013. [Google Scholar]
- Egger, M.; Smith, G.D.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef] [Green Version]
- Simpson, J.A.; Weiner, E.S.C.; Press, O.U. The Oxford English Dictionary; Clarendon Press: Oxford, UK, 1989. [Google Scholar]
- Corrigan, M.J.; Keeler, J.R.; Miller, H.D.; Khallouq, B.A.B.; Fowler, S.B. Music therapy and retinopathy of prematurity screening: Using recorded maternal singing and heartbeat for post exam recovery. J. Perinatol. 2020, 40, 1780–1788. [Google Scholar] [CrossRef]
- Garcia Guerra, G.; Joffe, A.R.; Sheppard, C.; Hewson, K.; Dinu, I.A.; Hajihosseini, M.; deCaen, A.; Jou, H.; Hartling, L.; Vohra, S.; et al. Music use for sedation in critically ill children (musicc trial): A pilot randomized controlled trial. J. Intensive Care 2021, 9, 7. [Google Scholar] [CrossRef]
- Hartling, L.; Newton, A.S.; Liang, Y.; Jou, H.; Hewson, K.; Klassen, T.P.; Curtis, S. Music to reduce pain and distress in the pediatric emergency department: A randomized clinical trial. JAMA Pediatr. 2013, 167, 826–835. [Google Scholar] [CrossRef]
- Hatem, T.P.; Lira, P.I.; Mattos, S.S. The therapeutic effects of music in children following cardiac surgery. J. Pediatr. 2006, 82, 186–192. [Google Scholar] [CrossRef] [Green Version]
- Noguchi, L.K. The effect of music versus nonmusic on behavioral signs of distress and self-report of pain in pediatric injection patients. J. Music Ther. 2006, 43, 16–38. [Google Scholar] [CrossRef] [PubMed]
- Sunitha Suresh, B.S.; de Oliveira, G.S., Jr.; Suresh, S. The effect of audio therapy to treat postoperative pain in children undergoing major surgery: A randomized controlled trial. Pediatr. Surg. Int. 2015, 31, 197–201. [Google Scholar] [CrossRef] [PubMed]
- Yinger, O.S. Music therapy as procedural support for young children undergoing immunizations: A randomized controlled study. J. Music Ther. 2016, 53, 336–363. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dogan Baki, E.; Ulu, S.; Yuksek, A.; Arican, H.; Sivaci, R. Does listening to music during tonsillectomy affect sevoflurane consumption? Med. Princ. Pract. 2018, 27, 343–349. Available online: https://www.ncbi.nlm.nih.gov/pubmed/29529606 (accessed on 2 January 2022). [CrossRef] [PubMed]
- Bergomi, P.; Chieppi, M.; Maini, A.; Mugnos, T.; Spotti, D.; Tzialla, C.; Scudeller, L. Nonpharmacological techniques to reduce pain in preterm infants who receive heel-lance procedure: A randomized controlled trial. Res. Theory Nurs. Pract. 2014, 28, 335–348. [Google Scholar] [CrossRef]
- Bulut, M.; Alemdar, D.K.; Bulut, A.; Şalcı, G. The effect of music therapy, hand massage, and kaleidoscope usage on postoperative nausea and vomiting, pain, fear, and stress in children: A randomized controlled trial. J. Perianesth Nurs. 2020, 35, 649–657. [Google Scholar] [CrossRef]
- Döra, Ö.; Büyük, E.T. Effect of white noise and lullabies on pain and vital signs in invasive interventions applied to premature babies. Pain Manag. Nurs. 2021, 22, 724–729. [Google Scholar] [CrossRef]
- Duymaz, T. The effects of music therapy on gross motor functions, pain and level of functional independence in children with cerebral palsy. Ann. Clin. Anal. Med. 2020, 11, 115–119. [Google Scholar]
- Kristjánsdóttir, Ó.; Kristjánsdóttir, G. Randomized clinical trial of musical distraction with and without headphones for adolescents’ immunization pain. Scand. J. Caring. Sci. 2011, 25, 19–26. [Google Scholar] [CrossRef]
- Kühlmann, A.Y.R.; van Rosmalen, J.; Staals, L.M.; Keyzer-Dekker, C.M.G.; Dogger, J.; de Leeuw, T.G.; van der Toorn, F.; Jeekel, J.; Wijnen, R.M.H.; van Dijk, M. Music interventions in pediatric surgery (the music under surgery in children study): A randomized clinical trial. Anesth. Analg. 2020, 130, 991–1001. [Google Scholar] [CrossRef]
- Longhi, E.; Pickett, N.; Hargreaves, D. Wellbeing and hospitalized children: Can music help? Psychol. Music. 2013, 43, 188–196. [Google Scholar] [CrossRef]
- Muzzi, E.; Ronfani, L.; Bossini, B.; Lezcano, C.; Orzan, E.; Barbi, E. Effects of intraoperative auditory stimulation on pain and agitation on awakening after pediatric adenotonsillectomy: A randomized clinical trial. JAMA Otolaryngol. Head Neck Surg. 2021, 147, 638–645. [Google Scholar] [CrossRef] [PubMed]
- Nilsson, U. The anxiety-and pain-reducing effects of music interventions: A systematic review. AORN J 2008, 87, 780–807. [Google Scholar] [CrossRef] [PubMed]
- Shabani, F.; Nayeri, N.D.; Karimi, R.; Zarei, K.; Chehrazi, M. Effects of music therapy on pain responses induced by blood sampling in premature infants: A randomized cross-over trial. Iran. J. Nurs. Midwifery Res. 2016, 21, 391–396. [Google Scholar] [CrossRef]
- Tekgündüz, K.; Polat, S.; Gürol, A.; Apay, S.E. Oral glucose and listening to lullaby to decrease pain in preterm infants supported with ncpap: A randomized controlled trial. Pain Manag. Nurs. 2019, 20, 54–61. [Google Scholar] [CrossRef]
- Antonelli, E.; Vagnoli, L.; Ciucci, E.; Vernucci, C.; Lachi, F.; Messeri, A. A comparison of nonpharmacologic interventions on the emotional state of children in the emergency department. Pediatr. Emerg. Care 2019, 35, 81–88. [Google Scholar] [CrossRef]
- Aydin, D.; Sahiner, N.C. Effects of music therapy and distraction cards on pain relief during phlebotomy in children. Appl. Nurs. Res. 2017, 33, 164–168. [Google Scholar] [CrossRef]
- Azeem, M.; Ejaz, Z.; Ashraf, A.; Bukhari, F.; Ali, M.; Rashid, A. Music for pain control following orthodontic initial archwire placement. Pak. J. Med. Health Sci. 2021, 15, 1347–1348. [Google Scholar] [CrossRef]
- Kurdahi Badr, L.; Demerjian, T.; Daaboul, T.; Abbas, H.; Zeineddine, M.H.; Charafeddine, L. Preterm infants exhibited less pain during a heel stick when they were played the same music their mothers listened to during pregnancy. Acta Paediatr. 2017, 106, 438–445. [Google Scholar] [CrossRef]
- Balan, R.; Bavdekar, S.B.; Jadhav, S. Can indian classical instrumental music reduce pain felt during venepuncture? Indian J. Pediatr. 2009, 76, 469–473. [Google Scholar] [CrossRef]
- Huang, Y.L.; Lei, Y.Q.; Liu, J.F.; Cao, H.; Yu, X.R.; Chen, Q. Comparison of the effectiveness of music video therapy and music therapy on pain after cardiothoracic surgery in preschool children. Heart Surg. Forum 2021, 24, e299–e304. [Google Scholar] [CrossRef] [PubMed]
- Konar, M.C.; Islam, K.; Sil, A.; Nayek, K.; Barik, K. Effect of music on outcomes of birth asphyxia: A randomized controlled trial. J. Trop. Pediatrics 2021, 67, fmab009. [Google Scholar] [CrossRef] [PubMed]
- Lin, Z.W.; Liu, J.F.; Xie, W.P.; Chen, Q.; Cao, H. The effect of music therapy on chronic pain, quality of life and quality of sleep in adolescents after transthoracic occlusion of ventricular septal defect. Heart Surg. Forum 2021, 24, e305–e310. [Google Scholar] [CrossRef] [PubMed]
- Momenabadi, A.; Radmehr, M.; Sadeghi, N. Effect of two methods of acupressure in hugo point and music on severity of pain during iv insertion in children. Pak. J. Med. Health Sci. 2020, 14, 697–700. [Google Scholar]
- Nguyen, T.N.; Nilsson, S.; Hellström, A.L.; Bengtson, A. Music therapy to reduce pain and anxiety in children with cancer undergoing lumbar puncture: A randomized clinical trial. J. Pediatr. Oncol. Nurs. 2010, 27, 146–155. [Google Scholar] [CrossRef] [PubMed]
- Shukla, V.V.; Bansal, S.; Nimbalkar, A.; Chapla, A.; Phatak, A.; Patel, D.; Nimbalkar, S. Pain control interventions in preterm neonates: A randomized controlled trial. Indian Pediatrics 2018, 55, 292–296. [Google Scholar] [CrossRef]
- Tang, L.; Wang, H.; Liu, Q.; Wang, F.; Wang, M.; Sun, J.; Zhao, L. Effect of music intervention on pain responses in premature infants undergoing placement procedures of peripherally inserted central venous catheter: A randomized controlled trial. Eur. J. Integr. Med. 2018, 19, 105–109. Available online: https://www.sciencedirect.com/science/article/pii/S1876382018300520 (accessed on 2 January 2022). [CrossRef]
- Uematsu, H.; Sobue, I. Effect of music (brahms lullaby) and non-nutritive sucking on heel lance in preterm infants: A randomized controlled crossover trial. Paediatr. Child. Health 2019, 24, e33–e39. [Google Scholar] [CrossRef] [Green Version]
- Yu, H.; Liu, Y.; Li, S.; Ma, X. Effects of music on anxiety and pain in children with cerebral palsy receiving acupuncture: A randomized controlled trial. Int. J. Nurs. Stud. 2009, 46, 1423–1430. [Google Scholar] [CrossRef]
- Zhu, J.; Hong-Gu, H.; Zhou, X.; Wei, H.; Gao, Y.; Ye, B.; Liu, Z.; Chan, S.W. Pain relief effect of breast feeding and music therapy during heel lance for healthy-term neonates in china: A randomized controlled trial. Midwifery 2015, 31, 365–372. [Google Scholar] [CrossRef]
- Barandouzi, Z.A.; Keshavarz, M.; Montazeri, A.; Ashayeri, H.; Rajaei, Z. Comparison of the analgesic effect of oral sucrose and/or music in preterm neonates: A double-blind randomized clinical trial. Complement. Ther. Med. 2020, 48, 102271. [Google Scholar] [CrossRef] [PubMed]
- Eid, M.M.; Abdelbasset, W.K.; Abdelaty, F.M.; Ali, Z.A. Effect of physical therapy rehabilitation program combined with music on children with lower limb burns: A twelve-week randomized controlled study. Burns 2021, 47, 1146–1152. [Google Scholar] [CrossRef] [PubMed]
- van der Heijden, M.J.E.; Jeekel, J.; Rode, H.; Cox, S.; van Rosmalen, J.; Hunink, M.G.M.; van Dijk, M. Can live music therapy reduce distress and pain in children with burns after wound care procedures? A randomized controlled trial. Burns 2018, 44, 823–833. [Google Scholar] [CrossRef] [PubMed]
- Sun, J.; Freeman, B.D.; Natanson, C. Chapter 22—Meta-analysis of clinical trials. In Principles and Practice of Clinical Research, 4th ed.; Gallin, J.I., Ognibene, F.P., Johnson, L.L., Eds.; Academic Press: Boston, MA, USA, 2018; pp. 317–327. [Google Scholar]
- Sauerland, S.; Seiler, C.M. Role of systematic reviews and meta-analysis in evidence-based medicine. World J. Surg. 2005, 29, 582–587. [Google Scholar] [CrossRef]
- González-Martín-Moreno, M.; Garrido-Ardila, E.M.; Jiménez-Palomares, M.; Gonzalez-Medina, G.; Oliva-Ruiz, P.; Rodríguez-Mansilla, J. Music-based interventions in paediatric and adolescents oncology patients: A systematic review. Children 2021, 8, 73. [Google Scholar] [CrossRef]
- O’Toole, A.; Francis, K.; Pugsley, L. Does music positively impact preterm infant outcomes? Adv. Neonatal Care 2017, 17, 192–202. Available online: https://www.ncbi.nlm.nih.gov/pubmed/28398914 (accessed on 2 January 2022). [CrossRef]
- van der Heijden, M.J.; Araghi, S.O.; Jeekel, J.; Reiss, I.K.; Hunink, M.G.; van Dijk, M. Do hospitalized premature infants benefit from music interventions? A systematic review of randomized controlled trials. PLoS ONE 2016, 11, e0161848. [Google Scholar] [CrossRef]
- da Silva Santa, I.N.; Schveitzer, M.C.; Santos, M.D.; Ghelman, R.; Filho, V.O. Music interventions in pediatric oncology: Systematic review and meta-analysis. Complement. Ther. Med. 2021, 59, 102725. [Google Scholar] [CrossRef]
- Kühlmann, A.Y.R.; de Rooij, A.; Kroese, L.F.; van Dijk, M.; Hunink, M.G.M.; Jeekel, J. Meta-analysis evaluating music interventions for anxiety and pain in surgery. Br. J. Surg. 2018, 105, 773–783. [Google Scholar] [CrossRef] [Green Version]
- Kakar, E.; Billar, R.J.; van Rosmalen, J.; Klimek, M.; Takkenberg, J.J.M.; Jeekel, J. Music intervention to relieve anxiety and pain in adults undergoing cardiac surgery: A systematic review and meta-analysis. Open Heart 2021, 8, e001474. [Google Scholar] [CrossRef]
- Hole, J.; Hirsch, M.; Ball, E.; Meads, C. Music as an aid for postoperative recovery in adults: A systematic review and meta-analysis. Lancet 2015, 386, 1659–1671. [Google Scholar] [CrossRef]
- Dale, V.H. The impact of perioperative music on abdominal surgery patients’ experience of postoperative pain: A systematic review and meta-analysis. J. Perioper. Pract. 2021, 31, 31–43. [Google Scholar] [CrossRef] [PubMed]
- Graven, S.; Browne, J. Auditory development in the fetus and infant. Newborn Infant Nurs. Rev. 2008, 8, 187–193. [Google Scholar] [CrossRef] [Green Version]
- Zhang, Q.; Cheng, Q.; Li, H.; Dong, X.; Tu, W. Evaluation of auditory perception development in neonates by quantitative electroencephalography and auditory event-related potentials. PLoS ONE 2017, 12, e0183728. [Google Scholar] [CrossRef] [Green Version]
- Haslbeck, B.F.; Bassler, D. Music from the very beginning-a neuroscience-based framework for music as therapy for preterm infants and their parents. Front. Behav. Neurosci. 2018, 12, 112. [Google Scholar] [CrossRef]
- Colagiuri, B.; Schenk, L.A.; Kessler, M.D.; Dorsey, S.G.; Colloca, L. The placebo effect: From concepts to genes. Neuroscience 2015, 307, 171–190. [Google Scholar] [CrossRef] [Green Version]
- Richard-Lalonde, M.; Gélinas, C.; Boitor, M.; Gosselin, E.; Feeley, N.; Cossette, S.; Chlan, L.L. The effect of music on pain in the adult intensive care unit: A systematic review of randomized controlled trials. J. Pain Symptom. Manag. 2020, 59, 1304–1319.e6. [Google Scholar] [CrossRef]
- Devlin, J.W.; Skrobik, Y.; Gélinas, C.; Needham, D.M.; Slooter, A.J.C.; Pandharipande, P.P.; Watson, P.L.; Weinhouse, G.L.; Nunnally, M.E.; Rochwerg, B.; et al. Clinical practice guidelines for the prevention and management of pain, agitation/sedation, delirium, immobility, and sleep disruption in adult patients in the ICU. Crit. Care Med. 2018, 46, e825–e873. [Google Scholar] [CrossRef] [Green Version]
- Bhasin, P. Music therapy improves post-operative outcomes-a special perspective. J. Phys. Ther. 2012, 4, 75–77. [Google Scholar]
| Authors & Year | Journal | Country | Study Design | Comparison | Participants, No. | Age, Mean (SD), y/m/w/d | Age Group | Specialization | Setting | Condition | Pain Types | Type/Genres/Titles of Music | Equip | Outcome Measure/Assessment Tools |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Antonelli et al., 2019 | Wolters kluwer | Italy | Parallel RCT | Music Control | 57 48 | 8.20 (3.3), y 8.30 (4.1), y | Infant/Children | Emergency | In | ER pressure | Chronic/Procedural | Multiple Combinations | Live | WBS |
| Aydin et al., 2017 | Applied nursing research | Turkey | Parallel RCT | Music Control | 50 50 | 8.68 (2.2), y 9.20 (2.6), y | Infant/Children | Pain clinic | Out | IV insertion | Prick pain | Pop music | SPK | WBS |
| Azeem et al., 2021 | Cochrane Central Register of Controlled Trials | Pakistan | Parallel RCT | Music Control | 25 25 | 12–16, y ♫ | Adolescent | Dentistry | Out | Postop pain | Chronic/Procedural | -- | -- | VAS |
| Badr et al., 2017 | Acta Paediatr | Lebanon | Cross-over RCT | Music Control | 42 | 34.83 (1.3), GA, w | Newborn | Pediatrics | In | Heel Lance | Prick pain | Kids music/ World music | HDP | N-PASS HR, RR, SpO2 |
| Bakı et al., 2018 | Medical Principles and Practice | Turkey | Parallel RCT | Music Control | 25 25 | 6.60 (2.95), y 6.24 (3.38), y | Infant/Children | General surgery | In | Postop Pain | Postoperative Pain | Kids music | HDP | WBS BP, HR |
| Balan et al., 2009 | Indian Pediatrics | India | Parallel RCT | Music Control | 50 50 | 8.27 (2.05), y 7.42 (2.19), y | Infant/Children | Pain clinic | In | IV insertion | Prick pain | World music | ERP | VAS |
| Barandouzi et al., 2019 | Complementary Therapies in Medicine | Iran | Parallel RCT | Music Control | 30 30 | 34.00 (1.41), GA, w 33.86 (1.35), GA, w | Newborn | Pediatrics | In | IV insertion | Prick pain | Kids music | HDP | PIPP |
| Bergomi et al., 2014 | Research and Theory for Nursing Practice | Italy | Cross-over RCT | Music Control | 35 | 37.00 (5.43), GA, w | Newborn | Neonatology | In | Heel Lance | Prick pain | Classical music | SPK | PIPP |
| Bulut et al., 2020 | Journal of perianesthesia nursing | Turkey | Parallel RCT | Music Control | 35 35 | 7.37 (0.91), y 7.20 (0.67), y | Infant/Children | Pediatric surgery | In | Postop Pain | Postoperative Pain | Classical music | SPK | WBS |
| Corrigan et al., 2020 | Perinatol | USA | Parallel RCT | Music Control | 43 54 | 34.80 (0.86), GA, w 34.50 (0.92), GA, w | Newborn | Ophthalmology | Out | ROP | Chronic/Procedural | Kids music | SPK | PIPP |
| Döra et al., 2021 | Pain management nursing | Turkey | Parallel RCT | Music Control | 22 22 | 32–37, w, GA ♫ | Newborn | Neonatal ICU | In | Blood collection | Prick pain | Classical music | SPK | PIPP HR, RR, SpO2 |
| Duymaz, 2020 | Annals of Clinical and Analytical Medicine | Turkey | Parallel RCT | Music Control | 60 60 | 7.42 (2.40), y 7.60 (2.60), y | Infant/Children | Neurology | Out | Rehabilitation | Chronic/Procedural | Classical music | SPK | WBS |
| Eid et al., 2020 | Burns | Egypt | Parallel RCT | Music Control | 15 15 | 9.83 (1.25), y 9.71 (1.16), y | Infant/Children | Physical therapy | In | Rehabilitation | Chronic/Procedural | Classical music | SPK | VAS |
| Guerra et al., 2021 | Journal of Intensive Care | Canada | Parallel RCT | Music Control | 20 20 | 1.16 (3.5) 2.02 (3.5) | Infant/Children | Pediatric ICU | In | ICU procedure | Chronic/Procedural | Classical music | HDP | FLACC |
| Hartling et al., 2013 | JAMA Pediatrics | Canada | Parallel RCT | Music Control | 21 21 | 64.00 (50.27), m 78.00 (70.24), m | Infant/Children | Pediatrics | In | IV insertion | Prick pain | Multiple Combinations | SPK | FPS-R HR |
| Hatem et al., 2006 | Jornal de Pediatria | Brasil | Parallel RCT | Music Control | 61 18 | 1d-16y ♫ | Infant/Children | Cardiology | In | Postop Pain | Postoperative Pain | Classical music | HDP | FPS BP, HR, RR, SpO2 |
| Huang et al., 2021 | The Heart Surgery Forum | China | Parallel RCT | Music Control | 42 42 | 4.8 (1.7), y 5.9 (1.7), y | Infant/Children | Pediatric Surgery | In | Postop pain | Postoperative Pain | -- | ERP | WBS HR, BP, RR, SpO2 |
| Konar et al., 2021 | Journal of Tropical Pediatrics | India | Parallel RCT | Music Control | 1546 1549 | 34.3 (3.1), w 34.5 (3.0), w | Newborn | Neonatology | In | IV insertion | Prick pain | World music | SPK | N-PASS |
| Kristjánsdóttir et al., 2011 | Scandinavian Journal of Caring Sciences | Iceland | Parallel RCT | Music Control | 79 39 | 14.00 (0.18), y | Adolescent | - | Out | Immunization | Prick pain | Multiple Combinations | HDP/SPK | VAS |
| Kühlmann et al., 2020 | Anesthesia and Analgesia | Netherlands | Parallel RCT | Music Control | 59 59 | 6.90 (14.46), m 7.30 (16.89), m | Infant/Children | Pediatric surgery | In | Postop Pain | Postoperative Pain | Classical music | HDP | COMFORT-B |
| Lin et al., 2021 | The Heart Surgery Forum | China | Parallel RCT | Music Control | 25 25 | 7.3 (1.0), y 6.9 (1.2), y | Infant/Children | Pediatric Surgery | Out | Postop chronic pain | Chronic/Procedural | Pop music | SPK | VAS |
| Longhi et al., 2013 | Psychology of Music | UK | Cross-over RCT | Music Control | 37 | 7d-4y ♫ | Infant/Children | Pediatrics | In | Illness pressure | Chronic/Procedural | Kids music | Live | CHEOPS HR, SpO2 |
| Momenabadi et al., 2020 | Pakistan Journal of Medical and Health Sciences | Iran | Parallel RCT | Music Control | 30 30 | 51.50 (10.52), m 51.33 (8.63), m | Infant/Children | Pediatric | In | IV insertion | Prick pain | -- | SPK | OPS |
| Muzzi et al., 2021 | JAMA Otolaryngol Head Neck Surg | Italy | Parallel RCT | Music Control | 26 28 | 4.5 (3.6–6.0), y ♪ 5.2 (3.6–7.0), y ♪ | Infant/Children | Otorhinolaryngology | In | Postop pain | Postoperative Pain | Classical music | ERP | WBS, VAS |
| Nguyen et al., 2010 | Journal of Pediatric Oncology Nursing | Vietnam | Parallel RCT | Music Control | 20 20 | 8.80 (1.59), y 9.40 (1.93), y | Infant/Children | Pediatrics | In | Lumbar puncture | Prick pain | Special composition | ERP | NRS BP, HR, RR, SpO2 |
| Nilsson et al., 2009 | Paediatric Anaesthesia | Sweden | Parallel RCT | Music Control | 40 40 | 12 (7–16), y ♪ 13.5 (7–16), y ♪ | Infant/Children | General surgery | In | Postop Pain | Postoperative Pain | Special composition | SPK | VAS |
| Noguchi et al., 2006 | Journal of Music Therapy | USA | Parallel RCT | Music Control | 21 20 | 4.55 (0.65), y | Infant/Children | Pediatrics | Out | Immunization | Prick pain | Special composition | HDP | FPS |
| Shabani et al., 2016 | Iranian Journal of Nursing and Midwifery Research | Ireland | Cross-over RCT | Music Control | 20 | 29–36, GA, w ♫ | Newborn | Neonatology | In | IV insertion | Prick pain | Special composition | SPK | NFCS HR, SpO2 |
| Shukla et al., 2018 | Indian Pediatrics | India | Parallel RCT | Music Control | 49 51 | 8.10 (8.21), d 6.50 (4.38), d | Newborn | Pediatrics | In | Heel Lance | Prick pain | World music | SPK | PIPP |
| Suresh et al., 2015 | Pediatric Surgery International | USA | Parallel RCT | Music Control | 18 19 | 10.90 (5.20), y 12.40 (5.34), y | Infant/Children | General surgery | In | Postop Pain | Postoperative Pain | Kids music | HDP | FPS-R |
| Tang et al., 2018 | European Journal of Integrative Medicine | China | Parallel RCT | Music Control | 30 30 | 32.57 (1.76), GA, w 32. 57 (1.83), w | Newborn | Pediatrics | In | PICC | Chronic/Procedural | Kids music | SPK | PIPP HR, SpO2 |
| Tekgündüz et al., 2019 | Pain management nursing | Turkey | Parallel RCT | Music Control | 35 37 | 2.00 (1.91), d 2.49 (2.12), d | Newborn | Neonatology | In | C-PAP | Chronic/Procedural | Kids music | SPK | PIPP; NIPS HR, SpO2 |
| Uematsu et al., 2019 | Paediatrics and Child Health (Canada) | Japan | Cross-over RCT | Music Control | 25 | 33.80 (1.5), GA, w | Newborn | Neonatology | In | Heel Lance | Prick pain | Classical music | SPK | PIPP HR, SpO2 |
| ven der Heijden et al., 2018 | Burns | South Africa | Parallel RCT | Music Control | 71 64 | 24.30 (71.79), m 20.80 (42.04), m | Infant/Children | Intensive care | In | Wound care | Chronic/Procedural | Multiple Combinations | Live | COMFORT-B |
| ven der Heijden et al., 2019 | Journal of pediatric psychology | South Africa | Parallel RCT | Music Control | 75 54 | 7.50 (11.27), y 7.70 (8.81), y | Infant/Children | Emergency | In | ER procedure | Chronic/Procedural | Special composition | SPK | FPS-R HR |
| Yinger et al., 2016 | Journal of Music Therapy | USA | Parallel RCT | Music Control | 29 29 | 48.10 (6.7), m | Infant/Children | Pediatrics | Out | Immunization | Prick pain | Kids music | Live | CAMPIS-R |
| Yu et al., 2009 | International Journal of Nursing Studies | China | Parallel RCT | Music Control | 30 30 | 8.26 (2.83), y 7.87 (3.35), y | Infant/Children | Traditional Chinese medicine | Out | Acupuncture | Prick pain | Pop music | HDP | WBS BP, HR, RR |
| Zhu et al., 2015 | Midwifery | China | Parallel RCT | Music Control | 62 61 | 3.37 (0.58), d 3.11 (0.49), d | Newborn | Neonatology | In | Heel Lance | Prick pain | Classical music | SPK | NIPS |
| Intervention/Moderator | k | n | Effect Size | 95% CI-L | 95% CI-U | p Value | I2 (%) |
|---|---|---|---|---|---|---|---|
| Type of Pain | |||||||
| Chronic/Procedural | 12 | 869 | −0.41 | −0.64 | −0.64 | <0.001 | 63 |
| Postoperative pain | 8 | 571 | −0.49 | −0.90 | −0.08 | 0.018 | 81 |
| Prick pain | 20 | 4161 | −0.66 | −1.10 | −0.23 | 0.003 | 95 |
| Music style | |||||||
| Classical music | 11 | 738 | −0.71 | −1.00 | −0.42 | <0.001 | 71 |
| Kids music | 9 | 489 | −0.44 | −0.62 | −0.27 | <0.001 | 0 |
| Multiple combinations | 5 | 400 | −0.08 | −0.28 | 0.12 | 0.420 | 0 |
| Pop music | 3 | 210 | −0.45 | −0.73 | −0.18 | 0.001 | 0 |
| Special composition | 5 | 254 | −0.45 | −0.97 | 0.07 | 0.092 | 79 |
| World music | 4 | 3316 | −0.78 | −1.96 | 0.40 | 0.196 | 98 |
| Type of Equipment | |||||||
| HDP/ERP | 15 | 862 | −0.49 | −0.73 | −0.26 | <0.001 | 63 |
| SPK | 20 | 4357 | −0.63 | −1.07 | −0.19 | 0.005 | 96 |
| Live | 4 | 332 | −0.15 | −0.36 | 0.06 | 0.160 | 0 |
| Other rating/Self-rating | |||||||
| Other rating | 19 | 4208 | −0.57 | −1.04 | −0.10 | 0.017 | 96 |
| Self-rating | 21 | 1393 | −0.54 | −0.76 | −0.32 | <0.001 | 75 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ting, B.; Tsai, C.-L.; Hsu, W.-T.; Shen, M.-L.; Tseng, P.-T.; Chen, D.T.-L.; Su, K.-P.; Jingling, L. Music Intervention for Pain Control in the Pediatric Population: A Systematic Review and Meta-Analysis. J. Clin. Med. 2022, 11, 991. https://doi.org/10.3390/jcm11040991
Ting B, Tsai C-L, Hsu W-T, Shen M-L, Tseng P-T, Chen DT-L, Su K-P, Jingling L. Music Intervention for Pain Control in the Pediatric Population: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine. 2022; 11(4):991. https://doi.org/10.3390/jcm11040991
Chicago/Turabian StyleTing, Berne, Chia-Lin Tsai, Wei-Ti Hsu, Mei-Ling Shen, Ping-Tao Tseng, Daniel Tzu-Li Chen, Kuan-Pin Su, and Li Jingling. 2022. "Music Intervention for Pain Control in the Pediatric Population: A Systematic Review and Meta-Analysis" Journal of Clinical Medicine 11, no. 4: 991. https://doi.org/10.3390/jcm11040991
APA StyleTing, B., Tsai, C.-L., Hsu, W.-T., Shen, M.-L., Tseng, P.-T., Chen, D. T.-L., Su, K.-P., & Jingling, L. (2022). Music Intervention for Pain Control in the Pediatric Population: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine, 11(4), 991. https://doi.org/10.3390/jcm11040991









