Hospitalizations for Anorexia Nervosa during the COVID-19 Pandemic in France: A Nationwide Population-Based Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Source of Data and Selection Criteria
2.3. Variables
2.4. Statistical Analysis
3. Results
3.1. During vs. before the COVID-19 Pandemic
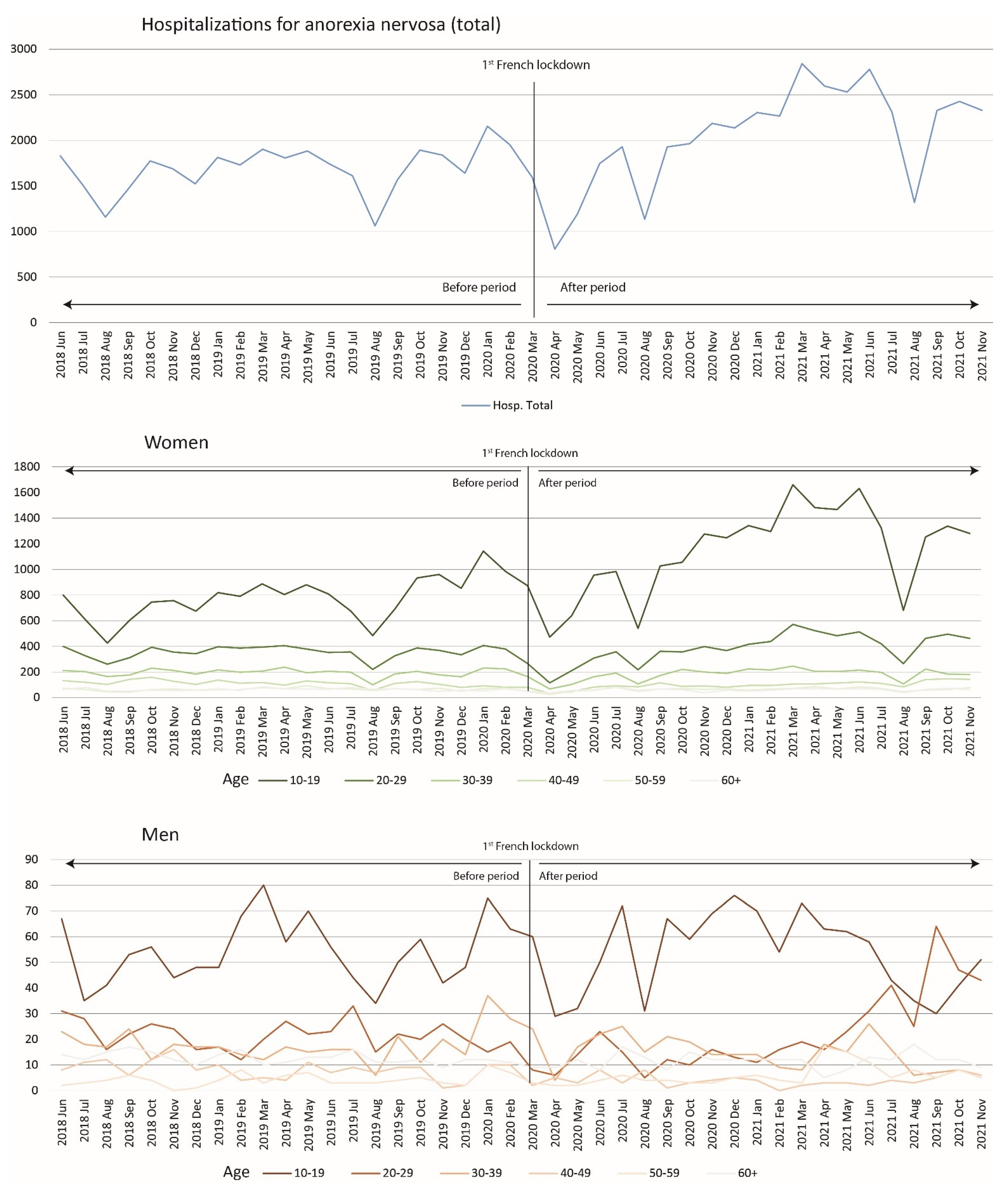
3.2. Monthly Changes
3.3. Multivariate Analysis: Risks of ICU Admissions and Hospitalization for AN with a Self-Harm Diagnosis
3.3.1. Factors Associated with ICU Admission of Patients with AN
3.3.2. Factors Associated with Admissions of Patients with AN for Self-Harm
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Carr, M.J.; Steeg, S.; Webb, R.T.; Kapur, N.; Chew-Graham, C.A.; Abel, K.M.; Hope, H.; Pierce, M.; Ashcroft, D.M. Effects of the COVID-19 pandemic on primary care-recorded mental illness and self-harm episodes in the UK: A population-based cohort study. Lancet Public Health 2021, 6, e124–e135. [Google Scholar] [CrossRef]
- Kendrick, K.; Isaac, M. Overview of behavioural and psychological consequences of COVID 19. Curr. Opin. Psychiatry 2021, 34, 477–484. [Google Scholar] [CrossRef] [PubMed]
- Liao, Y.H.; Fan, B.F.; Zhang, H.M.; Guo, L.; Lee, Y.; Wang, W.X.; Li, W.Y.; Gong, M.Q.; Lui, L.M.W.; Li, L.J.; et al. The impact of COVID-19 on subthreshold depressive symptoms: A longitudinal study. Epidemiol. Psychiatr. Sci. 2021, 30, e20. [Google Scholar] [CrossRef] [PubMed]
- Winkler, P.; Mohrova, Z.; Mlada, K.; Kuklova, M.; Kagstrom, A.; Mohr, P.; Formanek, T. Prevalence of current mental disorders before and during the second wave of COVID-19 pandemic: An analysis of repeated nationwide cross-sectional surveys. J. Psychiatr. Res. 2021, 139, 167–171. [Google Scholar] [CrossRef] [PubMed]
- COVID-19 Mental Disorders Collaborators. Global prevalence and burden of depressive and anxiety disorders in 204 countries and territories in 2020 due to the COVID-19 pandemic. Lancet Lond. Engl. 2021, 398, 1700–1712. [Google Scholar] [CrossRef]
- Revet, A.; Hebebrand, J.; Anagnostopoulos, D.; Kehoe, L.A.; Gradl-Dietsch, G.; COVID-19 Child and Adolescent Psychiatry Consortium; Klauser, P.; Anderluh, M.; Armando, M.; Askenazy, F.; et al. Perceived impact of the COVID-19 pandemic on child and adolescent psychiatric services after 1 year (February/March 2021): ESCAP CovCAP survey. Eur. Child Adolesc. Psychiatry, 2021; Online ahead of print. [Google Scholar] [CrossRef]
- Levaillant, M.; Wathelet, M.; Lamer, A.; Riquin, E.; Gohier, B.; Hamel-Broza, J.F. Impact of COVID-19 pandemic and lockdowns on the consumption of anxiolytics, hypnotics and antidepressants according to age groups: A French nationwide study. Psychol. Med. 2021; Online ahead of print. [Google Scholar] [CrossRef]
- Gloster, A.T.; Lamnisos, D.; Lubenko, J.; Presti, G.; Squatrito, V.; Constantinou, M.; Nicolaou, C.; Papacostas, S.; Aydın, G.; Chong, Y.Y.; et al. Impact of COVID-19 pandemic on mental health: An international study. PLoS ONE 2020, 15, e0244809. [Google Scholar] [CrossRef]
- Andersen, A.J.; Mary-Krause, M.; Bustamante, J.J.H.; Héron, M.; El Aarbaoui, T.; Melchior, M. Symptoms of anxiety/depression during the COVID-19 pandemic and associated lockdown in the community: Longitudinal data from the TEMPO cohort in France. BMC Psychiatry 2021, 21, 381. [Google Scholar] [CrossRef]
- Pierce, M.; Hope, H.; Ford, T.; Hatch, S.; Hotopf, M.; John, A.; Kontopantelis, E.; Webb, R.; Wessely, S.; McManus, S.; et al. Mental health before and during the COVID-19 pandemic: A longitudinal probability sample survey of the UK population. Lancet Psychiatry 2020, 7, 883–892. [Google Scholar] [CrossRef]
- Miniati, M.; Marzetti, F.; Palagini, L.; Marazziti, D.; Orrù, G.; Conversano, C.; Gemignani, A. Eating Disorders Spectrum during the COVID Pandemic: A Systematic Review. Front. Psychol. 2021, 12, 663376. [Google Scholar] [CrossRef]
- van Hoeken, D.; Hoek, H.W. Review of the burden of eating disorders: Mortality, disability, costs, quality of life, and family burden. Curr. Opin. Psychiatry 2020, 33, 521–527. [Google Scholar] [CrossRef]
- Zeppegno, P.; Calati, R.; Madeddu, F.; Gramaglia, C. The Interpersonal-Psychological Theory of Suicide to Explain Suicidal Risk in Eating Disorders: A Mini-Review. Front. Psychiatry 2021, 12, 690903. [Google Scholar] [CrossRef] [PubMed]
- Guinhut, M.; Godart, N.; Benadjaoud, M.A.; Melchior, J.C.; Hanachi, M. Five-year mortality of severely malnourished patients with chronic anorexia nervosa admitted to a medical unit. Acta Psychiatr. Scand. 2021, 143, 130–140. [Google Scholar] [CrossRef] [PubMed]
- Arcelus, J.; Mitchell, A.J.; Wales, J.; Nielsen, S. Mortality rates in patients with anorexia nervosa and other eating disorders. A meta-analysis of 36 studies. Arch. Gen. Psychiatry 2011, 68, 724–731. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Aranda, F.; Munguía, L.; Mestre-Bach, G.; Steward, T.; Etxandi, M.; Baenas, I.; Granero, R.; Sánchez, I.; Ortega, E.; Andreu, A.; et al. COVID Isolation Eating Scale (CIES): Analysis of the impact of confinement in eating disorders and obesity-A collaborative international study. Eur. Eat. Disord. Rev. J. Eat. Disord. Assoc. 2020, 28, 871–883. [Google Scholar] [CrossRef]
- Goldberg, L.; Ziv, A.; Vardi, Y.; Hadas, S.; Zuabi, T.; Yeshareem, L.; Gur, T.; Steinling, S.; Scheuerman, O.; Levinsky, Y. The effect of COVID-19 pandemic on hospitalizations and disease characteristics of adolescents with anorexia nervosa. Eur. J. Pediatr. 2022, 181, 1767–1771. [Google Scholar] [CrossRef] [PubMed]
- Lin, J.A.; Hartman-Munick, S.M.; Kells, M.R.; Milliren, C.E.; Slater, W.A.; Woods, E.R.; Forman, S.F.; Richmond, T.K. The Impact of the COVID-19 Pandemic on the Number of Adolescents/Young Adults Seeking Eating Disorder-Related Care. J. Adolesc. Health Off. Publ. Soc. Adolesc. Med. 2021, 69, 660–663. [Google Scholar] [CrossRef] [PubMed]
- Otto, A.K.; Jary, J.M.; Sturza, J.; Miller, C.A.; Prohaska, N.; Bravender, T.; Van Huysse, J. Medical Admissions Among Adolescents with Eating Disorders During the COVID-19 Pandemic. Pediatrics 2021, 148, e2021052201. [Google Scholar] [CrossRef] [PubMed]
- Toulany, A.; Kurdyak, P.; Guttmann, A.; Stukel, T.A.; Fu, L.; Strauss, R.; Fiksenbaum, L.; Saunders, N.R. Acute Care Visits for Eating Disorders among Children and Adolescents after the Onset of the COVID-19 Pandemic. J. Adolesc. Health Off. Publ. Soc. Adolesc. Med. 2022, 70, 42–47. [Google Scholar] [CrossRef]
- Tavolacci, M.P.; Ladner, J.; Dechelotte, P. COVID-19 Pandemic and Eating Disorders among University Students. Nutrients 2021, 13, 4294. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet Lond. Engl. 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Touyz, S.; Lacey, H.; Hay, P. Eating disorders in the time of COVID-19. J. Eat. Disord. 2020, 8, 19. [Google Scholar] [CrossRef] [PubMed]
- González-Monroy, C.; Gómez-Gómez, I.; Olarte-Sánchez, C.M.; Motrico, E. Eating Behaviour Changes during the COVID-19 Pandemic: A Systematic Review of Longitudinal Studies. Int. J. Environ. Res. Public Health 2021, 18, 11130. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, J.E.; Peterson, C.B. Anorexia Nervosa. N. Engl. J. Med. 2020, 382, 1343–1351. [Google Scholar] [CrossRef] [PubMed]
- Puckett, L.; Grayeb, D.; Khatri, V.; Cass, K.; Mehler, P. A Comprehensive Review of Complications and New Findings Associated with Anorexia Nervosa. J. Clin. Med. 2021, 10, 2555. [Google Scholar] [CrossRef]
- Jollant, F.; Roussot, A.; Corruble, E.; Chauvet-Gelinier, J.C.; Falissard, B.; Mikaeloff, Y.; Quantin, C. Hospitalization for self-harm during the early months of the COVID-19 pandemic in France: A nationwide retrospective observational cohort study. Lancet Reg. Health Eur. 2021, 6, 100102. [Google Scholar] [CrossRef]
- Zou, G. A modified poisson regression approach to prospective studies with binary data. Am. J. Epidemiol. 2004, 159, 702–706. [Google Scholar] [CrossRef]
- Ayuso-Mateos, J.L.; Morillo, D.; Haro, J.M.; Olaya, B.; Lara, E.; Miret, M. Changes in depression and suicidal ideation under severe lockdown restrictions during the first wave of the COVID-19 pandemic in Spain: A longitudinal study in the general population. Epidemiol. Psychiatr. Sci. 2021, 30, e49. [Google Scholar] [CrossRef]
- Wan Mohd Yunus, W.M.A.; Kauhanen, L.; Sourander, A.; Brown, J.S.L.; Peltonen, K.; Mishina, K.; Lempinen, L.; Bastola, K.; Gilbert, S.; Gyllenberg, D. Registered psychiatric service use, self-harm and suicides of children and young people aged 0–24 before and during the COVID-19 pandemic: A systematic review. Child Adolesc. Psychiatry Ment. Health 2022, 16, 15. [Google Scholar] [CrossRef]
- Bera, L.; Souchon, M.; Ladsous, A.; Colin, V.; Lopez-Castroman, J. Emotional and Behavioral Impact of the COVID-19 Epidemic in Adolescents. Curr. Psychiatry Rep. 2022, 24, 37–46. [Google Scholar] [CrossRef]
- Monteleone, P. Eating Disorders in the Era of the COVID-19 Pandemic: What Have We Learned? Int. J. Environ. Res. Public Health 2021, 18, 12381. [Google Scholar] [CrossRef]
- Solmi, F.; Downs, J.L.; Nicholls, D.E. COVID-19 and eating disorders in young people. Lancet Child Adolesc. Health 2021, 5, 316–318. [Google Scholar] [CrossRef]
- Herpertz-Dahlmann, B. Adolescent eating disorders: Update on definitions, symptomatology, epidemiology, and comorbidity. Child Adolesc. Psychiatr. Clin. N. Am. 2015, 24, 177–196. [Google Scholar] [CrossRef] [PubMed]
- Taquet, M.; Dercon, Q.; Luciano, S.; Geddes, J.R.; Husain, M.; Harrison, P.J. Incidence, co-occurrence, and evolution of long-COVID features: A 6-month retrospective cohort study of 273,618 survivors of COVID-19. PLoS Med. 2021, 18, e1003773. [Google Scholar] [CrossRef]
- Cliffe, C.; Shetty, H.; Himmerich, H.; Schmidt, U.; Stewart, R.; Dutta, R. Suicide attempts requiring hospitalization in patients with eating disorders: A retrospective cohort study. Int. J. Eat. Disord. 2020, 53, 458–465. [Google Scholar] [CrossRef] [PubMed]
- Campitelli, M.A.; Bronskill, S.E.; Maclagan, L.C.; Harris, D.A.; Cotton, C.A.; Tadrous, M.; Gruneir, A.; Hogan, D.B.; Maxwell, C.J. Comparison of Medication Prescribing Before and After the COVID-19 Pandemic Among Nursing Home Residents in Ontario, Canada. JAMA Netw. Open 2021, 4, e2118441. [Google Scholar] [CrossRef]

| Pre-COVID-19 | During COVID-19 | Total | Relative Risk (95% CI) for the pre- vs. during-COVID-19 Periods | ||||||
|---|---|---|---|---|---|---|---|---|---|
| June 2018–Feburary 2020 | March 2020–November 2021 | ||||||||
| N | % | N | % | N | % | ||||
| Hospitalizations | 35,536 | 42,643 | 78,179 | 1.20 (1.18–1.22) *** | £ | ||||
| Patients | 10,330 | 11,270 | 21,600 | 1.09 (1.06–1.12) *** | |||||
| Gender and age | |||||||||
| Female | 33,045 | 93.0 | 40,307 | 94.5 | 73,352 | 1.22 (1.20–1.24) *** | £ | ||
| Mean age | 25.6 (±14.6) | 23.4 (±13.2) | t-Test = −21.9; p < 0.0001 | $ | |||||
| 10–19 | 16,338 | 46.0 | 23,833 | 55.9 | 40,171 | 51.4 | 1.46 (1.43–1.49) *** | £ | |
| 20–29 | 7489 | 21.1 | 8016 | 18.8 | 15,505 | 19.8 | 1·07 (1.04–1.11) *** | ||
| 30–39 | 4125 | 11.6 | 3786 | 8.9 | 7911 | 10.1 | 0.92 (0.88–0.96) *** | ||
| 40–49 | 2367 | 6.7 | 2063 | 4.8 | 4430 | 5.7 | 0.87 (0.82–0.93) *** | ||
| 50–59 | 1380 | 3.9 | 1344 | 3.2 | 2724 | 3.5 | 0.97 (0.90.1.05) | ||
| 60+ | 1346 | 3.8 | 1265 | 3.0 | 2611 | 3.3 | 0.94 (0.87–1.02) | ||
| Male | 2491 | 2336 | 4827 | 0.94 (0.89–0.99) * | £ | ||||
| Mean age | 29.3 (±19.0) | 28.8 (±18.6) | t-Test = -0.9; p = 0.302 | $ | |||||
| 10–19 | 1139 | 2.6 | 1125 | 3.2 | 2264 | 2.9 | 0.99 (0.91–1.07) | £ | |
| 20–29 | 454 | 1.1 | 458 | 1.3 | 912 | 1.2 | 1.01 (0.89–1.15) | ||
| 30–39 | 373 | 0.7 | 308 | 1.1 | 681 | 0.9 | 0.83 (0.71–0.96) * | ||
| 40–49 | 171 | 0.2 | 82 | 0.5 | 253 | 0.3 | 0.48 (0.37–0.62) *** | ||
| 50–59 | 88 | 0.3 | 123 | 0.3 | 211 | 0.3 | 1.40 (1.06–1.84) * | ||
| 60+ | 266 | 0.6 | 240 | 0.8 | 506 | 0.6 | 0.90 (0.76–1.07) | ||
| Hosp. Characteristics | |||||||||
| Stays per patient | 3.44 (±8.4) | 3.78 (±10.5) | - | t-Test = 2.63; p = 0.008 | $ | ||||
| Mean length of stay (days) | 5.32 (±16.3) | 5.37 (±17.4) | - | t-Test = 0.49; p = 0.627 | |||||
| Self-harm | 1088 | 3.1 | 1341 | 3.1 | 2429 | 3.1 | 1.23 (1.14–1.34) *** | £ | |
| Hosp. In ICU | 452 | 1.3 | 428 | 1.0 | 880 | 1.1 | 0.95 (0.83–1.08) | ||
| Hosp. Death | 181 | 0.5 | 154 | 0.4 | 335 | 0.4 | HR = 0.73 (0.59–0.91); p = 0.004 | µ | |
| Hospitalization in Intensive Care Unit (N = 880) | Self-Harm Diagnosis during Hospitalization for AN (N = 2429) | |||||||
|---|---|---|---|---|---|---|---|---|
| BEFORE COVID-19 (N = 452) | DURING COVID-19 (N = 428) | BEFORE COVID-19 (N = 1088) | DURING COVID-19 (N = 1341) | |||||
| N | aOR | N | aOR | N | aOR | N | aOR | |
| Age class | ||||||||
| 10–19 | 55 | 0.16 (0.11–0.23) *** | 73 | 0.11 (0.08–0.15) *** | 771 | 3.12 (2.48–3.98) *** | 981 | 2.40 (1.89–3.05) *** |
| 20–29 | 108 | 0.89 (0.65–1.22) | 99 | 0.50 (0.37–0.67) *** | 150 | 1.15 (0.87–1.53) | 212 | 1.39 (1.06–1.81) * |
| 30–39 | Ref | Ref | ||||||
| 40–49 | 58 | 1.53 (1.07–2.19) * | 56 | 1.22 (0.86–1.72) | 39 | 0.85 (0.57–1.27) | 38 | 0.84 (0.56–1.25) |
| 50–59 | 71 | 2.86 (2.02–4.06) *** | 52 | 1.61 (1.13–2.30) ** | 35 | 1.11 (0.73–1.69) | 16 | 0.49 (0.28–0.85) * |
| 60+ | 91 | 2.97 (2.10–4.19) *** | 58 | 1.45 (1.01–2.09) * | 19 | 0.53 (0.31–0.89) * | 14 | 0.45 (0.25–0.81) ** |
| Gender | ||||||||
| Female | 422 | 1.32 (0.89–1.96) | 392 | 0.81 (0.57–1.17) | 1058 | 2.58 (1.79–3.73) *** | 1321 | 3.71 (2.38–5.80) *** |
| Other adverse outcome | ||||||||
| Hosp. death | 54 | 13.94 (9.63–20.18) *** | 28 | 8.42 (5.30–13.38) *** | 7 | 0.62 (0.27–1.43) | 1 | 0.20 (0.03–1.46) |
| Self-harm | 85 | 14.70 (11.22–19.25) *** | 85 | 14.26 (10.96–18.55) *** | ||||
| ICU | 85 | 15.05 (11.44–19.81) *** | 85 | 14.68 (11.27–19.13) *** | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chauvet-Gelinier, J.-C.; Roussot, A.; Vergès, B.; Petit, J.-M.; Jollant, F.; Quantin, C. Hospitalizations for Anorexia Nervosa during the COVID-19 Pandemic in France: A Nationwide Population-Based Study. J. Clin. Med. 2022, 11, 4787. https://doi.org/10.3390/jcm11164787
Chauvet-Gelinier J-C, Roussot A, Vergès B, Petit J-M, Jollant F, Quantin C. Hospitalizations for Anorexia Nervosa during the COVID-19 Pandemic in France: A Nationwide Population-Based Study. Journal of Clinical Medicine. 2022; 11(16):4787. https://doi.org/10.3390/jcm11164787
Chicago/Turabian StyleChauvet-Gelinier, Jean-Christophe, Adrien Roussot, Bruno Vergès, Jean-Michel Petit, Fabrice Jollant, and Catherine Quantin. 2022. "Hospitalizations for Anorexia Nervosa during the COVID-19 Pandemic in France: A Nationwide Population-Based Study" Journal of Clinical Medicine 11, no. 16: 4787. https://doi.org/10.3390/jcm11164787
APA StyleChauvet-Gelinier, J.-C., Roussot, A., Vergès, B., Petit, J.-M., Jollant, F., & Quantin, C. (2022). Hospitalizations for Anorexia Nervosa during the COVID-19 Pandemic in France: A Nationwide Population-Based Study. Journal of Clinical Medicine, 11(16), 4787. https://doi.org/10.3390/jcm11164787






