The Effect of COVID-19 on the Menstrual Cycle: A Systematic Review
Abstract
:1. Introduction
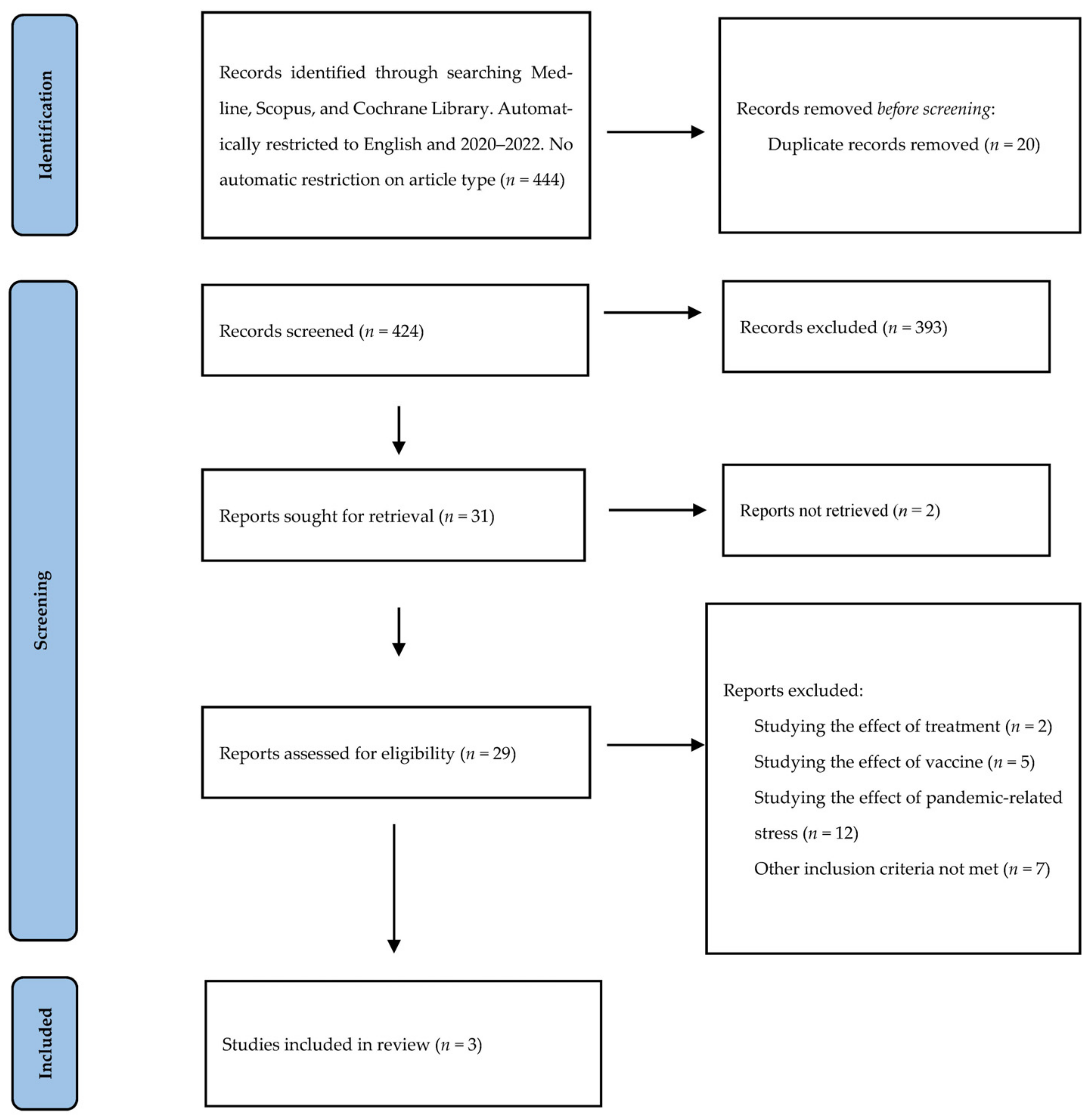
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO Coronavirus (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 21 February 2022).
- Lovato, A.; De Filippis, C. Clinical presentation of COVID-19: A systematic review focusing on upper airway symptoms. Ear Nose Throat J. 2020, 99, 569–576. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xie, Y.; Xu, E.; Bowe, B.; Al-Aly, Z. Long-term cardiovascular outcomes of COVID-19. Nat. Med. 2022, 28, 583–590. [Google Scholar] [CrossRef] [PubMed]
- Spudich, S.; Nath, A. Nervous system consequences of COVID-19. Science 2022, 375, 267–269. [Google Scholar] [CrossRef]
- Morgan, E. Pandemic Periods: Why Women’s Menstrual Cycles Have Gone Haywire. Available online: https://www.theguardian.com/society/2021/mar/25/pandemic-periods-why-womens-menstrual-cycles-have-gone-haywire (accessed on 21 February 2022).
- Phelan, N.; Behan, L.; Owens, L. The impact of the COVID-19 pandemic on women’s reproductive health. Front. Endocrinol. 2021, 12, 642755. [Google Scholar] [CrossRef] [PubMed]
- Chirgwin, K.; Feldman, J.; Muneyyirci-Delale, O.; Landesman, S.; Minkoff, H. Menstrual function in human immunodeficiency virus-infected women without acquired immunodeficiency syndrome. J. Acquir. Immune Defic. Syndr. Hum. Retrovirol. 1996, 12, 489–494. [Google Scholar] [CrossRef]
- King, E.; Albert, A.; Murray, M. HIV and amenorrhea. Aids 2019, 33, 483–491. [Google Scholar] [CrossRef]
- Kurmanova, A.; Kurmanova, G.; Lokshin, V. Reproductive dysfunctions in viral hepatitis. Gynecol. Endocrinol. 2016, 32, 37–40. [Google Scholar] [CrossRef]
- Li, K.; Chen, G.; Hou, H.; Liao, Q.; Chen, J.; Bai, H.; Lee, S.; Wang, C.; Li, H.; Cheng, L.; et al. Analysis of sex hormones and menstruation in COVID-19 women of child-bearing age. Reprod. BioMed. Online 2021, 42, 260–267. [Google Scholar] [CrossRef]
- Ding, T.; Wang, T.; Zhang, J.; Cui, P.; Chen, Z.; Zhou, S.; Yuan, S.; Ma, W.; Zhang, M.; Rong, Y.; et al. Analysis of ovarian injury associated with COVID-19 disease in reproductive-aged women in Wuhan, China: An observational study. Front. Med. 2021, 8, 635255. [Google Scholar] [CrossRef]
- Khan, S.; Shilen, A.; Heslin, K.; Ishimwe, P.; Allen, A.; Jacobs, E.; Farland, L. SARS-CoV-2 infection and subsequent changes in the menstrual cycle among participants in the Arizona CoVHORT study. Am. J. Obstet. Gynecol. 2022, 226, 270–273. [Google Scholar] [CrossRef]
- Catalfamo, C.; Heslin, K.; Shilen, A.; Khan, S.; Hunsaker, J.; Austhof, E.; Barraza, L.; Cordova-Marks, F.; Farland, L.; Garcia-Filion, P.; et al. Design of the Arizona CoVHORT: A population-based COVID-19 cohort. Front. Public Health 2021, 9, 620060. [Google Scholar] [CrossRef]
- Metlay, J.; Waterer, G.; Long, A.; Anzueto, A.; Brozek, J.; Crothers, K.; Cooley, L.; Dean, N.; Fine, M.; Flanders, S.; et al. Diagnosis and treatment of adults with community-acquired pneumonia. An official clinical practice guideline of the American Thoracic Society and Infectious Diseases Society of America. Am. J. Respir. Crit. Care Med. 2019, 200, e45–e67. [Google Scholar] [CrossRef] [PubMed]
- Guan, W.; Ni, Z.; Hu, Y.; Liang, W.; Ou, C.; He, J.; Liu, L.; Shan, H.; Lei, C.; Hui, D.; et al. Clinical characteristics of coronavirus disease 2019 in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar] [CrossRef] [PubMed]
- Nagma, S. To evaluate the effect of perceived stress on menstrual function. J. Clin. Diagn. Res. 2015, 9, QC01–QC03. [Google Scholar] [CrossRef] [PubMed]
- Ozimek, N.; Velez, K.; Anvari, H.; Butler, L.; Goldman, K.; Woitowich, N. Impact of stress on menstrual cyclicity during the coronavirus disease 2019 pandemic: A survey study. J. Womens Health 2022, 31, 84–90. [Google Scholar] [CrossRef]
- Coronavirus Vaccine-Weekly Summary of Yellow Card Reporting. Available online: https://www.gov.uk/government/publications/coronavirus-covid-19-vaccine-adverse-reactions/coronavirus-vaccine-summary-of-yellow-card-reporting#annex-1-vaccine-analysis-print (accessed on 16 February 2022).
- Edelman, A.; Boniface, E.; Benhar, E.; Han, L.; Matteson, K.; Favaro, C.; Pearson, J.; Darney, B. Association between menstrual cycle length and coronavirus disease 2019 (COVID-19) vaccination. Obstet. Gynecol. 2022, 139, 481–489. [Google Scholar] [CrossRef]
- Laganà, A.; Veronesi, G.; Ghezzi, F.; Ferrario, M.; Cromi, A.; Bizzarri, M.; Garzon, S.; Cosentino, M. Evaluation of menstrual irregularities after COVID-19 vaccination: Results of the MECOVAC survey. Open Med. 2022, 17, 475–484. [Google Scholar] [CrossRef]
- Therapeutic Management of Hospitalized Adults with COVID-19. Available online: https://www.covid19treatmentguidelines.nih.gov/ (accessed on 27 February 2022).
- Warner, P.; Whitaker, L.; Parker, R.; Weir, C.; Douglas, A.; Hansen, C.; Madhra, M.; Hillier, S.; Saunders, P.; Iredale, J.; et al. Low dose dexamethasone as treatment for women with heavy menstrual bleeding: A response-adaptive randomised placebo-controlled dose-finding parallel group trial (DexFEM). EBioMedicine 2021, 69, 103434. [Google Scholar] [CrossRef]
- Kunno, J.; Supawattanabodee, B.; Sumanasrethakul, C.; Wiriyasivaj, B.; Kuratong, S.; Kaewchandee, C. Comparison of different waves during the COVID-19 pandemic: Retrospective descriptive study in Thailand. Adv. Prev. Med. 2021, 2021, 5807056. [Google Scholar] [CrossRef]
- Iftimie, S.; López-Azcona, A.; Vallverdú, I.; Hernández-Flix, S.; De Febrer, G.; Parra, S.; Hernández-Aguilera, A.; Riu, F.; Joven, J.; Andreychuk, N.; et al. First and second waves of coronavirus disease-19: A comparative study in hospitalized patients in Reus, Spain. PLoS ONE 2021, 16, e0248029. [Google Scholar] [CrossRef]
- Volicer, B.; Burns, M. Preexisting correlates of hospital stress. Nurs. Res. 1977, 26, 408–415. [Google Scholar] [CrossRef] [PubMed]
- Mahajan, S.; Caraballo, C.; Li, S.; Dong, Y.; Chen, L.; Huston, S.; Srinivasan, R.; Redlich, C.; Ko, A.; Faust, J.; et al. SARS-CoV-2 Infection hospitalization rate and infection fatality rate among the non-congregate population in Connecticut. Am. J. Med. 2021, 134, 812–816.e2. [Google Scholar] [CrossRef] [PubMed]
- Vahey, G.; McDonald, E.; Marshall, K.; Martin, S.; Chun, H.; Herlihy, R.; Tate, J.; Kawasaki, B.; Midgley, C.; Alden, N.; et al. Risk factors for hospitalization among persons with COVID-19—Colorado. PLoS ONE 2021, 16, e0256917. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.; Kim, D.; Nam, G.; Nam, H.; Kim, Y.; Lee, S.; Han, K.; Park, Y. Association between metabolic syndrome and menstrual irregularity in middle-aged Korean women. Korean J. Fam. Med. 2016, 37, 31. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sharp, G.; Fraser, A.; Sawyer, G.; Kountourides, G.; Easey, K.; Ford, G.; Olszewska, Z.; Howe, L.; Lawlor, D.; Alvergne, A.; et al. The COVID-19 pandemic and the menstrual cycle: Research gaps and opportunities. Int. J. Epidemiol. 2021, 51, 691–700. [Google Scholar] [CrossRef]
| First Author, Year | Type of Study | Comparison | Sample Size | Sample Characteristics | Inclusion Criteria | Exclusion Criteria |
|---|---|---|---|---|---|---|
| Li et al., 2021 [10] | Cross-sectional hospital-based study | COVID-19 patients vs. controls and COVID-19 patients during disease vs. before | 177 cases (119 non-severe cases, 58 severe); 91 controls | Average age 36 | Women between 18 and 45 years old; confirmed COVID-19 | Pregnant or lactating; history of a diagnosis of ovarian dysfunction in the 6 months before onset of disease: manifestation of delayed menses, menstrual irregularities, or earlier menopause; prior hysterectomy or oophorectomy |
| Khan et al., 2021 [12] | Prospective population-based cohort study | COVID-19 patients that reported a change in menstrual cycle after infection vs. COVID-19 patients that reported no changes | 127 (20 participants that reported a change in their menstrual cycle after infection, 107 participants that did not report a change) | Patients that reported menstrual cycle irregularities: mean age 30.5; mean BMI 28.1. Patients that did not report menstrual cycle irregularities: mean age 30.6; mean BMI 27.6 | SARS-CoV-2-positive participants that were 18 to 45 years old, identified as women or nonbinary | Currently or recently pregnant, as of January 2020 |
| Ding et al., 2021 [11] | Cross-sectional hospital-based study | Severe vs. non-severe COVID-19 cases | 78 (61 non-severe cases, 17 severe) | Median age 43, median BMI 22.7, all had one child or more, 48% had a recent mental disorder, 12% had a history of benign gynecological disease, 36% had undergone gynecological surgery | Female patients of reproductive age and younger than 50 | Ovarian diseases or ovarian surgery history; denial of request for blood collection; pregnancy; taking oral or transdermal estrogen-containing products |
| First Author, Year | Main Findings |
|---|---|
| Li et al., 2021 [10] | Forty-five (25%) patients presented with menstrual volume changes and fifty (28%) patients had menstrual cycle changes, mainly concerning decreased volume (20%) and a prolonged cycle (19%); severely ill patients had more comorbidities than mildly ill patients (34% versus 8%). |
| Khan et al., 2021 [12] | People that reported changes in their menstrual cycle after SARS-CoV-2 infection reported more COVID-19 symptoms than those that did not. The mean age (30.5 vs. 30.6) and the mean BMI (28.1 vs. 27.0) of the two groups were similar. The percentage of patients of Hispanic ethnicity was higher among the patients that had reported menstrual cycle changes (50% vs. 24.3%). |
| Ding et al., 2021 [11] | Menstrual status (p = 0.55), menstrual volume (p = 0.066), phase of menstrual cycle (p = 0.58), and dysmenorrhea history (p = 0.12) were similar without significant differences between non-severe and severe COVID-19 women |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lebar, V.; Laganà, A.S.; Chiantera, V.; Kunič, T.; Lukanović, D. The Effect of COVID-19 on the Menstrual Cycle: A Systematic Review. J. Clin. Med. 2022, 11, 3800. https://doi.org/10.3390/jcm11133800
Lebar V, Laganà AS, Chiantera V, Kunič T, Lukanović D. The Effect of COVID-19 on the Menstrual Cycle: A Systematic Review. Journal of Clinical Medicine. 2022; 11(13):3800. https://doi.org/10.3390/jcm11133800
Chicago/Turabian StyleLebar, Vojka, Antonio Simone Laganà, Vito Chiantera, Tina Kunič, and David Lukanović. 2022. "The Effect of COVID-19 on the Menstrual Cycle: A Systematic Review" Journal of Clinical Medicine 11, no. 13: 3800. https://doi.org/10.3390/jcm11133800
APA StyleLebar, V., Laganà, A. S., Chiantera, V., Kunič, T., & Lukanović, D. (2022). The Effect of COVID-19 on the Menstrual Cycle: A Systematic Review. Journal of Clinical Medicine, 11(13), 3800. https://doi.org/10.3390/jcm11133800







