Positive and Negative Affect Changes during Gender-Affirming Hormonal Treatment: Results from the European Network for the Investigation of Gender Incongruence (ENIGI)
Abstract
1. Introduction
2. Experimental Section
2.1. Study Population
2.2. Gender-Affirming Hormone Therapy
2.3. Other Medication
2.4. Questionnaires
2.4.1. PANAS
2.4.2. Sexual Desire Inventory (SDI)
2.4.3. Psychological Battery Assessed Only at Baseline
2.5. Physical Changes
2.5.1. Ferriman and Gallwey Classification
2.5.2. Side-Effects Questionnaire
2.5.3. Gender-Affirming Surgery
2.6. Laboratory Analyses
2.7. Statistical Analyses
3. Results
3.1. Affect through the Course of Hormone Therapy
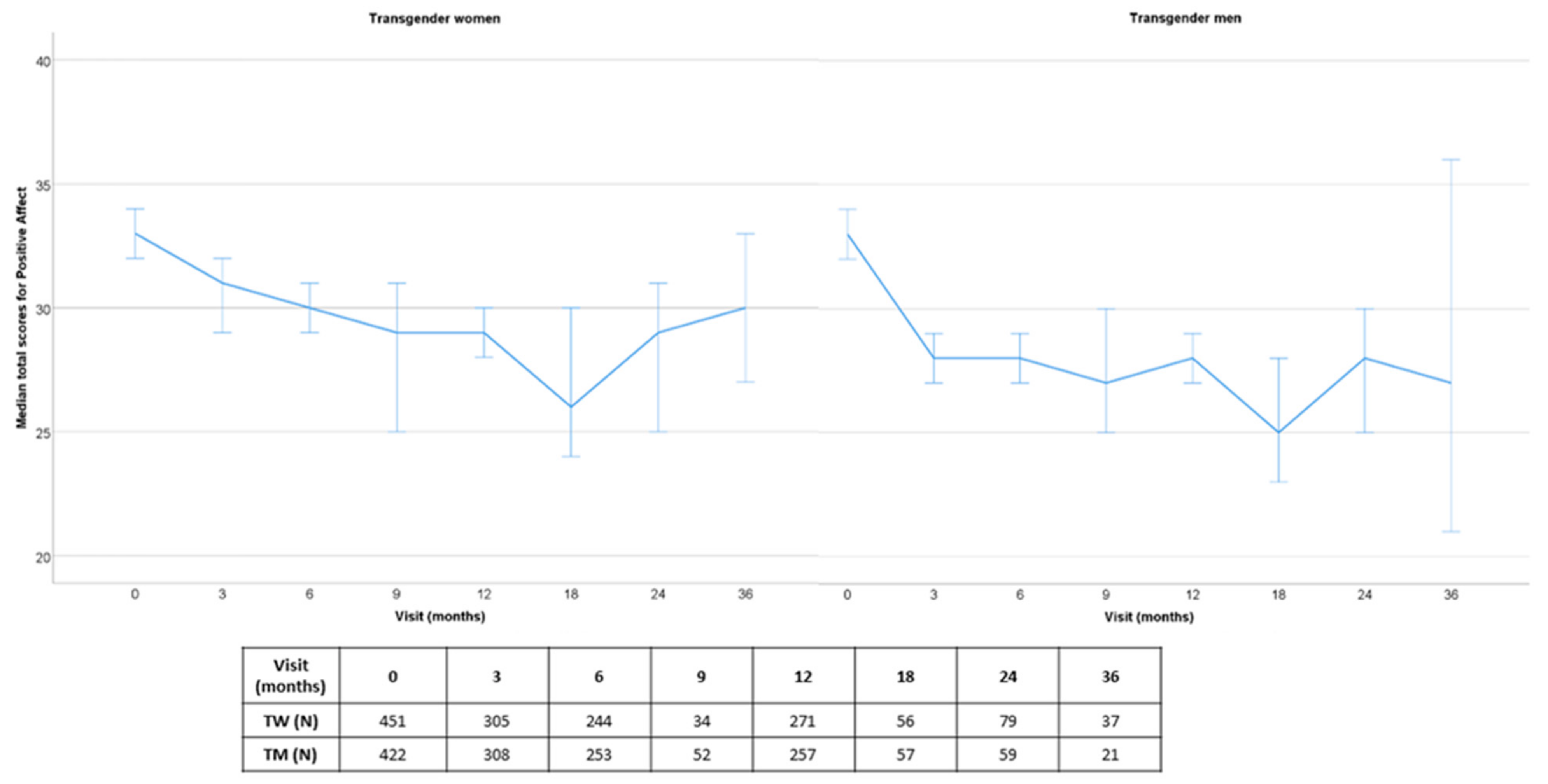
3.1.1. Positive Affect
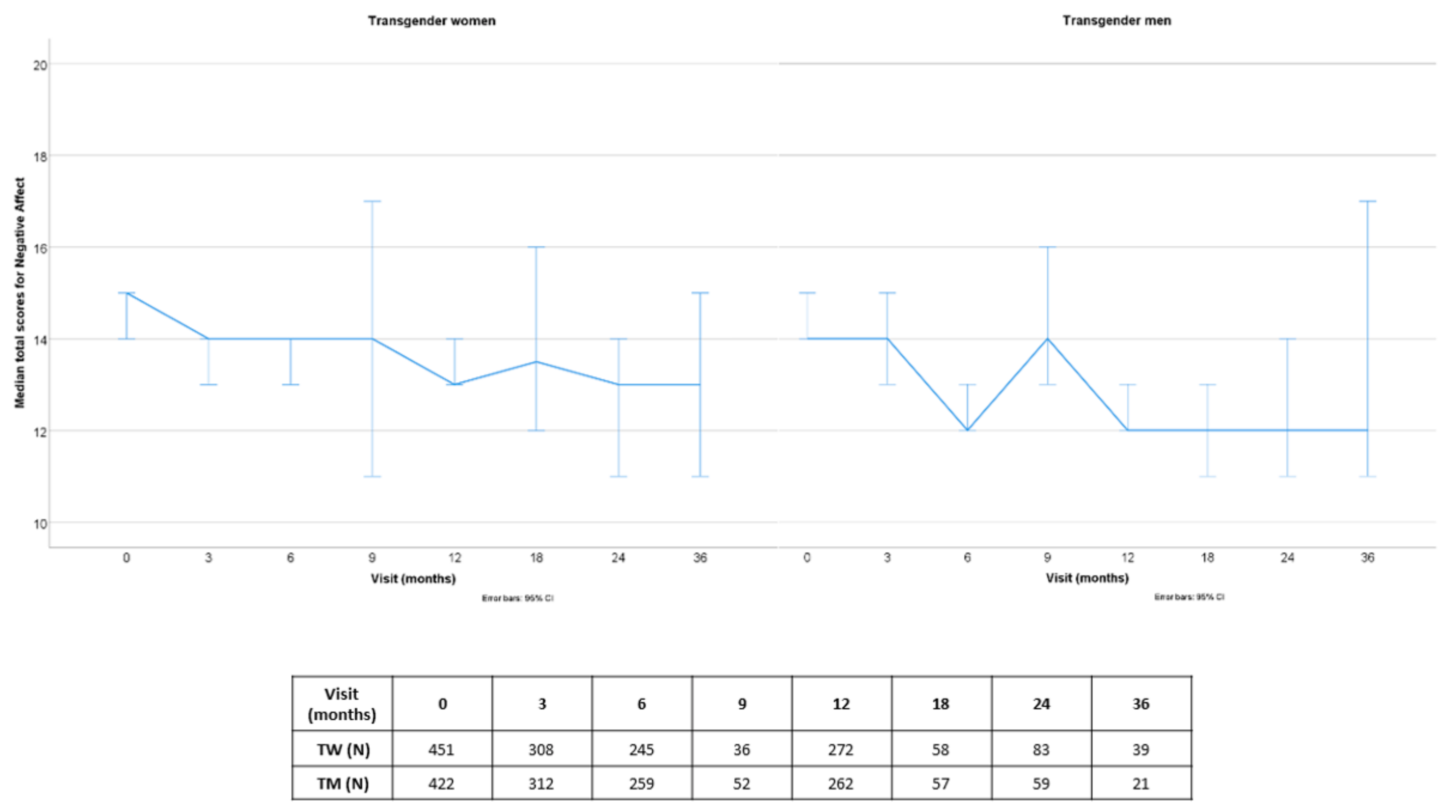
3.1.2. Negative Affect
3.1.3. Subgroup Analysis
3.2. Differential Effect of Feminization versus Masculinization
3.3. Physical Correlates of Affect
3.4. Psychological Correlates of Affect
3.4.1. Cross-Sectional Analyses
3.4.2. Prospective Analyses
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| TW | TM | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| M | Total UGDS | Total QOL | Total Social QOL | Total SCL-90R | Total SDI | Total UGDS | Total QOL | Total Social QOL | Total SCL-90R | Total SDI | ||
| 0 | Total PA | ρ | −0.374 * | −0.360 * | −0.350 * | −0.200 * | 0.12 | −0.145 | −0.14 | −0.14 | −0.116 | 0.194 * |
| p-value | <0.001 | <0.001 | <0.001 | <0.001 | 0.026 | 0.017 | 0.033 | 0.033 | 0.060 | <0.001 | ||
| n | 95 | 253 | 256 | 274 | 375 | 271 | 240 | 239 | 261 | 346 | ||
| Total NA | ρ | 0.044 | 0.260 * | 0.230 * | 0.530 * | 0.200 * | −0.040 | 0.400 * | 0.260 * | 0.422 * | 0.032 | |
| p-value | 0.669 | <0.001 | <0.001 | <0.001 | <0.001 | 0.511 | <0.001 | <0.001 | <0.001 | 0.539 | ||
| n | 96 | 261 | 264 | 283 | 384 | 278 | 250 | 250 | 271 | 362 | ||
| 3 | Total PA | ρ | −0.352 | −0.300 * | −0.330 * | −0.300 * | 0.14 | 0.019 | −0.21 | −0.24 | −0.147 | 0.240 * |
| p-value | 0.099 | <0.001 | <0.001 | <0.001 | 0.033 | 0.794 | 0.007 | 0.002 | 0.043 | <0.001 | ||
| n | 23 | 162 | 164 | 184 | 232 | 193 | 171 | 171 | 191 | 236 | ||
| Total NA | ρ | 0.366 | 0.19 | 0.143 | 0.470 * | 0.240 * | −0.006 | 0.380 * | 0.260 * | 0.455 * | 0.043 | |
| p-value | 0.078 | 0.014 | 0.064 | <0.001 | <0.001 | 0.936 | <0.001 | <0.001 | <0.001 | 0.511 | ||
| n | 24 | 166 | 168 | 189 | 232 | 196 | 174 | 174 | 194 | 239 | ||
| 6 | Total PA | ρ | −0.324 | −0.370 * | −0.290 * | −0.2 | −0.008 | 0.011 | −0.078 | −0.031 | −0.075 | 0.137 |
| p-value | 0.039 | <0.001 | <0.001 | 0.013 | 0.914 | 0.885 | 0.330 | 0.702 | 0.332 | 0.052 | ||
| n | 41 | 152 | 153 | 160 | 194 | 175 | 157 | 160 | 169 | 202 | ||
| Total NA | ρ | −0.138 | 0.122 | 0.118 | 0.440 * | 0.102 | −0.137 | 0.308 * | 0.139 | 0.413 * | 0.062 | |
| p-value | 0.382 | 0.137 | 0.150 | <0.001 | 0.157 | 0.069 | <0.001 | 0.078 | <0.001 | 0.372 | ||
| n | 42 | 150 | 151 | 159 | 194 | 177 | 159 | 162 | 172 | 207 | ||
| 9 | Total PA | ρ | −0.139 | −0.588 | −0.309 | −0.326 | 0.047 | −0.175 | −0.4 | −0.275 | 0.036 | 0.116 |
| p-value | 0.558 | 0.034 | 0.304 | 0.161 | 0.794 | 0.300 | 0.041 | 0.165 | 0.829 | 0.442 | ||
| n | 20 | 13 | 13 | 20 | 33 | 37 | 27 | 27 | 38 | 46 | ||
| Total NA | ρ | −0.115 | −0.030 | 0.083 | 0.409 | 0.001 | 0.063 | 0.137 | 0.277 | 0.434 | 0.247 | |
| p-value | 0.611 | 0.913 | 0.759 | 0.053 | 0.994 | 0.709 | 0.497 | 0.161 | 0.006 | 0.098 | ||
| n | 22 | 16 | 16 | 23 | 34 | 38 | 27 | 27 | 38 | 46 | ||
| 12 | Total PA | ρ | −0.200 | −0.24 | −0.312 * | −0.275 * | 0.228 | −0.102 | −0.128 | −0.132 | −0.091 | 0.174 |
| p-value | 0.095 | 0.003 | <0.001 | <0.001 | 0.001 | 0.175 | 0.113 | 0.099 | 0.232 | 0.014 | ||
| n | 71 | 153 | 156 | 177 | 207 | 179 | 154 | 157 | 173 | 199 | ||
| Total NA | ρ | 0.102 | 0.214 | 0.119 | 0.418 * | 0.101 | 0.097 | 0.247 | 0.113 | 0.384 * | 0.051 | |
| p-value | 0.398 | 0.008 | 0.138 | <0.001 | 0.149 | 0.192 | 0.002 | 0.151 | <0.001 | 0.473 | ||
| n | 71 | 154 | 157 | 178 | 205 | 183 | 160 | 163 | 179 | 202 | ||
| 18 | Total PA | ρ | −0.254 | −0.405 | −0.451 | −0.107 | 0.002 | 0.095 | 0.075 | −0.107 | 0.099 | −0.023 |
| p-value | 0.109 | 0.026 | 0.012 | 0.506 | 0.990 | 0.531 | 0.672 | 0.545 | 0.519 | 0.869 | ||
| n | 41 | 30 | 30 | 41 | 52 | 46 | 34 | 34 | 45 | 56 | ||
| Total NA | ρ | −0.089 | 0.272 | 0.168 | 0.421 | 0.006 | −0.023 | 0.227 | 0.173 | 0.162 | 0.062 | |
| p-value | 0.571 | 0.132 | 0.357 | 0.005 | 0.964 | 0.881 | 0.198 | 0.329 | 0.286 | 0.652 | ||
| n | 43 | 32 | 32 | 43 | 54 | 46 | 34 | 34 | 45 | 56 | ||
| 24 | Total PA | ρ | 0.233 | −0.066 | −0.214 | −0.009 | 0.131 | −0.072 | 0.012 | −0.045 | 0.039 | 0.174 |
| p-value | 0.100 | 0.691 | 0.192 | 0.949 | 0.260 | 0.646 | 0.944 | 0.793 | 0.805 | 0.195 | ||
| n | 51 | 39 | 39 | 49 | 76 | 43 | 37 | 37 | 43 | 57 | ||
| Total NA | ρ | 0.141 | 0.223 | 0.077 | 0.148 | −0.179 | 0.004 | 0.000 | −0.058 | 0.079 | −0.067 | |
| p-value | 0.310 | 0.155 | 0.630 | 0.296 | 0.112 | 0.982 | 0.998 | 0.734 | 0.614 | 0.621 | ||
| n | 54 | 42 | 42 | 52 | 80 | 43 | 37 | 37 | 43 | 57 | ||
| 36 | Total PA | ρ | −0.306 | −0.169 | −0.299 | 0.046 | 0.153 | −0.523 | 0.486 | 0.607 | 0.337 | −0.214 |
| p-value | 0.155 | 0.518 | 0.244 | 0.839 | 0.371 | 0.038 | 0.129 | 0.048 | 0.201 | 0.366 | ||
| n | 23 | 17 | 17 | 22 | 36 | 16 | 11 | 11 | 16 | 20 | ||
| Total NA | ρ | 0.207 | 0.217 | 0.202 | −0.115 | 0.118 | −0.246 | 0.017 | −0.275 | 0.018 | 0.135 | |
| p-value | 0.343 | 0.402 | 0.436 | 0.611 | 0.479 | 0.359 | 0.961 | 0.413 | 0.948 | 0.570 | ||
| n | 23 | 17 | 17 | 22 | 38 | 16 | 11 | 11 | 16 | 20 | ||
References
- American Psychiatric Association DSM-5 Diagnostic Classification. Diagnostic and Statistical Manual of Mental Disorders; American Psychiatric Association Publishing: Washington, DC, USA, 2013. [Google Scholar]
- Defreyne, J.; Kreukels, B.; T’Sjoen, G.; Stahporsius, A.; Den Heijer, M.; Heylens, G.; Elaut, E. No correlation between serum testosterone levels and state-level anger intensity in transgender people: Results from the European Network for the Investigation of Gender Incongruence. Horm. Behav. 2019, 110, 29–39. [Google Scholar] [CrossRef] [PubMed]
- Dekker, M.J.H.J.; Wierckx, K.; Van Caenegem, E.; Klaver, M.; Kreukels, B.P.; Elaut, E.; Fisher, A.D.; van Trotsenburg, M.A.A.; Schreiner, T.; den Heijer, M. A European network for the investigation of gender incongruence: Endocrine part. J. Sex. Med. 2016, 13, 994–999. [Google Scholar] [CrossRef] [PubMed]
- Defreyne, J.; Motmans, J.; T’sjoen, G. Healthcare costs and quality of life outcomes following gender affirming surgery in trans men: A review. Expert Rev. Pharm. Outcomes Res. 2017, 17, 543–556. [Google Scholar] [CrossRef] [PubMed]
- White Hughto, J.M.; Reisner, S.L. A Systematic Review of the Effects of Hormone Therapy on Psychological Functioning and Quality of Life in Transgender Individuals. Transgender Health 2016, 1, 21–31. [Google Scholar] [CrossRef]
- Nobili, A.; Glazebrook, C.; Arcelus, J. Quality of life of treatment-seeking transgender adults: A systematic review and meta-analysis. Rev. Endocr. Metab. Disord. 2018, 19, 199–220. [Google Scholar] [CrossRef]
- Carmel, T.C.; Erickson-Schroth, L. Mental health and the transgender population. J. Psychosoc. Nurs. Ment. Health Serv. 2016, 54, 44–48. [Google Scholar] [CrossRef]
- de Freitas, L.D.; Léda-Rêgo, G.; Bezerra-Filho, S.; Miranda-Scippa, Â. Psychiatric disorders in individuals diagnosed with gender dysphoria: A systematic review. Psychiatry Clin. Neurosci. 2020, 74, 99–104. [Google Scholar] [CrossRef]
- Cohen, J.N.; Taylor Dryman, M.; Morrison, A.S.; Gilbert, K.E.; Heimberg, R.G.; Gruber, J. Positive and Negative Affect as Links Between Social Anxiety and Depression: Predicting Concurrent and Prospective Mood Symptoms in Unipolar and Bipolar Mood Disorders. Behav. Ther. 2017, 48, 820–833. [Google Scholar] [CrossRef]
- Watson, D.; Clark, L.A.; Carey, G. Positive and Negative Affectivity and Their Relation to Anxiety and Depressive Disorders. J. Abnorm. Psychol. 1988, 97, 346–353. [Google Scholar] [CrossRef]
- Cohen, S.; Pressman, S.D. Positive affect and health. Curr. Dir. Psychol. Sci. 2006, 15, 122–125. [Google Scholar] [CrossRef]
- Pressman, S.D.; Cohen, S. Does positive affect influence health? Psychol. Bull. 2005, 131, 925–971. [Google Scholar] [CrossRef] [PubMed]
- Fisher, A.D.; Castellini, G.; Ristori, J.; Casale, H.; Cassioli, E.; Sensi, C.; Fanni, E.; Amato, A.M.L.; Bettini, E.; Mosconi, M.; et al. Cross-sex hormone treatment and psychobiological changes in transsexual persons: Two-year follow-up data. J. Clin. Endocrinol. Metab. 2016, 101, 4260–4269. [Google Scholar] [CrossRef] [PubMed]
- Kreukels, B.P.C.; Haraldsen, I.R.; De Cuypere, G.; Richter-Appelt, H.; Gijs, L.; Cohen-Kettenis, P.T. A European network for the investigation of gender incongruence: The ENIGI initiative. Eur. Psychiatry 2012, 27, 445–450. [Google Scholar] [CrossRef] [PubMed]
- Watson, D.; Clark, L.A.; Tellegen, A. Development and validation of brief measures of positive and negative affect: The PANAS scales. J. Pers. Soc. Psychol. 1988, 54, 1063. [Google Scholar] [CrossRef] [PubMed]
- Coleman, E.; Bockting, W.; Botzer, M.; Cohen-Kettenis, P.; De Cuypere, G.; Feldman, J.; Zucker, K. Standards of Care for the health of transsexual, transgender, and gender-nonconforming people. Int. J. Transgenderism 2012, 13, 165–232. [Google Scholar] [CrossRef]
- Engelen, U.; De Peuter, S.; Victoir, A.; Van Diest, I.; Van den Bergh, O. Verdere validering van de Positive and Negative Affect Schedule (PANAS) en vergelijking van twee Nederlandstalige versies. Gedrag Gezondh. 2006, 34, 61–70. [Google Scholar]
- Spector, I.P.; Carey, M.P.; Steinberg, L. The sexual desire inventory: Development, factor structure, and evidence of reliability. J. Sex Marital Ther. 1996, 175–190. [Google Scholar] [CrossRef]
- Defreyne, J.; Elaut, E.; Kreukels, B.; Fisher, A.D.; Castellini, G.; Staphorsius, A.; Den Heijer, M.; Heylens, G.; T’Sjoen, G. Sexual Desire Changes in Transgender Individuals Upon Initiation of Hormone Treatment: Results from the Longitudinal European Network for the Investigation of Gender Incongruence. J. Sex. Med. 2020, 17, 812–825. [Google Scholar] [CrossRef]
- Cohen-Kettenis, P.T.; van Goozen, S.H. Sex reassignment of adolescent transsexuals: A follow-up study. J. Am. Acad. Child Adolesc. Psychiatry 1997, 36, 263–271. [Google Scholar] [CrossRef]
- Arrindell, W.A.; Ettema, J.H.M. Symptom Checklist SCL-90: Handleiding Bij een Multidimensionele Psychopathologie-Indicator; Swets test Publishers: Lisse, The Netherlands, 2003. [Google Scholar]
- Bradburn, N.M. The Structure of Psychological Well-Being; Aldine: Chicago, IL, USA, 1969. [Google Scholar]
- Ferriman, D.; Gallwey, J.D. Clinical assessment of body hair growth in women. J. Clin. Endocrinol. Metab. 1961, 21, 1440–1447. [Google Scholar] [CrossRef]
- Wiepjes, C.M.; Vlot, M.C.; Klaver, M.; Nota, N.M.; de Blok, C.J.M.; de Jongh, R.T.; Lips, P.; Heijboer, A.C.; Fisher, A.D.; Schreiner, T. Bone Mineral Density Increases in Trans Persons After 1 Year of Hormonal Treatment: A Multicenter Prospective Observational Study. J. Bone Min. Res. 2017, 32, 1252–1260. [Google Scholar] [CrossRef] [PubMed]
- Holm, S. A simple sequentially rejective multiple test procedure. Scand. J. Stat. 1979, 6, 65–70. [Google Scholar]
- Hembree, W.C.; Cohen-Kettenis, P.; Delemarre-Van De Waal, H.A.; Gooren, L.J.; Meyer, W.J.; Spack, N.P.; Tangpricha, V.; Montori, V.M. Endocrine treatment of transsexual persons: An endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 2009, 94, 3132–3154. [Google Scholar] [CrossRef] [PubMed]
- Hengartner, M.P.; Kruger, T.H.C.; Geraedts, K.; Tronci, E.; Mancini, T.; Ille, F.; Egli, M.; Röblitz, S.; Ehrig, R.; Saleh, L.; et al. Negative affect is unrelated to fluctuations in hormone levels across the menstrual cycle: Evidence from a multisite observational study across two successive cycles. J. Psychosom. Res. 2017, 99, 21–27. [Google Scholar] [CrossRef]
- Zarrouf, F.A.; Artz, S.; Griffith, J.; Sirbu, C.; Kommor, M. Testosterone and depression: Systematic review and meta-analysis. J. Psychiatr. Pract. 2009, 15, 289–305. [Google Scholar] [CrossRef]
- Wierckx, K.; Elaut, E.; Van Hoorde, B.; Heylens, G.; De Cuypere, G.; Monstrey, S.; Weyers, S.; Hoebeke, P.; T’Sjoen, G. Sexual Desire in Trans Persons: Associations with Sex Reassignment Treatment. J. Sex. Med. 2014, 11, 107–118. [Google Scholar] [CrossRef]
- Bouman, W.P.; Davey, A.; Meyer, C.; Witcomb, G.L.; Arcelus, J. Predictors of psychological well-being among treatment seeking transgender individuals. Sex. Relatsh. Ther. 2016, 31, 359–375. [Google Scholar] [CrossRef]
| TW (n = 451) | TM (n = 422) | |||
|---|---|---|---|---|
| Age (years) | 27.0 [22.0–41.0] | 22.0 [20.0–28.0] | ||
| Baseline PA scores | 32.5 [27.0–37.0] | 33.0 [27.0–38.0] | ||
| Baseline NA scores | 14.0 [12.0–19.0] | 14.0 [12.0–19.0] | ||
| Gender-affirming hormonal therapy | Testosterone (60 missing) | AG 25 mg once daily | 18 (5.0%) | |
| AG 50 mg once daily | 106 (29.3%) | |||
| TU 1 g once every 12 weeks | 121 (33.4%) | |||
| TE once every 2 weeks | 112 (30.9%) | |||
| TE once every 3 weeks | 4 (1.1%) | |||
| Anti-androgens | CPA 50 | 451 (100%) | ||
| Estrogens (76 missing) | Gel | 4 (1.1%) | ||
| EV | 219 (58.4%) | |||
| Patch 100 mcg/72 h | 108 (39.2%) | |||
| Patch 50 mcg/72 h | 12 (4.4%) | |||
| Patch 75 mcg/72 h | 2 (0.7%) | |||
| Number of TM reporting menstruation (%) (184 missing) | 39 (16.4%) | |||
| Number of TM reporting spotting (%) (180 missing) | 31 (12.8%) | |||
| Number of TM using contraceptives (%) | 72 (15.9%) | |||
| Median Ferriman and Gallwey score | 1.0 [0.0–3.0] | |||
| Serum estradiol levels (pg/mL) | 25.3 [21.1–30.1] | 36.9 [22.5–76.8] | ||
| Serum testosterone levels (nmol/L) | 18.5 [14.0–23.3] | 1.2 [0.9–1.6] | ||
| Serum LH levels (U/L) | 3.9 [2.7–5.3] | 4.5 [2.4–7.7] | ||
| Serum FSH levels (U/L) | 3.5 [2.3–4.9] | 5.6 [3.3–7.2] | ||
| Serum SHBG levels (ng/dL) | 54.7 [35.0–81.0] | 36.8 [26.7–51.3] | ||
| Median Utrecht Gender Dysphoria (UGDS) scores | 22.0 [16.0–47.0] | 29.0 [28.0–32.0] | ||
| Median quality of life (QOL) scores | Total | 8.0 [7.0–9.0] | 8.0 [7.0–9.0] | |
| Social | 30.0 [26.0–33.0] | 30.0 [26.0–34.0] | ||
| Median total SCL-90-R, Symptom Checklist scores (SCL-90R) | 23.0 [8.0–47.3] | 23.0 [10.0–54.0] | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Matthys, I.; Defreyne, J.; Elaut, E.; Fisher, A.D.; Kreukels, B.P.C.; Staphorsius, A.; Den Heijer, M.; T’Sjoen, G. Positive and Negative Affect Changes during Gender-Affirming Hormonal Treatment: Results from the European Network for the Investigation of Gender Incongruence (ENIGI). J. Clin. Med. 2021, 10, 296. https://doi.org/10.3390/jcm10020296
Matthys I, Defreyne J, Elaut E, Fisher AD, Kreukels BPC, Staphorsius A, Den Heijer M, T’Sjoen G. Positive and Negative Affect Changes during Gender-Affirming Hormonal Treatment: Results from the European Network for the Investigation of Gender Incongruence (ENIGI). Journal of Clinical Medicine. 2021; 10(2):296. https://doi.org/10.3390/jcm10020296
Chicago/Turabian StyleMatthys, Imke, Justine Defreyne, Els Elaut, Alessandra Daphne Fisher, Baudewijntje P. C. Kreukels, Annemieke Staphorsius, Martin Den Heijer, and Guy T’Sjoen. 2021. "Positive and Negative Affect Changes during Gender-Affirming Hormonal Treatment: Results from the European Network for the Investigation of Gender Incongruence (ENIGI)" Journal of Clinical Medicine 10, no. 2: 296. https://doi.org/10.3390/jcm10020296
APA StyleMatthys, I., Defreyne, J., Elaut, E., Fisher, A. D., Kreukels, B. P. C., Staphorsius, A., Den Heijer, M., & T’Sjoen, G. (2021). Positive and Negative Affect Changes during Gender-Affirming Hormonal Treatment: Results from the European Network for the Investigation of Gender Incongruence (ENIGI). Journal of Clinical Medicine, 10(2), 296. https://doi.org/10.3390/jcm10020296





