Hypogonadism in Adult Males with Prader-Willi Syndrome—Clinical Recommendations Based on a Dutch Cohort Study, Review of the Literature and an International Expert Panel Discussion
Abstract
1. Introduction
2. Materials and Methods
2.1. Literature Search
2.2. Expert Opinion
2.3. Data Analysis
3. Results
3.1. Baseline Characteristics
3.2. Hypogonadism
3.3. Effect of Untreated Hypogonadism
3.4. Types of Hypogonadism
3.5. Literature Review
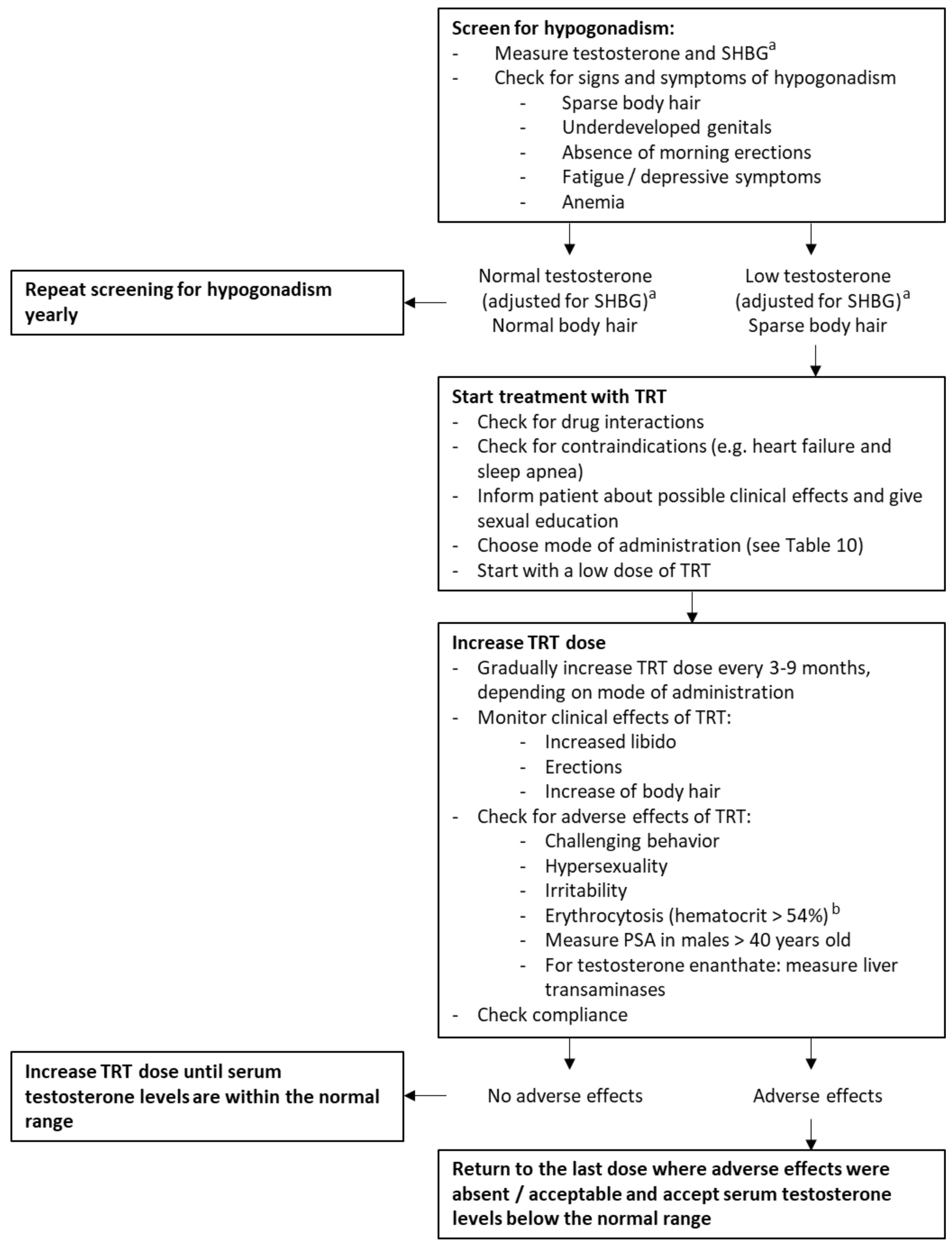
3.6. Expert Panel and Clinical Recommendations
4. Discussion
4.1. Type of Hypogonadism
4.2. Undertreatment
4.3. Importance of Treatment of Hypogonadism
4.3.1. Osteoporosis
4.3.2. Muscle and Fat
4.3.3. Fatigue
4.3.4. Cardiovascular Health
4.4. TRT Warnings and Precautions
4.5. Recommendations
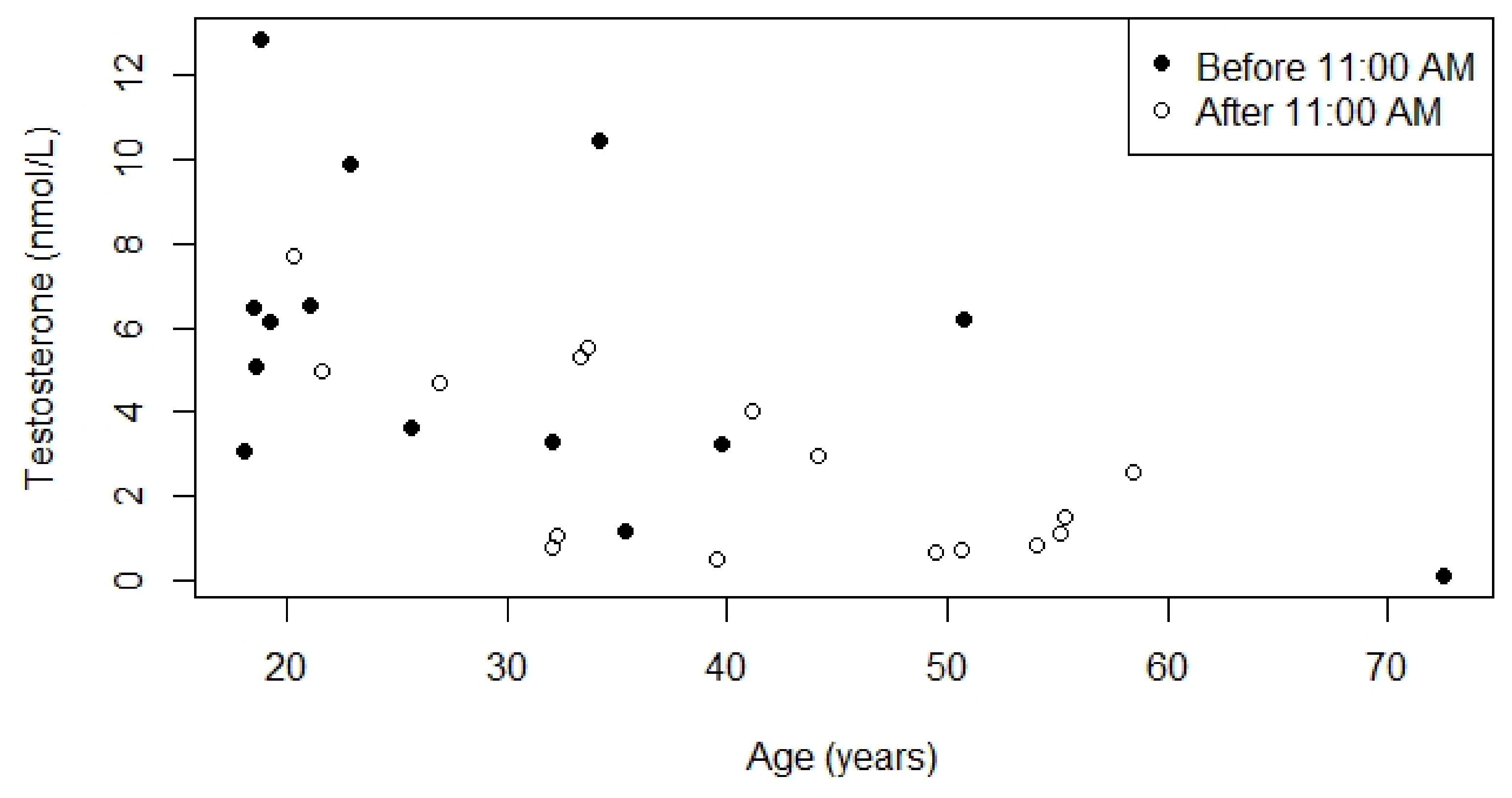
4.5.1. Interpretation of Hormone Levels
4.5.2. Sleep Apnea
4.5.3. Drug Interactions
4.5.4. Cardiac Failure
4.5.5. Challenging Behavior
4.5.6. Mode of Administration
4.5.7. Erythrocytosis
4.5.8. Prostate and Liver
4.5.9. Non-Compliance
4.6. Role of PWS Reference Centers
4.7. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Cheon, C.K. Genetics of Prader-Willi syndrome and Prader-Will-Like syndrome. Ann. Pediatr. Endocrinol. Metab. 2016, 21, 126–135. [Google Scholar] [CrossRef]
- Butler, M.G.; Hartin, S.N.; Hossain, W.A.; Manzardo, A.M.; Kimonis, V.; Dykens, E.; Gold, J.A.; Kim, S.J.; Weisensel, N.; Tamura, R.; et al. Molecular genetic classification in Prader-Willi syndrome: A multisite cohort study. J. Med. Genet. 2019, 56, 149–153. [Google Scholar] [CrossRef] [PubMed]
- Angulo, M.A.; Butler, M.G.; Cataletto, M.E. Prader-Willi syndrome: A review of clinical, genetic, and endocrine findings. J. Endocrinol. Investig. 2015, 38, 1249–1263. [Google Scholar] [CrossRef]
- Goldstone, A.P.; Holland, A.J.; Hauffa, B.P.; Hokken-Koelega, A.C.; Tauber, M.; Speakers Contributors at the Second Expert Meeting of the Comprehensive Care of Patients with PWS. Recommendations for the diagnosis and management of Prader-Willi syndrome. J. Clin. Endocrinol. Metab. 2008, 93, 4183–4197. [Google Scholar] [CrossRef]
- Cassidy, S.B. Prader-Willi syndrome. J. Med. Genet. 1997, 34, 917–923. [Google Scholar] [CrossRef]
- Holm, V.A.; Cassidy, S.B.; Butler, M.G.; Hanchett, J.M.; Greenswag, L.R.; Whitman, B.Y.; Greenberg, F. Prader-Willi syndrome: Consensus diagnostic criteria. Pediatrics 1993, 91, 398–402. [Google Scholar]
- Cassidy, S.B.; Schwartz, S.; Miller, J.L.; Driscoll, D.J. Prader-Willi syndrome. Gen. Med. 2012, 14, 10–26. [Google Scholar] [CrossRef]
- Partsch, C.A.; Lämmer, C.; Gillessen-Kaesbach, G.; Pankau, R. Adult patients with Prader-Willi syndrome: Clinical characteristics, life circumstances and growth hormone secretion. Growth Horm. IGF Res. 2000, 10, S81–S85. [Google Scholar] [CrossRef]
- Whittington, J.; Holland, A.; Webb, T.; Butler, J.; Clarke, D.; Boer, H. Relationship between clinical and genetic diagnosis of Prader-Willi syndrome. J. Med. Genet. 2002, 39, 926–932. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Grugni, G.; Morabito, F.; Crinò, A. Gonadal function and its disorders in simple obesity and in Prader-Willi syndrome. In Prader-Willi Syndrome as a Model for Obesity; Eiholzer, U., l’Allemad, D., Zipf, W., Eds.; Karger: Basel, Switzerland, 2003; pp. 140–155. [Google Scholar] [CrossRef]
- Höybye, C.; Thorén, M.; Böhm, B. Cognitive, emotional, physical and social effects of growth hormone treatment in adults with Prader-Willi syndrome. J. Intellect. Disabil. Res. 2005, 49, 245–252. [Google Scholar] [CrossRef] [PubMed]
- Miller, J.L.; Goldstone, A.P.; Couch, J.A.; Shuster, J.; He, G.; Driscoll, D.J.; Liu, Y.; Schmalfuss, I.M. Pituitary abnormalities in Prader-Willi syndrome and early onset morbid obesity. Am. J. Med. Genet. A 2008, 146A, 570–577. [Google Scholar] [CrossRef]
- Brandau, D.T.; Theodoro, M.; Garg, U.; Butler, M.G. Follicle stimulating and leutinizing hormones, estradiol and testosterone in Prader-Willi syndrome. Am. J. Med. Genet. A 2008, 146A, 665–669. [Google Scholar] [CrossRef]
- Sode-Carlsen, R.; Farholt, S.; Rabben, K.F.; Bollerslev, J.; Schreiner, T.; Jurik, A.G.; Christiansen, J.S.; Höybye, C. Body composition, endocrine and metabolic profiles in adults with Prader-Willi syndrome. Growth Horm. IGF Res. 2010, 20, 179–184. [Google Scholar] [CrossRef] [PubMed]
- Van Nieuwpoort, I.C.; Sinnema, M.; Castelijns, J.A.; Twisk, J.W.; Curfs, L.M.; Drent, M.L. The GH/IGF-I axis and pituitary function and size in adults with Prader-Willi syndrome. Horm. Res. Paediatr. 2011, 75, 403–411. [Google Scholar] [CrossRef] [PubMed]
- Radicioni, A.F.; Di Giorgio, G.; Grugni, G.; Cuttini, M.; Losacco, V.; Anzuini, A.; Spera, S.; Marzano, C.; Lenzi, A.; Cappa, M.; et al. Multiple forms of hypogonadism of central, peripheral or combined origin in males with Prader-Willi syndrome. Clin. Endocrinol. 2012, 76, 72–77. [Google Scholar] [CrossRef] [PubMed]
- Kido, Y.; Sakazume, S.; Abe, Y.; Oto, Y.; Itabashi, H.; Shiraishi, M.; Yoshino, A.; Tanaka, Y.; Obata, K.; Murakami, N.; et al. Testosterone replacement therapy to improve secondary sexual characteristics and body composition without adverse behavioral problems in adult male patients with Prader-Willi syndrome: An observational study. Am. J. Med. Genet. A 2013, 161A, 2167–2173. [Google Scholar] [CrossRef]
- Hirsch, H.J.; Eldar-Geva, T.; Bennaroch, F.; Pollak, Y.; Gross-Tsur, V. Sexual dichotomy of gonadal function in Prader-Willi syndrome from early infancy through the fourth decade. Hum. Reprod. 2015, 30, 2587–2596. [Google Scholar] [CrossRef]
- Coupaye, M.; Tauber, M.; Cuisset, L.; Laurier, V.; Bieth, E.; Lacorte, J.M.; Oppert, J.M.; Clement, K.; Poitou, C. Effect of Genotype and Previous GH Treatment on Adiposity in Adults With Prader-Willi Syndrome. J. Clin. Endocrinol. Metab. 2016, 101, 4895–4903. [Google Scholar] [CrossRef] [PubMed]
- Matsuyama, S.; Matsui, F.; Matsuoka, K.; Iijima, M.; Takeuchi, M.; Ida, S.; Matsumoto, F.; Mizokami, A. Gonadal function and testicular histology in males with Prader-Willi syndrome. Endocrinol. Diabetes Metab. 2019, 2, e00049. [Google Scholar] [CrossRef]
- Heksch, R.; Kamboj, M.; Anglin, K.; Obrynba, K. Review of Prader-Willi syndrome: The endocrine approach. Transl. Pediatr. 2017, 6, 274–285. [Google Scholar] [CrossRef] [PubMed]
- Eiholzer, U.; l’Allemand, D.; Rousson, V.; Schlumpf, M.; Gasser, T.; Girard, J.; Grüters, A.; Simoni, M. Hypothalamic and gonadal components of hypogonadism in boys with Prader-Labhart- Willi syndrome. J. Clin. Endocrinol. Metab. 2006, 91, 892–898. [Google Scholar] [CrossRef]
- Hirsch, H.J.; Eldar-Geva, T.; Benarroch, F.; Rubinstein, O.; Gross-Tsur, V. Primary testicular dysfunction is a major contributor to abnormal pubertal development in males with Prader-Willi syndrome. J. Clin. Endocrinol. Metab. 2009, 94, 2262–2268. [Google Scholar] [CrossRef] [PubMed]
- Muscogiuri, G.; Formoso, G.; Pugliese, G.; Ruggeri, R.M.; Scarano, E.; Colao, A.; Restare. Prader- Willi syndrome: An uptodate on endocrine and metabolic complications. Rev. Endocr. Metab. Disord. 2019, 20, 239–250. [Google Scholar] [CrossRef] [PubMed]
- Linnemann, K.; Schroder, C.; Mix, M.; Kruger, G.; Fusch, C. Prader-Labhart-Willi syndrome with central precocious puberty and empty sella syndrome. Acta Paediatr. 1999, 88, 1295–1297. [Google Scholar] [CrossRef]
- Crinò, A.; Schiaffini, R.; Ciampalini, P.; Spera, S.; Beccaria, L.; Benzi, F.; Bosio, L.; Corrias, A.; Gargantini, L.; Salvatoni, A.; et al. Hypogonadism and pubertal development in Prader-Willi syndrome. Eur. J. Pediatr. 2003, 162, 327–333. [Google Scholar] [CrossRef]
- Siemensma, E.P.; de Lind van Wijngaarden, R.F.; Otten, B.J.; de Jong, F.H.; Hokken-Koelega, A.C. Pubarche and serum dehydroepiandrosterone sulphate levels in children with Prader-Willi syndrome. Clin. Endocrinol. 2011, 75, 83–89. [Google Scholar] [CrossRef] [PubMed]
- Laurance, B.M.; Brito, A.; Wilkinson, J. Prader-Willi Syndrome after age 15 years. Arch. Dis. Child. 1981, 56, 181–186. [Google Scholar] [CrossRef]
- Marzullo, P.; Marcassa, C.; Campini, R.; Eleuteri, E.; Minocci, A.; Priano, L.; Temporelli, P.; Sartorio, A.; Vettor, R.; Liuzzi, A.; et al. The impact of growth hormone/insulin-like growth factor-I axis and nocturnal breathing disorders on cardiovascular features of adult patients with Prader-Willi syndrome. J. Clin. Endocrinol. Metab. 2005, 90, 5639–5646. [Google Scholar] [CrossRef] [PubMed]
- Hoybye, C.; Hilding, A.; Jacobsson, H.; Thoren, M. Metabolic profile and body composition in adults with Prader-Willi syndrome and severe obesity. J. Clin. Endocrinol. Metab. 2002, 87, 3590–3597. [Google Scholar] [CrossRef] [PubMed]
- Richard-Eaglin, A. Male and Female Hypogonadism. Nurs. Clin. North. Am. 2018, 53, 395–405. [Google Scholar] [CrossRef]
- Kloner, R.A.; Carson, C., 3rd; Dobs, A.; Kopecky, S.; Mohler, E.R., 3rd. Testosterone and Cardiovascular Disease. J. Am. Coll. Cardiol. 2016, 67, 545–557. [Google Scholar] [CrossRef]
- Molina-Vega, M.; Muñoz-Garach, A.; Damas-Fuentes, M.; Fernández-García, J.C.; Tinahones, F.J. Secondary male hypogonadism: A prevalent but overlooked comorbidity of obesity. Asian J. Androl. 2018, 20, 531–538. [Google Scholar] [CrossRef]
- Boese, A.C.; Kim, S.C.; Yin, K.J.; Lee, J.P.; Hamblin, M.H. Sex differences in vascular physiology and pathophysiology: Estrogen and androgen signaling in health and disease. Am. J. Physiol. Heart Circ. Physiol. 2017, 313, H524–H545. [Google Scholar] [CrossRef] [PubMed]
- Noordam, C.; Höybye, C.; Eiholzer, U. Prader-Willi Syndrome and Hypogonadism: A Review Article. Int. J. Mol. Sci. 2021, 22, 2705. [Google Scholar] [CrossRef] [PubMed]
- Pellikaan, K.; Rosenberg, A.G.W.; Kattentidt-Mouravieva, A.A.; Kersseboom, R.; Bos-Roubos, A.G.; Veen-Roelofs, J.M.C.; van Wieringen, N.; Hoekstra, F.M.E.; van den Berg, S.A.A.; van der Lely, A.J.; et al. Missed Diagnoses and Health Problems in Adults With Prader-Willi Syndrome: Recommendations for Screening and Treatment. J. Clin. Endocrinol. Metab. 2020, 105, e4671–e4687. [Google Scholar] [CrossRef]
- Crawford, E.D.; Poage, W.; Nyhuis, A.; Price, D.A.; Dowsett, S.A.; Gelwicks, S.; Muram, D. Measurement of testosterone: How important is a morning blood draw? Curr. Med. Res. Opin. 2015, 31, 1911–1914. [Google Scholar] [CrossRef] [PubMed]
- Bhasin, S.; Brito, J.P.; Cunningham, G.R.; Hayes, F.J.; Hodis, H.N.; Matsumoto, A.M.; Snyder, P.J.; Swerdloff, R.S.; Wu, F.C.; Yialamas, M.A. Testosterone Therapy in Men With Hypogonadism: An Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 2018, 103, 1715–1744. [Google Scholar] [CrossRef]
- Napolitano, L.; Barone, B.; Morra, S.; Celentano, G.; La Rocca, R.; Capece, M.; Morgera, V.; Turco, C.; Caputo, V.F.; Spena, G.; et al. Hypogonadism in Patients with Prader Willi Syndrome: A Narrative Review. Int. J. Mol. Sci. 2021, 22, 1993. [Google Scholar] [CrossRef] [PubMed]
- Vogels, A.; Moerman, P.; Frijns, J.P.; Bogaert, G.A. Testicular histology in boys with Prader-Willi syndrome: Fertile or infertile? J. Urol. 2008, 180, 1800–1804. [Google Scholar] [CrossRef]
- Katcher, M.L.; Bargman, G.J.; Gilbert, E.F.; Opitz, J.M. Absence of spermatogonia in the Prader-Willi syndrome. Eur. J. Pediatr. 1977, 124, 257–260. [Google Scholar] [CrossRef] [PubMed]
- Färber, C.; Gross, S.; Neesen, J.; Buiting, K.; Horsthemke, B. Identification of a testis-specific gene (C15orf2) in the Prader-Willi syndrome region on chromosome 15. Genomics 2000, 65, 174–183. [Google Scholar] [CrossRef] [PubMed]
- Snyder, P.J.; Peachey, H.; Berlin, J.A.; Hannoush, P.; Haddad, G.; Dlewati, A.; Santanna, J.; Loh, L.; Lenrow, D.A.; Holmes, J.H.; et al. Effects of testosterone replacement in hypogonadal men. J. Clin. Endocrinol. Metab. 2000, 85, 2670–2677. [Google Scholar] [CrossRef] [PubMed]
- Donze, S.H.; Kuppens, R.J.; Bakker, N.E.; van Alfen-van der Velden, J.; Hokken-Koelega, A.C.S. Bone mineral density in young adults with Prader-Willi syndrome: A randomized, placebo-controlled, crossover GH trial. Clin. Endocrinol. 2018, 88, 806–812. [Google Scholar] [CrossRef] [PubMed]
- Bhasin, S.; Woodhouse, L.; Casaburi, R.; Singh, A.B.; Bhasin, D.; Berman, N.; Chen, X.; Yarasheski, K.E.; Magliano, L.; Dzekov, C.; et al. Testosterone dose-response relationships in healthy young men. Am. J. Physiol. Endocrinol. Metab. 2001, 281, E1172–E1181. [Google Scholar] [CrossRef]
- Grugni, G.; Marzullo, P. Diagnosis and treatment of GH deficiency in Prader-Willi syndrome. Best Pract. Res. Clin. Endocrinol. Metab. 2016, 30, 785–794. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Cunningham, G.; Dobs, A.; Iranmanesh, A.; Matsumoto, A.M.; Snyder, P.J.; Weber, T.; Berman, N.; Hull, L.; Swerdloff, R.S. Long-term testosterone gel (AndroGel) treatment maintains beneficial effects on sexual function and mood, lean and fat mass, and bone mineral density in hypogonadal men. J. Clin. Endocrinol. Metab. 2004, 89, 2085–2098. [Google Scholar] [CrossRef]
- Wagner, G.J.; Rabkin, J.G.; Rabkin, R. Testosterone as a treatment for fatigue in HIV+ men. Gen. Hosp. Psychiatry 1998, 20, 209–213. [Google Scholar] [CrossRef]
- Pexman-Fieth, C.; Behre, H.M.; Morales, A.; Kan-Dobrosky, N.; Miller, M.G. A 6-month observational study of energy, sexual desire, and body proportions in hypogonadal men treated with a testosterone 1% gel. Aging Male 2014, 17. [Google Scholar] [CrossRef]
- Petering, R.C.; Brooks, N.A. Testosterone Therapy: Review of Clinical Applications. Am. Fam. Physician 2017, 96, 441–449. [Google Scholar]
- Butler, M.G.; Manzardo, A.M.; Heinemann, J.; Loker, C.; Loker, J. Causes of death in Prader-Willi syndrome: Prader-Willi Syndrome Association (USA) 40-year mortality survey. Genet. Med. 2017, 19, 635–642. [Google Scholar] [CrossRef]
- Pacoricona Alfaro, D.L.; Lemoine, P.; Ehlinger, V.; Molinas, C.; Diene, G.; Valette, M.; Pinto, G.; Coupaye, M.; Poitou-Bernert, C.; Thuilleaux, D.; et al. Causes of death in Prader-Willi syndrome: Lessons from 11 years’ experience of a national reference center. Orphanet J. Rare Dis. 2019, 14, 238. [Google Scholar] [CrossRef]
- Diaconu, R.; Donoiu, I.; Mirea, O.; Bălşeanu, T.A. Testosterone, cardiomyopathies, and heart failure: A narrative review. Asian J. Androl. 2021, 23, 348–356. [Google Scholar] [CrossRef]
- Cittadini, A.; Isidori, A.M.; Salzano, A. Testosterone therapy and cardiovascular diseases. Cardiovasc. Res. 2021. [Google Scholar] [CrossRef]
- Cooper, L.A.; Page, S.T.; Amory, J.K.; Anawalt, B.D.; Matsumoto, A.M. The association of obesity with sex hormone-binding globulin is stronger than the association with ageing—Implications for the interpretation of total testosterone measurements. Clin. Endocrinol. 2015, 83, 828–833. [Google Scholar] [CrossRef]
- Richards, A.; Quaghebeur, G.; Clift, S.; Holland, A.; Dahlitz, M.; Parkes, D. The upper airway and sleep apnoea in the Prader-Willi syndrome. Clin. Otolaryngol. Allied Sci. 1994, 19, 193–197. [Google Scholar] [CrossRef] [PubMed]
- Proffitt, J.; Osann, K.; McManus, B.; Kimonis, V.E.; Heinemann, J.; Butler, M.G.; Stevenson, D.A.; Gold, J.A. Contributing factors of mortality in Prader-Willi syndrome. Am. J. Med. Genet. A 2019, 179, 196–205. [Google Scholar] [CrossRef] [PubMed]
- Paragliola, R.M.; Prete, A.; Kaplan, P.W.; Corsello, S.M.; Salvatori, R. Treatment of hypopituitarism in patients receiving antiepileptic drugs. Lancet Diabetes Endocrinol. 2015, 3, 132–140. [Google Scholar] [CrossRef]
- Hansen, C.H.; Larsen, L.W.; Sørensen, A.M.; Halling-Sørensen, B.; Styrishave, B. The six most widely used selective serotonin reuptake inhibitors decrease androgens and increase estrogens in the H295R cell line. Toxicol. In Vitro 2017, 41, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Svalheim, S.; Sveberg, L.; Mochol, M.; Taubøll, E. Interactions between antiepileptic drugs and hormones. Seizure 2015, 28, 12–17. [Google Scholar] [CrossRef]
- Daniel, W.A. The influence of long-term treatment with psychotropic drugs on cytochrome P450: The involvement of different mechanisms. Expert Opin. Drug Metab. Toxicol. 2005, 1, 203–217. [Google Scholar] [CrossRef]
- Drobnis, E.Z.; Nangia, A.K. Psychotropics and Male Reproduction. Adv. Exp. Med. Biol. 2017, 1034, 63–101. [Google Scholar] [CrossRef] [PubMed]
- Pavlidi, P.; Kokras, N.; Dalla, C. Antidepressants’ effects on testosterone and estrogens: What do we know? Eur. J. Pharmacol. 2021, 899, 173998. [Google Scholar] [CrossRef] [PubMed]
- Veldhuis, J.D.; Frystyk, J.; Iranmanesh, A.; Orskov, H. Testosterone and estradiol regulate free insulin-like growth factor I (IGF-I), IGF binding protein 1 (IGFBP-1), and dimeric IGF-I/IGFBP-1 concentrations. J. Clin. Endocrinol. Metab. 2005, 90, 2941–2947. [Google Scholar] [CrossRef]
- Gibney, J.; Wolthers, T.; Johannsson, G.; Umpleby, A.M.; Ho, K.K. Growth hormone and testosterone interact positively to enhance protein and energy metabolism in hypopituitary men. Am. J. Physiol. Endocrinol. Metab. 2005, 289, E266–E271. [Google Scholar] [CrossRef]
- Kenyon, A.; Knowlton, K.; Sandiford, I.; Koch, F.C.; Lotwin, G. A comparative study of the metabolic effects of testosterone propionate in normal men and women and in eunuchoidism1,2. Endocrinology 1940, 26, 26–45. [Google Scholar] [CrossRef]
- Sinnema, M.; Maaskant, M.A.; van Schrojenstein Lantman-de Valk, H.M.; van Nieuwpoort, I.C.; Drent, M.L.; Curfs, L.M.; Schrander-Stumpel, C.T. Physical health problems in adults with Prader-Willi syndrome. Am. J. Med. Genet. A 2011, 155A, 2112–2124. [Google Scholar] [CrossRef]
- Krauser, D.G.; Lloyd-Jones, D.M.; Chae, C.U.; Cameron, R.; Anwaruddin, S.; Baggish, A.L.; Chen, A.; Tung, R.; Januzzi, J.L., Jr. Effect of body mass index on natriuretic peptide levels in patients with acute congestive heart failure: A ProBNP Investigation of Dyspnea in the Emergency Department (PRIDE) substudy. Am. Heart J. 2005, 149, 744–750. [Google Scholar] [CrossRef]
- Abadilla, K.A.; Dobs, A.S. Topical testosterone supplementation for the treatment of male hypogonadism. Drugs 2012, 72, 1591–1603. [Google Scholar] [CrossRef]
- Swerdloff, R.S.; Wang, C.; Cunningham, G.; Dobs, A.; Iranmanesh, A.; Matsumoto, A.M.; Snyder, P.J.; Weber, T.; Longstreth, J.; Berman, N. Long-term pharmacokinetics of transdermal testosterone gel in hypogonadal men. J. Clin. Endocrinol. Metab. 2000, 85, 4500–4510. [Google Scholar] [CrossRef]
- Margo, K.; Winn, R. Testosterone treatments: Why, when, and how? Am. Fam. Physician 2006, 73, 1591–1598. [Google Scholar] [PubMed]
- Bond, P.; Llewellyn, W.; Van Mol, P. Anabolic androgenic steroid-induced hepatotoxicity. Med. Hypotheses 2016, 93, 150–153. [Google Scholar] [CrossRef] [PubMed]
- Falahati-Nini, A.; Riggs, B.L.; Atkinson, E.J.; O’Fallon, W.M.; Eastell, R.; Khosla, S. Relative contributions of testosterone and estrogen in regulating bone resorption and formation in normal elderly men. J. Clin. Investig. 2000, 106, 1553–1560. [Google Scholar] [CrossRef] [PubMed]
- Baas, W.; Kohler, T.S. Testosterone replacement therapy and voiding dysfunction. Transl. Androl. Urol. 2016, 5, 890–897. [Google Scholar] [CrossRef] [PubMed]
- Tyagi, A.; Rajalakshmi, M.; Jeyaraj, D.A.; Sharma, R.S.; Bajaj, J.S. Effects of long-term use of testosterone enanthate. II. Effects on lipids, high and low density lipoprotein cholesterol and liver function parameters. Int. J. Androl. 1999, 22, 347–355. [Google Scholar] [CrossRef]
- Sadowska-Krępa, E.; Kłapcińska, B.; Nowara, A.; Jagsz, S.; Szołtysek-Bołdys, I.; Chalimoniuk, M.; Langfort, J.; Chrapusta, S.J. High-dose testosterone supplementation disturbs liver pro-oxidant/antioxidant balance and function in adolescent male Wistar rats undergoing moderate-intensity endurance training. PeerJ 2020, 8, e10228. [Google Scholar] [CrossRef] [PubMed]
- Feighan, S.M.; Hughes, M.; Maunder, K.; Roche, E.; Gallagher, L. A profile of mental health and behaviour in Prader-Willi syndrome. J. Intellect. Disabil. Res. 2020, 64, 158–169. [Google Scholar] [CrossRef] [PubMed]
- Clarke, D.J.; Boer, H.; Chung, M.C.; Sturmey, P.; Webb, T. Maladaptive behaviour in Prader-Willi syndrome in adult life. J. Intellect. Disabil. Res. 1996, 40 Pt 2, 159–165. [Google Scholar] [CrossRef] [PubMed]
| Males with PWS | |
|---|---|
| n = 57 | |
| Age in years, median (IQR) | 29 (20–40) |
| BMI in kg/m2, median (IQR) | 27 (26–32) |
| Overweight (BMI 25–30 kg/m2), n (%) | 29 (51%) |
| Obesity (BMI > 30 kg/m2), n (%) | 17 (30%) |
| Genetic subtype | |
| Deletion | 29 (51%) |
| mUPD a | 20 (35%) |
| ICD | 2 (4%) |
| Unknown | 6 (11%) |
| Growth hormone treatment | |
| Only during childhood | 4 (7%) |
| Only during adulthood | 1 (2%) |
| Both | 20 (35%) |
| Never | 32 (56%) |
| Current growth hormone treatment | 19 (33%) |
| Living situation | |
| With family | 16 (28%) |
| In a specialized PWS group home | 8 (14%) |
| In a non-specialized facility | 32 (56%) |
| Other b | 1 (2%) |
| Education level | |
| Secondary vocational education | 2 (4%) |
| Pre-vocational secondary education | 2 (4%) |
| Special education | 43 (75%) |
| No education | 1 (2%) |
| Unknown | 9 (16%) |
| Relationship status | |
| In a relationship with sexual intercourse | 2 (4%) |
| In a relationship without sexual intercourse | 10 (18%) |
| Not in a relationship | 37 (65%) |
| Unknown | 8 (14%) |
| Cryptorchidism | 36 (63%) |
| Of which underwent orchidopexy, n (% of cryptorchidism) | 34 (94%) |
| Of which underwent orchidectomy, n (% of cryptorchidism) | 2 (6%) |
| No cryptorchidism | 5 (9%) |
| Cryptorchidism unknown | 16 (28%) |
| Small penile length | |
| Yes | 22 (39%) |
| No | 11 (19%) |
| Unknown | 24 (42%) |
| Males with PWS | |
|---|---|
| n = 57 | |
| Hypogonadism before screening, n (%) | 28 (49%) |
| Of which treated, n (% of hypogonadal) | 24 (86%) |
| Type of testosterone replacement therapy before screening | |
| Gel, n (% of treated) | 12 (50%) |
| Injections, n (% of treated) | 10 (42%) |
| Short-acting, n (% of treated) | 9 (38%) |
| Long-acting, n (% of treated) | 1 (4%) |
| Oral, n (% of treated) | 2 (8%) |
| Newly diagnosed hypogonadism, n (%) | 28 (49%) |
| Hypogonadism after screening, n (%) | 56 (98%) |
| Of which currently treated, n (% of hypogonadal) | 42 (75%) |
| Current type of testosterone replacement therapy | |
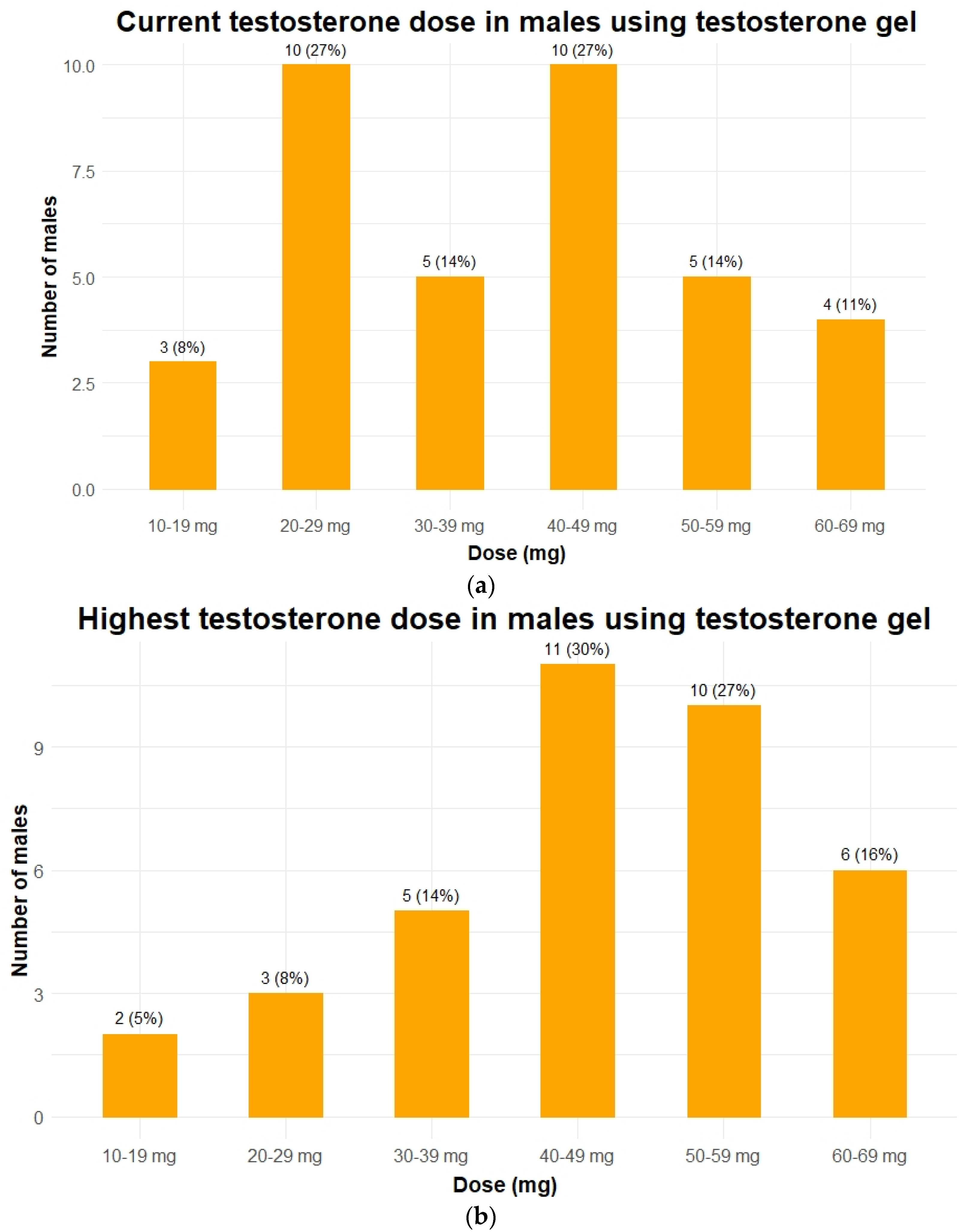
| Gel, n (% of treated) | 37 (88%) |
| Injections, n (% of treated) | 3 (7%) |
| Short-acting, n (% of treated) | 3 (7%) |
| Long-acting, n (% of treated) | 0 (0%) |
| Oral, n (% of treated) | 2 (5%) |
| Decrease in testosterone dose due to challenging behavior | |
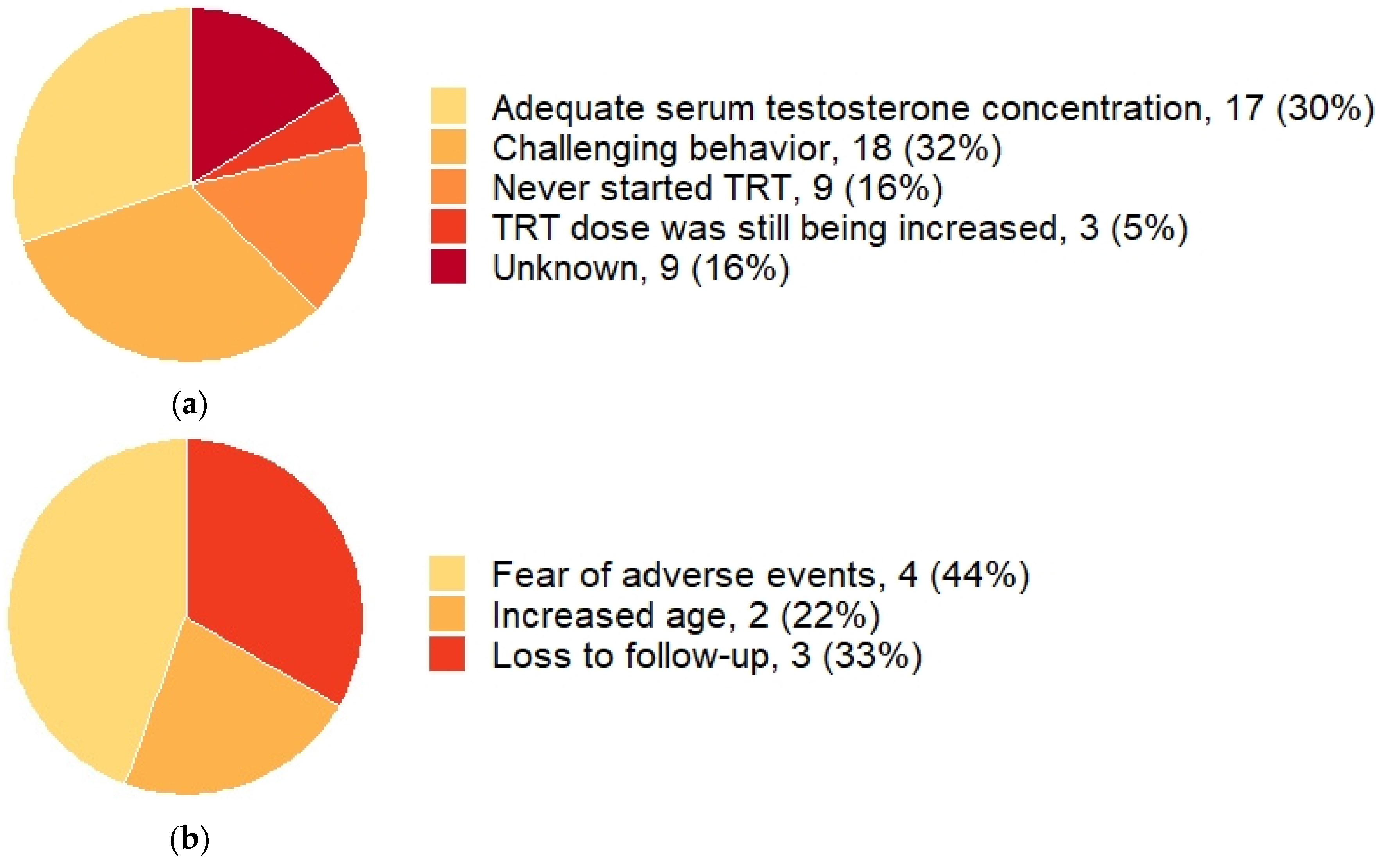
| Yes, n (%) | 18 (32%) |
| Of which had increased testosterone concentrations, n (% of yes) a | 1 (6%) |
| Of which had normal testosterone concentrations, n (% of yes) a | 2 (11%) |
| Of which had inadequate testosterone concentrations, n (% of yes) a | 15 (83%) |
| Of which reported a decrease in challenging behavior after the testosterone dose was decreased, n (% of yes) | 11 (61%) |
| No, n (%) | 31 (54%) |
| Unknown, n (%) | 8 (14%) |
| Problems with compliance to testosterone replacement therapy | |
| Yes, n (%) | 6 (11%) |
| High suspicion of non-compliance, n (%) | 5 (9%) |
| No problems with compliance reported, n (%) | 36 (63%) |
| Never used testosterone replacement therapy, n (%) | 10 (18%) |
| Enlarged breasts | |
| Yes, n (%) | 8 (14%) |
| Gynaecomastia, n (% of enlarged breasts) | 1 (13%) |
| Lipomastia, n (% of enlarged breasts) | 2 (25%) |
| Unknown, n (% of enlarged breasts) | 5 (63%) |
| No or not assessed, n (%) | 49 (86%) |
| Number of Observations | Untreated Male Hypogonadism n = 32 | Number of Observations | Treated/No Male Hypogonadism n = 25 | p-Value | p-Value after Correction for Age | |
|---|---|---|---|---|---|---|
| Age, median (IQR) | 32 | 35 (26–50) | 25 | 23 (19–30) | 0.003 | NA |
| BMI, median (IQR) | 32 | 29 (27–38) | 25 | 26 (23–27) | <0.001 | 0.001 |
| Overweight, n (%) | 15 (47%) | 14 (56%) | ||||
| Obesity, n (%) | 14 (44%) | 3 (12%) | ||||
| Anemia, n (%) | 32 | 11 (34%) | 24 | 4 (17%) | 0.09 | 0.15 |
| Hemoglobin in mmol/L, median (IQR) | 32 | 8.2 (8.0–9.0) | 24 | 9.3 (8.6–9.7) | 0.009 | 0.03 |
| Hemoglobin in g/dL, median (IQR) | 32 | 13.2 (12.9–14.5) | 24 | 15.0 (13.9–15.6) | ||
| Hematocrit in L/L, median (IQR) | 18 | 0.43 (0.42–0.45) | 18 | 0.45 (0.43–0.48) | 0.02 | 0.2 |
| Subjective complaints | ||||||
| Daytime sleepiness, n (%) | 26 | 17 (65%) | 22 | 7 (32%) | 0.02 | 0.09 |
| Fatigue, n (%) | 25 | 7 (28%) | 22 | 4 (18%) | 0.4 | 0.5 |
| Sexual complaints, n (%) | 25 | 3 (12%) | 22 | 2 (9%) | 0.7 | NA a |
| Temper tantrums, n (%) | 26 | 13 (50%) | 22 | 11 (50%) | 1 | 0.7 |
| FSH/Inhibin B Axis | ||||
| Hypothalamic dysfunction (low FSH)  | Hypothalamic or no dysfunction a (normal FSH)  | Testicular dysfunction (high FSH)  | ||
| LH/Testosterone axis | Hypothalamic dysfunction (low/normal LH with low T)  | 1 (3%) | 6 (18%) | 18 (55%) |
| No dysfunction (normal LH with normal T)  | 0 (0%) | 0 (0%) | 1 (3%) | |
| Testicular dysfunction (high LH with low T)  | 0 (0%) | 0 (0%) | 7 (21%) | |
| Article | n | Country | Age Range (Years) | Genotype (Deletion/mUPD/ICD/Translocation) | Mean BMI (kg/m2) | Assays Used | Definition Hypogonadism |
|---|---|---|---|---|---|---|---|
| Partsch et al. (2000) [8] | 7 | Germany | 18–34 a | All deletion or mUPD | 46 a | commercially available immunoassays | testosterone levels below the normal range |
| Whittington et al. (2002) [9] b | 31 | United Kingdom | 18–46 | NA c | NA | NA | undescended testes at birth and/or small genitalia |
| Grugni et al. (2003) [10] | 7 | Italy | 19–29 | 7/0/0/0 | 37 | FSH, LH: immunochemiluminescent assays testosterone: chemiluminescent immunoassay | testosterone levels below the normal range |
| Höybye et al. (2005) [11] b | 7 | Sweden | 19–36 | 0/1/0/0 (6 NA) c | Median 28 | commercially available immunoassays | low testosterone or treatment with sex steroids |
| Miller et al. (2008) [12] b | 10 | Florida, USA | 18–34 | 6/4/0/0 | 38 | commercially available radioimmunoassays | Hypogonadotropic hypogonadism: delayed onset of puberty (i.e., >14 years) in addition to low gonadotropin levels for age |
| Brandau et al. (2008) [13] b | 20 | Missouri, USA | 18–45 | 12/8/0/0 | 35 | FSH, LH: chemiluminescence assays testosterone: radioimmunoassay | testosterone levels below the normal range |
| Sode-Carlsen et al. (2010) [14] b | 21 | Denmark, Norway, Sweden | 18–39 | 13/1/1/0 (6 NA) c | Median 25 | commercially available immunoassays | low testosterone or treatment with sex steroids |
| Van Nieuwpoort et al. (2011) [15] | 4 | The Netherlands | 21–42 | 14/1/0/0 a | 29 | commercially available immunoassays | low testosterone or treatment with sex steroids |
| Radicioni et al. (2012) [16] b | 17 | Italy | 18–42 | 13/4/0/0 | 42 | FSH, LH, testosterone: chemiluminescent microparticle immunoassay Inhibin B: enzymatically amplified two-site two-step sandwich-type immunoassay (ELISA) SHBG: immunoradiometric assay | testosterone and/or inhibin B levels below the normal range |
| Kido et al. (2013) [17] | 16 | Japan | 18–48 | 15/1/0/0 | 33 | NA | testosterone level <300 ng/dL and Tanner stage less than IV. |
| Hirsch et al. (2015) [18] b | 18 | Israel | 18–36 | 11/7/0/0 | 29 | LH, FSH, testosterone: immunoassays Inhibin B, AMH: Two-site enzyme-linked immunosorbent assay (ELISA) SHBG: immunochemiluminescence | NA |
| Coupaye et al. (2016) [19] b | 31 | France | 18–58 a | 42/24/0/0 a,d | 39 a | routine techniques | testosterone level <320 ng/dL or treatment with sex steroids |
| Matsuyama et al. (2019) [20] | 11 | Japan | 18–NA (Mean ± SD: 19.9 ± 2.3) | 6/0/1/0 (4 NA) | NA | LH, FSH: two-site enzyme immune-assay testosterone: chemiluminescent immunoassay | NA |
| Article | Hypogonadism n (%) | Primary Hypogonadism/Central Hypogonadism | FSH, Mean (Range) | LH, Mean (Range) | Testosterone, Mean (Range) | SHBG, Mean (Range) | Inhibin B, Mean (Range) | AMH, Mean (Range) |
|---|---|---|---|---|---|---|---|---|
| Partsch et al. (2000) [8] | 7 (100%) | - a | - | - | - | - | - | - |
| Whittington et al. (2002) [9] | 30 (100%) (1 NA) | - | - | - | - | - | - | - |
| Grugni et al. (2003) [10] | 5 (71%) | - | 12.4 (0.1–30.6) IU/L | 6.0 (0.7–15.1) IU/L | 3.0 (0.5–6.9) ng/mL 10.4 (1.7–23.9) nmol/L | - | - | - |
| Höybye et al. (2005) [11] | 4 (57%) | 0/3 (1 NA) | 4.2 (2.7–10) IU/L | 2.8 (0.6–5.1) IU/L | 9.7 (1.9–37) nmol/L | - | - | - |
| Miller et al. (2008) [12] | 10 (100%) | 0/10 | - | - | - | - | - | - |
| Brandau et al. (2008) [13] | 17 (89%) (1 NA) | - | 14.8 (0.1–52.0) IU/L | 3.1 (0.1–8.0) IU/L | 1.3 (0.3–4.0) ng/mL 4.5 (1.0–13.9) nmol/L | - | - | - |
| Sode-Carlsen et al. (2010) [14] | 14 (67%) | 8/2 (4 NA) | 18.5 (<0.2–64) IU/L | 3.5 (<1.0–13.5) IU/L | 10 (1.9–39.5) nmol/L | - | - | - |
| Van Nieuwpoort et al. (2011) [15] | 4 (100%) | 0/2 (2 NA) | Median 1.1 IU/L | Median 0.43 IU/L | Median 3.2 nmol/L | Median 17.9 nmol/L | - | - |
| Radicioni et al. (2012) [16] | 17 (100%) | 2/9 Combined: 6 | 11.6 (0.05–46.6) IU/L | 2.5 (0.04–7.2) IU/L | 3.7 (1.4–13.7) nmol/L | 22.9 (6.8–42.7) nmol/L | 14.0 (3.0–38.3) pg/mL | - |
| Kido et al. (2013) [17] | - b | 0/3 (13 NA) | 18.9 (<0.5–43.3) IU/L | 4.0 (<0.5–12.8) IU/L | 99 (24–190) ng/dL 3.4 (0.8–6.6) nmol/L | - | - | - |
| Hirsch et al. (2015) [18] | - | - | 16.3 (0.1–55.9) IU/L | 3.0 (0.1–10.5) IU/L | 1.8 (0.2–4.7) nmol/L | 34.2 (9.0–73.8) nmol/L | 72.4 (0.1–269.0) pg/mL (n = 17) | 12.13 (0.17–62.40) ng/mL (n = 16) |
| Coupaye et al. (2016) [19] | 30 (97%) | - | Mean ± SD 13.2 ± 16 IU/L | Mean ± SD 3.2 ± 3.1 IU/L | 1.3 (0.2–4.0) ng/mL 4.5 (0.7–14) nmol/L | Mean ± SD 30.0 ± 20.0 nmol/L | Mean ± SD 36 ± 38 pg/mL | Mean ± SD 9.5 ± 15.3 ng/mL |
| Matsuyama et al. (2019) [20] | - | - | 19.5 (7.5–30.8) IU/L | 4.0 (1.0–5.3) IU/L | 248 (102–509) ng/dL 8.6 (3.5–17.6) nmol/L | - | - | - |
| Expert 1 and Expert 2 a | Expert 3 | Expert 4 | |
|---|---|---|---|
| (Past) experience | Short-acting injections | Long-acting injections, transdermal gel | Long-acting injections, transdermal gel |
| Preferred mode of administration in PWS | Short-acting injections | Transdermal gel followed by long-acting injections | Long-acting injections, transdermal gel |
| Mode of administration advised against | Oral testosterone | Short-acting injections, oral testosterone | None |
| Preferred starting dose in testosterone naïve patients | Short-acting injections: 125 mg every 3–4 weeks | Long-acting injections: 200 mg every 12 weeks Transdermal gel: 10 mg daily | Long-acting injections: 250–500 mg for the first injection Transdermal gel: 10–30 mg depending on testosterone level |
| Preferred follow-up dose | Short-acting injections: After 6 months: increase to 200 mg every 3–4 weeks and then 250 mg every 3–4 weeks depending on serum testosterone concentrations, clinical signs and adverse effects | Long-acting injections: Every 6–9 months: increase by 200–300 mg, depending on serum testosterone and SHBG concentration Transdermal gel: Every 3–6 months: increase by 10 mg | Long-acting injections: Depending on the increase in serum testosterone concentration, injection of 500–1000 mg after 6 weeks. After 12 weeks, depending on the testosterone level obtained, injection of 500–1000 mg, which is then continued every 12 weeks aiming for a serum testosterone concentration within the normal range Transdermal gel: Gradual increase over 1–4 weeks to 30–50 mg daily, aiming for a serum testosterone concentration within the normal range |
| Biochemical follow up | Testosterone, Hb, Ht after each change of TRT dose. Once the final dose of TRT has been obtained, measurement of testosterone, Hb, Ht every year | Testosterone, Hb, Ht, SHBG, estradiol every 6 months or prior to dose increase | Testosterone, LH, FSH, Hb, Ht every 6–12 months, cholesterol every 12 months |
| Considerations: | Only short-acting injections are reimbursed in these experts’ country (France), while transdermal gel is no longer available | Start with transdermal gel as this allows gradual dose up-titration and immediate cessation if behavioral problems occur. Once established on final transdermal dose, switch to long-acting injections as this has smoother pharmacokinetics than short-acting injections and does not need to be applied daily, though depending on patient preference may continue transdermal gel | Short-acting injections not available in the expert’s country (Sweden). Decision for long-acting injections or transdermal gel based on patient preference, most patients prefer injections instead of transdermal gel |
| Additional remarks | With gradual increases in testosterone dose behavioral problems do not appear to be an issue. Once established on long-acting injections measure testosterone concentrations ~1–2 months after injection and at trough just prior to injection as may need to increase injection frequency rather than dose |
| Expert 5 | Expert 6 | Expert 7 | Expert 8 | |
|---|---|---|---|---|
| (Past) experience | Long-acting injections, transdermal gel, oral testosterone | Short-acting injections, transdermal gel | Short-acting injections, transdermal gel | Short-acting injections, transdermal gel |
| Preferred mode of administration in PWS | Transdermal gel | Short-acting injections, transdermal gel | Short-acting injections, transdermal gel | Long-acting injections |
| Mode of administration advised against | Short-acting injections, oral testosterone | Long-acting injections, oral testosterone | Oral testosterone | None |
| Preferred starting dose in testosterone naïve patients | Transdermal gel: 12.5 mg daily | Short-acting injections: 50 mg every month Transdermal gel: 10 mg daily | Short-acting injections: 100–125 mg every 4 weeks Long-acting injections: 250–500 mg every 3 months Transdermal gel: 10 mg daily | Short-acting injections: 100 mg every month Transdermal gel: 50 mg daily |
| Preferred follow-up dose | Long-acting injections: Every 3–6 months: adjust dosing interval based on trough testosterone level Transdermal gel: Every 3–4 months: increase dose by 12.5 mg based on serum testosterone concentration and clinical response | Short-acting injections: Every 3–6 months: increase by 50 mg Transdermal gel: Every 4 weeks: increase by 10 mg | Short-acting and long-acting injections: Low dose for many years Transdermal gel: Every 6–8 weeks: increase by 10 mg | Short-acting injections and transdermal gel: Check up to see if testosterone has normalized after 3–4 months and increase dose based on serum testosterone concentration and clinical response |
| Biochemical follow up | Testosterone, Hb, Ht every 6–12 months | LH, FSH, testosterone, Hb, Ht, liver transaminases every 6 months and prior to any dose modification | Testosterone, Hb, Ht, liver transaminases every 6–8 months | Testosterone, Hb, Ht every 3–4 months |
| Considerations | Start with transdermal gel as this can be stopped quickly and is most suitable due to more physiological testosterone concentrations. When patient achieves normal testosterone level, either continue transdermal gel or switch to long-acting injections, based on patient preference. | Transdermal gel when the patient is compliant and the family reliable, otherwise short-acting injections. | Transdermal gel is most suitable as it results in more physiological testosterone concentrations and can be stopped instantly if behavioral problems appear, but compliance is better with injections. | Long-acting would be most suitable, but is not reimbursed in this country (Spain). |
| Additional remarks |
| Expert 9 | Expert 10 | Expert 11 | |
|---|---|---|---|
| (Past) experience | Short-acting injections, transdermal gel | Short-acting injections, long-acting injections, transdermal gel | Transdermal gel, short-acting injections, long-acting injections, oral testosterone |
| Preferred mode of administration in PWS | Transdermal gel | Short-acting injections, transdermal gel | Transdermal gel |
| Mode of administration advised against | Oral testosterone | None | Oral testosterone |
| Preferred starting dose in testosterone naïve patients | Short-acting injections: 50–100 mg, depending on serum testosterone concentration and age Transdermal gel: 12.5–25 mg, depending on serum testosterone concentration and age | Short-acting injections: 25 mg every week or 50 mg every month Transdermal gel: 25 mg daily | Transdermal gel: 10 mg daily |
| Preferred follow-up dose | Short-acting injections: Every 6 months: increase by 50 to 100 mg Transdermal gel: Every 6 months: increase by 12.5 to 25 mg | Short-acting injections: Every 3 months: increase by 25 mg Transdermal gel: Every 3 months: increase by 25 mg | Transdermal gel: Every 4 weeks: increase by 10 mg |
| Biochemical follow up | Testosterone, Hb, Ht every 6 months | Testosterone, Hb, Ht, inhibin B every 3 months | LH, FSH, testosterone, Hb, Ht every 3 months |
| Considerations | Transdermal gel is most suitable as this results in stable serum testosterone concentrations, but this requires a reliable caregiver and can cause skin irritation and skin picking. | Short-acting injections and gel are tolerated best and easy to dose adjust. | Transdermal gel is most suitable as it can be stopped immediately when behavioral challenges occur due to the short half-life time. |
| Additional remarks | Use gel in the morning and apply gel to shoulders, not belly (due to increased abdominal fat in PWS). |
| TRT Formulation | Examples | Starting Dose | Dose Increase | Advantages | Disadvantages |
|---|---|---|---|---|---|
| Transdermal gel | Testosterone (e.g., Androgel®, Testim®, Tostran®, Testogel®, Testavan®) | 10 mg daily | Increase dose by 10 mg every 3–6 months until testosterone values within the normal range are achieved |
|
|
| Short-acting injections | Testosterone decanoate/isocaproate/phenylpropionate/propionate mixture (e.g., Sustanon®) Testosterone enanthate or cypionate (e.g., Xyosted®, Andortardyl®) | 50–125 mg every month | Increase dose by 25–100 mg every 3–6 months until serum testosterone concentrations within the normal range are achieved |
|
|
| Long-acting injections | Testosterone undecanoate (e.g., Nebido®, Reandron®, AVEED®) | 200–500 mg every 3 months | Increase dose by 200–500 mg every 3–9 months until serum testosterone concentrations within the normal range are achieved |
|
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pellikaan, K.; Ben Brahim, Y.; Rosenberg, A.G.W.; Davidse, K.; Poitou, C.; Coupaye, M.; Goldstone, A.P.; Høybye, C.; Markovic, T.P.; Grugni, G.; et al. Hypogonadism in Adult Males with Prader-Willi Syndrome—Clinical Recommendations Based on a Dutch Cohort Study, Review of the Literature and an International Expert Panel Discussion. J. Clin. Med. 2021, 10, 4361. https://doi.org/10.3390/jcm10194361
Pellikaan K, Ben Brahim Y, Rosenberg AGW, Davidse K, Poitou C, Coupaye M, Goldstone AP, Høybye C, Markovic TP, Grugni G, et al. Hypogonadism in Adult Males with Prader-Willi Syndrome—Clinical Recommendations Based on a Dutch Cohort Study, Review of the Literature and an International Expert Panel Discussion. Journal of Clinical Medicine. 2021; 10(19):4361. https://doi.org/10.3390/jcm10194361
Chicago/Turabian StylePellikaan, Karlijn, Yassine Ben Brahim, Anna G. W. Rosenberg, Kirsten Davidse, Christine Poitou, Muriel Coupaye, Anthony P. Goldstone, Charlotte Høybye, Tania P. Markovic, Graziano Grugni, and et al. 2021. "Hypogonadism in Adult Males with Prader-Willi Syndrome—Clinical Recommendations Based on a Dutch Cohort Study, Review of the Literature and an International Expert Panel Discussion" Journal of Clinical Medicine 10, no. 19: 4361. https://doi.org/10.3390/jcm10194361
APA StylePellikaan, K., Ben Brahim, Y., Rosenberg, A. G. W., Davidse, K., Poitou, C., Coupaye, M., Goldstone, A. P., Høybye, C., Markovic, T. P., Grugni, G., Crinò, A., Caixàs, A., Eldar-Geva, T., Hirsch, H. J., Gross-Tsur, V., Butler, M. G., Miller, J. L., van den Berg, S. A. A., van der Lely, A. J., & de Graaff, L. C. G. (2021). Hypogonadism in Adult Males with Prader-Willi Syndrome—Clinical Recommendations Based on a Dutch Cohort Study, Review of the Literature and an International Expert Panel Discussion. Journal of Clinical Medicine, 10(19), 4361. https://doi.org/10.3390/jcm10194361








