Identification of Patients with Similar Gait Compensating Strategies Due to Unilateral Hip Osteoarthritis and the Effect of Total Hip Replacement: A Secondary Analysis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Gait Analysis
2.3. Principal Component Analysis and Cluster Analysis
2.4. Statistical Analysis
3. Results
3.1. Participants
3.2. Characterization of the Identified Clusters
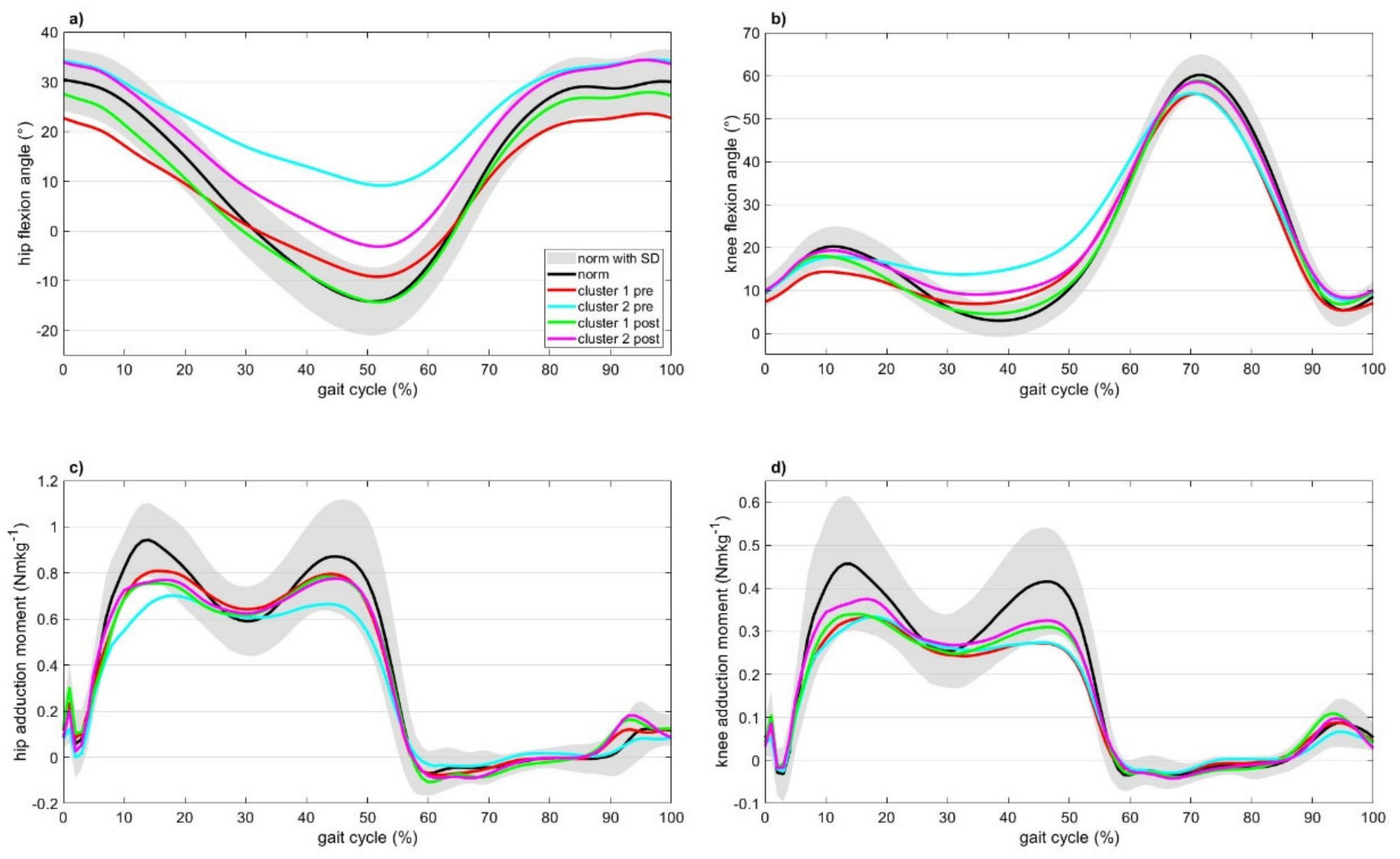
3.3. Gait Parameters of the Identified Clusters and the Effect of Surgery
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Damen, J.; Van Rijn, R.M.; Emans, P.J.; Hilberdink, W.K.H.A.; Wesseling, J.; Oei, E.H.G.; Bierma-Zeinstra, S.M.A. Prevalence and development of hip and knee osteoarthritis according to American College of Rheumatology criteria in the CHECK cohort. Arthritis Res. Ther. 2019, 21, 4. [Google Scholar] [CrossRef] [Green Version]
- Postler, A.; Ramos, A.L.; Goronzy, J.; Günther, K.-P.; Lange, T.; Schmitt, J.; Zink, A.; Hoffmann, F. Prevalence and treatment of hip and knee osteoarthritis in people aged 60 years or older in Germany: An analysis based on health insurance claims data. Clin. Interv. Aging 2018, 13, 2339–2349. [Google Scholar] [CrossRef] [Green Version]
- Fuchs, J.; Rabenberg, M.; Scheidt-Nave, C. Prevalence of selected musculoskeletal conditions in Germany—Results of the German health interview and examination survey for adults (DEGS1). Bundesgesundheitsbl 2013, 56, 723–732. [Google Scholar] [CrossRef]
- Wieczorek, M.; Rotonda, C.; Coste, J.; Pouchot, J.; Saraux, A.; Guillemin, F.; Rat, A.-C. Trajectory analysis combining pain and physical function in individuals with knee and hip osteoarthritis: Results from the French KHOALA cohort. Rheumatology 2020, 59, 3488–3498. [Google Scholar] [CrossRef]
- Neuprez, A.; Neuprez, A.H.; Kaux, J.-F.; Kurth, W.; Daniel, C.; Thirion, T.; Huskin, J.-P.; Gillet, P.; Bruyère, O.; Reginster, J.-Y. Total joint replacement improves pain, functional quality of life, and health utilities in patients with late-stage knee and hip osteoarthritis for up to 5 years. Clin. Rheumatol. 2020, 39, 861–871. [Google Scholar] [CrossRef] [PubMed]
- Miki, H.; Sugano, N.; Hagio, K.; Nishii, T.; Kawakami, H.; Kakimoto, A.; Nakamura, N.; Yoshikawa, H. Recovery of walking speed and symmetrical movement of the pelvis and lower extremity joints after unilateral THA. J. Biomech. 2004, 37, 443–455. [Google Scholar] [CrossRef] [PubMed]
- Stief, F.; Schmidt, A.; Van Drongelen, S.; Lenarz, K.; Froemel, D.; Tarhan, T.; Lutz, F.; Meurer, A. Abnormal loading of the hip and knee joints in unilateral hip osteoarthritis persists two years after total hip replacement. J. Orthop. Res. 2018, 36, 2167–2177. [Google Scholar] [CrossRef] [Green Version]
- Foucher, K.C.; Hurwitz, D.E.; Wimmer, M.A. Preoperative gait adaptations persist one year after surgery in clinically well-functioning total hip replacement patients. J. Biomech. 2007, 40, 3432–3437. [Google Scholar] [CrossRef]
- Andriacchi, T.P.; Mündermann, A. The role of ambulatory mechanics in the initiation and progression of knee osteoarthritis. Curr. Opin. Rheumatol. 2006, 18, 514–518. [Google Scholar] [CrossRef] [PubMed]
- Wesseling, M.; De Groote, F.; Meyer, C.; Corten, K.; Simon, J.-P.; Desloovere, K.; Jonkers, I. Gait alterations to effectively reduce hip contact forces. J. Orthop. Res. 2015, 33, 1094–1102. [Google Scholar] [CrossRef]
- Ardestani, M.M.; Moazen, M.; Jin, Z. Sensitivity analysis of human lower extremity joint moments due to changes in joint kinematics. Med. Eng. Phys. 2015, 37, 165–174. [Google Scholar] [CrossRef]
- Shakoor, N.; Foucher, K.C.; Wimmer, M.A.; Mikolaitis-Preuss, R.A.; Fogg, L.F.; Block, J.A. Asymmetries and relationships between dynamic loading, muscle strength, and proprioceptive acuity at the knees in symptomatic unilateral hip osteoarthritis. Arthritis Res. Ther. 2014, 16, 455. [Google Scholar] [CrossRef] [Green Version]
- Shakoor, N.; Block, J.A.; Shott, S.; Case, J.P. Nonrandom evolution of end-stage osteoarthritis of the lower limbs. Arthritis Rheum. 2002, 46, 3185–3189. [Google Scholar] [CrossRef]
- Braeken, A.M.; Lochhaas-Gerlach, J.A.; Gollish, J.D.; Myles, J.D.; Mackenzie, T.A. Determinants of 6–12 month post-operative functional status and pain after elective total hip replacement. Int. J. Qual. Health Care 1997, 9, 413–418. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holstege, M.S.; Lindeboom, R.; Lucas, C. Preoperative quadriceps strength as a predictor for short-term functional outcome after total hip replacement. Arch. Phys. Med. Rehabil. 2011, 92, 236–241. [Google Scholar] [CrossRef] [PubMed]
- Kamimura, A.; Sakakima, H.; Tsutsumi, F.; Sunahara, N. Preoperative predictors of ambulation ability at different time points after total hip arthroplasty in patients with osteoarthritis. Rehabil. Res. Pract. 2014, 2014, 1–7. [Google Scholar] [CrossRef] [Green Version]
- Beaulieu, M.L.; Lamontagne, M.; Beaulé, P.E. Lower limb biomechanics during gait do not return to normal following total hip arthroplasty. Gait Posture 2010, 32, 269–273. [Google Scholar] [CrossRef]
- Böhm, H.; Hagemeyer, D.; Thummerer, Y.; Kipping, R.; Stöckle, U.; Scheuerer, K. Rehabilitation of gait in patients after total hip arthroplasty: Comparison of the minimal invasive Yale 2-incision technique and the conventional lateral approach. Gait Posture 2016, 44, 110–115. [Google Scholar] [CrossRef] [PubMed]
- Foucher, K.C.; Freels, S. Preoperative factors associated with postoperative gait kinematics and kinetics after total hip arthroplasty. Osteoarthr. Cartil. 2015, 23, 1685–1694. [Google Scholar] [CrossRef] [Green Version]
- Ferber, R.; Osis, S.T.; Hicks, J.L.; Delp, S.L. Gait biomechanics in the era of data science. J. Biomech. 2016, 49, 3759–3761. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Halilaj, E.; Rajagopal, A.; Fiterau, M.; Hicks, J.L.; Hastie, T.J.; Delp, S.L. Machine learning in human movement bio-mechanics: Best practices, common pitfalls, and new opportunities. J. Biomech. 2018, 81, 1–11. [Google Scholar] [CrossRef]
- Gupta, S.; Sedamkar, R.R. Machine learning for healthcare: Introduction. In Machine Learning with Health Care Perspective; Jain, V., Chatterjee, J.M., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 1–25. [Google Scholar]
- Rozumalski, A.; Schwartz, M.H. Crouch gait patterns defined using k-means cluster analysis are related to underlying clinical pathology. Gait Posture 2009, 30, 155–160. [Google Scholar] [CrossRef] [PubMed]
- Böhm, H.; Oestreich, C.; Rethwilm, R.; Federolf, P.; Döderlein, L.; Fujak, A.; Dussa, C.U. Cluster analysis to identify foot motion patterns in children with flexible flatfeet using gait analysis—A statistical approach to detect decompensated pathology? Gait Posture 2019, 71, 151–156. [Google Scholar] [CrossRef] [PubMed]
- Figueiredo, P.; Silva, A.; Sampaio, A.; Vilas-Boas, J.P.; Fernandes, R.J. Front crawl sprint performance: A cluster analysis of biomechanics, energetics, coordinative, and anthropometric determinants in young swimmers. Mot. Control. 2016, 20, 209–221. [Google Scholar] [CrossRef] [Green Version]
- Phinyomark, A.; Osis, S.; Hettinga, B.A.; Ferber, R. Kinematic gait patterns in healthy runners: A hierarchical cluster analysis. J. Biomech. 2015, 48, 3897–3904. [Google Scholar] [CrossRef] [PubMed]
- Hoerzer, S.; Von Tscharner, V.; Jacob, C.; Nigg, B.M. Defining functional groups based on running kinematics using self-organizing maps and support vector machines. J. Biomech. 2015, 48, 2072–2079. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, A.; Meurer, A.; Lenarz, K.; Vogt, L.; Froemel, D.; Lutz, F.; Barker, J.; Stief, F. Unilateral hip osteoarthritis: The effect of compensation strategies and anatomic measurements on frontal plane joint loading. J. Orthop. Res. 2016, 35, 1764–1773. [Google Scholar] [CrossRef]
- Van Drongelen, S.; Kaldowski, H.; Fey, B.; Tarhan, T.; Assi, A.; Stief, F.; Meurer, A. Determination of leg alignment in hip osteoarthritis patients with the EOS® System and the effect on external joint moments during gait. Appl. Sci. 2020, 10, 7777. [Google Scholar] [CrossRef]
- Van Drongelen, S.; Kaldowski, H.; Tarhan, T.; Assi, A.; Meurer, A.; Stief, F. Are changes in radiological leg alignment and femoral parameters after total hip replacement responsible for joint loading during gait? BMC Musculoskelet. Disord. 2019, 20, 526. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mazoochian, F.; Schmidutz, F.; Fottner, A.; Jansson, V. Modified mini-Hardinge access for hip prosthesis implantation in the supine position. Oper. Orthop. Traumatol. 2014, 26, 171–183. [Google Scholar] [CrossRef] [PubMed]
- Blasimann, A.; Dauphinee, S.W.; Staal, J.B. Translation, cross-cultural adaptation, and psychometric properties of the german version of the hip disability and osteoarthritis outcome score. J. Orthop. Sports Phys. Ther. 2014, 44, 989–997. [Google Scholar] [CrossRef] [PubMed]
- Nilsdotter, A.K.; Lohmander, L.S.; Klässbo, M.; Roos, E.M. Hip disability and osteoarthritis outcome score (HOOS)—Validity and responsiveness in total hip replacement. BMC Musculoskelet. Disord. 2003, 4, 10–18. [Google Scholar] [CrossRef] [Green Version]
- Harris, W.H. Traumatic arthritis of the hip after dislocation and acetabular fractures: Treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J. Bone Jt. Surg. Am. 1969, 51, 737–755. [Google Scholar] [CrossRef]
- Stief, F.; Böhm, H.; Michel, K.; Schwirtz, A.; Döderlein, L. Reliability and accuracy in three-dimensional gait analysis: A comparison of two lower body protocols. J. Appl. Biomech. 2013, 29, 105–111. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Perron, M.; Malouin, F.; Moffet, H.; McFadyen, B.J. Three-dimensional gait analysis in women with a total hip arthroplasty. Clin. Biomech. 2000, 15, 504–515. [Google Scholar] [CrossRef]
- Ward, J.H. Hierarchical grouping to optimize an objective function. J. Am. Stat. Assoc. 1963, 58, 236–244. [Google Scholar] [CrossRef]
- Rein, R.; Button, C.; Davids, K.; Summers, J. Cluster analysis of movement patterns in multiarticular actions: A tutorial. Mot. Control. 2010, 14, 211–239. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hof, A.L. Scaling gait data to body size. Gait Posture 1996, 4, 222–223. [Google Scholar] [CrossRef]
- Steultjens, M.P.M.; Dekker, J.; Van Baar, M.E.; Oostendorp, R.A.B.; Bijlsma, J.W.J. Range of joint motion and disability in patients with osteoarthritis of the knee or hip. Rheumatology 2000, 39, 955–961. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holla, J.; Steultjens, M.; van der Leeden, M.; Roorda, L.; Bierma-Zeinstra, S.; Broeder, A.D.; Dekker, J. Determinants of range of joint motion in patients with early symptomatic osteoarthritis of the hip and/or knee: An exploratory study in the CHECK cohort. Osteoarthr. Cartil. 2011, 19, 411–419. [Google Scholar] [CrossRef] [Green Version]
- Doherty, M.; Richards, N.; Hornby, J.; Powell, R. Relation between synovial fluid C3 degradation products and local joint inflammation in rheumatoid arthritis, osteoarthritis, and crystal associated arthropathy. Ann. Rheum. Dis. 1988, 47, 190–197. [Google Scholar] [CrossRef]
- Ismailidis, P.; Egloff, C.; Hegglin, L.; Pagenstert, G.; Kernen, R.; Eckardt, A.; Ilchmann, T.; Mündermann, A.; Nüesch, C. Kinematic changes in patients with severe knee osteoarthritis are a result of reduced walking speed rather than disease severity. Gait Posture 2020, 79, 256–261. [Google Scholar] [CrossRef] [PubMed]
- Ewen, A.M.; Stewart, S.; St Clair Gibson, A.; Kashyap, S.N.; Caplan, N. Post-operative gait analysis in total hip re-placement patients—A review of current literature and meta-analysis. Gait Posture 2012, 36, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Kiss, R.M.; Illyés, Á. Comparison of gait parameters in patients following total hip arthroplasty with a direct-lateral or antero-lateral surgical approach. Hum. Mov. Sci. 2012, 31, 1302–1316. [Google Scholar] [CrossRef] [PubMed]
- Robbins, S.M.; Gomes, S.K.; Huk, O.L.; Zukor, D.J.; Antoniou, J. The influence of lateral and posterior total hip arthroplasty approaches on muscle activation and joint mechanics during gait. J. Arthroplast. 2020, 35, 1891–1899.e5. [Google Scholar] [CrossRef] [PubMed]
| Parameter | Patients | Healthy Controls | p-Value |
|---|---|---|---|
| Age (years) | 60.6 (9.9) | 64.2 (7.0) | 0.041 |
| Height (m) | 1.73 (0.07) | 1.69 (0.10) | 0.009 |
| Body mass (kg) | 80.3 (11.5) | 69.0 (12.6) | <0.001 |
| Body Mass Index (kgm−2) | 26.7 (2.9) | 24.2 (2.8) | <0.001 |
| Gender (men/women) | 30/21 | 21/25 | 0.195 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
van Drongelen, S.; Stetter, B.J.; Böhm, H.; Stief, F.; Stein, T.; Meurer, A. Identification of Patients with Similar Gait Compensating Strategies Due to Unilateral Hip Osteoarthritis and the Effect of Total Hip Replacement: A Secondary Analysis. J. Clin. Med. 2021, 10, 2167. https://doi.org/10.3390/jcm10102167
van Drongelen S, Stetter BJ, Böhm H, Stief F, Stein T, Meurer A. Identification of Patients with Similar Gait Compensating Strategies Due to Unilateral Hip Osteoarthritis and the Effect of Total Hip Replacement: A Secondary Analysis. Journal of Clinical Medicine. 2021; 10(10):2167. https://doi.org/10.3390/jcm10102167
Chicago/Turabian Stylevan Drongelen, Stefan, Bernd J. Stetter, Harald Böhm, Felix Stief, Thorsten Stein, and Andrea Meurer. 2021. "Identification of Patients with Similar Gait Compensating Strategies Due to Unilateral Hip Osteoarthritis and the Effect of Total Hip Replacement: A Secondary Analysis" Journal of Clinical Medicine 10, no. 10: 2167. https://doi.org/10.3390/jcm10102167
APA Stylevan Drongelen, S., Stetter, B. J., Böhm, H., Stief, F., Stein, T., & Meurer, A. (2021). Identification of Patients with Similar Gait Compensating Strategies Due to Unilateral Hip Osteoarthritis and the Effect of Total Hip Replacement: A Secondary Analysis. Journal of Clinical Medicine, 10(10), 2167. https://doi.org/10.3390/jcm10102167







