Examining Vaccine Hesitancy in Sub-Saharan Africa: A Survey of the Knowledge and Attitudes among Adults to Receive COVID-19 Vaccines in Ghana
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Setting and Sampling
2.3. Statistical Analysis
2.4. Multinomial Logit Model Specification
3. Results
3.1. Participant Characteristics
3.2. Vaccination Willingness and Hesitancy
3.3. Factors Associated with COVID-19 Vaccination Intention
| Explanatory Variable | Model I (Weighted Sample) | Model II (Unweighted Sample) | ||||||
|---|---|---|---|---|---|---|---|---|
| Not Decided | Unlikely | Not Decided | Unlikely | |||||
| Odds Ratio (95% CI) | Average Marginal Effect (95% CI) | Odds Ratio (95% CI) | Average Marginal Effect (95% CI) | Odds Ratio (95% CI) | Average Marginal Effect (95% CI) | Odds Ratio (95% CI) | Average Marginal Effect (95% CI) | |
| Age | ||||||||
| Ref: 15–25 years | ||||||||
| 26–35 years | 0.796 (0.42–1.49) | −0.021 (−0.13–0.09) | 0.689 (0.36–1.31) | −0.048 (−0.15–0.05) | 0.798 (0.52–1.22) | −0.012 (−0.09–0.09) | 0.609 (0.39–0.95) ** | −0.073 (−0.15–0.003) * |
| 36–45 years | 1.098 (0.56–2.14) | 0.015 (−0.11–0.14) | 1.051 (0.53–2.10) | 0.002 (−0.11–0.11) | 0.888 (0.57–1.39) | 0.004 (−0.08–0.08) | 0.657 (0.41–1.05) * | −0.067 (−0.15–0.01) |
| 46–55 years | 1.067 (0.51–2.25) | 0.050 (−0.09–0.19) | 0.564 (0.25–1.27) | −0.092 (−0.21–0.02) | 0.680 (0.41–1.13) | −0.24 (−0.11–0.06) | 0.411 (0.24–0.72) *** | −0.12 (−0.21–0.03) *** |
| >55 years | 0.466 (0.23–0.95) ** | −0.098 (−0.22–0.02) | 0.473 (0.22–0.003) * | −0.079 (−0.19–0.03) | 0.528 (0.33–0.74) *** | −0.059 (−0.14–0.02) | 0.309 (0.18–0.52) *** | −0.145 (−0.22–0.07) *** |
| Education | ||||||||
| Ref: JSS | ||||||||
| Secondary | 0.379 (0.09–1.56) | −0.178 (−0.46–0.10) | 0.823 (0.16–4.25) | 0.020 (−0.19–0.23) | 0.599 (0.21–1.71) | −0.094 (−0.31–0.13) | 0.756 (0.21–2.71) | −0.010 (−0.18–0.16) |
| Tertiary | 0.839 (0.25– 2.82) | −0.059 (−0.32–0.20) | 1.367 (0.32–5.90) | 0.058 (−0.13–0.24) | 0.612 (0.23–1.60) | −0.099 (−0.30–0.10) | 0.887 (0.28–2.86) | 0.013 (−0.15–0.17) |
| Postgraduate | 0.467 (0.14–1.60) | −0.149 (−0.41–0.11) | 0.922 (0.21–4.05) | 0.028 (−0.16–0.21) | 0.380 (0.14–1.00) ** | −0.170 (−0.37–0.03) | 0.633 (0.20–2.06) | −0.014 (−0.7–0.15) |
| Other | 2.180 (0.28–17.05) | −0.005 (−0.40–0.39) | 5.837 (0.62–55.00) | 0.251 (−0.11–0.61) | 2.001 (0.52–7.72) | 0.102 (−0.19–0.39) | 2.052 (0.41–10.17) | 0.054 (−0.18–0.29) |
| Gender | ||||||||
| Ref: Female | ||||||||
| Male | 0.643 (0.47–0.87) *** | −0.069 (−0.13–0.01) ** | 0.753 (0.53–1.07) | −0.019 (−0.07–0.03) | 0.655 (0.53–0.80) *** | −0.065 (−0.10–0.03) *** | 0.746 (0.59–0.94) ** | −0.022 (−0.06–0.01) |
| Region | ||||||||
| Ref: Ahafo | ||||||||
| Ashanti | 0.526 (0.12–2.41) | −0.156 (−0.50–0.19) | 1.422 (0.14–14.47) | 0.081 (−0.16–0.32) | 0.810 (0.15–4.24) | −0.049 (−0.37–0.28) | 1.177 (0.12–11.13) | 0.034 (−0.26–0.33) |
| Bono | 0.712 (0.13–3.77) | −0.103 (−0.47–0.26) | 1.597 (0.14–18.63) | 0.081 (−0.19–0.35) | 1.311 (0.22–7.90) | 0.040 (−0.32–0.40) | 1.355 (0.12–14.72) | 0.028 (−0.28–0.34) |
| Bono East | 0.548 (0.09–3.46) | −0.168 (−0.55–0.22) | 1.982 (0.15–26.86) | 0.136 (−0.18–0.45) | 0.779 (0.11–5.34) | −0.065 (−0.43–0.30) | 1.398 (0.11–17.06) | 0.064 (−0.28–0.41) |
| Central | 0.461 (0.09–2.24) | −0.193 (−0.54–0.15) | 1.815 (0.17–19.09) | 0.130 (−0.12–0.38) | 0.733 (0.13–4.03) | −0.079 (−0.41–0.25) | 1.483 (0.15–14.45) | 0.078 (−0.22–0.38) |
| Eastern | 0.781 (0.17–3.65) | −0.060 (−0.41–0.29) | 1.085 (0.10–11.43) | 0.022 (−0.22–0.26) | 1.181 (0.22–6.31) | 0.037 (−0.29–0.37) | 0.969 (0.10–9.54) | −0.012 (−0.31–0.28) |
| GreaterAccra | 0.478 (0.11–2.11) | −0.164 (−0.50–0.17) | 1.166 (0.12–11.31) | 0.056 (−0.18–0.29) | 0.742 (0.14–3.78) | −0.056 (−0.38–0.26) | 0.969 (0.11–8.93) | 0.010 (−0.28–0.30) |
| North East | 0.260 (0.02–4.04) | −0.255 (−0.70–0.19) | 1.019 (0.04–25.00) | 0.059 (−0.33–0.45) | 0.599 (0.04–10.02) | −0.098 (−0.57–0.38) | 1.122 (0.05–26.60) | 0.041 (−0.41–0.49) |
| Northern | 0.926 (0.19–4.54) | −0.083 (−0.44–0.27) | 2.571 (0.23–28.25) | 0.145 (−0.12–0.41) | 1.316 (0.23–7.43) | 0.018 (−0.32–0.36) | 1.850 (0.18–18.76) | 0.080 (−0.23–0.39) |
| Oti | 0.778 (0.14–4.43) | −0.075 (−0.46–0.31) | 1.386 (0.11–17.04) | 0.054 (−0.22–0.33) | 1.089 (0.17–7.12) | 0.007 (−0.36–0.38) | 1.205 (0.10–14.52) | 0.022 (−0.31–0.35) |
| Savannah | 0.289 (0.03–2.46) | −0.274 (−0.65–0.11) | 2.312 (0.16–32.79) | 0.203 (−0.15–0.56) | 0.446 (0.05–4.18) | −0.154 (−0.52–0.21) | 1.610 (0.13–20.24) | 0.118 (−0.25–0.49) |
| Upper East | 0.558 (0.10–3.01) | −0.154 (−0.52–0.21) | 1.677 (0.15–19.37) | 0.105 (−0.16–0.37) | 0.902 (0.15–5.44) | −0.036 (−0.38–0.31) | 1.345 (0.13–14.20) | 0.050 (−0.26–0.36) |
| Upper West | 0.525 (0.10–2.69) | −0.146 (−0.50–0.21) | 1.155 (0.10–13.84) | 0.050 (−0.22–0.32) | 0.729 (0.13–4.25) | −0.052 (−0.39–0.29) | 0.812 (0.08–8.77) | −0.013 (−0.32–0.29) |
| Volta | 1.191 (0.24–5.93) | −0.064 (−0.42–0.29) | 3.675 (0.35–38.85) | 0.192 (−0.07–0.45) | 1.986 (0.35–11.19) | 0.063 (−0.28–0.40) | 3.03 (0.30–30.26) | 0.137 (−0.17–0.44) |
| Western | 0.540 (0.11–2.64) | −0.156 (−0.51–0.19) | 1.565 (0.15–16.61) | 0.095 (−0.16–0.35) | 0.875 (0.16–4.84) | −0.040 (−0.37–0.29) | 1.292 (0.13–12.79) | 0.045 (−0.26–0.35) |
| Western North | 0.876 (0.13–5.95) | −0.043 (−0.46–0.38) | 1.268 (0.07–22.09) | 0.035 (−0.28–0.35) | 1.22 (0.17–901) | 0.051 (−0.35–0.45) | 0.842 (0.05–13.11) | −0.031 (−0.37–0.30) |
| Primary Info Source | ||||||||
| Ref: Official Publications | ||||||||
| Media-TV | 1.085 (0.56–2.09) | −0.018 (−0.14–0.11) | 1.99 (0.89–4.44) * | 0.087 (0.003–0.17) ** | 1.102 (0.72–1.69) | 0.019 (−0.05–0.09) | 0.981 (0.60–1.59) | −0.007 (−0.08–0.06) |
| Newspapers | 0.453 (0.14–1.48) | −0.178 (−0.34–0.02) ** | 3.105 (1.05–9.19) ** | 0.220 (0.05–0.39) ** | 0.592 (0.26–1.34) | −0.087 (−0.20–0.02) | 1.190 (0.58–2.45) | 0.050 (−0.06–0.16) |
| Social media | 0.978 (0.49–1.93) | −0.034 (−0.16–0.10) | 1.848 (0.81–4.20) | 0.081 (−0.006–0.17) * | 1.188 (0.76–1.87) | 0.028 (−0.05–0.11) | 1.082 (0.65–1.80) | 0.003 (−0.07–0.08) |
| Word of mouth | 1.080 (0.36–3.28) | −0.026 (−0.23–0.18) | 2.218 (0.72–6.87) | 0.105 (−0.05–0.26) | 0.930 (0.44–1.97) | −0.023 (−0.15–0.10) | 1.257 (0.57–2.76) | 0.040 (−0.08–0.16) |
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO. WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19—11 March 2020. 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020 (accessed on 22 June 2021).
- Ghana Health Service. COVID-19 Updates. 2021. Available online: https://www.ghanahealthservice.org/covid19/archive.php (accessed on 9 May 2021).
- Colbourn, T. COVID-19: Extending or relaxing distancing control measures. Lancet Public Health 2020, 5, e236–e237. [Google Scholar] [CrossRef] [Green Version]
- Hartley, D.M.; Perencevich, E.N. Public health interventions for COVID-19: Emerging evidence and implications for an evolving public health crisis. JAMA 2020, 323, 1908–1909. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pan, A.; Liu, L.; Wang, C.; Guo, H.; Hao, X.; Wang, Q.; Huang, J.; He, N.; Yu, H.; Lin, X.; et al. Association of public health interventions with the epidemiology of the COVID-19 outbreak in Wuhan, China. JAMA 2020, 323, 1915–1923. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fisher, D.; Teo, Y.Y.; Nabarro, D. Assessing national performance in response to COVID-19. Lancet 2020, 396, 653–655. [Google Scholar] [CrossRef]
- Scally, G.; Jacobson, B.; Abbasi, K. The UK’s public health response to covid-19. BMJ 2020. [Google Scholar] [CrossRef]
- Schuchat, A.; CDC COVID-19 Response Team. Public health response to the initiation and spread of pandemic COVID-19 in the United States, 24 February–21 April, 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 551. [Google Scholar] [CrossRef] [PubMed]
- Tabari, P.; Amini, M.; Moghadami, M.; Moosavi, M. International public health responses to COVID-19 outbreak: A rapid review. Iran. J. Med Sci. 2020, 45, 157. [Google Scholar]
- Thayer, W.M.; Hasan, M.Z.; Sankhla, P.; Gupta, S. An interrupted time series analysis of the lockdown policies in India: A national-level analysis of COVID-19 incidence. Health Policy Plan. 2021. [Google Scholar] [CrossRef]
- Frempong, N.K.; Acheampong, T.; Apenteng, O.O.; Nakua, E.; Amuasi, J.H. Does the data tell the true story? A modelling study of early COVID-19 pandemic suppression and mitigation strategies in Ghana. medRxiv 2021. [Google Scholar] [CrossRef]
- Quakyi, N.K. Ghana’s COVID-19 Vaccine Rollout Is Struggling to Keep Up with Its Great Start. 2021. Available online: https://theconversation.com/ghanas-covid-19-vaccine-rollout-is-struggling-to-keep-up-with-its-great-start-159579 (accessed on 9 May 2021).
- Quakyi, N.K.; Asante, N.A.A.; Nartey, Y.A.; Bediako, Y.; Sam-Agudu, N.A. Ghana’s COVID-19 response: The Black Star can do even better. BMJ Glob. Health 2021, 6, e005569. [Google Scholar] [CrossRef]
- Bloom, D.E. The value of vaccination. In Hot Topics in Infection and Immunity in Children VII; Springer: New York, NY, USA, 2011; pp. 1–8. [Google Scholar]
- Londono, S.E.; Li, X.; Toor, J.; de Villiers, M.J.; Nayagam, S.; Hallett, T.B.; Gaythorpe, K.A. How can the public health impact of vaccination be estimated? medRxiv 2021. [Google Scholar] [CrossRef]
- Preaud, E.; Durand, L.; Macabeo, B.; Farkas, N.; Sloesen, B.; Palache, A.; Samson, S.I. Annual public health and economic benefits of seasonal influenza vaccination: A European estimate. BMC Public Health 2014, 14, 1–12. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Randolph, H.E.; Barreiro, L.B. Herd immunity: Understanding COVID-19. Immunity 2020, 52, 737–741. [Google Scholar] [CrossRef] [PubMed]
- WHO. Coronavirus Disease (COVID-19): Herd Immunity, Lockdowns and COVID-19. 2020. Available online: https://www.who.int/news-room/q-a-detail/herd-immunity-lockdowns-and-covid-19 (accessed on 9 May 2021).
- D’souza, G.; Dowdy, D. What Is Herd Immunity and How Can We Achieve It With COVID-19? Johns Hopkins Bloomberg School of Public Health. 2021. Available online: https://www.jhsph.edu/covid-19/articles/achieving-herd-immunity-with-covid19.html (accessed on 23 June 2021).
- Aschwanden, C. Five reasons why COVID herd immunity is probably impossible. Nature 2021, 591, 520–522. [Google Scholar] [CrossRef]
- McNeil, D.G., Jr. How Much Herd Immunity Is Enough? 2020. Available online: https://www.nytimes.com/2020/12/24/health/herd-immunity-covid-coronavirus.html (accessed on 22 June 2021).
- WHO. Episode #1—Herd immunity. 2020. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/media-resources/science-in-5/episode-1 (accessed on 22 June 2021).
- MacDonald, N.E. Vaccine hesitancy: Definition, scope and determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef]
- Dubé, E.; MacDonald, N.E. How can a global pandemic affect vaccine hesitancy? Expert Rev. Vaccines 2020. [Google Scholar] [CrossRef]
- Dubé, E.; Laberge, C.; Guay, M.; Bramadat, P.; Roy, R.; Bettinger, J.A. Vaccine hesitancy: An overview. Hum. Vaccines Immunother. 2013, 9, 1763–1773. [Google Scholar] [CrossRef]
- Dubé, E.; Vivion, M.; MacDonald, N.E. Vaccine hesitancy, vaccine refusal and the anti-vaccine movement: Influence, impact and implications. Expert Rev. Vaccines 2015, 14, 99–117. [Google Scholar] [CrossRef]
- MacDonald, N.E.; Butler, R.; Dubé, E. Addressing barriers to vaccine acceptance: An overview. Hum. Vaccines Immunother. 2018, 14, 218–224. [Google Scholar] [CrossRef] [Green Version]
- Yaqub, O.; Castle-Clarke, S.; Sevdalis, N.; Chataway, J. Attitudes to vaccination: A critical review. Soc. Sci. Med. 2014, 112, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Jennings, W.; Stoker, G.; Bunting, H.; Valgarðsson, V.O.; Gaskell, J.; Devine, D.; McKay, L.; Mills, M.C. Lack of trust, conspiracy beliefs, and social media use predict COVID-19 vaccine hesitancy. Vaccines 2021, 9, 593. [Google Scholar] [CrossRef] [PubMed]
- Murphy, J.; Vallières, F.; Bentall, R.P.; Shevlin, M.; McBride, O.; Hartman, T.K.; McKay, R.; Bennett, K.; Mason, L.; Gibson-Miller, J.; et al. Psychological characteristics associated with COVID-19 vaccine hesitancy and resistance in Ireland and the United Kingdom. Nat. Commun. 2021, 12, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Peretti-Watel, P.; Seror, V.; Cortaredona, S.; Launay, O.; Raude, J.; Verger, P.; Fressard, L.; Beck, F.; Legleye, S.; L’Haridon, O.; et al. A future vaccination campaign against COVID-19 at risk of vaccine hesitancy and politicisation. Lancet Infect. Dis. 2020, 20, 769–770. [Google Scholar] [CrossRef]
- Sallam, M. COVID-19 vaccine hesitancy worldwide: A concise systematic review of vaccine acceptance rates. Vaccines 2021, 9, 160. [Google Scholar] [CrossRef]
- Troiano, G.; Nardi, A. Vaccine hesitancy in the era of COVID-19. Public Health 2021. [Google Scholar] [CrossRef]
- Cerda, A.A.; García, L.Y. Hesitation and refusal factors in individuals’ decision-making processes regarding a Coronavirus disease 2019 vaccination. Front. Public Health 2021, 9, 626852. [Google Scholar] [CrossRef]
- Dror, A.A.; Eisenbach, N.; Taiber, S.; Morozov, N.G.; Mizrachi, M.; Zigron, A.; Srouji, S.; Sela, E. Vaccine hesitancy: The next challenge in the fight against COVID-19. Eur. J. Epidemiol. 2020, 35, 775–779. [Google Scholar] [CrossRef]
- WHO. Report of the Sage Working Group on Vaccine Hesitancy. 2014. Available online: https://www.who.int/immunization/sage/meetings/2014/october/1_Report_WORKING_GROUP_vaccine_hesitancy_final.pdf (accessed on 9 May 2021).
- Wiysonge, C.S.; Ndwandwe, D.; Ryan, J.; Jaca, A.; Batouré, O.; Anya, B.P.M.; Cooper, S. Vaccine hesitancy in the era of COVID-19: Could lessons from the past help in divining the future? Hum. Vaccines Immunother. 2021, 1–3. [Google Scholar] [CrossRef]
- Khubchandani, J.; Sharma, S.; Price, J.H.; Wiblishauser, M.J.; Sharma, M.; Webb, F.J. COVID-19 vaccination hesitancy in the United States: A rapid national assessment. J. Community Health 2021, 46, 270–277. [Google Scholar] [CrossRef]
- Chen, M.; Li, Y.; Chen, J.; Wen, Z.; Feng, F.; Zou, H.; Fu, C.; Chen, L.; Shu, Y.; Sun, C. An online survey of the attitude and willingness of Chinese adults to receive COVID-19 vaccination. Hum. Vaccines Immunother. 2021, 1–10. [Google Scholar] [CrossRef]
- Dzinamarira, T.; Nachipo, B.; Phiri, B.; Musuka, G. COVID-19 vaccine roll-out in South Africa and Zimbabwe: Urgent need to address community preparedness, fears and hesitancy. Vaccines 2021, 9, 250. [Google Scholar] [CrossRef] [PubMed]
- Gagneux-Brunon, A.; Detoc, M.; Bruel, S.; Tardy, B.; Rozaire, O.; Frappe, P.; Botelho-Nevers, E. Intention to get vaccinations against COVID-19 in French healthcare workers during the first pandemic wave: A cross-sectional survey. J. Hosp. Infect. 2021, 108, 168–173. [Google Scholar] [CrossRef] [PubMed]
- Agyekum, M.W.; Afrifa-Anane, G.F.; Kyei-Arthur, F.; Addo, B. Acceptability of COVID-19 vaccination among health care workers in Ghana. Adv. Public Health 2021, 2021, 9998176. [Google Scholar] [CrossRef]
- Reuters. Ghana Aims to Get 17.6 Million Doses of COVID-19 Vaccine by June. 2021. Available online: https://www.reuters.com/article/uk-health-coronavirus-ghana-idUSKBN2A11KB (accessed on 9 May 2021).
- ModernGhana. Ghana on Course to Procure 42 Million More COVID-19 vaccines—Akufo-Addo Assures. 2021. Available online: https://www.modernghana.com/news/1070581/ghana-on-course-to-procure-42-million-more-covid.html (accessed on 9 May 2021).
- Sevencan, S. Ghana to Receive over 1M Doses of Sputnik V Vaccine. 2021. Available online: https://www.aa.com.tr/en/africa/ghana-to-receive-over-1m-doses-of-sputnik-v-vaccine/2227628 (accessed on 9 May 2021).
- BBC. Covax Vaccine-Sharing Scheme Delivers First Doses to Ghana. 2021. Available online: https://www.bbc.co.uk/news/world-africa-56180161 (accessed on 9 May 2021).
- WHO. COVID-19 Vaccine Doses Shipped by the COVAX Facility Head to Ghana, Marking Beginning of Global Rollout. 2021. Available online: https://www.who.int/news/item/24-02-2021-covid-19-vaccine-doses-shipped-by-the-covax-facility-head-to-ghana-marking-beginning-of-global-rollout (accessed on 9 May 2021).
- Dontoh, E. Ghana Gets Second Batch of AstraZeneca Vaccines from Covax. 2021. Available online: https://www.bloomberg.com/news/articles/2021-05-07/ghana-gets-second-batch-of-astrazeneca-vaccines-from-covax (accessed on 9 May 2021).
- WHO. Emerging Lessons from Africa’s COVID-19 Vaccine Rollout—Ghana. 2021. Available online: https://www.afro.who.int/news/emerging-lessons-africas-covid-19-vaccine-rollout (accessed on 9 May 2021).
- Afolabi, A.A.; Ilesanmi, O.S. Dealing with vaccine hesitancy in Africa: The prospective COVID-19 vaccine context. Pan. Afr. Med. J. 2021, 38. [Google Scholar] [CrossRef]
- Rufai, N.A. After Botched Ebola Vaccine Trial, Ghana Struggles with Vaccine Hesitancy. 2021. Available online: https://www.pbs.org/newshour/show/after-botched-ebola-vaccine-trial-ghana-struggles-with-vaccine-hesitancy (accessed on 9 May 2021).
- Johnson, T.P. Snowball Sampling: Introduction. Wiley StatsRef: Statistics Reference Online. 2014. Available online: https://onlinelibrary.wiley.com/doi/abs/10.1002/9781118445112.stat05720 (accessed on 26 January 2021).
- Carrieri, V.; Madio, L.; Principe, F. Vaccine hesitancy and (fake) news: Quasi-experimental evidence from Italy. Health Econ. 2019, 28, 1377–1382. [Google Scholar] [CrossRef]
- Hansen, P.R.; Schmidtblaicher, M. A dynamic model of vaccine compliance: How fake news undermined the Danish HPV vaccine program. J. Bus. Econ. Stat. 2021, 39, 259–271. [Google Scholar] [CrossRef]
- Salathé, M.; Bonhoeffer, S. The effect of opinion clustering on disease outbreaks. J. R. Soc. Interface 2008, 5, 1505–1508. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Allcott, H.; Gentzkow, M.; Yu, C. Trends in the diffusion of misinformation on social media. Res. Politics 2019, 6, 2053168019848554. [Google Scholar] [CrossRef] [Green Version]
- Apuke, O.D.; Omar, B. Fake news and COVID-19: Modelling the predictors of fake news sharing among social media users. Telemat. Inform. 2021, 56, 101475. [Google Scholar] [CrossRef]
- Chou, W.Y.S.; Oh, A.; Klein, W.M. Addressing health-related misinformation on social media. JAMA 2018, 320, 2417–2418. [Google Scholar] [CrossRef]
- Rampersad, G.; Althiyabi, T. Fake news: Acceptance by demographics and culture on social media. J. Inf. Technol. Politics 2020, 17, 1–11. [Google Scholar] [CrossRef]
- World Bank. GNI per Capita, Atlas Method (Current US$)—Ghana | Data. 2021. Available online: https://data.worldbank.org/indicator/NY.GNP.PCAP.CD?locations=GH (accessed on 3 May 2021).
- Ghana Statistical Service. Projected Population by Age and Sex, 260 Districts 2020. 2020. Available online: https://statsghana.gov.gh/nationalaccount_macros.php?Stats=MTA1NTY1NjgxLjUwNg==/webstats/s679n2sn87 (accessed on 3 May 2021).
- Abdelhafiz, A.S.; Mohammed, Z.; Ibrahim, M.E.; Ziady, H.H.; Alorabi, M.; Ayyad, M.; Sultan, E.A. Knowledge, perceptions, and attitude of Egyptians towards the novel coronavirus disease (COVID-19). J. Community Health 2020, 45, 881–890. [Google Scholar] [CrossRef]
- Chow, M.Y.K.; Danchin, M.; Willaby, H.W.; Pemberton, S.; Leask, J. Parental attitudes, beliefs, behaviours and concerns towards childhood vaccinations in Australia: A national online survey. Aust. Fam. Physician 2017, 46, 145–151. [Google Scholar]
- Larson, H.J.; Jarrett, C.; Schulz, W.S.; Chaudhuri, M.; Zhou, Y.; Dube, E.; Schuster, M.; MacDonald, N.E.; Wilson, R. Measuring vaccine hesitancy: The development of a survey tool. Vaccine 2015, 33, 4165–4175. [Google Scholar] [CrossRef] [Green Version]
- Schwarzinger, M.; Watson, V.; Arwidson, P.; Alla, F.; Luchini, S. COVID-19 vaccine hesitancy in a representative working-age population in France: A survey experiment based on vaccine characteristics. Lancet Public Health 2021, 6, e210–e221. [Google Scholar] [CrossRef]
- Ahmad, H.; Halim, H. Determining sample size for research activities. Selangor Bus. Rev. 2017, 2, 20–34. [Google Scholar]
- Kasiulevičius, V.; Šapoka, V.; Filipavičiūtė, R. Sample size calculation in epidemiological studies. Gerontologija 2006, 7, 225–231. [Google Scholar]
- Woolson, R.F.; Bean, J.A.; Rojas, P.B. Sample size for case-control studies using Cochran’s statistic. Biometrics 1986, 42, 927–932. [Google Scholar] [CrossRef]
- Kolenikov, S. Calibrating survey data using iterative proportional fitting (raking). Stata J. 2014, 14, 22–59. [Google Scholar] [CrossRef] [Green Version]
- Mercer, A.; Lau, A.; Kennedy, C. How Different Weighting Methods Work—Pew Research Center Method. 2018. Available online: https://www.pewresearch.org/methods/2018/01/26/how-different-weighting-methods-work (accessed on 3 May 2021).
- Greene, W.H. Econometric Analysis, 8th ed.; Pearson Education, Inc.: New York, NY, USA, 2003. [Google Scholar]
- CDC. COVID-19 and Your Health. 2020. Available online: https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/older-adults.html (accessed on 22 April 2021).
- UK Government. Chapter 14a—COVID-19-SARS-CoV-2. 2021. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/978508/Green_book_chapter_16April2021.pdf (accessed on 22 April 2021).
- Edwards, B.; Biddle, N.; Gray, M.; Sollis, K. COVID-19 vaccine hesitancy and resistance: Correlates in a nationally representative longitudinal survey of the Australian population. PLoS ONE 2021, 16, e0248892. [Google Scholar] [CrossRef]
- Latkin, C.A.; Dayton, L.; Yi, G.; Colon, B.; Kong, X. Mask usage, social distancing, racial, and gender correlates of COVID-19 vaccine intentions among adults in the US. PLoS ONE 2021, 16, e0246970. [Google Scholar] [CrossRef] [PubMed]
- Latkin, C.A.; Dayton, L.; Yi, G.; Konstantopoulos, A.; Boodram, B. Trust in a COVID-19 vaccine in the US: A social-ecological perspective. Soc. Sci. Med. 2021, 270, 113684. [Google Scholar] [CrossRef] [PubMed]
- Cordina, M.; Lauri, M.A. Attitudes towards COVID-19 vaccination, vaccine hesitancy and intention to take the vaccine. Pharm. Pract. 2021, 19. [Google Scholar] [CrossRef]
- Inglehart, R.; Norris, P. The developmental theory of the gender gap: Women’s and men’s voting behavior in global perspective. Int. Political Sci. Rev. 2000, 21, 441–463. [Google Scholar] [CrossRef]
- Meleo-Erwin, Z.; Basch, C.; MacLean, S.A.; Scheibner, C.; Cadorett, V. “To each his own”: Discussions of vaccine decision-making in top parenting blogs. Hum. Vaccines Immunother. 2017, 13, 1895–1901. [Google Scholar] [CrossRef]
- Puri, N.; Coomes, E.A.; Haghbayan, H.; Gunaratne, K. Social media and vaccine hesitancy: New updates for the era of COVID-19 and globalised infectious diseases. Hum. Vaccines Immunother. 2020, 16, 1–8. [Google Scholar] [CrossRef]
- He, Z.; Ren, L.; Yang, J.; Guo, L.; Feng, L.; Ma, C.; Wang, X.; Leng, Z.; Tong, X.; Zhou, W.; et al. Seroprevalence and humoral immune durability of anti-SARS-CoV-2 antibodies in Wuhan, China: A longitudinal, population-level, cross-sectional study. Lancet 2021, 397, 1075–1084. [Google Scholar] [CrossRef]
- Poustchi, H.; Darvishian, M.; Mohammadi, Z.; Shayanrad, A.; Delavari, A.; Bahadorimonfared, A.; Eslami, S.; Javanmard, S.H.; Shakiba, E.; Somi, M.H.; et al. SARS-CoV-2 antibody seroprevalence in the general population and high-risk occupational groups across 18 cities in Iran: A population-based cross-sectional study. Lancet Infect. Dis. 2021, 21, 473–481. [Google Scholar] [CrossRef]
- Shakiba, M.; Nazari, S.S.H.; Mehrabian, F.; Rezvani, S.M.; Ghasempour, Z.; Heidarzadeh, A. Seroprevalence of COVID-19 virus infection in Guilan province, Iran. medRxiv 2020. [Google Scholar] [CrossRef]
- Majiya, H.; Aliyu-Paiko, M.; Balogu, V.T.; Musa, D.A.; Salihu, I.M.; Kawu, A.A.; Bashir, I.Y.; Sani, A.R.; Baba, J.; Muhammad, A.T.; et al. Seroprevalence of SARS-CoV-2 in Niger State: A Pilot Cross Sectional Study. Medrxiv 2020. [Google Scholar] [CrossRef]
- Mulenga, L.B.; Hines, J.Z.; Fwoloshi, S.; Chirwa, L.; Siwingwa, M.; Yingst, S.; Wolkon, A.; Barradas, D.T.; Favaloro, J.; Zulu, J.E.; et al. Prevalence of SARS-CoV-2 in six districts in Zambia in July, 2020: A cross-sectional cluster sample survey. Lancet Glob. Health 2021, 9, e773–e781. [Google Scholar] [CrossRef]
- Uyoga, S.; Adetifa, I.M.; Karanja, H.K.; Nyagwange, J.; Tuju, J.; Wanjiku, P.; Aman, R.; Mwangangi, M.; Amoth, P.; Kasera, K.; et al. Seroprevalence of anti–SARS-CoV-2 IgG antibodies in Kenyan blood donors. Science 2021, 371, 79–82. [Google Scholar] [CrossRef] [PubMed]
- George, J.A.; Khoza, S.; Mayne, E.; Dlamini, S.; Kone, N.; Jassat, W.; Chetty, K.; Centner, C.; Pillay, T.; Maphayi, M.R.; et al. Sentinel seroprevalence of SARS-CoV-2 in the Gauteng province, South Africa August to October 2020. medRxiv 2021. [Google Scholar] [CrossRef]
- Kemp, S. Digital in Ghana: All the Statistics You Need in 2021—DataReportal—Global Digital Insights. 2021. Available online: https://datareportal.com/reports/digital-2021-ghana (accessed on 3 July 2021).
- Abedin, M.; Islam, M.A.; Rahman, F.N.; Reza, H.M.; Hossain, M.Z.; Hossain, M.A.; Hossain, A. Willingness to vaccinate against COVID-19 among Bangladeshi adults: Understanding the strategies to optimize vaccination coverage. PLoS ONE 2021, 16, e0250495. [Google Scholar] [CrossRef] [PubMed]
- Le, X.T.; Nguyen, H.T.; Le, H.T.; Do, T.T.; Nguyen, T.H.; Vu, L.G.; Ho, R.C. Rural–urban differences in preferences for influenza vaccination among women of childbearing age: Implications for local vaccination service implementation in Vietnam. Trop. Med. Int. Health 2021, 26, 228–236. [Google Scholar] [CrossRef]
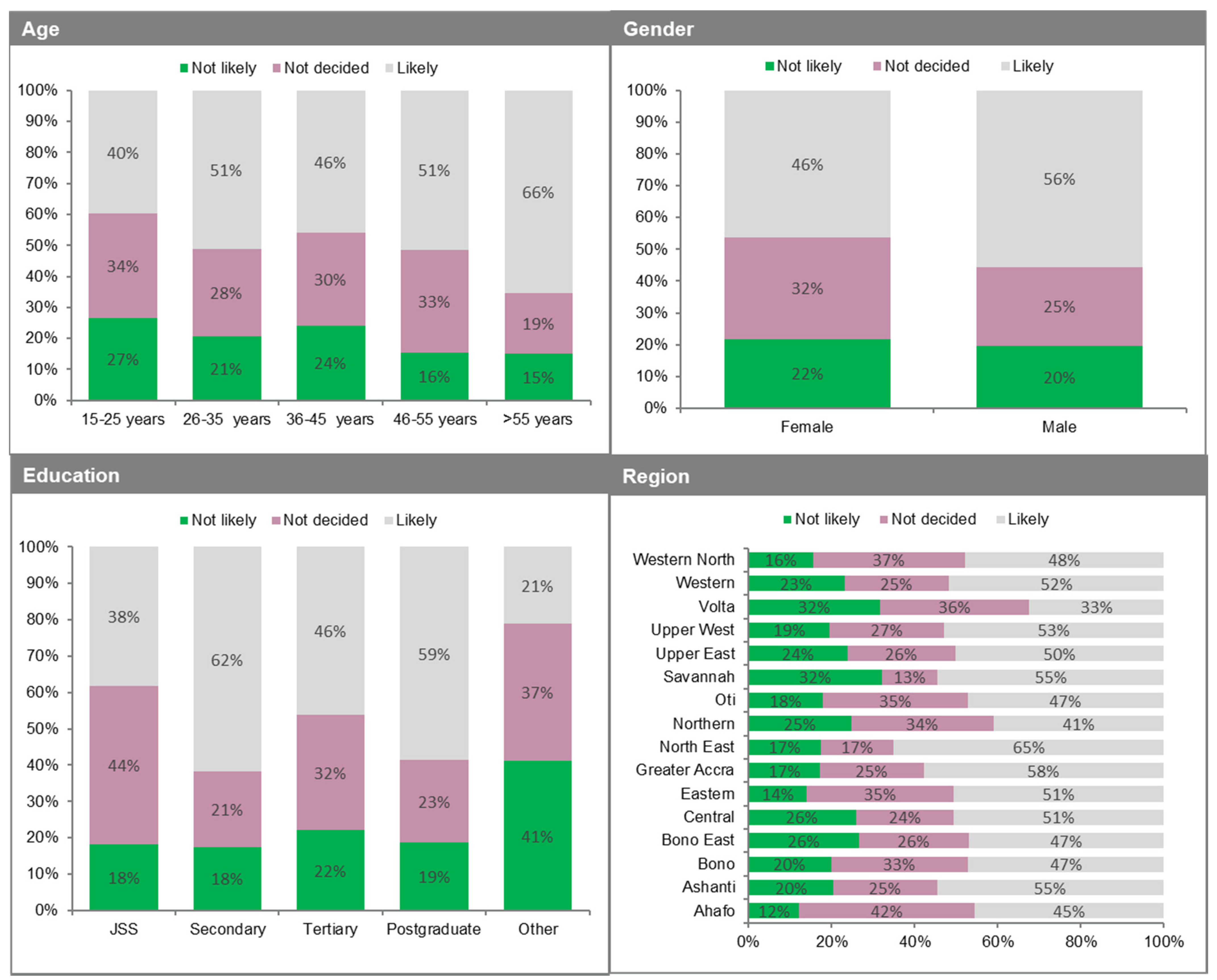

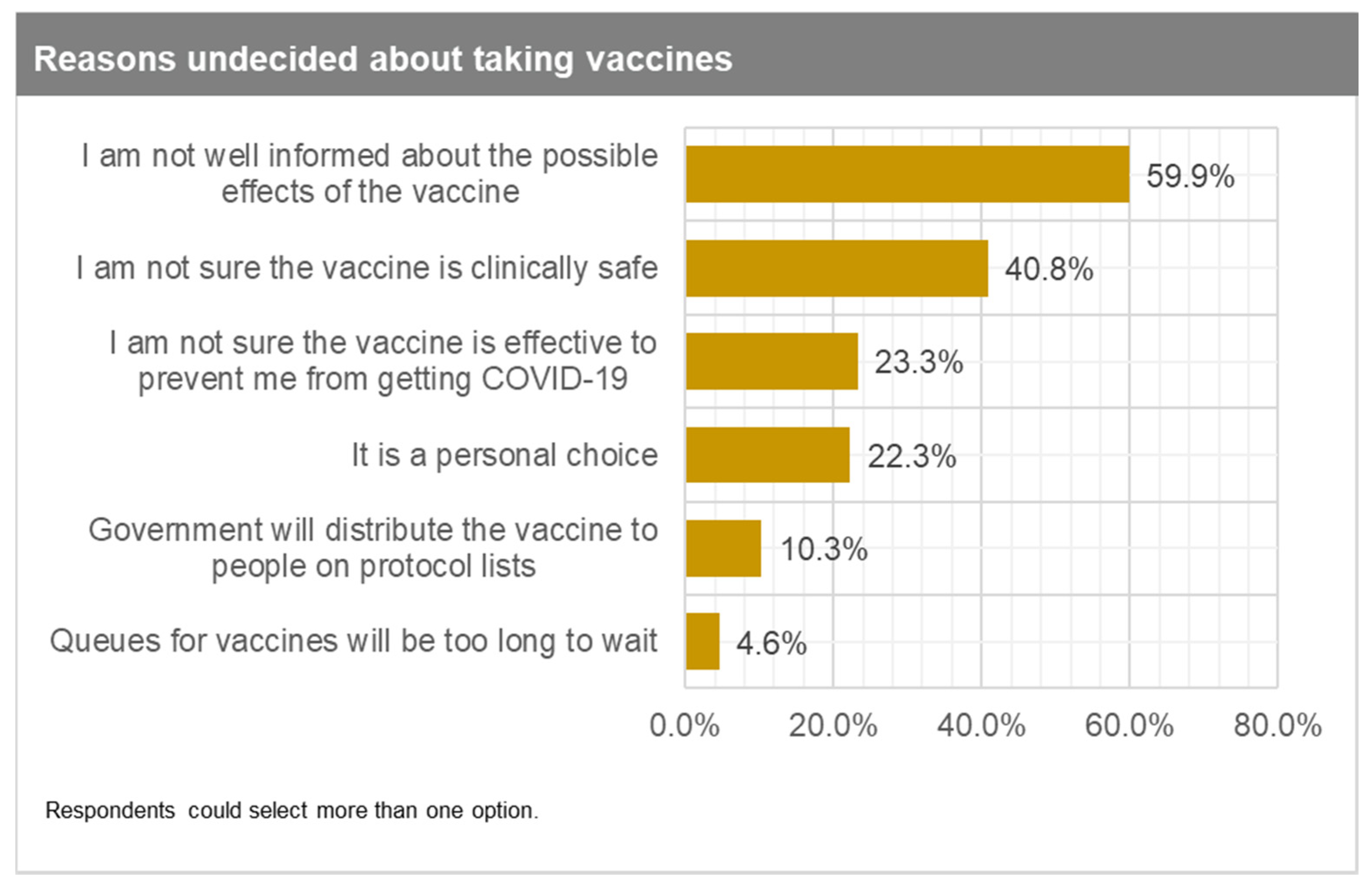
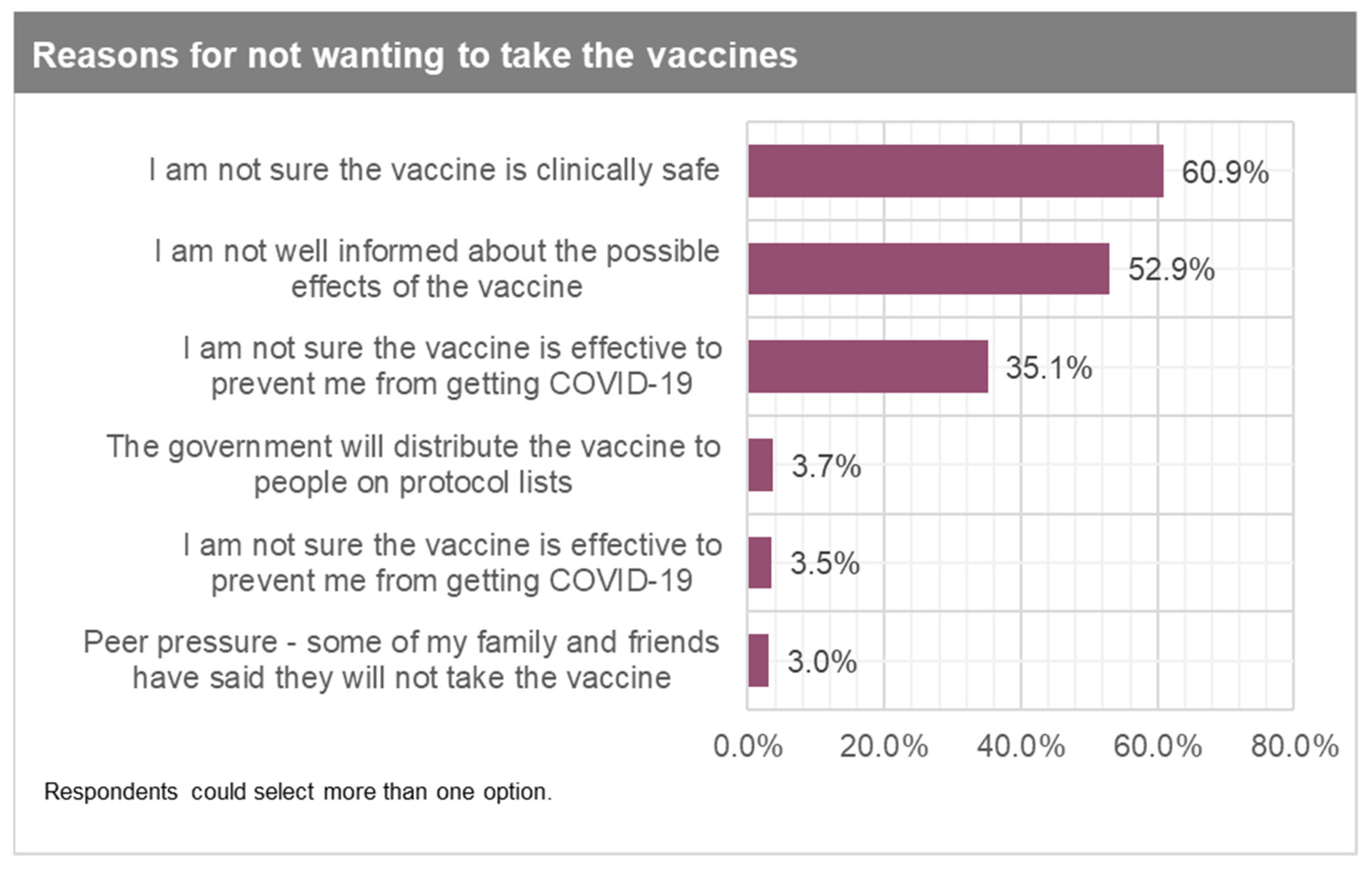
| Variable | Total Weighted Sample N (%) | Likelihood of Taking COVID-19 Vaccine | |||
|---|---|---|---|---|---|
| Likely | Undecided | Unlikely | p-Value | ||
| Total sample | 2345 (100) | 1197 (51%) | 662 (28%) | 486 (21%) | - |
| Gender | |||||
| Female | 1122 (48%) | 518 (46%) | 359 (32%) | 245 (22%) | 0.0083 *** |
| Male | 1223 (52%) | 679 (56%) | 303 (25%) | 241 (20%) | |
| Age group | |||||
| 15–25 | 177 (8%) | 70 (40%) | 59 (34%) | 47 (27%) | 0.0068 *** |
| 26–35 | 1104 (47%) | 565 (51%) | 311 (28%) | 228 (21%) | |
| 36–45 | 546 (23%) | 251 (46%) | 163 (30%) | 132 (24%) | |
| 46–55 | 208 (9%) | 107 (51%) | 69 (33%) | 32 (16%) | |
| Above 55 | 310 (13%) | 203 (66%) | 60 (19%) | 47 (15%) | |
| Education | |||||
| Junior Secondary (JSS) | 30 (1%) | 11 (38%) | 13 (44%) | 5 (18%) | 0.0042 *** |
| Senior Secondary (SSS) | 103 (4%) | 64 (62%) | 21 (21%) | 18 (18%) | |
| Tertiary | 1339 (57%) | 619 (46%) | 425 (32%) | 295 (22%) | |
| Postgraduate | 852 (36%) | 499 (59%) | 194 (23%) | 159 (19%) | |
| Other | 21 (1%) | 4 (21%) | 8 (37%) | 9 (41%) | |
| Tested for COVID-19 | |||||
| No | 1729 (74%) | 826 (48%) | 524 (30%) | 379 (22%) | 0.0013 *** |
| Yes | 615 (26%) | 371 (60%) | 138 (22%) | 107 (17%) | |
| Primary Source of Information | |||||
| Books/Journals/Official Publications | 124 (5%) | 73 (59%) | 35 (28%) | 16 (13%) | 0.3970 |
| Media-TV | 1364 (58%) | 692 (51%) | 391 (29%) | 281 (20%) | |
| Newspapers/Print Media | 74 (3%) | 38 (52%) | 10 (13%) | 25 (35%) | |
| Social Media | 708 (30%) | 358 (51%) | 203 (29%) | 147 (21%) | |
| Word of Mouth (Family and Friends) | 76 (3%) | 36 (48%) | 23 (31%) | 17 (22%) | |
| Region | |||||
| Ahafo | 48 (2%) | 22 (45%) | 20 (42%) | 6 (12%) | 0.7493 |
| Ashanti | 452 (19%) | 247 (55%) | 113 (25%) | 92 (20%) | |
| Bono | 91 (4%) | 43 (47%) | 30 (33%) | 18 (20%) | |
| Bono East | 79 (3%) | 37 (47%) | 21 (26%) | 21 (26%) | |
| Central | 200 (9%) | 101 (51%) | 47 (24%) | 52 (26%) | |
| Eastern | 251 (11%) | 127 (51%) | 89 (35%) | 35 (14%) | |
| Greater Accra | 464 (20%) | 268 (58%) | 116 (25%) | 80 (17%) | |
| North East | 35 (1%) | 23 (65%) | 6 (17%) | 6 (17%) | |
| Northern | 125 (5%) | 51 (41%) | 43 (34%) | 31 (25%) | |
| Oti | 51 (2%) | 24 (47%) | 18 (35%) | 9 (18%) | |
| Savannah | 34 (1%) | 18 (55%) | 4 (13%) | 11 (32%) | |
| Upper East | 85 (4%) | 43 (50%) | 22 (26%) | 20 (24%) | |
| Upper West | 49 (2%) | 26 (53%) | 14 (27%) | 10 (19%) | |
| Volta | 151 (6%) | 49 (33%) | 54 (36%) | 48 (32%) | |
| Western | 162 (7%) | 84 (52%) | 41 (25%) | 37 (23%) | |
| Western North | 69 (3%) | 33 (48%) | 25 (37%) | 11 (16%) | |
| Variable | Assuming No Naturally Acquired Immunity | Assuming 10% Naturally Acquired Immunity | Assuming 20% Naturally Acquired Immunity | |||
|---|---|---|---|---|---|---|
| Population (Millions) | Percentage (%) | Population (Millions) | Percentage (%) | Population (millions) | Percentage (%) | |
| (A) Ghana 2020 total population (GSS) | 31.07 | 100.00% | 31.07 | 100.00% | 31.07 | 100.00% |
| (B) % of the total population needed for herd immunity | 21.75 | 70.00% | 18.64 | 60.00% | 15.54 | 50.00% |
| (C) Ghana’s adult population more than 15 years (GSS) | 19.57 | 63.00% | 16.47 | 53.00% | 13.36 | 43.00% |
| (D) Adult population more than 15 years likely to take vaccine (from survey) | 9.98 | 51.00% | 8.40 | 51.00% | 6.81 | 51.00% |
| (E) Difference (C–D) | 9.59 | 49.00% | 8.07 | 49.00% | 6.55 | 49.00% |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Acheampong, T.; Akorsikumah, E.A.; Osae-Kwapong, J.; Khalid, M.; Appiah, A.; Amuasi, J.H. Examining Vaccine Hesitancy in Sub-Saharan Africa: A Survey of the Knowledge and Attitudes among Adults to Receive COVID-19 Vaccines in Ghana. Vaccines 2021, 9, 814. https://doi.org/10.3390/vaccines9080814
Acheampong T, Akorsikumah EA, Osae-Kwapong J, Khalid M, Appiah A, Amuasi JH. Examining Vaccine Hesitancy in Sub-Saharan Africa: A Survey of the Knowledge and Attitudes among Adults to Receive COVID-19 Vaccines in Ghana. Vaccines. 2021; 9(8):814. https://doi.org/10.3390/vaccines9080814
Chicago/Turabian StyleAcheampong, Theophilus, Eli A. Akorsikumah, John Osae-Kwapong, Musah Khalid, Alfred Appiah, and John H. Amuasi. 2021. "Examining Vaccine Hesitancy in Sub-Saharan Africa: A Survey of the Knowledge and Attitudes among Adults to Receive COVID-19 Vaccines in Ghana" Vaccines 9, no. 8: 814. https://doi.org/10.3390/vaccines9080814
APA StyleAcheampong, T., Akorsikumah, E. A., Osae-Kwapong, J., Khalid, M., Appiah, A., & Amuasi, J. H. (2021). Examining Vaccine Hesitancy in Sub-Saharan Africa: A Survey of the Knowledge and Attitudes among Adults to Receive COVID-19 Vaccines in Ghana. Vaccines, 9(8), 814. https://doi.org/10.3390/vaccines9080814






