Acceptance of COVID-19 Vaccination in Cancer Patients in Hong Kong: Approaches to Improve the Vaccination Rate
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Setting and Design
2.2. Survey Questionnaire
2.3. Data Processing and Analyses
3. Results
3.1. Acceptance of COVID-19 Vaccination by Cancer Patients
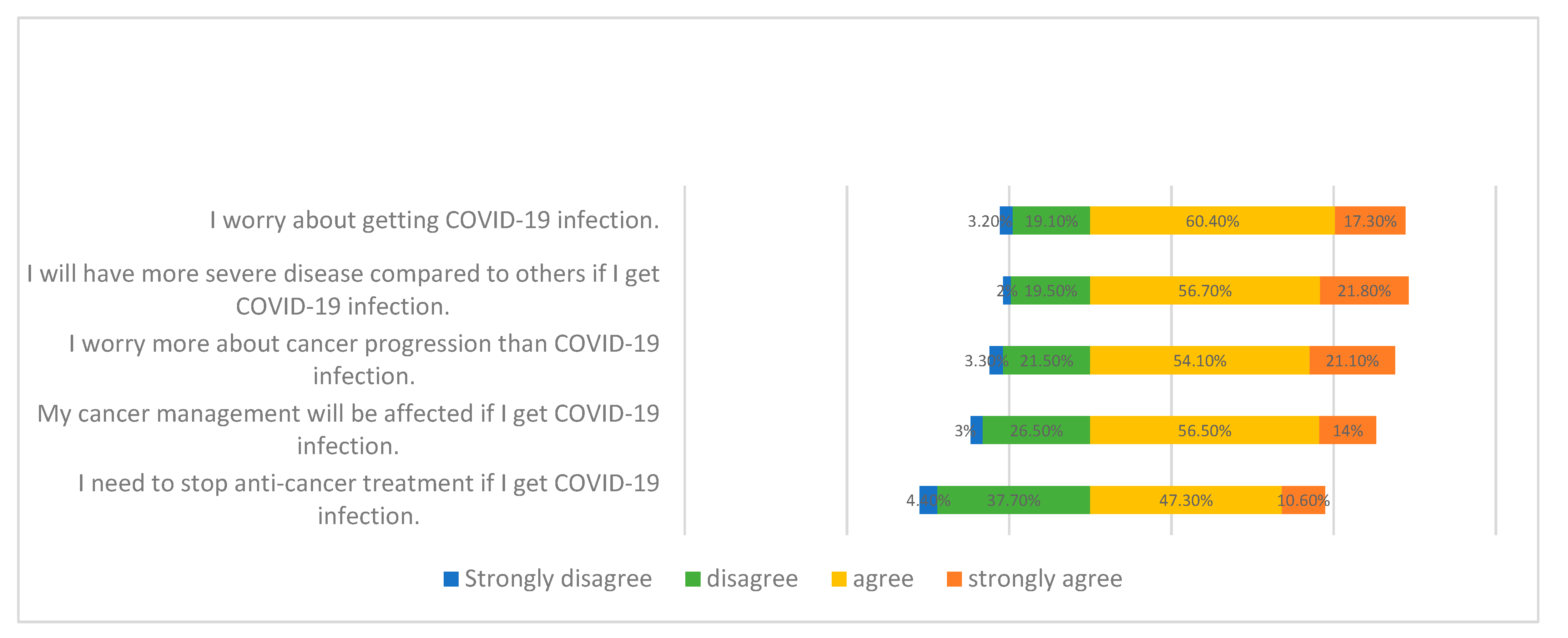
3.2. Perception of COVID-19 Pandemic
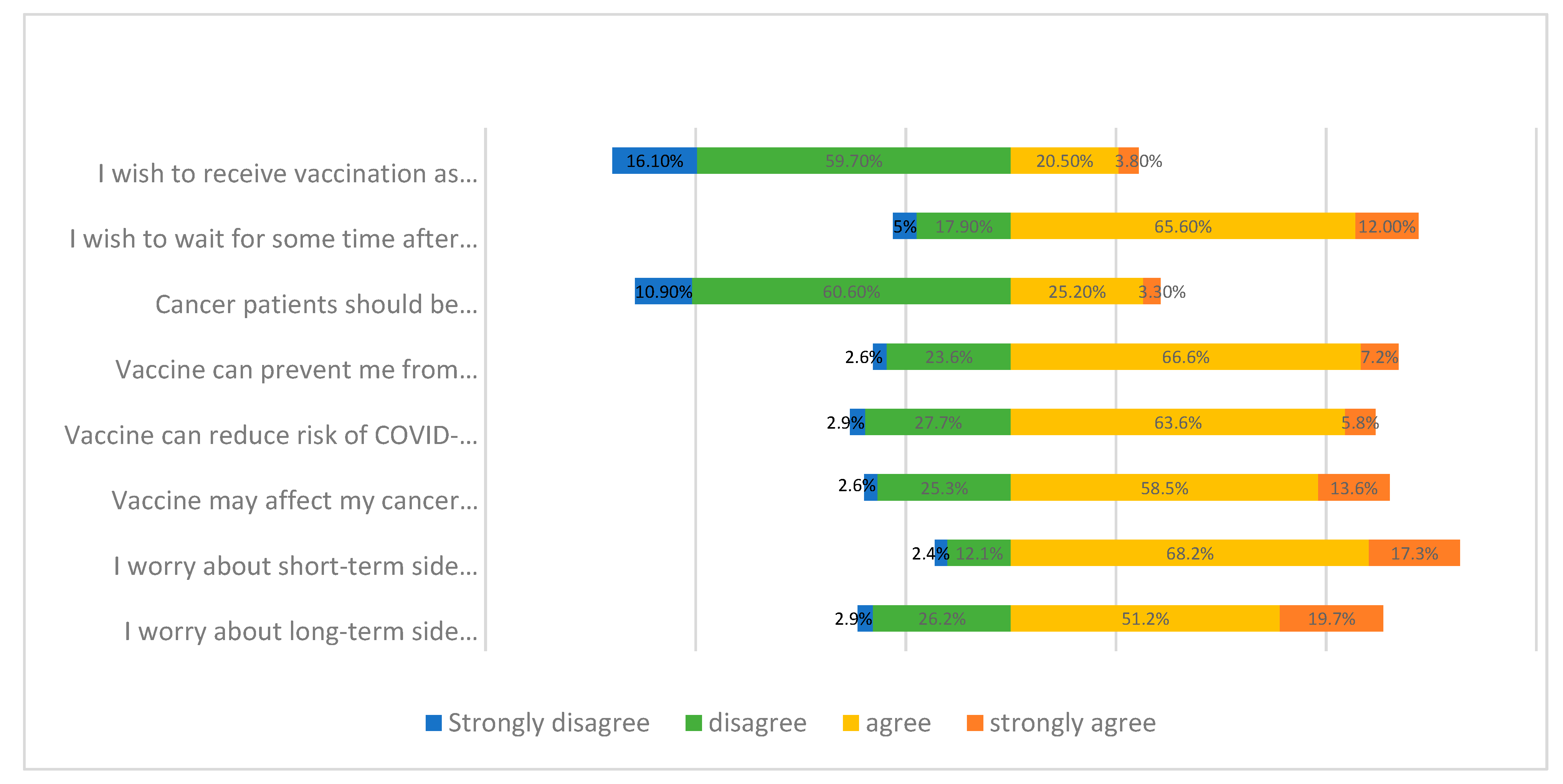
3.3. Concerns about Cancer and COVID-19 Vaccination
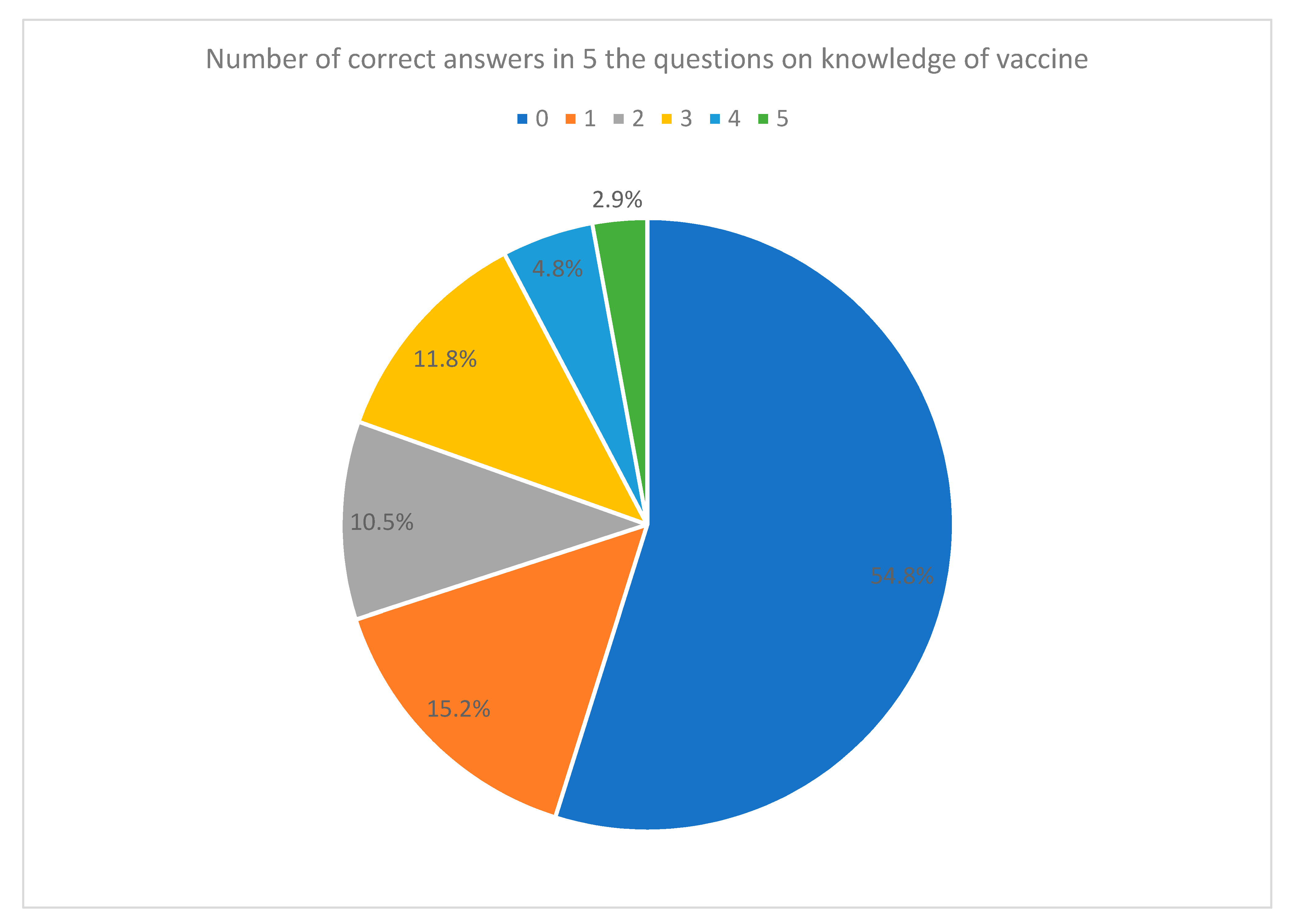
3.4. Basic Knowledge on COVID-19 Vaccination
3.5. Independent Variables Associated with COVID-19 Vaccine Acceptance
3.6. Information Cancer Patients Want to Know
3.7. Vaccine Preference
4. Discussion
4.1. Cancer Patients Should Be Well-Informed about the Risk of COVID-19
4.2. Cancer Patients Should Not Compare COVID-19 Infection with Cancer
4.3. Despite the Limited Efficacy and Safety Data of COVID-19 Vaccines in Cancer Patients, International Health Organisations Already Recommend COVID-19 Vaccines to Cancer Patients Given the Well-Known Knowledge on Other Common Vaccines
4.4. Focused Education on COVID-19 Vaccination Should Be Given to Cancer Patients and Their Care Providers
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A. Participant’s Questionnaire
|
|
- 7.
- Type of Cancer (You can choose more than one answer.):Lung cancerBowel cancerGastric cancer, esophageal cancer, pancreatic cancer, liver cancerBreast cancerHead and neck cancer (including nasopharyngeal cancer)Skin cancerThyroid cancerGynecological cancer includes uterine cancer, cervical cancer, and ovarian cancerUrology cancer includes kidney cancer, bladder cancer, prostate cancerHematological cancers include leukemia and lymphomaSarcomaOthers, please specify: ____________________
- 8.
- Stage of Disease:Stage I–IIIStage IV
- 9.
- Currently receiving (You can choose more than one answer.):Recovered, no further treatmentAnti-cancer systemic treatment (chemotherapy, hormonal therapy, targeted therapy, immunotherapy)RadiotherapyPalliative therapyNot yet received therapy
- 10.
- Did you receive flu vaccination in the past 12 months?YesNo
- 11
- Have you ever felt uncomfortable after vaccination?Yes, please specify: ________________________NoNot applicable
| A Strongly disagree | B Disagree | C Agree | D Strongly agree | |
| (1) I worry about getting COVID-19 infection. | ||||
| (2) I will have more severe disease compared to others if I get COVID-19 infection. | ||||
| (3) I need to stop anti-cancer treatment if I get COVID-19 infection. | ||||
| (4) My cancer management will be affected if I get COVID-19 infection. | ||||
| (5) I worry more about cancer progression than COVID-19 infection. | ||||
| (6) Vaccine can prevent me from COVID-19 infection. | ||||
| (7) Vaccine can reduce risk of COVID-19 complications. | ||||
| (8) I worry that vaccine will affect my anti-cancer treatment. | ||||
| (9) I worry about short-term side effects of vaccine. | ||||
| (10) I worry about long-term side effects of vaccine. | ||||
| (11) I wish to receive vaccination as soon as possible. | ||||
| (12) I wish to wait for some time after vaccine implementation. | ||||
| (13) Cancer patients should be prioritised to have vaccination. |
| A Sinovac | B BioNTech | C AstraZeneca | D Not sure | |
| (1) Which of the following vaccines use “genetically modified messenger RNA (mRNA)” as a technology platform? | ||||
| (2) Which of the following vaccine uses a technical platform that previously known for hepatitis A vaccine? | ||||
| (3) Which of the following vaccines needs to be stored at extremely low temperature (−70 °C) to maintain effectiveness? | ||||
| (4) Which of the following vaccines has serious side effects including transverse myelitis? | ||||
| (5) Which of the following vaccines has a clinical protective effectiveness of 95%? |
- The normal range for hemoglobin for a male is 13.3–17.2 g/dL. Joe’s hemoglobin is 9.7 g/dL. Is Joe within the normal range?YesNo
- A biopsy of a tumor is done to:Remove itDiagnose itTreat it
- If a patient has stage 1 cancer, it means the cancer is:LocalizedIn nearby organsIn distant sites
- The role of a physical therapist is to talk to a patient about emotional needs.TrueFalse
- A tumor is considered “inoperable” when it cannot be treated with:Radiation TherapySurgeryChemotherapy
- Sally will get radiation therapy once a day, Monday through Friday. If Sally has therapy for 4 weeks, how many times will she get radiation therapy?51520
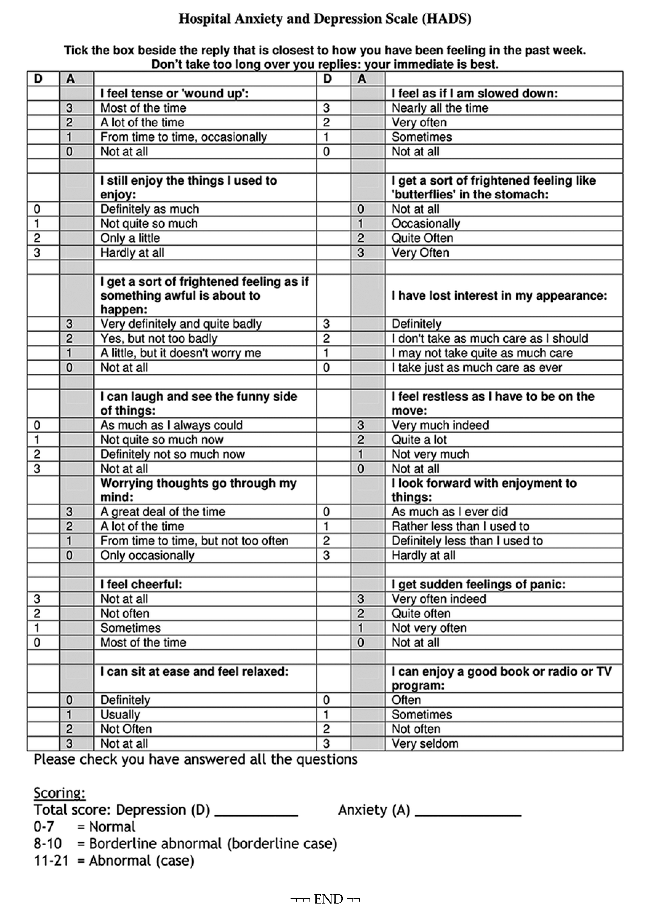
Appendix B. Participant’s Characteristics
| Number | Percentage | |
| Total number of patients | 660 | |
| Gender | ||
| 228 | 34.5% |
| 432 | 65.5% |
| Age | ||
| 51 | 7.7% |
| 130 | 19.7% |
| 177 | 26.8% |
| 188 | 28.5% |
| 114 | 17.3% |
| Marriage | ||
| 103 | 15.6% |
| 470 | 71.2% |
| 59 | 8.9% |
| 28 | 4.2% |
| Education | ||
| 104 | 15.8% |
| 308 | 46.7% |
| 59 | 8.9% |
| 189 | 28.6% |
| Employment status | ||
| 245 | 37.1% |
| 237 | 35.9% |
| 120 | 18.2% |
| 58 | 8.8% |
| Medical insurance | ||
| 283 | 42.9% |
| Type of cancer | ||
| 114 | 17.3% |
| 154 | 23.3% |
| 192 | 29.1% |
| 88 | 13.3% |
| 46 | 7.0% |
| 30 | 4.5% |
| 7 | 1.1% |
| 29 | 4.4% |
| Stage of disease | ||
| 276 | 41.8% |
| 384 | 58.2% |
| Currently on anticancer systemic treatment | ||
| 204 | 30.9% |
| 456 | 69.1% |
| Received flu vaccine in the past 12 months | ||
| 141 | 21.4% |
| Had discomfort after flu vaccine? | ||
| 41 | 6.2% |
References
- COVID-19 Coronavirus Pandemic. Available online: https://www.worldometers.info/coronavirus/ (accessed on 31 May 2021).
- The Government of Hong Kong Special Administrative Region. COVID Vaccine. Available online: https://www.covidvaccine.gov.hk/en/ (accessed on 31 May 2021).
- Wong, M.C.S.; Wong, E.L.Y.; Huang, J.; Cheung, A.W.L.; Law, K.; Chong, M.K.C.; Ng, R.W.Y.; Lai, C.K.C.; Boon, S.S.; Lau, J.T.F.; et al. Acceptance of the COVID-19 vaccine based on the health belief model: A population-based survey in Hong Kong. Vaccine 2021, 39, 1148–1156. [Google Scholar] [CrossRef] [PubMed]
- Consensus Interim Recommendations on the Use of COVID-19 Vaccines in Hong Kong (As of Jan 7, 2021). Scientific Committee on Emerging and Zoonotic Disease and Scientific Committee on Vaccine Preventable Diseases. Available online: https://www.chp.gov.hk/files/pdf/consensus_interim_recommendations_on_the_use_of_covid19_vaccines_inhk.pdf (accessed on 31 May 2021).
- Giannakoulis, V.G.; Papoutsi, E.; Siempos, I.I. Effect of cancer on clinical outcomes of patients with COVID-19: A meta-analysis of patient data. JCO Glob. Oncol. 2020, 6, 799–808. [Google Scholar] [CrossRef] [PubMed]
- Monin, L.; Laing, A.G.; Muñoz-Ruiz, M.; McKenzie, D.R.; Del Molino Del Barrio, I.; Alaguthurai, T.; Domingo-Vila, C.; Hayday, T.S.; Graham, C.; Seow, J.; et al. Safety and immunogenicity of one versus two doses of the COVID-19 vaccine BNT162b2 for patients with cancer: Interim analysis of a prospective observational study. Lancet Oncol. 2021. [Google Scholar] [CrossRef]
- Dumenci, L.; Matsuyama, R.; Riddle, D.L.; Cartwright, L.A.; Perera, R.A.; Chung, H.; Siminoff, L.A. Measurement of cancer health literacy and identification of patients with limited cancer health literacy. J. Health Commun. 2014, 19, 205–224. [Google Scholar] [CrossRef] [PubMed]
- Annunziata, M.A.; Muzzatti, B.; Bidoli, E.; Flaiban, C.; Bomben, F.; Piccinin, M.; Gipponi, K.M.; Mariutti, G.; Busato, S.; Mella, S. Hospital Anxiety and Depression Scale (HADS) accuracy in cancer patients. Support Care Cancer 2020, 28, 3921–3926. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Berger, N.A.; Xu, R. Analyses of risk, racial disparity, and outcomes among US patients with cancer and COVID-19 infection. JAMA Oncol. 2021, 7, 220–227. [Google Scholar] [CrossRef] [PubMed]
- Yu, J.; Ouyang, W.; Chua, M.L.K.; Xie, C. SARS-CoV-2 transmission in patients with cancer at a tertiary care hospital in Wuhan, China. JAMA Oncol. 2020, 6, 1108–1110. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rogado, J.; Obispo, B.; Pangua, C.; Serrano-Montero, G.; Martín Marino, A.; Pérez-Pérez, M.; López-Alfonso, A.; Gullón, P.; Lara, M.Á. COVID-19 transmission, outcome and associated risk factors in cancer patients at the first month of the pandemic in a Spanish hospital in Madrid. Clin. Transl. Oncol. 2020, 22, 2364–2368. [Google Scholar] [CrossRef] [PubMed]
- Liang, W.; Guan, W.; Chen, R.; Wang, W.; Li, J.; Xu, K.; Li, C.; Ai, Q.; Lu, W.; Liang, H.; et al. Cancer patients in SARS-CoV-2 infection: A nationwide analysis in China. Lancet Oncol. 2020, 21, 335–337. [Google Scholar] [CrossRef]
- Kuderer, N.M.; Choueiri, T.K.; Shah, D.P.; Shyr, Y.; Rubinstein, S.M.; Rivera, D.R.; Shete, S.; Hsu, C.Y.; Desai, A.; de Lima Lopes, G., Jr.; et al. COVID-19 and Cancer Consortium. Clinical impact of COVID-19 on patients with cancer (CCC19): A cohort study. Lancet 2020, 395, 1907–1918. [Google Scholar] [CrossRef]
- Halpin, S.J.; McIvor, C.; Whyatt, G.; Adams, A.; Harvey, O.; McLean, L.; Walshaw, C.; Kemp, S.; Corrado, J.; Singh, R.; et al. Postdischarge symptoms and rehabilitation needs in survivors of COVID-19 infection: A cross-sectional evaluation. J. Med. Virol. 2021, 93, 1013–1022. [Google Scholar] [CrossRef] [PubMed]
- Carfì, A.; Bernabei, R.; Landi, F. Gemelli Against COVID-19 Post-Acute Care Study Group. Persistent Symptoms in Patients After Acute COVID-19. JAMA 2020, 324, 603–605. [Google Scholar] [CrossRef] [PubMed]
- Puntmann, V.O.; Carerj, M.L.; Wieters, I.; Fahim, M.; Arendt, C.; Hoffmann, J.; Shchendrygina, A.; Escher, F.; Vasa-Nicotera, M.; Zeiher, A.M.; et al. Outcomes of Cardiovascular Magnetic Resonance Imaging in Patients Recently Recovered From Coronavirus Disease 2019 (COVID-19). JAMA Cardiol. 2020, 5, 1265–1273. [Google Scholar] [CrossRef] [PubMed]
- Grist, J.T.; Chen, M.; Collier, G.J.; Raman, B.; AbuEid, G.; McIntyre, A.; Matthews, V.; Fraser, E.; Ho, L.P.; Wild, J.M.; et al. Hyperpolarized (129)Xe MRI Abnormalities in Dyspneic Participants 3 Months after COVID-19 Pneumonia: Preliminary Results. Radiology 2021, 210033. [Google Scholar] [CrossRef] [PubMed]
- Polack, F.P.; Thomas, S.J.; Kitchin, N.; Absalon, J.; Gurtman, A.; Lockhart, S.; Perez, J.L.; Pérez Marc, G.; Moreira, E.D.; Zerbini, C.; et al. Safety and efficacy of the BNT162b2 mRNA Covid-19 vaccine. N. Engl. J. Med. 2020, 383, 2603–2615. [Google Scholar] [CrossRef] [PubMed]
- National Comprehensive Cancer Network. Preliminary recommendations of the NCCN COVID-19 Vaccination Advisory Committee* Version 2.0 3/10/2021. NCCN. Available online: https://www.nccn.org/docs/default-source/covid-19/2021_covid-19_vaccination_guidance_v2-0.pdf?sfvrsn=b483da2b_2 (accessed on 31 May 2021).
- SEOM. Update on the Positioning and Recommendations of SEOM in Relation to the Vaccination Campaign Against COVID-19 in Cancer Patients. Posicionamiento y recomendaciones de seom en relació n con la campaña de vacunación frente ll Covid-19 en pacientes con cáncer [Spanish]. Sociedad Española de Oncología Médica. Available online: https://seom.org/images/Posicionamiento_SEOM_vacunacion_COVID19_pacientes_con_cancer.pdf (accessed on 31 May 2021).
- ESMO Statements for Vaccination against COVID-19 in Patients with Cancer. Available online: https://www.esmo.org/covid-19-and-cancer/covid-19-vaccination (accessed on 31 May 2021).
- MSK COVID-19 Vaccine Interim Guidelines for Cancer Patients. Available online: https://www.asco.org/sites/new-www.asco.org/files/content-files/covid-19/2021-MSK-COVID19-VACCINE-GUIDELINES.pdf (accessed on 31 May 2021).
- Cancer Research UK. A Study Looking at COVID-19 and People Who Have Cancer (SOAP). Available online: https://www.cancerresearchuk.org/about-cancer/find-a-clinical-trial/a-study-looking-at-covid-19-and-people-who-have-cancer-soap#undefined (accessed on 31 May 2021).
| Variables | Total | Participants Likely to Get a COVID-19 Vaccine | Odds Ratio | 95% C.I. | p-Value | |||
|---|---|---|---|---|---|---|---|---|
| N = 660 | N = 118 | |||||||
| 17.9% | ||||||||
| n | % | n (%) | Lower | Upper | ||||
| Gender | ||||||||
| Men | 228 | 34.5% | 54 | (23.7) | ref | |||
| Women | 432 | 65.5% | 64 | (14.8) | 0.56 | 0.37 | 0.84 | 0.005 |
| Age | ||||||||
| 18–60 | 358 | 54.2% | 58 | (16.2) | ref | |||
| ≥61 | 302 | 45.8% | 60 | (19.9) | 1.28 | 0.861 | 1.911 | 0.221 |
| Marital status | ||||||||
| Not married | 190 | 28.8% | 37 | (19.5) | ref | |||
| Married | 470 | 71.2% | 81 | (17.2) | 0.86 | 0.56 | 1.33 | 0.497 |
| Employment status | ||||||||
| Not working | 415 | 62.9% | 73 | (17.6) | ref | |||
| Working | 245 | 37.1% | 45 | (18.4) | 1.05 | 0.699 | 1.59 | 0.801 |
| Education | ||||||||
| Below tertiary level | 412 | 62.4% | 79 | (19.2) | ref | |||
| Tertiary level or above | 248 | 37.6% | 39 | (15.7) | 0.79 | 0.52 | 1.20 | 0.263 |
| Medical insurance | ||||||||
| No | 377 | 57.1% | 78 | (20.7) | ref | |||
| Yes | 283 | 42.9% | 40 | (14.1) | 0.63 | 0.42 | 0.96 | 0.030 |
| Stage of disease | ||||||||
| Stage I–III | 276 | 41.8% | 52 | (18.8) | ref | |||
| Stage IV | 384 | 58.2% | 66 | (17.2) | 0.90 | 0.60 | 1.34 | 0.585 |
| Currently on anticancer systemic treatment | ||||||||
| No (Radiotherapy/survivors/palliative care) | 204 | 30.9% | 43 | (21.1) | ref | |||
| Yes (On anticancer systemic treatment) | 456 | 69.1% | 75 | (16.4) | 0.74 | 0.49 | 1.12 | 0.151 |
| Flu vaccination in the past 12 months | ||||||||
| No | 519 | 78.6% | 91 | (17.5) | ref | |||
| Yes | 141 | 21.4% | 27 | (19.1) | 1.11 | 0.69 | 1.79 | 0.657 |
| CHLT-6 score | 0.79 | 0.68 | 0.91 | 0.001 | ||||
| HADS Depression score | ||||||||
| Normal/ borderline abnormal (score <11) | 458 | 69.4% | 94 | (20.5) | ref | |||
| Abnormal (score ≥11) | 202 | 30.6% | 24 | (11.9) | 0.52 | 0.32 | 0.85 | 0.008 |
| HADS Anxiety score | ||||||||
| Normal/ borderline abnormal (score <11) | 607 | 92.0% | 108 | (17.8) | ref | |||
| Abnormal (score ≥11) | 53 | 8.0% | 10 | (18.9) | 1.08 | 0.52 | 2.21 | 0.845 |
| Variables | Total | Participants Likely to Get a COVID-19 Vaccine | Odds Ratio | 95% C.I. | p-Value | ||
|---|---|---|---|---|---|---|---|
| N = 660 | N = 118 | ||||||
| 17.9% | |||||||
| n | n (%) | Lower | Upper | ||||
| Gender | |||||||
| Men | 228 | 54 | (23.7) | ref | |||
| Women | 432 | 64 | (14.8) | 0.70 | 0.45 | 1.09 | 0.115 |
| Age | |||||||
| 18–60 | 358 | 58 | (16.2) | ref | |||
| >61 | 302 | 60 | (19.9) | 0.93 | 0.59 | 1.47 | 0.746 |
| Medical insurance | |||||||
| No | 377 | 78 | (20.7) | ref | |||
| Yes | 283 | 40 | (14.1) | 0.65 | 0.41 | 1.04 | 0.071 |
| Stage of disease | |||||||
| Stage I–III | 276 | 52 | (18.8) | ref | |||
| Stage IV | 384 | 66 | (17.2) | 0.81 | 0.51 | 1.30 | 0.383 |
| Currently on anticancer systemic treatment | |||||||
| No (Radiotherapy/survivors/palliative care) | 204 | 43 | (21.1) | ref | |||
| Yes (On anticancer systemic treatment) | 456 | 75 | (16.4) | 0.62 | 0.38 | 1.01 | 0.056 |
| Worry about getting COVID-19 infection | |||||||
| No | 147 | 28 | (19.0) | ref | |||
| Yes | 513 | 90 | (17.5) | 1.12 | 0.65 | 1.92 | 0.692 |
| Worry more about cancer progression than COVID-19 infection | |||||||
| No | 163 | 32 | (19.6) | ref | |||
| Yes | 497 | 86 | (17.3) | 0.84 | 0.50 | 1.40 | 0.497 |
| Believe that COVID-19 vaccine can prevent COVID-19 infection | |||||||
| No | 173 | 14 | (8.1) | ref | |||
| Yes | 487 | 104 | (21.4) | 2.97 | 1.59 | 5.56 | 0.001 |
| Worry that COVID-19 vaccine will affect cancer treatment | |||||||
| No | 184 | 38 | (20.7) | ref | |||
| Yes | 476 | 80 | (16.8) | 1.09 | 0.65 | 1.84 | 0.733 |
| Worry about short-term side effects of vaccine | |||||||
| No | 96 | 20 | (20.8) | ref | |||
| Yes | 564 | 98 | (17.4) | 1.31 | 0.67 | 2.54 | 0.431 |
| Worry about long-term side effects of vaccine | |||||||
| No | 192 | 53 | (27.6) | ref | |||
| Yes | 468 | 65 | (13.9) | 0.46 | 0.28 | 0.76 | 0.002 |
| CHLT-6 score | 0.75 | 0.64 | 0.89 | 0.001 | |||
| HADS Depression score | |||||||
| Normal/borderline abnormal (score <11) | 458 | 94 | (20.5) | ref | |||
| Abnormal (score ≥11) | 202 | 24 | (11.9) | 0.49 | 0.29 | 0.82 | 0.007 |
| HADS Anxiety score | |||||||
| Normal/borderline abnormal (score <11) | 607 | 108 | (17.8) | ref | |||
| Abnormal (score ≥11) | 53 | 10 | (18.9) | 0.66 | 0.29 | 1.50 | 0.325 |
| Variables | Total | Participants Have Preference on Type of Vaccine | Odds Ratio | 95% C.I. | p-Value | ||
|---|---|---|---|---|---|---|---|
| N = 660 | N = 376 | ||||||
| 57.0% | |||||||
| n | n (%) | Lower | Upper | ||||
| Gender | |||||||
| Men | 228 | 132 | (57.9) | ref | |||
| Women | 432 | 244 | (56.5) | 0.68 | 0.47 | 0.97 | 0.038 |
| Age | |||||||
| 18–60 | 358 | 219 | (61.2) | ref | |||
| >61 | 302 | 157 | (52.0) | 0.80 | 0.57 | 1.15 | 0.216 |
| Medical insurance | |||||||
| No | 377 | 201 | (55.3) | ref | |||
| Yes | 283 | 175 | (61.8) | 1.19 | 0.83 | 1.69 | 0.340 |
| Stage of disease | |||||||
| Stage I–III | 276 | 145 | (52.5) | ref | |||
| Stage IV | 384 | 231 | (60.2) | 1.23 | 0.86 | 1.75 | 0.261 |
| Currently on anticancer systemic treatment | |||||||
| No (Radiotherapy/survivors/palliative care) | 204 | 133 | (65.2) | ref | |||
| Yes (On anticancer systemic treatment) | 456 | 243 | (53.3) | 0.66 | 0.45 | 0.98 | 0.038 |
| Worry about getting COVID-19 infection | |||||||
| No | 147 | 76 | (51.7) | ref | |||
| Yes | 513 | 300 | (58.5) | 1.09 | 0.71 | 1.67 | 0.683 |
| Worry more about cancer progression than COVID-19 infection | |||||||
| No | 163 | 96 | (58.9) | ref | |||
| Yes | 497 | 280 | (56.3) | 0.98 | 0.66 | 1.48 | 0.938 |
| Believe that COVID-19 vaccine can prevent COVID-19 infection | |||||||
| No | 173 | 92 | (53.2) | ref | |||
| Yes | 487 | 284 | (58.3) | 1.16 | 0.79 | 1.70 | 0.454 |
| Worry that COVID-19 vaccine will affect cancer treatment | |||||||
| No | 184 | 111 | (60.3) | ref | |||
| Yes | 476 | 265 | (55.7) | 0.87 | 0.57 | 1.32 | 0.508 |
| Worry about short-term side effects of vaccine | |||||||
| No | 96 | 51 | (53.1) | ref | |||
| Yes | 564 | 325 | (57.6) | 1.39 | 0.81 | 2.39 | 0.235 |
| Worry about long-term side effects of vaccine | |||||||
| No | 192 | 107 | (55.7) | ref | |||
| Yes | 468 | 269 | (57.5) | 1.28 | 0.83 | 1.95 | 0.263 |
| CHLT-6 score | 1.23 | 1.07 | 1.41 | 0.004 | |||
| Knowledge about vaccine | 1.38 | 1.21 | 1.57 | 0.001 | |||
| HADS Depression score | |||||||
| Normal/borderline abnormal (score <11) | 458 | 277 | (60.5) | ref | |||
| Abnormal (score ≥11) | 202 | 99 | (49.0) | 0.64 | 0.44 | 0.92 | 0.015 |
| HADS Anxiety score | |||||||
| Normal/borderline abnormal (score <11) | 607 | 346 | (57.0) | ref | |||
| Abnormal (score ≥11) | 53 | 30 | (56.6) | 0.78 | 0.42 | 1.45 | 0.430 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chan, W.-L.; Ho, Y.-H.T.; Wong, C.K.-H.; Choi, H.C.-W.; Lam, K.-O.; Yuen, K.-K.; Kwong, D.; Hung, I. Acceptance of COVID-19 Vaccination in Cancer Patients in Hong Kong: Approaches to Improve the Vaccination Rate. Vaccines 2021, 9, 792. https://doi.org/10.3390/vaccines9070792
Chan W-L, Ho Y-HT, Wong CK-H, Choi HC-W, Lam K-O, Yuen K-K, Kwong D, Hung I. Acceptance of COVID-19 Vaccination in Cancer Patients in Hong Kong: Approaches to Improve the Vaccination Rate. Vaccines. 2021; 9(7):792. https://doi.org/10.3390/vaccines9070792
Chicago/Turabian StyleChan, Wing-Lok, Yuen-Hung Tricia Ho, Carlos King-Ho Wong, Horace Cheuk-Wai Choi, Ka-On Lam, Kwok-Keung Yuen, Dora Kwong, and Ivan Hung. 2021. "Acceptance of COVID-19 Vaccination in Cancer Patients in Hong Kong: Approaches to Improve the Vaccination Rate" Vaccines 9, no. 7: 792. https://doi.org/10.3390/vaccines9070792
APA StyleChan, W.-L., Ho, Y.-H. T., Wong, C. K.-H., Choi, H. C.-W., Lam, K.-O., Yuen, K.-K., Kwong, D., & Hung, I. (2021). Acceptance of COVID-19 Vaccination in Cancer Patients in Hong Kong: Approaches to Improve the Vaccination Rate. Vaccines, 9(7), 792. https://doi.org/10.3390/vaccines9070792







