A Mixed-Methods Study to Evaluate Elementary School Staff’s Acceptability, Delivery Challenges, and Communication Regarding the Implementation of School-Located Influenza Vaccination Program in Hong Kong
Abstract
:1. Introduction
1.1. The Hong Kong Context
1.2. Study Objectives
- What were the attitudes about and intention to initiate or continue the implementation of SIVP among elementary school staff?
- What were the delivery challenges experienced by school staff over the past two years of program implementation?
- How were SIVP communicated with parents and students via schools, and how was the consent process implemented?
2. Materials and Methods
2.1. Participants and Data Collection
2.1.1. Questionnaire-Based Survey
2.1.2. In-Depth Interviews
2.1.3. Retrieving School Newsletters
2.2. Data Analysis
3. Results
3.1. Questionnaire-Based Survey
3.2. In-Depth Interviews
3.2.1. Acceptability of SIVP
3.2.2. Challenges in Program Delivery
3.2.3. Communication with Parents and Students about SIVP
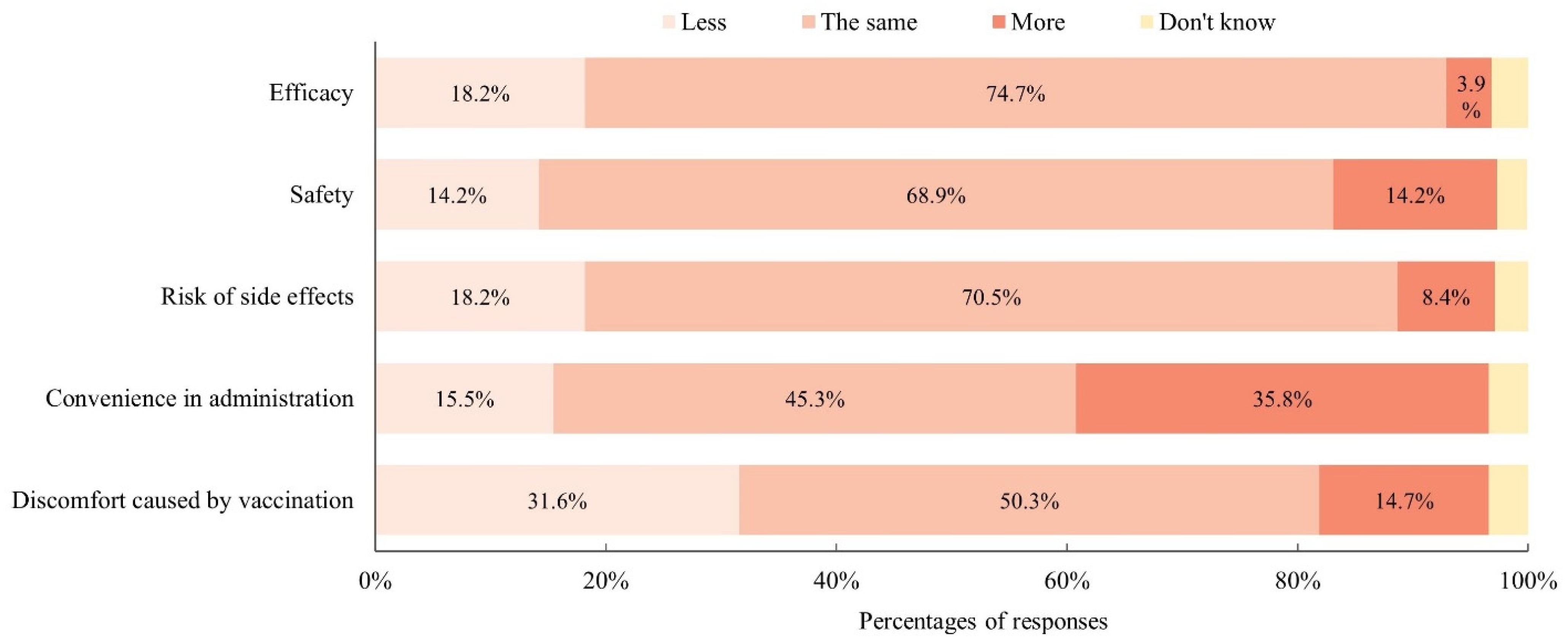
3.2.4. Preference for Type of Influenza Vaccine
3.3. Content Analysis of School Newsletters about SIVP
4. Discussion
5. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Somes, M.P.; Turner, R.M.; Dwyer, L.J.; Newall, A.T. Estimating the annual attack rate of seasonal influenza among unvaccinated individuals: A systematic review and meta-analysis. Vaccine 2018, 36, 3199–3207. [Google Scholar] [CrossRef]
- Lafond, K.E.; Nair, H.; Rasooly, M.H.; Valente, F.; Booy, R.; Rahman, M.; Kitsutani, P.; Yu, H.; Guzman, G.; Coulibaly, D.; et al. Global role and burden of influenza in pediatric respiratory hospitalizations, 1982–2012: A Systematic Analysis. PLoS Med. 2016, 13, 1001977. [Google Scholar] [CrossRef] [Green Version]
- Lau, Y.L.; Wong, W.H.S.; Hattangdi-Haridas, S.R.; Chow, C.B. Evaluating impact of school outreach vaccination programme in Hong Kong influenza season 2018–2019. Hum. Vaccines Immunother. 2020, 16, 823–826. [Google Scholar] [CrossRef] [Green Version]
- Gallagher, N.; Jessop, L.; Sartaj, M.; Johnston, J. Impact of live attenuated influenza vaccination programme for healthy children in Northern Ireland: A comparison of seven influenza seasons. Vaccine 2018, 36, 521–526. [Google Scholar] [CrossRef]
- Yin, J.K.; Heywood, A.E.; Georgousakis, M.; King, C.; Chiu, C.; Isaacs, D.; Macartney, K.K. Systematic review and meta-analysis of indirect protection afforded by vaccinating children against seasonal influenza: Implications for policy. Clin. Infect. Dis. 2017, 65, 719–728. [Google Scholar] [CrossRef]
- Benjamin-Chung, J.; Arnold, B.F.; Kennedy, C.J.; Mishra, K.; Pokpongkiat, N.; Nguyen, A.; Jilek, W.; Holbrook, K.; Pan, E.; Kirley, P.D. Evaluation of a city-wide school-located influenza vaccination program in Oakland, California, with respect to vaccination coverage, school absences, and laboratory-confirmed influenza: A matched cohort study. PLoS Med. 2020, 17, e1003238. [Google Scholar] [CrossRef]
- Pebody, R.G.; Sinnathamby, M.A.; Warburton, F.; Andrews, N.; Boddington, N.L.; Zhao, H.; Yonova, I.; Ellis, J.; Tessier, E.; Donati, M.; et al. Uptake and impact of vaccinating primary school-age children against influenza: Experiences of a live attenuated influenza vaccine programme, England, 2015/16. Eurosurveillance 2018, 23, 1700496. [Google Scholar] [CrossRef]
- Williams, V.; Rousculp, M.D.; Price, M.; Coles, T.; Therrien, M.; Griffin, J. Elementary school-located influenza vaccine pro-grams: Key stakeholder experiences from initiation to continuation. J. Sch. Nurs. 2012, 28, 256–267. [Google Scholar] [CrossRef] [Green Version]
- Schieber, R.A.; Kennedy, A.; Kahn, E.B. Early experience conducting school-located vaccination programs for seasonal influenza. Pediatrics 2012, 129. [Google Scholar] [CrossRef] [Green Version]
- Allison, M.A.; Reyes, M.; Young, P.; Calame, L.; Sheng, X.; Weng, H.-Y.C.; Byington, C.L. Parental Attitudes About Influenza Immunization and School-Based Immunization for School-Aged Children. Pediatr. Infect. Dis. J. 2010, 29, 751–755. [Google Scholar] [CrossRef]
- Herlitz, L.; MacIntyre, H.; Osborn, T.; Bonell, C. The sustainability of public health interventions in schools: A systematic review. Implement. Sci. 2020, 15, 1–28. [Google Scholar] [CrossRef]
- Kwong, K.L.; Lung, D.; Nin Wong, S.; Que, T.L.; Kwong, N.S. Influenza-related hospitalisations in children. J. Paediatr. Child. Heal. 2009, 45, 660–664. [Google Scholar] [CrossRef]
- Chiu, S.S.; Chan, K.-H.; So, L.Y.; Chen, R.; Chan, E.L.Y.; Peiris, J.S.M. The population based socioeconomic burden of pediatric influenza-associated hospitalization in Hong Kong. Vaccine 2012, 30, 1895–1900. [Google Scholar] [CrossRef]
- Department of Health; The Government of the Hong Kong Special Administrative Region. Seasonal Influenza Vaccination School Outreach. 2021. Available online: https://www.chp.gov.hk/en/features/100634.html (accessed on 28 May 2021).
- Hong Kong Department of Health. Statistics on Vaccination Programmes in the Past 3 years. Hong Kong, China; 2021. Available online: https://www.chp.gov.hk/en/features/102226.html (accessed on 28 May 2021).
- Boddington, N.L.; Pearson, I.; Whitaker, H.; Mangtani, P.; Pebody, R.G. Effectiveness of influenza vaccination in preventing hospitalisation due to influenza in children: A systematic review and meta-analysis. Clin. Inf. Dis. 2021, 27. [Google Scholar] [CrossRef]
- Santibanez, T.A.; Kahn, K.E.; Bridges, C.B. Do parents prefer inactivated or live attenuated influenza vaccine for their children? Vaccine 2018, 36, 7300–7305. [Google Scholar] [CrossRef] [PubMed]
- Sreenivasan, M.V.; He, H.H.; Park, S.Y. Administration time between seasonal live-attenuated influenza vaccine and trivalent influenza vaccine during the “Stop Flu at School” campaign—Hawaii. Pub. Health Rep. 2014, 129, 229–236. [Google Scholar] [CrossRef]
- Kassianos, G.; MacDonald, P.; Aloysius, I.; Reynolds, A.J.V. Implementation of the United Kingdom’s childhood influenza national vaccination programme: A review of clinical impact and lessons learned over six influenza seasons. Vaccine 2020, 38, 5747–5758. [Google Scholar] [CrossRef]
- Kwong, J.C.; Pereira, J.A.; Quach, S.; Pellizzari, R.; Dusome, E.; Russell, M.L. Randomized evaluation of live attenuated vs. in-activated influenza vaccines in schools (RELATIVES) pilot study: A cluster randomized trial. Vaccine 2015, 33, 535–541. [Google Scholar] [CrossRef] [Green Version]
- National Center for Immunization and Respiratory Diseases. Vaccine Information Statements. 2011. Available online: https://www.cdc.gov/flu/school/slv/support.htm (accessed on 30 May 2021).
- Hull, H.F.; Ambrose, C.S. Current experience with school-located influenza vaccination programs in the United States: A re-view of the medical literature. Hum. Vaccin. 2011, 7, 153–160. [Google Scholar] [CrossRef] [Green Version]
- The Government of the Hong Kong Special Administrative Region. 2019–2020 seasonal influenza vaccination programmes to be launched in October 2019. Available online: https://www.info.gov.hk/gia/general/201907/17/P2019071600660.htm?fontSize=1 (accessed on 30 May 2021).
- National Association of County and City Health Officials. Influenza School-Located Vaccination (SLV): Information for Planners. 2011. Available online: https://www.cdc.gov/flu/pdf/school/SLV_information.pdf. (accessed on 28 May 2021).
- National Association of School Nurses. School-Located Vaccination (Position Statement). 2017. Available online: https://www.nasn.org/advocacy/professional-practice-documents/position-statements/ps-slv (accessed on 30 May 2021).
- Lee, R.L. The role of school nurses in delivering accessible health services for primary and secondary school students in Hong Kong. J. Clin. Nurs. 2011, 20, 2968–2977. [Google Scholar] [CrossRef]
- Lee, R.L.; Loke, A.Y.; Wu, C.S.; Ho, A.P. The lifestyle behaviours and psychosocial well-being of primary school students in Hong Kong. J. Clin. Nurs. 2010, 19, 1462–1472. [Google Scholar] [CrossRef] [PubMed]
- Sugaya, N.; Shinjoh, M.; Nakata, Y.; Tsunematsu, K.; Yamaguchi, Y.; Komiyama, O.; Takahashi, H.; Mitamura, K.; Narabayashi, A.; Takahashi, T. Three-season effectiveness of inactivated influenza vaccine in preventing influenza illness and hospitalization in children in Japan, 2013–2016. Vaccine 2018, 36, 1063–1071. [Google Scholar] [CrossRef]
- Sohn, Y.J.; Choi, J.H.; Choi, Y.Y.; Choe, Y.J.; Kim, K.; Kim, Y.K. Effectiveness of trivalent inactivated influenza vaccines in children during 2017–2018 season in Korea: Comparison of test-negative analysis by rapid and RT-PCR influenza tests. Int. J. Infect. Dis. 2020, 99, 199–203. [Google Scholar] [CrossRef] [PubMed]
- Ishiwada, N.; Suzuki, C.; Hasebe, S.; Tsuchiya, A.; Takeuchi, N.; Hishiki, H.; Sato, Y.; Sugita, K. The effects of health education on health science teachers’ intention to recommend adolescent HPV vaccine for female students in Japan. Hum. Vaccines Immunother. 2020, 16, 2752–2757. [Google Scholar] [CrossRef] [PubMed]
- McHugh, M.L. Interrater reliability: The kappa statistic. Biochem. Med. (Zagreb) 2012, 22, 276–282. [Google Scholar] [CrossRef] [PubMed]
- Protzel, B.P.; Orenstein, W.A.; Hinman, A.R.; Gazmararian, J. Stakeholder attitudes toward influenza vaccination policy in the United States. Health Promot. Pract. 2009, 11, 807–816. [Google Scholar] [CrossRef]
- Cummings, G.E.; Ruff, E.; Guthrie, S.H.; Hoffmaster, M.A.; Leitch, L.L.; King, J.C. Successful use of volunteers to conduct school-located mass influenza vaccination clinics. Pediatrics 2012, 129, S88–S95. [Google Scholar] [CrossRef] [Green Version]
- Cawley, J.; Hull, H.F.; Rousculp, M.D. Strategies for implementing school-located influenza vaccination of children: A systematic literature review. J. Sch. Health. 2010, 80, 167–175. [Google Scholar] [CrossRef]
- Alsuhaibani, M.; Alaqeel, A. Impact of the COVID-19 pandemic on routine childhood immunization in Saudi Arabia. Vaccines 2020, 8, 581. [Google Scholar] [CrossRef]
- Perman, S.; Turner, S.; Ramsay, A.I.G.; Baim-Lance, A.; Utley, M.; Fulop, N.J. School-based vaccination programmes: A systematic review of the evidence on organisation and delivery in high income countries. BMC Public Health 2017, 17, 1–11. [Google Scholar] [CrossRef]
- Keren, R.; Zaoutis, T.E.; Bridges, C.B.; Herrera, G.; Watson, B.M.; Wheeler, A.B.; Licht, D.J.; Luan, X.Q.; Coffin, S.E. Neurological and neuromuscular disease as a risk factor for respiratory failure in children hospitalized with influenza infection. JAMA 2005, 294, 2188–2194. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- McLenon, J.; Rogers, M.A. The fear of needles: A systematic review and meta-analysis. J. Adv. Nurs. 2018, 75, 30–42. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reiss, D.R.; Karako-Eyal, N. Informed consent to vaccination: Theoretical, legal, and empirical insights. Am. J. Law Med. 2019, 45, 357–419. [Google Scholar] [CrossRef] [PubMed]
- Kata, A. A postmodern Pandora’s box: Anti-vaccination misinformation on the Internet. Vaccine 2010, 28, 1709–1716. [Google Scholar] [CrossRef] [PubMed]
- Weinberg, A.G. Nontraditional uses of live attenuated influenza vaccine: School-located influenza vaccination. J. Pediatr. Infect. Dis. Soc. 2020, 9, S19–S23. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | N (%) |
|---|---|
| Sex | |
| Female | 299 (78.7) |
| Male | 70 (18.4) |
| Missing | 11 (2.9) |
| Age group (years) | |
| 18–24 | 9 (2.4) |
| 25–34 | 123 (32.4) |
| 35–44 | 125 (32.9) |
| 45–54 | 86 (22.6) |
| 55 or above | 25 (6.6) |
| Missing | 12 (3.2) |
| Marital status | |
| Single | 151 (39.7) |
| Married | 218 (57.4) |
| Divorced/Separated/Widowed | 5 (1.4) |
| Missing | 6 (1.6) |
| Educational attainment | |
| Primary or below | 2 (0.5) |
| Secondary or matriculation | 13 (3.4) |
| Tertiary | 362 (95.3) |
| Missing | 3 (0.8) |
| Types of participants’ school | |
| Full-government-subsidized school | 330 (86.8) |
| Partial-government-subsidized school | 20 (5.3) |
| Private school | 29 (7.6) |
| Missing | 1 (0.3) |
| Role of participants at school | |
| School principal | 18 (4.7) |
| Administrator | 70 (18.4) |
| Teacher | 275 (72.4) |
| School nurse/social worker/teacher assistant | 15 (4.0) |
| Missing | 2 (0.5) |
| Year of working experience (years) | |
| 0–5 | 151 (39.7) |
| 5–10 | 65 (17.1) |
| 10–20 | 92 (24.2) |
| ≥20 | 67 (17.6) |
| Missing | 5 (1.3) |
| Monthly income (HKD) a | |
| ≤19,999 | 36 (9.5) |
| 20,000–39,999 | 105 (27.6) |
| 40,000 or above | 231 (60.8) |
| Missing/Refused | 8 (2.1) |
| ID | Sex | Age Groups | 2018–2019 | 2019–2020 | School Type | Position | Working Years |
|---|---|---|---|---|---|---|---|
| SD1 | F | 45–54 | NA | IIV | AS | Admin | >20 |
| SD2 | F | 45–54 | L | IIV | AS | Teacher | 10–20 |
| SD3 | M | 45–54 | L | LAIV | AS | Admin | >20 |
| SD4 | F | ≥55 | I | IIV | AS | Admin | >20 |
| SD5 | F | 35–44 | I | IIV | AS | Teacher | 10–20 |
| SD6 | F | 45–54 | I | IIV | AS | Principal | 0–5 |
| SD7 | F | 45–54 | I | IIV | PS | Principle | >20 |
| SD8 | F | 25–34 | L | LAIV | AS | Teacher | 0–5 |
| SD9 | F | 45–54 | L | LAIV | AS | Teacher | >20 |
| SD10 | F | 45–54 | I | IIV | SS | Teacher | >20 |
| SD11 | F | 35–44 | I | IIV | AS | Teacher | 10–20 |
| SD12 | F | 25–34 | I | IIV | AS | Teacher | 0–5 |
| SD13 | M | 35–44 | I | IIV | AS | Teacher | 5–10 |
| SD14 | F | 35–44 | I | IIV | SS | Teacher | 0–5 |
| SD15 | F | 55 or above | I | IIV | AS | Principle | 10–20 |
| SD16 | F | 35–44 | NA | IIV | AS | Admin | >20 |
| SD17 | F | 35–44 | I | IIV | AS | Teacher | 10–20 |
| SD18 | F | 45–54 | I | IIV | SS | Teacher | 5–10 |
| SD19 | F | 45–54 | NA | IIV | AS | Teacher | >20 |
| SD20 | M | 35–44 | I | IIV | AS | Admin | 10–20 |
| SD21 | F | 25–34 | L | LAIV | AS | Teacher | 10–20 |
| SD22 | F | 25–34 | I | IIV | AS | Teacher | 0–5 |
| SD23 | M | 45–54 | NA | LAIV | AS | Admin | 10–20 |
| Number of Schools (%) | |
|---|---|
| The process of obtaining parents’ consent | |
| Type A | 47 (44.8) |
| Type B | 43 (41.0) |
| Type C | 15 (14.2) |
| Mentioning logistical arrangement of SIVP (e.g., time, procedure) | 105 (100.0) |
| Indicating positive attitudes about childhood SIV (e.g., “encourage”) | 72 (68.6) |
| Mentioning benefit of taking SIV | 49 (46.7) |
| Individual benefit (e.g., reduce sickness and absenteeism) | 28 (26.7) |
| Social benefit (community benefit) | 21 (20.0) |
| Mentioning risk of influenza to children | 24 (22.9) |
| The severe consequences of influenza virus infection | 14 (13.3) |
| Children’s high susceptibility to influenza infection at school | 21 (20.0) |
| Mentioning vaccine contraindication and eligibility for taking SIV | 20 (19.0) |
| Mentioning that SIV was recommended by health professional | 15 (14.3) |
| Mentioning that influenza vaccine is safe | 7 (6.7) |
| Mentioning the positive effect after introducing SIVP (e.g., reduction in students’ sickness due to influenza) | 1 (1.0) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liao, Q.; Dong, M.; Yuan, J.; Lam, W.W.T.; Cowling, B.J.; So, H.C.; Ip, D.K.M. A Mixed-Methods Study to Evaluate Elementary School Staff’s Acceptability, Delivery Challenges, and Communication Regarding the Implementation of School-Located Influenza Vaccination Program in Hong Kong. Vaccines 2021, 9, 1175. https://doi.org/10.3390/vaccines9101175
Liao Q, Dong M, Yuan J, Lam WWT, Cowling BJ, So HC, Ip DKM. A Mixed-Methods Study to Evaluate Elementary School Staff’s Acceptability, Delivery Challenges, and Communication Regarding the Implementation of School-Located Influenza Vaccination Program in Hong Kong. Vaccines. 2021; 9(10):1175. https://doi.org/10.3390/vaccines9101175
Chicago/Turabian StyleLiao, Qiuyan, Meihong Dong, Jiehu Yuan, Wendy Wing Tak Lam, Benjamin J. Cowling, Hau Chi So, and Dennis Kai Ming Ip. 2021. "A Mixed-Methods Study to Evaluate Elementary School Staff’s Acceptability, Delivery Challenges, and Communication Regarding the Implementation of School-Located Influenza Vaccination Program in Hong Kong" Vaccines 9, no. 10: 1175. https://doi.org/10.3390/vaccines9101175
APA StyleLiao, Q., Dong, M., Yuan, J., Lam, W. W. T., Cowling, B. J., So, H. C., & Ip, D. K. M. (2021). A Mixed-Methods Study to Evaluate Elementary School Staff’s Acceptability, Delivery Challenges, and Communication Regarding the Implementation of School-Located Influenza Vaccination Program in Hong Kong. Vaccines, 9(10), 1175. https://doi.org/10.3390/vaccines9101175






