Ocular Complications after COVID-19 Vaccination, Vaccine Adverse Event Reporting System
Abstract
1. Introduction
2. Materials and Methods
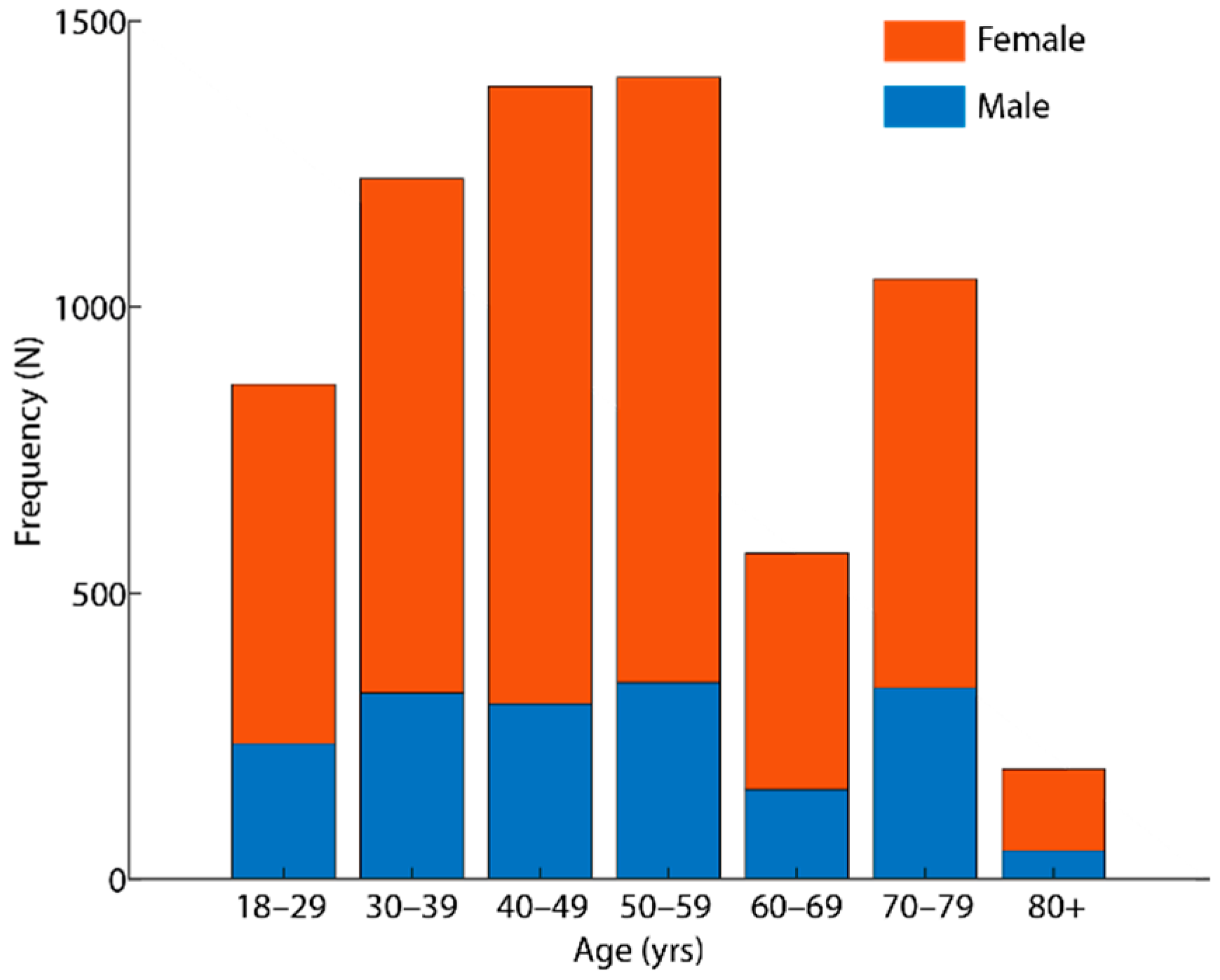
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Sadoff, J.; Gray, G.; Vandebosch, A.; Cárdenas, V.; Shukarev, G.; Grinsztejn, B.; Goepfert, P.A.; Truyers, C.; Fennema, H.; Spiessens, B.; et al. Safety and Efficacy of Single-Dose Ad26.COV2.S Vaccine against Covid-19. N. Engl. J. Med. 2021, 384, 2187–2201. [Google Scholar] [CrossRef] [PubMed]
- Voysey, M.; Clemens, S.A.C.; Madhi, S.A.; Weckx, L.Y.; Folegatti, P.M.; Aley, P.K.; Angus, B.; Baillie, V.L.; Barnabas, S.L.; Bhorat, Q.E.; et al. Safety and efficacy of the ChAdOx1 nCoV-19 vaccine (AZD1222) against SARS-CoV-2: An interim analysis of four randomised controlled trials in Brazil, South Africa, and the UK. Lancet 2021, 397, 99–111. [Google Scholar] [CrossRef]
- Baden, L.R.; El Sahly, H.M.; Essink, B.; Kotloff, K.; Frey, S.; Novak, R.; Diemert, D.; Spector, S.A.; Rouphael, N.; Creech, C.B.; et al. Efficacy and Safety of the mRNA-1273 SARS-CoV-2 Vaccine. N. Engl. J. Med. 2021, 384, 403–416. [Google Scholar] [CrossRef]
- Polack, F.P.; Thomas, S.J.; Kitchin, N.; Absalon, J.; Gurtman, A.; Lockhart, S.; Perez, J.L.; Pérez Marc, G.; Moreira, E.D.; Zerbini, C.; et al. Safety and Efficacy of the BNT162b2 mRNA COVID-19 Vaccine. N. Engl. J. Med. 2020, 383, 2603–2615. [Google Scholar] [CrossRef] [PubMed]
- Gee, J.; Marquez, P.; Su, J.; Calvert, G.M.; Liu, R.; Myers, T.; Nair, N.; Martin, S.; Clark, T.; Markowitz, L.; et al. First Month of COVID-19 Vaccine Safety Monitoring—United States, December 14, 2020–January 13, 2021. MMWR Morb. Mortal. Wkly. Rep. 2021, 70, 283–288. [Google Scholar] [CrossRef] [PubMed]
- Mudie, L.I.; Zick, J.D.; Dacey, M.S.; Palestine, A.G. Panuveitis following Vaccination for COVID-19. Ocul. Immunol. Inflamm. 2021, 29, 741–742. [Google Scholar] [CrossRef] [PubMed]
- Girbardt, C.; Busch, C.; Al-Sheikh, M.; Gunzinger, J.M.; Invernizzi, A.; Xhepa, A.; Unterlauft, J.D.; Rehak, M. Retinal Vascular Events after mRNA and Adenoviral-Vectored COVID-19 Vaccines—A Case Series. Vaccines 2021, 9, 1349. [Google Scholar] [CrossRef] [PubMed]
- Sood, A.B.; O’Keefe, G.; Bui, D.; Jain, N. Vogt-Koyanagi-Harada Disease Associated with Hepatitis B Vaccination. Ocul. Immunol. Inflamm. 2019, 27, 524–527. [Google Scholar] [CrossRef]
- Stewart, O.; Chang, B.; Bradbury, J. Simultaneous administration of hepatitis B and polio vaccines associated with bilateral optic neuritis. Br. J. Ophthalmol. 1999, 83, 1200–1201. [Google Scholar] [CrossRef][Green Version]
- Jorge, L.F.; Queiroz, R.P.; Gasparin, F.; Vasconcelos-Santos, D.V. Presumed Unilateral Acute Idiopathic Maculopathy following H1N1 Vaccination. Ocul. Immunol. Inflamm. 2021, 29, 1151–1153. [Google Scholar] [CrossRef]
- Marinho, P.M.; Nascimento, H.; Romano, A.; Muccioli, C.; Belfort, R., Jr. Diffuse uveitis and chorioretinal changes after yellow fever vaccination: A re-emerging epidemic. Int. J. Retin. Vitr. 2019, 5, 30. [Google Scholar] [CrossRef] [PubMed]
- Shah, S.P.; Goren, J.F.; Lazzara, M.D.; Strominger, M.B.; Hedges, T.R.; Duker, J.S.; Reichel, E. Acute macular neuroretinopathy associated with the use of norepinephrine reuptake inhibitors: A case series and OCT findings. Retin. Cases Brief Rep. 2013, 7, 146–149. [Google Scholar] [CrossRef]
- Shimabukuro, T.T.; Nguyen, M.; Martin, D.; DeStefano, F. Safety monitoring in the Vaccine Adverse Event Reporting System (VAERS). Vaccine 2015, 33, 4398–4405. [Google Scholar] [CrossRef]
- Ding, S.; Prevention, N.J.P.C.F.D.C.A.; Xiong, Y.; Pan, H.; Li, Z.; Tang, S.; Huang, X.; Li, J.; Shi, Y.; Fu, W.; et al. Suspected Yellow Fever Case Determined to be Adverse Vaccine Reaction. China CDC Wkly. 2019, 1, 54–55. Available online: https://www.ncbi.nlm.nih.gov/pubmed/34594604 (accessed on 2 June 2022). [CrossRef] [PubMed]
- Center for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research. Available online: https://wonder.cdc.gov/vaers.html (accessed on 22 December 2021).
- Vandenbroucke, J.P.; von Elm, E.; Altman, D.G.; Gøtzsche, P.C.; Mulrow, C.D.; Pocock, S.J.; Poole, C.; Schlesselman, J.J.; Egger, M.; STROBE Initiative. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): Explanation and elaboration. Int. J. Surg. 2014, 12, 1500–1524. [Google Scholar] [CrossRef] [PubMed]
- Pichi, F.; Aljneibi, S.; Neri, P.; Hay, S.; Dackiw, C.; Ghazi, N.G. Association of Ocular Adverse Events with Inactivated COVID-19 Vaccination in Patients in Abu Dhabi. JAMA Ophthalmol. 2021, 139, 1131–1135. [Google Scholar] [CrossRef] [PubMed]
- Pawar, N.; Maheshwari, D.; Ravindran, M.; Padmavathy, S. Ophthalmic complications of COVID-19 vaccination. Indian J. Ophthalmol. 2021, 69, 2900–2902. [Google Scholar] [CrossRef] [PubMed]
- Testi, I.; Brandao-de-Resende, C.; Agrawal, R.; Pavesio, C.; Group C-VOIES. Ocular inflammatory events following COVID-19 vaccination: A multinational case series. J. Ophthalmic Inflamm. Infect. 2022, 12, 4. [Google Scholar] [CrossRef] [PubMed]
- Zhong, Y.; Wang, K.; Zhu, Y.; Lyu, D.; Yu, Y.; Li, S.; Yao, K. Ocular manifestations in COVID-19 patients: A systematic review and meta-analysis. Travel Med. Infect. Dis. 2021, 44, 102191. [Google Scholar] [CrossRef]
- Cheng, J.Y.; Margo, C.E. Ocular adverse events following vaccination: Overview and update. Surv. Ophthalmol. 2022, 67, 293–306. [Google Scholar] [CrossRef]
- MacNeil, J.R.; Su, J.R.; Broder, K.R.; Guh, A.Y.; Gargano, J.W.; Wallace, M.; Hadler, S.C.; Scobie, H.M.; Blain, A.E.; Moulia, D.; et al. Updated Recommendations from the Advisory Committee on Immunization Practices for Use of the Janssen (Johnson & Johnson) COVID-19 Vaccine After Reports of Thrombosis with Thrombocytopenia Syndrome Among Vaccine Recipients—United States, April 2021. MMWR. Morb. Mortal. Wkly. Rep. 2021, 70, 651–656. [Google Scholar] [CrossRef] [PubMed]
- Belghmaidi, S.; Nassih, H.; Boutgayout, S.; El Fakiri, K.; El Qadiry, R.; Hajji, I.; Bourrahouate, A.; Moutaouakil, A. Third Cranial Nerve Palsy Presenting with Unilateral Diplopia and Strabismus in a 24-Year-Old Woman with COVID-19. Am. J. Case Rep. 2020, 21, e925897. [Google Scholar] [CrossRef] [PubMed]
- Sen, M.; Honavar, S.G.; Sharma, N.; Sachdev, M.S. COVID-19 and Eye: A Review of Ophthalmic Manifestations of COVID-19. Indian J. Ophthalmol. 2021, 69, 488–509. [Google Scholar] [CrossRef] [PubMed]
- Leung, E.H.; Fan, J.; Flynn, H.W., Jr.; Albini, T.A. Ocular and Systemic Complications of COVID-19: Impact on Patients and Healthcare. Clin. Ophthalmol. 2022, 16, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Stone, C.A., Jr.; Rukasin, C.R.F.; Beachkofsky, T.M.; Phillips, E.J. Immune-mediated adverse reactions to vaccines. Br. J. Clin. Pharmacol. 2019, 85, 2694–2706. [Google Scholar] [CrossRef] [PubMed]
- Rosenthal, S.; Chen, R. The reporting sensitivities of two passive surveillance systems for vaccine adverse events. Am. J. Public Health 1995, 85, 1706–1709. [Google Scholar] [CrossRef]
- Eberth, J.M.; Kline, K.N.; Moskowitz, D.A.; Montealegre, J.R.; Scheurer, M.E. The role of media and the Internet on vaccine adverse event reporting: A case study of human papillomavirus vaccination. J. Adolesc. Health 2014, 54, 289–295. [Google Scholar] [CrossRef] [PubMed]
| Adverse Event | Count (N) | Percentage |
|---|---|---|
| Blepharospasm | 145 | 2.17 |
| Blurred vision | 1785 | 26.69 |
| Dry eye | 64 | 0.96 |
| Exophthalmos | 18 | 0.27 |
| Extraocular muscle paresis/ophthalmoplegia | 333 | 4.98 |
| Eye contusion | 57 | 0.85 |
| Eye hemorrhage | 95 | 1.42 |
| Eye hypoaesthesia | 48 | 0.72 |
| Eyelid swelling, ocular hyperemia, conjunctivitis | 2229 | 33.33 |
| Eyelid ptosis | 102 | 1.53 |
| Ophthalmic herpes zoster/simplex | 43 | 0.64 |
| Photophobia | 265 | 3.96 |
| Visual impairment | 1322 | 19.77 |
| Vitreous floaters | 182 | 2.72 |
| Total | 6688 | 100.00 |
| Diagnosis | Vaccine Type | Group Count |
|---|---|---|
| Blepharospasm | Janssen | 21 |
| Moderna | 51 | |
| Pfizer | 73 | |
| Blurred vision | Janssen | 287 |
| Moderna | 630 | |
| Pfizer | 868 | |
| Dry eye | Janssen | 2 |
| Moderna | 22 | |
| Pfizer | 40 | |
| Exophthalmos | Janssen | 5 |
| Moderna | 6 | |
| Pfizer | 7 | |
| Extraocular muscle paresis/ophthalmoplegia | Janssen | 57 |
| Moderna | 129 | |
| Pfizer | 147 | |
| Eye contusion | Janssen | 7 |
| Moderna | 23 | |
| Pfizer | 27 | |
| Eye hemorrhage | Janssen | 18 |
| Moderna | 41 | |
| Pfizer | 36 | |
| Eye hypoesthesia | Janssen | 1 |
| Moderna | 18 | |
| Pfizer | 29 | |
| Eyelid swelling, ocular hyperemia, conjunctivitis | Janssen | 154 |
| Moderna | 907 | |
| Pfizer | 1168 | |
| Eyelid ptosis | Janssen | 4 |
| Moderna | 38 | |
| Pfizer | 60 | |
| Ophthalmic herpes zoster/simplex | Janssen | 2 |
| Moderna | 18 | |
| Pfizer | 23 | |
| Photophobia | Janssen | 31 |
| Moderna | 105 | |
| Pfizer | 129 | |
| Visual impairment | Janssen | 182 |
| Moderna | 502 | |
| Pfizer | 638 | |
| Vitreous floaters | Janssen | 19 |
| Moderna | 62 | |
| Pfizer | 101 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nyankerh, C.N.A.; Boateng, A.K.; Appah, M. Ocular Complications after COVID-19 Vaccination, Vaccine Adverse Event Reporting System. Vaccines 2022, 10, 941. https://doi.org/10.3390/vaccines10060941
Nyankerh CNA, Boateng AK, Appah M. Ocular Complications after COVID-19 Vaccination, Vaccine Adverse Event Reporting System. Vaccines. 2022; 10(6):941. https://doi.org/10.3390/vaccines10060941
Chicago/Turabian StyleNyankerh, Cyril N. A., Akosua K. Boateng, and Mary Appah. 2022. "Ocular Complications after COVID-19 Vaccination, Vaccine Adverse Event Reporting System" Vaccines 10, no. 6: 941. https://doi.org/10.3390/vaccines10060941
APA StyleNyankerh, C. N. A., Boateng, A. K., & Appah, M. (2022). Ocular Complications after COVID-19 Vaccination, Vaccine Adverse Event Reporting System. Vaccines, 10(6), 941. https://doi.org/10.3390/vaccines10060941






