Rate of Hospitalizations and Mortality of Respiratory Syncytial Virus Infection Compared to Influenza in Older People: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Sources and Searches
2.2. Study Selection
2.3. Data Extraction
2.4. Outcomes
2.5. Quality Assessment
2.6. Data Synthesis and Analysis
3. Results
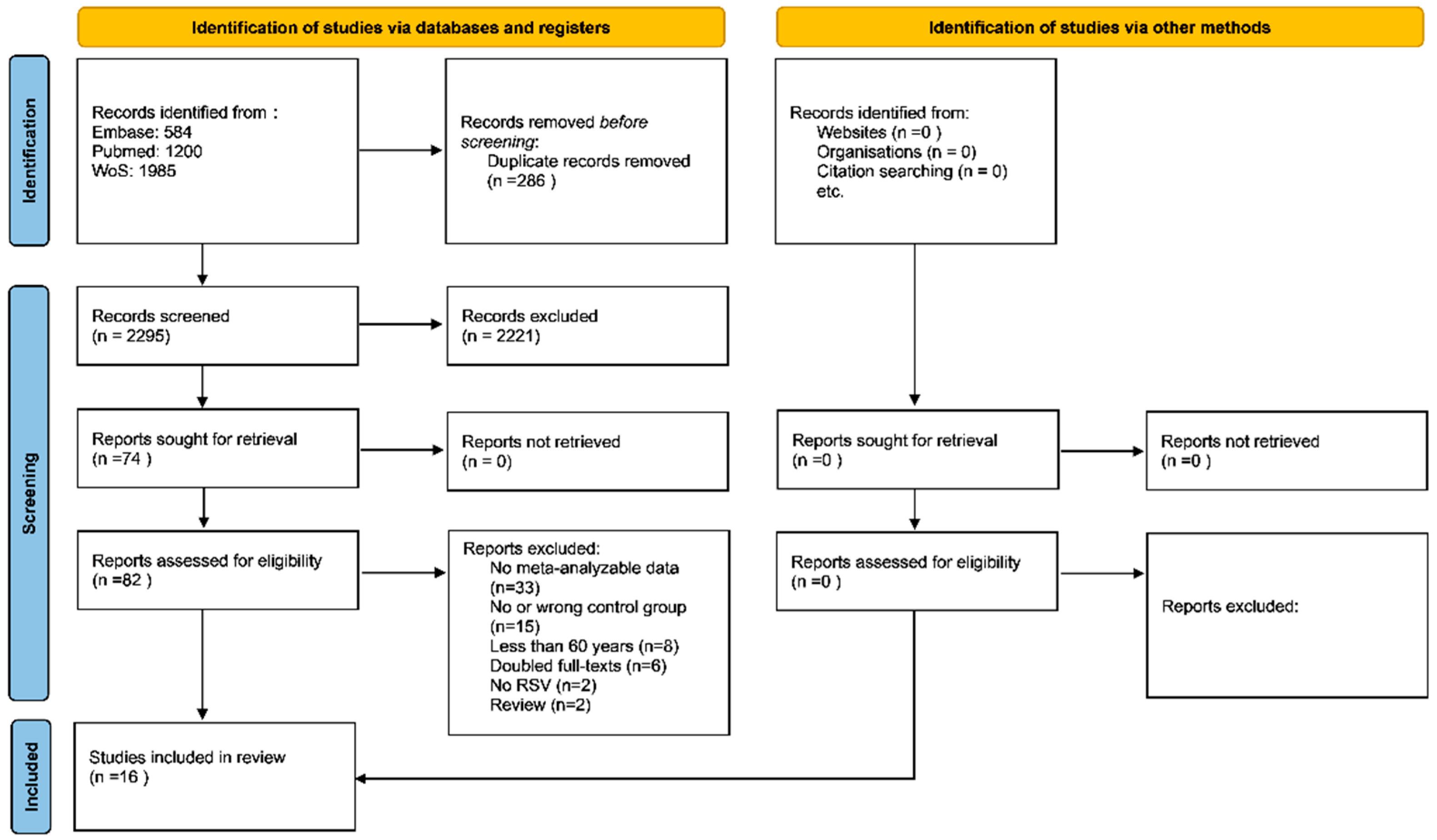
3.1. Search Results
3.2. Study and Patient Characteristics
3.3. Rate of Hospitalizations and Mortality in RSV vs. Influenza: Meta-Analysis
3.4. Sensitivity Analyses
3.5. Risk of Bias
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hall, C.B.; Weinberg, G.A.; Iwane, M.K.; Blumkin, A.K.; Edwards, K.M.; Staat, M.A.; Auinger, P.; Griffin, M.R.; Poehling, K.A.; Erdman, D. The burden of respiratory syncytial virus infection in young children. N. Engl. J. Med. 2009, 360, 588–598. [Google Scholar] [CrossRef]
- Staadegaard, L.; Caini, S.; Wangchuk, S.; Thapa, B.; de Almeida, W.A.F.; de Carvalho, F.C.; Njouom, R.; Fasce, R.A.; Bustos, P.; Kyncl, J. The global epidemiology of RSV in community and hospitalized care: Findings from 15 countries. Open Forum Infect. Dis. 2021, 8, ofab159. [Google Scholar] [CrossRef]
- Branche, A.R.; Falsey, A.R. Respiratory syncytial virus infection in older adults: An under-recognized problem. Drugs Aging 2015, 32, 261–269. [Google Scholar] [CrossRef] [PubMed]
- Troeger, C.; Blacker, B.; Khalil, I.A.; Rao, P.C.; Cao, J.; Zimsen, S.R.; Albertson, S.B.; Deshpande, A.; Farag, T.; Abebe, Z. Estimates of the global, regional, and national morbidity, mortality, and aetiologies of lower respiratory infections in 195 countries, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet Infect. Dis. 2018, 18, 1191–1210. [Google Scholar] [CrossRef] [PubMed]
- Handforth, J.; Friedland, J.; Sharland, M. Basic epidemiology and immunopathology of RSV in children. Paediatr. Respir. Rev. 2000, 1, 210–214. [Google Scholar] [CrossRef]
- Branche, A.R.; Saiman, L.; Walsh, E.E.; Falsey, A.R.; Sieling, W.D.; Greendyke, W.; Peterson, D.R.; Vargas, C.Y.; Phillips, M.; Finelli, L. Incidence of respiratory syncytial virus infection among hospitalized adults, 2017–2020. Clin. Infect. Dis. 2022, 74, 1004–1011. [Google Scholar] [CrossRef] [PubMed]
- Martinez, F.J.; Foster, G.; Curtis, J.L.; Criner, G.; Weinmann, G.; Fishman, A.; DeCamp, M.M.; Benditt, J.; Sciurba, F.; Make, B. Predictors of mortality in patients with emphysema and severe airflow obstruction. Am. J. Respir. Crit. Care Med. 2006, 173, 1326–1334. [Google Scholar] [CrossRef]
- Falsey, A.R.; Walsh, E.E.; Esser, M.T.; Shoemaker, K.; Yu, L.; Griffin, M.P. Respiratory syncytial virus–associated illness in adults with advanced chronic obstructive pulmonary disease and/or congestive heart failure. J. Med. Virol. 2019, 91, 65–71. [Google Scholar] [CrossRef]
- Walsh, E.E.; Peterson, D.R.; Falsey, A.R. Risk factors for severe respiratory syncytial virus infection in elderly persons. J. Infect. Dis. 2004, 189, 233–238. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Respiratory syncytial virus activity—United States, July 2007–December 2008. MMWR. Morb. Mortal. Wkly. Rep. 2008, 57, 1355–1358. [Google Scholar]
- Hansen, C.L.; Chaves, S.S.; Demont, C.; Viboud, C. Mortality Associated with Influenza and Respiratory Syncytial Virus in the US, 1999–2018. JAMA Netw. Open 2022, 5, e220527. [Google Scholar] [CrossRef] [PubMed]
- Bosco, E.; van Aalst, R.; McConeghy, K.W.; Silva, J.; Moyo, P.; Eliot, M.N.; Chit, A.; Gravenstein, S.; Zullo, A.R. Estimated cardiorespiratory hospitalizations attributable to influenza and respiratory syncytial virus among long-term care facility residents. JAMA Netw. Open 2021, 4, e2111806. [Google Scholar] [CrossRef] [PubMed]
- Shi, T.; Denouel, A.; Tietjen, A.K.; Campbell, I.; Moran, E.; Li, X.; Campbell, H.; Demont, C.; Nyawanda, B.O.; Chu, H.Y.; et al. Global Disease Burden Estimates of Respiratory Syncytial Virus-Associated Acute Respiratory Infection in Older Adults in 2015: A Systematic Review and Meta-Analysis. J. Infect. Dis. 2020, 222, S577–S583. [Google Scholar] [CrossRef]
- Shi, T.; Arnott, A.; Semogas, I.; Falsey, A.R.; Openshaw, P.; Wedzicha, J.A.; Campbell, H.; Nair, H. The Etiological Role of Common Respiratory Viruses in Acute Respiratory Infections in Older Adults: A Systematic Review and Meta-analysis. J. Infect. Dis. 2020, 222, S563–S569. [Google Scholar] [CrossRef]
- Agius, G.; Dindinaud, G.; Biggar, R.; Peyre, R.; Vaillant, V.; Ranger, S.; Poupet, J.; Cisse, M.; Castets, M. An epidemic of respiratory syncytial virus in elderly people: Clinical and serological findings. J. Med. Virol. 1990, 30, 117–127. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, e1–e34. [Google Scholar] [CrossRef]
- Higgins, J.P.; Thomas, J.; Chandler, J.; Cumpston, M.; Li, T.; Page, M.J.; Welch, V.A. Cochrane Handbook for Systematic Reviews of Interventions; John Wiley & Sons: Hoboken, NJ, USA, 2019. [Google Scholar]
- Luchini, C.; Stubbs, B.; Solmi, M.; Veronese, N. Assessing the quality of studies in meta-analyses: Advantages and limitations of the Newcastle Ottawa Scale. World J. Meta-Anal. 2017, 5, 80–84. [Google Scholar] [CrossRef]
- Luchini, C.; Veronese, N.; Nottegar, A.; Shin, J.I.; Gentile, G.; Granziol, U.; Soysal, P.; Alexinschi, O.; Smith, L. Assessing the quality of studies in meta-research: Review/guidelines on the most important quality assessment tools. Pharm. Stat. 2021, 20, 185–195. [Google Scholar] [CrossRef] [PubMed]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Control. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Egger, M.; Smith, G.D.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef]
- Duval, S.; Tweedie, R. Trim and fill: A simple funnel-plot–based method of testing and adjusting for publication bias in meta-analysis. Biometrics 2000, 56, 455–463. [Google Scholar] [CrossRef] [PubMed]
- Ackerson, B.; Tseng, H.F.; Sy, L.S.; Solano, Z.; Slezak, J.; Luo, Y.; Fischetti, C.A.; Shinde, V. Severe Morbidity and Mortality Associated with Respiratory Syncytial Virus Versus Influenza Infection in Hospitalized Older Adults. Clin. Infect. Dis. 2019, 69, 197–203. [Google Scholar] [CrossRef] [PubMed]
- Auvinen, R.; Syrjänen, R.; Ollgren, J.; Nohynek, H.; Skogberg, K. Clinical characteristics and population-based attack rates of respiratory syncytial virus versus influenza hospitalizations among adults—An observational study. Influenza Other Respir. Viruses 2021, 16, 276–288. [Google Scholar] [CrossRef]
- Falsey, A.R.; Hennessey, P.A.; Formica, M.A.; Cox, C.; Walsh, E.E. Respiratory syncytial virus infection in elderly and high-risk adults. N. Engl. J. Med. 2005, 352, 1749–1759. [Google Scholar] [CrossRef] [PubMed]
- Gilca, R.; Amini, R.; Douville-Fradet, M.; Charest, H.; Dubuque, J.; Boulianne, N.; Skowronski, D.M.; De Serres, G. Other Respiratory Viruses Are Important Contributors to Adult Respiratory Hospitalizations and Mortality Even During Peak Weeks of the Influenza Season. Open Forum Infect. Dis. 2014, 1, ofu086. [Google Scholar] [CrossRef] [PubMed]
- Korsten, K.; Adriaenssens, N.; Coenen, S.; Butler, C.; Ravanfar, B.; Rutter, H.; Allen, J.; Falsey, A.; Pirçon, J.-Y.; Gruselle, O.; et al. Burden of respiratory syncytial virus infection in community-dwelling older adults in Europe (RESCEU): An international prospective cohort study. Eur. Respir. J. 2021, 57, 2002688. [Google Scholar] [CrossRef] [PubMed]
- Loubet, P.; Lenzi, N.; Valette, M.; Foulongne, V.; Krivine, A.; Houhou, N.; Lagathu, G.; Rogez, S.; Alain, S.; Duval, X.; et al. Clinical characteristics and outcome of respiratory syncytial virus infection among adults hospitalized with influenza-like illness in France. Clin. Microbiol. Infect. 2017, 23, 253–259. [Google Scholar] [CrossRef]
- Malosh, R.E.; Martin, E.T.; Callear, A.P.; Petrie, J.G.; Lauring, A.S.; Lamerato, L.; Fry, A.M.; Ferdinands, J.; Flannery, B.; Monto, A.S. Respiratory syncytial virus hospitalization in middle-aged and older adults. J. Clin. Virol. 2017, 96, 37–43. [Google Scholar] [CrossRef]
- Matias, G.; Taylor, R.; Haguinet, F.; Schuck-Paim, C.; Lustig, R.; Shinde, V. Estimates of hospitalization attributable to influenza and RSV in the US during 1997–2009, by age and risk status. BMC Public Health 2017, 17, 271. [Google Scholar] [CrossRef]
- MÜLler-Pebody, B.; Crowcroft, N.S.; Zambon, M.C.; Edmunds, W.J. Modelling hospital admissions for lower respiratory tract infections in the elderly in England. Epidemiol. Infect. 2006, 134, 1150–1157. [Google Scholar] [CrossRef]
- Rabarison, J.H.; Tempia, S.; Harimanana, A.; Guillebaud, J.; Razanajatovo, N.H.; Ratsitorahina, M.; Heraud, J.-M. Burden and epidemiology of influenza- and respiratory syncytial virus-associated severe acute respiratory illness hospitalization in Madagascar, 2011–2016. Influenza Other Respir. Viruses 2019, 13, 138–147. [Google Scholar] [CrossRef] [PubMed]
- Schanzer, D.L.; Langley, J.M.; Tam, T.W.S. Role of influenza and other respiratory viruses in admissions of adults to Canadian hospitals. Influenza Other Respir. Viruses 2008, 2, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Sharp, A.; Minaji, M.; Panagiotopoulos, N.; Reeves, R.; Charlett, A.; Pebody, R. Estimating the burden of adult hospital admissions due to RSV and other respiratory pathogens in England. Influenza Other Respir. Viruses 2021, 16, 125–131. [Google Scholar] [CrossRef]
- Tseng, H.F.; Sy, L.; Ackerson, B.; Fischetti, C.; Slezak, J.; Luo, Y.; Solano, Z.; Chen, S.; Shinde, V. Morbidity, and Short- and Intermediate-Term Mortality, in Adults ≥60 Years Hospitalized with Respiratory Syncytial Virus Infection vs. Seasonal Influenza Virus Infection. Open Forum Infect. Dis. 2017, 4, S318–S319. [Google Scholar] [CrossRef][Green Version]
- Widmer, K.; Zhu, Y.; Williams, J.V.; Griffin, M.R.; Edwards, K.M.; Talbot, H.K. Rates of Hospitalizations for Respiratory Syncytial Virus, Human Metapneumovirus, and Influenza Virus in Older Adults. J. Infect. Dis. 2012, 206, 56–62. [Google Scholar] [CrossRef]
- Ellis, S.E.; Coffey, C.S.; Mitchel, E.F., Jr.; Dittus, R.S.; Griffin, M.R. Influenza- and respiratory syncytial virus-associated morbidity and mortality in the nursing home population. J. Am. Geriatr. Soc. 2003, 51, 761–767. [Google Scholar] [CrossRef]
- Falsey, A.R.; Walsh, E.E.; House, S.; Vandenijck, Y.; Ren, X.; Keim, S.; Kang, D.; Peeters, P.; Witek, J.; Ispas, G. Risk factors and medical resource utilization of respiratory syncytial virus, human metapneumovirus, and influenza-related hospitalizations in adults—A global study during the 2017–2019 epidemic seasons (hospitalized acute respiratory tract infection [HARTI] study). Open Forum Infect. Dis. 2021, 8, ofab491. [Google Scholar]
- Bagga, B.; Woods, C.W.; Veldman, T.H.; Gilbert, A.; Mann, A.; Balaratnam, G.; Lambkin-Williams, R.; Oxford, J.S.; McClain, M.T.; Wilkinson, T. Comparing influenza and RSV viral and disease dynamics in experimentally infected adults predicts clinical effectiveness of RSV antivirals. Antivir. Ther. 2013, 18, 785–792. [Google Scholar] [CrossRef] [PubMed]
- Lee, N.; Walsh, E.E.; Sander, I.; Stolper, R.; Zakar, J.; Wyffels, V.; Myers, D.; Fleischhackl, R. Delayed diagnosis of respiratory syncytial virus infections in hospitalized adults: Individual patient data, record review analysis and physician survey in the United States. J. Infect. Dis. 2019, 220, 969–979. [Google Scholar] [CrossRef]
- Tramuto, F.; Maida, C.M.; Di Naro, D.; Randazzo, G.; Vitale, F.; Restivo, V.; Costantino, C.; Amodio, E.; Casuccio, A.; Graziano, G. Respiratory Syncytial Virus: New Challenges for Molecular Epidemiology Surveillance and Vaccination Strategy in Patients with ILI/SARI. Vaccines 2021, 9, 1334. [Google Scholar] [CrossRef]
- Sah, P.; Alfaro-Murillo, J.A.; Fitzpatrick, M.C.; Neuzil, K.M.; Meyers, L.A.; Singer, B.H.; Galvani, A.P. Future epidemiological and economic impacts of universal influenza vaccines. Proc. Natl. Acad. Sci. USA 2019, 116, 20786–20792. [Google Scholar] [CrossRef] [PubMed]
- Warren-Gash, C.; Blackburn, R.; Whitaker, H.; McMenamin, J.; Hayward, A.C. Laboratory-confirmed respiratory infections as triggers for acute myocardial infarction and stroke: A self-controlled case series analysis of national linked datasets from Scotland. Eur. Respir. J. 2018, 51, 1701794. [Google Scholar] [CrossRef]
- Barker, W.H.; Borisute, H.; Cox, C. A study of the impact of influenza on the functional status of frail older people. Arch. Intern. Med. 1998, 158, 645–650. [Google Scholar] [CrossRef] [PubMed]
- Kubale, J.; Kuan, G.; Gresh, L.; Ojeda, S.; Schiller, A.; Sanchez, N.; Lopez, R.; Azziz-Baumgartner, E.; Wraith, S.; Harris, E. Individual-level association of influenza infection with subsequent pneumonia: A case-control and prospective cohort study. Clin. Infect. Dis. 2021, 73, e4288–e4295. [Google Scholar] [CrossRef]
- Demurtas, J.; Celotto, S.; Beaudart, C.; Sanchez-Rodriguez, D.; Balci, C.; Soysal, P.; Solmi, M.; Celotto, D.; Righi, E.; Smith, L. The efficacy and safety of influenza vaccination in older people: An umbrella review of evidence from meta-analyses of both observational and randomized controlled studies. Ageing Res. Rev. 2020, 62, 101118. [Google Scholar] [CrossRef]
- Gomez, G.B.; Mahé, C.; Chaves, S.S. Uncertain effects of the pandemic on respiratory viruses. Science 2021, 372, 1043–1044. [Google Scholar] [CrossRef]
- Mazur, N.I.; Terstappen, J.; Baral, R.; Bardají, A.; Beutels, P.; Buchholz, U.J.; Cohen, C.; Crowe Jr, J.E.; Cutland, C.L.; Eckert, L. Respiratory syncytial virus prevention within reach: The vaccine and monoclonal antibody landscape. Lancet Infect. Dis. 2022, 8, S1473-3099(22)00291-2. [Google Scholar] [CrossRef]
- Stephens, L.M.; Varga, S.M. Considerations for a respiratory syncytial virus vaccine targeting an elderly population. Vaccines 2021, 9, 624. [Google Scholar] [CrossRef]
- Ison, M. A respiratory syncytial virus (RSV) prefusion F protein candidate vaccine (RSVPreF3 OA) is efficacious in adults ≥60 years of age (YOA). In Proceedings of the ID Week, Washington, DC, USA, 19–23 October 2022. [Google Scholar]
- Riccò, M.; Cerviere, M.P.; Corrado, S.; Ranzieri, S.; Marchesi, F. Respiratory Syncytial Virus: An Uncommon Cause of Febrile Seizures-Results from a Systematic Review and Meta-Analysis. Pediatr. Rep. 2022, 14, 55. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. Syst. Rev. 2021, 10, 1–11. [Google Scholar] [CrossRef]
| Author, Year | Type of Study | Sample Size | Mean Age | Diagnosis of RSV and Influenza | Follow-Up (Months) | NOS |
|---|---|---|---|---|---|---|
| Ackerson, 2019 | Retrospective | 2523 | 78 | PCR and culture | 12 | 8 |
| Auvinen, 2021 | Prospective | 974 | 76 | PCR | 48 | 8 |
| Ellis, 2003 | Retrospective | 10,581 | 65+ | Antigent tests and cultures | 48 | 7 |
| Falsey, 2005 | Prospective | 146 | 72 | RT-PCR, Serologic test, viral culture | 48 | 8 |
| Falsey, 2021 | Prospective | 604 | 65.6 | PCR | 3 | 8 |
| Gilca, 2014 | Prospective | 210 | Luminex RVP FAST assay | 48 | 7 | |
| Gonçalo Matias, 2017 | Retrospective | 64,456 | 65+ | Weekly influenza update | 144 | 7 |
| Korsten, 2020 | Prospective | 1040 | 75 | PCR | 48 | 8 |
| Loubet, 2016 | Prospective | 1452 | 74 | PCR | 12 | 8 |
| Malosh, 2017 | Prospective | 426 | PCR | 24 | 8 | |
| Muller-Pebody, 2006 | Prospective | 551,633 | 65+ | ICD-10 | 36 | 7 |
| Rabarison, 2019 | Retrospective | 375 | PCR | 60 | 8 | |
| Schanzer, 2008 | Retrospecitve | 103,262 | Hospitalization Morbidity Database (HMDB)14 | 60 | 7 | |
| Sharp, 2021 | Retrospective | 21,787 | 65–74 | Antigene detection, culture, and genomic/pcr/lcr detection | 84 | 8 |
| Tseng, 2017 | Prospective | 2586 | 60+ | PCR | 48 | 8 |
| Widemer, 2012 | Prospective | 29 | 65+ | PCR | 36 | 8 |
| Total | 9 studies: prospective; 7 studies: retrospective | 762,084 | 73.4 | 9 studies: PCR; 7 studies: others | 48 (range: 3–84) |
| Cumulative Incidence | Incidence Rate (Per 100,000 Persons-Year) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Outcome | N of Studies (Participants) | RR | 95% CI | p-Value | I2 | Egger’s Test (p-Value) | N of Studies | MD | 95% CI | p-Value | I2 | Egger’s Test (p-Value) |
| Hospitalization | 5 | 0.93 | 0.53–1.62 | 0.80 | 0 | −0.73 (p = 0.08) | 10 | −262 | −755; 229 | 0.30 | 99 | −6.57 (p = 0.20) |
| Mortality | 4 | 1.19 | 0.98–1.45 | 0.08 | 0 | 0.57 (p = 0.10) | 2 | 15 | −133; 162 | 0.85 | 0 | Not possible |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maggi, S.; Veronese, N.; Burgio, M.; Cammarata, G.; Ciuppa, M.E.; Ciriminna, S.; Di Gennaro, F.; Smith, L.; Trott, M.; Dominguez, L.J.; et al. Rate of Hospitalizations and Mortality of Respiratory Syncytial Virus Infection Compared to Influenza in Older People: A Systematic Review and Meta-Analysis. Vaccines 2022, 10, 2092. https://doi.org/10.3390/vaccines10122092
Maggi S, Veronese N, Burgio M, Cammarata G, Ciuppa ME, Ciriminna S, Di Gennaro F, Smith L, Trott M, Dominguez LJ, et al. Rate of Hospitalizations and Mortality of Respiratory Syncytial Virus Infection Compared to Influenza in Older People: A Systematic Review and Meta-Analysis. Vaccines. 2022; 10(12):2092. https://doi.org/10.3390/vaccines10122092
Chicago/Turabian StyleMaggi, Stefania, Nicola Veronese, Marianna Burgio, Giorgia Cammarata, Maria Elena Ciuppa, Stefano Ciriminna, Francesco Di Gennaro, Lee Smith, Mike Trott, Ligia J. Dominguez, and et al. 2022. "Rate of Hospitalizations and Mortality of Respiratory Syncytial Virus Infection Compared to Influenza in Older People: A Systematic Review and Meta-Analysis" Vaccines 10, no. 12: 2092. https://doi.org/10.3390/vaccines10122092
APA StyleMaggi, S., Veronese, N., Burgio, M., Cammarata, G., Ciuppa, M. E., Ciriminna, S., Di Gennaro, F., Smith, L., Trott, M., Dominguez, L. J., Giammanco, G. M., De Grazia, S., Costantino, C., Vitale, F., & Barbagallo, M. (2022). Rate of Hospitalizations and Mortality of Respiratory Syncytial Virus Infection Compared to Influenza in Older People: A Systematic Review and Meta-Analysis. Vaccines, 10(12), 2092. https://doi.org/10.3390/vaccines10122092













