Rural-Urban Disparities in Vaccine Hesitancy among Adults in South Tyrol, Italy
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Data Collection
2.2. Rurality
2.3. Questionnaire
2.4. Vaccine Hesitancy (Dependent Variable)
2.5. Putative Predictors of Vaccine Hesitancy (Independent Variables)
2.6. Statistical Analysis
3. Results
3.1. Population Characteristics
3.2. Vaccination Perception
3.2.1. Compulsory Vaccination for Non-Coronaviruses
3.2.2. Vaccination for Coronaviruses
3.2.3. Vaccine-Hesitancy-Related Attitudes in Residence Groups
3.3. Predictors of Vaccine Hesitancy
3.3.1. Vaccine-Hesitancy-Related Attitudes in Residence Groups
3.3.2. Attitudes of Rural Vaccine Hesitancy
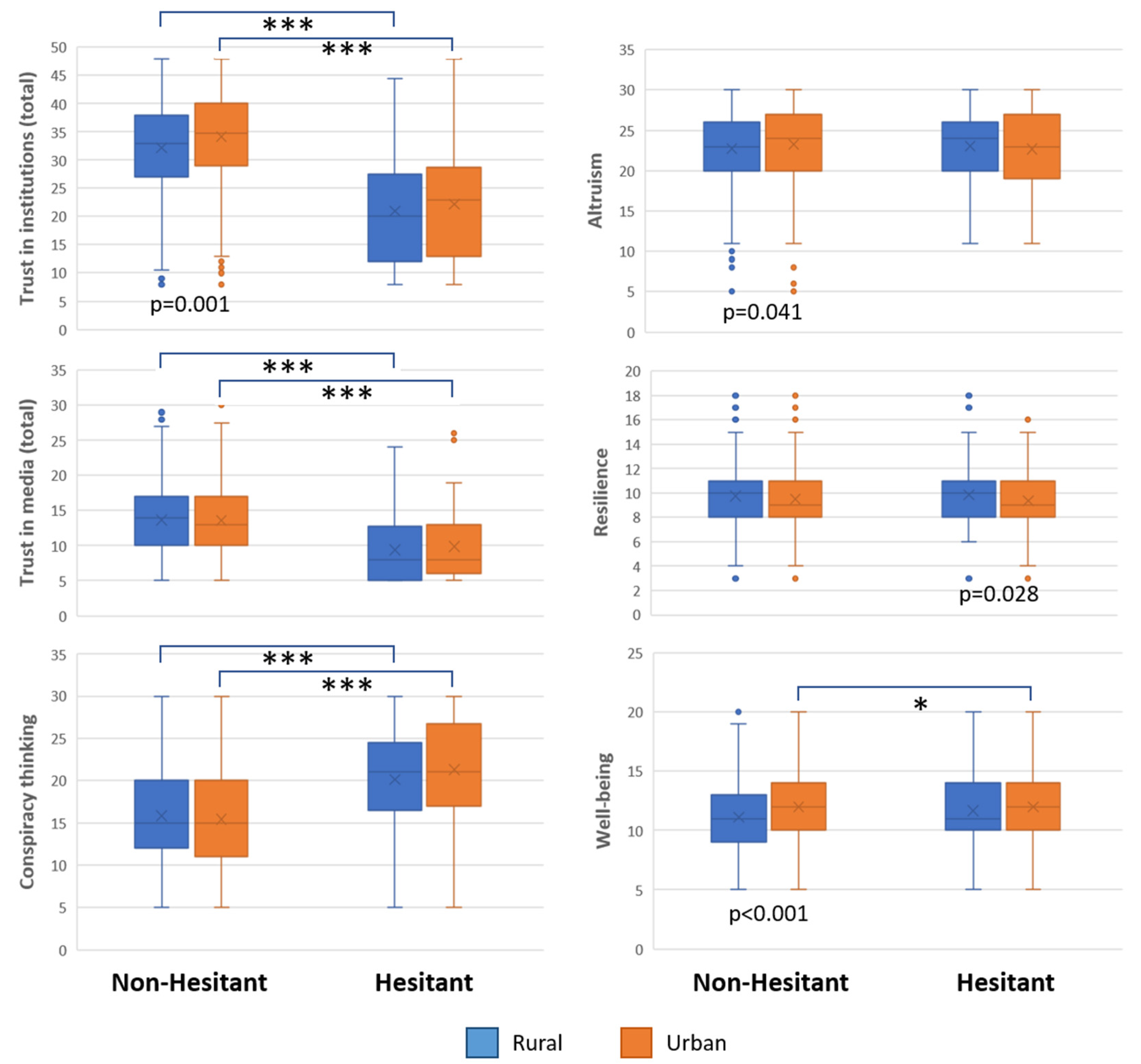
3.3.3. Composite Scores for Trust in Information Sources and Institutions, Conspiracy Theories, Altruism, Resilience and Wellbeing
3.4. Multivariate Logistic Regression for Predictors of Hesitancy
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Barchielli, B.; Cricenti, C.; Gallè, F.; Sabella, E.A.; Liguori, F.; Da Molin, G.; Liguori, G.; Orsi, G.B.; Giannini, A.M.; Ferracuti, S.; et al. Climate Changes, Natural Resources Depletion, COVID-19 Pandemic, and Russian-Ukrainian War: What Is the Impact on Habits Change and Mental Health? Int. J. Environ. Res. Public Health 2022, 19, 11929. [Google Scholar] [CrossRef] [PubMed]
- Bauch, C.T.; Galvani, A.P. Social Factors in Epidemiology. Science 2013, 342, 47–49. [Google Scholar] [CrossRef] [PubMed]
- Harrison, E.A.; Wu, J.W. Vaccine Confidence in the Time of COVID-19. Eur. J. Epidemiol. 2020, 35, 325–330. [Google Scholar] [CrossRef] [PubMed]
- Hudson, A.; Montelpare, W.J. Predictors of Vaccine Hesitancy: Implications for COVID-19 Public Health Messaging. Int. J. Environ. Res. Public Health 2021, 18, 8054. [Google Scholar] [CrossRef]
- Radiotelevisione Italiana Impfkampagne: Wochen-Negativrekord in Südtirol—TGR Tagesschau. Available online: https://www.rainews.it/tgr/tagesschau/articoli/2021/09/tag-Impfkampagne-Wochenbilanz-Suedtirol-20210906-a3614331-14e6-43cd-80eb-447bd32fb552.html (accessed on 17 July 2022).
- Barbieri, V.; Wiedermann, C.J.; Lombardo, S.; Ausserhofer, D.; Plagg, B.; Piccoliori, G.; Gärtner, T.; Wiedermann, W.; Engl, A. Vaccine Hesitancy in the Second Year of the Coronavirus Pandemic in South Tyrol, Italy: A Representative Cross-Sectional Survey. Vaccines 2022, 10, 1584. [Google Scholar] [CrossRef]
- Bubola, E. In Italy’s Alps, Traditional Medicine Flourishes, as Does Covid. The New York Times, 16 December 2021. [Google Scholar]
- Polašek, O.; Wazny, K.; Adeloye, D.; Song, P.; Chan, K.Y.; Bojude, D.A.; Ali, S.; Bastien, S.; Becerra-Posada, F.; Borrescio-Higa, F.; et al. Research Priorities to Reduce the Impact of COVID-19 in Low- and Middle-Income Countries. J. Glob. Health 2022, 12, 09003. [Google Scholar] [CrossRef]
- Zhai, Y.; Santibanez, T.A.; Kahn, K.E.; Srivastav, A.; Walker, T.Y.; Singleton, J.A. Rural, Urban, and Suburban Differences in Influenza Vaccination Coverage among Children. Vaccine 2020, 38, 7596–7602. [Google Scholar] [CrossRef]
- Bennett, K.J.; Bellinger, J.D.; Probst, J.C. Receipt of Influenza and Pneumonia Vaccinations: The Dual Disparity of Rural Minorities. J. Am. Geriatr. Soc. 2010, 58, 1896–1902. [Google Scholar] [CrossRef]
- Albers, A.N.; Thaker, J.; Newcomer, S.R. Barriers to and Facilitators of Early Childhood Immunization in Rural Areas of the United States: A Systematic Review of the Literature. Prev. Med. Rep. 2022, 27, 101804. [Google Scholar] [CrossRef]
- Bernstein, E.; DeRycke, E.; Han, L.; Bastian, L.; Bean-Mayberry, B.; Bade, B.; Brandt, C.; Farmer, M.M.; Crothers, K.A.; Skanderson, M. Racial and Rural Disparities in COVID-19 Vaccination Uptake in a National Sample of Veterans. Am. J. Respir. Crit. Care Med. 2022, 205, A3695. [Google Scholar]
- Sun, Y.; Monnat, S.M. Rural-Urban and within-Rural Differences in COVID-19 Vaccination Rates. J. Rural Health 2021, 38, 916–922. [Google Scholar] [CrossRef] [PubMed]
- Hubach, R.D.; Shannon, B.; Morgan, K.D.; Alexander, C.; O’Neil, A.M.; Ernst, C.; Giano, Z. COVID-19 Vaccine Hesitancy among Rural Oklahomans. Rural Remote Health 2022, 22, 7128. [Google Scholar] [CrossRef] [PubMed]
- Burke, P.F.; Masters, D.; Massey, G. Enablers and Barriers to COVID-19 Vaccine Uptake: An International Study of Perceptions and Intentions. Vaccine 2021, 39, 5116–5128. [Google Scholar] [CrossRef] [PubMed]
- Faye, S.L.B.; Krumkamp, R.; Doumbia, S.; Tounkara, M.; Strauss, R.; Ouedraogo, H.G.; Sagna, T.; Barry, A.M.; Mbawah, A.K.; Doumbia, C.O.; et al. Factors Influencing Hesitancy towards Adult and Child COVID-19 Vaccines in Rural and Urban West Africa: A Cross-Sectional Study. BMJ Open 2022, 12, e059138. [Google Scholar] [CrossRef] [PubMed]
- Mann, S.; Christini, K.; Chai, Y.; Chang, C.-P.; Hashibe, M.; Kepka, D. Vaccine Hesitancy and COVID-19 Immunization among Rural Young Adults. Prev. Med. Rep. 2022, 28, 101845. [Google Scholar] [CrossRef]
- Lee, J.; Huang, Y. COVID-19 Vaccine Hesitancy: The Role of Socioeconomic Factors and Spatial Effects. Vaccines 2022, 10, 352. [Google Scholar] [CrossRef]
- Kuchi, S.; Parida, S.P. COVID-19 Vaccination Hesitancy and Attitude Post-Initiation of Vaccination Drive, a Cross-Sectional Study across Odisha. J. Fam. Med. Prim. Care 2022, 11, 1996–2001. [Google Scholar] [CrossRef]
- Joshi, A.; Surapaneni, K.M.; Kaur, M.; Bhatt, A.; Nash, D.; El-Mohandes, A. A Cross Sectional Study to Examine Factors Influencing COVID-19 Vaccine Acceptance, Hesitancy and Refusal in Urban and Rural Settings in Tamil Nadu, India. PLoS ONE 2022, 17, e0269299. [Google Scholar] [CrossRef]
- Heiniger, S.; Schliek, M.; Moser, A.; von Wyl, V.; Höglinger, M. Differences in COVID-19 Vaccination Uptake in the First 12 Months of Vaccine Availability in Switzerland—A Prospective Cohort Study. Swiss Med. Wkly. 2022, 152, w30162. [Google Scholar] [CrossRef]
- Wisniak, A.; Baysson, H.; Pullen, N.; Nehme, M.; Pennacchio, F.; Zaballa, M.-E.; Guessous, I.; Stringhini, S.; The Specchio-COVID19 Study Group. COVID-19 Vaccination Acceptance in the Canton of Geneva: A Cross-Sectional Population-Based Study. Swiss Med. Wkly. 2021, 151, w30080. [Google Scholar] [CrossRef]
- World Health Organization. Survey Tool and Guidance—Rapid, Simple, Flexible Behavioural Insights on COVID-19. Monitoring Knowledge, Risk Perceptions, Preventive Behaviours and Trust to Inform Pandemic Outbreak Response; Regional Office of Europe: Copenhagen, Denmark, 2020. [Google Scholar]
- Taherdoost, H. Determining Sample Size; How to Calculate Survey Sample Size. Int. J. Econ. Manag. Syst. 2017, 2, al-02557333. [Google Scholar]
- Landesinstitut für Statistik der Autonomen Provinz Bozen—Südtirol. COVID-19: Einstellungen und Verhalten der Bürger. Jänner 2021; astatinfo; Landesverwaltung der Autonomen Provinz Bozen—Südtirol: Bolzano, Italia, 2021. [Google Scholar]
- WHO Regional Office for Europe. COVID-19 Snapshot MOnitoring (COSMO Standard): Monitoring Knowledge, Risk Perceptions, Preventive Behaviours, and Public Trust in the Current Coronavirus Outbreak—WHO Standard Protocol; WHO Regional Office for Europe: København, Danmark, 2020. [Google Scholar]
- Sørensen, K.; Van den Broucke, S.; Pelikan, J.M.; Fullam, J.; Doyle, G.; Slonska, Z.; Kondilis, B.; Stoffels, V.; Osborne, R.H.; Brand, H.; et al. Measuring Health Literacy in Populations: Illuminating the Design and Development Process of the European Health Literacy Survey Questionnaire (HLS-EU-Q). BMC Public Health 2013, 13, 948. [Google Scholar] [CrossRef] [PubMed]
- Brewer, N.T.; Chapman, G.B.; Gibbons, F.X.; Gerrard, M.; McCaul, K.D.; Weinstein, N.D. Meta-Analysis of the Relationship between Risk Perception and Health Behavior: The Example of Vaccination. Health Psychol. 2007, 26, 136–145. [Google Scholar] [CrossRef] [PubMed]
- Schweitzer, M.E.; Hershey, J.C.; Bradlow, E.T. Promises and Lies: Restoring Violated Trust. Organ. Behav. Hum. Decis. Process. 2006, 101, 1–19. [Google Scholar] [CrossRef]
- Pearson, S.D.; Raeke, L.H. Patients’ Trust in Physicians: Many Theories, Few Measures, and Little Data. J. Gen. Intern. Med. 2000, 15, 509–513. [Google Scholar] [CrossRef]
- Bruder, M.; Haffke, P.; Neave, N.; Nouripanah, N.; Imhoff, R. Measuring Individual Differences in Generic Beliefs in Conspiracy Theories Across Cultures: Conspiracy Mentality Questionnaire. Front. Psychol. 2013, 4, 225. [Google Scholar] [CrossRef]
- Smith, B.W.; Dalen, J.; Wiggins, K.; Tooley, E.; Christopher, P.; Bernard, J. The Brief Resilience Scale: Assessing the Ability to Bounce Back. Int. J. Behav. Med. 2008, 15, 194–200. [Google Scholar] [CrossRef]
- Bhatta, T.R.; Kahana, E.; Lekhak, N.; Kahana, B.; Midlarsky, E. Altruistic Attitudes Among Older Adults: Examining Construct Validity and Measurement Invariance of a New Scale. Innov. Aging 2021, 5, igaa060. [Google Scholar] [CrossRef]
- Gamliel, E.; Peer, E. Attribute Framing Affects the Perceived Fairness of Health Care Allocation Principles. Judgm. Decis. Mak. 2010, 5, 11. [Google Scholar]
- Brewer, N.T.; Chapman, G.B.; Rothman, A.J.; Leask, J.; Kempe, A. Increasing Vaccination: Putting Psychological Science Into Action. Psychol. Sci. Public Interest J. Am. Psychol. Soc. 2017, 18, 149–207. [Google Scholar] [CrossRef]
- Teixeira da Silva, D.; Biello, K.; Lin, W.Y.; Valente, P.K.; Mayer, K.H.; Hightow-Weidman, L.; Bauermeister, J.A. COVID-19 Vaccine Acceptance among an Online Sample of Sexual and Gender Minority Men and Transgender Women. Vaccines 2021, 9, 204. [Google Scholar] [CrossRef] [PubMed]
- Valckx, S.; Crèvecoeur, J.; Verelst, F.; Vranckx, M.; Hendrickx, G.; Hens, N.; Van Damme, P.; Pepermans, K.; Beutels, P.; Neyens, T. Individual Factors Influencing COVID-19 Vaccine Acceptance in between and during Pandemic Waves (July–December 2020). Vaccine 2022, 40, 151–161. [Google Scholar] [CrossRef] [PubMed]
- Killgore, W.D.S.; Cloonan, S.A.; Taylor, E.C.; Dailey, N.S. The COVID-19 Vaccine Is Here-Now Who Is Willing to Get It? Vaccines 2021, 9, 339. [Google Scholar] [CrossRef] [PubMed]
- Kiefer, M.K.; Mehl, R.; Costantine, M.M.; Landon, M.B.; Mallampati, D.; Manuck, T.A.; Rood, K.M.; Venkatesh, K.K. Association between Social Vulnerability and COVID-19 Vaccination Hesitancy in Pregnant and Postpartum Individuals. Am. J. Obstet. Gynecol. 2022, 226, S704–S705. [Google Scholar] [CrossRef]
- Morrison, T. The Impact of Politics, Religion, and Rurality on COVID-19 Vaccine Hesitancy in Oregon: A Cross-Sectional Study. Rural Remote Health 2022, 22, 7140. [Google Scholar] [CrossRef] [PubMed]
- Simanjorang, C.; Pangandaheng, N.; Tinungki, Y.; Medea, G.P. The Determinants of SARS-CoV-2 Vaccine Hesitancy in a Rural Area of an Indonesia–Philippines Border Island: A Mixed-Method Study. Enferm. Clínica Engl. Ed. 2022, in press. [Google Scholar] [CrossRef]
- Olusanya, O.A.; Bednarczyk, R.A.; Davis, R.L.; Shaban-Nejad, A. Addressing Parental Vaccine Hesitancy and Other Barriers to Childhood/Adolescent Vaccination Uptake During the Coronavirus (COVID-19) Pandemic. Front. Immunol. 2021, 12, 663074. [Google Scholar] [CrossRef]
- Newman, A.M. Moving beyond Mistrust: Centering Institutional Change by Decentering the White Analytical Lens. Bioethics 2022, 36, 267–273. [Google Scholar] [CrossRef]
- Larson, H.J.; Gakidou, E.; Murray, C.J.L. The Vaccine-Hesitant Moment. N. Engl. J. Med. 2022, 387, 58–65. [Google Scholar] [CrossRef]
- Raffetti, E.; Mondino, E.; Di Baldassarre, G. COVID-19 Vaccine Hesitancy in Sweden and Italy: The Role of Trust in Authorities. Scand. J. Public Health 2022, 50, 14034948221099410. [Google Scholar] [CrossRef]
- Gleason, J.L.; Jamison, A.; Freimuth, V.S.; Quinn, S.C. Home Remedy Use and Influenza Vaccination among African American and White Adults: An Exploratory Study. Prev. Med. 2019, 125, 19–23. [Google Scholar] [CrossRef] [PubMed]
- Guay, M.; Gosselin, V.; Petit, G.; Baron, G.; Gagneur, A. Determinants of Vaccine Hesitancy in Quebec: A Large Population-Based Survey. Hum. Vaccines Immunother. 2019, 15, 2527–2533. [Google Scholar] [CrossRef] [PubMed]
| Variable | Total n = 1426 N (%) | Rural n = 824 N (%) | Urban n = 602 N (%) | Urban vs. Rural † |
|---|---|---|---|---|
| Age (years) | ||||
| 18–34 | 334 (23.4) | 203 (24.6) | 131 (21.7) | n.s. |
| 35–49 | 355 (24.9) | 216 (26.2) | 139 (23.1) | |
| 50–64 | 391 (27.5) | 215 (26.1) | 176 (29.4) | |
| ≥64 | 346 (24.2) | 190 (23.1) | 156 (25.9) | |
| Gender | ||||
| Male | 691 (51.5) | 397 (48.2) | 294 (48.8) | n.s. |
| Female | 735 (48.5) | 427 (51.8) | 308 (51.2) | |
| Education | ||||
| Middle school or lower | 317 (22.2) | 183 (22.2) | 134 (22.2) | <0.001 |
| Vocational school | 411 (28.8) | 288 (34.9) | 123 (20.6) | |
| High school | 411 (28.8) | 234 (28.4) | 177 (29.4) | |
| University | 287 (20.1) | 119 (14.5) | 168 (27.9) | |
| Citizenship | ||||
| Italian | 1308 (91.7) | 763 (92.6) | 545 (90.5) | n.s. |
| Other | 118 (8.3) | 61 (7.4) | 57 (9.5) | |
| Native Language § | ||||
| German | 879 (61.7) | 659 (80.0) | 220 (36.6) | <0.001 |
| Italian | 384 (26.9) | 70 (8.5) | 314 (52.7) | |
| Ladin | 57 (4) | 50 (6.1) | 7 (1.2) | |
| More than one/another language | 106 (7.4) | 45 (5.5) | 61 (10.1) | |
| Household/Family structure (more than one answer possible) | ||||
| Single | 236 (16.6) | 137 (16.6) | 99 (16.4) | n.s. |
| Children 0–6 years of age | 178 (12.5) | 116 (14.1) | 62 (10.3) | 0.034 |
| Adolescents 7–17 years of age | 277 (19.4) | 174 (21.1) | 103 (17.1) | n.s. |
| COVID-19 patients at risk § | 302 (21.2) | 175 (21.2) | 127 (21.1) | n.s. |
| None of the above | 522 (36.6) | 294 (35.7) | 228 (37.9) | n.s. |
| Working in the health sector | ||||
| Yes | 85 (6) | 45 (5.5) | 40 (6.7) | n.s. |
| No | 1341 (94) | 779 (85.0) | 562 (79.6) | |
| Chronic disease(s) | ||||
| Yes | 247 (17.3) | 124 (15.0) | 123 (20.4) | 0.008 |
| No | 1179 (82.7) | 700 (85.0) | 479 (79.6) | |
| Relatives or friends died from COVID-19 | ||||
| Yes | 124 (8.7) | 61 (7.4) | 63 (10.5) | 0.043 |
| No | 1302 (91.3) | 763 (92.6) | 539 (89.5) | |
| Economic situation (last 3 months) | ||||
| Better | 43 (3) | 20 (2.4) | 23 (3.8) | 0.003 |
| The same | 974 (68.3) | 539 (65.5) | 435 (72.2) | |
| Worse | 375 (26.3) | 246 (29.8) | 129 (21.5) | |
| Don’t know | 34 (2.4) | 19 (2.3) | 15 (2.5) | |
| Non-COVID-19 vaccine hesitancy | ||||
| Non-hesitant | 157 (88.2) | 99 (85.3) | 58 (93.5) | n.s. |
| Hesitant | 21 (11.8) | 17 (14.7) | 4 (6.5) | |
| COVID-19 vaccine hesitancy | ||||
| Non-hesitant | 1204 (84.4) | 679 (82.4) | 525 (87.2) | --- |
| Hesitant | 222 (15.6) | 145 (17.6) | 77 (12.8) | |
| Rural n = 842 Nagelkerkes R2 = 0.627 | Urban n = 602 Nagelkerkes R2 = 0.577 | |||||
|---|---|---|---|---|---|---|
| Regression Coefficient B | p-Value | OR = Exp(B) [95% CI] | Regression Coefficient B | p-Value | OR = Exp(B) [95% CI] | |
| Age | −0.045 | <0.0001 | 18.196 [0.937; 0.975] | −0.024 | 0.039 | 0.976 [0.954; 0.999] |
| High Educational level # | −0.244 | n.s. | 0.784 [0.569; 1.080] | −0.252 | n.s. | 0.777 [0.549; 1.101] |
| Family and risk patterns | ||||||
| Children 0-6 years of age | 0.448 | n.s. | 1.565 [0.785; 3.121] | 0.383 | n.s. | 1.466 [0.550; 3.909] |
| A family member or relative died from COVID-19 | −0.532 | n.s. | 0.588 [0.200; 1.730] | −0.433 | n.s. | 0.648 [0.184; 2.282] |
| Chronic disease | −1.469 | 0.020 | 0.230 [0.067; 0.792] | −0.770 | n.s. | 0.463 [0.159; 1.344] |
| Search for information | 0.180 | 0.033 | 1.198 [1.104; 1.414] | 0.253 | 0.006 | 1.288 [1.074; 1.545] |
| Altruism (total score) | 0.077 | 0.014 | 1.080 [1.016; 1.149] | 0.009 | n.s. | 1.009 [0.939; 1.085] |
| Well-being (total score) | 0.021 | n.s. | 1.021 [0.937; 1.113] | −0.022 | n.s. | 0.978 [0.879; 1.088] |
| Resilience (total score) | 0.143 | 0.024 | 1.154 [1.019; 1.308] | −0.054 | n.s. | 0.948 [0.824; 1.090] |
| Trust | ||||||
| Agree with the national vaccination | −1.679 | <0.001 | 0.187 [0.128; 0.271] | −1.695 | < 0.001 | 0.184 [0.114; 0.296] |
| Trust in institutions (total score) | −0.105 | <0.001 | 0.900 [0.871; 0.930] | −0.062 | 0.003 | 0.940 [0.903; 0.979] |
| Mother tongue + | ||||||
| Italian | n.s. | n.s. | ||||
| German | −0.964 | n.s. | 0.381 [0.124; 1.168] | −0.392 | n.s. | 0.676 [0.304; 1.504] |
| Ladin | −0.744 | n.s. | 0.475 [0.111; 2.043] | −1.584 | n.s. | 0.205 [0.001; 68.762] |
| Another language | −0.227 | n.s. | 0.797 [0.191; 3.336] | 0.109 | n.s. | 1.116 [0.425; 2.931] |
| Bad Economic situation | −0.057 | n.s. | 0.945 [0.637; 1.401] | 0.130 | n.s. | 1.138 [0.425; 2.931] |
| Conspiracy thinking (total score) | 0.059 | 0.018 | 1.061 [1.010; 1.114] | 0.152 | <0.001 | 1.164 [1.085; 1.249] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barbieri, V.; Wiedermann, C.J.; Lombardo, S.; Plagg, B.; Gärtner, T.; Ausserhofer, D.; Wiedermann, W.; Engl, A.; Piccoliori, G. Rural-Urban Disparities in Vaccine Hesitancy among Adults in South Tyrol, Italy. Vaccines 2022, 10, 1870. https://doi.org/10.3390/vaccines10111870
Barbieri V, Wiedermann CJ, Lombardo S, Plagg B, Gärtner T, Ausserhofer D, Wiedermann W, Engl A, Piccoliori G. Rural-Urban Disparities in Vaccine Hesitancy among Adults in South Tyrol, Italy. Vaccines. 2022; 10(11):1870. https://doi.org/10.3390/vaccines10111870
Chicago/Turabian StyleBarbieri, Verena, Christian J. Wiedermann, Stefano Lombardo, Barbara Plagg, Timon Gärtner, Dietmar Ausserhofer, Wolfgang Wiedermann, Adolf Engl, and Giuliano Piccoliori. 2022. "Rural-Urban Disparities in Vaccine Hesitancy among Adults in South Tyrol, Italy" Vaccines 10, no. 11: 1870. https://doi.org/10.3390/vaccines10111870
APA StyleBarbieri, V., Wiedermann, C. J., Lombardo, S., Plagg, B., Gärtner, T., Ausserhofer, D., Wiedermann, W., Engl, A., & Piccoliori, G. (2022). Rural-Urban Disparities in Vaccine Hesitancy among Adults in South Tyrol, Italy. Vaccines, 10(11), 1870. https://doi.org/10.3390/vaccines10111870







