Associations between Dietary Polyphenols and Type 2 Diabetes in a Cross-Sectional Analysis of the PREDIMED-Plus Trial: Role of Body Mass Index and Sex
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Dietary Assessment and Polyphenol Intake
2.3. Ascertainment of T2D
2.4. Assessment of Covariates
2.5. Statistical Methods
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- The World Health Organization. Global Report on Diabetes; The World Health Organization: Geneva, Switzerland, 2016; ISBN 9789241565257. Available online: http://www.who.int/about/licensing/copyright_form/index.html (accessed on 15 July 2019).
- Ley, S.H.; Hamdy, O.; Mohan, V.; Hu, F.B. Prevention and management of type 2 diabetes: Dietary components and nutritional strategies. Lancet 2014, 383, 1999–2007. [Google Scholar] [CrossRef]
- Guasch-Ferré, M.; Merino, J.; Sun, Q.; Fitó, M.; Salas-Salvadó, J. Dietary Polyphenols, Mediterranean Diet, Prediabetes, and Type 2 Diabetes: A Narrative Review of the Evidence. Oxid. Med. Cell. Longev. 2017, 2017, 6723931. [Google Scholar] [CrossRef] [PubMed]
- Babu, P.V.A.; Liu, D.; Gilbert, E.R. Recent advances in understanding the anti-diabetic actions of dietary flavonoids. J. Nutr. Biochem. 2013, 24, 1777–1789. [Google Scholar] [CrossRef] [PubMed]
- Marques, C.; Fernandes, I.; Norberto, S.; Sá, C.; Teixeira, D.; de Freitas, V.; Mateus, N.; Calhau, C.; Faria, A. Pharmacokinetics of blackberry anthocyanins consumed with or without ethanol: A randomized and crossover trial. Mol. Nutr. Food Res. 2016, 60, 2319–2330. [Google Scholar] [CrossRef] [PubMed]
- Novotny, J.A.; Chen, T.Y.; Terekhov, A.I.; Gebauer, S.K.; Baer, D.J.; Ho, L.; Pasinetti, G.M.; Ferruzzi, M.G. The effect of obesity and repeated exposure on pharmacokinetic response to grape polyphenols in humans. Mol. Nutr. Food Res. 2017, 61. [Google Scholar] [CrossRef] [PubMed]
- Manach, C.; Scalbert, A.; Morand, C.; Rémésy, C.; Jiménez, L. Polyphenols: food sources and bioavailability. Am. J. Clin. Nutr. 2004, 79, 727–747. [Google Scholar] [CrossRef]
- Martínez-González, M.A.; Buil-Cosiales, P.; Corella, D.; Bulló, M.; Fitó, M.; Vioque, J.; Romaguera, D.; Martínez, J.A.; Wärnberg, J.; López-Miranda, J.; et al. Cohort Profile: Design and methods of the PREDIMED-Plus randomized trial. Int. J. Epidemiol. 2018, 48, 387o–388o. [Google Scholar] [CrossRef]
- Willett, W.C.; Howe, G.R.; Kushi, L.H. Adjustment for total energy intake in epidemiologic studies. Am. J. Clin. Nutr. 1997, 65, 1220S–1228S, discussion 1229S–1231S. [Google Scholar] [CrossRef]
- Fernández-Ballart, J.D.; Piñol, J.L.; Zazpe, I.; Corella, D.; Carrasco, P.; Toledo, E.; Perez-Bauer, M.; Martínez-González, M.A.; Salas-Salvadó, J.; Martín-Moreno, J.M. Relative validity of a semi-quantitative food-frequency questionnaire in an elderly Mediterranean population of Spain. Br. J. Nutr. 2010, 103, 1808–1816. [Google Scholar] [CrossRef]
- Mataix, J. Tablas de Composición de Alimentos [Food Composition Tables], 4th ed.; Universidad de Granada: Granada, Spain, 2003. [Google Scholar]
- Moreiras, O.; Carbajal, A.; Cabrera, L.; Hoyos, M.D.C.C. Tablas de Composición de Alimentos. Guía de Prácticas; Ediciones Pirámide (Grupo Anaya, SA): Madrid, Spain, 2018. [Google Scholar]
- Schröder, H.; Fitó, M.; Estruch, R.; Martínez-González, M.A.; Corella, D.; Salas-Salvadó, J.; Lamuela-Raventós, R.; Ros, E.; Salaverría, I.; Fiol, M.; et al. A Short Screener is Valid for Assessing Mediterranean Diet Adherence among Older Spanish Men and Women. J. Nutr. 2011, 141, 1140–1145. [Google Scholar] [CrossRef]
- Medina-Remón, A.; Barrionuevo-González, A.; Zamora-Ros, R.; Andres-Lacueva, C.; Estruch, R.; Martínez-González, M.-A.; Diez-Espino, J.; Lamuela-Raventos, R.M. Rapid Folin-Ciocalteu method using microtiter 96-well plate cartridges for solid phase extraction to assess urinary total phenolic compounds, as a biomarker of total polyphenols intake. Anal. Chim. Acta 2009, 634, 54–60. [Google Scholar] [CrossRef] [PubMed]
- Medina-Remón, A.; Tresserra-Rimbau, A.; Arranz, S.; Estruch, R.; Lamuela-Raventos, R.M. Polyphenols excreted in urine as biomarkers of total polyphenol intake. Bioanalysis 2012, 4, 2705–2713. [Google Scholar] [CrossRef] [PubMed]
- Elosua, R.; Marrugat, J.; Molina, L.; Pons, S.; Pujol, E. Validation of the Minnesota Leisure Time Physical Activity Questionnaire in Spanish men. The MARATHOM Investigators. Am. J. Epidemiol. 1994, 139, 1197–1209. [Google Scholar] [CrossRef] [PubMed]
- Barros, A.J.D.; Hirakata, V.N. Alternatives for logistic regression in cross-sectional studies: An empirical comparison of models that directly estimate the prevalence ratio. BMC Med. Res. Methodol. 2003, 3, 21. [Google Scholar] [CrossRef] [PubMed]
- Zamora-Ros, R.; Forouhi, N.G.; Sharp, S.J.; González, C.A.; Buijsse, B.; Guevara, M.; van der Schouw, Y.T.; Amiano, P.; Boeing, H.; Bredsdorff, L.; et al. Dietary intakes of individual flavanols and flavonols are inversely associated with incident type 2 diabetes in European populations. J. Nutr. 2014, 144, 335–343. [Google Scholar] [CrossRef] [PubMed]
- Eng, Q.Y.; Thanikachalam, P.V.; Ramamurthy, S. Molecular understanding of Epigallocatechin gallate (EGCG) in cardiovascular and metabolic diseases. J. Ethnopharmacol. 2018, 210, 296–310. [Google Scholar] [CrossRef] [PubMed]
- Burton-Freeman, B.; Brzeziński, M.; Park, E.; Sandhu, A.; Xiao, D.; Edirisinghe, I. A selective role of dietary anthocyanins and flavan-3-ols in reducing the risk of type 2 diabetes mellitus: A review of recent evidence. Nutrients 2019, 11, 841. [Google Scholar] [CrossRef]
- Lin, X.; Zhang, I.; Li, A.; Manson, J.E.; Sesso, H.D.; Wang, L.; Liu, S. Cocoa Flavanol Intake and Biomarkers for Cardiometabolic Health: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. J. Nutr. 2016, 146, 2325–2333. [Google Scholar] [CrossRef]
- Zamora-Ros, R.; Forouhi, N.G.; Sharp, S.J.; González, C.A.; Buijsse, B.; Guevara, M.; van der Schouw, Y.T.; Amiano, P.; Boeing, H.; Bredsdorff, L.; et al. The association between dietary flavonoid and lignan intakes and incident type 2 diabetes in European populations: The EPIC-InterAct study. Diabetes Care 2013, 36, 3961–3970. [Google Scholar] [CrossRef]
- Jennings, A.; Welch, A.A.; Spector, T.; Macgregor, A.; Cassidy, A. Intakes of anthocyanins and flavones are associated with biomarkers of insulin resistance and inflammation in women. J. Nutr. 2014, 144, 202–208. [Google Scholar] [CrossRef]
- Wedick, N.M.; Pan, A.; Cassidy, A.; Rimm, E.B.; Sampson, L.; Rosner, B.; Willett, W.; Hu, F.B.; Sun, Q.; van Dam, R.M. Dietary flavonoid intakes and risk of type 2 diabetes in US men and women. Am. J. Clin. Nutr. 2012, 95, 925–933. [Google Scholar] [CrossRef] [PubMed]
- Salas-Salvadó, J.; Martinez-González, M.Á.; Bulló, M.; Ros, E. The role of diet in the prevention of type 2 diabetes. Nutr. Metab. Cardiovasc. Dis. 2011, 21, B32–B48. [Google Scholar] [CrossRef] [PubMed]
- Bidel, S.; Tuomilehto, J. The Emerging Health Benefits of Coffee with an Emphasis on Type 2 Diabetes and Cardiovascular Disease. Eur. Endocrinol. 2010, 9, 99. [Google Scholar] [CrossRef] [PubMed]
- Lane, J.D.; Barkauskas, C.E.; Surwit, R.S.; Feinglos, M.N. Caffeine impairs glucose metabolism in type 2 diabetes. Diabetes Care 2004, 27, 2047–2048. [Google Scholar] [CrossRef][Green Version]
- Tresserra-Rimbau, A.; Guasch-Ferré, M.; Salas-Salvadó, J.; Toledo, E.; Corella, D.; Castañer, O.; Guo, X.; Gómez-Gracia, E.; Lapetra, J.; Arós, F.; et al. Intake of Total Polyphenols and Some Classes of Polyphenols Is Inversely Associated with Diabetes in Elderly People at High Cardiovascular Disease Risk. J. Nutr. 2016, 146, 767–777. [Google Scholar] [CrossRef]
- Bagul, P.K.; Banerjee, S.K. Application of resveratrol in diabetes: Rationale, strategies and challenges. Curr. Mol. Med. 2015, 15, 312–330. [Google Scholar] [CrossRef]
- Vallianou, N.G.; Evangelopoulos, A.; Kazazis, C. Resveratrol and diabetes. Rev. Diabet. Stud. 2013, 10, 236–242. [Google Scholar] [CrossRef]
- Rezaeiamiri, E.; Bahramsoltani, R.; Rahimi, R. Plant-derived natural agents as dietary supplements for the regulation of glycosylated hemoglobin: A review of clinical trials. Clin. Nutr. 2019, 10. [Google Scholar] [CrossRef]
- Talaei, M.; Pan, A. Role of phytoestrogens in prevention and management of type 2 diabetes. World J. Diabetes 2015, 6, 271–283. [Google Scholar] [CrossRef]
- Sun, Q.; Wedick, N.M.; Pan, A.; Townsend, M.K.; Cassidy, A.; Franke, A.A.; Rimm, E.B.; Hu, F.B.; van Dam, R.M. Gut microbiota metabolites of dietary lignans and risk of type 2 diabetes: A prospective investigation in two cohorts of U.S. women. Diabetes Care 2014, 37, 1287–1295. [Google Scholar] [CrossRef]
- Sun, Q.; Wedick, N.M.; Tworoger, S.S.; Pan, A.; Townsend, M.K.; Cassidy, A.; Franke, A.A.; Rimm, E.B.; Hu, F.B.; van Dam, R.M. Urinary Excretion of Select Dietary Polyphenol Metabolites is Associated with a Lower Risk of Type 2 Diabetes in Proximate but Not Remote Follow-Up in a Prospective Investigation in 2 Cohorts of US Women. J. Nutr. 2015, 145, 1280–1288. [Google Scholar] [CrossRef] [PubMed]
- Jacques, P.F.; Cassidy, A.; Rogers, G.; Peterson, J.J.; Meigs, J.B.; Dwyer, J.T. Higher dietary flavonol intake is associated with lower incidence of type 2 diabetes. J. Nutr. 2013, 143, 1474–1480. [Google Scholar] [CrossRef] [PubMed]
- Scalbert, A.; Manach, C.; Morand, C.; Rémésy, C.; Jiménez, L. Dietary polyphenols and the prevention of diseases. Crit. Rev. Food Sci. Nutr. 2005, 45, 287–306. [Google Scholar] [CrossRef] [PubMed]
- Tresserra-Rimbau, A.; Lamuela-Raventos, R.M.; Moreno, J.J. Polyphenols, food and pharma. Current knowledge and directions for future research. Biochem. Pharmacol. 2018, 156, 186–195. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 | p-Value |
|---|---|---|---|---|---|
| n | 1659 | 1658 | 1658 | 1658 | |
| Total polyphenols (mg/day), median (min–max) | 561 (73–662) | 736 (663–812) | 896 (813–994) | 1146 (995–3377) | |
| Sex, males, n (%) | 775 (46.7) | 871 (47.5) | 775 (53.3) | 679 (59.1) | <0.001 |
| Age (years) | 64.9 ± 4.9 | 65.0 ± 4.8 | 65.0 ± 4.9 | 65.1 ± 5.0 | 0.65 |
| Body mass index (kg/m2) | 32.6 ± 3.5 | 32.6 ± 3.5 | 32.6 ± 3.5 | 32.4 ± 3.3 | 0.07 |
| Diabetic, n (%) | 489 (29.5) | 523 (31.5) | 519 (31.3) | 511 (30.8) | 0.57 |
| Insulin, n (%) | 82 (4.9) | 88 (5.3) | 76 (4.6) | 68 (4.1) | 0.40 |
| Metformin, n (%) | 356 (21.5) | 405 (24.4) | 394 (23.8) | 389 (23.5) | 0.21 |
| Other glucose lowering medication, n (%) | 306 (18.4) | 342 (20.6) | 341 (20.6) | 336 (20.3) | 0.35 |
| Fasting glucose (mg/dL) | 113 ± 29 | 113 ± 29 | 114 ± 31 | 113 ± 28 | 0.59 |
| Glycated hemoglobin (mmol/L) | 6.1 ± 0.9 | 6.1 ± 0.8 | 6.1 ± 1.0 | 6.1 ± 0.8 | 0.54 |
| Physical activity, (METS·min/week) | 2252 ± 2216 | 2434 ± 2249 | 2437 ± 2275 | 2733 ± 2435 | <0.001 |
| Smoking status, n (%) | |||||
| Smoker | 231 (13.9) | 235 (14.2) | 242 (14.6) | 258 (15.6) | <0.001 |
| Former, >1 year | 623 (37.6) | 642 (38.7) | 709 (42.8) | 762 (46.0) | |
| Never | 804 (48.5) | 780 (47.0) | 706 (42.6) | 638 (38.5) | |
| Education level, n (%) | |||||
| High | 308 (18.6) | 319 (19.2) | 363 (21.9) | 464 (28.0) | <0.001 |
| Medium | 484 (29.2) | 467 (28.2) | 485 (29.3) | 477 (28.8) | |
| Low | 867 (52.3) | 872 (52.6) | 810 (48.8) | 717 (43.2) |
| Nutrients and Foods | Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 | p-Value |
|---|---|---|---|---|---|
| n | 1659 | 1658 | 1658 | 1658 | |
| Total energy (kJ/day) (kcal/day) | 10272 ± 2293 (2454 ± 548) | 9481 ± 2256 (2265 ± 539) | 9670 ± 2293 (2310 ± 548) | 10180 ± 2294 (2432 ± 548) | <0.001 |
| Carbohydrates (g/day) | 246 ± 75 | 229 ± 70 | 237 ± 71 | 251 ± 73 | <0.001 |
| Fiber (g/day) | 23 ± 7 | 25 ± 8 | 27 ± 8 | 30 ± 10 | <0.001 |
| Proteins (g/day) | 100 ± 22 | 95 ± 22 | 96 ± 22 | 99 ± 22 | <0.001 |
| MUFAs (g/day) | 57 ± 16 | 52 ± 16 | 52 ± 16 | 54 ± 16 | <0.001 |
| PUFAs (g/day) | 18 ± 7 | 16 ± 6 | 16 ± 6 | 17 ± 6 | <0.001 |
| SFAs (g/day) | 28 ± 9 | 25 ± 8 | 25 ± 8 | 26 ± 9 | <0.001 |
| Alcohol (g/day) | 10 ± 14 | 10 ± 14 | 11 ± 14 | 14 ± 17 | <0.001 |
| 17-point MedDiet score | 7.7 ± 2.5 | 8.5 ± 2.6 | 8.7 ± 2.6 | 9.2 ± 2.7 | <0.001 |
| Food items (g/day) | |||||
| Vegetables | 299 ± 125 | 319 ± 129 | 336 ± 134 | 357 ± 160 | <0.001 |
| Fruits | 262 ± 146 | 324 ± 160 | 381 ± 181 | 470 ± 261 | <0.001 |
| Legumes | 21 ± 11 | 21 ± 11 | 20 ± 11 | 21 ± 12 | 0.23 |
| Cereals | 164 ± 83 | 144 ± 74 | 147 ± 77 | 146 ± 77 | <0.001 |
| Dairy | 358 ± 205 | 338 ± 193 | 341 ± 196 | 347 ± 211 | 0.02 |
| Meat | 160 ± 62 | 145 ± 58 | 143 ± 56 | 143 ± 56 | <0.001 |
| Olive oil | 43 ± 18 | 39 ± 17 | 39 ± 16 | 39 ± 16 | <0.001 |
| Fish | 101 ± 50 | 101 ± 48 | 102 ± 45 | 105 ± 47 | 0.05 |
| Nuts | 13 ± 16 | 14 ± 17 | 15 ± 17 | 17 ± 19 | <0.001 |
| Cookies, pastries, and sweets | 27 ± 31 | 23 ± 28 | 25 ± 28 | 32 ± 32 | <0.001 |
| Sugar | 8 ± 13 | 7 ± 11 | 6 ± 11 | 6 ± 12 | <0.001 |
| Soft drinks | 31 ± 82 | 20 ± 56 | 20 ± 62 | 16 ± 51 | <0.001 |
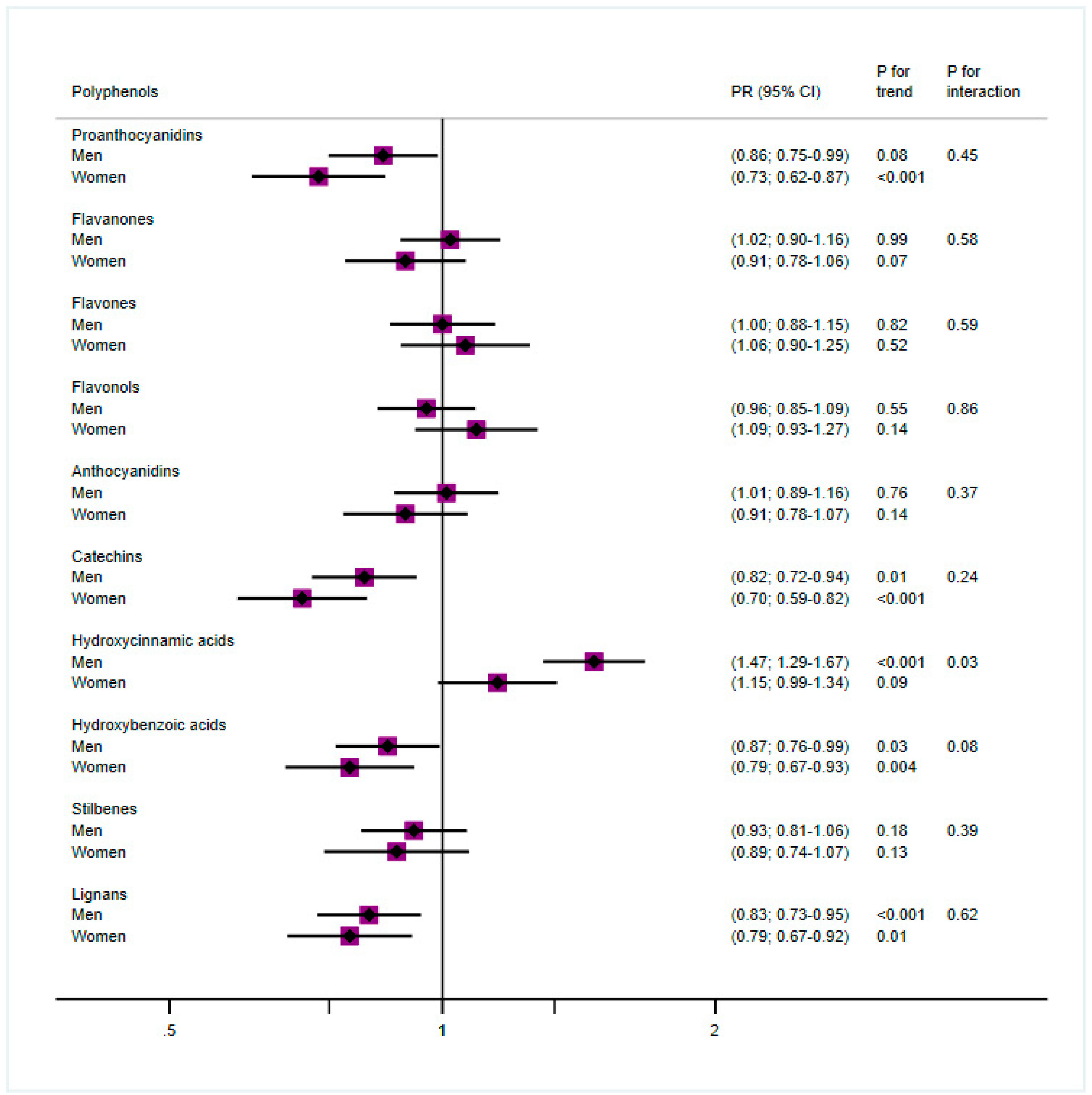
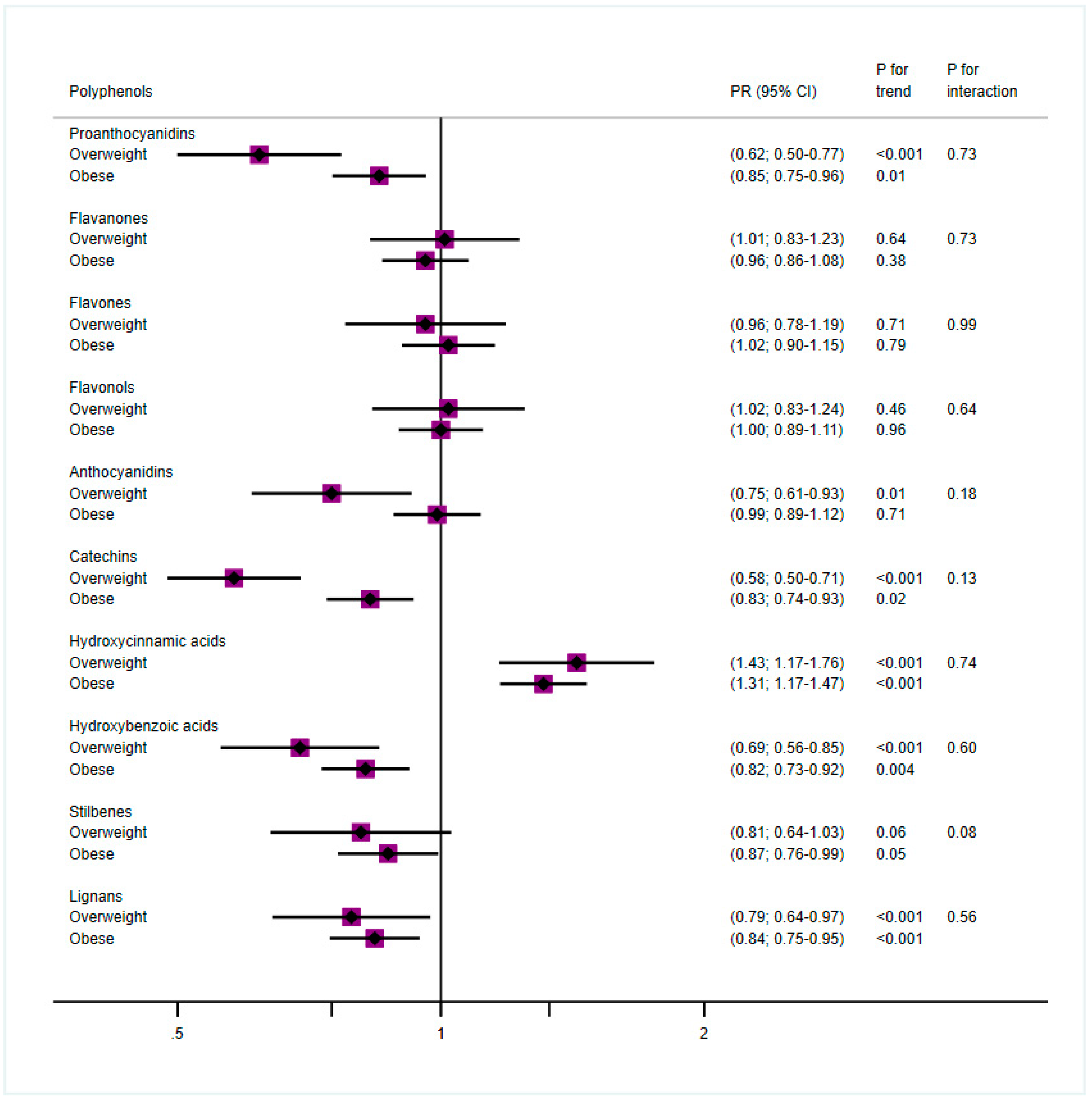
| Men | Women | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Overweight (BMI < 30) | Obese (BMI ≥ 30) | Overweight (BMI < 30) | Obese (BMI ≥ 30) | ||||||||||
| n = 971 (314 cases, 32%) | n = 2453 (828 cases, 34%) | n = 802 (194 cases, 24%) | n = 2407 (706 cases, 29%) | ||||||||||
| Q4 vs. Q1 | p-value | p-trend | Q4 vs. Q1 | p-value | p-trend | Q4 vs. Q1 | p-value | p-trend | Q4 vs. Q1 | p-value | p-trend | ||
| Proanthocyanidins | Mean intake, mg/day | 458.9 vs. 63.5 | 434.2 vs. 53.1 | 435.3 vs. 57.9 | 415.3 vs. 51.4 | ||||||||
| Cases | 69 vs. 87 | 179 vs. 188 | 33 vs. 54 | 153 vs. 190 | |||||||||
| PR (CI)—unadjusted | 0.81 (0.62–1.05) | 0.11 | 0.18 | 0.96 (0.67–1.14) | 0.67 | 0.79 | 0.62 (0.42–0.91) | 0.02 | 0.01 | 0.81 (0.67–0.97) | 0.02 | 0.02 | |
| PR (CI)—model 1 | 0.81 (0.63–1.05) | 0.12 | 0.20 | 0.98 (0.83–1.17) | 0.83 | 0.95 | 0.64 (0.43–0.94) | 0.02 | 0.01 | 0.82 (0.68–0.98) | 0.03 | 0.03 | |
| PR (CI)—model 2 | 0.75 (0.59–0.95) | 0.02 | 0.04 | 0.93 (0.79–1.11) | 0.43 | 0.48 | 0.51 (0.34–0.76) | 0.001 | <0.001 | 0.79 (0.66–0.95) | 0.01 | 0.01 | |
| Flavanones | Mean intake, mg/day | 185.3 vs. 16.6 | 180.4 vs. 16.8 | 179.8 vs. 17.6 | 183.6 vs. 15.3 | ||||||||
| Cases | 90 vs. 74 | 211 vs. 203 | 48 vs. 53 | 179 vs. 184 | |||||||||
| PR (CI)—unadjusted | 1.22 (0.95–1.57) | 0.11 | 0.37 | 1.04 (0.89–1.22) | 0.59 | 0.47 | 0.92 (0.66–1.30) | 0.65 | 0.67 | 0.98 (0.82–1.16) | 0.80 | 0.47 | |
| PR (CI)—model 1 | 1.26 (0.98–1.62) | 0.07 | 0.26 | 1.05 (0.90–1.23) | 0.54 | 0.43 | 0.94 (0.67–1.33) | 0.74 | 0.72 | 0.96 (0.81–1.14) | 0.67 | 0.35 | |
| PR (CI)—model 2 | 1.05 (0.84–1.32) | 0.66 | 0.86 | 0.98 (0.85–1.15) | 0.84 | 0.93 | 0.82 (0.58–1.16) | 0.26 | 0.24 | 0.92 (0.78–1.09) | 0.35 | 0.12 | |
| Flavones | Mean intake, mg/day | 126.4 vs. 29.7 | 131.2 vs. 30.3 | 131.8 vs. 32.0 | 139.6 vs. 31.4 | ||||||||
| Cases | 92 vs. 65 | 219 vs. 183 | 49 vs. 45 | 181 vs. 157 | |||||||||
| PR (CI)—unadjusted | 1.41 (1.08–1.83) | 0.01 | 0.004 | 1.21 (1.03–1.42) | 0.02 | 0.01 | 1.11 (0.78–1.59) | 0.54 | 0.87 | 1.16 (0.96–1.39) | 0.12 | 0.13 | |
| PR (CI)—model 1 | 1.42 (1.09–1.86) | 0.01 | 0.003 | 1.22 (1.03–1.43) | 0.02 | 0.009 | 1.16 (0.81–1.65) | 0.43 | 0.69 | 1.18 (0.98–1.41) | 0.08 | 0.08 | |
| PR (CI)—model 2 | 1.00 (0.78–1.29) | 0.99 | 0.65 | 0.99 (0.84–1.16) | 0.90 | 0.90 | 0.94 (0.66–1.34) | 0.73 | 0.50 | 1.08 (0.90–1.31) | 0.39 | 0.35 | |
| Flavonols | Mean intake, mg/day | 84.1 vs. 29.4 | 83.2 vs. 29.1 | 81.6 vs. 32.0 | 83.6 vs. 29.9 | ||||||||
| Cases | 87 vs. 73 | 228 vs. 201 | 53 vs. 44 | 184 vs. 179 | |||||||||
| PR (CI)—unadjusted | 1.24 (0.96–1.60) | 0.11 | 0.06 | 1.13 (0.97–1.32) | 0.11 | 0.18 | 1.22 (0.86–1.73) | 0.26 | 0.14 | 1.03 (0.87–1.23) | 0.72 | 0.54 | |
| PR (CI)—model 1 | 1.25 (0.96–1.62) | 0.10 | 0.05 | 1.13 (0.97–1.32) | 0.12 | 0.21 | 1.27 (0.89–1.81) | 0.11 | 0.09 | 1.09 (0.91–1.29) | 0.34 | 0.25 | |
| PR (CI)—model 2 | 0.97 (0.76–1.23) | 0.79 | 0.95 | 0.96 (0.83–1.12) | 0.62 | 0.45 | 1.16 (0.82–1.64) | 0.40 | 0.19 | 1.05 (0.89–1.25) | 0.57 | 0.50 | |
| Anthocyanidins | Mean intake, mg/day | 94.9 vs. 13.9 | 97.6 vs. 13.3 | 82.0 vs. 11.8 | 87.5 vs. 10.1 | ||||||||
| Cases | 67 vs. 73 | 224 vs. 174 | 47 vs. 47 | 172 vs. 185 | |||||||||
| PR (CI)—unadjusted | 0.93 (0.70–1.23) | 0.60 | 0.29 | 1.29 (1.10–1.52) | 0.002 | 0.005 | 1.02 (0.72–1.45) | 0.90 | 0.93 | 0.93 (0.79–1.11) | 0.44 | 0.28 | |
| PR (CI)—model 1 | 0.93 (0.70–1.23) | 0.61 | 0.29 | 1.28 (1.09–1.51) | 0.003 | 0.007 | 1.07 (0.75–1.54) | 0.62 | 0.91 | 0.93 (0.79–1.11) | 0.45 | 0.27 | |
| PR (CI)—model 2 | 0.80 (0.62–1.05) | 0.14 | 0.02 | 1.10 (0.94–1.29) | 0.22 | 0.30 | 0.89 (0.63–1.26) | 0.50 | 0.32 | 0.93 (0.78–1.10) | 0.38 | 0.24 | |
| Catechins | Mean intake, mg /day | 57.9 vs. 10.3 | 58.7 vs. 9.7 | 55.3 vs. 8.9 | 53.4 vs. 8.2 | ||||||||
| Cases | 68 vs. 92 | 194 vs. 198 | 34 vs. 67 | 144 vs. 200 | |||||||||
| PR (CI)—unadjusted | 0.75 (0.58–0.97) | 0.03 | 0.03 | 0.99 (0.84–1.17) | 0.92 | 0.69 | 0.51 (0.36–0.73) | 0.001 | <0.001 | 0.72 (0.60–0.86) | <0.001 | <0.001 | |
| PR (CI)—model 1 | 0.76 (0.58–0.98) | 0.03 | 0.04 | 1.01 (0.86–1.19) | 0.88 | 0.52 | 0.53 (0.37–0.77) | 0.001 | 0.002 | 0.75 (0.62–0.90) | 0.002 | 0.002 | |
| PR (CI)—model 2 | 0.64 (0.51–0.81) | <0.001 | <0.001 | 0.91 (0.77–1.06) | 0.23 | 0.50 | 0.48 (0.33–0.69) | <0.001 | <0.001 | 0.77 (0.64–0.92) | 0.004 | 0.003 | |
| Hydroxycinnamic acids | Mean intake, mg/day | 435.3 vs. 122.3 | 457.0 vs. 127.2 | 407.2 vs. 123.6 | 426.1 vs. 125.7 | ||||||||
| Cases | 97 vs. 63 | 244 vs. 180 | 45 vs. 50 | 195 vs. 174 | |||||||||
| PR (CI)—unadjusted | 1.54 (1.18–2.00) | 0.001 | 0.003 | 1.36 (1.16–1.59) | <0.001 | <0.001 | 1.13 (0.80–1.61) | 0.49 | 0.46 | 1.13 (0.95–1.33) | 0.17 | 0.19 | |
| PR (CI)—model 1 | 1.52 (1.17–1.98) | 0.002 | 0.005 | 1.35 (1.16–1.58) | <0.001 | <0.001 | 1.14 (0.81–1.62) | 0.45 | 0.44 | 1.12 (0.94–1.33) | 0.20 | 0.20 | |
| PR (CI)—model 2 | 1.62 (1.26–2.08) | <0.001 | <0.001 | 1.43 (1.23–1.66) | <0.001 | <0.001 | 1.15 (0.82–1.62) | 0.41 | 0.40 | 1.16 (0.98–1.37) | 0.08 | 0.09 | |
| Hydroxybenzoic acids | Mean intake, mg/day | 30.7 vs. 6.5 | 31.7 vs. 5.8 | 24.2 vs. 5.2 | 22.3 vs. 4.2 | ||||||||
| Cases | 72 vs. 78 | 208 vs. 197 | 38 vs. 59 | 149 vs. 191 | |||||||||
| PR (CI)—unadjusted | 0.93 (0.71–1.22) | 0.61 | 0.32 | 1.06 (0.90–1.24) | 0.48 | 0.36 | 0.65 (0.45–0.93) | 0.02 | 0.02 | 0.78 (0.65–0.94) | 0.008 | 0.005 | |
| PR (CI)—model 1 | 0.93 (0.71–1.22) | 0.61 | 0.32 | 1.05 (0.89–1.23) | 0.56 | 0.44 | 0.68 (0.47–0.97) | 0.04 | 0.04 | 0.82 (0.68–0.99) | 0.04 | 0.03 | |
| PR (CI)—model 2 | 0.76 (0.60–0.97) | 0.03 | 0.01 | 0.92 (0.79–1.07) | 0.28 | 0.34 | 0.62 (0.43–0.89) | 0.01 | 0.01 | 0.83 (0.69–1.00) | 0.05 | 0.04 | |
| Stilbenes | Mean intake, mg/day | 9.9 vs. 0.0 | 9.9 vs. 0.0 | 3.86 vs. 0.00 | 3.04 vs. 0.00 | ||||||||
| Cases | 68 vs. 71 | 221 vs. 191 | 44 vs. 42 | 148 vs. 185 | |||||||||
| PR (CI)—unadjusted | 0.99 (0.74–1.31) | 0.93 | 0.50 | 1.16 (0.99–1.36) | 0.07 | 0.09 | 1.04 (0.72–1.52) | 0.74 | 0.83 | 0.81 (0.67–0.97) | 0.03 | 0.02 | |
| PR (CI)—model 1 | 0.99 (0.75–1.32) | 0.97 | 0.54 | 1.16 (0.99–1.36) | 0.07 | 0.09 | 1.10 (0.75–1.59) | 0.55 | 0.63 | 0.83 (0.69–1.00) | 0.05 | 0.04 | |
| PR (CI)—model 2 | 0.80 (0.61–1.05) | 0.12 | 0.03 | 0.99 (0.84–1.16) | 0.78 | 0.97 | 0.92 (0.61–1.37) | 0.68 | 0.63 | 0.86 (0.70–1.06) | 0.15 | 0.12 | |
| Lignans | Mean intake, mg/day | 2.20 vs. 1.00 | 2.22 vs. 1.00 | 2.12 vs. 1.33 | 2.15 vs. 1.00 | ||||||||
| Cases | 71 vs. 75 | 221 vs. 207 | 44 vs. 47 | 156 vs. 197 | |||||||||
| PR (CI)—unadjusted | 0.93 (0.71–1.22) | 0.61 | 0.52 | 1.06 (0.91–1.24) | 0.44 | 0.71 | 0.95 (0.66–1.36) | 0.77 | 0.61 | 0.80 (0.67–0.95) | 0.012 | 0.005 | |
| PR (CI)—model 1 | 0.94 (0.66–1.24) | 0.66 | 0.59 | 1.07 (0.91–1.25) | 0.95 | 0.65 | 1.00 (0.69–1.45) | 0.99 | 0.81 | 0.81 (0.68–0.97) | 0.02 | 0.01 | |
| PR (CI)—model 2 | 0.70 (0.54–0.90) | 0.005 | 0.004 | 0.88 (0.76–1.03) | 0.06 | 0.04 | 0.88 (0.61–1.26) | 0.47 | 0.34 | 0.77 (0.64–0.92) | 0.004 | 0.002 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tresserra-Rimbau, A.; Castro-Barquero, S.; Vitelli-Storelli, F.; Becerra-Tomas, N.; Vázquez-Ruiz, Z.; Díaz-López, A.; Corella, D.; Castañer, O.; Romaguera, D.; Vioque, J.; et al. Associations between Dietary Polyphenols and Type 2 Diabetes in a Cross-Sectional Analysis of the PREDIMED-Plus Trial: Role of Body Mass Index and Sex. Antioxidants 2019, 8, 537. https://doi.org/10.3390/antiox8110537
Tresserra-Rimbau A, Castro-Barquero S, Vitelli-Storelli F, Becerra-Tomas N, Vázquez-Ruiz Z, Díaz-López A, Corella D, Castañer O, Romaguera D, Vioque J, et al. Associations between Dietary Polyphenols and Type 2 Diabetes in a Cross-Sectional Analysis of the PREDIMED-Plus Trial: Role of Body Mass Index and Sex. Antioxidants. 2019; 8(11):537. https://doi.org/10.3390/antiox8110537
Chicago/Turabian StyleTresserra-Rimbau, Anna, Sara Castro-Barquero, Facundo Vitelli-Storelli, Nerea Becerra-Tomas, Zenaida Vázquez-Ruiz, Andrés Díaz-López, Dolores Corella, Olga Castañer, Dora Romaguera, Jesús Vioque, and et al. 2019. "Associations between Dietary Polyphenols and Type 2 Diabetes in a Cross-Sectional Analysis of the PREDIMED-Plus Trial: Role of Body Mass Index and Sex" Antioxidants 8, no. 11: 537. https://doi.org/10.3390/antiox8110537
APA StyleTresserra-Rimbau, A., Castro-Barquero, S., Vitelli-Storelli, F., Becerra-Tomas, N., Vázquez-Ruiz, Z., Díaz-López, A., Corella, D., Castañer, O., Romaguera, D., Vioque, J., Alonso-Gómez, Á. M., Wärnberg, J., Martínez, J. A., Serra-Majem, L., Estruch, R., Tinahones, F. J., Lapetra, J., Pintó, X., Tur, J. A., ... Salas-Salvadó, J. (2019). Associations between Dietary Polyphenols and Type 2 Diabetes in a Cross-Sectional Analysis of the PREDIMED-Plus Trial: Role of Body Mass Index and Sex. Antioxidants, 8(11), 537. https://doi.org/10.3390/antiox8110537




















