Visual Dysfunction in Parkinson’s Disease
Abstract
1. Introduction
2. Ocular and Visual Impairments in Parkinson’s Disease
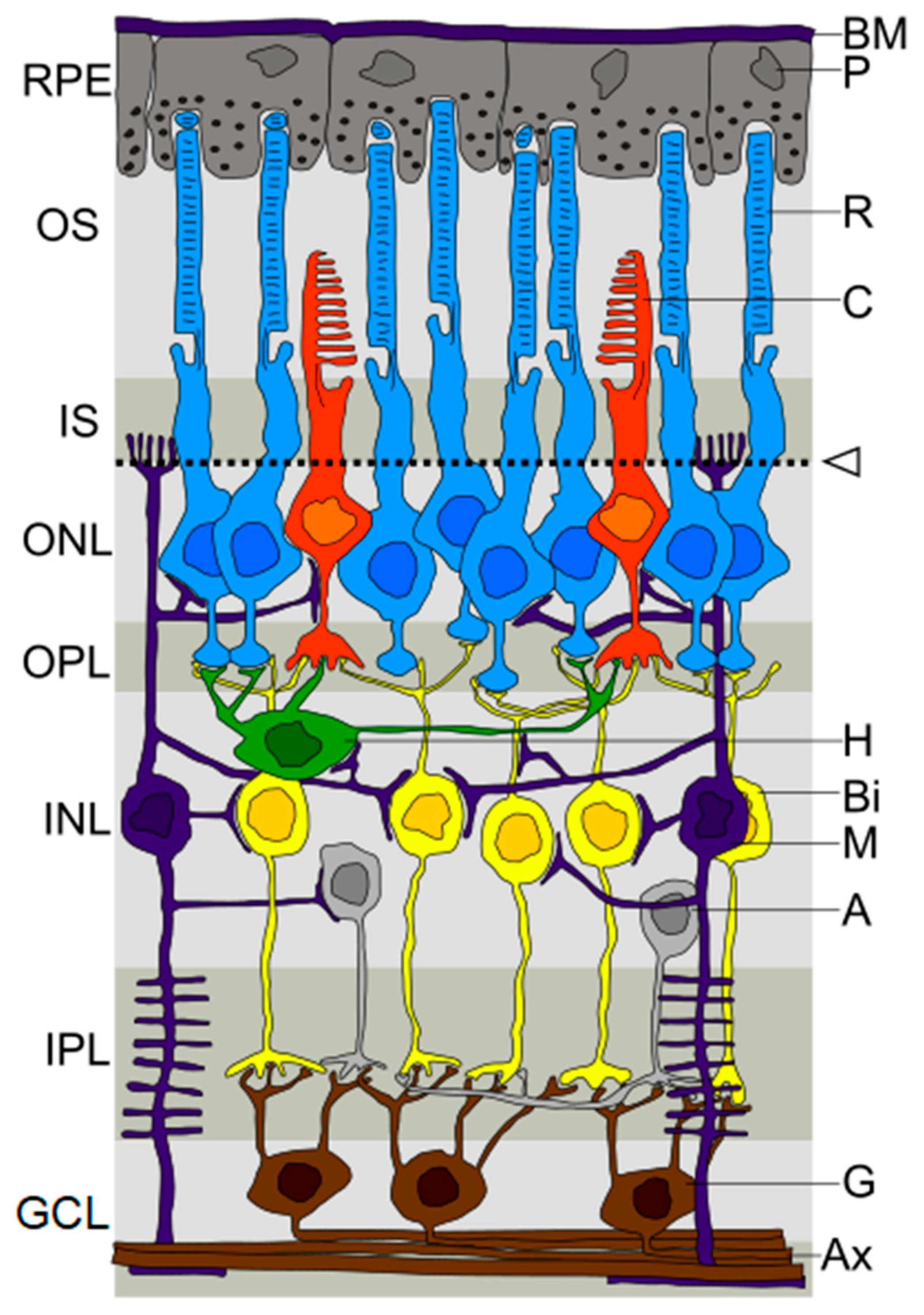
2.1. Retinal Changes
2.2. Glaucomatous Disturbances
2.3. Pupil Reactivity
2.4. Eyelid and Blink Reflex
2.5. Visual Acuity, Contrast Sensitivity, and Color Vision in PD
2.6. Visual Hallucinations
3. Visual Cognition Impairments in Parkinson’s Disease
3.1. Visuospatial Impairment
3.2. Visuoperceptive Impairment
3.3. Visuoconstructive Impairment
4. Side-of-Onset and Type of Parkinson’s Disease in Relation to Visual Symptoms
5. Gender Influence in Visuospatial Symptoms in Parkinson’s Disease
6. Neuroanatomical Correlates of Visuospatial and Visuoperceptive Deficits in Parkinson’s Disease
7. Functional Neuroimage Correlates of VS/VP Deficits in Parkinsons’ Disease
8. Neuroanatomical Correlates of Parkinson’s Disease Visual Hallucinations
9. Functional Neuroimage Correlates of Parkinsons’ Disease Visual Hallucinations
10. Neurochemistry of VS/VP Deficits in Parkinsons’ Disease
11. Genetic Factors of VS/VP Deficits in Parkinsons’ Disease
12. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lee, A.; Gilbert, R.M. Epidemiology of Parkinson Disease. Neurol. Clin. 2016, 34, 955–965. [Google Scholar] [CrossRef]
- Poewe, W.; Seppi, K.; Tanner, C.M.; Halliday, G.M.; Brundin, P.; Volkmann, J.; Schrag, A.-E.; Lang, A.E. Parkinson disease. Nat. Rev. Dis. Primer 2017, 3, 17013. [Google Scholar] [CrossRef] [PubMed]
- Zhai, S.; Tanimura, A.; Graves, S.M.; Shen, W.; Surmeier, D.J. Striatal synapses, circuits, and Parkinson’s disease. Curr. Opin. Neurobiol. 2018, 48, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Lemke, M.R.; Fuchs, G.; Gemende, I.; Herting, B.; Oehlwein, C.; Reichmann, H.; Rieke, J.; Volkmann, J. Depression and Parkinson’s disease. J. Neurol. 2004, 251 (Suppl. S6), vi24–vi27. [Google Scholar] [CrossRef]
- Davidsdottir, S.; Cronin-Golomb, A.; Lee, A. Visual and spatial symptoms in Parkinson’s disease. Vision Res. 2005, 45, 1285–1296. [Google Scholar] [CrossRef]
- Janvin, C.C.; Larsen, J.P.; Salmon, D.P.; Galasko, D.; Hugdahl, K.; Aarsland, D. Cognitive profiles of individual patients with Parkinson’s disease and dementia: Comparison with dementia with lewy bodies and Alzheimer’s disease. Mov. Disord. 2006, 21, 337–342. [Google Scholar] [CrossRef]
- Garcia-Diaz, A.I.; Segura, B.; Baggio, H.C.; Marti, M.J.; Valldeoriola, F.; Compta, Y.; Bargallo, N.; Uribe, C.; Campabadal, A.; Abos, A.; et al. Structural Brain Correlations of Visuospatial and Visuoperceptual Tests in Parkinson’s Disease. J. Int. Neuropsychol. Soc. 2018, 24, 33–44. [Google Scholar] [CrossRef] [PubMed]
- Kawabata, K.; Ohdake, R.; Watanabe, H.; Bagarinao, E.; Hara, K.; Ogura, A.; Masuda, M.; Kato, T.; Yokoi, T.; Katsuno, M.; et al. Visuoperceptual disturbances in Parkinson’s disease. Clin. Park. Relat. Disord. 2020, 3, 100036. [Google Scholar] [CrossRef]
- Pieri, V.; Diederich, N.J.; Raman, R.; Goetz, C.G. Decreased color discrimination and contrast sensitivity in Parkinson’s disease. J. Neurol. Sci. 2000, 172, 7–11. [Google Scholar] [CrossRef]
- Almer, Z.; Klein, K.S.; Marsh, L.; Gerstenhaber, M.; Repka, M.X. Ocular motor and sensory function in Parkinson’s disease. Ophthalmology 2012, 119, 178–182. [Google Scholar] [CrossRef]
- Antoniades, C.A.; Kennard, C. Ocular motor abnormalities in neurodegenerative disorders. Eye 2015, 29, 200–207. [Google Scholar] [CrossRef]
- Nowacka, B.; Lubinski, W.; Honczarenko, K.; Potemkowski, A.; Safranow, K. Ophthalmological features of Parkinson disease. Med. Sci. Monit. Int. Med. J. Exp. Clin. Res. 2014, 20, 2243–2249. [Google Scholar] [CrossRef]
- Nucci, C.; Martucci, A.; Cesareo, M.; Garaci, F.; Morrone, L.A.; Russo, R.; Corasaniti, M.T.; Bagetta, G.; Mancino, R. Links among glaucoma, neurodegenerative, and vascular diseases of the central nervous system. Prog. Brain Res. 2015, 221, 49–65. [Google Scholar] [CrossRef]
- Gibson, G.; Mottram, P.G.; Burn, D.J.; Hindle, J.V.; Landau, S.; Samuel, M.; Hurt, C.S.; Brown, R.G.; M Wilson, K.C. Frequency, prevalence, incidence and risk factors associated with visual hallucinations in a sample of patients with Parkinson’s disease: A longitudinal 4-year study. Int. J. Geriatr. Psychiatry 2013, 28, 626–631. [Google Scholar] [CrossRef] [PubMed]
- Lee, A.C.; Harris, J.P.; Calvert, J.E. Impairments of mental rotation in Parkinson’s disease. Neuropsychologia 1998, 36, 109–114. [Google Scholar] [CrossRef] [PubMed]
- Harris, J.P.; Atkinson, E.A.; Lee, A.C.; Nithi, K.; Fowler, M.S. Hemispace differences in the visual perception of size in left hemiParkinson’s disease. Neuropsychologia 2003, 41, 795–807. [Google Scholar] [CrossRef] [PubMed]
- Owen, A.M.; Beksinska, M.; James, M.; Leigh, P.N.; Summers, B.A.; Marsden, C.D.; Quinn, N.P.; Sahakian, B.J.; Robbins, T.W. Visuospatial memory deficits at different stages of Parkinson’s disease. Neuropsychologia 1993, 31, 627–644. [Google Scholar] [CrossRef] [PubMed]
- Possin, K.L.; Filoteo, J.V.; Song, D.D.; Salmon, D.P. Spatial and Object Working Memory Deficits in Parkinson’s Disease are Due to Impairment in Different Underlying Processes. Neuropsychology 2008, 22, 585–595. [Google Scholar] [CrossRef]
- Possin, K.L. Visual Spatial Cognition in Neurodegenerative Disease. Neurocase 2010, 16, 466–487. [Google Scholar] [CrossRef]
- Weil, R.S.; Schrag, A.E.; Warren, J.D.; Crutch, S.J.; Lees, A.J.; Morris, H.R. Visual dysfunction in Parkinson’s disease. Brain 2016, 139, 2827–2843. [Google Scholar] [CrossRef]
- Hertanti, A.; Retnawati, H.; Wutsqa, D.U. The role of spatial experience in mental rotation. J. Phys. Conf. Ser. 2019, 1320, 012043. [Google Scholar] [CrossRef]
- Tinella, L.; Lopez, A.; Caffò, A.O.; Nardulli, F.; Grattagliano, I.; Bosco, A. Cognitive Efficiency and Fitness-to-Drive along the Lifespan: The Mediation Effect of Visuospatial Transformations. Brain Sci. 2021, 11, 1028. [Google Scholar] [CrossRef]
- Ghazi-Saidi, L. Visuospatial and Executive Deficits in Parkinson’s Disease: A Review. Acta Sci. Neurol. 2020, 3, 08–26. [Google Scholar] [CrossRef]
- Ekker, M.S.; Janssen, S.; Seppi, K.; Poewe, W.; de Vries, N.M.; Theelen, T.; Nonnekes, J.; Bloem, B.R. Ocular and visual disorders in Parkinson’s disease: Common but frequently overlooked. Park. Relat. Disord. 2017, 40, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Urwyler, P.; Nef, T.; Killen, A.; Collerton, D.; Thomas, A.; Burn, D.; McKeith, I.; Mosimann, U.P. Visual complaints and visual hallucinations in Parkinson’s disease. Park. Relat. Disord. 2014, 20, 318–322. [Google Scholar] [CrossRef]
- Biousse, V.; Skibell, B.C.; Watts, R.L.; Loupe, D.N.; Drews-Botsch, C.; Newman, N.J. Ophthalmologic features of Parkinson’s disease. Neurology 2004, 62, 177–180. [Google Scholar] [CrossRef]
- Armstrong, R.A. Oculo-Visual Dysfunction in Parkinson’s Disease. J. Park. Dis. 2015, 5, 715–726. [Google Scholar] [CrossRef] [PubMed]
- Buhmann, C.; Kraft, S.; Hinkelmann, K.; Krause, S.; Gerloff, C.; Zangemeister, W.H. Visual Attention and Saccadic Oculomotor Control in Parkinson’s Disease. Eur. Neurol. 2015, 73, 283–293. [Google Scholar] [CrossRef]
- Tomsak, R.L.; Daroff, R.B. Ophthalmologic features of Parkinson’s disease. Neurology 2004, 63, 940–941. [Google Scholar] [CrossRef]
- Mahlknecht, P.; Seppi, K.; Poewe, W. The Concept of Prodromal Parkinson’s Disease. J. Park. Dis. 2015, 5, 681–697. [Google Scholar] [CrossRef]
- Chrysou, A.; Jansonius, N.M.; van Laar, T. Retinal layers in Parkinson’s disease: A meta-analysis of spectral-domain optical coherence tomography studies. Park. Relat. Disord. 2019, 64, 40–49. [Google Scholar] [CrossRef] [PubMed]
- Hajee, M.E.; March, W.F.; Lazzaro, D.R.; Wolintz, A.H.; Shrier, E.M.; Glazman, S.; Bodis-Wollner, I.G. Inner retinal layer thinning in Parkinson disease. Arch. Ophthalmol. 2009, 127, 737–741. [Google Scholar] [CrossRef]
- Huang, J.; Li, Y.; Xiao, J.; Zhang, Q.; Xu, G.; Wu, G.; Liu, T.; Luo, W. Combination of Multifocal Electroretinogram and Spectral-Domain OCT Can Increase Diagnostic Efficacy of Parkinson’s Disease. Park. Dis. 2018, 2018, 4163239. [Google Scholar] [CrossRef] [PubMed]
- Unlu, M.; Gulmez Sevim, D.; Gultekin, M.; Karaca, C. Correlations among multifocal electroretinography and optical coherence tomography findings in patients with Parkinson’s disease. Neurol. Sci. 2018, 39, 533–541. [Google Scholar] [CrossRef] [PubMed]
- Kaur, M.; Saxena, R.; Singh, D.; Behari, M.; Sharma, P.; Menon, V. Correlation Between Structural and Functional Retinal Changes in Parkinson Disease. J. Neuro-Ophthalmol. 2015, 35, 254–258. [Google Scholar] [CrossRef]
- Garcia-Martin, E.; Rodriguez-Mena, D.; Satue, M.; Almarcegui, C.; Dolz, I.; Alarcia, R.; Seral, M.; Polo, V.; Larrosa, J.M.; Pablo, L.E. Electrophysiology and optical coherence tomography to evaluate Parkinson disease severity. Investig. Ophthalmol. Vis. Sci. 2014, 55, 696–705. [Google Scholar] [CrossRef]
- Moschos, M.M.; Tagaris, G.; Markopoulos, I.; Margetis, I.; Tsapakis, S.; Kanakis, M.; Koutsandrea, C. Morphologic changes and functional retinal impairment in patients with Parkinson disease without visual loss. Eur. J. Ophthalmol. 2011, 21, 24–29. [Google Scholar] [CrossRef]
- Archibald, N.K.; Clarke, M.P.; Mosimann, U.P.; Burn, D.J. Retinal thickness in Parkinson’s disease. Park. Relat. Disord. 2011, 17, 431–436. [Google Scholar] [CrossRef]
- Tsironi, E.E.; Dastiridou, A.; Katsanos, A.; Dardiotis, E.; Veliki, S.; Patramani, G.; Zacharaki, F.; Ralli, S.; Hadjigeorgiou, G.M. Perimetric and retinal nerve fiber layer findings in patients with Parkinson’s disease. BMC Ophthalmol. 2012, 12, 54. [Google Scholar] [CrossRef]
- Sari, E.S.; Koc, R.; Yazici, A.; Sahin, G.; Ermis, S.S. Ganglion cell-inner plexiform layer thickness in patients with Parkinson disease and association with disease severity and duration. J. Neuro-Ophthalmol. 2015, 35, 117–121. [Google Scholar] [CrossRef]
- Liu, L.; Jia, Y.; Takusagawa, H.L.; Pechauer, A.D.; Edmunds, B.; Lombardi, L.; Davis, E.; Morrison, J.C.; Huang, D. Optical Coherence Tomography Angiography of the Peripapillary Retina in Glaucoma. JAMA Ophthalmol. 2015, 133, 1045–1052. [Google Scholar] [CrossRef] [PubMed]
- Sung, M.S.; Choi, S.-M.; Kim, J.; Ha, J.Y.; Kim, B.-C.; Heo, H.; Park, S.W. Inner retinal thinning as a biomarker for cognitive impairment in de novo Parkinson’s disease. Sci. Rep. 2019, 9, 11832. [Google Scholar] [CrossRef] [PubMed]
- Hartmann, P.; Schmid, M.G. Retina Layers. Available online: https://de.wikipedia.org/wiki/Datei:Retina.jpg (accessed on 19 July 2023).
- Alves, J.N.; Westner, B.U.; Højlund, A.; Weil, R.S.; Dalal, S.S. Structural and functional changes in the retina in Parkinson’s disease. J. Neurol. Neurosurg. Psychiatry 2023, 94, 448–456. [Google Scholar] [CrossRef]
- Bodis-Wollner, I. Neuropsychological and perceptual defects in Parkinson’s disease. Park. Relat. Disord. 2003, 9 (Suppl. S2), S83–S89. [Google Scholar] [CrossRef]
- Ahn, J.; Lee, J.-Y.; Kim, T.W.; Yoon, E.J.; Oh, S.; Kim, Y.K.; Kim, J.-M.; Woo, S.J.; Kim, K.W.; Jeon, B. Retinal thinning associates with nigral dopaminergic loss in de novo Parkinson disease. Neurology 2018, 91, e1003–e1012. [Google Scholar] [CrossRef] [PubMed]
- Bodis-Wollner, I.; Kozlowski, P.B.; Glazman, S.; Miri, S. α-synuclein in the inner retina in parkinson disease. Ann. Neurol. 2014, 75, 964–966. [Google Scholar] [CrossRef]
- Beach, T.G.; Carew, J.; Serrano, G.; Adler, C.H.; Shill, H.A.; Sue, L.I.; Sabbagh, M.N.; Akiyama, H.; Cuenca, N.; Arizona Parkinson’s Disease Consortium. Phosphorylated α-synuclein-immunoreactive retinal neuronal elements in Parkinson’s disease subjects. Neurosci. Lett. 2014, 571, 34–38. [Google Scholar] [CrossRef]
- Ortuño-Lizarán, I.; Beach, T.G.; Serrano, G.E.; Walker, D.G.; Adler, C.H.; Cuenca, N. Phosphorylated α-synuclein in the retina is a biomarker of Parkinson’s disease pathology severity. Mov. Disord. 2018, 33, 1315–1324. [Google Scholar] [CrossRef]
- Lee, J.-Y.; Kim, J.M.; Ahn, J.; Kim, H.-J.; Jeon, B.S.; Kim, T.W. Retinal nerve fiber layer thickness and visual hallucinations in Parkinson’s Disease. Mov. Disord. 2014, 29, 61–67. [Google Scholar] [CrossRef]
- Miri, S.; Shrier, E.M.; Glazman, S.; Ding, Y.; Selesnick, I.; Kozlowski, P.B.; Bodis-Wollner, I. The avascular zone and neuronal remodeling of the fovea in Parkinson disease. Ann. Clin. Transl. Neurol. 2015, 2, 196–201. [Google Scholar] [CrossRef]
- Litvinenko, I.V.; Boyko, E.V.; Kulikov, A.N.; Dynin, P.S.; Trufanov, A.G.; Mal’tsev, D.S.; Yurin, A.A. The Relationship between Visuospatial Impairments and Retinal and Cortical Thickness in Parkinson’s Disease. Hum. Physiol. 2017, 43, 863–869. [Google Scholar] [CrossRef]
- Hannaway, N.; Zarkali, A.; Leyland, L.-A.; Bremner, F.; Nicholas, J.M.; Wagner, S.K.; Roig, M.; Keane, P.A.; Toosy, A.; Chataway, J.; et al. Visual dysfunction is a better predictor than retinal thickness for dementia in Parkinson’s disease. J. Neurol. Neurosurg. Psychiatry 2023, 0, 1–9. [Google Scholar] [CrossRef]
- Bayer, A.U.; Keller, O.N.; Ferrari, F.; Maag, K.-P. Association of glaucoma with neurodegenerative diseases with apoptotic cell death: Alzheimer’s disease and Parkinson’s disease. Am. J. Ophthalmol. 2002, 133, 135–137. [Google Scholar] [CrossRef] [PubMed]
- Yenice, O.; Onal, S.; Midi, I.; Ozcan, E.; Temel, A.; I-Gunal, D. Visual field analysis in patients with Parkinson’s disease. Park. Relat. Disord. 2008, 14, 193–198. [Google Scholar] [CrossRef]
- Ture, S.; Inci, I.; Gedizlioglu, M. Abnormalities of contrast sensitivity, visual fields and visual evoked potentials in Parkinson’s disease and effect of dopaminergic treatment. J. Neurol. 2007, 254 (Suppl. S3). [Google Scholar] [CrossRef]
- Zhao, L.; Li, J.; Feng, L.; Zhang, C.; Zhang, W.; Wang, C.; He, Y.; Wen, D.; Song, W. Depicting Developing Trend and Core Knowledge of Primary Open-Angle Glaucoma: A Bibliometric and Visualized Analysis. Front. Med. 2022, 9, 922527. [Google Scholar] [CrossRef] [PubMed]
- Micieli, G.; Tassorelli, C.; Martignoni, E.; Pacchetti, C.; Bruggi, P.; Magri, M.; Nappi, G. Disordered pupil reactivity in Parkinson’s disease. Clin. Auton. Res. 1991, 1, 55–58. [Google Scholar] [CrossRef] [PubMed]
- Alhassan, M.; Hovis, J.K.; Almeida, Q.J. Pupil light reflex in Parkinson’s disease patients with and without freezing of gait symptoms. Saudi J. Ophthalmol. 2021, 35, 332. [Google Scholar] [CrossRef]
- Hori, N.; Takamori, M.; Hirayama, M.; Watanabe, H.; Nakamura, T.; Yamashita, F.; Ito, H.; Mabuchi, N.; Sobue, G. Pupillary supersensitivity and visual disturbance in Parkinson’s disease. Clin. Auton. Res. 2008, 18, 20–27. [Google Scholar] [CrossRef]
- Postuma, R.B.; Gagnon, J.-F.; Pelletier, A.; Montplaisir, J. Prodromal autonomic symptoms and signs in Parkinson’s disease and dementia with Lewy bodies. Mov. Disord. 2013, 28, 597–604. [Google Scholar] [CrossRef]
- You, S.; Hong, J.-H.; Yoo, J. Analysis of pupillometer results according to disease stage in patients with Parkinson’s disease. Sci. Rep. 2021, 11, 17880. [Google Scholar] [CrossRef]
- Fotiou, D.F.; Stergiou, V.; Tsiptsios, D.; Lithari, C.; Nakou, M.; Karlovasitou, A. Cholinergic deficiency in Alzheimer’s and Parkinson’s disease: Evaluation with pupillometry. Int. J. Psychophysiol. 2009, 73, 143–149. [Google Scholar] [CrossRef] [PubMed]
- Kahya, M.; Lyons, K.E.; Pahwa, R.; Akinwuntan, A.E.; He, J.; Devos, H. Pupillary Response to Postural Demand in Parkinson’s Disease. Front. Bioeng. Biotechnol. 2021, 9, 617028. [Google Scholar] [CrossRef]
- Agostino, R.; Bologna, M.; Dinapoli, L.; Gregori, B.; Fabbrini, G.; Accornero, N.; Berardelli, A. Voluntary, spontaneous, and reflex blinking in Parkinson’s disease. Mov. Disord. 2008, 23, 669–675. [Google Scholar] [CrossRef] [PubMed]
- Lamberti, P.; De Mari, M.; Zenzola, A.; Aniello, M.S.; Defazio, G. Frequency of apraxia of eyelid opening in the general population and in patients with extrapyramidal disorders. Neurol. Sci. 2002, 23 (Suppl. S2), S81–S82. [Google Scholar] [CrossRef]
- Nagino, K.; Sung, J.; Oyama, G.; Hayano, M.; Hattori, N.; Okumura, Y.; Fujio, K.; Akasaki, Y.; Huang, T.; Midorikawa-Inomata, A.; et al. Prevalence and characteristics of dry eye disease in Parkinson’s disease: A systematic review and meta-analysis. Sci. Rep. 2022, 12, 18348. [Google Scholar] [CrossRef] [PubMed]
- Shaikh, A.G. Translational neurophysiology of Parkinson’s disease: Can’t blink on an eye blink. J. Neurophysiol. 2015, 114, 761–762. [Google Scholar] [CrossRef]
- Valls-Sole, J.; Defazio, G. Blepharospasm: Update on Epidemiology, Clinical Aspects, and Pathophysiology. Front. Neurol. 2016, 7, 45. [Google Scholar] [CrossRef]
- Armstrong, R.A. Visual signs and symptoms of Parkinson’s disease. Clin. Exp. Optom. 2008, 91, 129–138. [Google Scholar] [CrossRef]
- Sescousse, G.; Ligneul, R.; van Holst, R.J.; Janssen, L.K.; de Boer, F.; Janssen, M.; Berry, A.S.; Jagust, W.J.; Cools, R. Spontaneous eye blink rate and dopamine synthesis capacity: Preliminary evidence for an absence of positive correlation. Eur. J. Neurosci. 2018, 47, 1081–1086. [Google Scholar] [CrossRef]
- Reddy, V.C.; Patel, S.V.; Hodge, D.O.; Leavitt, J.A. Corneal sensitivity, blink rate, and corneal nerve density in progressive supranuclear palsy and Parkinson disease. Cornea 2013, 32, 631–635. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, R.A. Visual Symptoms in Parkinson’s Disease. Park. Dis. 2011, 2011, 908306. [Google Scholar] [CrossRef] [PubMed]
- Silva, M.F.; Faria, P.; Regateiro, F.S.; Forjaz, V.; Januário, C.; Freire, A.; Castelo-Branco, M. Independent patterns of damage within magno-, parvo- and koniocellular pathways in Parkinson’s disease. Brain 2005, 128, 2260–2271. [Google Scholar] [CrossRef]
- Piro, A.; Tagarelli, A.; Nicoletti, G.; Fletcher, R.; Quattrone, A. Color vision impairment in Parkinson’s disease. J. Park. Dis. 2014, 4, 317–319. [Google Scholar] [CrossRef] [PubMed]
- Hamedani, A.G.; Willis, A.W. Self-reported visual dysfunction in Parkinson disease: The Survey of Health, Ageing and Retirement in Europe. Eur. J. Neurol. 2020, 27, 484–489. [Google Scholar] [CrossRef]
- Polo, V.; Satue, M.; Rodrigo, M.J.; Otin, S.; Alarcia, R.; Bambo, M.P.; Fuertes, M.I.; Larrosa, J.M.; Pablo, L.E.; Garcia-Martin, E. Visual dysfunction and its correlation with retinal changes in patients with Parkinson’s disease: An observational cross-sectional study. BMJ Open 2016, 6, e009658. [Google Scholar] [CrossRef]
- Büttner, T.; Müller, T.; Kuhn, W. Effects of apomorphine on visual functions in Parkinson’s disease. J. Neural Transm. 2000, 107, 87–94. [Google Scholar] [CrossRef]
- Diederich, N.J.; Raman, R.; Leurgans, S.; Goetz, C.G. Progressive worsening of spatial and chromatic processing deficits in Parkinson disease. Arch. Neurol. 2002, 59, 1249–1252. [Google Scholar] [CrossRef]
- Leyland, L.-A.; Bremner, F.D.; Mahmood, R.; Hewitt, S.; Durteste, M.; Cartlidge, M.R.E.; Lai, M.M.-M.; Miller, L.E.; Saygin, A.P.; Keane, P.A.; et al. Visual tests predict dementia risk in Parkinson disease. Neurol. Clin. Pract. 2020, 10, 29–39. [Google Scholar] [CrossRef]
- Weil, R.S.; Reeves, S. Hallucinations in Parkinson’s disease: New insights into mechanisms and treatments. Adv. Clin. Neurosci. Rehabil. 2020, 19, ONNS5189. [Google Scholar] [CrossRef]
- Shine, J.M.; O’Callaghan, C.; Halliday, G.M.; Lewis, S.J.G. Tricks of the mind: Visual hallucinations as disorders of attention. Prog. Neurobiol. 2014, 116, 58–65. [Google Scholar] [CrossRef] [PubMed]
- Yao, N.; Shek-Kwan Chang, R.; Cheung, C.; Pang, S.; Lau, K.K.; Suckling, J.; Rowe, J.B.; Yu, K.; Ka-Fung Mak, H.; Chua, S.; et al. The default mode network is disrupted in parkinson’s disease with visual hallucinations. Hum. Brain Mapp. 2014, 35, 5658–5666. [Google Scholar] [CrossRef] [PubMed]
- Onofrj, M.; Carrozzino, D.; D’Amico, A.; Di Giacomo, R.; Delli Pizzi, S.; Thomas, A.; Onofrj, V.; Taylor, J.-P.; Bonanni, L. Psychosis in parkinsonism: An unorthodox approach. Neuropsychiatr. Dis. Treat. 2017, 13, 1313–1330. [Google Scholar] [CrossRef] [PubMed]
- Sweet, R.D.; McDowell, F.H.; Feigenson, J.S.; Loranger, A.W.; Goodell, H. Mental symptoms in Parkinson’s disease during chronic treatment with levodopa. Neurology 1976, 26, 305–310. [Google Scholar] [CrossRef]
- Poewe, W. Psychosis in Parkinson’s disease. Mov. Disord. 2003, 18 (Suppl. S6), S80–S87. [Google Scholar] [CrossRef] [PubMed]
- Zahodne, L.B.; Fernandez, H.H. Pathophysiology and treatment of psychosis in Parkinson’s disease: A review. Drugs Aging 2008, 25, 665–682. [Google Scholar] [CrossRef]
- Russo, M.; Carrarini, C.; Dono, F.; Rispoli, M.G.; Di Pietro, M.; Di Stefano, V.; Ferri, L.; Bonanni, L.; Sensi, S.L.; Onofrj, M. The Pharmacology of Visual Hallucinations in Synucleinopathies. Front. Pharmacol. 2019, 10, 1379. [Google Scholar] [CrossRef]
- Anang, J.B.M.; Gagnon, J.-F.; Bertrand, J.-A.; Romenets, S.R.; Latreille, V.; Panisset, M.; Montplaisir, J.; Postuma, R.B. Predictors of dementia in Parkinson disease. Neurology 2014, 83, 1253–1260. [Google Scholar] [CrossRef]
- Uc, E.Y.; McDermott, M.P.; Marder, K.S.; Anderson, S.W.; Litvan, I.; Como, P.G.; Auinger, P.; Chou, K.L.; Growdon, J.C.; Parkinson Study Group DATATOP Investigators. Incidence of and risk factors for cognitive impairment in an early Parkinson disease clinical trial cohort. Neurology 2009, 73, 1469–1477. [Google Scholar] [CrossRef]
- Aarsland, D.; Larsen, J.P.; Tandberg, E.; Laake, K. Predictors of nursing home placement in Parkinson’s disease: A population-based, prospective study. J. Am. Geriatr. Soc. 2000, 48, 938–942. [Google Scholar] [CrossRef]
- Kalbe, E.; Rehberg, S.P.; Heber, I.; Kronenbuerger, M.; Schulz, J.B.; Storch, A.; Linse, K.; Schneider, C.; Gräber, S.; Liepelt-Scarfone, I.; et al. Subtypes of mild cognitive impairment in patients with Parkinson’s disease: Evidence from the LANDSCAPE study. J. Neurol. Neurosurg. Psychiatry 2016, 87, 1099–1105. [Google Scholar] [CrossRef]
- Lawrence, B.J.; Gasson, N.; Loftus, A.M. Prevalence and Subtypes of Mild Cognitive Impairment in Parkinson’s Disease. Sci. Rep. 2016, 6, 33929. [Google Scholar] [CrossRef] [PubMed]
- Johnson, D.K.; Langford, Z.; Garnier-Villarreal, M.; Morris, J.C.; Galvin, J.E. Onset of Mild Cognitive Impairment in Parkinson Disease. Alzheimer Dis. Assoc. Disord. 2016, 30, 127–133. [Google Scholar] [CrossRef] [PubMed]
- Caspell-Garcia, C.; Simuni, T.; Tosun-Turgut, D.; Wu, I.-W.; Zhang, Y.; Nalls, M.; Singleton, A.; Shaw, L.A.; Kang, J.-H.; Trojanowski, J.Q.; et al. Multiple modality biomarker prediction of cognitive impairment in prospectively followed de novo Parkinson disease. PLoS ONE 2017, 12, e0175674. [Google Scholar] [CrossRef]
- Pino, R.D.; Acera, M.; Murueta-Goyena, A.; Lucas-Jiménez, O.; Ojeda, N.; Ibarretxe-Bilbao, N.; Peña, J.; Reyero, P.; Cortés, J.; Tijero, B.; et al. Visual dysfunction is associated with cognitive impairment in Parkinson’s disease. Park. Relat. Disord. 2021, 92, 22–25. [Google Scholar] [CrossRef]
- Dubois, B.; Pillon, B. Cognitive deficits in Parkinson’s disease. J. Neurol. 1997, 244, 2–8. [Google Scholar] [CrossRef]
- Waterfall, M.L.; Crowe, S.F. Meta-analytic comparison of the components of visual cognition in Parkinson’s disease. J. Clin. Exp. Neuropsychol. 1995, 17, 759–772. [Google Scholar] [CrossRef] [PubMed]
- Norton, D.J.; Nguyen, V.A.; Lewis, M.F.; Reynolds, G.O.; Somers, D.C.; Cronin-Golomb, A. Visuospatial Attention to Single and Multiple Objects Is Independently Impaired in Parkinson’s Disease. PLoS ONE 2016, 11, e0150013. [Google Scholar] [CrossRef]
- Gullett, J.M.; Price, C.C.; Nguyen, P.; Okun, M.S.; Bauer, R.M.; Bowers, D. Reliability of three Benton Judgment of Line Orientation short forms in idiopathic Parkinson’s disease. Clin. Neuropsychol. 2013, 27, 1167–1178. [Google Scholar] [CrossRef]
- Segura, B.; Baggio, H.C.; Marti, M.J.; Valldeoriola, F.; Compta, Y.; Garcia-Diaz, A.I.; Vendrell, P.; Bargallo, N.; Tolosa, E.; Junque, C. Cortical thinning associated with mild cognitive impairment in Parkinson’s disease. Mov. Disord. 2014, 29, 1495–1503. [Google Scholar] [CrossRef]
- Renfroe, J.B.; Turner, T.H.; Hinson, V.K. Assessing Visuospatial Skills in Parkinson’s: Comparison of Neuropsychological Assessment Battery Visual Discrimination to the Judgment of Line Orientation. Arch. Clin. Neuropsychol. 2017, 32, 123–127. [Google Scholar] [CrossRef] [PubMed]
- Levin, B.E.; Llabre, M.M.; Reisman, S.; Weiner, W.J.; Sanchez-Ramos, J.; Singer, C.; Brown, M.C. Visuospatial impairment in Parkinson’s disease. Neurology 1991, 41, 365–369. [Google Scholar] [CrossRef] [PubMed]
- Finton, M.J.; Lucas, J.A.; Graff-Radford, N.R.; Uitti, R.J. Analysis of visuospatial errors in patients with Alzheimer’s disease or Parkinson’s disease. J. Clin. Exp. Neuropsychol. 1998, 20, 186–193. [Google Scholar] [CrossRef] [PubMed]
- Alegret, M.; Vendrell, P.; Junque, C.; Valldeoriola, F.; Tolosa, E. Visuospatial Deficits in Parkinsons Disease Assessed by Judgment of Line Orientation Test: Error Analyses and Practice Effects. J. Clin. Exp. Neuropsychol. 2001, 23, 592–598. [Google Scholar] [CrossRef]
- Kemps, E.; Szmalec, A.; Vandierendonck, A.; Crevits, L. Visuo-spatial processing in Parkinson’s disease: Evidence for diminished visuo-spatial sketch pad and central executive resources. Park. Relat. Disord. 2005, 11, 181–186. [Google Scholar] [CrossRef]
- Kawashima, S.; Shimizu, Y.; Ueki, Y.; Matsukawa, N. Impairment of the visuospatial working memory in the patients with Parkinson’s Disease: An fMRI study. BMC Neurol. 2021, 21, 335. [Google Scholar] [CrossRef]
- Crucian, G.P.; Barrett, A.M.; Burks, D.W.; Riestra, A.R.; Roth, H.L.; Schwartz, R.L.; Triggs, W.J.; Bowers, D.; Friedman, W.; Greer, M.; et al. Mental object rotation in Parkinson’s disease. J. Int. Neuropsychol. Soc. 2003, 9, 1078–1087. [Google Scholar] [CrossRef]
- Duncombe, M.E.; Bradshaw, J.L.; Iansek, R.; Phillips, J.G. Parkinsonian patients without dementia or depression do not suffer from bradyphrenia as indexed by performance in mental rotation tasks with and without advance information. Neuropsychologia 1994, 32, 1383–1396. [Google Scholar] [CrossRef]
- Amick, M.M.; Schendan, H.E.; Ganis, G.; Cronin-Golomb, A. Frontostriatal circuits are necessary for visuomotor transformation: Mental rotation in Parkinson’s disease. Neuropsychologia 2006, 44, 339–349. [Google Scholar] [CrossRef]
- Bek, J.; Humphries, S.; Poliakoff, E.; Brady, N. Mental rotation of hands and objects in ageing and Parkinson’s disease: Differentiating motor imagery and visuospatial ability. Exp. Brain Res. 2022, 240, 1991–2004. [Google Scholar] [CrossRef]
- Pereira, J.B.; Junqué, C.; Martí, M.-J.; Ramirez-Ruiz, B.; Bargalló, N.; Tolosa, E. Neuroanatomical substrate of visuospatial and visuoperceptual impairment in Parkinson’s disease. Mov. Disord. 2009, 24, 1193–1199. [Google Scholar] [CrossRef]
- Archibald, N.K.; Hutton, S.B.; Clarke, M.P.; Mosimann, U.P.; Burn, D.J. Visual exploration in Parkinson’s disease and Parkinson’s disease dementia. Brain 2013, 136, 739–750. [Google Scholar] [CrossRef] [PubMed]
- Raskin, S.A.; Borod, J.C.; Wasserstein, J.; Bodis-Wollner, I.; Coscia, L.; Yahr, M.D. Visuospatial orientation in Parkinson’s disease. Int. J. Neurosci. 1990, 51, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Shine, J.M.; Muller, A.J.; O’Callaghan, C.; Hornberger, M.; Halliday, G.M.; Lewis, S.J. Abnormal connectivity between the default mode and the visual system underlies the manifestation of visual hallucinations in Parkinson’s disease: A task-based fMRI study. NPJ Park. Dis. 2015, 1, 15003. [Google Scholar] [CrossRef] [PubMed]
- Laatu, S.; Revonsuo, A.; Pihko, L.; Portin, R.; Rinne, J.O. Visual object recognition deficits in early Parkinson’s disease. Park. Relat. Disord. 2004, 10, 227–233. [Google Scholar] [CrossRef]
- Koh, S.-B.; Suh, S.-I.; Kim, S.-H.; Kim, J.H. Stereopsis and extrastriate cortical atrophy in Parkinson’s disease: A voxel-based morphometric study. Neuroreport 2013, 24, 229–232. [Google Scholar] [CrossRef]
- Sun, L.; Zhang, H.; Gu, Z.; Cao, M.; Li, D.; Chan, P. Stereopsis impairment is associated with decreased color perception and worse motor performance in Parkinson’s disease. Eur. J. Med. Res. 2014, 19, 29. [Google Scholar] [CrossRef]
- Kim, S.-H.; Park, J.-H.; Kim, Y.H.; Koh, S.-B. Stereopsis in drug naïve Parkinson’s disease patients. Can. J. Neurol. Sci. 2011, 38, 299–302. [Google Scholar] [CrossRef]
- Ba, F.; Sang, T.T.; He, W.; Fatehi, J.; Mostofi, E.; Zheng, B. Stereopsis and Eye Movement Abnormalities in Parkinson’s Disease and Their Clinical Implications. Front. Aging Neurosci. 2022, 14, 783773. [Google Scholar] [CrossRef]
- Jaywant, A.; Shiffrar, M.; Roy, S.; Cronin-Golomb, A. Impaired perception of biological motion in Parkinson’s disease. Neuropsychology 2016, 30, 720–730. [Google Scholar] [CrossRef]
- Kloeters, S.; Hartmann, C.J.; Pundmann, V.D.; Schnitzler, A.; Südmeyer, M.; Lange, J. Impaired perception of human movements in Parkinson’s disease. Behav. Brain Res. 2017, 317, 88–94. [Google Scholar] [CrossRef] [PubMed]
- Uc, E.Y.; Rizzo, M.; Anderson, S.W.; Qian, S.; Rodnitzky, R.L.; Dawson, J.D. Visual dysfunction in Parkinson disease without dementia. Neurology 2005, 65, 1907–1913. [Google Scholar] [CrossRef] [PubMed]
- Scarpina, F.; Ambiel, E.; Albani, G.; Pradotto, L.G.; Mauro, A. Utility of Boston Qualitative Scoring System for Rey-Osterrieth Complex Figure: Evidence from a Parkinson’s Diseases sample. Neurol. Sci. 2016, 37, 1603–1611. [Google Scholar] [CrossRef]
- De Lucia, N.; Trojano, L.; Vitale, C.; Grossi, D.; Barone, P.; Santangelo, G. The closing-in phenomenon in Parkinson’s disease. Park. Relat. Disord. 2015, 21, 793–796. [Google Scholar] [CrossRef] [PubMed]
- Ambron, E.; Della Sala, S. A critical review of closing-in. Neuropsychology 2017, 31, 105–117. [Google Scholar] [CrossRef] [PubMed]
- Ambron, E.; Piretti, L.; Lunardelli, A.; Coslett, H.B. Closing-in Behavior and Parietal Lobe Deficits: Three Single Cases Exhibiting Different Manifestations of the Same Behavior. Front. Psychol. 2018, 9, 1617. [Google Scholar] [CrossRef]
- De Lucia, N.; Grossi, D.; Mauro, A.; Trojano, L. Closing-in in Parkinson’s disease individuals with dementia: An experimental study. J. Clin. Exp. Neuropsychol. 2015, 37, 946–955. [Google Scholar] [CrossRef]
- Miller, I.N.; Cronin-Golomb, A. Gender differences in Parkinson’s disease: Clinical characteristics and cognition. Mov. Disord. 2010, 25, 2695–2703. [Google Scholar] [CrossRef]
- Verreyt, N.; Nys, G.M.S.; Santens, P.; Vingerhoets, G. Cognitive Differences Between Patients with Left-sided and Right-sided Parkinson’s Disease. A Review. Neuropsychol. Rev. 2011, 21, 405–424. [Google Scholar] [CrossRef]
- Lally, H.; Hart, A.R.; Bay, A.A.; Kim, C.; Wolf, S.L.; Hackney, M.E. Association Between Motor Subtype and Visuospatial and Executive Function in Mild-Moderate Parkinson Disease. Arch. Phys. Med. Rehabil. 2020, 101, 1580–1589. [Google Scholar] [CrossRef]
- Davidsdottir, S.; Wagenaar, R.; Young, D.; Cronin-Golomb, A. Impact of optic flow perception and egocentric coordinates on veering in Parkinson’s disease. Brain 2008, 131, 2882–2893. [Google Scholar] [CrossRef]
- Schendan, H.E.; Amick, M.M.; Cronin-Golomb, A. Role of a lateralized parietal-basal ganglia circuit in hierarchical pattern perception: Evidence from Parkinson’s disease. Behav. Neurosci. 2009, 123, 125–136. [Google Scholar] [CrossRef]
- Seichepine, D.R.; Neargarder, S.; Davidsdottir, S.; Reynolds, G.O.; Cronin-Golomb, A. Side and type of initial motor symptom influences visuospatial functioning in Parkinson’s disease. J. Park. Dis. 2015, 5, 75–83. [Google Scholar] [CrossRef] [PubMed]
- Baumann, C.R.; Held, U.; Valko, P.O.; Wienecke, M.; Waldvogel, D. Body side and predominant motor features at the onset of Parkinson’s disease are linked to motor and nonmotor progression. Mov. Disord. 2014, 29, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Locascio, J.; Corkin, S.; Growdon, J. Relation Between Clinical Characteristics of Parkinson’s Disease and Cognitive Decline. J. Clin. Exp. Neuropsychol. 2003, 25, 94–109. [Google Scholar] [CrossRef]
- Oltra, J.; Uribe, C.; Campabadal, A.; Inguanzo, A.; Monté-Rubio, G.C.; Martí, M.J.; Compta, Y.; Valldeoriola, F.; Junque, C.; Segura, B. Sex Differences in Brain and Cognition in de novo Parkinson’s Disease. Front. Aging Neurosci. 2022, 13, 791532. [Google Scholar] [CrossRef] [PubMed]
- Passoti, C.; Zanzaglia, R.; Sinforiani, E.; Minafra, B.; Bertaina, I.; Pacchetti, C. Cognitive function in Parkinson’s disease: The influence of gender. Basal Ganglia 2013, 3, 131–135. [Google Scholar] [CrossRef]
- Bayram, E.; Banks, S.J.; Shan, G.; Kaplan, N.; Caldwell, J.Z.K. Sex Differences in Cognitive Changes in de Novo Parkinson’s Disease. J. Int. Neuropsychol. Soc. 2020, 26, 241–249. [Google Scholar] [CrossRef]
- Cronin-Golomb, A.; Braun, A.E. Visuospatial dysfunction and problem solving in Parkinson’s disease. Neuropsychology 1997, 11, 44–52. [Google Scholar] [CrossRef]
- Garcia-Diaz, A.I.; Segura, B.; Baggio, H.C.; Uribe, C.; Campabadal, A.; Abos, A.; Marti, M.J.; Valldeoriola, F.; Compta, Y.; Bargallo, N.; et al. Cortical thinning correlates of changes in visuospatial and visuoperceptual performance in Parkinson’s disease: A 4-year follow-up. Park. Relat. Disord. 2018, 46, 62–68. [Google Scholar] [CrossRef]
- Baggio, H.-C.; Segura, B.; Sala-Llonch, R.; Marti, M.-J.; Valldeoriola, F.; Compta, Y.; Tolosa, E.; Junqué, C. Cognitive impairment and resting-state network connectivity in Parkinson’s disease. Hum. Brain Mapp. 2015, 36, 199–212. [Google Scholar] [CrossRef] [PubMed]
- Filoteo, J.V.; Reed, J.D.; Litvan, I.; Harrington, D.L. Volumetric correlates of cognitive functioning in nondemented patients with Parkinson’s disease. Mov. Disord. 2014, 29, 360–367. [Google Scholar] [CrossRef]
- Rektorova, I.; Biundo, R.; Marecek, R.; Weis, L.; Aarsland, D.; Antonini, A. Grey Matter Changes in Cognitively Impaired Parkinson’s Disease Patients. PLoS ONE 2014, 9, e85595. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.E.; Park, H.-J.; Song, S.K.; Sohn, Y.H.; Lee, J.D.; Lee, P.H. Neuroanatomic basis of amnestic MCI differs in patients with and without Parkinson disease. Neurology 2010, 75, 2009–2016. [Google Scholar] [CrossRef]
- Foster, E.R.; Black, K.J.; Antenor-Dorsey, J.A.V.; Perlmutter, J.S.; Hershey, T. Motor asymmetry and substantia nigra volume are related to spatial delayed response performance in Parkinson disease. Brain Cogn. 2008, 67, 1–10. [Google Scholar] [CrossRef]
- Hattori, T.; Orimo, S.; Aoki, S.; Ito, K.; Abe, O.; Amano, A.; Sato, R.; Sakai, K.; Mizusawa, H. Cognitive status correlates with white matter alteration in Parkinson’s disease. Hum. Brain Mapp. 2012, 33, 727–739. [Google Scholar] [CrossRef]
- Lenka, A.; Jhunjhunwala, K.R.; Saini, J.; Pal, P.K. Structural and functional neuroimaging in patients with Parkinson’s disease and visual hallucinations: A critical review. Park. Relat. Disord. 2015, 21, 683–691. [Google Scholar] [CrossRef] [PubMed]
- Eberling, J.L.; Richardson, B.C.; Reed, B.R.; Wolfe, N.; Jagust, W.J. Cortical glucose metabolism in Parkinson’s disease without dementia. Neurobiol. Aging 1994, 15, 329–335. [Google Scholar] [CrossRef]
- Bohnen, N.I.; Minoshima, S.; Giordani, B.; Frey, K.A.; Kuhl, D.E. Motor correlates of occipital glucose hypometabolism in Parkinson’s disease without dementia. Neurology 1999, 52, 541–546. [Google Scholar] [CrossRef]
- Hosokai, Y.; Nishio, Y.; Hirayama, K.; Takeda, A.; Ishioka, T.; Sawada, Y.; Suzuki, K.; Itoyama, Y.; Takahashi, S.; Fukuda, H.; et al. Distinct patterns of regional cerebral glucose metabolism in Parkinson’s disease with and without mild cognitive impairment. Mov. Disord. 2009, 24, 854–862. [Google Scholar] [CrossRef]
- Kawabata, K.; Tachibana, H.; Kasama, S. Cerebral blood flow and cognitive function in Parkinson’s disease. Int. Congr. Ser. 2002, 1232, 583–586. [Google Scholar] [CrossRef]
- Bohnen, N.I.; Koeppe, R.A.; Minoshima, S.; Giordani, B.; Albin, R.L.; Frey, K.A.; Kuhl, D.E. Cerebral Glucose Metabolic Features of Parkinson Disease and Incident Dementia: Longitudinal Study. J. Nucl. Med. 2011, 52, 848–855. [Google Scholar] [CrossRef] [PubMed]
- Caproni, S.; Muti, M.; Renzo, A.D.; Principi, M.; Caputo, N.; Calabresi, P.; Tambasco, N. Subclinical Visuospatial Impairment in Parkinson’s Disease: The Role of Basal Ganglia and Limbic System. Front. Neurol. 2014, 5, 152. [Google Scholar] [CrossRef]
- Göttlich, M.; Münte, T.F.; Heldmann, M.; Kasten, M.; Hagenah, J.; Krämer, U.M. Altered Resting State Brain Networks in Parkinson’s Disease. PLoS ONE 2013, 8, e77336. [Google Scholar] [CrossRef]
- Pereira, J.B.; Aarsland, D.; Ginestet, C.E.; Lebedev, A.V.; Wahlund, L.-O.; Simmons, A.; Volpe, G.; Westman, E. Aberrant cerebral network topology and mild cognitive impairment in early Parkinson’s disease. Hum. Brain Mapp. 2015, 36, 2980–2995. [Google Scholar] [CrossRef] [PubMed]
- Lou, W.; Shi, L.; Wang, D.; Tam, C.W.C.; Chu, W.C.W.; Mok, V.C.T.; Cheng, S.-T.; Lam, L.C.W. Decreased activity with increased background network efficiency in amnestic MCI during a visuospatial working memory task. Hum. Brain Mapp. 2015, 36, 3387–3403. [Google Scholar] [CrossRef]
- Amboni, M.; Tessitore, A.; Esposito, F.; Santangelo, G.; Picillo, M.; Vitale, C.; Giordano, A.; Erro, R.; de Micco, R.; Corbo, D.; et al. Resting-state functional connectivity associated with mild cognitive impairment in Parkinson’s disease. J. Neurol. 2015, 262, 425–434. [Google Scholar] [CrossRef]
- Li, Y.; Liang, P.; Jia, X.; Li, K. Abnormal regional homogeneity in Parkinson’s disease: A resting state fMRI study. Clin. Radiol. 2016, 71, e28–e34. [Google Scholar] [CrossRef]
- Weil, R.S.; Hsu, J.K.; Darby, R.R.; Soussand, L.; Fox, M.D. Neuroimaging in Parkinson’s disease dementia: Connecting the dots. Brain Commun. 2019, 1, fcz006. [Google Scholar] [CrossRef]
- Vignando, M.; Ffytche, D.; Lewis, S.J.G.; Lee, P.H.; Chung, S.J.; Weil, R.S.; Hu, M.T.; Mackay, C.E.; Griffanti, L.; Pins, D.; et al. Mapping brain structural differences and neuroreceptor correlates in Parkinson’s disease visual hallucinations. Nat. Commun. 2022, 13, 519. [Google Scholar] [CrossRef]
- Ramírez-Ruiz, B.; Martí, M.-J.; Tolosa, E.; Giménez, M.; Bargalló, N.; Valldeoriola, F.; Junqué, C. Cerebral atrophy in Parkinson’s disease patients with visual hallucinations. Eur. J. Neurol. 2007, 14, 750–756. [Google Scholar] [CrossRef]
- Pagonabarraga, J.; Soriano-Mas, C.; Llebaria, G.; López-Solà, M.; Pujol, J.; Kulisevsky, J. Neural correlates of minor hallucinations in non-demented patients with Parkinson’s disease. Park. Relat. Disord. 2014, 20, 290–296. [Google Scholar] [CrossRef]
- Shin, S.; Lee, J.; Hong, J.; Sunwoo, M.K.; Sohn, Y.; Lee, P. Neuroanatomical substrates of visual hallucinations in patients with non-demented Parkinson’s disease. J. Neurol. Neurosurg. Psychiatry 2012, 83, 1155–1161. [Google Scholar] [CrossRef]
- Gama, R.L.; Bruin, V.M.S.; Távora, D.G.F.; Duran, F.L.S.; Bittencourt, L.; Tufik, S. Structural brain abnormalities in patients with Parkinson’s disease with visual hallucinations: A comparative voxel-based analysis. Brain Cogn. 2014, 87, 97–103. [Google Scholar] [CrossRef] [PubMed]
- Goldman, J.G.; Stebbins, G.T.; Dinh, V.; Bernard, B.; Merkitch, D.; deToledo-Morrell, L.; Goetz, C.G. Visuoperceptive region atrophy independent of cognitive status in patients with Parkinson’s disease with hallucinations. Brain 2014, 137, 849–859. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, H.; Senda, J.; Kato, S.; Ito, M.; Atsuta, N.; Hara, K.; Tsuboi, T.; Katsuno, M.; Nakamura, T.; Hirayama, M.; et al. Cortical and subcortical brain atrophy in Parkinson’s disease with visual hallucination. Mov. Disord. 2013, 28, 1732–1736. [Google Scholar] [CrossRef] [PubMed]
- Ibarretxe-Bilbao, N.; Ramírez-Ruiz, B.; Tolosa, E.; Marti, M.; Valldeoriola, F.; Bargalló, N.; Junqué, C. Hippocampal head atrophy predominance in Parkinson’s disease with hallucinations and with dementia. J. Neurol. 2008, 255, 1324–1331. [Google Scholar] [CrossRef] [PubMed]
- Janzen, J.; van ‘t Ent, D.; Lemstra, A.W.; Berendse, H.W.; Barkhof, F.; Foncke, E.M.J. The pedunculopontine nucleus is related to visual hallucinations in Parkinson’s disease: Preliminary results of a voxel-based morphometry study. J. Neurol. 2012, 259, 147–154. [Google Scholar] [CrossRef]
- Lawn, T.; Ffytche, D. Cerebellar correlates of visual hallucinations in Parkinson’s disease and Charles Bonnet Syndrome. Cortex 2021, 135, 311–325. [Google Scholar] [CrossRef]
- Stebbins, G.T.; Goetz, C.G.; Carrillo, M.C.; Bangen, K.J.; Turner, D.A.; Glover, G.H.; Gabrieli, J.D.E. Altered cortical visual processing in PD with hallucinations: An fMRI study. Neurology 2004, 63, 1409–1416. [Google Scholar] [CrossRef]
- Nagano-Saito, A.; Washimi, Y.; Arahata, Y.; Iwai, K.; Kawatsu, S.; Ito, K.; Nakamura, A.; Abe, Y.; Yamada, T.; Kato, T.; et al. Visual hallucination in Parkinson’s disease with FDG PET. Mov. Disord. 2004, 19, 801–806. [Google Scholar] [CrossRef] [PubMed]
- Boecker, H.; Ceballos-Baumann, A.O.; Volk, D.; Conrad, B.; Forstl, H.; Haussermann, P. Metabolic alterations in patients with Parkinson disease and visual hallucinations. Arch. Neurol. 2007, 64, 984–988. [Google Scholar] [CrossRef] [PubMed]
- Park, H.K.; Kim, J.S.; Im, K.C.; Kim, M.J.; Lee, J.-H.; Lee, M.C.; Kim, J.; Chung, S.J. Visual Hallucinations and Cognitive Impairment in Parkinson’s Disease. Can. J. Neurol. Sci. 2013, 40, 657–662. [Google Scholar] [CrossRef] [PubMed]
- Oishi, N.; Udaka, F.; Kameyama, M.; Sawamoto, N.; Hashikawa, K.; Fukuyama, H. Regional cerebral blood flow in Parkinson disease with nonpsychotic visual hallucinations. Neurology 2005, 65, 1708–1715. [Google Scholar] [CrossRef] [PubMed]
- Shine, J.M.; Halliday, G.M.; Naismith, S.L.; Lewis, S.J.G. Visual misperceptions and hallucinations in Parkinson’s disease: Dysfunction of attentional control networks? Mov. Disord. 2011, 26, 2154–2159. [Google Scholar] [CrossRef]
- Kiferle, L.; Ceravolo, R.; Giuntini, M.; Linsalata, G.; Puccini, G.; Volterrani, D.; Bonuccelli, U. Caudate dopaminergic denervation and visual hallucinations: Evidence from a 123I-FP-CIT SPECT study. Park. Relat. Disord. 2014, 20, 761–765. [Google Scholar] [CrossRef]
- Shine, J.M.; Halliday, G.M.; Gilat, M.; Matar, E.; Bolitho, S.J.; Carlos, M.; Naismith, S.L.; Lewis, S.J.G. The role of dysfunctional attentional control networks in visual misperceptions in Parkinson’s disease. Hum. Brain Mapp. 2014, 35, 2206–2219. [Google Scholar] [CrossRef]
- Hall, J.M.; O’Callaghan, C.; Muller, A.J.; Ehgoetz Martens, K.A.; Phillips, J.R.; Moustafa, A.A.; Lewis, S.J.G.; Shine, J.M. Changes in structural network topology correlate with severity of hallucinatory behavior in Parkinson’s disease. Netw. Neurosci. 2019, 3, 521–538. [Google Scholar] [CrossRef]
- Zarkali, A.; McColgan, P.; Ryten, M.; Reynolds, R.; Leyland, L.-A.; Lees, A.J.; Rees, G.; Weil, R.S. Differences in network controllability and regional gene expression underlie hallucinations in Parkinson’s disease. Brain 2020, 143, 3435–3448. [Google Scholar] [CrossRef]
- Zarkali, A.; McColgan, P.; Leyland, L.A.; Lees, A.J.; Weil, R.S. Longitudinal thalamic white and grey matter changes associated with visual hallucinations in Parkinson’s disease. J. Neurol. Neurosurg. Psychiatry 2022, 93, 169–179. [Google Scholar] [CrossRef]
- van Ommen, M.M.; van Laar, T.; Renken, R.; Cornelissen, F.W.; Bruggeman, R. Visual Hallucinations in Psychosis: The Curious Absence of the Primary Visual Cortex. Schizophr. Bull. 2023, 49, S68–S81. [Google Scholar] [CrossRef] [PubMed]
- Popova, E. Role of Dopamine in Retinal Function. In Webvision: The Organization of the Retina and Visual System; Kolb, H., Fernandez, E., Nelson, R., Eds.; University of Utah Health Sciences Center: Salt Lake City, UT, USA, 2020. [Google Scholar]
- Warwick, R.A.; Heukamp, A.S.; Riccitelli, S.; Rivlin-Etzion, M. Dopamine differentially affects retinal circuits to shape the retinal code. J. Physiol. 2023, 601, 1265–1286. [Google Scholar] [CrossRef] [PubMed]
- Railo, H.; Olkoniemi, H.; Eeronheimo, E.; Pääkkönen, O.; Joutsa, J.; Kaasinen, V. Dopamine and eye movement control in Parkinson’s disease: Deficits in corollary discharge signals? PeerJ 2018, 6, e6038. [Google Scholar] [CrossRef] [PubMed]
- Crawford, T.J.; Henderson, L.; Kennard, C. Abnormalities of nonvisually-guided eye movements in Parkinson’s disease. Brain 1989, 112, 1573–1586. [Google Scholar] [CrossRef] [PubMed]
- Hanna-Pladdy, B.; Pahwa, R.; Lyons, K.E. Dopaminergic Basis of Spatial Deficits in Early Parkinson’s Disease. Cereb. Cortex Commun. 2021, 2, tgab042. [Google Scholar] [CrossRef]
- Ravina, B.; Marder, K.; Fernandez, H.H.; Friedman, J.H.; McDonald, W.; Murphy, D.; Aarsland, D.; Babcock, D.; Cummings, J.; Endicott, J.; et al. Diagnostic criteria for psychosis in Parkinson’s disease: Report of an NINDS, NIMH work group. Mov. Disord. 2007, 22, 1061–1068. [Google Scholar] [CrossRef]
- Bohnen, N.I.; Kaufer, D.I.; Hendrickson, R.; Ivanco, L.S.; Lopresti, B.J.; Constantine, G.M.; Mathis, C.A.; Davis, J.G.; Moore, R.Y.; Dekosky, S.T. Cognitive correlates of cortical cholinergic denervation in Parkinson’s disease and parkinsonian dementia. J. Neurol. 2006, 253, 242–247. [Google Scholar] [CrossRef]
- Manganelli, F.; Vitale, C.; Santangelo, G.; Pisciotta, C.; Iodice, R.; Cozzolino, A.; Dubbioso, R.; Picillo, M.; Barone, P.; Santoro, L. Functional involvement of central cholinergic circuits and visual hallucinations in Parkinson’s disease. Brain 2009, 132, 2350–2355. [Google Scholar] [CrossRef]
- Firbank, M.J.; Parikh, J.; Murphy, N.; Killen, A.; Allan, C.L.; Collerton, D.; Blamire, A.M.; Taylor, J.-P. Reduced occipital GABA in Parkinson disease with visual hallucinations. Neurology 2018, 91, e675–e685. [Google Scholar] [CrossRef]
- Cho, S.S.; Strafella, A.P.; Duff-Canning, S.; Zurowski, M.; Vijverman, A.; Bruno, V.; Aquino, C.C.; Criaud, M.; Rusjan, P.M.; Houle, S.; et al. The Relationship Between Serotonin-2A Receptor and Cognitive Functions in Nondemented Parkinson’s Disease Patients with Visual Hallucinations. Mov. Disord. Clin. Pract. 2017, 4, 698–709. [Google Scholar] [CrossRef]
- Marras, C.; Schüle, B.; Munhoz, R.P.; Rogaeva, E.; Langston, J.W.; Kasten, M.; Meaney, C.; Klein, C.; Wadia, P.M.; Lim, S.-Y.; et al. Phenotype in parkinsonian and nonparkinsonian LRRK2 G2019S mutation carriers. Neurology 2011, 77, 325–333. [Google Scholar] [CrossRef] [PubMed]
- Alcalay, R.N.; Caccappolo, E.; Mejia-Santana, H.; Tang, M.-X.; Rosado, L.; Orbe Reilly, M.; Ruiz, D.; Ross, B.; Verbitsky, M.; Kisselev, S.; et al. Cognitive performance of GBA mutation carriers with early-onset PD: The CORE-PD study. Neurology 2012, 78, 1434–1440. [Google Scholar] [CrossRef] [PubMed]
- Zokaei, N.; McNeill, A.; Proukakis, C.; Beavan, M.; Jarman, P.; Korlipara, P.; Hughes, D.; Mehta, A.; Hu, M.T.M.; Schapira, A.H.V.; et al. Visual short-term memory deficits associated with GBA mutation and Parkinson’s disease. Brain 2014, 137, 2303–2311. [Google Scholar] [CrossRef]
- Neumann, J.; Bras, J.; Deas, E.; O’Sullivan, S.S.; Parkkinen, L.; Lachmann, R.H.; Li, A.; Holton, J.; Guerreiro, R.; Paudel, R.; et al. Glucocerebrosidase mutations in clinical and pathologically proven Parkinson’s disease. Brain 2009, 132, 1783–1794. [Google Scholar] [CrossRef]
- Nombela, C.; Rowe, J.B.; Winder-Rhodes, S.E.; Hampshire, A.; Owen, A.M.; Breen, D.P.; Duncan, G.W.; Khoo, T.K.; Yarnall, A.J.; Firbank, M.J.; et al. Genetic impact on cognition and brain function in newly diagnosed Parkinson’s disease: ICICLE-PD study. Brain 2014, 137, 2743–2758. [Google Scholar] [CrossRef]
- Garcia-Diaz, A.I.; Segura, B.; Baggio, H.C.; Marti, M.J.; Valldeoriola, F.; Compta, Y.; Vendrell, P.; Bargallo, N.; Tolosa, E.; Junque, C. Structural MRI correlates of the MMSE and pentagon copying test in Parkinson’s disease. Park. Relat. Disord. 2014, 20, 1405–1410. [Google Scholar] [CrossRef]
- Powell, A.; Ireland, C.; Lewis, S.J.G. Visual Hallucinations and the Role of Medications in Parkinson’s Disease: Triggers, Pathophysiology, and Management. J. Neuropsychiatry Clin. Neurosci. 2020, 32, 334–343. [Google Scholar] [CrossRef] [PubMed]
- Nantel, J.; McDonald, J.C.; Tan, S.; Bronte-Stewart, H. Deficits in visuospatial processing contribute to quantitative measures of freezing of gait in Parkinson’s disease. Neuroscience 2012, 221, 151–156. [Google Scholar] [CrossRef] [PubMed]

| Domain | Task | Cortical Region |
|---|---|---|
| Visuoperceptual | Facial Recognition Test (FRT) [112,141] Visual Form Discrimination Test (VFDT) [112] | Fusiform Gyrus (BA 19, 36) Parahippocampal Middle Occipital Gyrus Inferior Frontal Gyrus (BA 47) Left Lateral Occipital Bilateral Superior Parietal (BA 7, 40) Superior Occipital (BA 19) Inferior Frontal Gyrus (BA 47) |
| Visuospatial | Judgement Line Orientation Task (JLO) [143] | Bilateral Superior Temporal Right Lateral Occipital |
| Visuoconstructive | Pentagon Copy Test (PCT) [143] | Right Supplementary Motor Left Rostral Middle Frontal Pars Triangularis Left Cuneus |
| Domain | Task | Cortical Region |
|---|---|---|
| Visuoperceptual | Facial Recognition Test (FRT) Symbol Digit Modalities Test (SDMT) | Left Lingual Gyrus Left Superior Temporal Left Parahippocampal Left Lingual Gyrus Right Parahippocampal |
| Visuospatial | Judgement Line Orientation Task (JLO) | Left Insula Inferior Temporal Superior Temporal Right Fusiform Gyrus |
| Visuoconstruction | Pentagon Copy Test (PCT) | Left Entorhinal Middle and Inferior Temporal Gyri Medial Temporal Pole Parahippocampal Fusiform Cortex Lingual Cortex Lateral Occipital Cortex |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nieto-Escamez, F.; Obrero-Gaitán, E.; Cortés-Pérez, I. Visual Dysfunction in Parkinson’s Disease. Brain Sci. 2023, 13, 1173. https://doi.org/10.3390/brainsci13081173
Nieto-Escamez F, Obrero-Gaitán E, Cortés-Pérez I. Visual Dysfunction in Parkinson’s Disease. Brain Sciences. 2023; 13(8):1173. https://doi.org/10.3390/brainsci13081173
Chicago/Turabian StyleNieto-Escamez, Francisco, Esteban Obrero-Gaitán, and Irene Cortés-Pérez. 2023. "Visual Dysfunction in Parkinson’s Disease" Brain Sciences 13, no. 8: 1173. https://doi.org/10.3390/brainsci13081173
APA StyleNieto-Escamez, F., Obrero-Gaitán, E., & Cortés-Pérez, I. (2023). Visual Dysfunction in Parkinson’s Disease. Brain Sciences, 13(8), 1173. https://doi.org/10.3390/brainsci13081173









