The Effects of the Early Start Denver Model for Children with Autism Spectrum Disorder: A Meta-Analysis
Abstract
1. Introduction
1.1. Naturalistic Developmental Behavioral Interventions
1.2. Early Start Denver Model
1.3. Research Questions
2. Materials and Methods
2.1. Eligibility Criteria
2.2. Search Procedure
2.3. Data Extraction and Coded Variables
2.4. Analytic Strategies
3. Results
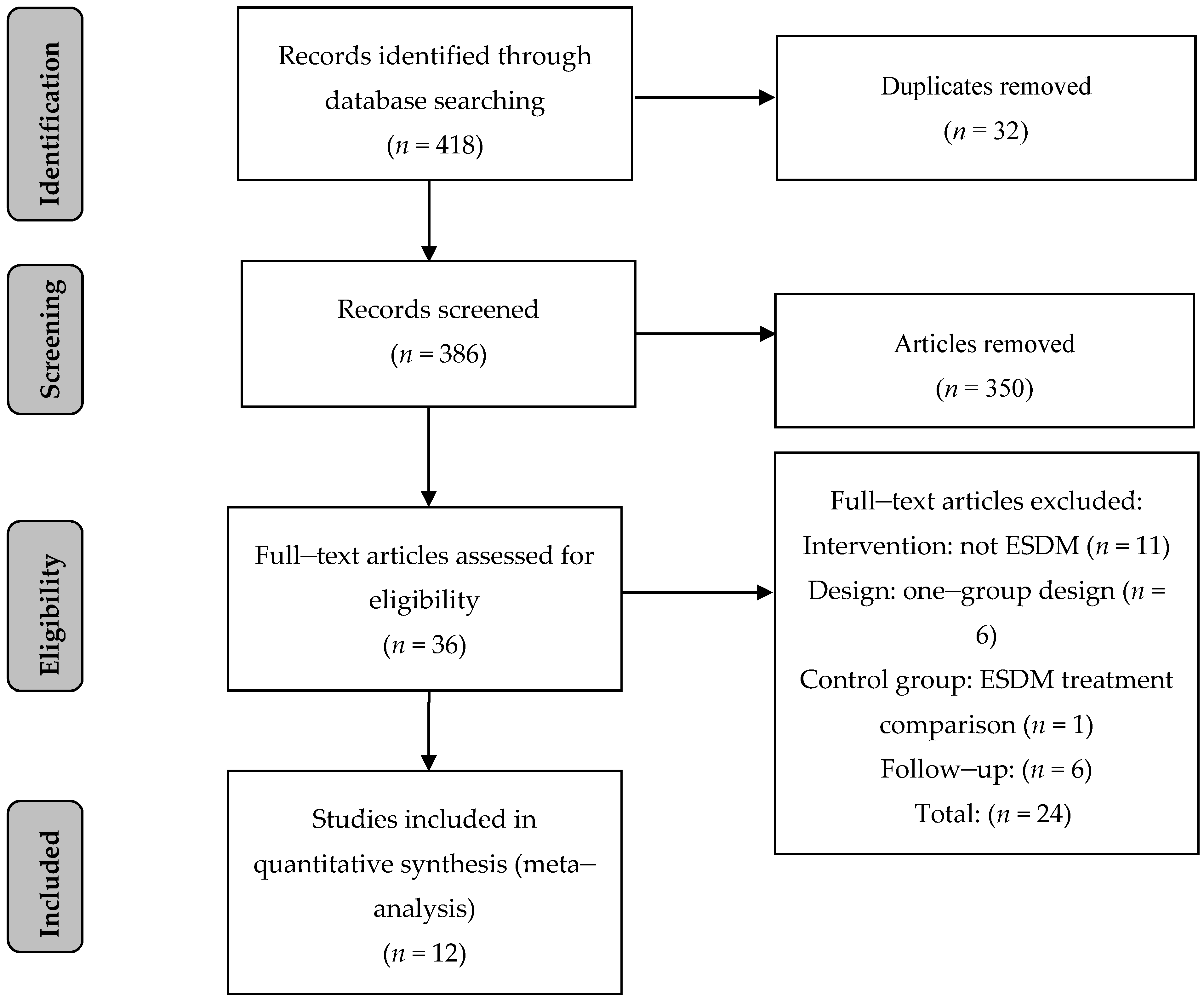
3.1. Study Selection
3.2. Study Characteristics
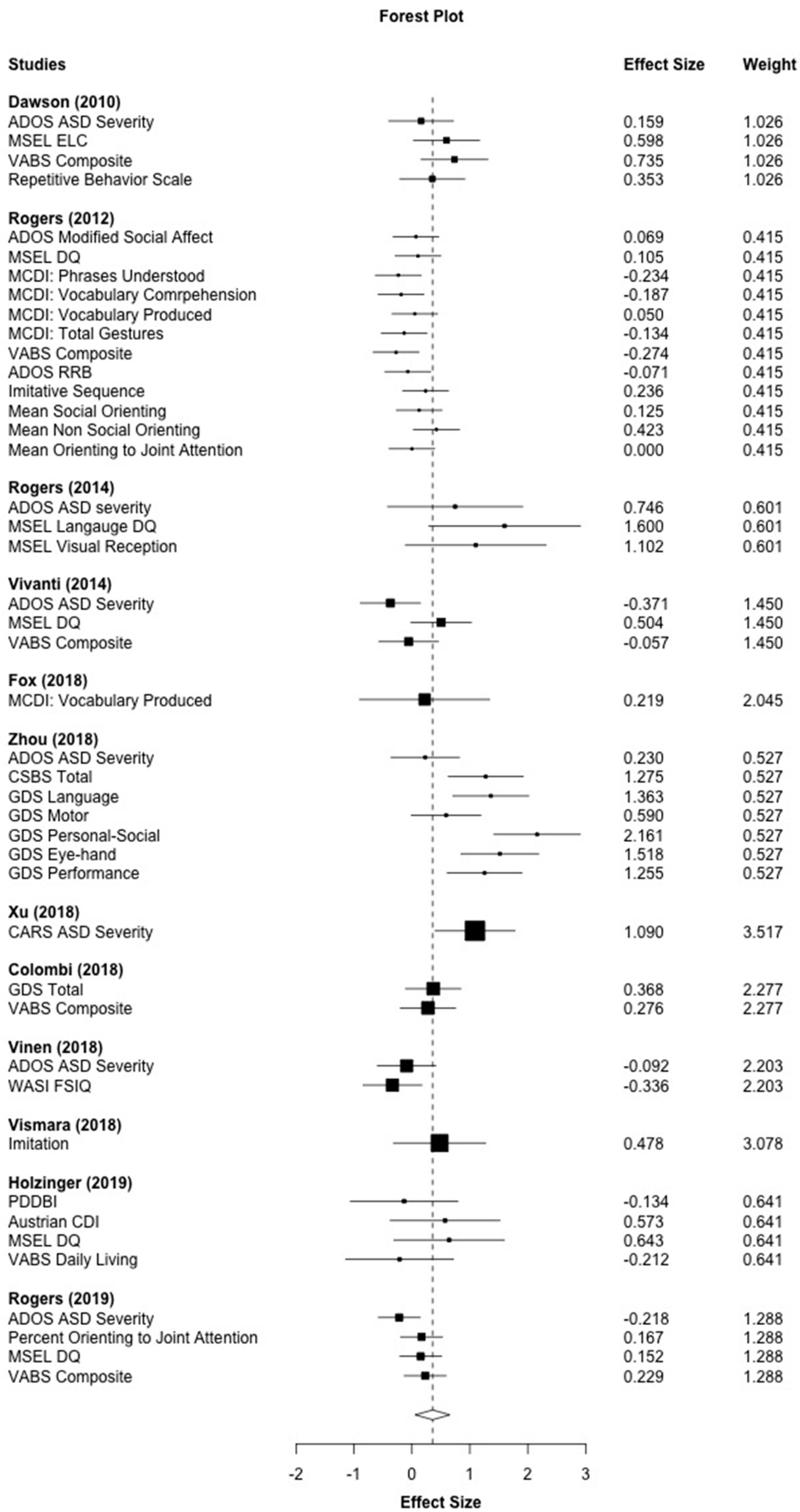
3.3. Overall Outcomes
3.4. Study Quality Indicators
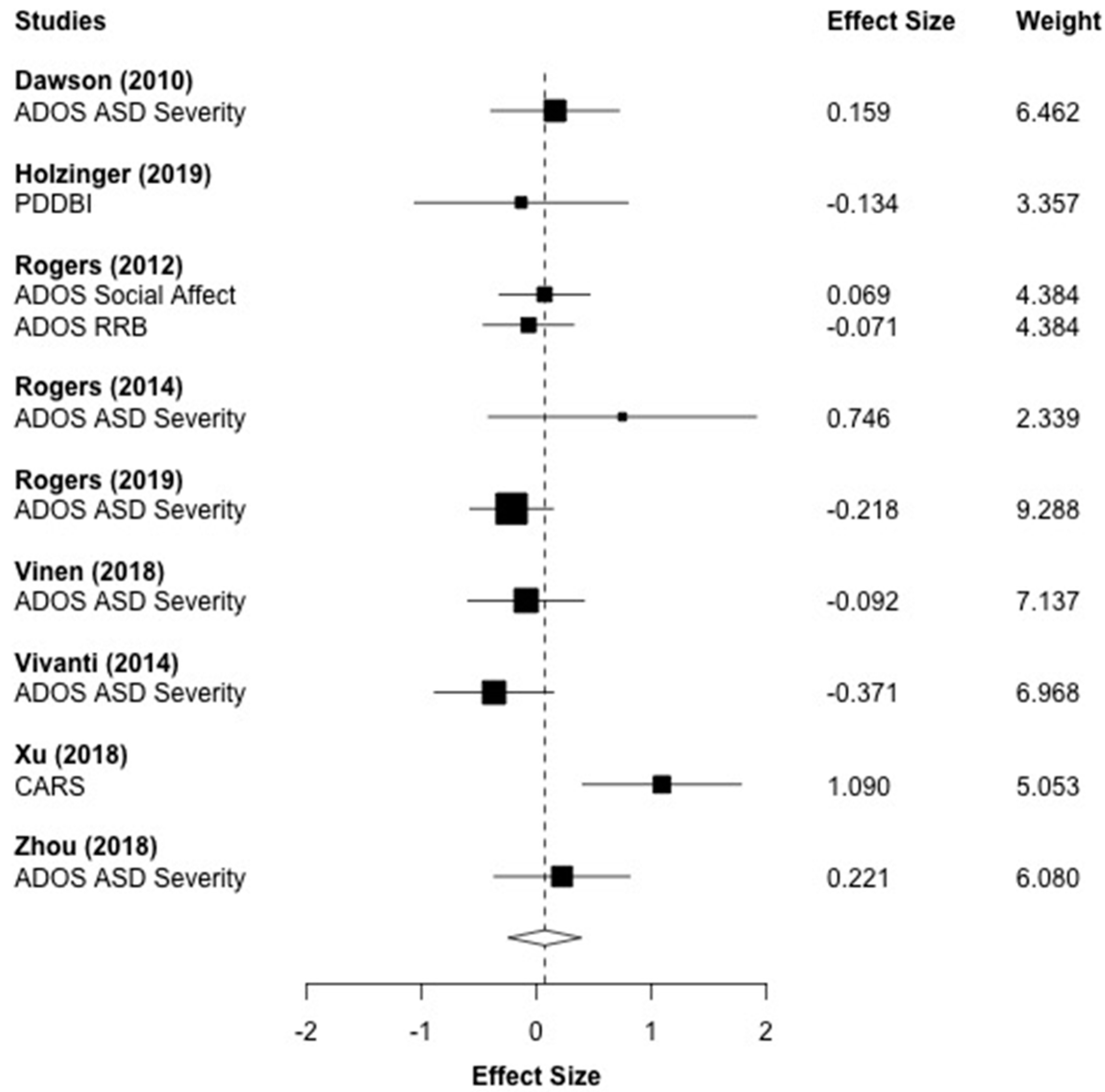
3.5. Autism Symptoms
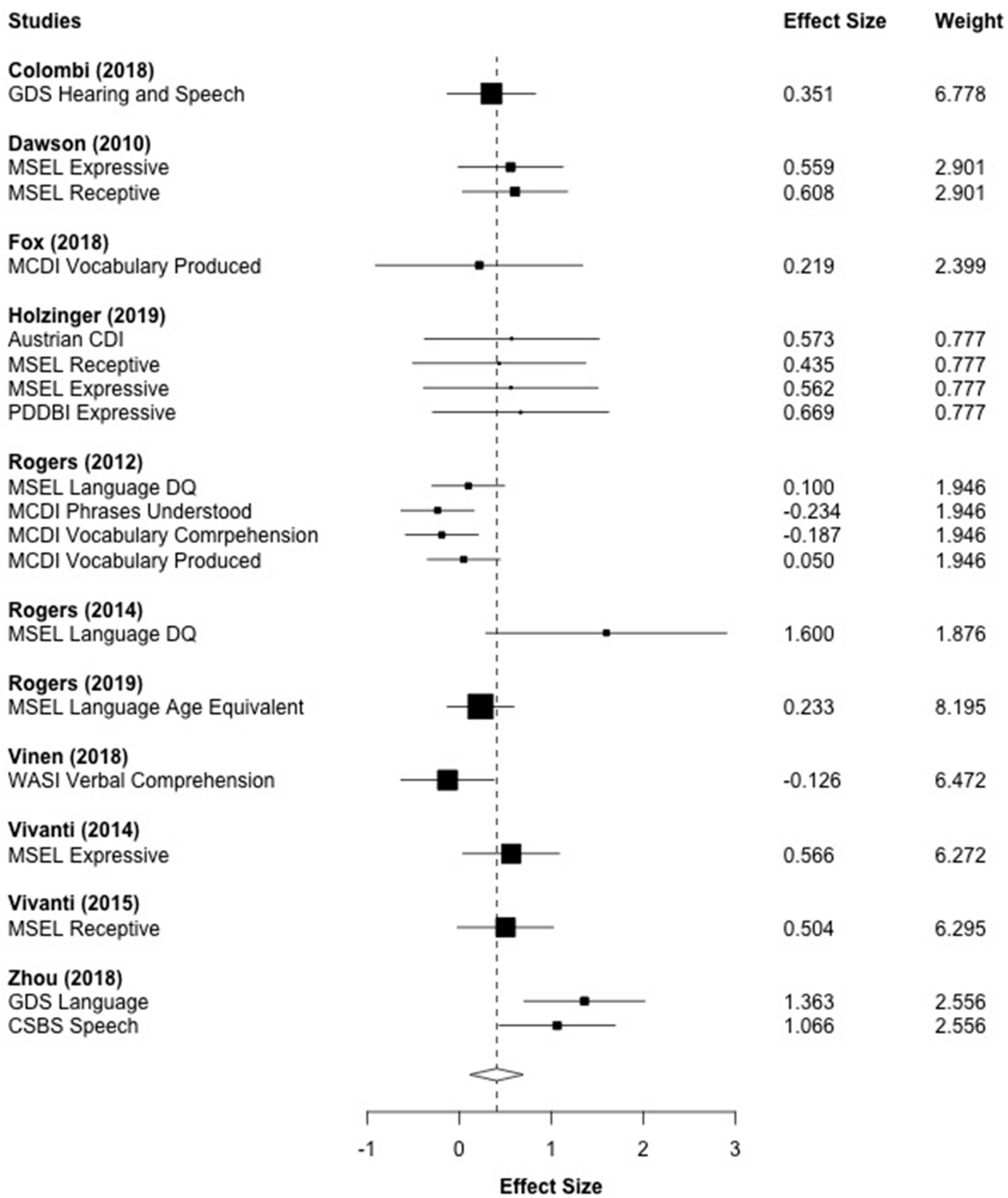
3.6. Language
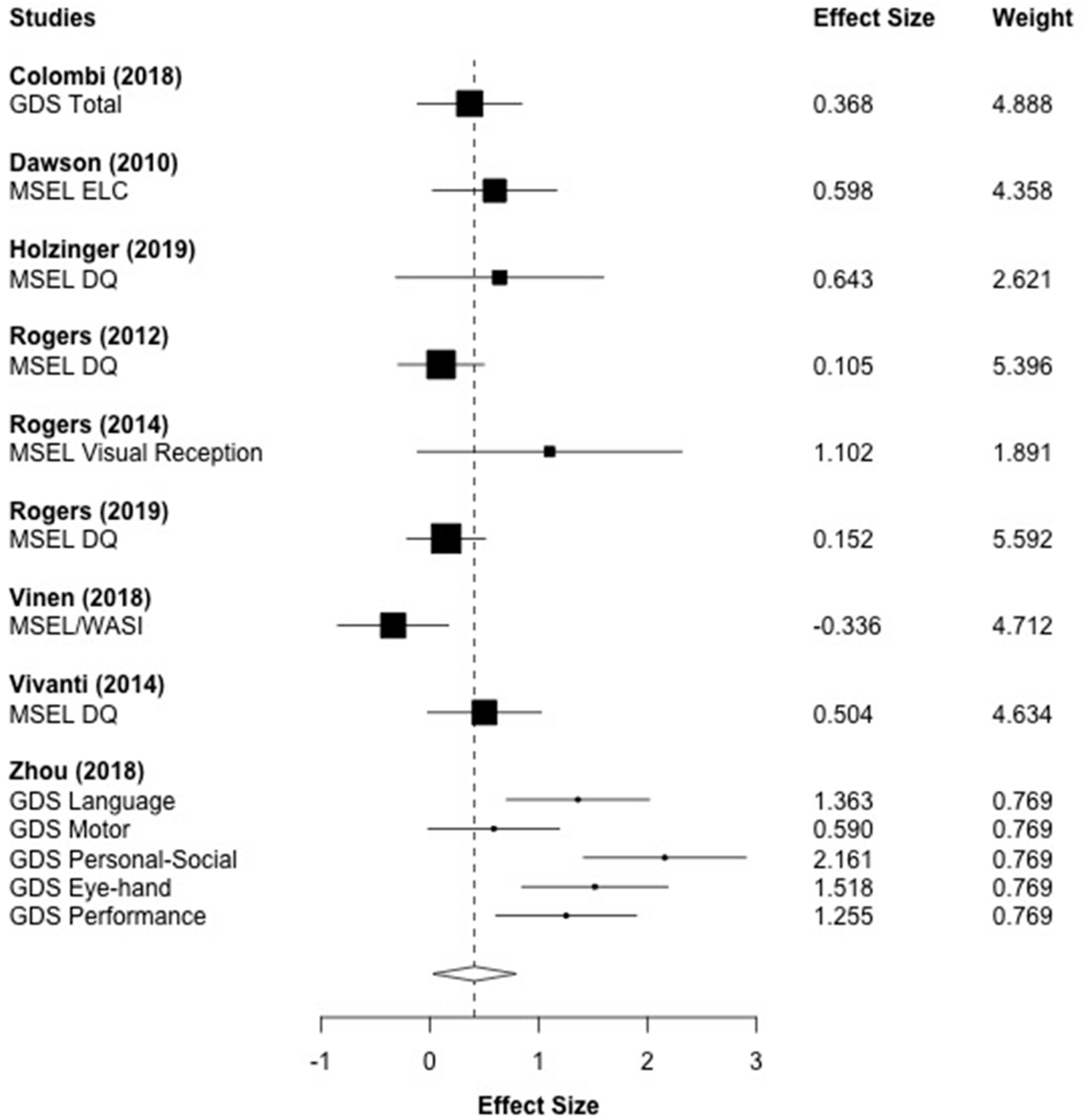
3.7. Cognition
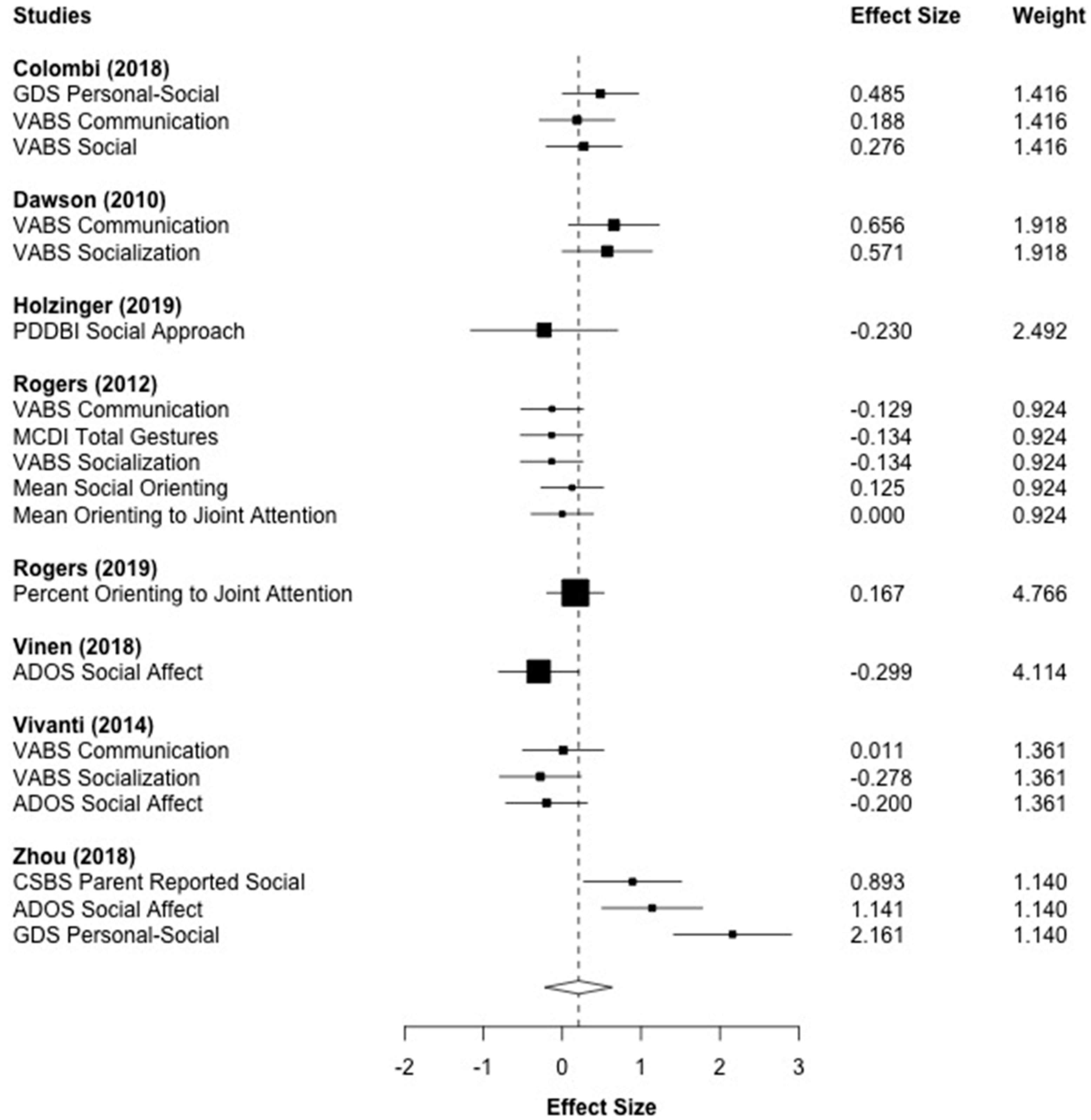
3.8. Social Communication
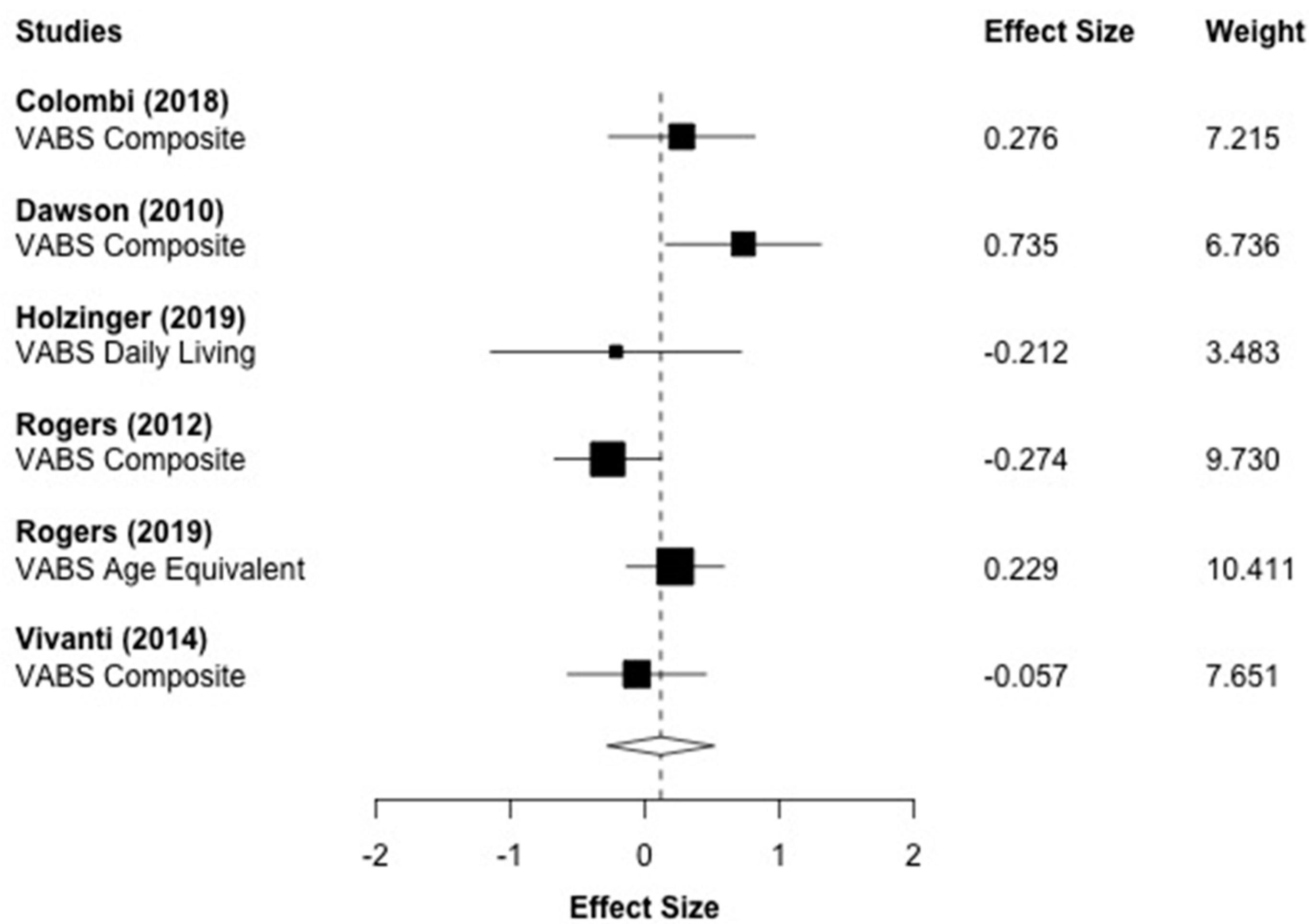
3.9. Adaptive Functioning
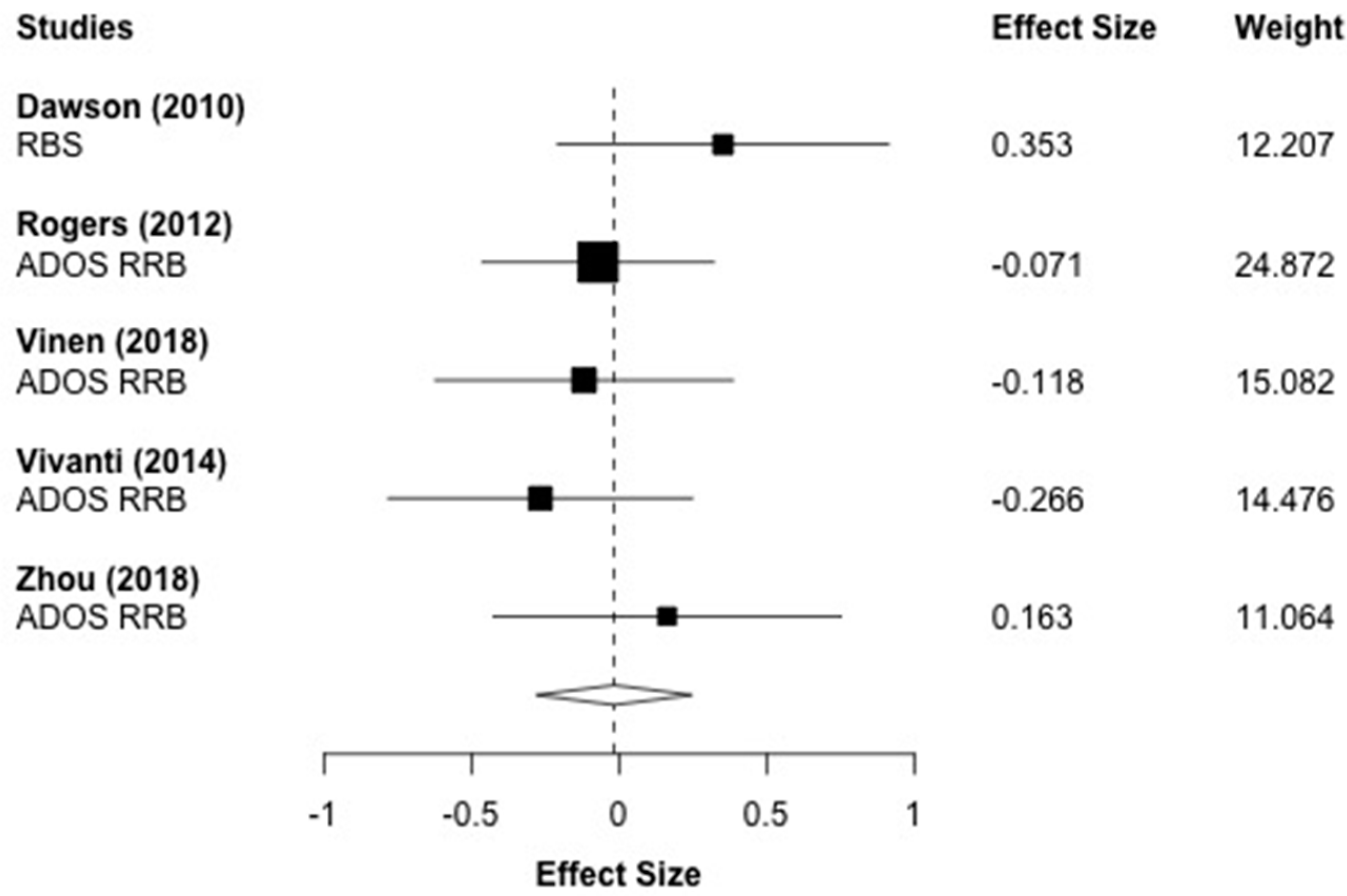
3.10. Repetitive Behaviors
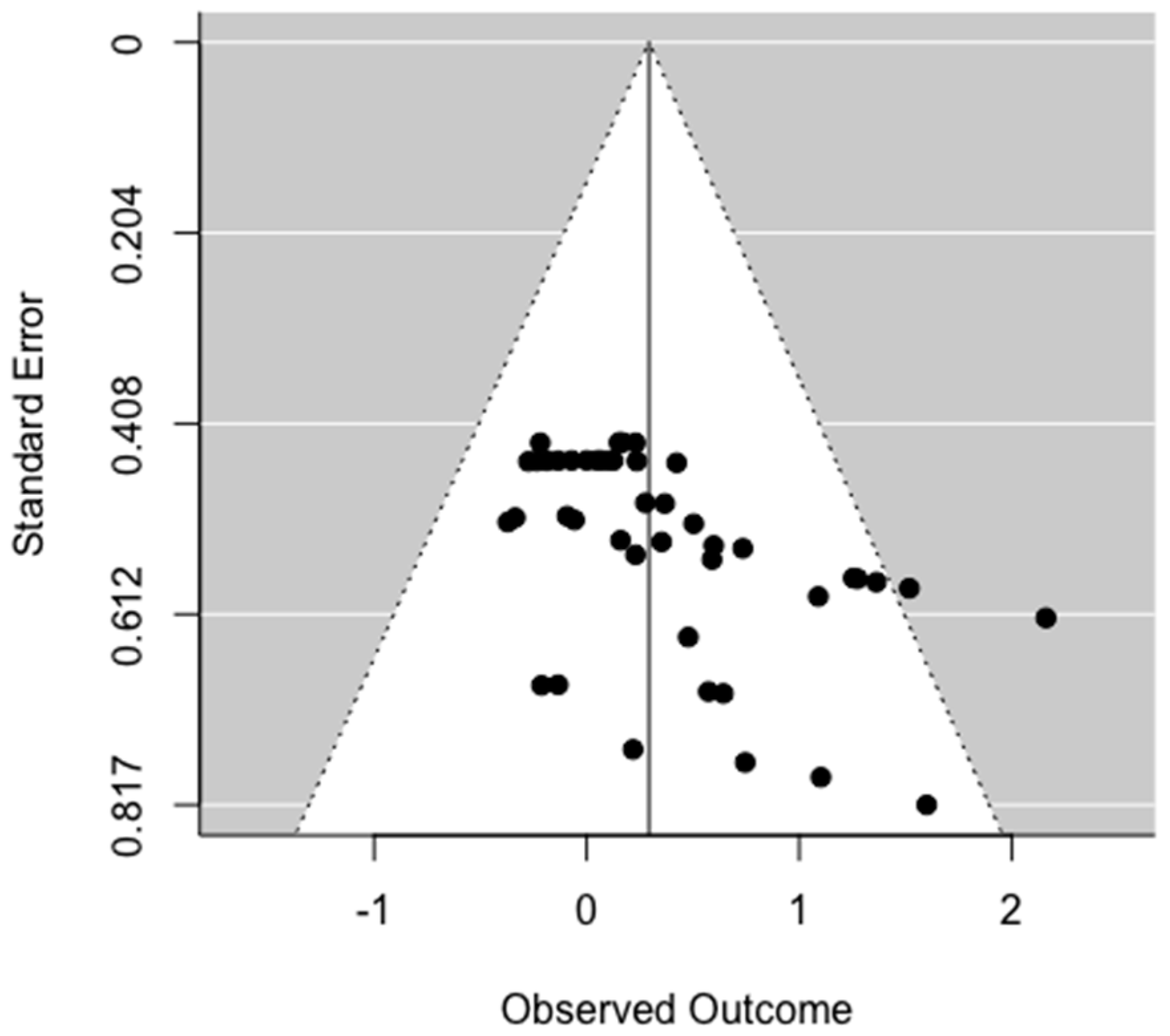
3.11. Publication Bias
4. Discussion
Limitations and Future Directions
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A
| Author (Year) | Intervention Group (n) | Control Group (n) | Control Group |
|---|---|---|---|
| Dawson (2010) [25] | 24 | 24 | Treatment as usual, plus intervention recommendations, community referrals, and reading material |
| Rogers (2012) [26] | 49 | 49 | Treatment as usual |
| Rogers (2014) [13] | 7 | 25 | Treatment as usual |
| Vivanti (2014) [23] | 27 | 30 | Group-based “generic” intervention program for children with autism spectrum disorders (ASD) |
| Fox (2018) [21] | 5 | 5 | Waitlist |
| Zhou (2018) [22] | 23 | 20 | Treatment as usual |
| Xu (2018) [27] | 20 | 20 | Eclectic intervention services matching the amount of time the Early Start Denver Model (ESDM) group received |
| Colombi (2018) [28] | 22 | 70 | Treatment as usual |
| Vinen (2018) [24] | 31 | 28 | Group-based eclectic intervention program for children with ASD |
| Vismara (2018) [29] | 16 | 14 | Monthly check-ins and access to online material |
| Holzinger (2019) [30] | 7 | 6 | Treatment as usual |
| Rogers (2019) [31] | 55 | 63 | Treatment as usual |
Appendix B
References
- Maenner, M.J.; Shaw, K.A.; Baio, J.; Washington, A.; Patrick, M.; DiRienzo, M.; Christensen, D.L.; Wiggins, L.D.; Pettygrove, S.; Andrews, J.G.; et al. Prevalence of autism spectrum disorder among children aged 8 years—Autism and developmental disabilities monitoring network, 11 Sites, United States, 2016. MMWR. Surveill. Summ. 2020, 69, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Zwaigenbaum, L.; Bauman, M.; Choueiri, R.; Kasari, C.; Carter, A.S.; Granpeesheh, R.; Mailloux, Z.; Roley, S.S.; Wagner, S.; Fein, D.; et al. Early intervention for children with autism spectrum disorder under 3 years of age: Recommendations for practice and research. Pediatrics 2015, 136, S60–S81. [Google Scholar] [CrossRef] [PubMed]
- Corsello, C.M. Early intervention in autism. Infants Young Child. 2005, 18, 74–85. [Google Scholar] [CrossRef]
- Amendah, D.; Peacock, G.; Grosse, S.D.; Mandell, D.S.; Geschwind, D.; Dawson, G. The economic costs of autism: A review. Autism Spectrum Disorders 2011, 1347–1360. [Google Scholar] [CrossRef]
- Schreibman, L.; Dawson, G.; Stahmer, A.C.; Landa, R.J.; Rogers, S.J.; McGee, G.G.; Kasari, C.; Ingersoll, B.; Kaiser, A.; Bruinsma, Y.; et al. Naturalistic developmental behavioral interventions: Empirically validated treatments for autism spectrum disorder. J. Autism Dev. Disord. 2015, 45, 2411–2428. [Google Scholar] [CrossRef]
- Sandbank, M.; Bottema-Beutel, K.; Crowley, S.; Cassidy, M.; Dunham, K.; Feldman, J.I.; Crank, J.; Albarran, S.A.; Raj, S.; Mahbub, P.; et al. Project AIM: Autism intervention meta-analysis for studies of young children. Psychol. Bull. 2020, 146, 1–29. [Google Scholar] [CrossRef] [PubMed]
- Fuller, E.A.; Kaiser, A.P. The effects of early intervention on social communication outcomes for children with autism spectrum disorder: A meta-analysis. J. Autism Dev. Disord. 2019, 50, 1683–1700. [Google Scholar] [CrossRef] [PubMed]
- Yoder, P.; Bottema-Beutel, K.; Woynaroski, T.; Chandrasekhar, R.; Sandbank, M. Social communication intervention effects vary by dependent variable type in preschoolers with autism spectrum disorders. Evidence-Based Commun. Assess. Interv. 2014, 7, 150–174. [Google Scholar] [CrossRef] [PubMed]
- Rogers, S.J.; Dawson, G. Early Start Denver Model for Young Children with Autism: Promoting Language, Learning, and Engagement; Guilford Press: New York, NY, USA, 2010. [Google Scholar]
- Cidav, Z.; Munson, J.; Estes, A.; Dawson, G.; Rogers, S.; Mandell, D. Cost offset associated with early start denver model for children with autism. J. Am. Acad. Child Adolesc. Psychiatry 2017, 56, 777–783. [Google Scholar] [CrossRef]
- Waddington, H.; Van Der Meer, L.; Sigafoos, J. Effectiveness of the early start denver model: A systematic review. Rev. J. Autism Dev. Disord. 2016, 3, 93–106. [Google Scholar] [CrossRef]
- Baril, E.M.; Humphreys, B.P. An evaluation of the research evidence on the early start denver model. J. Early Interv. 2017, 39, 321–338. [Google Scholar] [CrossRef]
- Rogers, S.J.; Vismara, L.; Wagner, A.L.; McCormick, C.; Young, G.; Ozonoff, S. Autism treatment in the first year of life: A pilot study of infant start, a parent-implemented intervention for symptomatic infants. J. Autism Dev. Disord. 2014, 44, 2981–2995. [Google Scholar] [CrossRef] [PubMed]
- Mullen, E.M. Mullen scales of early learning; AGS: Circle Pines, MN, USA, 1995. [Google Scholar]
- Michael, B.; Larry, V.H.; Julian, H.; Hannah, R.W. Introduction to Meta-Analysis; John Wiley Sons Ltd.: West Sussex, UK, 2009. [Google Scholar]
- Borenstein, M.; Cooper, H.; Hedges, L.; Valentine, J. Effect sizes for continuous data. Handb. Res. Synth. Meta-Anal. 2009, 2, 221–235. [Google Scholar]
- Fisher, Z.; Tipton, E.; Zhipeng, H.; Fisher, M.Z. Package ‘Robumeta.’ Retrieved From 2017. Available online: https://cran.r-project.org/web/packages/robumeta/robumeta.pdf (accessed on 19 January 2020).
- Tanner-Smith, E.E.; Tipton, E.; Polanin, J.R. Handling complex meta-analytic data structures using robust variance estimates: A tutorial in R. J. Dev. Life-Course Criminol. 2016, 2, 85–112. [Google Scholar] [CrossRef]
- Thalheimer, W.; Cook, S. How to calculate effect sizes from published research: A simplified methodology. Work-Learn. Res. 2002, 1, 1–9. [Google Scholar]
- Egger, M.; Smith, G.D.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef]
- Fox, S.A. An Early Start Denver Model-Based Group Intervention for Parents of Very Young Children Diagnosed with or at Risk for Autism Spectrum Disorder. Ph.D. Thesis, University at Albany. Department of Psychology, Albany, NY, USA, 2017. [Google Scholar]
- Zhou, B.; Xu, Q.; Li, H.; Zhang, Y.; Wang, Y.; Xu, X.; Rogers, S.J. Effects of parent-implemented early start denver model intervention on chinese toddlers with autism spectrum disorder: A non-randomized controlled trial. Autism Res. 2018, 11, 654–666. [Google Scholar] [CrossRef]
- Vivanti, G.; The Victorian ASELCC Team; Paynter, J.; Duncan, E.; Fothergill, H.; Dissanayake, C.; Rogers, S.J. Effectiveness and feasibility of the early start denver model implemented in a group-based community childcare setting. J. Autism Dev. Disord. 2014, 44, 3140–3153. [Google Scholar] [CrossRef] [PubMed]
- Vinen, Z.; Clark, M.; Paynter, J.; Dissanayake, C. School age outcomes of children with autism spectrum disorder who received community-based early interventions. J. Autism Dev. Disord. 2017, 48, 1673–1683. [Google Scholar] [CrossRef] [PubMed]
- Dawson, G.; Rogers, S.; Munson, J.; Smith, M.; Winter, J.; Greenson, J.; Donaldson, A.; Varley, J. Randomized, controlled trial of an intervention for toddlers with autism: The Early Start Denver Model. Pediatrics 2009, 125, e17–e23. [Google Scholar] [CrossRef] [PubMed]
- Rogers, S.J.; Estes, A.; Lord, C.; Vismara, L.; Winter, J.; Fitzpatrick, A.; Guo, M.; Dawson, G. Effects of a brief early start denver model (ESDM)–based parent intervention on toddlers at risk for autism spectrum disorders: A randomized controlled trial. J. Am. Acad. Child Adolesc. Psychiatry 2012, 51, 1052–1065. [Google Scholar] [CrossRef] [PubMed]
- Xu, Y.; Yang, J.; Yao, J.; Chen, J.; Zhuang, X.; Wang, W.; Zhang, X.; Lee, G.T. A pilot study of a culturally adapted early intervention for young children with autism spectrum disorders in China. J. Early Interv. 2017, 40, 52–68. [Google Scholar] [CrossRef]
- Colombi, C.; Narzisi, A.; Ruta, L.; Cigala, V.; Gagliano, A.; Pioggia, G.; Siracusano, R.; Rogers, S.J.; Muratori, F.; Team, P.P. Implementation of the early start denver model in an Italian community. Autism 2016, 22, 126–133. [Google Scholar] [CrossRef] [PubMed]
- Vismara, L.A.; McCormick, C.E.B.; Wagner, A.L.; Monlux, K.; Nadhan, A.; Young, G.S. Telehealth parent training in the early start denver model: Results from a randomized controlled study. Focus Autism Other Dev. Disabil. 2016, 33, 67–79. [Google Scholar] [CrossRef]
- Holzinger, D.; Laister, D.; Vivanti, G.; Barbaresi, W.J.; Fellinger, J. Feasibility and outcomes of the early start denver model implemented with low intensity in a community setting in Austria. J. Dev. Behav. Pediatr. 2019, 40, 354–363. [Google Scholar] [CrossRef]
- Rogers, S.; Estes, A.; Lord, C.; Munson, J.; Rocha, M.; Winter, J.; Greenson, J.; Colombi, C.; Dawson, G.; Vismara, L.A.; et al. A multisite randomized controlled two-phase trial of the early start denver model compared to treatment as usual. J. Am. Acad. Child Adolesc. Psychiatry 2019, 58, 853–865. [Google Scholar] [CrossRef]
- Sparrow, S.S.; Cicchetti, D.V.; Balla, D.A. The vineland adaptive behavior scales. Major Psychol. Assess. Instrum. 1989, 2, 199–231. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Earlbam Associates: New York, NY, USA, 1988. [Google Scholar]
- Hampton, L.H.; Kaiser, A. Intervention effects on spoken-language outcomes for children with autism: A systematic review and meta-analysis. J. Intellect. Disabil. Res. 2016, 60, 444–463. [Google Scholar] [CrossRef]
- Lord, C.; Rutter, M.; DiLavore, P.C.; Risi, S. Autism Diagnostic Observation Schedule--Generic. PsycTESTS Dataset. 1999. Available online: https://psycnet.apa.org/doiLanding?doi=10.1037%2Ft17256-000 (accessed on 12 June 2020).
- Grzadzinski, R.; Carr, T.; Colombi, C.; McGuire, K.; Dufek, S.; Pickles, A.; Lord, C. Measuring changes in social communication behaviors: Preliminary development of the brief observation of social communication change (BOSCC). J. Autism Dev. Disord. 2016, 46, 2464–2479. [Google Scholar] [CrossRef]
| Inclusion Criteria | Criteria | Corresponding Search Terms |
|---|---|---|
| Participants | Autism spectrum disorder, all participants younger than age 6 | |
| Intervention | Early Start Denver Model | “Early Start Denver Model” (Anywhere) |
| Comparison | Treatment as usual, waitlist control, general information only, referral to other services, or non-ESDM intervention | assign* OR group OR BAU OR “wait list” OR RCT OR random* OR quasi OR control* OR trial (Abstract) |
| Outcome | Any child outcome | |
| Study Design | Group design study, including randomized control trial and quasi experimental design |
| Author (year) [ref] | Country | Participants (n) | Average Age (Years) | Percent Male | Intervention Length (Weeks) | Hours per Week | Primary Implementer | Parent Coaching | Group | Fidelity | Blind Assessors | Random Assignment |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Dawson (2010) [25] | USA | 48 | 1.95 | 72 | 104 | 20 | Professional | yes | no | 85% | yes | yes |
| Rogers (2012) [26] | USA | 98 | 1.75 | 77.55 | 12 | 1 | Parent | yes | no | 75% | yes | yes |
| Rogers (2014) [13] | USA | 11 | 0.75 | 65.63 | 18 | 1 | Parent | yes | no | 91% | yes | no |
| Vivanti (2014) [23] | Australia | 57 | 3.4 | 87.72 | 52 | 15 | Professional | yes | yes | 92% | no | no |
| Fox (2018) [21] | USA | 10 | 2.73 | 70 | 6 | 3 | Parent | yes | yes | NA | yes | |
| Zhou (2018) [22] | China | 43 | 2.21 | 88.37 | 26 | 1.5 | Parent | yes | mix | 80% | yes | no |
| Xu (2018) [27] | China | 40 | 3.77 | 88.75 | 8 | 5 | Professional | yes | no | 85% | yes | yes |
| Colombi (2018) [28] | Italy | 92 | 2.76 | 24 | 6 | Professional | no | no | 80% * | no | no | |
| Vinen (2018) [24] | USA | 59 | 3.11 | 88.1 | 156 † | 15–20 | Professional | yes | yes | 80% * | yes | no |
| Vismara (2018) [29] | USA | 30 | 2.46 | 70.83 | 12 | 1.5 | Parent | yes | no | yes | yes | |
| Holzinger (2019) [30] | Austria | 16 | 3.62 | 100 | 52 | 4.6 | Professional | no | no | 80% * | no | no |
| Rogers (2019) [31] | USA | 118 | 1.72 | 77.97 | 116 | 16 | Professional | yes | no | 84% | yes | yes |
| Study Author (Year) [ref] | Outcome Measure | Post-Test Mean (SD): Intervention Group | Post-Test Mean (SD): Control Group | Hedges’ g (SE) | Distal | General-ized | Parent Report | CME |
|---|---|---|---|---|---|---|---|---|
| Dawson (2010) [25] | ADOS ASD severity | 7 (1.9) | 7.3 (1.8) | 0.16 (0.28) | Yes | Yes | No | No |
| MSEL ELC | 78.6 (24.2) | 66.3 (15.3) | 0.60 (0.29) | Yes | Yes | No | No | |
| VABS Composite | 68.7 (15.9) | 59.1 (8.8) | 0.73 (0.29) | Yes | Yes | Yes | Yes | |
| Repetitive Behavior Scale | 16.7 (13.1) | 22.0 (16.3) | 0.35 (0.29) | Yes | Yes | Yes | Yes | |
| Rogers (2012) [26] | ADOS Modified Social Affect | 26.6 (10.1) | 27.3 (10.6) | 0.07 (0.20) | Yes | Yes | No | No |
| MSEL DQ | 69.8 (17.9) | 67.9 (17.9) | 0.11 (0.20) | Yes | Yes | No | No | |
| MCDI: Phrases Understood | 12.7 (9.11) | 14.8 (8.1) | −0.23 (0.20) | Yes | Yes | Yes | Yes | |
| MCDI: Vocabulary Comprehension | 106.5 (96.8) | 125.7 (106.4) | −0.19 (0.20) | Yes | Yes | Yes | Yes | |
| MCDI: Vocabulary Produced | 42.3 (62.0) | 38.9 (73.7) | 0.05 (0.20) | Yes | Yes | Yes | Yes | |
| MCDI: Total Gestures | 28.02 (12.6) | 29.8 (13.5) | −0.13 (0.20) | Yes | Yes | Yes | Yes | |
| VABS Composite | 77.4 (9.6) | 80.3 (11.3) | −0.27 (0.20) | Yes | Yes | Yes | Yes | |
| ADOS RRB | 4.0 (1.9) | 3.8 (2.0) | −0.07 (0.20) | Yes | Yes | No | No | |
| Imitative Sequence | 4.6 (3.5) | 3.8 (3.4) | 0.24 (0.20) | No | Yes | No | No | |
| Mean Social Orienting | 0.5 (0.3) | 0.4 (0.4) | 0.13 (0.20) | No | Yes | No | No | |
| Mean Non-Social Orienting | 0.7 (0.3) | 0.6 (0.4) | 0.42 (0.20) | No | Yes | No | No | |
| Mean orient to Joint Attention | 0.3 (0.3) | 0.3 (0.3) | 0.00 (0.20) | No | Yes | No | No | |
| Rogers (2014) [13] | ADOS ASD severity | 3.3 (3.4) | 6.3 (3.9) | 0.75 (0.59) | Yes | Yes | No | No |
| MSEL Language | 92.4 (29.5) | 45.6 (20.3) | 1.60 (0.67) | Yes | Yes | No | No | |
| MSEL Visual reception | 96.1 (16.4) | 78.7 (9.3) | 1.10 (0.62) | Yes | Yes | No | No | |
| Vivanti (2014) [23] | ADOS ASD Severity | 6.9 (2.3) | 6.1 (1.6) | −0.37 (0.26) | Yes | Yes | No | No |
| MSEL DQ | 67.2 (20.2) | 56.3 (22.5) | 0.50 (0.27) | Yes | Yes | No | No | |
| VABS Composite | 72.1 (13.5) | 73.0 (15.5) | −0.06 (0.26) | Yes | Yes | Yes | Yes | |
| Fox (2018) [21] | MCDI: Vocabulary Produced | 164.4 (188.2) | 124.2 (140.7) | 0.22 (0.57) | Yes | Yes | Yes | Yes |
| Zhou (2018) [22] | ADOS ASD Severity | 6.3 (1.3) | 6.6 (1.1) | 0.23 (0.30) | Yes | Yes | No | No |
| CSBS Total | 40.9 (8.1) | 29.1 (10.3) | 1.27 (0.33) | Yes | Yes | Yes | Yes | |
| GDS Language | 68.6 (22.1) | 37.7 (22.5) | 1.36 (0.33) | Yes | Yes | No | No | |
| GDS Motor | 80.3 (15.1) | 71.7 (13.3) | 0.59 (0.31) | Yes | Yes | No | No | |
| GDS Personal-Social | 74.5 (10.6) | 51.0 (10.8) | 2.16 (0.38) | Yes | Yes | No | No | |
| GDS Eye-hand | 76.0 (13.3) | 56.1 (12.4) | 1.52 (0.34) | Yes | Yes | No | No | |
| GDS Performance | 75.2 (10.3) | 58.9 (15.1) | 1.25 (0.33) | Yes | Yes | No | No | |
| Xu (2018) [27] | ASD CARS severity | 30.4 (5.5) | 37.3 (6.7) | 1.09 (0.35) | Yes | Yes | No | No |
| Colombi (2018) [28] | GDS Total | 0.37 (0.24) | Yes | Yes | No | No | ||
| VABS Composite | 0.28 (0.24) | Yes | Yes | Yes | No | |||
| Vinen (2018) [24] | ADOS ASD Severity | 8.0 (2.6) | 7.8 (2.1) | −0.09 (0.26) | Yes | Yes | No | No |
| WASI FSIQ | 76.1 (20.8) | 82.8 (18.5) | −0.34 (0.24) | Yes | Yes | No | No | |
| Vismara (2018) [29] | Imitation | 1.4 (1.0) | 0.9 (0.8) | 0.48 (0.41) | No | No | Yes | Yes |
| Holzinger (2019) [30] | PDDBI | 41.7 (13.1) | 40.0 (10.7) | −0.13 (0.47) | Yes | Yes | Yes | No |
| Austrian CDI | 324.7 (201.9) | 193.8 (229.5) | 0.57 (0.48) | Yes | Yes | Yes | No | |
| MSEL DQ | 63.5 (20.2) | 50.0 (19.5) | 0.64 (0.49) | Yes | Yes | No | No | |
| VABS Daily Living | 81.9 (17.4) | 85.4 (13.5) | −0.21 (0.47) | Yes | Yes | Yes | No | |
| Rogers (2019) [31] | ADOS ASD severity | 6.7 (2.0) | 6.2 (2.5) | −0.22 (0.18) | Yes | Yes | No | No |
| Response to joint attention | 76.1 (26.9) | 70.7 (36.6) | 0.17 (0.18) | No | Yes | No | No | |
| MSEL DQ | 83.1 (26.1) | 79.1 (25.6) | 0.15 (0.18) | Yes | Yes | No | No | |
| VABS Composite | 39.8 (12.1) | 36.7 (14.3) | 0.23 (0.18) | Yes | Yes | Yes | Yes |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fuller, E.A.; Oliver, K.; Vejnoska, S.F.; Rogers, S.J. The Effects of the Early Start Denver Model for Children with Autism Spectrum Disorder: A Meta-Analysis. Brain Sci. 2020, 10, 368. https://doi.org/10.3390/brainsci10060368
Fuller EA, Oliver K, Vejnoska SF, Rogers SJ. The Effects of the Early Start Denver Model for Children with Autism Spectrum Disorder: A Meta-Analysis. Brain Sciences. 2020; 10(6):368. https://doi.org/10.3390/brainsci10060368
Chicago/Turabian StyleFuller, Elizabeth A., Kelsey Oliver, Sarah F. Vejnoska, and Sally J. Rogers. 2020. "The Effects of the Early Start Denver Model for Children with Autism Spectrum Disorder: A Meta-Analysis" Brain Sciences 10, no. 6: 368. https://doi.org/10.3390/brainsci10060368
APA StyleFuller, E. A., Oliver, K., Vejnoska, S. F., & Rogers, S. J. (2020). The Effects of the Early Start Denver Model for Children with Autism Spectrum Disorder: A Meta-Analysis. Brain Sciences, 10(6), 368. https://doi.org/10.3390/brainsci10060368





