Correlation between Myocardial Function and Electric Current Pulsatility of the Sputnik Left Ventricular Assist Device: In-Vitro Study
Abstract
1. Introduction
2. Materials and Methods
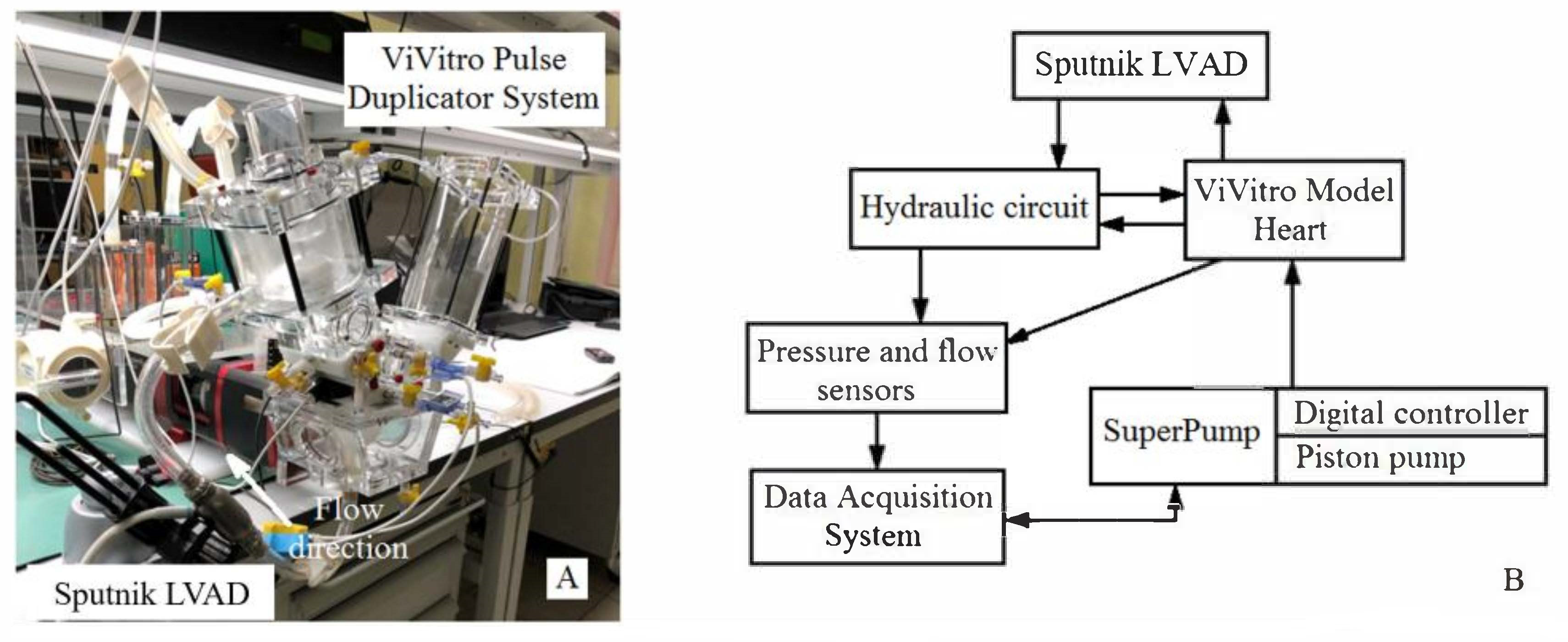
2.1. Experimental Setup and Device Description
2.2. Investigated Parameters
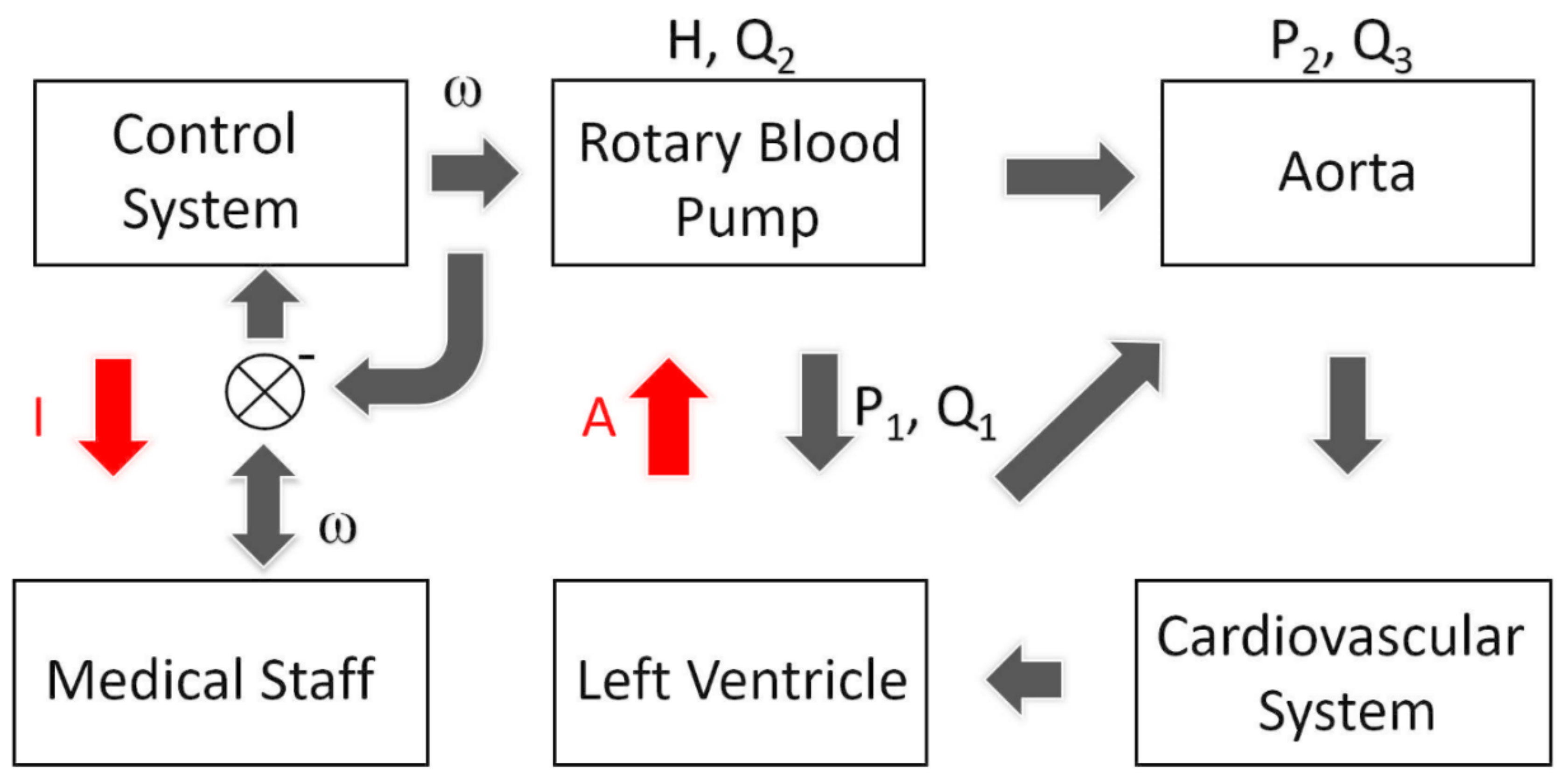
2.3. Correlation between CVS and Pump Parameters
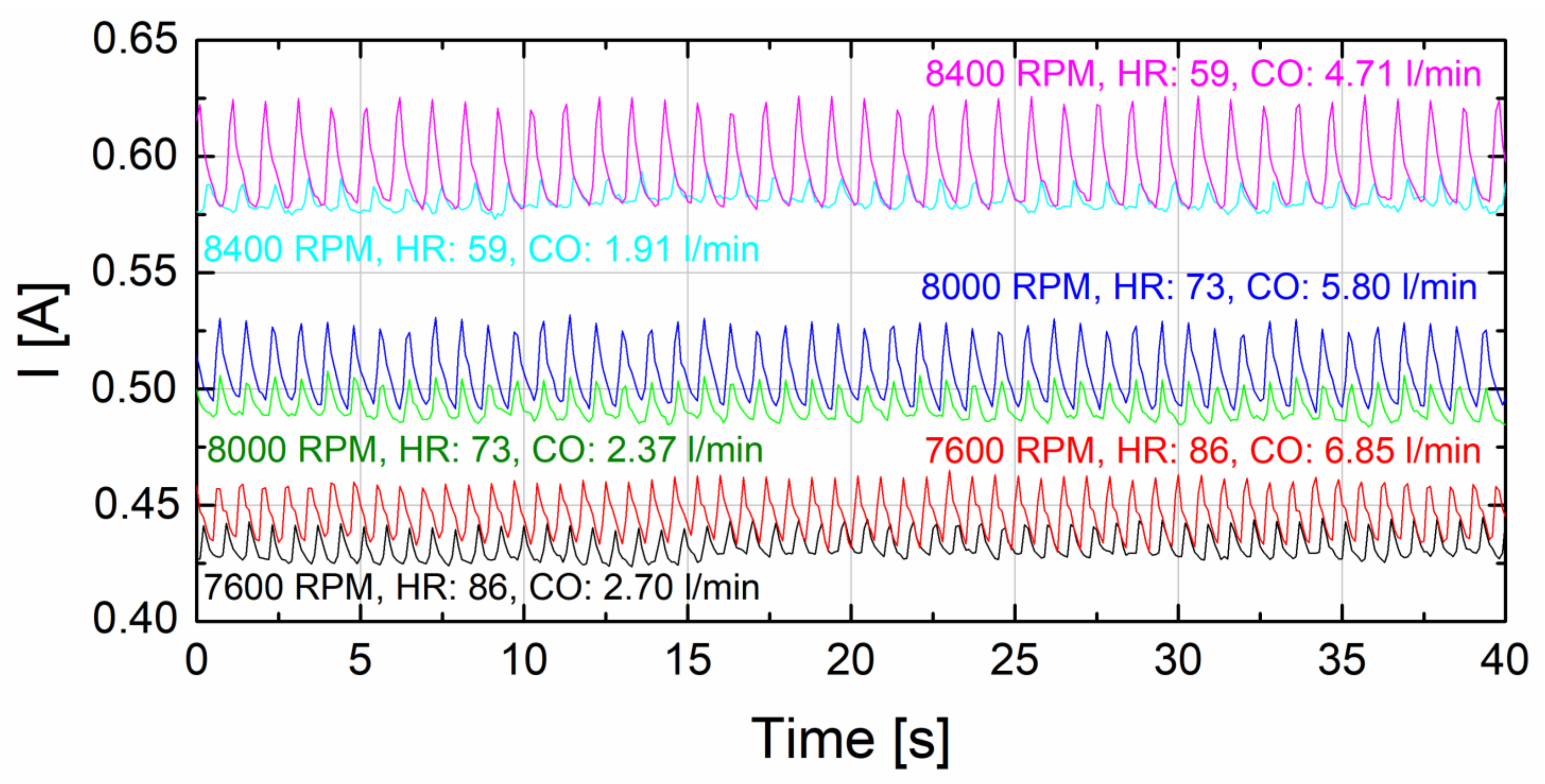
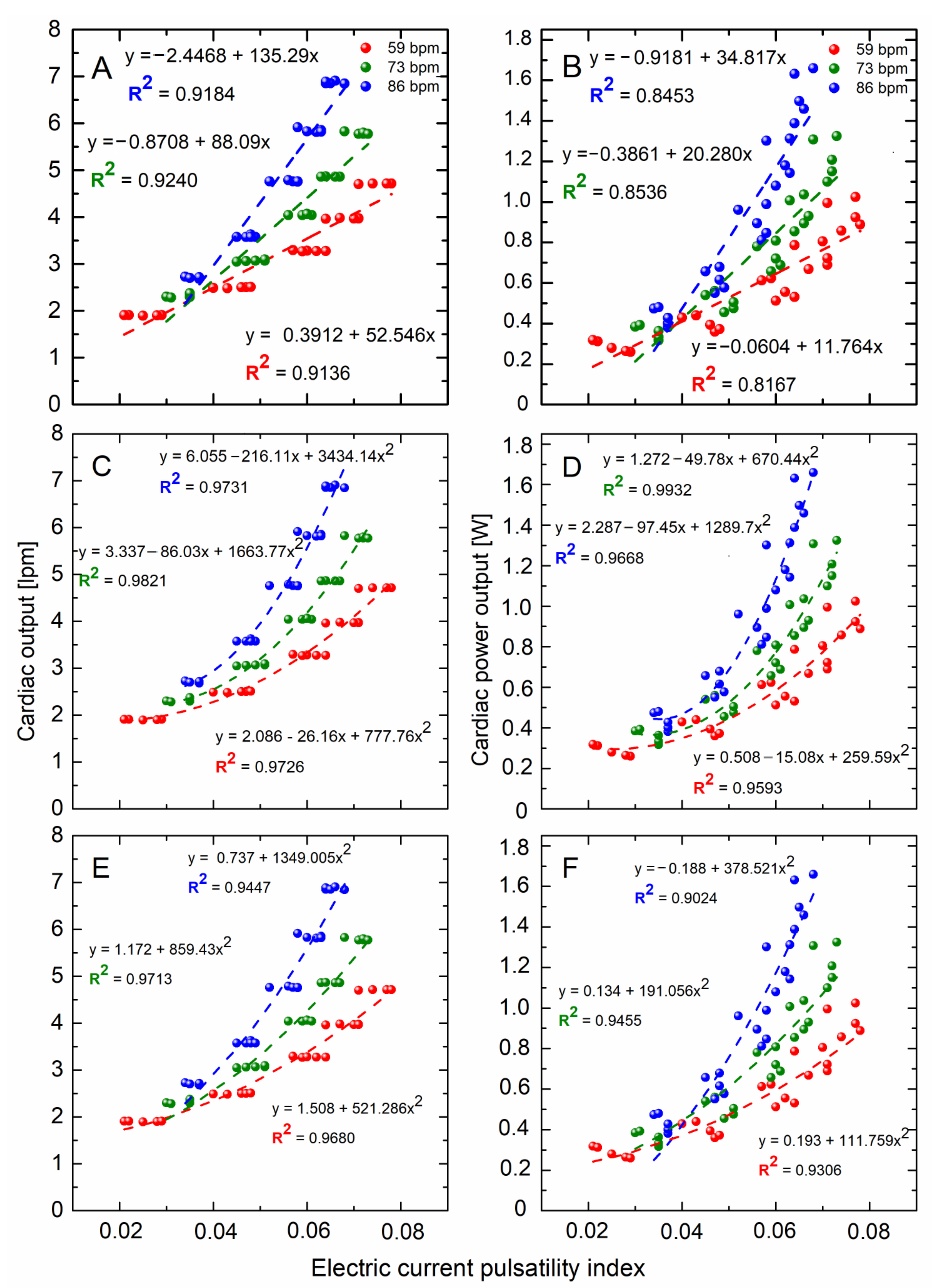
3. Results
4. Discussion
4.1. Applicability for Physiological Pump Control
4.2. Study limitations
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Kirklin, J.K.; Pagani, F.D.; Kormos, R.L.; Stevenson, L.W.; Blume, E.D.; Myers, S.L.; Miller, M.A.; Baldwin, J.T.; Young, J.B.; Naftel, D.C. Eighth annual INTERMACS report: Special focus on framing the impact of adverse events. J. Heart Lung Transplant. 2017, 36, 1080–1086. [Google Scholar] [CrossRef] [PubMed]
- Kado, Y.; Miyamoto, T.; Fukamachi, K.; Karimov, J.H. Update on the management and associated challenges of adult patients treated with veno-arterial extracorporeal membrane oxygenation. Expert Rev. Med. Devices 2019, 16, 483–491. [Google Scholar] [CrossRef]
- Topkara, V.K.; Garan, A.R.; Fine, B.; Godier-Furnémont, A.F.; Breskin, A.; Cagliostro, B.; Yuzefpolskaya, M.; Takeda, K.; Takayama, H.; Mancini, D.M.; et al. Myocardial Recovery in Patients Receiving Contemporary Left Ventricular Assist Devices. Circ. Heart Fail. 2016, 9, e003157. [Google Scholar] [CrossRef] [PubMed]
- Frazier, O.H.; Baldwin, A.C.W.; Demirozu, Z.T.; Segura, A.M.; Hernandez, R.; Taegtmeyer, H.; Mallidi, H.; Cohn, W.E. Ventricular reconditioning and pump explantation in patients supported by continuous-flow left ventricular assist devices. J. Heart Lung Transplant. 2015, 34, 766–772. [Google Scholar] [CrossRef]
- Knierim, J.; Heck, R.; Pieri, M.; Schoenrath, F.; Soltani, S.; Stawowy, P.; Dreysse, S.; Stein, J.; Müller, M.; Mulzer, J.; et al. Outcomes from a recovery protocol for patients with continuous-flow left ventricular assist devices. J. Heart Lung Transplant. 2019, 38, 440–448. [Google Scholar] [CrossRef] [PubMed]
- Moscato, F.; Schima, H. Mechanical Circulatory Support in End-Stage Heart Failure; Montalto, A., Loforte, A., Musumeci, F., Krabatsch, T., Slaughter, M.S., Eds.; Springer International Publishing: Cham, Switzerland, 2017; ISBN 978-3-319-43381-3. [Google Scholar]
- Swetz, K.M.; Freeman, M.R.; Mueller, P.S.; Park, S.J. Clinical management of continuous-flow left ventricular assist devices in advanced heart failure. J. Heart Lung Transplant. 2010, 29, 1081. [Google Scholar] [CrossRef] [PubMed]
- Jakovljevic, D.G.; Yacoub, M.H.; Schueler, S.; MacGowan, G.A.; Velicki, L.; Seferovic, P.M.; Hothi, S.; Tzeng, B.-H.; Brodie, D.A.; Birks, E.; et al. Left Ventricular Assist Device as a Bridge to Recovery for Patients with Advanced Heart Failure. J. Am. Coll. Cardiol. 2017, 69, 1924–1933. [Google Scholar] [CrossRef] [PubMed]
- Hall, S.G.; Garcia, J.; Larson, D.F.; Smith, R. Cardiac power index: Staging heart failure for mechanical circulatory support. Perfusion 2012, 27, 456–461. [Google Scholar] [CrossRef] [PubMed]
- Teuteberg, J.J.; Cleveland, J.C.; Cowger, J.; Higgins, R.S.; Goldstein, D.J.; Keebler, M.; Kirklin, J.K.; Myers, S.L.; Salerno, C.T.; Stehlik, J.; et al. The Society of Thoracic Surgeons Intermacs 2019 Annual Report: The Changing Landscape of Devices and Indications. Ann. Thorac. Surg. 2020, 109, 649–660. [Google Scholar] [CrossRef]
- Naiyanetr, P.; Moscato, F.; Vollkron, M.; Zimpfer, D.; Wieselthaler, G.; Schima, H. Continuous assessment of cardiac function during rotary blood pump support: A contractility index derived from pump flow. J. Heart Lung Transplant. 2010, 29, 37–44. [Google Scholar] [CrossRef]
- Salamonsen, R.F.; Lim, E.; Gaddum, N.; AlOmari, A.-H.H.; Gregory, S.D.; Stevens, M.; Mason, D.G.; Fraser, J.F.; Timms, D.; Karunanithi, M.K.; et al. Theoretical Foundations of a Starling-Like Controller for Rotary Blood Pumps. Artif. Organs 2012, 36, 787–796. [Google Scholar] [CrossRef]
- Endo, G.; Araki, K.; Oshikawa, M.; Kojima, K.; Nakamura, K.; Matsuzaki, Y.; Onitsuka, T. A Safe Automatic Driving Method for a Continuous Flow Ventricular Assist Device Based on Motor Current Pulsatility:In Vitro Evaluation. ASAIO J. 2002, 48, 83–89. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.; Boston, J.R.; Antaki, J.F. Hemodynamic Controller for Left Ventricular Assist Device Based on Pulsatility Ratio. Artif. Organs 2007, 31, 114–125. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.; Boston, J.R.; Antaki, J.F. An investigation of the pump operating characteristics as a novel control index for LVAD control. Int. J. Control. Autom. Syst. 2005, 3, 100–108. [Google Scholar]
- Choi, S.; Antaki, J.E.; Boston, R.; Thomas, D. A sensorless approach to control of a turbodynamic left ventricular assist system. IEEE Trans. Control Syst. Technol. 2001, 9, 473–482. [Google Scholar] [CrossRef]
- Slaughter, M.S.; Pagani, F.D.; Rogers, J.G.; Miller, L.W.; Sun, B.; Russell, S.D.; Starling, R.C.; Chen, L.; Boyle, A.J.; Chillcott, S.; et al. Clinical management of continuous-flow left ventricular assist devices in advanced heart failure. J. Heart Lung Transplant. 2010, 29, S1–S39. [Google Scholar] [CrossRef] [PubMed]
- Cotter, G.; Williams, S.G.; Vered, Z.; Tan, L.B. Role of cardiac power in heart failure. Curr. Opin. Cardiol. 2003, 18, 215–222. [Google Scholar] [CrossRef] [PubMed]
- Mendoza, D.D.; Cooper, H.A.; Panza, J.A. Cardiac power output predicts mortality across a broad spectrum of patients with acute cardiac disease. Am. Heart J. 2007, 153, 366–370. [Google Scholar] [CrossRef] [PubMed]
- Jakovljevic, D.G.; George, R.S.; Donovan, G.; Nunan, D.; Henderson, K.; Bougard, R.S.; Yacoub, M.H.; Birks, E.J.; Brodie, D.A. Comparison of Cardiac Power Output and Exercise Performance in Patients with Left Ventricular Assist Devices, Explanted (Recovered) Patients, and Those With Moderate to Severe Heart Failure. Am. J. Cardiol. 2010, 105, 1780–1785. [Google Scholar] [CrossRef]
- Chiu, W.-C.; Girdhar, G.; Xenos, M.; Alemu, Y.; Soares, J.S.; Einav, S.; Slepian, M.; Bluestein, D. Thromboresistance Comparison of the HeartMate II Ventricular Assist Device with the Device Thrombogenicity Emulation-Optimized Heart Assist 5 VAD. J. Biomech. Eng. 2014, 136, 021014. [Google Scholar] [CrossRef]
- Meaney, E. Formula and nomogram for the sphygmomanometric calculation of the mean arterial pressure. Heart 2000, 84, 64. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.R.; Jorde, U.P. Creating adequate pulsatility with a continuous flow left ventricular assist device. Curr. Opin. Cardiol. 2016, 31, 329–336. [Google Scholar] [CrossRef] [PubMed]
- Rangasamy, S.; Madan, S.; Saeed, O.; Goldstein, D.J.; Jorde, U.P.; Negassa, A.; Patel, S.R. Noninvasive Measures of Pulsatility and Blood Pressure During Continuous-Flow Left Ventricular Assist Device Support. ASAIO J. 2019, 65, 241–246. [Google Scholar] [CrossRef] [PubMed]
- Gupta, S.; Muthiah, K.; Woldendorp, K.; Robson, D.; Jansz, P.; Hayward, C.S. Derivation of indices of left ventricular contractility in the setting of continuous-flow left ventricular assist device support. Artif. Organs 2014, 38, 1029–1034. [Google Scholar] [CrossRef] [PubMed]
- Yokoyama, Y.; Kawaguchi, O.; Kitao, T.; Kimura, T.; Steinseifer, U.; Takatani, S. Prediction of the external work of the native heart from the dynamic H-Q curves of the rotary blood pumps during left heart bypass. Artif. Organs 2010, 34, 766–777. [Google Scholar] [CrossRef]
- Pugovkin, A.A.; Markov, A.G.; Selishchev, S.V.; Korn, L.; Walter, M.; Leonhardt, S.; Bockeria, L.A.; Bockeria, O.L.; Telyshev, D.V. Advances in Hemodynamic Analysis in Cardiovascular Diseases Investigation of Energetic Characteristics of Adult and Pediatric Sputnik Left Ventricular Assist Devices during Mock Circulation Support. Cardiol. Res. Pract. 2019, 2019, 1–15. [Google Scholar] [CrossRef]
- Hetzer, R.; Müller, J.; Weng, Y.; Wallukat, G.; Spiegelsberger, S.; Loebe, M. Cardiac recovery in dilated cardiomyopathy by unloading with a left ventricular assist device. Ann. Thorac. Surg. 1999, 68, 742–749. [Google Scholar] [CrossRef]
- Burkhoff, D.; Klotz, S.; Mancini, D.M. LVAD-Induced Reverse Remodeling: Basic and Clinical Implications for Myocardial Recovery. J. Card. Fail. 2006, 12, 227–239. [Google Scholar] [CrossRef]
- Karantonis, D.M.; Lovell, N.H.; Ayre, P.J.; Mason, D.G.; Cloherty, S.L. Identification and Classification of Physiologically Significant Pumping States in an Implantable Rotary Blood Pump. Artif. Organs 2006, 30, 671–679. [Google Scholar] [CrossRef]
- Granegger, M.; Masetti, M.; Laohasurayodhin, R.; Schloeglhofer, T.; Zimpfer, D.; Schima, H.; Moscato, F. Continuous Monitoring of Aortic Valve Opening in Rotary Blood Pump Patients. IEEE Trans. Biomed. Eng. 2016, 63, 1201–1207. [Google Scholar] [CrossRef]
- Vollkron, M.; Schima, H.; Huber, L.; Benkowski, R.; Morello, G.; Wieselthaler, G. Development of a suction detection system for axial blood pumps. Artif. Organs 2004, 28, 709–716. [Google Scholar] [CrossRef]
- Karantonis, D.M.; Lim, E.; Mason, D.G.; Salamonsen, R.F.; Ayre, P.J.; Lovell, N.H. Noninvasive Activity-based Control of an Implantable Rotary Blood Pump: Comparative Software Simulation Study. Artif. Organs 2010, 34, E34–E45. [Google Scholar] [CrossRef]
- Meki, M.; Wang, Y.; Sethu, P.; Ghazal, M.; El-Baz, A.; Giridharan, G. A Sensorless Rotational Speed-Based Control System for Continuous Flow Left Ventricular Assist Devices. IEEE Trans. Biomed. Eng. 2020, 67, 1050–1060. [Google Scholar] [CrossRef] [PubMed]
- Ferrari, M.; Kruzliak, P.; Spiliopoulos, K. An insight into short- and long-term mechanical circulatory support systems. Clin. Res. Cardiol. 2014, 104, 95–111. [Google Scholar] [CrossRef]
- Giridharan, G.A.; Skliar, M. Physiological Control of Blood Pumps Using Intrinsic Pump Parameters: A Computer Simulation Study. Artif. Organs 2006, 30, 301–307. [Google Scholar] [CrossRef]
- Pennings, K.A.M.A.; Martina, J.R.; Rodermans, B.F.M.; Lahpor, J.R.; Van De Vosse, F.N.; De Mol, B.A.J.M.; Rutten, M.C.M. Pump flow estimation from pressure head and power uptake for the heartassist5, heartmate II, and heartware vads. ASAIO J. 2013, 59, 420–426. [Google Scholar] [CrossRef]
- Ayre, P.J.; Lovell, N.H.; Woodard, J.C. Non-invasive flow estimation in an implantable rotary blood pump: A study considering non-pulsatile and pulsatile flows. Physiol. Meas. 2003, 24, 179–189. [Google Scholar] [CrossRef] [PubMed]
- Malagutti, N.; Karantonis, D.M.; Cloherty, S.L.; Ayre, P.J.; Mason, D.G.; Salamonsen, R.F.; Lovell, N.H. Noninvasive Average Flow Estimation for an Implantable Rotary Blood Pump: A New Algorithm Incorporating the Role of Blood Viscosity. Artif. Organs 2007, 31, 45–52. [Google Scholar] [CrossRef]
- Wakisaka, Y.; Okuzono, Y.; Taenaka, Y.; Chikanari, K.; Masuzawa, T.; Takano, H. Establishment of flow estimation for an implantable centrifugal blood pump. ASAIO J. 1997, 43, M659–M662. [Google Scholar] [CrossRef] [PubMed]
- Boës, S.; Thamsen, B.; Haas, M.; Daners, M.S.; Meboldt, M.; Granegger, M. Hydraulic Characterization of Implantable Rotary Blood Pumps. IEEE Trans. Biomed. Eng. 2019, 66, 1618–1927. [Google Scholar] [CrossRef]
- Pauls, J.P.; Stevens, M.C.; Bartnikowski, N.; Fraser, J.F.; Gregory, S.D.; Tansley, G. Evaluation of Physiological Control Systems for Rotary Left Ventricular Assist Devices: An In-Vitro Study. Ann. Biomed. Eng. 2016, 44, 2377–2387. [Google Scholar] [CrossRef]
- Wu, Y. Adaptive Physiological Speed/Flow Control of Rotary Blood Pumps in Permanent Implantation Using Intrinsic Pump Parameters. ASAIO J. 2009, 55, 335–339. [Google Scholar] [CrossRef]
- Telyshev, D.; Denisov, M.; Pugovkin, A.; Selishchev, S.; Nesterenko, I. The Progress in the Novel Pediatric Rotary Blood Pump Sputnik Development. Artif. Organs 2018, 42, 432–443. [Google Scholar] [CrossRef] [PubMed]
- Telyshev, D.; Denisov, M.; Markov, A.; Fresiello, L.; Verbelen, T.; Selishchev, S. Energetics of blood flow in Fontan circulation under VAD support. Artif. Organs 2020, 44, 50–57. [Google Scholar] [CrossRef] [PubMed]
- Porfiryev, A.; Markov, A.; Galyastov, A.; Denisov, M.; Burdukova, O.; Gerasimenko, A.Y.; Telyshev, D. Fontan Hemodynamics Investigation via Modeling and Experimental Characterization of Idealized Pediatric Total Cavopulmonary Connection. Appl. Sci. 2020, 10, 6910. [Google Scholar] [CrossRef]
- Rubtsova, E.; Markov, A.; Selishchev, S.; Karimov, J.H.; Telyshev, D. Mathematical modeling of the Fontan blood circulation supported with pediatric ventricular assist device. Comput. Methods Biomech. Biomed. Eng. 2021, 1–10. [Google Scholar] [CrossRef]
- Nguyen, D.Q.; Thourani, V.H. Third-Generation Continuous Flow Left Ventricular Assist Devices. Innovations 2010, 5, 250–258. [Google Scholar] [CrossRef]
- Loree, H.M.; Bourque, K.; Gernes, D.B.; Scott Richardson, J.; Poirier, V.L.; Barletta, N.; Fleischli, A.; Foiera, G.; Gempp, T.M.; Schoeb, R.; et al. The HeartMate III: Design and in vivo studies of a Maglev centrifugal left ventricular assist device. Artif. Organs 2001, 25, 386–391. [Google Scholar] [CrossRef]
- Pagani, F.D. Continuous-Flow Rotary Left Ventricular Assist Devices with “3rd Generation” Design. Semin. Thorac. Cardiovasc. Surg. 2008, 20, 255–263. [Google Scholar] [CrossRef] [PubMed]
- Tansley, G.; Vidakovic, S.; Reizes, J. Fluid dynamic characteristics of the VentrAssist rotary blood pump. Artif. Organs 2000, 24, 483–487. [Google Scholar] [CrossRef]
- Telyshev, D.V. A Mathematical Model for Estimating Physiological Parameters of Blood Flow through Rotary Blood Pumps. Biomed. Eng. 2020, 54, 163–168. [Google Scholar] [CrossRef]
- Masuzawa, T.; Osa, M.; Mapley, M. Motor design and impeller suspension. In Mechanical Circulatory and Respiratory Support; Gregory, S.D., Stevens, M.C., Fraser, J.F., Eds.; Academic Press: London, UK, 2018; pp. 335–377. ISBN 9780128104910. [Google Scholar]
- Boës, S. Hydraulic Characteristics and Flow-Field Related Hemocompatibility of Rotary Blood Pump Designs; ETH Zurich: Zürich, Switzerland, 2018. [Google Scholar]
- Smith, P.A.; Wang, Y.; Groß-Hardt, S.; Graefe, R. Hydraulic design. In Mechanical Crculatory and Respiratory Support; Gregory, S.D., Stevens, M.C., Fraser, J.F., Eds.; Academic Press: London, UK, 2018; pp. 301–334. ISBN 978-0-12-810491-0. [Google Scholar]
- Selishchev, S.V.; Telyshev, D.V. Optimisation of the sputnik-VAD design. Int. J. Artif. Organs 2016, 39, 407–414. [Google Scholar] [CrossRef] [PubMed]
- Selishchev, S.V.; Telyshev, D.V. Ventricular assist device sputnik: Description, technical features and characteristics. Trends Biomater. Artif. Organs 2015, 29, 207–210. [Google Scholar]
- Gautier, S.V.; Shevchenko, A.O.; Itkin, G.P.; Zakharevich, V.M.; Poptsov, V.N.; Drobyshev, A.A.; Telyshev, D.V. Artificial heart in Russia: Past, present, and future. Artif. Organs 2020, 53, aor.13860. [Google Scholar]
| Response | HR, bpm | Regression Equation | Term | Estimate | SE | p-Value |
|---|---|---|---|---|---|---|
| CO | 59 | 0.39 | 0.19 | 0.0514 | ||
| 52.6 | 3.3 | 6.20 × 10−14 | ||||
| F-test vs. constant | 255 | 6.20 × 10−14 | ||||
| 2.1 | 0.3 | 2.10 × 10−07 | ||||
| −26.2 | 12.1 | 0.043 | ||||
| 777.8 | 120.3 | 2.09 × 10−06 | ||||
| F-test vs. constant | 410 | 1.51 × 10−17 | ||||
| 1.51 | 0.07 | 9.34 × 10−16 | ||||
| 521.3 | 19.7 | 3.67 × 10−18 | ||||
| F-test vs. constant | 698 | 3.67 × 10−18 | ||||
| Pearson’s r | 0.9577 | 6.20 × 10−14 | ||||
| Spearman’s ρ | 0.9720 | 5.75 × 10−16 | ||||
| 73 | −0.9 | 0.3 | 0.007 | |||
| 88.09 | 5.15 | 1.41 × 10−14 | ||||
| F-test vs. constant | 293 | 1.41 × 10−14 | ||||
| 3.3 | 0.5 | 3.99 × 10−06 | ||||
| −86.0 | 21.9 | 0.0008 | ||||
| 1663.8 | 210.6 | 1.01 × 10−07 | ||||
| F-test vs. constant | 635 | 1.65 × 10−19 | ||||
| 1.17 | 0.11 | 9.21 × 10−10 | ||||
| 859.43 | 31.45 | 6.75 × 10−18 | ||||
| F-test vs. constant | 747 | 6.75 × 10−18 | ||||
| Pearson’s r | 0.9629 | 1.41 × 10−14 | ||||
| Spearman’s ρ | 0.9716 | 6.84 × 10−16 | ||||
| 86 | −2.45 | 0.45 | 1.41 × 10−05 | |||
| 135.3 | 8.2 | 3.17 × 10−14 | ||||
| F-test vs. constant | 271 | 3.17 × 10−14 | ||||
| 6.1 | 1.4 | 0.0004 | ||||
| −216.11 | 58.03 | 0.0014 | ||||
| 3434.1 | 571.5 | 8.81 × 10−06 | ||||
| F-test vs. constant | 382 | 4.59 × 10−16 | ||||
| 0.7 | 0.2 | 0.003 | ||||
| 1349.0 | 69.6 | 6.98 × 10−15 | ||||
| F-test vs. constant | 376 | 6.98 × 10−15 | ||||
| Pearson’s r | 0.9601 | 3.17 × 10−14 | ||||
| Spearman’s ρ | 0.9484 | 5.83 × 10−13 | ||||
| Response | HR, bpm | Regression Equation | Term | Estimate | SE | p-Value |
|---|---|---|---|---|---|---|
| CPO | 59 | −0.06 | 0.07 | 0.37 | ||
| 11.76 | 1.13 | 3.69 × 10−10 | ||||
| F-test vs. constant | 108 | 3.69 × 10−10 | ||||
| 0.51 | 0.08 | 1.43 × 10−05 | ||||
| −15.1 | 3.8 | 0.001 | ||||
| 259.6 | 37.9 | 3.85 × 10−06 | ||||
| F-test vs. constant | 213 | 2.93 × 10−12 | ||||
| 0.19 | 0.03 | 1.01 × 10−05 | ||||
| 111.8 | 7.6 | 2.62 × 10−10 | ||||
| F-test vs. constant | 216 | 2.62 × 10−10 | ||||
| Pearson’s r | 0.9080 | 3.69 × 10−10 | ||||
| Spearman’s ρ | 0.9345 | 8.37 × 10−12 | ||||
| 73 | −0.4 | 0.1 | 0.0008 | |||
| 20.3 | 1.7 | 7.27 × 10−11 | ||||
| F-test vs. constant | 135 | 7.27 × 10−11 | ||||
| 1.27 | 0.09 | 1.93 × 10−09 | ||||
| −49.8 | 3.9 | 4.70 × 10−09 | ||||
| 670.4 | 38.4 | 6.72 × 10−11 | ||||
| F-test vs. constant | 1.17 × 103 | 2.61 × 10−16 | ||||
| 0.13 | 0.04 | 0.0023 | ||||
| 191.1 | 10.8 | 2.18 × 10−12 | ||||
| F-test vs. constant | 313 | 2.18 × 10−12 | ||||
| Pearson’s r | 0.9170 | 1.17 × 10−10 | ||||
| Spearman’s ρ | 0.9557 | 1.04 × 10−13 | ||||
| 86 | −0.92 | 0.16 | 1.11 × 10−05 | |||
| 34.82 | 3.03 | 5.20 × 10−11 | ||||
| F-test vs. constant | 132 | 5.20 × 10−11 | ||||
| 2.3 | 0.4 | 2.13 × 10−05 | ||||
| −97.5 | 16.8 | 1.32 × 10−05 | ||||
| 1289.7 | 164.9 | 2.35 × 10−07 | ||||
| F-test vs. constant | 307 | 3.44 × 10−15 | ||||
| −0.19 | 0.09 | 0.046 | ||||
| 378.5 | 27.1 | 8.88 × 10−12 | ||||
| F-test vs. constant | 195 | 8.88 × 10−12 | ||||
| Pearson’s r | 0.9229 | 5.20 × 10−11 | ||||
| Spearman’s ρ | 0.9574 | 6.68 × 10−14 | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Telyshev, D.V.; Pugovkin, A.A.; Ephimov, I.A.; Markov, A.; Leonhardt, S.; Walter, M.; Karimov, J.H.; Selishchev, S.V. Correlation between Myocardial Function and Electric Current Pulsatility of the Sputnik Left Ventricular Assist Device: In-Vitro Study. Appl. Sci. 2021, 11, 3359. https://doi.org/10.3390/app11083359
Telyshev DV, Pugovkin AA, Ephimov IA, Markov A, Leonhardt S, Walter M, Karimov JH, Selishchev SV. Correlation between Myocardial Function and Electric Current Pulsatility of the Sputnik Left Ventricular Assist Device: In-Vitro Study. Applied Sciences. 2021; 11(8):3359. https://doi.org/10.3390/app11083359
Chicago/Turabian StyleTelyshev, Dmitry V., Alexander A. Pugovkin, Ivan A. Ephimov, Aleksandr Markov, Steffen Leonhardt, Marian Walter, Jamshid H. Karimov, and Sergey V. Selishchev. 2021. "Correlation between Myocardial Function and Electric Current Pulsatility of the Sputnik Left Ventricular Assist Device: In-Vitro Study" Applied Sciences 11, no. 8: 3359. https://doi.org/10.3390/app11083359
APA StyleTelyshev, D. V., Pugovkin, A. A., Ephimov, I. A., Markov, A., Leonhardt, S., Walter, M., Karimov, J. H., & Selishchev, S. V. (2021). Correlation between Myocardial Function and Electric Current Pulsatility of the Sputnik Left Ventricular Assist Device: In-Vitro Study. Applied Sciences, 11(8), 3359. https://doi.org/10.3390/app11083359








