Management of Patients under Treatment with Monoclonal Antibodies and New Biological Therapies
Abstract
:1. Introduction
- -
- Previous or current treatment with antiresorptive or antiangiogenic agents.
- -
- Exposed bone or bone that can be probed through an intra- or extra-oral fistula in the maxillofacial region, which has persisted for more than 8 weeks.
- -
- Absence of radiotherapy or previous metastasis in the jaw [2].
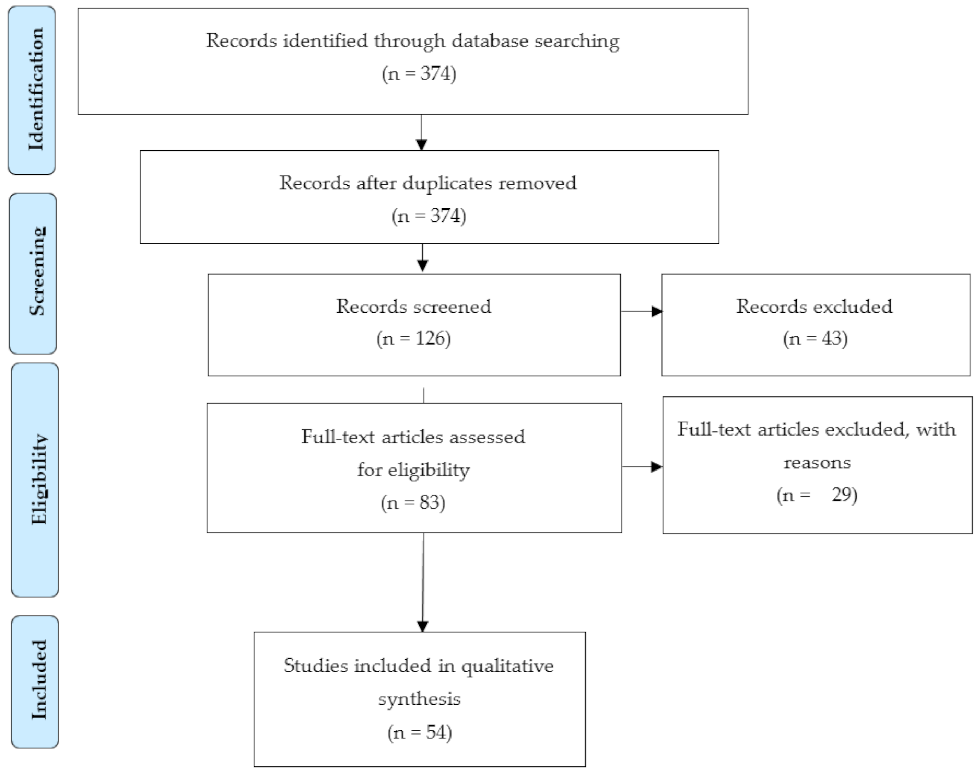
2. Material and Methods
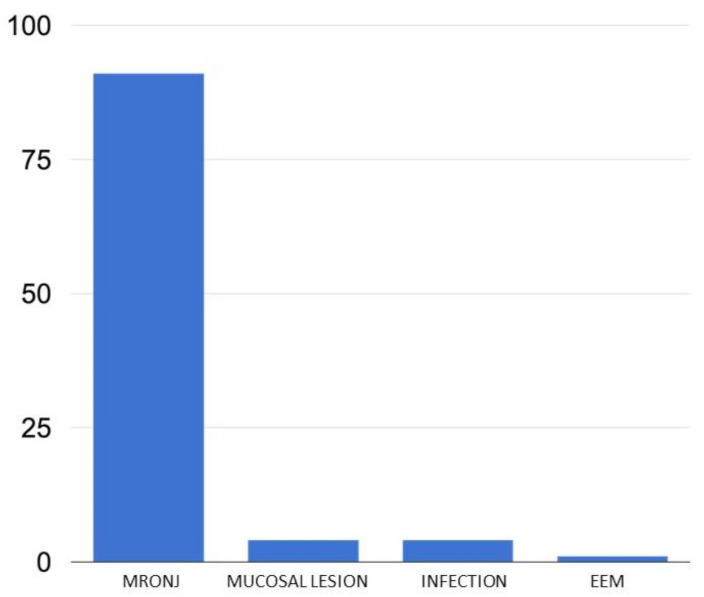
3. Results
4. Discussion
4.1. Management of Patients Undergoing Treatment with Biological Therapies
4.2. Management of Complications Associated with Biological Therapies
4.3. Study Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Radfar, L.; Ahmadabadi, R.E.; Masood, F.; Scofield, R.H. Biological therapy and dentistry: A review paper. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2015, 120, 594–601. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ruggiero, S.L.; Dodson, T.B.; Fantasia, J.; Goodday, R.; Aghaloo, T.; Mehrotra, B.; O’Ryan, F. American Association of Oral and Maxillofacial Surgeons Position Paper on Medication-Related Osteonecrosis of the Jaw—2014 Update. J. Oral Maxillofac. Surg. 2014, 72, 1938–1956. [Google Scholar] [CrossRef]
- Yarom, N.; Shapiro, C.L.; Peterson, D.E.; Van Poznak, C.H.; Bohlke, K.; Ruggiero, S.L.; O’Ryan, F. Medication-Related Osteonecrosis of the Jaw: MASCC/ISOO/ASCO Clinical Practice Guideline. J. Clin. Oncol. 2019, 37, 2270–2290. [Google Scholar] [CrossRef]
- Vigarios, N.P.; Epstein, J.B.; Sibaud, V. Oral mucosal changes induced by anticancer targeted therapies and immune checkpoint inhibitors. Support Care Cancer 2017, 25, 1713–1739. [Google Scholar]
- Keribin, P.; Guerrot, D.; Jardin, F.; Moizan, H. Osteonecrosis of the Jaw in a Patient Presenting with Post-Transplantation Lymphoproliferative Disorder Treated With Rituximab: A Case Report. J. Oral Maxillofac. Surg. 2017, 75, 2599–2605. [Google Scholar] [CrossRef]
- Maluf, G.; Pinho, M.C.D.; Cunha, S.R.D.B.D.; Santos, P.S.D.S.; Fregnani, E.R. Surgery Combined with LPRF in Denosumab Osteonecrosis of the Jaw: Case Report. Braz. Dent. J. 2016, 27, 353–358. [Google Scholar] [CrossRef]
- Pichardo, S.E.C.; Kuypers, S.C.C.; van Merkesteyn, J.P.R. Denosumab osteonecrosis of the mandible: A new entity? A case report. J. Craniomaxillofac. Surg. 2013, 41, e65–e69. [Google Scholar] [CrossRef]
- Niibe, K.; Ouchi, T.; Iwasaki, R.; Nakagawa, T.; Horie, N. Osteonecrosis of the jaw in patients with dental prostheses being treated with bisphosphonates or denosumab. J. Prosthodont. Res. 2015, 59, 3–5. [Google Scholar] [CrossRef]
- Badr, M.; Kyriakidou, E.; Atkins, S.; Harrison, S. Aggressive denosumab-related jaw necrosis—A case series. Br. Dent. J. 2017, 223, 13–16. [Google Scholar] [CrossRef] [PubMed]
- Nifosi, A.F.; Nifosi, L.; Nifosi, G. Osteonecrosis of the Jaw in a patient treated with denosumab and temsirolimus. SAJ Case Rep. 2017, 4, 1–4. [Google Scholar]
- Allegra, A.; Oteri, G.; Alonci, A.; Bacci, F.; Penna, G.; Minardi, V.; Maisanoa, V.; Musolino, C. Association of osteonecrosis of the jaws and POEMS syndrome in a patient assuming rituximab. J. Craniomaxillofac. Surg. 2014, 42, 279–282. [Google Scholar] [CrossRef] [PubMed]
- Baur, D.A.; Weber, J.M.; Collette, D.C.; Dhaliwal, H.; Quereshy, F. Osteonecrosis of the Jaws Unrelated to Bisphosphonate Exposure: A Series of 4 Cases. J. Oral Maxillofac. Surg. 2012, 70, 2802–2808. [Google Scholar] [CrossRef]
- Javelot, M.-J.; Sergheraert, J.; Agbo-Godeau, S.; Levy-Weil, F.; Laurence, S.; Goudot, P.; Khonsarie, R.-H.; Mauprivezb, C. Rituximab as a trigger factor of medication-related osteonecrosis of the jaw. A case report. J. Stomatol. Oral Maxillofac. 2020, 121, 300–304. [Google Scholar] [CrossRef]
- Weigert, K.; Lewgoy, J.; Mazzoleni, D.S.; Franco, F.R.; Lisandra, E.; Henrique Sasso, J. Rituximab and osteonecrosis of the jaws: Case study. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2014, 117, e188–e189. [Google Scholar] [CrossRef]
- Manzie, T.; Vujcich, N.; Chan, A. Osteonecrosis of the jaw in an anti-resorptive naïve patient taking trastuzumab and pertuzumab: Case report. Aust. Dent. J. 2020, 65, 305–307. [Google Scholar] [CrossRef]
- Mauceri, R.; Panzarella, V.; Morreale, I.; Campisi, G. Medication-related osteonecrosis of the jaw in a cancer patient receiving lenvatinib. Int. J. Oral Maxillofac. Surg. 2019, 48, 1530–1532. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fleissig, Y.; Regev, E.; Lehman, H. Sunitinib related osteonecrosis of jaw: A case report. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2012, 113, e1–e3. [Google Scholar] [CrossRef] [PubMed]
- Brunello, A.; Saia, G.; Bedogni, A.; Scaglione, D.; Basso, U. Worsening of osteonecrosis of the jaw during treatment with sunitinib in a patient with metastatic renal cell carcinoma. Bone 2009, 44, 173–175. [Google Scholar] [CrossRef]
- Koch, F.P.; Walter, C.; Hansen, T.; Jäger, E.; Wagner, W. Osteonecrosis of the jaw related to sunitinib. Oral Maxillofac. Surg. 2011, 15, 63–66. [Google Scholar] [CrossRef] [PubMed]
- Melloni, C.; Tuttolomondo, A.; Anfosso, A.; Calamia, C.; Clemente, F.D.; Cordova, A. Sunitinib related osteonecrosis of the jaw (SURONJ): A rare occurrence? Eur. J. Plast. Surg. 2016, 39, 161–162. [Google Scholar] [CrossRef]
- Nicolatou-Galitis, O.; Schiødt, M.; Mendes, R.A.; Ripamonti, C.; Hope, S.; Drudge-Coates, L.; Niepel, D.; Van den Wyngaert, T. Medication-related osteonecrosis of the jaw: Definition and best practice for prevention, diagnosis, and treatment. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2019, 127, 117–135. [Google Scholar] [CrossRef] [Green Version]
- Agrillo, A.; Nastro Siniscalchi, E.; Facchini, A.; Filiaci, F.; Ungari, C. Osteonecrosis of the jaws in patients assuming bisphosphonates and sunitinib: Two case reports. Eur. Rev. Med. Pharmacol. Sci. 2012, 16, 952–957. [Google Scholar]
- Watters, A.L.; Epstein, J.B.; Agulnik, M. Oral complications of targeted cancer therapies: A narrative literature review. Oral Oncol. 2011, 47, 441–448. [Google Scholar] [CrossRef]
- Cillo, J.E.; Barbosa, N. Adalimumab-Related Dental Implant Infection. J. Oral Maxillofac. Surg. 2019, 77, 1165–1169. [Google Scholar] [CrossRef]
- Filler, S.G.; Yeaman, M.R.; Sheppard, D.C. Tumor Necrosis Factor Inhibition and Invasive Fungal Infections. Clin. Infect. Dis. 2005, 41, S208–S212. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Edwards, D.; Boritz, E.; Cowen, E.W.; Brown, R.S. Erythema multiforme major following treatment with infliximab. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2013, 115, e36–e40. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Estilo, C.L.; Fornier, M.; Farooki, A.; Carlson, D.; Bohle, G.; Huryn, J.M. Osteonecrosis of the Jaw Related to Bevacizumab. J. Clin. Oncol. 2008, 26, 4037–4038. [Google Scholar] [CrossRef]
- Greuter, S.; Schmid, F.; Ruhstaller, T.; Thuerlimann, B. Bevacizumab-associated osteonecrosis of the jaw. Ann. Oncol. 2008, 19, 2091–2092. [Google Scholar] [CrossRef] [PubMed]
- Agostino, N.M.; Gingrich, R.; Drabick, J.J. Bevacizumab Demonstrates Prolonged Disease Stabilization in Patients with Heavily Pretreated Metastatic Renal Cell Carcinoma: A Case Series and Review of the Literature. Adv. Urol. 2010, 2010, 687043. [Google Scholar] [CrossRef] [Green Version]
- Bettini, G.; Blandamura, S.; Saia, G.; Bedogni, A. Bevacizumab-related osteonecrosis of the mandible is a self-limiting disease process. BMJ Case Rep. 2012, 2012, bcr2012007284. [Google Scholar] [PubMed] [Green Version]
- Binello, P.B.; Bandelloni, R.; Labanca, M.; Buffoli, B.; Rezzani, R.; Rodella, L.F. Osteonecrosis and the Jaws and Bevacizumab Therapy: A Case Report. Int. J. Immunopathol. Pharmacol. 2012, 25, 789–791. [Google Scholar] [CrossRef] [Green Version]
- Campisi, G.; Fedele, S.; Fusco, V.; Pizzo, G.; Di Fede, O.; Bedogni, A. Epidemiology, clinical manifestations, risk reduction and treatment strategies of jaw osteonecrosis in cancer patients exposed to antiresorptive agents. Future. Oncol. 2014, 10, 257–275. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pakosch, D.; Papadimas, D.; Munding, J.; Kawa, D.; Kriwalsky, M.S. Osteonecrosis of the mandible due to anti-angiogenic agent, bevacizumab. Oral Maxillofac. Surg. 2013, 17, 303–306. [Google Scholar] [CrossRef] [PubMed]
- Santos-Silva, A.R.; Belizário Rosa, G.A.; de Castro Júnior., G.; Dias, R.B.; Prado Ribeiro, A.C.; Brandão, T.B. Osteonecrosis of the mandible associated with bevacizumab therapy. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2013, 115, e32–36. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Serra, E.; Paolantonio, M.; Spoto, G.; Mastrangelo, F.; Tetè, S.; Dolci, M. Bevacizumab-Related Osteneocrosis of the Jaw. Int. J. Immunopathol. Pharmacol. 2009, 22, 1121–1123. [Google Scholar] [CrossRef]
- Tzermpos, F.; Ismail, A.; Pavli, M.; Tosios, K.I. Osteonecrosis of the mandible in a patient with lung adenocarcinoma undergoing anti-angiogenic therapy with bevacizumab: Bevacizumab associated osteonecrosis of the jaw. Oral Surg. 2016, 9, 40–46. [Google Scholar] [CrossRef]
- Hopp, R.N.; Pucci, J.; Santos-Silva, A.R.; Jorge, J. Osteonecrosis After Administration of Intravitreous Bevacizumab. J. Oral Maxillofac. Surg. 2012, 70, 632–635. [Google Scholar] [CrossRef] [PubMed]
- Erovigni, F.; Gambino, A.; Cabras, M.; Fasciolo, A.; Bianchi, S.; Bellini, E.; Fusco, V. Delayed Diagnosis of Osteonecrosis of the Jaw (ONJ) Associated with Bevacizumab Therapy in Colorectal Cancer Patients: Report of Two Cases. Dent. J. 2016, 4, 39. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mohamed, H.A.M.; Nielsen, C.E.N.; Schiodt, M. Medication related osteonecrosis of the jaws associated with targeted therapy as monotherapy and in combination with antiresorptives. A report of 7 cases from the Copenhagen Cohort. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2018, 125, 157–163. [Google Scholar] [CrossRef]
- Kim, D.W.; Jung, Y.-S.; Park, H.-S.; Jung, H.-D. Osteonecrosis of the jaw related to everolimus: A case report. Br. J. Oral Maxillofac. Surg. 2013, 51, e302–e304. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, D.; Tsubota, Y.; Utsunomiya, T.; Sueoka, N.; Ueda, A.; Endo, K.; Yoshikawa, K.; Kon, M. Osteonecrosis of the jaw associated with everolimus: A case report. Mol. Clin. Oncol. 2017, 6, 255–257. [Google Scholar] [CrossRef] [Green Version]
- Jung, T.-Y. Osteonecrosis of jaw after antiangiogenic agent administration in a renal cell carcinoma patient. Oral Maxillofac. Surg. Cases 2017, 3, 27–33. [Google Scholar] [CrossRef]
- Giancola, F.; Campisi, G.; Lo Russo, L.; Muzio, L.L.; Di Fede, O. Osteonecrosis of the jaw related to everolimus and bisphosphonate: A unique case report? Ann. Stomatol. 2013, 4, 20–21. [Google Scholar]
- Mawardi, H.; Enzinger, P.; McCleary, N.; Manon, R.; Villa, A.; Treister, N.; Woo, S.B. Osteonecrosis of the jaw associated with ziv-aflibercept. J. Gastrointest. Oncol. 2016, 6, e81–e87. [Google Scholar] [CrossRef] [Green Version]
- Ponzetti, A.; Pinta, F.; Spadi, R.; Mecca, C.; Fanchini, L.; Zanini, M.; Ciuffreda, L.; Racca, P. Jaw Osteonecrosisassociated with Aflibercept, Irinotecan and Fluorouracil: Attention to Oral District. Tumori 2016, 102, S74–77. [Google Scholar] [CrossRef] [PubMed]
- Zarringhalam, P.; Brizman, E.; Shakib, K. Medication-related osteonecrosis of the jaw associated with aflibercept. Br. J. Oral Maxillofac. Surg. 2017, 55, 314–315. [Google Scholar] [CrossRef] [PubMed]
- Viviano, M.; Rossi, M.; Cocca, S. A rare case of osteonecrosis of the jaw related to imatinib. J. Korean. Assoc. Oral Maxillofac. Surg. 2017, 43, 120. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Owosho, A.A.; Scordo, M.; Yom, S.K.; Randazzo, J.; Chapman, P.B.; Huryn, J.M.; Estilo, C.L. Osteonecrosis of the jaw a new complication related to Ipilimumab. Oral Oncol. 2015, 51, e100–e101. [Google Scholar] [CrossRef] [Green Version]
- Marino, R.; Orlandi, F.; Arecco, F.; Gandolfo, S.; Pentenero, M. Osteonecrosis of the jaw in a patient receiving cabozantinib. Aust. Dent. J. 2015, 60, 528–531. [Google Scholar] [CrossRef]
- Ebker, T.; Rech, J.; von Wilmowsky, C.; Neukam, F.W.; Stockmann, P. Fulminant course of osteonecrosis of the jaw in a rheumatoid arthritis patient following oral bisphosphonate intake and biologic therapy. Rheumatology 2013, 52, 218–220. [Google Scholar] [CrossRef] [Green Version]
- Garuti, F.; Camelli, V.; Spinardi, L.; Bucci, L.; Trevisani, F. Osteonecrosis of the Jaw during Sorafenib Therapy for Hepatocellular Carcinoma. Tumori 2016, 102, S69–S70. [Google Scholar] [CrossRef]
- Patel, V.; Sproat, C.; Kwok, J.; Tanna, N. Axitinib-related osteonecrosis of the jaw. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2017, 124, e257–e260. [Google Scholar] [CrossRef] [PubMed]
- Antonuzzo, L.; Lunghi, A.; Giommoni, E.; Brugia, M.; Di Costanzo, F. Regorafenib Also Can Cause Osteonecrosis of the Jaw. J. Natl. Cancer. Inst. 2016, 108, djw002. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Preidl, R.H.; Ebker, T.; Raithel, M.; Wehrhan, F.; Neukam, F.W.; Stockmann, P. Osteonecrosis of the jaw in a Crohn’s disease patient following a course of Bisphosphonate and Adalimumab therapy: A case report. BMC Gastroenterol. 2014, 14, 6. [Google Scholar] [CrossRef] [Green Version]
- Cassoni, A.; Romeo, U.; Terenzi, V.; Della Monaca, M.; Rajabtork Zadeh, O.; Raponi, I.; Fadda, M.T.; Polimeni, A.; Valentini, V. Adalimumab: Another Medication Related to Osteonecrosis of the Jaws? Case. Rep. Dent. 2016, 2016, 1–6. [Google Scholar] [CrossRef] [Green Version]
- Favia, G.; Tempesta, A.; Limongelli, L.; Crincoli, V.; Iannone, F.; Lapadula, G.; Maiorano, E. A Case of Osteonecrosis of the Jaw in a Patient with Crohn’s Disease Treated with Infliximab. Am. J. Case. Rep. 2017, 18, 1351–1356. [Google Scholar] [CrossRef] [Green Version]
- Girolomoni, G.; Altomare, G.; Ayala, F.; Berardesca, E.; Calzavara-Pinton, P.; Chimenti, S.; Peserico, A.; Guerra, A.P.; Vena, G.A. Safety of anti-TNFα agents in the treatment of psoriasis and psoriatic arthritis. Immunopharmacol. Immunotoxicol. 2012, 34, 548–560. [Google Scholar] [CrossRef] [PubMed]
- Hasegawa, T.; Kawakita, A.; Ueda, N.; Funahara, R.; Tachibana, A.; Kobayashi, M.; Kondou, E.; Takeda, D.; Kojima, Y.; Sato, S.; et al. A multicenter retrospective study of the risk factors associated with medication-related osteonecrosis of the jaw after tooth extraction in patients receiving oral bisphosphonate therapy: Can primary wound closure and a drug holiday really prevent MRONJ? Osteoporos. Int. 2017, 28, 2465–2473. [Google Scholar] [CrossRef]
- Song, M. Dental care for patients taking antiresorptive drugs: A literature review. Restor. Dent. Endod. 2019, 44, e42. [Google Scholar] [CrossRef] [Green Version]
- Di Fede, O.; Panzarella, V.; Mauceri, R.; Fusco, V.; Bedogni, A.; Lo Muzio, L.; Board, S.O.; Campisi, G. The Dental Management of Patients at Risk of Medication-Related Osteonecrosis of the Jaw: New Paradigm of Primary Prevention. BioMed. Res. Int. 2018, 2018, 1–10. [Google Scholar] [CrossRef]
- Beth-Tasdogan, N.H.; Mayer, B.; Hussein, H.; Zolk, O. Interventions for managing medication-related osteonecrosis of the jaw. Cochrane. Database. Syst. Rev. 2017, 10, CD012432. [Google Scholar] [CrossRef]
- Rollason, V.; Laverrière, A.; MacDonald, L.C.I.; Walsh, T.; Tramèr, M.R.; Vogt-Ferrier, N.B. Interventions for treating bisphosphonate-related osteonecrosis of the jaw (BRONJ). Cochrane. Database. Syst. Rev. 2016, 2, CD008455. [Google Scholar] [CrossRef] [PubMed]
| Author | Age | Sex | Diseases | Medication | Biological Therapies | Causal Factor | Mronj Stage | Mronj Treatment |
|---|---|---|---|---|---|---|---|---|
| Maluf et al. [6] (2016) | 69 | M | Lung cancer metastasis | Irinotecan (QT) | Denosumab | Implant surgery | Mandibular ONJ 2 | Surgical |
| 44 | F | Breast cancer and bone metastasis | Dexamethasone and Fulvestrant | Denosumab y Bevacizumab | Endodontic surgery | Mandibular ONJ 2 | Surgical | |
| Sarina et al. [7] (2013) | 74 | M | Prostate cancer, lung and bone metastasis | QT, Bicalutamida, Goserelina, Dutasterida, Calcium y Vitamin D3 y Zoledronic acid | Denosumab | - | Mandibular ONJ 2 | Surgical |
| Kunimichi et al. [8] (2015) | 60 | F | Breast cancer | - | Denosumab | Poorly fitting prosthesis | Mandibular ONJ 1 | - |
| Badr et al. [9] (2017) | 55 | F | Breast cancer | - | Denosumab | Tooth extraction | Mandibular ONJ 3 | Hospitable treatment |
| 76 | F | Breast cancer metastasis | Hormone therapy and radiation therapy | Denosumab | Tooth extraction | Mandibular ONJ 1 | Surgical | |
| 66 | F | Bone, liver and peritoneum metastasis from breast cancer | QT and opioids | Denosumab | Tooth extraction | Mandibular ONJ 3 | Surgical | |
| 66 | F | Bone metástasis and breast cancer | Hormone therapy and opioids. Prior zoledronic acid therapy. | Denosumab | Poorly fitting prosthesis | Maxillary ONJ 3 | Conservative | |
| Nifosi et al. [10] (2017) | 47 | M | Renal adenocarcinoma | Calcium and Vitamin D | Temsirolimus y Denosumab | - | Mandibular ONJ 2 | Conservative |
| Allegra et al. [11] (2014) | 56 | M | Waldenstron’s macroglobulinemia, POEMS syndrome, lymphoplasmacytic lymphoma | QT (Doxorrubicin, Cyclophosphamide, Vincristine, Prednisone) | Rituximab | Tooth extraction | Mandibular ONJ 2 | Conservative |
| Keribin et al. [5] (2017) | 69 | M | Nephropathy IgA | Immunoglobulin, Ranitidine, Trimethoprim + Sulfamethoxazole, Valganciclovir, Ofloxacin, Itraconozanol, Manidipine, Nebivolo, Perindopril, Indapamide | Rituximab y Tacrolimus | - | Maxillary and mandibular ONJ 2 | Surgical |
| Baur et al. [12] (2012) | 58 | M | Lymphoma cells B | Chemotherapy (Doxorrubicin, Cyclophosphamide, Vincristine, Prednisone), Diltiazem, Atorvastatin, Meloxicam, Lisinopril, Hydroclorothiazide, Insulina, Metformin and Aspirin. | Rituximab | - | Mandibular ONJ 2 | Surgical |
| Javelot et al. [13] (2020) | 69 | F | Rheumatoid arthritis | Prednisolone, Leflunomid, Valsartan y Vitamin D3. Previous treatment with Risedronate and Infliximab. | Rituximab | Herpetic gingivostomatitis | Mandibular ONJ 2 | Surgical |
| Weigert et al. [14] (2014) | 39 | M | Non- Hogdkin lymphoma | Ciclofosfamide, Vincristine, Doxorrubicin y Prednisone | Rituximab | - | Mandibular ONJ 0 | Conservative |
| Manzie et al. [15] (2019) | 76 | F | Breast cancer metastasis | Chemotherapy, Carboplatin, Gemcitabine, Epirubicine, Paclitaxel, Amlodipine, Irebsartan | Trastuzumab + Pertuzumab | - | Mandibular ONJ 2 | Surgical |
| Mauceri et al. [16] (2019) | 58 | M | Hurtle’s cell carcinoma, lung metastasis | Radiotherapy, chemotherapy (Doxorrubicin, Cisplatin), Ciclofosfamide, Metrotexate | Lenvatinib | Tooth extraction | Maxillary ONJ 1 | Conservative |
| Fleissig et al. [17] (2012) | 58 | F | Renal carcinoma, Osteoporosis | Levothyroxine sodium | Sunitinib | Tooth extraction | Mandibular ONJ 2 | Conservative |
| Brunello et al. [18] (2009) | 59 | M | Renal carcinoma with ischial and pulmonary metastasis | Previous zoledronic acid | Sunitinib | - | Mandibular ONJ 2 | Conservative |
| Koch et al. [19] (2011) | 59 | M | Renal carcinoma, soft tissues metastasis | Interferon, Vinblastine, Ramipril, Hydroclorothiazide, Metropolol, Levothyroxine | Sorafenib y Sunitib | Tooth extraction | Mandibular ONJ 1 | Surgical |
| Melloni et al. [20] (2016) | 62 | M | Renal carcinoma, cutaneous metastasis | Interferon, IL-2 | Sunitinib | Tooth extraction | Mandibular ONJ 3 | Surgical |
| Nicolatou-Galitis et al. [21] (2012) | 19 | F | Renal carcinoma | Cisplatin | Sunitinib y Everolimus | - | Mandibular ONJ 2 | Conservative |
| 64 | F | Renal carcinoma | Prednisolone, L-4 | Sunitinib | Prosthesis trauma | Mandibular ONJ 2 | Surgical | |
| Agrillo et al. [22] (2012) | 65 | M | Renal carcinoma | Previous zoledronic acid | Sunitinib | - | ONJ 3 maxilar | Surgical |
| 67 | M | Renal carcinoma | Previous zoledronic acid | Sunitinib y Temsirolimus | - | Mandibular ONJ 3 | Surgical | |
| Estilo et al. [27] (2008) | 33 | F | Glioblastoma multiforme | Radiotherapy, Temozolomide | Bevacizumab | - | Mandibular ONJ 2 | - |
| 51 | F | Infiltrating ductal carcinoma | Chemotherapy(Doxorrubicin+ciclofosfamide, hormonal therapy, Paclitaxel, radiotherapy, Capecitabine | Bevacizumab | - | Mandibular ONJ 2 | Surgical | |
| Greuter et al. [28] (2008) | 63 | F | Breast cancer | Doxorrubicin | Bevacizumab | Tooth extraction | Maxillary ONJ 3 | Surgical |
| Agostino et al. [29] (2010) | 73 | M | Renal carcinoma | - | Sunitinib, Temsirolimus y Bevacizumab | - | - | - |
| 76 | M | Renal carcinoma | IL-2 | Sorafenib, Sunitinib, Temsirolimus y Bevacizumab | - | - | - | |
| 68 | M | Renal carcinoma | IL-2 | Sunitinib, Everolimus y Bevacizumab | - | - | - | |
| 58 | F | Renal carcinoma | IL-2 | Sunitinib, Sorafenib, Temsirolimus y Bevacizumab | - | - | - | |
| Bettini et al. [30] (2012) | 57 | F | Lung cancer | Chemotherapy, Gentamicine, Cisplatin, Corticosteroids, Lincomicine | Bevacizumab | - | Mandibular ONJ 2 mandibular | Surgical |
| Brunamonti et al. [31] (2012) | 47 | M | Adenocarcinoma | Epirubicin+Cisplatin | Bevacizumab | - | Mandibular ONJ 2 | Surgical |
| Fusco et al. [32] (2014) | 60 | M | Rectal cancer, lung metastasis | Chemotherapy and radiotherapy | Bevacizumab | Tooth extraction | Mandibular ONJ 2 | Conservative |
| Pakosch et al. [33] (2013) | 53 | F | Pancreas cancer | Gemcitabine, Folinic acid, Oxaliplatin, Paclitaxel | Erlotinib, Bevacizumab y Sorafenib | Poorly fitted prosthesis | Mandibular ONJ 2 | Surgical |
| Santos-Silva et al. [34] (2013) | 61 | M | Renal carcinoma | Captopril, Hidroclorotiazide | Bevacizumab y Temsirolimus | - | Mandibular ONJ 2 | Conservative |
| Serra et al. [35] (2009) | 64 | M | Lung adenocarcinoma | Cisplatin, Gemcitabine | Bevacizumab | - | Mandibular ONJ 2 | Surgical |
| Tzermpos et al. [36] (2014) | 69 | M | Lung cancer | Chemotherapy (Carboplatin+ Docetaxel), Cortisone | Bevacizumab | Poorly fitted prosthesis | Mandibular ONJ 2 | Surgical |
| Hopp et al. [37] (2012) | 58 | M | Retinal vascular thrombosis | - | Bevacizumab | - | Mandibular ONJ 2 | Surgical |
| Erovigni et al. [38] (2016) | 79 | M | Colon adenocarcinoma | Capecitabin, Oxaliplatin, Fluoracil, Folínic acid, Irinotecan, radiotherapy | Bevacizumab | Tooth extraction | Mandibular ONJ 2 | Conservative |
| 60 | M | Rectal cancer, lung and brain metastasis | Chemotherapy and radiotherapy | Bevacizumab | Tooth extraction | Mandibular ONJ 2 | Conservative | |
| Mawardi et al. [44] (2016) | 43 | M | Metastasis of colorectal carinoma | 5-fluorouracil, Leucovorin, Irinotecan | Aflibercept | - | Mandibular ONJ 1 | Surgical |
| 63 | M | Gastrointestinal metastatuc carcinoid | 5-fluorouracil, Leucovorin and Oxaliplatin | Aflibercept | - | Mandibular ONJ 1 | Conservative | |
| 51 | M | Esophageal carcinoma metastasis | - | Aflibercept | Tooth extraction | Mandibular ONJ 1 | Conservative | |
| Ponzetti et al. [45] (2016) | 64 | F | Metastasis of colorectal carinoma | 5-fluoracil, Irinotecan and Levofolinic Acid | Aflibercept | - | Mandibular ONJ 1 | Conservative |
| Zarringhalam et al. [46] (2017) | 47 | M | Intestine, liver, peritoneum and pelvis metastasis | - | Aflibercept | - | Mandibular ONJ 1 | Conservative |
| Viviano et al. [47] (2017) | 72 | M | Gastrointestinal stromal tumor | - | Imatinib | Tooth extraction | Mandibular ONJ 2 | Surgical |
| Owosho et al. [48] (2015) | 52 | M | Melanoma metastasis in the iliac region and pancreas | - | Ipilimumab | - | Mandibular ONJ 2 | Surgical |
| Kim et al. [40] (2013) | 52 | M | Bone metastasis from thyroid cancer | Previous zoledronc acid treatment | Everolimus | - | Mandibular ONJ 2 | Conservative |
| Yamamoto et al. [41] (2017) | 80 | F | Breast cancer | Capecitabine, Tamoxifen, Fulvestrant y Exemestan | Everolimus | - | Mandibular ONJ 2 | Conservative |
| Jung et al. [42] (2017) | 62 | F | Renal carcinoma | - | Everolimus y Pazopanib | Implant surgery | Mandibular ONJ 2 | Surgical |
| Giancola et al. [43] (2013) | 64 | M | Renal carcinoma metastasis | Previous zoledronc acid treatment | Everolimus | - | Mandibular ONJ 2 | Surgical |
| Garuti et al. [51] (2017) | 74 | M | Hepatic cancer | - | Sorafenib | Tooth extraction | Mandibular ONJ 1 | Conservative |
| Marino et al. [49] (2015) | 51 | F | Liver and lymph nodes metástasis from thyroid cancer | Levotiroxine, Calcitriol, Vitamin D3, Duloxetine, Propanolol, Lansoprazole y Loperamide | Cabozantinib | Tooth extraction | Mandibular ONJ 2 | Surgical |
| Mohamed et al. [39] (2018) | 70 | M | Renal carcinoma | - | Sunitinib, Everolimus, Pazopanib | Tooth extraction | Mandibular ONJ 1 | Conservative |
| 53 | F | Lung cancer | Carboplatin, Cisplatin, Vironelbine Zoledronic | Erlotinib, Afatinib y Denosumab | Tooth extraction | Maxillary ONJ 2 | Surgical | |
| 55 | F | Lung cancer | Carboplatine, Vironelbine, Alimeta. | Bevacizumab | Tooth extraction | Maxillary ONJ 1 | Conservative | |
| 66 | M | Multiforme glioblastoma | Temozolomide, Irinotecan | Bevacizumab | Trauma by intraoral radiography | Mandibular ONJ 2 | Conservative | |
| 74 | F | Multiple myeloma | Cyclophosphamide, Thalidomide, Alkaran, Capecitabine, Oxaliplatin, Folfiri, Irinotecan, and Pamidronate | Bevacizumab y Cetuximab | Spontaneous | Mandibular ONJ 1 | Surgical | |
| 53 | F | Leukemia | Citarabine and Vincristine | Nilotinib y Dasanitib | Gingival ulcer | Mandibular ONJ 2 | Surgical | |
| 81 | F | Leukemia | Capecitabine, Alendronate | Trastuzumab, Imatinib y Denosumab | Tooth extraction | Mandibular ONJ 2 | Surgical | |
| Patel et al. [52] (2017) | 67 | M | Lung, brain, skin, hearth and pelvis metástasis from renal carcinoma | Amlodipine, Ramipril, Levetiracetam, Dexamethasone, Lansoprazole, Morphine, Metoclopramide, Amiodarone hydrochloride, and Cholecalciferol. Previous treatment Pazopanib and Nivolumab | Axitinib | - | Maxillary ONJ 1 | Conservative |
| Antonuzzo et al. [53] (2016) | 59 | F | Metastatic colorectal cancer | - | Regorafenib | - | Maxillary ONJ 3 | - |
| Preidl et al. [54] (2014) | 36 | F | Crohn disease | Steroids, Risedronate, Zoledronic acid, Prednisolone | Adalimumab | Tooth extraction | Mandibular ONJ 3 | Surgical |
| Cassoni et al. [55] (2016) | 63 | F | Idiopathic arthritis | Salazopyrin | Adalimumab | Implant surgery | Mandibular ONJ mandibular | Surgical |
| Favia et al. [56] (2017) | 49 | F | Chron disease | - | Infliximab | Tooth extraction | Mandibular ONJ 3 mandibular | Surgical |
| Ekber et al. [50] (2013) | 74 | F | Rheumatoid arthritis and osteoporosis | Methotrexate, Prednisolone, Folic Acid, Ibuprofen, Pantoprazole, Calcium, Vit. D. Previous treatment with zoledronic acid. | Infliximab | Tooth extraction | Mandibular ONJ 3 | Surgical |
| Tocilizumab | Tarthrectomy | Mandibular ONJ 3 | Surgical |
| Drug | Trade Name | Category |
|---|---|---|
| Adalimumab | Humira | MAB |
| Afatinib | Giotrif | TKI |
| Aflibercept | Zaltrap, Eylea | Fusion prothein |
| Axitinib | Inlyta | TKI |
| Bevacizumab | Avastin | MAB |
| Cabozantinib | Cometriq, Cabometyx | TKI |
| Dasatinib | Sprycel | TKI |
| Denosumab | Xgeva, Prolia | MAB |
| Erlotinib | Tarceva | TKI |
| Everolimus | Afinitor | mTOR inhibitor |
| Imatinib | Gleevec | TKI |
| Infliximab | Remicade | MAB |
| Ipilimumab | Yervoy | MAB |
| Lenvatinib | Lenvima | TKI |
| Nilotinib | Tasigna | TKI |
| Pazopanib | Votrient | TKI |
| Regorafenib | Stivarga | TKI |
| Rituximab | Erbitux, Rituxan | MAB |
| Sorafenib | Nexavar | TKI |
| Sunitinib | Sutent | TKI |
| Tacrolimus | Advagraf | mTOR inhibitor |
| Temsirolimus | Torisel | mTOR inhibitor |
| Tocilizumab | Actembra | MAB |
| Trastuzumab+Pertuzumab | Herceptin + Perjeta | MAB |
| Grade | Treatment |
|---|---|
| Risk: No apparent necrotic bone | Treatment not indicated, patient education |
| Grade 0: No clinical evidence of bone necrosis, but nonspecific clinical findings, radiographic changes, and symptoms. | Systemic management, including the use of analgesics and antibiotic. |
| Grade 1: Exposure and bone necrosis, or fistulas that can be probed to bone in asymptomatic patients without evidence of infection. | Antibacterial rinses, clinical follow-up, patient education. |
| Grade 2: Exposure and bone necrosis, or fistulas that can be probed to the bone, associated with infection with pain or erythema in the region of exposed bone with or without purulent drainage. | Symptomatic treatment with oral antibiotics, antibacterial rinses, pain control, debridement to relieve soft tissue irritation and control infection. |
| Grade 3: Presence of one of the following signs: bone exposure and necrosis that extends beyond the alveolar region, pathological fractures, extraoral fistulas, oro-nasal or oro-antral communication, osteolysis that extends to the lower border of the mandible or floor of the breast. | Antibacterial rinses, antibiotic therapy and pain control, surgical debridement or resection to alleviate infection and long-lasting pain. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Amigo-Basilio, M.; Álvarez-González, C.; Cobo-Vázquez, C.; Leco-Berrocal, I.; Sáez-Alcaide, L.M.; Méniz-García, C. Management of Patients under Treatment with Monoclonal Antibodies and New Biological Therapies. Appl. Sci. 2021, 11, 4865. https://doi.org/10.3390/app11114865
Amigo-Basilio M, Álvarez-González C, Cobo-Vázquez C, Leco-Berrocal I, Sáez-Alcaide LM, Méniz-García C. Management of Patients under Treatment with Monoclonal Antibodies and New Biological Therapies. Applied Sciences. 2021; 11(11):4865. https://doi.org/10.3390/app11114865
Chicago/Turabian StyleAmigo-Basilio, Marta, Covadonga Álvarez-González, Carlos Cobo-Vázquez, Isabel Leco-Berrocal, Luis Miguel Sáez-Alcaide, and Cristina Méniz-García. 2021. "Management of Patients under Treatment with Monoclonal Antibodies and New Biological Therapies" Applied Sciences 11, no. 11: 4865. https://doi.org/10.3390/app11114865
APA StyleAmigo-Basilio, M., Álvarez-González, C., Cobo-Vázquez, C., Leco-Berrocal, I., Sáez-Alcaide, L. M., & Méniz-García, C. (2021). Management of Patients under Treatment with Monoclonal Antibodies and New Biological Therapies. Applied Sciences, 11(11), 4865. https://doi.org/10.3390/app11114865






