Topical Application of Chlorhexidine Gel with Brush-On Technique in the Tailored Treatment of Plaque Induced Gingivitis
Abstract
1. Introduction
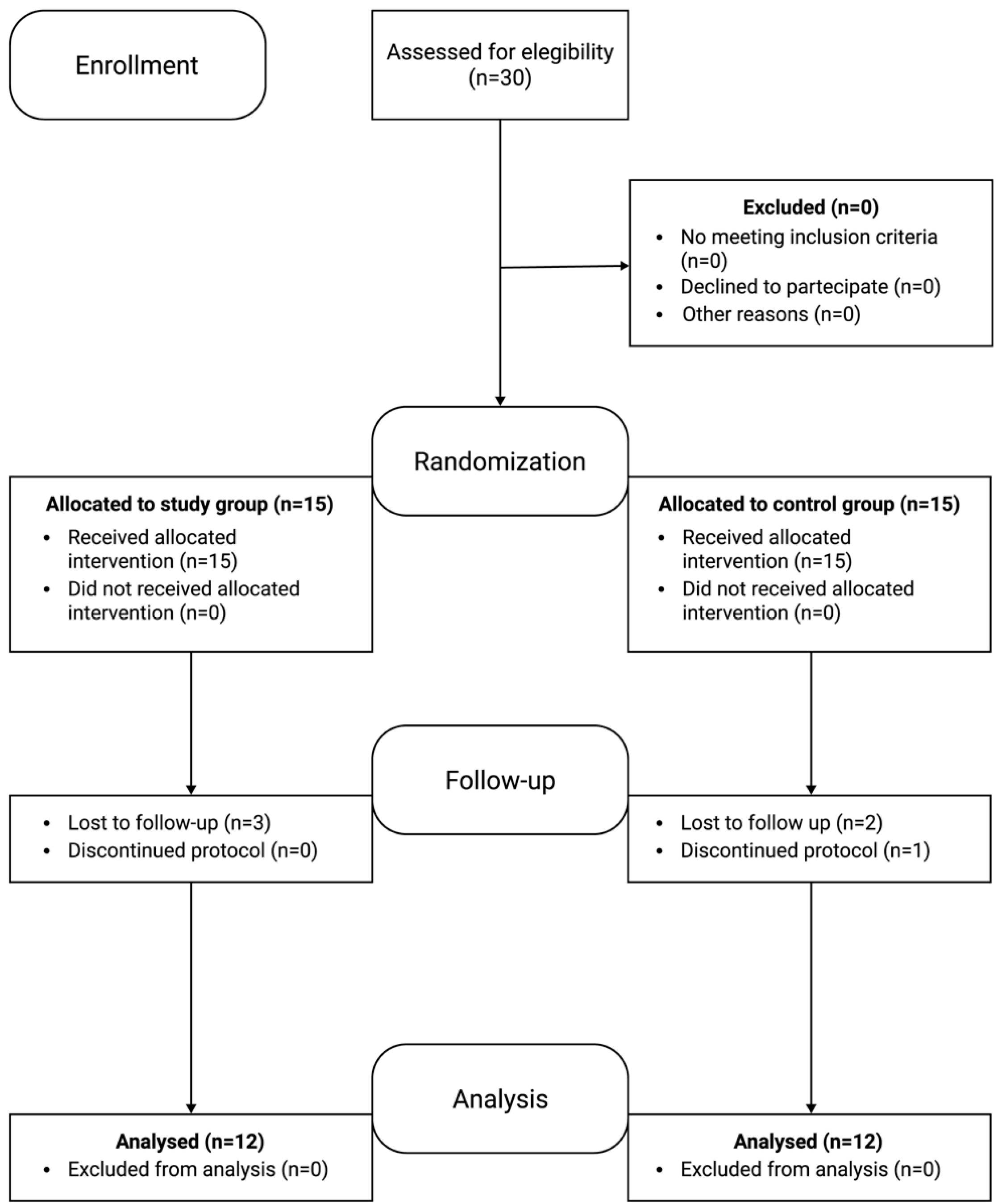
2. Materials and Methods
Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- White, D.A.; Tsakos, G.; Pitts, N.B.; Fuller, E.; Douglas, G.; Murray, J.J.; Steele, J. Adult Dental Health Survey 2009: Common oral health conditions and their impact on the population. Br. Dent. J. 2012, 213, 567–572. [Google Scholar] [CrossRef] [PubMed]
- Trombelli, L.; Farina, R.; Silva, C.O.; Tatakis, D.N. Plaque-induced gingivitis: Case definition and diagnostic considerations. J. Periodontol. 2018, 89, 46–73. [Google Scholar] [CrossRef] [PubMed]
- Murakami, S.; Mealey, B.L.; Mariotti, A.; Chapple, I.L. Dental-plaque induced gingival conditions. J. Periodontol. 2018, 89, 17–27. [Google Scholar] [CrossRef] [PubMed]
- American Academy of Periodontology-Research, Science, and Therapy Committee; American Academy of Pediatric Dentistry. Treatment of plaque-induced gingivitis, chronic periodontitis, and other clinical conditions. Pediatr. Dent. 2005, 27, 202–211. [Google Scholar]
- Lang, N.P.; Schätzle, M.A.; Löe, H. Gingivitis as a risk factor in periodontal disease. J. Clin. Periodontol. 2009, 36, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Tatakis, D.N.; Trombelli, L. Modulation of clinical expression of plaque-induced gingivitis. I. Background review and rationale. J. Clin. Periodontol. 2004, 31, 229–238. [Google Scholar] [CrossRef] [PubMed]
- David, S.C.; Mário, T.G.; De Freitas, G.C.; Kantorski, K.Z.; Wikesjö, U.M.E.; Moreira, C.H.C. Correlation between plaque control and gingival health using short and extended oral hygiene intervals. Clin. Oral. Investig. 2018, 22, 2593–2597. [Google Scholar] [CrossRef]
- Graziani, F.; Karapetsa, D.; Alonso, B.; Herrera, D. Nonsurgical and surgical treatment of periodontitis: How many options for one disease? Periodontol. 2000 2017, 75, 152–188. [Google Scholar] [CrossRef]
- Westfelt, E. Rationale of mechanical plaque control. J. Clin. Periodontol. 1996, 23, 263–267. [Google Scholar] [CrossRef]
- Serrano, J.; Escribano, M.; Roldán, S.; Martín, C.; Herrera, D. Efficacy of adjunctive anti-plaque chemical agents in managing gingivitis: A systematic review and meta-analysis. J. Clin. Periodontol. 2015, 42, 106–138. [Google Scholar] [CrossRef]
- Jentsch, H.F.; Eckert, F.R.; Eschrich, K.; Stratul, S.I.; Kneist, S. Antibacterial action of Chlorhexidine/thymol containing varnishes in vitro and in vivo. Int. J. Dent. Hyg. 2014, 12, 168–173. [Google Scholar] [CrossRef] [PubMed]
- Park, E.; Na, H.S.; Kim, S.M.; Wallet, S.; Cha, S.; Chung, J. Xylitol, an anticaries agent, exhibits potent inhibition of inflammatory responses in human THP-1-derived macrophages infected with Porphyromonas gingivalis. J. Periodontol. 2014, 85, 212–223. [Google Scholar] [CrossRef] [PubMed]
- Löe, H. The Gingival Index, the Plaque Index and the Retention Index Systems. J. Periodontol. 1967, 38, 610–616. [Google Scholar] [CrossRef]
- Nardi, G.M.; Sabatini, S.; Guerra, F.; Tatullo, M.; Ottolenghi, L. Tailored Brushing Method (TBM): An innovative simple protocol to improve oral care. J. Biomed. 2016, 1, 26–31. [Google Scholar] [CrossRef][Green Version]
- Frencken, J.E.; Sharma, P.; Stenhouse, L.; Green, D.; Laverty, D.; Dietrich, T. Global epidemiology of dental caries and severe periodontitis - a comprehensive review. J. Clin. Periodontol. 2017, 44, 94–105. [Google Scholar] [CrossRef]
- Durham, J.; Fraser, H.M.; McCracken, G.I.; Stone, K.M.; John, M.T.; Preshaw, P.M. Impact of periodontitis on oral health-related quality of life. J. Dent. 2013, 41, 370–376. [Google Scholar] [CrossRef]
- Chapple, I.L. Primary prevention of periodontitis: Managing gingivitis. J. Clin. Periodontol. 2015, 42, 71–76. [Google Scholar] [CrossRef]
- Van der Weijden, F.A.; Slot, D.E. Efficacy of homecare regimens for mechanical plaque removal in managing gingivitis a meta review. J. Clin. Periodontol. 2015, 42, 77–91. [Google Scholar] [CrossRef]
- Ribeiro, L.G.; Hashizume, L.N.; Maltz, M. The effect of different formulations of chlorhexidine in reducing levels of mutans streptococci in the oral cavity: A systematic review of the literature. J. Dent. 2007, 35, 359–370. [Google Scholar] [CrossRef]
- Supranoto, S.; Slot, D.; Addy, M.; Van der Weijden, G. The effect of chlorhexidine dentifrice or gel versus chlorhexidine mouthwash on plaque, gingivitis, bleeding and tooth discoloration: A systematic review. Int. J. Dent. Hyg. 2014, 13, 83–92. [Google Scholar] [CrossRef]
- Campus, G.; Cagetti, M.G.; Sale, S.; Petruzzi, M.; Solinas, G.; Strohmenger, L.; Lingström, P. Six months of high-dose xylitol in high-risk caries subjects—A 2-year randomised, clinical trial. Clin. Oral. Investig. 2013, 17, 785–791. [Google Scholar] [CrossRef] [PubMed]
- Hallström, H.; Lindgren, S.; Twetman, S. Effect of a chlorhexidine-containing brush-on gel on peri-implant mucositis. Int. J. Dent. Hyg. 2017, 15, 149–153. [Google Scholar] [CrossRef] [PubMed]
- Clavero, J.; Baca, P.; Paloma González, M.; Valderrama, M.J. Efficacy chlorhexidine-thymol varnish (Cervitec) against plaque accumulation and gingival inflammation in a geriatric population. Gerodontology 2006, 23, 43–47. [Google Scholar] [CrossRef] [PubMed]
| Group | n. Patients | Decrease t0–t3 (%) | p Value | |
|---|---|---|---|---|
| FMPS | Study Control | 12 12 | 87% 75% | 0.03 * 0.03 * |
| GI | Study Control | 12 12 | 84% 80% | 0.03 * 0.03 * |
| Patients | Plaque Score (Means) | Gingival Index (Means) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | Mean Age | Sex | t0 | t1 | t2 | t3 | Δ(t0–t3) | t0 | t1 | t2 | t3 | Δ(t0–t3) | |
| Study group | 12 | 50 | F = 7 M = 5 | 2.11 SD = 0.6 | 1.09 SD = 0.3 | 0.63 SD = 0.2 | 0.31 SD = 0.1 | 1.83 SD = 0.5 | 1.6 SD = 0.5 | 0.9 SD = 0.3 | 0.54 SD = 0.2 | 0.26 SD = 0.1 | 1.34 SD = 0.4 |
| Control group | 12 | 46 | F = 6 M = 6 | 1.16 SD = 0.5 | 0.58 SD = 0.4 | 0.46 SD = 0.4 | 0.48 SD = 0.3 | 0.87 SD = 0.3 | 1.87 SD = 1.1 | 1.46 SD = 1.4 | 0.87 SD = 0.5 | 0.68 SD = 0.5 | 1.17 SD = 0.6 |
| p value | 0.21 | 0.68 | 0.16 | 0.5 | 0.5 | 0.42 | 0.049 | 0.13 | 0.34 | 0.48 | 0.29 | 0.17 | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nardi, G.M.; Grassi, R.; Campus, G.; Pareti, M.L.; Stasio, D.D.; Petruzzi, M.; della Vella, F. Topical Application of Chlorhexidine Gel with Brush-On Technique in the Tailored Treatment of Plaque Induced Gingivitis. Appl. Sci. 2020, 10, 6014. https://doi.org/10.3390/app10176014
Nardi GM, Grassi R, Campus G, Pareti ML, Stasio DD, Petruzzi M, della Vella F. Topical Application of Chlorhexidine Gel with Brush-On Technique in the Tailored Treatment of Plaque Induced Gingivitis. Applied Sciences. 2020; 10(17):6014. https://doi.org/10.3390/app10176014
Chicago/Turabian StyleNardi, Gianna Maria, Roberta Grassi, Guglielmo Campus, Maria Letizia Pareti, Dario Di Stasio, Massimo Petruzzi, and Fedora della Vella. 2020. "Topical Application of Chlorhexidine Gel with Brush-On Technique in the Tailored Treatment of Plaque Induced Gingivitis" Applied Sciences 10, no. 17: 6014. https://doi.org/10.3390/app10176014
APA StyleNardi, G. M., Grassi, R., Campus, G., Pareti, M. L., Stasio, D. D., Petruzzi, M., & della Vella, F. (2020). Topical Application of Chlorhexidine Gel with Brush-On Technique in the Tailored Treatment of Plaque Induced Gingivitis. Applied Sciences, 10(17), 6014. https://doi.org/10.3390/app10176014








