Particle (Soot) Pollution in Port Harcourt Rivers State, Nigeria—Double Air Pollution Burden? Understanding and Tackling Potential Environmental Public Health Impacts
Abstract
1. Introduction
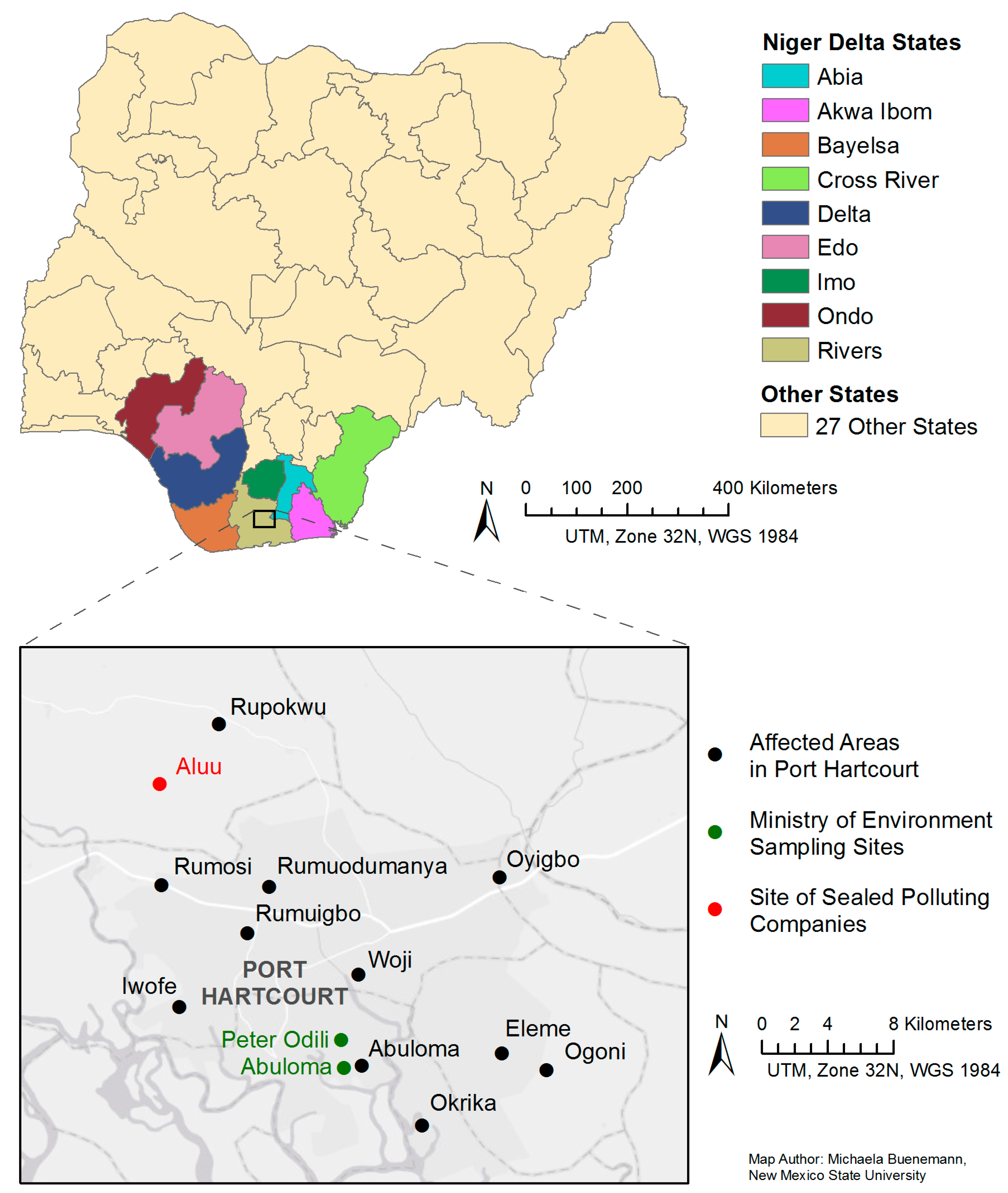
1.1. The Niger Delta
Port Harcourt
1.2. Double Air Pollution Burden
1.3. Prevailing Air Quality Problems
2. Criteria Air Pollutants—The United States Environmental Protection Agency (EPA)
3. Seriousness of the Problem
3.1. Public Health Impacts
3.2. Carcinogenicity of Soot and Other Particle Pollution
3.3. High Risk Populations
3.3.1. Preexisting Diseases
Cardiovascular Disease (CVD)
Coronary Artery Disease (CAD)
Congestive Heart Failure (CHF)
3.3.2. Respiratory Disease
Chronic Obstructive Pulmonary Disease (COPD)
Asthma
3.3.3. Children and Older Adults
3.3.4. Socioeconomic Status (SES)
3.4. Environmental Consequences
3.5. Socioeconomic Costs
4. Stakeholders’ Reaction
4.1. Public Response
4.2. Government Action
4.3. Task Force Findings
4.4. Other Sources of Particle Polution
4.5. Lessons from Nigeria’s 2014–2015 Ebola Virus Disease (EVD) Prevention
5. The Role of Environmental Policy and Regulation
5.1. Environmental Impact Assessment (EIA) Act 1992
5.2. National Environmental Standards and Regulation Enforcement Agency (NESREA) Act 2007
Some Regulations under NESREA
National Effluent Limitation Regulations
National Environmental Protection (Pollution Abatement in Industries and Facilities producing Waste) Regulations (1991)
Federal Solid and Hazardous Waste Management Regulations (1991)
Harmful Wastes (Special Criminal Provisions) Act of 1988
5.3. Factories Act, CAP F1, LFN 2004
5.4. Infringements and Penalties
6. Discussion
6.1. Implications for Public Health
6.2. Violations of Environmental Regulations
6.3. Current Situation
7. Conclusions
Acknowledgments
Conflicts of Interest
References
- World Health Organization (WHO). WHO Releases Country Estimates on Air Pollution Exposure and Health Impact. Available online: http://www.who.int/mediacentre/news/releases/2016/air-pollution-estimates/en/ (accessed on 23 July 2017).
- The World Bank. Little Green Data Book 2015. Available online: https://openknowledge.worldbank.org/bitstream/handle/10986/22025/9781464805608.pdf (accessed on 26 July 2017).
- World Health Organization (WHO). Air Pollution. Available online: http://www.who.int/ceh/risks/cehair/en/ (assessed on 1 August 2017).
- World Health Organization (WHO). Air Pollution Levels Rising in Many of the World’s Poorest Cities. Available online: http://www.who.int/mediacentre/news/releases/2016/air-pollution-rising/en/ (accessed on 23 July 2017).
- Godson, R.E.E.A.; Sridhar, M.K.C. Industrial Emissions and Health Hazards among Selected Factory Workers at Eleme, Nigeria. Int. J. Environ. Health Res. 2009, 9, 43–51. [Google Scholar]
- Rim-Rukeh, A. An Assessment of Indoor Air Quality in Selected Households in Squatter Settlements Warri, Nigeria. Adv. Life Sci. 2015, 5, 1–11. [Google Scholar] [CrossRef]
- Nwachukwu, A.N.; Chukwuocha, E.O.; Igbudu, O. A Survey on the Effects of Air Pollution on Diseases of the People of Rivers State, Nigeria. Afr. J. Environ. Sci. Technol. 2012, 6, 371–379. [Google Scholar] [CrossRef]
- Ubong, I.U.; Ubong, U.U.; Ubong, U.E.; Ukonta, R.; Ishmael, D. Distribution of Particulate Matter in Cawthorne Channels Air Basin in Nigeria. Environ. Pollut. 2015, 4, 19–26. [Google Scholar] [CrossRef]
- Adoki, A. Air Quality Survey of some locations in the Niger Delta Area. J. Appl. Sci. Environ. Manag. 2012, 16, 125–134. [Google Scholar]
- Godson, A.R.; Sridhar, M.K.; Bamgboye, E.A. Environmental Risk Factors and Health Outcomes in Selected Communities of the Niger Delta Area, Nigeria. Perspect. Public Health 2009, 129, 183–191. [Google Scholar]
- Godson, R.E.E.A.; Sridhar, M.K.C.; Asuzu, C.M. Environmental Risk Factors and Hospital-Based Cancers in Two Nigerian Cities. J. Public Health Epidemiol. 2010, 2, 216–223. [Google Scholar]
- Allen, F. Dangerous Air Pollution in the City of Port Harcourt. Pambazuka News. Available online: https://www.pambazuka.org/node/96487 (accessed on 29 July 2017).
- World. Nigeria Battles Hazardous Air Pollution: Black Soot Fills the Air in the City of Port Harcourt. Available online: https://world.wng.org/2017/02/nigeria_battles_hazardous_air_pollution (accessed on 2 August 2017).
- Punch. The Black Soot Plague in Port Harcourt. Available online: http://punchng.com/black-soot-plague-port-harcourt/ (accessed on 25 July 2017).
- Odum, A.; Ogbada, E.I. Evaluating the Financial Implication of Arms Struggle in the Niger Delta Region of Nigeria. Int. Cent. Bus. Res. 2014, 3, 38–43. [Google Scholar]
- Niger Delta Development Commission (NDDC). Niger Delta Regional Development Master Plan; Summary of Draft Report; NDDC: Port Harcourt, Nigeria, 2004.
- Barbier, E.B.; Acreman, M.C.; Knowler, D. Economic Valuation of Wetlands, a Guide for Policy Makers and Planners; Ramsar Convention Bureau: Gland, Switzerland, 1997. [Google Scholar]
- Wetlands International. Conserving and Restoring Wetlands in Nigeria’s Niger River Delta. Available online: https://www.wetlands.org/casestudy/conserving-and-restoring-wetlands-in-nigerias-niger-river-delta/ (accessed on 25 October 2017).
- Francis, P.; LaPin, D.; Rossiasco, P. Securing Development and Peace in the Niger Delta a Social and Conflict Analysis for Change; Woodrow Wilson International Center for Scholars: Washington, DC, USA, 2011. [Google Scholar]
- Okonkwo, C.N.P.; Kumar, L.; Taylor, S. The Niger Delta Wetland Ecosystem: What Threatens It and Why Should We Protect It? Afr. J. Environ. Sci. Technol. 2015, 9, 451–463. [Google Scholar]
- Ogri, O.R. A review of the Nigerian petroleum industry and the associated environmental problems. Environmentalist 2001, 21, 11–21. [Google Scholar] [CrossRef]
- Niger Delta Development Commission (NDDC). Draft Copy of the Niger Delta Regional Development Master Plan; Directorate of Planning; NDDC: Port Harcourt, Nigeria, 2005.
- United Nations Development Programme. Niger Delta Human Development Report; United Nations Development Programme: New York, NY, USA, 2006. [Google Scholar]
- Brookings. Analysis of Community-Driven Development in Nigeria’s Niger Delta Region: Use of the Institutional Analysis and Development (IAD) Framework. Available online: https://www.brookings.edu/wp-content/uploads/2016/06/Akassa-Revised-WEB.pdf (accessed on 6 November 2017).
- Balouga, J. The Niger Delta: Defusing the Time Bomb. International Association for Energy Economics. 2009. Available online: https://www.iaee.org/documents/newsletterarticles/109balouga.pdf (accessed on 27 October 2017).
- Akukwe, T.I.; Ogbodo, I.T.C. Spatial Analysis of Vulnerability to Flooding in Port Harcourt Metropolis, Nigeria. SAGE 2015, 5. [Google Scholar] [CrossRef]
- Weli, E.V.; Efe, I.S. Climate and Epidemiology of Malaria in Port Harcourt Region, Nigeria. AJCC 2015, 4, 40–47. [Google Scholar] [CrossRef]
- American Association for the Advancement of Science. Eye on Nigeria: Technical Report. Available online: https://www.aaas.org/sites/default/files/AAAS_EyesOnNigeria_Technical_Report.pdf (accessed on 23 November 2017).
- Kio-Lawson, D.; Dekor, J.B. Port Harcourt, the Garden City: A Garden of Residents Nightmare. World Environ. 2014, 4, 111–120. [Google Scholar] [CrossRef]
- Weli, E.V.; Worlu, S.O. Recent Rainstorm Dynamics and Its Implications for Flood Frequency in Sub-Humid Tropical City of Port Harcourt Nigeria. J. Geogr. Thought 2011, 12, 31–81. [Google Scholar]
- Eludoyin, O.S.; Weli, E.V. Spatial Analysis of Flood Vulnerability Levels in Port Harcourt Metropolis Using GIS. J. Earth Sci. Eng. 2011, 2, 617–623. [Google Scholar]
- Vanwambeke, S.O.; Lambin, E.F.; Eichhorn, M.P.; Flasse, S.P.; Harbach, R.E.; Oskam, L.; Somboon, P.; van Beers, S.; van Benthem, B.H.; Walton, C.; et al. Impact of Land-Use Change on Dengue and Malaria in Northern Thailand. EcoHealth 2007, 4, 37–51. [Google Scholar] [CrossRef]
- Uyigue, E.; Agho, M. Coping with Climate Change and Environmental Degradation in the Niger Delta of Southern Nigeria. Community Research and Development, Centre Benin City. Available online: http://priceofoil.org/content/uploads/2007/06/07.06.11%20-%20Climate_Niger_Delta.pdf (accessed on 26 August 2017).
- United Nations Environment Program (UNEP). Environmental Assessment of Ogoniland. Available online: http://postconflict.unep.ch/publications/OEA/UNEP_OEA.pdf (accessed on 29 October 2017).
- Fagbeja, M.A.; Hill, J.; Chatterton, T.; Longhurst, J.; Akinyede, J. Residential-Source Emission Inventory for the Niger Delta—A Methodological Approach. J. Sustain. Dev. 2013, 6, 98–120. [Google Scholar] [CrossRef]
- Ede, P.N. Pollution and the Rivers State Environment. Niger. Res. Rev. 1998, 1, 81–89. [Google Scholar]
- Ede, P.N.; Edokpa, D.O. Regional Air Quality of the Nigeria’s Niger Delta. Open J. Air Pollut. 2015, 4, 7–15. [Google Scholar] [CrossRef]
- Gobo, A.; Richard, G.; Ubong, I. Health Impact of Gas Flares on Igwuruta/Umuechem Communities in Rivers State. J. Appl. Sci. Environ. Manag. 2010, 13, 27–33. [Google Scholar] [CrossRef]
- Agency for Toxic Substances and Diseases Registry (ASTDR). Nitrogen Oxides. Available online: https://www.atsdr.cdc.gov/toxfaqs/tfacts175.pdf (accessed on 24 September 2017).
- Agency for Toxic Substances and Diseases Registry (ASTDR). Interaction Profile for Toxic Substances: Benzene, Toluene, Ethylbenzene and Xylene. Available online: https://www.atsdr.cdc.gov/interactionprofiles/ip05.html (accessed on 24 September 2017).
- Yakubu, O.H. Addressing Environmental Health Problems in Ogoniland through Implementation of United Nations Environment Program Recommendations: Environmental Management Strategies. Environments 2017, 4, 28. [Google Scholar] [CrossRef]
- Okonkwo, S.; Okpala, K.; Opara, M.F. Assessment of Automobile Induced Pollution in an Urban Area (A Case Study of Port-Harcourt City, Rivers State, Nigeria). J. Chem. Proc. Eng. 2014, 25, 12–15. [Google Scholar]
- Weli, E.V. Atmospheric Concentration of Particulate Pollutants and its Implications for Respiratory Health Hazard Management in Port Harcourt Metropolis, Nigeria. Civ. Environ. Res. 2014, 9, 11–17. [Google Scholar]
- Quartz Africa. Four of the World’s Worst-Ranked Cities for Air Quality Are in Nigeria. Available online: https://qz.com/686071/four-of-the-worlds-worst-ranked-countries-for-air-quality-are-in-nigeria/ (accessed on 30 June 2017).
- World Health Organization (WHO). WHO Global Urban Ambient Air Pollution Database (Update 2016). Available online: http://www.who.int/phe/health_topics/outdoorair/databases/cities/en/ (accessed on 30 June 2017).
- United State Environmental Protection Agency (USEPA). Environment and Contaminants: Criteria Air Pollutants. Available online: https://www.epa.gov/sites/production/files/2015-10/documents/ace3_criteria_air_pollutants.pdf (accessed on 6 October 2017).
- American Institute for Conservation of Historic and Artistic Works. The Hidden Hazards of Fire Soot. Available online: http://www.conservation-us.org/docs/default-source/periodicals/2010-09-sept-aicnews.pdf?sfvrsn=6 (accessed on 20 July 2017).
- United States Environmental Protection Agency (USEPA). Particulate Matter (PM) Pollution: Particulate Matter (PM) Basics. Available online: https://www.epa.gov/pm-pollution/particulate-matter-pm-basics#PM (accessed on 14 August 2017).
- World Health Organization. Global Health Risks: Mortality and Burden of Disease Attributable to Select Major Risks; World Health Organization: Geneva, Switzerland, 2009. [Google Scholar]
- Lelieveld, J.; Evans, J.S.; Fnais, M.; Giannadaki, D.; Pozzer, A. The Contribution of Outdoor Air Pollution Sources to Premature Mortality on a Global Scale. Nature 2015, 525, 367–371. [Google Scholar] [CrossRef] [PubMed]
- The State of Alaska, Division of Air Quality- Air Non-Point and Mobile Sources. Particulate Matter- Background Information. Available online: http://dec.alaska.gov/air/anpms/pm/pm_bckgrd.htm (accessed on 2 August 2017).
- United States Environmental Protection Agency (USEPA). Particulate Matter (PM) Pollution: Health and Environmental Effects of Particulate Matter (PM). Available online: https://www.epa.gov/pm-pollution/health-and-environmental-effects-particulate-matter-pm (accessed on 2 August 2017).
- American Lung Association: ‘State of the Air 2017’—Despite Progress, 4 in 10 Americans at Risk from Air Pollution. Available online: http://www.lung.org/about-us/media/top-stories/state-of-the-air-2017.html (accessed on 25 July 2017).
- International Agency for Research on Cancer (IARC). Polynuclear aromatic compounds, Part 4, bitumens, coal-tars and derived products, shale-oils and soots. IARC Monogr. Eval. Carcinog. Risk Chem. Hum. 1985, 35, 1–247. [Google Scholar] [PubMed]
- Evanoff, B.A.; Gustavsson, P.; Hogstedt, C. Mortality and Incidence of Cancer in a Cohort of Swedish Chimney Sweeps: An Extended Follow up Study. Br. J. Ind. Med. 1993, 50, 450–459. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Particle Pollution. Available online: https://www.cdc.gov/air/particulate_matter.html (accessed on 10 August 2017).
- International Agency for Research on Cancer (IARC). Overall evaluations of carcinogenicity: An updating of IARC Monographs volumes 1 to 42. IARC Monogr. Eval. Carcinog. Risk Chem. Hum. Suppl. 1987, 7, 1–440. [Google Scholar] [PubMed]
- Peel, J.L.; Metzger, K.B.; Klein, M.; Flanders, W.D.; Mulholland, J.A.; Tolbert, P.E. Ambient Air Pollution And Cardiovascular Emergency Department Visits In Potentially Sensitive Groups. Am. J. Epidemiol. 2007, 165, 625–633. [Google Scholar] [CrossRef] [PubMed]
- Sun, Q.; Yue, P.; Kirk, R.I.; Wang, A.; Moatti, D.; Jin, X.; Lu, B.; Schecter, A.D.; Lippmann, M.; Gordon, T.; et al. Ambient Air Particulate Matter Exposure And Tissue Factor Expression In Atherosclerosis. Inhal. Toxicol. 2008, 20, 127–137. [Google Scholar] [CrossRef] [PubMed]
- Park, S.K.; O’Neill, M.S.; Vokonas, P.S.; Sparrow, D.; Schwartz, J. Effects Of Air Pollution On Heart Rate Variability: The VA Normative Aging Study. Environ. Health Perspect. 2005, 113, 304–309. [Google Scholar] [CrossRef] [PubMed]
- Bartoli, C.R.; Wellenius, G.A.; Coull, B.A.; Akiyama, I.; Diaz, E.A.; Lawrence, J.; Okabe, K.; Verrier, R.L.; Godleski, J.J. Concentrated Ambient Particles Alter Myocardial Blood Flow during Acute Ischemia in Conscious Canines. Environ. Health Perspect. 2009, 117, 333–337. [Google Scholar] [CrossRef] [PubMed]
- Wellenius, G.A.; Coull, B.A.; Godleski, J.J.; Koutrakis, P.; Okabe, K.; Savage, S.T. Inhalation of Concentrated Ambient Air Particles Exacerbates Myocardial Ischemia in Conscious Dogs. Environ. Health Perspect. 2003, 111, 402–408. [Google Scholar] [CrossRef] [PubMed]
- Pope, C.A., III; Muhlestein, J.B.; May, H.T.; Renlund, D.G.; Anderson, J.L.; Horne, B.D. Ischemic Heart Disease Events Triggered by Short-Term Exposure to Fine Particulate Air Pollution. Circulation 2006, 114, 2443–2448. [Google Scholar] [CrossRef] [PubMed]
- Bateson, T.F.; Schwartz, J. Who Is Sensitive to the Effects of Particulate Air Pollution on Mortality? A Case-Crossover Analysis of Effect Modifiers. Epidemiology 2004, 15, 143–149. [Google Scholar] [CrossRef] [PubMed]
- Lagorio, S.; Forastiere, F.; Pistelli, R.; Iavarone, I.; Michelozzi, P.; Fano, V.; Marconi, A.; Ziemacki, G.; Ostro, B.D. Air Pollution and Lung Function Among Susceptible Adult Subjects: A Panel Study. Environ. Health 2006, 5, 11. [Google Scholar] [CrossRef] [PubMed]
- Trenga, C.A.; Sullivan, J.H.; Schildcrout, J.S.; Shepherd, K.P.; Shapiro, G.G.; Liu, L.J.; Kaufman, J.D.; Koenig, J.Q. Effect of Particulate Air Pollution on Lung Function in Adult and Pediatric Subjects in a Seattle Panel Study. Chest J. 2006, 129, 1614–1622. [Google Scholar] [CrossRef] [PubMed]
- Bennett, W.D.; Zeman, K.L.; Kim, C.; Mascarella, J. Enhanced Deposition of Fine Particles in COPD Patients Spontaneously Breathing at Rest. Inhal. Toxicol. 1997, 9, 1–14. [Google Scholar]
- Brown, J.S.; Zeman, K.L.; Bennett, W.D. Ultrafine Particle Deposition and Clearance in the Healthy and Obstructed Lung. Am. J. Respir. Crit. Care Med. 2002, 166, 1240–1247. [Google Scholar] [CrossRef] [PubMed]
- Gent, J.F.; Triche, E.W.; Holford, T.R.; Belanger, K.; Bracken, M.B.; Beckett, W.S.; Leaderer, B.P. Association of Low-Level Ozone and Fine Particles with Respiratory Symptoms in Children with Asthma. JAMA 2003, 290, 1859–1867. [Google Scholar] [CrossRef] [PubMed]
- Rabinovitch, N.; Strand, M.; Gelfand, E.W. Particulate Levels Are Associated with Early Asthma Worsening in Children with Persistent Disease. Am. J. Respir. Crit. Care Med. 2006, 173, 1098–1105. [Google Scholar] [CrossRef] [PubMed]
- Desqueyroux, H.; Pujet, J.C.; Prosper, M.; Squinazi, F.; Momas, I. Short-Term Effects of Low-Level Air Pollution on Respiratory Health of Adults Suffering from Moderate to Severe Asthma. Environ. Res. 2002, 89, 29–37. [Google Scholar] [CrossRef] [PubMed]
- Gong, H., Jr.; Linn, W.S.; Sioutas, C.; Terrell, S.L.; Clark, K.W.; Anderson, K.R.; Terrell, L.L. Controlled Exposures of Healthy and Asthmatic Volunteers to Concentrated Ambient Fine Particles in Los Angeles. Inhal. Toxicol. 2003, 15, 305–325. [Google Scholar] [CrossRef] [PubMed]
- Host, S.; Larrieu, S.; Pascal, L.; Blanchard, M.; Declercq, C.; Fabre, P. Short-Term Associations Between Fine and Coarse Particles and Hospital Admissions for Cardiorespiratory Diseases in Six French Cities. Occup. Environ. Med. 2007, 65, 544–551. [Google Scholar] [CrossRef] [PubMed]
- Peel, J.L.; Tolbert, P.E.; Klein, M.; Metzger, K.B.; Flanders, W.D.; Knox, T. Ambient Air Pollution and Respiratory Emergency Department Visits. Epidemiology 2005, 16, 164–174. [Google Scholar] [CrossRef] [PubMed]
- Mauad, T.; Rivero, D.H.; de Oliveira, R.C.; Lichtenfels, A.J.; Guimarães, E.T.; de Andre, P.A. Chronic Exposure to Ambient Levels of Urban Particles Affects Mouse Lung Development. Am. J. Respir. Crit. Care Med. 2008, 178, 721–728. [Google Scholar] [CrossRef] [PubMed]
- Pinkerton, K.E.; Zhou, Y.; Zhong, C.; Smith, K.R.; Teague, S.V.; Kennedy, I.M. Mechanisms of Particulate Matter Toxicity in Neonatal and Young Adult Rat Lungs. Res. Rep. Health Eff. Inst. 2008, 135, 3–41. [Google Scholar]
- Sacks, J.D.; Stanek, L.W.; Luben, T.J.; Johns, D.O.; Buckley, B.J.; Brown, J.S.; Ross, M. Particulate Matter–Induced Health Effects: Who Is Susceptible? Environ. Health Perspect. 2011, 119, 446–454. [Google Scholar] [CrossRef] [PubMed]
- Pope, C.; Renlund, D.; Kfoury, A.; May, H.; Horne, B. Relation of Heart Failure Hospitalization to Exposure to Fine Particulate Air Pollution. Am. J. Cardiol. 2008, 102, 1230–1234. [Google Scholar] [CrossRef] [PubMed]
- Larrieu, S.; Jusot, J.F.; Blanchard, M.; Prouvost, H.; Declercq, C.; Fabre, P. Short-Term Effects of Air Pollution on Hospitalizations for Cardiovascular Diseases in Eight French Cities: The PSAS Program. Sci. Total Environ. 2007, 387, 105–112. [Google Scholar] [CrossRef] [PubMed]
- Devlin, R.B.; Ghio, A.J.; Kehrl, H.; Sanders, G.; Cascio, W. Elderly Humans Exposed to Concentrated Air Pollution Particles Have Decreased Heart Rate Variability. Eur. Respir. J. 2003, 40, 76S–80S. [Google Scholar] [CrossRef]
- Fung, K.Y.; Luginaah, I.; Gorey, K.M.; Webster, G. Air Pollution and Daily Hospitalization Rates for Cardiovascular and Respiratory Diseases in London, Ontario. Int. J. Environ. Stud. 2005, 62, 677–685. [Google Scholar] [CrossRef] [PubMed]
- Gong, H., Jr.; Linn, W.S.; Terrell, S.L.; Anderson, K.R.; Clark, K.W.; Sioutas, C. Exposures of Elderly Volunteers with and without Chronic Obstructive Pulmonary Disease (COPD) to Concentrated Ambient Fine Particulate Pollution. Inhal. Toxicol. 2004, 16, 731–744. [Google Scholar] [CrossRef] [PubMed]
- Franklin, M.; Zeka, A.; Schwartz, J. Association between PM2.5 and All-Cause and Specific-Cause Mortality in 27 U.S. Communities. J. Expo. Sci. Environ. Epidemiol. 2007, 17, 279–287. [Google Scholar] [CrossRef] [PubMed]
- Zeka, A.; Zanobetti, A.; Schwartz, J. Individual-Level Modifiers of the Effects of Particulate Matter on Daily Mortality. Am. J. Epidemiol. 2006, 163, 849–859. [Google Scholar] [CrossRef] [PubMed]
- Naess, Ø.; Nafstad, P.; Aamodt, G.; Claussen, B.; Rosland, P. Relation Between Concentration of Air Pollution and Cause Specific Mortality: Four-Year Exposures to Nitrogen Dioxide and Particulate Matter Pollutants in 470 Neighborhoods in Oslo, Norway. Am. J. Epidemiol. 2007, 165, 435–443. [Google Scholar] [CrossRef] [PubMed]
- Dutton, D.B.; Levine, S. Overview, Methodological Critique, and Reformulation. In Pathways to Health; Bunker, J.P., Gomby, D.S., Kehrer, B.H., Eds.; Henry, J. Kaiser Family Foundation: Menlo Park, CA, USA, 1989; pp. 29–69. [Google Scholar]
- Kan, H.; London, S.J.; Chen, G.; Zhang, Y.; Song, G.; Zhao, N.; Jiang, L.; Chen, B. Season, Sex, Age, and Education as Modifiers of the Effects of Outdoor Air Pollution on Daily Mortality in Shanghai, China: The Public Health and Air Pollution in Asia (PAPA) Study. Environ. Health Perspect. 2008, 116, 1183–1188. [Google Scholar] [CrossRef] [PubMed]
- Jerrett, M.; Burnett, R.T.; Brook, J.; Kanaroglou, P.; Giovis, C.; Finkelstein, N.; Hutchison, B. Do Socioeconomic Characteristics Modify the Short-Term Association between Air Pollution and Mortality? Evidence from a Zonal Time Series in Hamilton, Canada. J. Epidemiol. Community Health 2004, 58, 31–40. [Google Scholar] [CrossRef] [PubMed]
- Ostro, B.; Broadwin, R.; Green, S.; Feng, W.Y.; Lipsett, M. Fine Particulate Air Pollution and Mortality in Nine California Counties: Results from CALFINE. Environ. Health Perspect. 2006, 114, 29–33. [Google Scholar] [CrossRef] [PubMed]
- Ostro, B.D.; Feng, W.Y.; Broadwin, R.; Malig, B.J.; Green, R.S.; Lipsett, M.J. The Impact of Components of Fine Particulate Matter on Cardiovascular Mortality in Susceptible Subpopulations. Occup. Environ. Med. 2008, 65, 750–756. [Google Scholar] [CrossRef] [PubMed]
- Finkelstein, M.; Jerrett, M.; DeLuca, P.; Finkelstein, N.; Verma, D.K.; Chapman, K.; Sears, M.R. A Cohort Study of Income, Air Pollution and Mortality. Can. Med. Assoc. J. 2003, 169, 397–402. [Google Scholar]
- Wilson, W.E.; Mar, T.F.; Koenig, J.Q. Influence of Exposure Error and Effect Modification by Socioeconomic Status on the Association of Acute Cardiovascular Mortality with Particulate Matter in Phoenix. J. Expo. Sci. Environ. Epidemiol. 2007, 17, S11–S19. [Google Scholar] [CrossRef] [PubMed]
- Niaja.com. 5 Ways to Live Healthy with the Black Soot Pollution in Port Harcourt. Available online: https://www.naij.com/1089333-5-ways-live-healthy-black-soot-pollution-port-harcourt.html (accessed on 28 July 2017).
- The Guardian. Residents Leave Port Harcourt over Sooth Emission. Available online: https://guardian.ng/features/health/residents-leave-port-harcourt-over-sooth-emission/ (accessed on 29 July 2017).
- Africanews. Nigerians Demonstrate over Soot Pollution. Available online: http://www.africanews.com/2017/02/15/nigerians-demonstrate-over-soot-pollution// (accessed on 26 July 2017).
- The Guardian. Air Pollution: Rivers Resident Decry Invasion by Black Soot. Available online: https://guardian.ng/sunday-magazine/air-pollution-rivers-resident-decry-invasion-by-black-soot/ (accessed on 11 July 2017).
- Global Patriot. FG Declares Air Pollution in Port Harcourt an “Emergency Situation”. Available online: http://globalpatriotnews.com/fg-declares-air-pollution-in-port-harcort-an-emergency-situation/ (accessed on 29 July 2017).
- The Sun. Checking Air Pollution in Port Harcourt. Available online: http://sunnewsonline.com/checking-air-pollution-in-port-harcourt/ (accessed on 29 July 2017).
- Vanguard. Black Soot: 6 Million Rivers Residents Risk Cancer—Specialists. Available online: http://www.vanguardngr.com/2017/02/black-soot-6-million-rivers-residents-risk-cancer-specialists/ (accessed on 28 July 2017).
- Sweet Crude. Nigeria: Cancer Causing Black Soot Assail Port Harcourt, Residents Panic. Available online: http://sweetcrudereports.com/2017/02/11/nigeria-cancer-causing-black-soot-assail-port-harcourt-residents-panic/ (accessed on 12 July 2017).
- Daily Post. Black Soot: Rivers Government Seals Three Companies. Available online: http://dailypost.ng/2017/02/11/black-soot-rivers-government-seals-3-companies/ (accessed on 6 November 2017).
- The Economist. How Nigeria Stopped Ebola. Available online: https://www.economist.com/blogs/economist-explains/2014/10/economist-explains-6 (accessed on 4 August 2017).
- World Health Organization (WHO). Statement on the 1st Meeting of the IHR Emergency Committee on the 2014 Ebola Outbreak in West Africa. Available online: http://www.who.int/mediacentre/news/statements/2014/ebola-20140808/en/ (accessed on 2 July 2017).
- Nigeria Population 2017. World Population Review. Available online: http://worldpopulationreview.com/countries/nigeria-population/ (accessed on 2 July 2017).
- Oleribe, O.O.; Crossey, M.M.E.; Taylor-Robinson, S.D. Nigerian Response to the 2014 Ebola Viral Disease Outbreak: Lessons and Cautions. Pan Afr. Med. J. 2015, 22, 13. [Google Scholar] [PubMed]
- Constitution of the Federal Republic of Nigeria 1999. Available online: http://www.nigeria-law.org/ConstitutionOfTheFederalRepublicOfNigeria.htm#Chapter_2 (accessed on 7 November 2017).
- Environmental Law Research Institute (ELRI). A Synopsis of Laws and Regulations on the Environment in Nigeria. Available online: http://www.elri-ng.org/newsandrelease2.html (accessed on 4 October 2017).
- Environmental Impact Assessment. Decree No 86 of 1992, Laws of the Federation of Nigeria. Available online: http://www.nigerialaw.org/Environmental%20Impact%20Assessment%20Decree%20No.%2086%201992.htm (accessed on 7 November 2017).
- National Environmental Standards and Regulations Enforcement Agency (Establishment) Act, 2007. Available online: http://extwprlegs1.fao.org/docs/pdf/nig120569.pdf (accessed on 7 November 2017).
- Nkwocha, E.E.; Egejuru, R.O. Effects of Industrial Air Pollution on the Respiratory Health of Children. Int. J. Environ. Sci. Technol. 2008, 5, 509–516. [Google Scholar] [CrossRef]
- Onwuchekwa, C.A.; Asekomeh, E.G. Geriatric Admissions in a Developing Country: Experience from a Tertiary Centre in Nigeria. Ethn. Dis. 2009, 19, 359–362. [Google Scholar] [PubMed]
- Index Mundi. Nigerian Age Structure. Available online: http://www.indexmundi.com/nigeria/age_structure.html (accessed on 9 November 2017).
- Weli, E.V.; Adegoke, O.J.; Kpang, B.M. The Epidemiology of Cardio-Vascular Diseases in Relation to the Air Quality of Abattoirs in Port Harcourt, Nigeria. World J Cardiovasc. Dis. 2016, 6, 94–107. [Google Scholar] [CrossRef]
- Amnesty International. Nigeria: Petroleum, Pollution and Poverty in the Niger Delta. Available online: https://www.amnesty.de/files/Amnesty_Bericht_Niger_Delta_09.pdf (accessed on 26 October 2017).

© 2017 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yakubu, O.H. Particle (Soot) Pollution in Port Harcourt Rivers State, Nigeria—Double Air Pollution Burden? Understanding and Tackling Potential Environmental Public Health Impacts. Environments 2018, 5, 2. https://doi.org/10.3390/environments5010002
Yakubu OH. Particle (Soot) Pollution in Port Harcourt Rivers State, Nigeria—Double Air Pollution Burden? Understanding and Tackling Potential Environmental Public Health Impacts. Environments. 2018; 5(1):2. https://doi.org/10.3390/environments5010002
Chicago/Turabian StyleYakubu, Okhumode H. 2018. "Particle (Soot) Pollution in Port Harcourt Rivers State, Nigeria—Double Air Pollution Burden? Understanding and Tackling Potential Environmental Public Health Impacts" Environments 5, no. 1: 2. https://doi.org/10.3390/environments5010002
APA StyleYakubu, O. H. (2018). Particle (Soot) Pollution in Port Harcourt Rivers State, Nigeria—Double Air Pollution Burden? Understanding and Tackling Potential Environmental Public Health Impacts. Environments, 5(1), 2. https://doi.org/10.3390/environments5010002




