Factors Which Influence Owners When Deciding to Use Chemotherapy in Terminally Ill Pets
Simple Summary
Abstract
1. Introduction
Chemotherapy Treatment
2. Method
2.1. Participants
2.2. Survey Design
2.3. Data Analysis
3. Results
4. Discussion
- Physical functioning (physiological, biomechanical and neural parameters, and the ability to perform routine tasks—quantitative assessment),
- Psychological functioning (cognitive abilities, mental health status, mood and personality—quantitative and qualitative assessment). It should be noted these facets are difficult to assess within animals and general behavioral changes may need to be considered to provide a measure of psychological function,
- Social functioning (environmental interaction and relationships—qualitative assessment),
- Role activities (motivation, communication, play and exercise—quantitative and qualitative assessment),
- Overall life satisfaction (enjoyment and fulfilment—qualitative assessment), and,
- Perception of health status (overall rating—quantitative and qualitative assessment).
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Adelstein, D.J.; Saxton, J.P.; Rybicki, L.A.; Esclamado, R.M.; Wood, B.G.; Strome, M.; Lavertu, P.; Lorenz, R.R.; Carroll, M.A. Multiagent concurrent chemoradiotherapy for locoreginally advances squamous cell head and neck cancer: Mature result from a single institution. J. Clin. Oncol. 2006, 24, 1064–1071. [Google Scholar] [CrossRef] [PubMed]
- Wilkowski, R.; Thoma, M.; Weingandt, H.; Duhmke, E.; Heinemann, V. Chemoradiation for ductal pancreatic carcinoma: Principles of combining chemotherapy with radiations, definition of target volume and radiation dose. J. Pancreas 2005, 6, 216–230. [Google Scholar]
- Rakovitch, E.; Tsao, M.; Ung, Y.; Pignol, J.P.; Cheung, P.; Chow, E. Comparison of the efficacy and acute toxicity of weekly versus daily chemoradiotherapy for non-small-cell lung cancer: A meta-analysis. Int. J. Radiat. Oncol. Biol. Phys. 2004, 58, 196–203. [Google Scholar] [CrossRef]
- Macmillian Cancer Support. What Is Chemotherapy? Available online: Https://www.macmillan.org.uk/information-and-support/treating/chemotherapy/chemotherapy-explained/what-is-chemotherapy.html (accessed on 27 January 2016).
- Wolfesberger, B.; Tonar, Z.; Fuchs-Baumgartinger, A.; Walter, I.; Skalicky, M.; Witter, K.; Thalhammer, J.G.; Pagitz, M.; Kleiter, M. Angiogenic markers in canine lymphoma tissues do not predict survival times in chemotherapy treated dogs. Res. Vet. Sci. 2012, 92, 444–450. [Google Scholar] [CrossRef] [PubMed]
- Withrow, S.J. Why worry about cancer in pets? In Withrow and MacEwen’s Small Animal Clinical Oncology, 4th ed.; Withrow, S.J., Vail, D.M., Eds.; Saunders Elsevier: Philadelphia, PA, USA, 2007; pp. xv–xvii. [Google Scholar]
- Dobson, J.M. Introduction: Cancer in cats and dogs. In BSAVA Manual of Canine and Feline Oncology, 3rd ed.; Dobson, J.M., Duncan, B., Lascelles, X., Eds.; British Small Animal Veterinary Association: Guarantee, UK, 2011; pp. 1–5. [Google Scholar]
- Animal Heath Trust Cancer Research. Available online: http://www.aht.org.uk/cms-display/science_oncology.html (accessed on 20 January 2016).
- International Cat Care. Cancer in Cats. Available online: http://icatcare.org/advice/cat-health/cancer-cats (accessed on 20 January 2016).
- Animal Cancer Trust. Types of Cancer. Available online: http://www.animalcancertrust.co.uk/types-of-cancer (accessed on 2 March 2016).
- Wang, S.L.; Lee, I.J.; Liao, A.T. Comparison of efficacy and toxicity of doxorubicin and mitoxantrone in combination of chemotherapy for canine lymphoma. Can. Vet. J. 2016, 57, 271–276. [Google Scholar] [PubMed]
- Pirrone, F.; Pierantoni, L.; Mazzola, S.M.; Vigo, D.; Albertini, M. Owner and animal factors predict the incidence of, and wner reaction towards, problematic behaviours in companion dogs. J. Vet. Behav. Clin. Appl. Res. 2015, 10, 295–301. [Google Scholar] [CrossRef]
- Arkow, P. Application of ethics to animal welfare. Appl. Anim. Behav. Sci. 1998, 59, 193–200. [Google Scholar]
- Royal College of Veterinary Surgeons. Communication and Consent. Available online: http://www.rcvs.org.uk/advice-and-guidance/code-of-professional-conduct-for-veterinary-surgeons/supporting-guidance/communication-and-consent (accessed on 27 January 2016).
- Jacobs, H.H. Ethics in pediatric end-of-life care: A nursing perspective. J. Pediatr. Nurs. 2005, 20, 360–369. [Google Scholar] [CrossRef] [PubMed]
- Wright, A.L.; Zhang, B.; Keating, N.L.; Weeks, J.C.; Prigerson, H.G. Associations between palliative chemotherapy and adult cancer patients’ end of life care and place of death: Prospective cohort study. Br. Med. J. 2014. [Google Scholar] [CrossRef] [PubMed]
- Giuffrida, M.A.; Kerrigan, S.M. Quality of life measurement in prospective studies of cancer treatments in dogs and cats. J. Vet. Intern. Med. 2014, 28, 1824–1829. [Google Scholar] [CrossRef] [PubMed]
- Macdonald, J.; Gray, C. “Informed consent”—How do we get it right? Vet. Nurs. J. 2014, 29, 101–103. [Google Scholar] [CrossRef]
- Wright, I.M. Complications and consent. Equine Vet. Educ. 2014, 26, 292–293. [Google Scholar] [CrossRef]
- Panting, G. Informed consent. Orthop. Trauma 2010, 24, 441–446. [Google Scholar] [CrossRef]
- Hamilton, A. Chemotherapy: What progress in the last 5 years? J. Clin. Oncol. 2005, 23, 1760–1775. [Google Scholar] [CrossRef] [PubMed]
- Cannon, C.; Borgatti, A.; Henson, M.; Husbands, B. Evaluation of a combination chemotherapy protocol including lomustine and doxorubicin in canine histiocytic sarcoma. J. Small Anim. Pract. 2015, 56, 425–429. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, W.; Fossum, T.W.; Kitchell, B.E.; Couto, C.G.; Theilen, G.H. Use of cisplatin for treatment of appendicular osteosarcoma in dogs. J. Am. Vet. Med. Assoc. 1988, 192, 507–511. [Google Scholar] [PubMed]
- Elliott, J.W.; Cripps, P.; Marrington, A.M.; Grant, I.A.; Blackwood, L. Epirubicin as part of a multi-agent chemotherapy protocol for canine lymphoma. Vet. Comp. Oncol. 2013, 11, 185–198. [Google Scholar] [CrossRef] [PubMed]
- Taylor, S.S.; Goodfellow, M.R.; Browne, W.J.; Walding, B.; Murphy, S.; Tzannes, S.; Gerou-Ferriani, M.; Schwartz, A.; Dobson, J.M. Feline extranodal lymphoma: Response to chemotherapy and survival in 110 cats. J. Small Anim. Pract. 2009, 50, 584–592. [Google Scholar] [CrossRef] [PubMed]
- McNeil, C.J.; Sorenmo, K.U.; Shofer, F.S.; Gibeon, L.; Durham, A.C.; Barber, L.G.; Baez, J.L.; Overley, B. Evaluation of adjuvant doxorubicin-based chemotherapy for the treatment of feline mammary carcinoma. J. Vet. Intern. Med. 2009, 23, 123–129. [Google Scholar] [CrossRef] [PubMed]
- Wendelburg, K.M.; Price, L.L.; Burgess, K.E.; Lyons, J.A.; Lew, F.H.; Berg, J. Survival time of dogs with splenic hemangiosarcoma treated by splenectomy with or without adjuvant chemotherapy: 208 cases (2001–2012). J. Am. Vet. Med. Assoc. 2015, 247, 393–403. [Google Scholar] [CrossRef] [PubMed]
- Weeks, J.C.; Catalano, P.J.; Cronin, A.; Finkelman, M.D.; Mack, J.W.; Keating, N.L.; Schrag, D. Patients’ expectations about effects of chemotherapy for advanced cancer. N. Engl. J. Med. 2012, 367, 1616–1625. [Google Scholar] [CrossRef] [PubMed]
- Vols, K.K.; Heden, M.A.; Kristensen, A.T.; Sandoe, P. Quality of life assessment in dogs and cats receiving chemotherapy—A review of current methods. Vet. Comp. Oncol. 2016. [Google Scholar] [CrossRef]
- Boden, E.; Andrews, A. Black’s Veterinary Dictionary (Online); Bloomsbury: London, UK, 2015. [Google Scholar]
- Shehadeh, N.J.; Ensley, J.F.; Kucuk, O.; Black, C.; Yoo, G.H.; Jacobs, J.; Lin, H.S.; Heilbrun, L.K.; Smith, D.; Kim, H. Benefit of postoperative chemoradiotherapy for patients with unknown primary squamous cell carcinoma of the head and neck. Head Neck 2006, 28, 1090–1098. [Google Scholar] [CrossRef] [PubMed]
- Hume, K.R.; Johnson, J.L.; Williams, L.E. Adverse effects of concurrent carboplatin chemotherapy and radiation therapy in dogs. J. Vet. Intern. Med. 2009, 23, 24–30. [Google Scholar] [CrossRef] [PubMed]
- Morrow, G.R.; Roscoe, J.A.; Hickok, J.T.; Andrews, P.L.; Matteson, S. Nausea and emesis: Evidence for a biobehavioural perspective. Support. Care Cancer 2002, 10, 96–105. [Google Scholar] [CrossRef] [PubMed]
- Axiak-Bechtal, S.; Fowler, B.; Yu, D.H.; Amorim, J.; Tsuruta, K.; DeClue, A. Chemotherapy and remission status do not alter pre-existing innate immune dysfunction in dogs with lymphoma. Res. Vet. Sci. 2014, 97, 230–237. [Google Scholar] [CrossRef] [PubMed]
- Lane, A.E.; Black, M.L.; Wyatt, K.M. Toxicity and efficacy of a novel doxorubicin and carboplatin chemotherapy protocol for the treatment of canine appendicular osteosarcoma following limb amputation. Aust. Vet. J. 2012, 90, 69–74. [Google Scholar] [CrossRef] [PubMed]
- Myers, J.S. Cancer and chemotherapy related cognitive changes: The patient experience. Semin. Oncol. Nurs. 2013, 29, 300–307. [Google Scholar] [CrossRef] [PubMed]
- Navari, R.M. 5-HT3 receptors as important mediators of nausea and vomiting due to chemotherapy. Biochim. Biophys. Acta 2015, 1848, 2738–2746. [Google Scholar] [CrossRef] [PubMed]
- Xenoulis, P.G. Nausea: Is it a big “little problem” in animals? Vet. J. 2015, 203, 267. [Google Scholar] [CrossRef] [PubMed]
- Tzannes, S.; Hammond, M.F.; Murphy, S.; Sparks, A.; Blackwood, L. Owners perception of their cats quality of life during COP chemotherapy for lymphoma. J. Feline Med. Surg. 2008, 10, 73–81. [Google Scholar] [CrossRef] [PubMed]
- Belshaw, Z.; Asher, L.; Harvey, N.D.; Dean, R.S. Quality of life assessment in domestic dogs: An evidence-based rapid review. Vet. J. 2015, 206, 203–212. [Google Scholar] [CrossRef] [PubMed]
- Yeates, M.; Main, D. Assessment of companion animal quality of life in veterinary practice and research. J. Small Anim. Pract. 2009, 50, 274–281. [Google Scholar] [CrossRef] [PubMed]
- Lynch, S.; Savary-Bataille, K.; Leeuw, B.; Argyle, D.J. Development of a questionnaire assessing health-related quality-of-life in dogs and cats with cancer. Vet. Comp. Oncol. 2010, 9, 172–182. [Google Scholar] [CrossRef] [PubMed]
- Reynolds, C.A.; Oyama, M.A.; Rush, J.E.; Rozanski, E.A.; Singletary, G.E.; Brown, D.C.; Cunningham, S.M.; Fox, P.R.; Bond, B.; Adin, D.B.; et al. Perceptions of quality of life and priorities of owners of cats with heart disease. J. Vet. Intern. Med. 2010, 24, 1421–1426. [Google Scholar] [CrossRef] [PubMed]
- Hamilton, M.J.; Sarcornrattana, O.; Illiopoulou, M.; Xie, Y.; Kitchell, B. Questionnaire-based assessment of owner concerns and doctor responsiveness: 107 canine chemotherapy patients. J. Small Anim. Pract. 2012, 53, 627–633. [Google Scholar] [CrossRef] [PubMed]
- Finlay, J.; Wyatt, K.; Black, M. Evaluation of the risks of chemotherapy in dogs with thrombocytopenia. Vet. Comp. Oncol. 2017, 15, 151–162. [Google Scholar] [CrossRef] [PubMed]
- Salmons, J. Doing Qualitative Research Online; Sage Publications: London, UK, 2016. [Google Scholar]
- Bruce, I. Questionnaire Design How to Plan, Structure and Write Survey Material for Effective Market Research, 3rd ed.; Kogan Page Limited: New Delhi, India, 2013. [Google Scholar]
- Charmaz, C. Constructing Grounded Theory: A Practical Guide through Qualitative Analysis; Sage Publications: London, UK, 2006. [Google Scholar]
- Li, S.Y.W.; Rakow, T.; Newell, B.R. Personal experience in doctor and patient decision making: From psychology to medicine. J. Eval. Clin. Pract. 2009, 15, 993–995. [Google Scholar] [CrossRef] [PubMed]
- Karimian, Z.; Kojuri, J.; Sagheb, M.M.; Mahboudi, A.; Saber, M.; Amini, M.; Dehghani, M.R. Comparison of residents’ approaches to clinical decisions before and after the implementation of evidence based medicine course. J. Adv. Med. Educ. Prof. 2013, 2, 170–175. [Google Scholar]
- Roykenes, K. “My math and me”: Nursing students’ previous experiences in learning mathematics. Nurse Educ. Pract. 2016, 16, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Wisk, T.M. Informed consent. Plast. Surg. Nurse 2006, 26, 203. [Google Scholar] [CrossRef]
- Sinding, C.; Hudak, P.; Wiernikowski, J.; Aronson, J.; Miller, P.; Gould, J.; Fitzpatrick-Lewis, D. “I like to be an informed person but...” negotiating responsibility for treatment decisions in cancer care. Soc. Sci. Med. 2010, 71, 1094–1101. [Google Scholar] [CrossRef] [PubMed]
- Oostendorp, L.J.M.; Ottevanger, P.B.; Van De Wouw, A.J.; Honkoop, A.H.; Los, M.; Van Der Graaf, W.T.A.; Stalmeier, P.F.M. Patients’ preferences for information about the benefits and risks of second-line palliative chemotherapy and their oncologist’s awareness of these preferences. J. Cancer Educ. 2016, 31, 443–448. [Google Scholar] [CrossRef] [PubMed]
- Crosby, R.D.; Kalotkin, R.L.; Williams, R. Defining clinically meaningful change in health related quality of life. J. Clin. Epidemiol. 2003, 56, 395–407. [Google Scholar] [CrossRef]
- Brooks, R. EuroQoL the current state of play. Health Policy 1996, 37, 53–72. [Google Scholar] [CrossRef]
- Bergner, M.; Bobbit, R.A.; Carter, C.A. The sickness impact profile: Development and final revision of a health status measure. Med. Care 1981, 19, 787–803. [Google Scholar] [CrossRef] [PubMed]
- Ware, J.E.; Sherbourne, C.D. The MOS short form health survey (SF-36). Med. Care 1992, 30, 473–483. [Google Scholar] [CrossRef] [PubMed]
- De Haes, J.L.J.M.; Olscheski, M.; Fayers, P.M. Measuring Quality of Life of Cancer Patients with the Rotterdam Symptom Checklist (RSCL): A Manual; Groningen Northern Centre for Health Care Research: Groningen, The Netherlands, 1996. [Google Scholar]
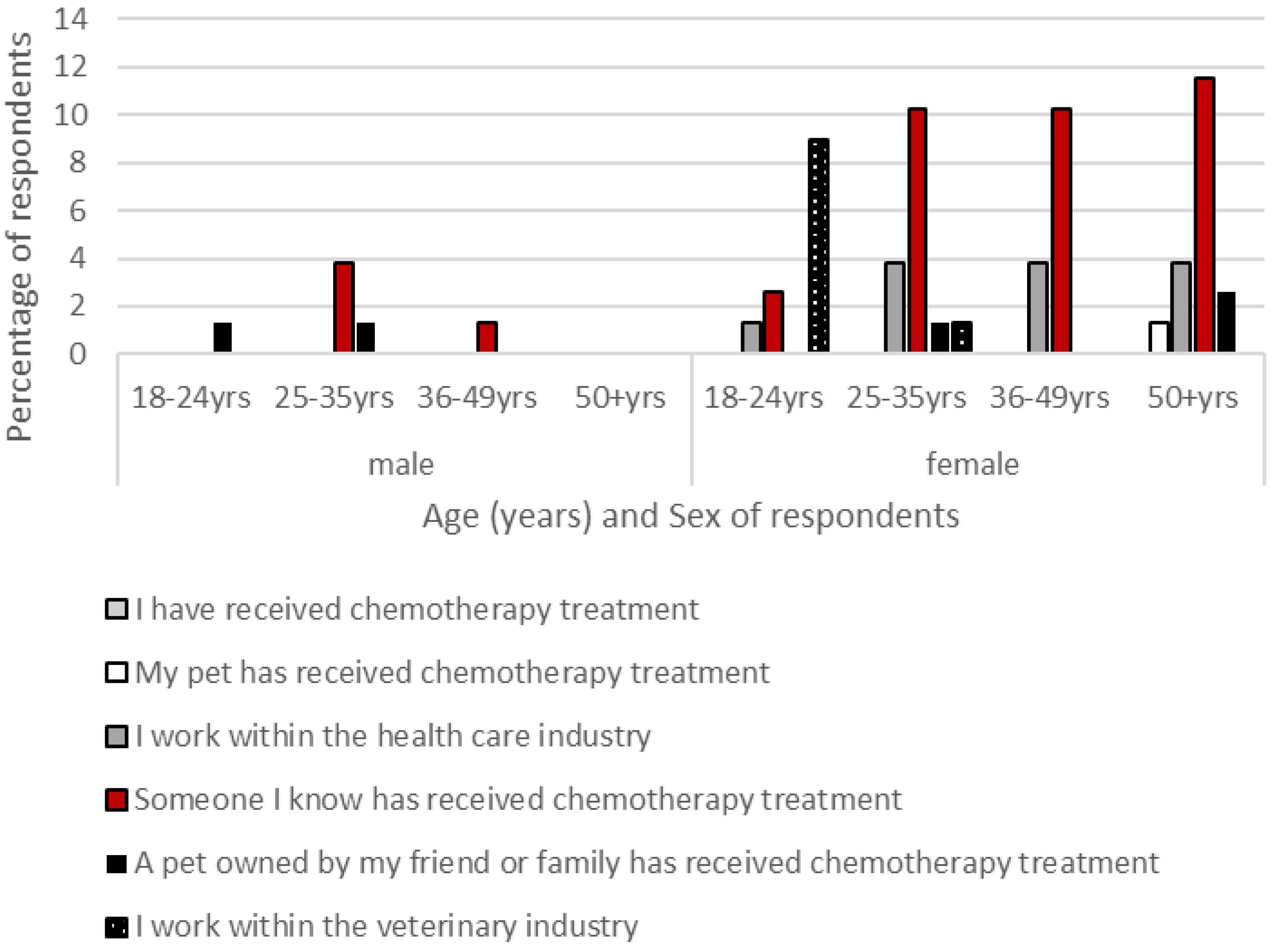
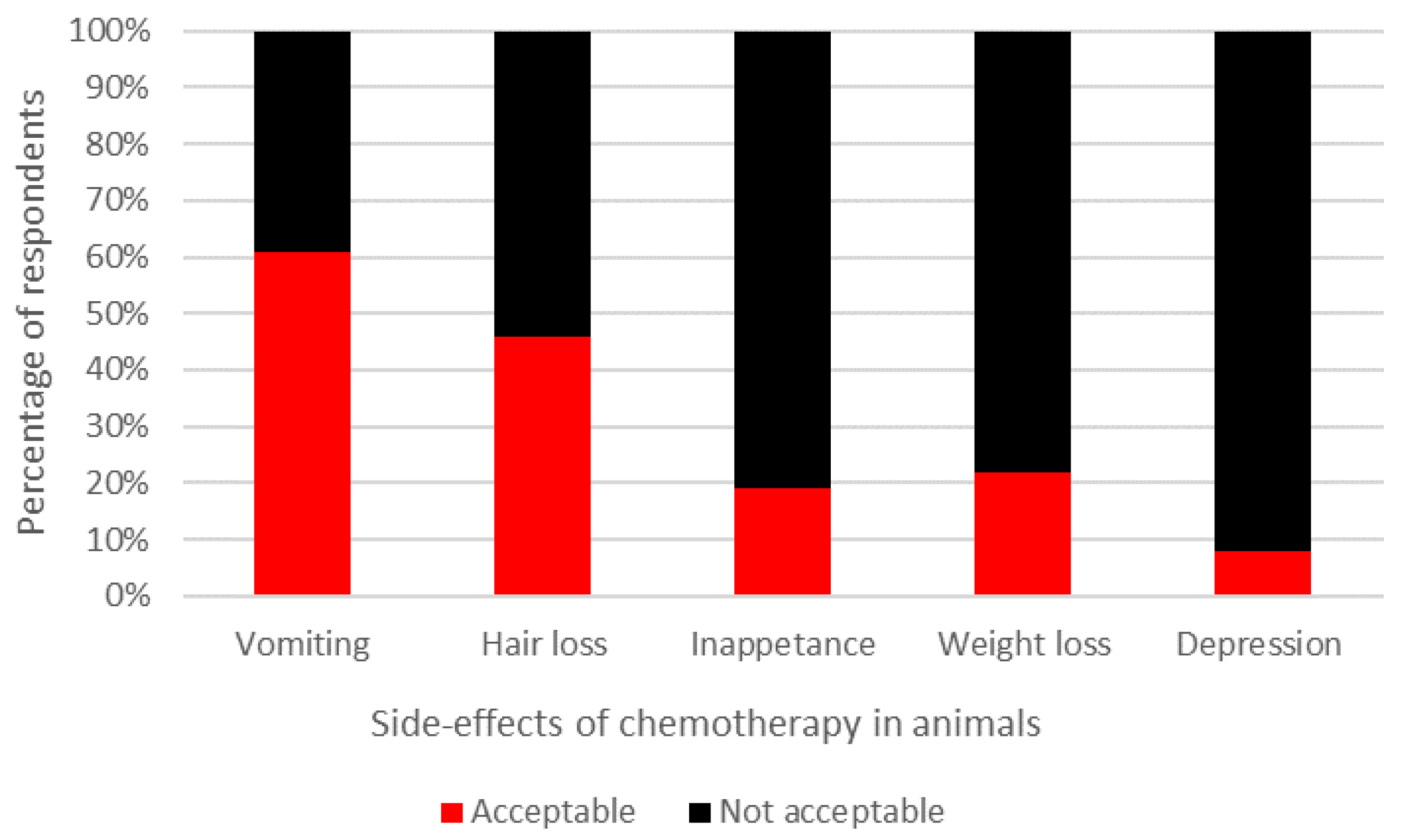
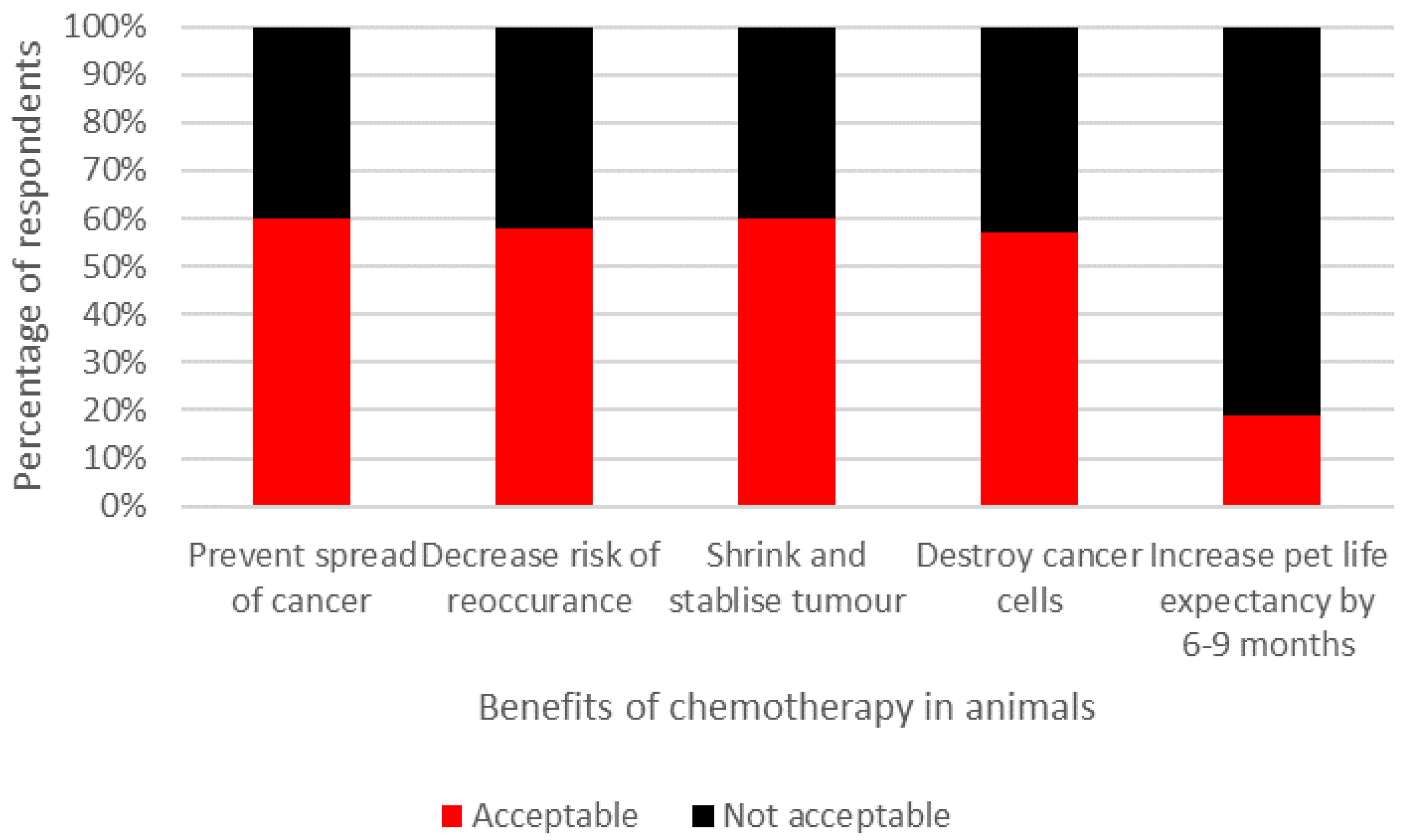
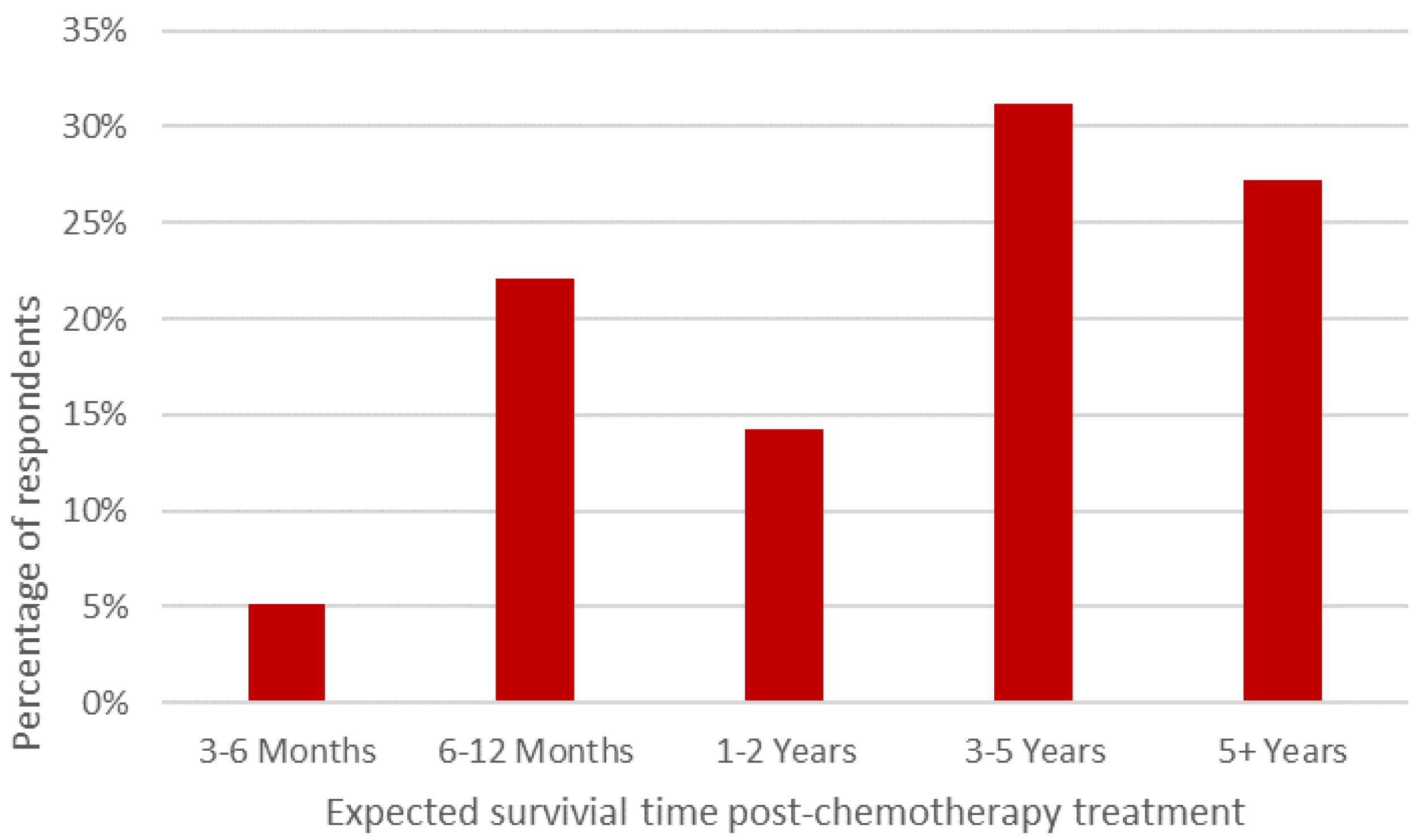
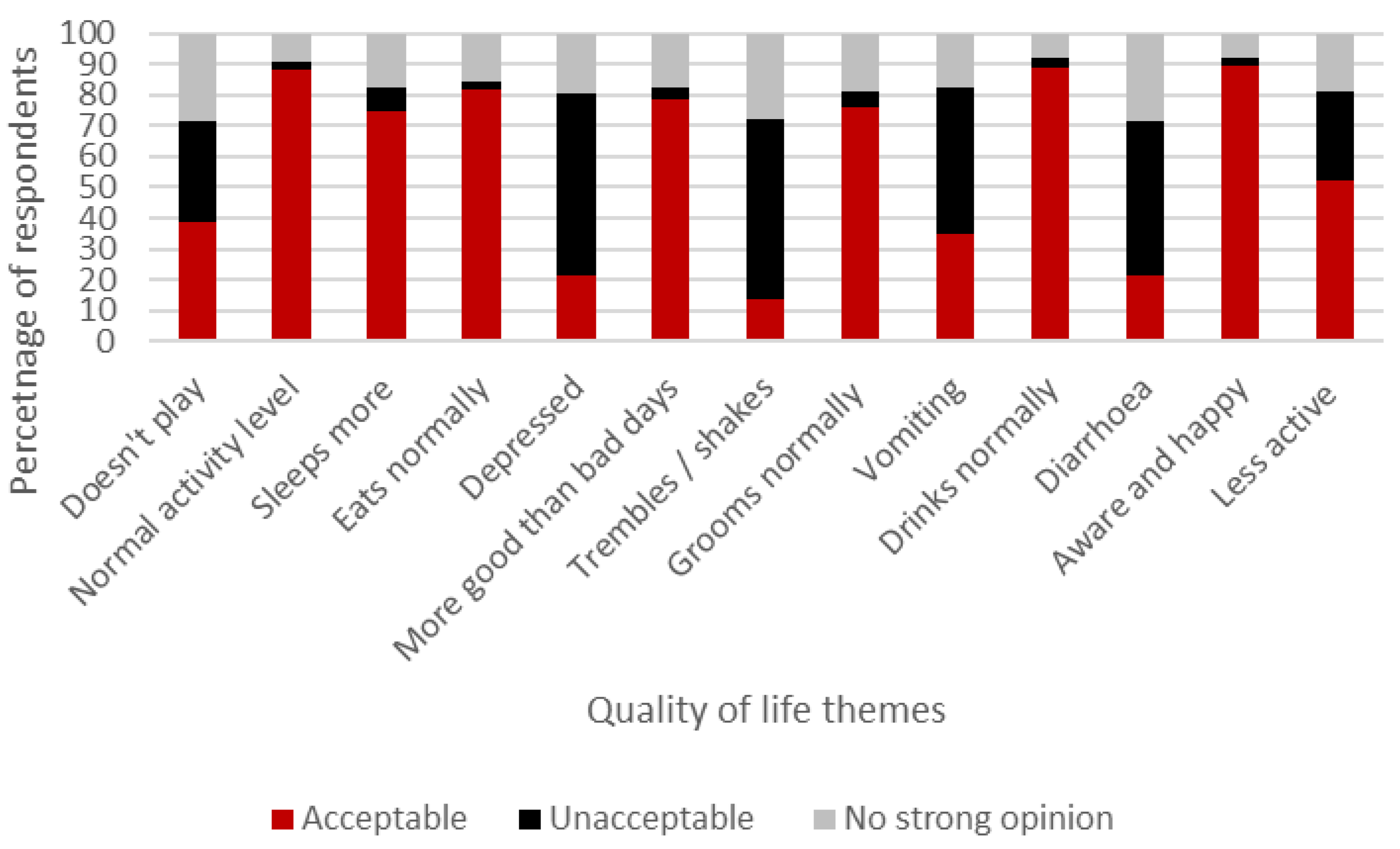
| Participants Were Asked to Rate if They Found the Potential Impact of Chemotherapy in Animals, for the Questions Listed, as Acceptable or Unacceptable. |
|---|
| My pet does not play during chemotherapy |
| My pet’s activity is the same during chemotherapy |
| My pet sleeps more than usual during chemotherapy |
| My pet eats normally during chemotherapy |
| My pets seem depressed during chemotherapy |
| My pet has more good days then bad during chemotherapy |
| My pet trembles and shakes occasionally during chemotherapy |
| My pet grooms normally during chemotherapy |
| My pet experiences vomiting during chemotherapy |
| My pet drinks normal amounts during chemotherapy |
| My pet has diarrhoea during chemotherapy |
| My pet is aware and happy when I’m present during chemotherapy |
| My pet is less active during chemotherapy |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Williams, J.; Phillips, C.; Byrd, H.M. Factors Which Influence Owners When Deciding to Use Chemotherapy in Terminally Ill Pets. Animals 2017, 7, 18. https://doi.org/10.3390/ani7030018
Williams J, Phillips C, Byrd HM. Factors Which Influence Owners When Deciding to Use Chemotherapy in Terminally Ill Pets. Animals. 2017; 7(3):18. https://doi.org/10.3390/ani7030018
Chicago/Turabian StyleWilliams, Jane, Catherine Phillips, and Hollie Marie Byrd. 2017. "Factors Which Influence Owners When Deciding to Use Chemotherapy in Terminally Ill Pets" Animals 7, no. 3: 18. https://doi.org/10.3390/ani7030018
APA StyleWilliams, J., Phillips, C., & Byrd, H. M. (2017). Factors Which Influence Owners When Deciding to Use Chemotherapy in Terminally Ill Pets. Animals, 7(3), 18. https://doi.org/10.3390/ani7030018





