Prevalence and Subtype Distribution of Blastocystis sp. in Senegalese School Children
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethics Approval
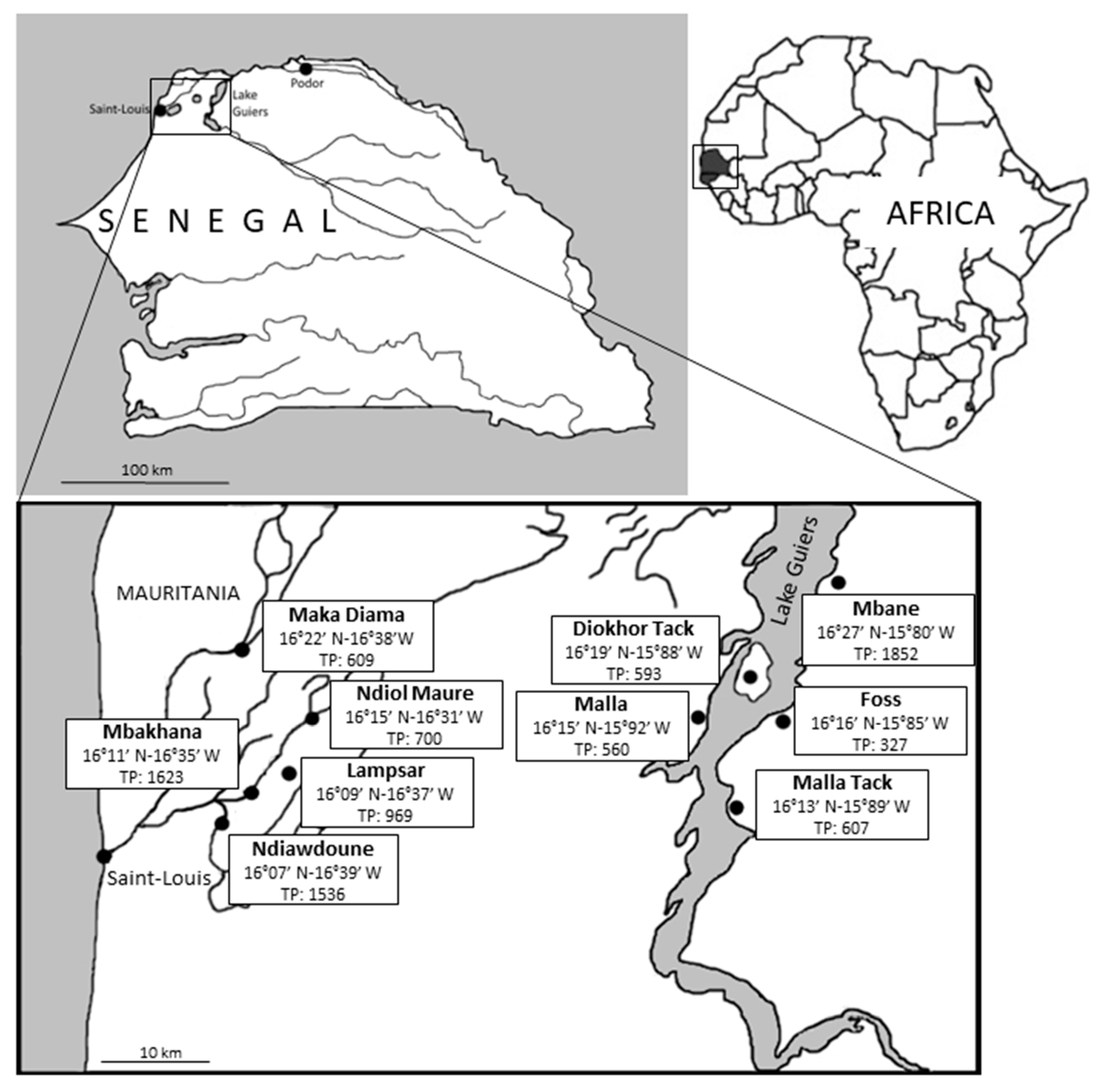
2.2. Sampling Sites
2.3. Cohort and Collection of Samples
2.4. DNA Extraction and Molecular Subtyping of Blastocystis sp. Isolates
2.5. Statistical Analysis
3. Results
Prevalence of Blastocystis sp. in the Cohort of Senegalese School Children
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Boreham, P.F.L.; Stenzel, D.J. Blastocystis in humans and animals: Morphology, biology, and epizootiology. Adv. Parasitol. 1993, 32, 1–70. [Google Scholar] [PubMed]
- Tan, K.S.W. Blastocystis in humans and animals: New insights using modern methodologies. Vet. Parasitol. 2004, 126, 121–144. [Google Scholar] [CrossRef]
- Yoshikawa, H.; Koyama, Y.; Tsuchiya, E.; Takami, K. Blastocystis phylogeny among various isolates from humans to insects. Parasitol. Int. 2016, 65, 750–759. [Google Scholar] [CrossRef] [PubMed]
- Cian, A.; El Safadi, D.; Osman, M.; Moriniere, R.; Gantois, N.; Benamrouz-Vanneste, S.; Delgado-Viscogliosi, P.; Guyot, K.; Li, L.L.; Monchy, S.; et al. Molecular epidemiology of Blastocystis sp. in various animal groups from two French zoos and evaluation of potential zoonotic risk. PLoS ONE 2017, 12, e0169659. [Google Scholar] [CrossRef] [PubMed]
- Tan, K.S.W. New insights on classification, identification, and clinical relevance of Blastocystis spp. Clin. Microbiol. Rev. 2008, 21, 639–665. [Google Scholar] [CrossRef]
- Scanlan, P.D.; Stensvold, C.R. Blastocystis: Getting to grips with our guileful guest. Trends Parasitol. 2013, 29, 523–529. [Google Scholar] [CrossRef]
- Yoshikawa, H.; Yoshida, K.; Nakajima, A.; Yamanari, K.; Iwatani, S.; Kimata, I. Fecal-oral transmission of the cyst form of Blastocystis hominis in rats. Parasitol. Res. 2004, 94, 391–396. [Google Scholar] [CrossRef]
- El Safadi, D.; Cian, A.; Nourrisson, C.; Pereira, B.; Morelle, C.; Bastien, P.; Bellanger, A.P.; Botterel, F.; Candolfi, E.; Desoubeaux, G.; et al. Prevalence, risk factors for infection and subtype distribution of the intestinal parasite Blastocystis sp. from a large-scale multi-center study in France. BMC Infect. Dis. 2016, 16, 451. [Google Scholar] [CrossRef]
- Menu, E.; Mary, C.; Toga, I.; Raoult, D.; Ranque, S.; Bittar, F. A hospital qPCR-based survey of 10 gastrointestinal parasites in routine diagnostic screening, Marseille, France. Epidemiol. Infect. 2019, 147, e100. [Google Scholar] [CrossRef]
- Bart, A.; Wentink-Bonnema, E.M.S.; Gilis, H.; Verhaar, N.; Wassenaar, C.J.A.; van Vugt, M.; Goorhuis, A.; Van Gool, T. Diagnosis and subtype analysis of Blastocystis sp. in 442 patients in a hospital setting in the Netherlands. BMC Infect. Dis. 2013, 13, 389. [Google Scholar] [CrossRef]
- Muadica, A.S.; Köster, P.C.; Dashti, A.; Bailo, B.; Hernandez-de-Mingo, M.; Reh, L.; Balasegaram, S.; Verlander, N.Q.; Ruiz Chercoles, E.; Carmena, D. Molecular diversity of Giardia duodenalis, Cryptosporidium spp. and Blastocystis sp. in asymptomatic school children in Leganés, Madrid (Spain). Microorganisms 2020, 8, 466. [Google Scholar] [CrossRef] [PubMed]
- El Safadi, D.; Gaayeb, L.; Meloni, D.; Cian, A.; Poirier, P.; Wawrzyniak, I.; Delbac, F.; Dabboussi, F.; Delhaes, L.; Seck, M.; et al. Children of Senegal River Basin show the highest prevalence of Blastocystis sp. ever observed worldwide. BMC Infect. Dis. 2014, 14, 164. [Google Scholar] [CrossRef] [PubMed]
- Lokmer, A.; Cian, A.; Froment, A.; Gantois, N.; Viscogliosi, E.; Chabé, M.; Ségurel, L. Use of shotgun metagenomics for the identification of protozoa in the gut microbiota of healthy individuals from worldwide populations with various industrialization levels. PLoS ONE 2019, 14, e0211139. [Google Scholar] [CrossRef] [PubMed]
- Osman, M.; El Safadi, D.; Cian, A.; Benamrouz, S.; Nourrisson, C.; Poirier, P.; Pereira, B.; Razakandrainibe, R.; Pinon, A.; Lambert, C.; et al. Prevalence and risk factors for intestinal protozoan infections with Cryptosporidium, Giardia, Blastocystis and Dientamoeba among schoolchildren in Tripoli, Lebanon. PLoS Negl. Trop. Dis. 2016, 10, e0004496. [Google Scholar]
- Noradilah, S.A.; Moktar, N.; Anuar, T.S.; Lee, I.L.; Salleh, F.M.; Manap, S.N.A.A.; Mohtar, N.S.H.M.; Azrul, S.M.; Abdullah, W.O.; Nordin, A.; et al. Molecular epidemiology of blastocystosis in Malaysia: Does seasonal variation play an important role in determining the distribution and risk factors of Blastocystis subtype infections in the Aboriginal community? Parasit. Vectors 2017, 10, 360. [Google Scholar] [CrossRef] [PubMed]
- Rojas-Velazquez, L.; Maloney, J.G.; Molokin, A.; Moran, P.; Serrano-Vazquez, A.; Gonzalez, E.; Perez-Juarez, H.; Ximenez, C.; Santin, M. Use of next-generation amplicon sequencing to study Blastocystis genetic diversity in a rural human population from Mexico. Parasit. Vectors 2019, 12, 566. [Google Scholar] [CrossRef]
- Higuera, A.; Villamizar, X.; Herrera, G.; Giraldo, J.C.; Vasquez-A, L.R.; Urbano, P.; Villalobos, O.; Tovar, C.; Ramirez, J.D. Molecular detection and genotyping of intestinal protozoa from different biogeographical regions of Colombia. PeerJ 2020, 8, e8554. [Google Scholar] [CrossRef]
- Clark, C.G.; van der Giezen, M.; Alfellani, M.A.; Stensvold, C.R. Recent developments in Blastocystis research. Adv. Parasitol. 2013, 82, 1–32. [Google Scholar]
- Stensvold, C.R.; Clark, C.G. Current status of Blastocystis: A personal view. Parasitol. Int. 2016, 65, 763–771. [Google Scholar] [CrossRef]
- Kurt, Ö.; Dogruman Al, F.; Tanyüksel, M. Eradication of Blastocystis in humans: Really necessary for all? Parasitol. Int. 2016, 65, 797–801. [Google Scholar] [CrossRef]
- Fréalle, E.; El Safadi, D.; Cian, A.; Aubry, E.; Certad, G.; Osman, M.; Wacrenier, A.; Dutoit, E.; Creusy, C.; Dubos, F.; et al. Acute Blastocystis-associated appendicular peritonitis in a child, Casablanca, Morocco. Emerg. Infect. Dis. 2015, 21, 91–94. [Google Scholar] [CrossRef] [PubMed]
- Lepczynska, M.; Chen, W.C.; Dzika, E. Mysterious chronic urticarial caused by Blastocystis spp.? Int. J. Derm. 2015, 55, 259–266. [Google Scholar] [CrossRef]
- Ajjampur, S.S.; Tan, K.S.W. Pathogenic mechanisms in Blastocystis spp.-Interpreting results from in vitro and in vivo studies. Parasitol. Int. 2016, 65, 772–779. [Google Scholar] [CrossRef] [PubMed]
- Noël, C.; Dufernez, F.; Gerbod, D.; Edgcomb, V.P.; Delgado-Viscogliosi, P.; Ho, L.C.; Singh, M.; Wintjens, R.; Sogin, M.L.; Capron, M.; et al. Molecular phylogenies of Blastocystis isolates from different hosts: Implications for genetic diversity, identification of species, and zoonosis. J. Clin. Microbiol. 2005, 43, 348–355. [Google Scholar] [CrossRef] [PubMed]
- Stensvold, C.R.; Suresh, G.K.; Tan, K.S.; Thompson, R.C.; Traub, R.J.; Viscogliosi, E.; Yoshikawa, H.; Clark, C.G. Terminology for Blastocystis subtypes a consensus. Trends Parasitol. 2007, 23, 93–96. [Google Scholar] [CrossRef] [PubMed]
- Alfellani, M.A.; Taner-Mulla, D.; Jacob, A.S.; Imeede, C.A.; Yoshikawa, H.; Stensvold, C.R.; Clark, C.G. Genetic diversity of Blastocystis in livestock and zoo animals. Protist 2013, 164, 497–509. [Google Scholar] [CrossRef]
- Zhao, G.H.; Hu, X.F.; Liu, T.L.; Hu, R.S.; Yu, Z.Q.; Yang, W.B.; Wu, Y.L.; Yu, S.K.; Song, J.K. Molecular characterization of Blastocystis sp. in captive wild animals in Qinling Mountains. Parasitol. Res. 2017, 116, 2327–2333. [Google Scholar] [CrossRef]
- Maloney, J.G.; Lombard, J.E.; Urie, N.J.; Shivley, C.B.; Santin, M. Zoonotic and genetically diverse subtypes of Blastocystis in US preweaned dairy heifer calves. Parasitol. Res. 2019, 118, 575–582. [Google Scholar] [CrossRef]
- Stensvold, C.R.; Clark, C.G. Pre-empting Pandora’box: Blastocystis subtypes revisited. Trends Parasitol. 2020, 36, 229–232. [Google Scholar] [CrossRef]
- Gantois, N.; Lamot, A.; Seesao, Y.; Creusy, C.; Li, L.L.; Monchy, S.; Benamrouz-Vanneste, S.; Karpouzopoulos, J.; Bourgain, J.L.; Rault, C.; et al. First report on the prevalence and subtype distribution of Blastocystis sp. in edible marine fish and marine mammals: A large-scale study conducted in Atlantic Northeast and on the coasts of Northern France. Microorganisms 2020, 8, 460. [Google Scholar] [CrossRef]
- Alfellani, M.A.; Stensvold, C.R.; Vidal-Lapiedra, A.; Onuoha, E.S.; Fagbenro-Beyioku, A.F.; Clark, C.G. Variable geographic distribution of Blastocystis subtypes and its potential implications. Acta Trop. 2013, 126, 11–18. [Google Scholar] [CrossRef] [PubMed]
- Ramírez, J.D.; Sánchez, A.; Hernández, C.; Florez, C.; Bernal, M.C.; Giraldo, J.C.; Reyes, P.; Lopez, M.C.; Garcia, L.; Cooper, P.J.; et al. Geographic distribution of human Blastocystis subtypes in South America. Infect. Genet. Evol. 2016, 41, 32–35. [Google Scholar] [CrossRef] [PubMed]
- Stensvold, C.R.; Alfellani, M.A.; Norskov-Lauritsen, S.; Prip, K.; Victory, E.L.; Maddox, C.; Nielsen, H.V.; Clark, C.G. Subtype distribution of Blastocystis isolates from synanthropic and zoo animals and identification of a new subtype. Int. J. Parasitol. 2009, 39, 473–479. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Owen, H.; Traub, R.J.; Cuttell, L.; Inpankaew, T.; Bielefeldt-Ohmann, H. Molecular epidemiology of Blastocystis in pigs and their in-contact humans in Southeast Queensland, Australia, and Cambodia. Vet. Parasitol. 2014, 203, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Greige, S.; El Safadi, D.; Bécu, N.; Gantois, N.; Pereira, B.; Chabé, M.; Benamrouz-Vanneste, S.; Certad, G.; El Hage, R.; Chemaly, M.; et al. Prevalence and subtype distribution of Blastocystis sp. isolates from poultry in Lebanon and evidence of zoonotic potential. Parasit. Vectors 2018, 11, 389. [Google Scholar] [CrossRef] [PubMed]
- Souppart, L.; Moussa, H.; Cian, A.; Sanciu, G.; Poirier, P.; El Alaoui, H.; Delbac, F.; Boorom, K.; Delhaes, L.; Dei-Cas, E.; et al. Subtype analysis of Blastocystis isolates from symptomatic patients in Egypt. Parasitol. Res. 2010, 106, 505–511. [Google Scholar] [CrossRef]
- Poulsen, C.S.; Efunshile, A.; Nelson, J.A.; Stensvold, C.R. Epidemiological aspects of Blastocystis colonization in children in Ilero, Nigeria. Am. J. Trop. Med. Hyg. 2016, 95, 175–179. [Google Scholar] [CrossRef]
- D’Alfonso, R.; Santoro, M.; Essi, D.; Monsia, A.; Kaboré, Y.; Glé, C.; Di Cave, D.; Sorge, R.P.; Di Cristianzano, V.; Berrilli, F. Blastocystis in Côte d’Ivoire: Molecular identification and epidemiological data. Eur. J. Clin. Microbiol. Infect. Dis. 2017, 36, 2243–2250. [Google Scholar] [CrossRef]
- Poirier, P.; Wawrzyniak, I.; Albert, A.; El Alaoui, H.; Delbac, F.; Livrelli, V. Development and evaluation of a real-time PCR assay for detection and quantification of Blastocystis parasites in human stool samples: Prospective study of patients with hematological malignancies. J. Clin. Microbiol. 2011, 49, 975–983. [Google Scholar] [CrossRef]
- Stensvold, C.R.; Alfellani, M.; Clark, C.G. Levels of genetic diversity vary dramatically between Blastocystis subtypes. Infect. Genet. Evol. 2012, 12, 263–273. [Google Scholar] [CrossRef]
- Forsell, J.; Granlund, M.; Samuelsson, L.; Koskiniemi, S.; Edebro, H.; Evengard, B. High occurrence of Blastocystis sp. subtypes 1–3 and Giardia intestinalis assemblage B among patients in Zanzibar, Tanzania. Parasit. Vectors 2016, 9, 370. [Google Scholar] [CrossRef] [PubMed]
- Dacal, E.; Saugar, J.M.; de Lucio, A.; Hernandez-de-Mingo, M.; Robinson, E.; Köster, P.C.; Aznar-Ruiz-de-Alegria, M.L.; Espasa, M.; Ninda, A.; Gandasegui, J.; et al. Prevalence and molecular characterization of Strongyloides stercoralis, Giardia duodenalis, Cryptosporidium spp., and Blastocystis spp. isolates in school children in Cubal, Western Angola. Parasit. Vectors 2018, 11, 67. [Google Scholar] [CrossRef]
- Beghini, F.; Pasolli, E.; Truong, T.D.; Putignani, L.; Caccio, S.M.; Segata, N. Large-scale comparative metagenomics of Blastocystis, a common member of the human gut microbiome. Isme J. 2017, 11, 2848–2863. [Google Scholar] [CrossRef] [PubMed]
- Greigert, V.; Abou-Bacar, A.; Brunet, J.; Nourrisson, C.; Pfaff, A.W.; Benarbia, L.; Pereira, B.; Randrianarivelojosia, M.; Razafindrakoto, J.-L.; Rakotomalala, R.S.; et al. Human intestinal parasites in Mahajanga, Madagascar: The kingdom of the protozoa. PLoS ONE 2018, 13, e0204576. [Google Scholar] [CrossRef]
- Lebba, V.; Santangelo, F.; Totino, V.; Pantanella, F.; Monsia, A.; Di Cristanziano, V.; Di Cave, D.; Schippa, S.; Berrilli, F.; D’Alfonso, R. Gut microbiota related to Giardia duodenalis, Entamoeba spp. and Blastocystis hominis infections in humans from Côte d’Ivoire. J. Infect. Dev. Ctries. 2016, 10, 1035–1041. [Google Scholar]
- Kodio, A.; Coulibaly, D.; Kassoum Koné, A.; Konaté, S.; Doumbo, S.; Guindo, A.; Bittar, F.; Gouriet, F.; Raoult, D.; Aly Thera, M.; et al. Blastocystis colonization is associated with increased diversity and altered gut bacterial communities in healthy Malian children. Microorganisms 2019, 7, 649. [Google Scholar] [CrossRef] [PubMed]
- Ben Abda, I.; Maatoug, N.; Ben Romdhane, R.; Bouhelmi, N.; Zallegua, N.; Aoun, K.; Viscogliosi, E.; Bouratbine, A. Prevalence and subtype identification of Blastocystis sp. in healthy individuals in the Tunis area, Tunisia. Am. J. Trop. Med. Hyg. 2017, 96, 202–204. [Google Scholar] [CrossRef][Green Version]
- Abdulsalam, A.M.; Ithoi, I.; Al-Mekhlafi, H.M.; Al-Mekhlafi, A.M.; Ahmed, A.; Surin, J. Subtype distribution of Blastocystis isolates in Sebha, Libya. PLoS ONE 2013, 8, e84372. [Google Scholar] [CrossRef]
- El Deeb, H.K.; Khodeer, S. Blastocystis spp.: Frequency and subtype distribution in iron deficiency anemic versus non-anemic subjects from Egypt. J. Parasitol. 2013, 99, 599–602. [Google Scholar] [CrossRef]
- Fouad, S.A.; Basyoni, M.M.A.; Fahmy, R.A.; Kobaisi, M.H. The pathogenic role of different Blastocystis hominis genotypes isolated from patients with irritable bowel syndrome. ArabJ. Gastroenterol. 2011, 12, 194–200. [Google Scholar] [CrossRef]
- Hameed, D.M.A.; Hassanin, O.M.; Zuel-Fakkar, N.M. Association of Blastocystis hominis genetic subtypes with urticaria. Parasitol. Res. 2011, 108, 553–560. [Google Scholar] [CrossRef] [PubMed]
- Hussein, E.M.; Hussein, A.M.; Eida, M.M.; Atwa, M.M. Pathophysiological variability of different genotypes of human Blastocystis hominis Egyptian isolates in experimentally infected rats. Parasitol. Res. 2008, 102, 853–860. [Google Scholar] [CrossRef] [PubMed]
- Petrasova, J.; Uzlikova, M.; Kostka, M.; Petrzelkova, K.J.; Huffman, M.A.; Modry, D. Diversity and host specificity of Blastocystis in syntopic primates on Rubondo Island, Tanzania. Int. J. Parasitol. 2011, 41, 1113–1120. [Google Scholar] [CrossRef] [PubMed]
- Remy, M.; Sondaz, D.; Philip, J.; Calvet, F.; Daoud, W. Drainage basin of the Senegal River, sanitary conditions in 2010. Part I: Illnesses directly linked to the water. Médecine Trop. Revue Corps Santé Colonial 2011, 71, 123–128. [Google Scholar]
- Zhu, W.; Tao, W.; Gong, B.; Yang, H.; Li, Y.; Song, M.; Lu, Y.; Li, W. First report of Blastocystis infections in cattle in China. Vet. Parasitol. 2017, 246, 38–42. [Google Scholar] [CrossRef]
- Greige, S.; El Safadi, D.; Khaled, S.; Gantois, N.; Baydoun, M.; Chemaly, M.; Benamrouz-Vanneste, S.; Chabé, M.; Osman, M.; Certad, G.; et al. First report on the prevalence and subtype distribution of Blastocystis sp. in dairy cattle in Lebanon and assessment of zoonotic transmission. Acta Trop. 2019, 194, 23–29. [Google Scholar] [CrossRef]
- Noradilah, S.A.; Lee, I.L.; Anuar, T.S.; Salleh, F.M.; Abdul Manap, S.N.; Mohd Mohtar, N.S.; Azrul, S.M.; Abdullah, W.O.; Moktar, N. Occurrence of Blastocystis sp. in water catchments at Malay villages and Aboriginal settlement during wet and dry seasons in Peninsular Malaysia. Peerj 2016, 4, e2541. [Google Scholar] [CrossRef]
- Qi, M.; Wei, Z.; Zhang, Y.; Zhang, Q.; Li, J.; Zhang, L.; Wang, R. Genetic diversity of Blastocystis in kindergarten children in southern Xinjiang, China. Parasit. Vectors 2020, 13, 15. [Google Scholar] [CrossRef]
- Ramirez, J.D.; Florez, C.; Olivera, M.; Bernal, M.C.; Giraldo, J.C. Blastocystis subtyping and its association with intestinal parasites in children from different geographical regions of Colombia. PLoS ONE 2017, 12, e0172586. [Google Scholar] [CrossRef]

| Villages | Water Sources and Usage |
|---|---|
| Area of Saint-Louis | |
| Maka Diama | Tap water a (Drinking, washing, domestic activities b) |
| Senegal River (Domestic activities b, bathing, irrigating crops) | |
| Ndiol Maure | Tap water a (Drinking, washing, domestic activities b) |
| Lampsar River (Domestic activities b, bathing, irrigating crops) | |
| Lampsar | Tap water a (Drinking, washing, domestic activities b) |
| Lampsar River (Domestic activities b, bathing, irrigating crops) | |
| Mbakhana | Tap water a (Drinking, washing, domestic activities b) |
| Lampsar River (Domestic activities b, bathing, irrigating crops) | |
| Ndiawdoune | Tap water a (Drinking, washing, domestic activities b) |
| Ngalam River (Domestic activities b, bathing, irrigating crops) | |
| Area of Lake Guiers | |
| Mbane | Tap water a (Drinking, washing, domestic activities b) |
| Lake Guiers (Domestic activities b, bathing, irrigating crops) | |
| Diokhor Tack | Lake Guiers (Drinking, washing, domestic activities b, bathing, irrigating crops) |
| Foss | Lake Guiers (Drinking, washing, domestic activities b, bathing, irrigating crops) |
| Public and private water wells (Drinking, washing) | |
| Malla | Tap water non-potable at a single point in the village (Drinking, washing, domestic activities b) |
| Lake Guiers (Drinking, washing, domestic activities b, bathing, irrigating crops) | |
| Malla Tack | Tap water non-potable in 3 houses of the village (Washing, domestic activities b) |
| Lake Guiers (Drinking, washing, domestic activities b, bathing, irrigating crops) |
| Villages | Samples (n) | Positive Samples (n) | Prevalence (%) | Blastocystis sp. STs | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| ST1 | ST2 | ST3 | ST7 | ST10 | ST14 | MI a | ||||
| Area of Saint-Louis | ||||||||||
| Maka Diama | 75 | 57 | 76.0 | 15 | 15 | 13 | 0 | 1 | 0 | 13 |
| Ndiol Maure | 71 | 47 | 66.2 | 18 | 12 | 9 | 0 | 0 | 0 | 8 |
| Lampsar | 86 | 77 | 89.5 | 8 | 27 | 27 | 2 | 0 | 0 | 13 |
| Mbakhana | 81 | 72 | 88.9 | 11 | 27 | 13 | 0 | 0 | 1 | 20 |
| Ndiawdoune | 50 | 50 | 100 | 0 | 24 | 10 | 1 | 0 | 1 | 14 |
| Total area | 363 | 303 | 83.5 | 52 | 105 | 72 | 3 | 1 | 2 | 68 |
| Area of the Lake Guiers | ||||||||||
| Mbane | 89 | 46 | 51.7 | 17 | 11 | 10 | 0 | 0 | 0 | 8 |
| Diokhor Tack | 104 | 80 | 76.9 | 22 | 32 | 7 | 0 | 0 | 0 | 19 |
| Foss | 25 | 23 | 92.0 | 7 | 8 | 3 | 0 | 0 | 0 | 5 |
| Malla | 54 | 51 | 94.4 | 2 | 34 | 3 | 0 | 0 | 0 | 12 |
| Malla Tack | 96 | 85 | 88.5 | 13 | 36 | 12 | 0 | 1 | 0 | 23 |
| Total area | 368 | 285 | 77.4 | 61 | 121 | 35 | 0 | 1 | 0 | 67 |
| Grand total | 731 | 588 | 80.4 | 113 | 226 | 107 | 3 | 2 | 2 | 135 |
| Villages | ST1 Isolates | ST1 Genotypes/15 | ST2 Isolates | ST2 Genotypes/20 | ST3 Isolates | ST3 Genotypes/8 | Total ST1, ST2 and ST3 Isolates | Total ST1, ST2 and ST3 Genotypes/43 | Total Solates/Total Genotypes |
|---|---|---|---|---|---|---|---|---|---|
| Area of Saint-Louis | |||||||||
| Maka Diama | 15 | 3 | 15 | 5 | 13 | 4 | 43 | 12 | 3.6 |
| Ndiol Maure | 18 | 11 | 12 | 6 | 9 | 4 | 39 | 21 | 1.9 |
| Lampsar | 8 | 2 | 27 | 3 | 27 | 4 | 62 | 9 | 6.9 |
| Mbakhana | 11 | 4 | 27 | 4 | 13 | 5 | 51 | 13 | 3.9 |
| Ndiawdoune | 0 | 0 | 24 | 2 | 10 | 2 | 34 | 4 | 8.5 |
| Average | 229 | 30 | 7.6 | ||||||
| Area of Lake Guiers | |||||||||
| Mbane | 17 | 6 | 11 | 4 | 10 | 3 | 38 | 13 | 2.9 |
| Diokhor Tack | 22 | 4 | 32 | 4 | 7 | 1 | 61 | 9 | 6.8 |
| Foss | 7 | 5 | 8 | 3 | 3 | 3 | 18 | 11 | 1.6 |
| Malla | 2 | 1 | 34 | 3 | 3 | 2 | 39 | 6 | 6.5 |
| Malla Tack | 13 | 6 | 36 | 12 | 12 | 4 | 61 | 22 | 2.8 |
| Average | 217 | 27 | 8.0 |
| African Region/Countries | Prevalence | Subtyped Isolates | Subtyping Method | Blastocystis sp. STs | Mixed Infection | Reference | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ST1 | ST2 | ST3 | ST4 | ST5 | ST6 | ST7 | ST10 | ST14 | ||||||
| North Africa | ||||||||||||||
| Tunisia | NA a | 61 | Sequencing | 18 | 10 | 31 | 1 | 0 | 0 | 1 | 0 | 0 | 0 | [47] |
| Libya | 28.0% | 38 | Sequencing | 19 | 3 | 15 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | [31] |
| Libya | NA a | 48 | Sequencing | 26 | 13 | 9 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [48] |
| Egypt | NA a | 36 | PCR-STS b | 6 | 0 | 30 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [49] |
| Egypt | NA a | 110 | PCR-STS b | 15 | 0 | 49 | 0 | 0 | 33 | 13 | 0 | 0 | 0 | [50] |
| Egypt | NA a | 33 | Sequencing | 0 | 0 | 33 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [51] |
| Egypt | NA a | 21 | Sequencing | 4 | 4 | 13 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [36] |
| Egypt | NA a | 44 | PCR-STS b | 8 | 0 | 24 | 0 | 0 | 8 | 4 | 0 | 0 | 0 | [52] |
| Total | 391 | 96 | 30 | 204 | 1 | 0 | 41 | 19 | 0 | 0 | 0 | |||
| West Africa | ||||||||||||||
| Nigeria | 84.0% | 127 | Sequencing | 51 | 42 | 33 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | [37] |
| Nigeria | 49.0% | 22 | Sequencing | 10 | 0 | 9 | 3 | 0 | 0 | 0 | 0 | 0 | 1 | [31] |
| Côte d’Ivoire | 58.2% | 64 | Sequencing | 32 | 14 | 18 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [38] |
| Côte d’Ivoire | 70.0% | 0 | NA a | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [45] |
| Liberia | 70.0% | 25 | Sequencing | 7 | 7 | 8 | 3 | 0 | 0 | 0 | 0 | 0 | 5 | [31] |
| Senegal | 80.4% | 453 | Sequencing | 113 | 226 | 107 | 0 | 0 | 0 | 3 | 2 | 2 | 135 | Present study |
| Senegal | 100% | 103 | Sequencing | 29 | 21 | 51 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | [12] |
| Mali | 49.7% | 0 | NA a | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [46] |
| Total | 794 | 242 | 310 | 226 | 8 | 0 | 0 | 4 | 2 | 2 | 141 | |||
| Central Africa | ||||||||||||||
| Angola | 25.6% | 75 | Sequencing | 23 | 23 | 27 | 0 | 1 | 0 | 1 | 0 | 0 | 0 | [42] |
| Cameroon | 88.2% | 65 | Sequencing | 23 | 9 | 33 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [13] |
| Total | 140 | 46 | 32 | 60 | 0 | 1 | 0 | 1 | 0 | 0 | 0 | |||
| East Africa | ||||||||||||||
| Tanzania | 81.8% | 34 | Metagenomics | 11 | 13 | 10 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [13] |
| Tanzania | 55.6% | 15 | Metagenomics | 1 | 12 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [43] |
| Tanzania | 60.9% | 92 | Sequencing | 36 | 28 | 27 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | [41] |
| Tanzania | NA a | 6 | Sequencing | 1 | 3 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | [53] |
| Total | 147 | 19 | 56 | 41 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | |||
| Southern Africa | ||||||||||||||
| Madagascar | 64.5% | 158 | Sequencing | 80 | 36 | 42 | 0 | 0 | 0 | 0 | 0 | 0 | 13 | [44] |
| Total | 158 | 80 | 36 | 42 | 0 | 0 | 0 | 0 | 0 | 0 | 13 | |||
| Grand total | 1630 | 513 | 464 | 573 | 9 | 1 | 41 | 25 | 2 | 2 | 154 | |||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Khaled, S.; Gantois, N.; Ly, A.T.; Senghor, S.; Even, G.; Dautel, E.; Dejager, R.; Sawant, M.; Baydoun, M.; Benamrouz-Vanneste, S.; et al. Prevalence and Subtype Distribution of Blastocystis sp. in Senegalese School Children. Microorganisms 2020, 8, 1408. https://doi.org/10.3390/microorganisms8091408
Khaled S, Gantois N, Ly AT, Senghor S, Even G, Dautel E, Dejager R, Sawant M, Baydoun M, Benamrouz-Vanneste S, et al. Prevalence and Subtype Distribution of Blastocystis sp. in Senegalese School Children. Microorganisms. 2020; 8(9):1408. https://doi.org/10.3390/microorganisms8091408
Chicago/Turabian StyleKhaled, Salma, Nausicaa Gantois, Amadou Tidjani Ly, Simon Senghor, Gaël Even, Ellena Dautel, Romane Dejager, Manasi Sawant, Martha Baydoun, Sadia Benamrouz-Vanneste, and et al. 2020. "Prevalence and Subtype Distribution of Blastocystis sp. in Senegalese School Children" Microorganisms 8, no. 9: 1408. https://doi.org/10.3390/microorganisms8091408
APA StyleKhaled, S., Gantois, N., Ly, A. T., Senghor, S., Even, G., Dautel, E., Dejager, R., Sawant, M., Baydoun, M., Benamrouz-Vanneste, S., Chabé, M., Ndiaye, S., Schacht, A.-M., Certad, G., Riveau, G., & Viscogliosi, E. (2020). Prevalence and Subtype Distribution of Blastocystis sp. in Senegalese School Children. Microorganisms, 8(9), 1408. https://doi.org/10.3390/microorganisms8091408







