Development of a Portable Detection Method for Enteric Viruses from Ambient Air and Its Application to a Wastewater Treatment Plant
Abstract
1. Introduction
2. Materials and Methods
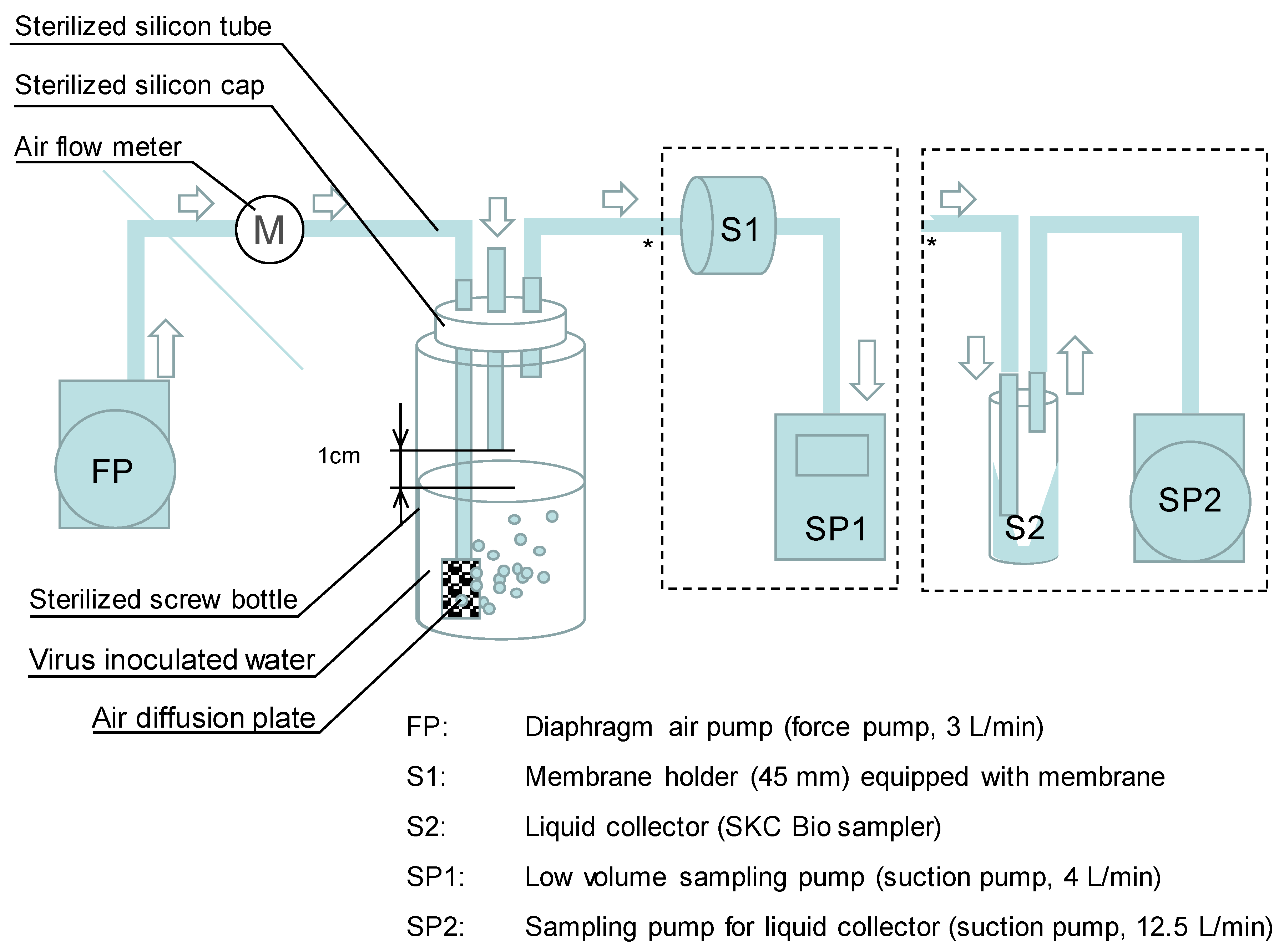
2.1. Development of Collection Method and Laboratory Evaluation
2.2. qPCR Assay
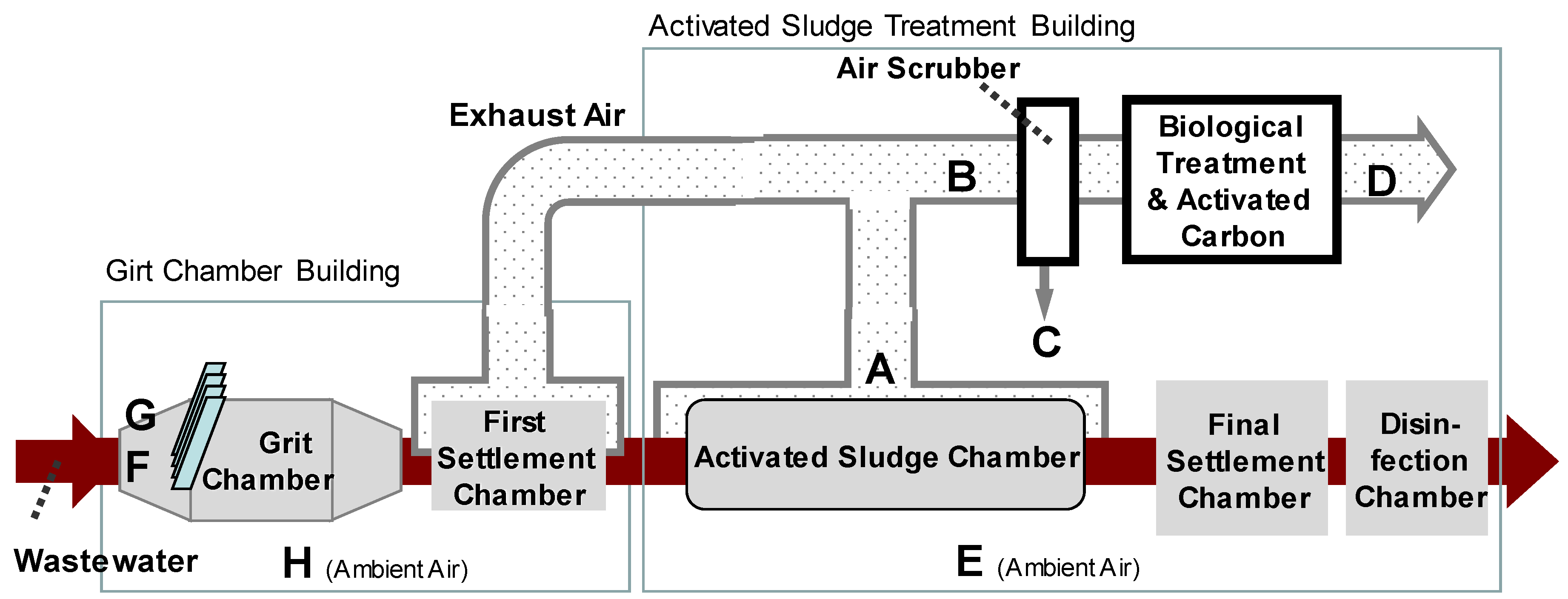
2.3. Sampling at the Wastewater Treatment Plant
3. Results and Discussion
3.1. Evaluation of the Developed Sampling Method
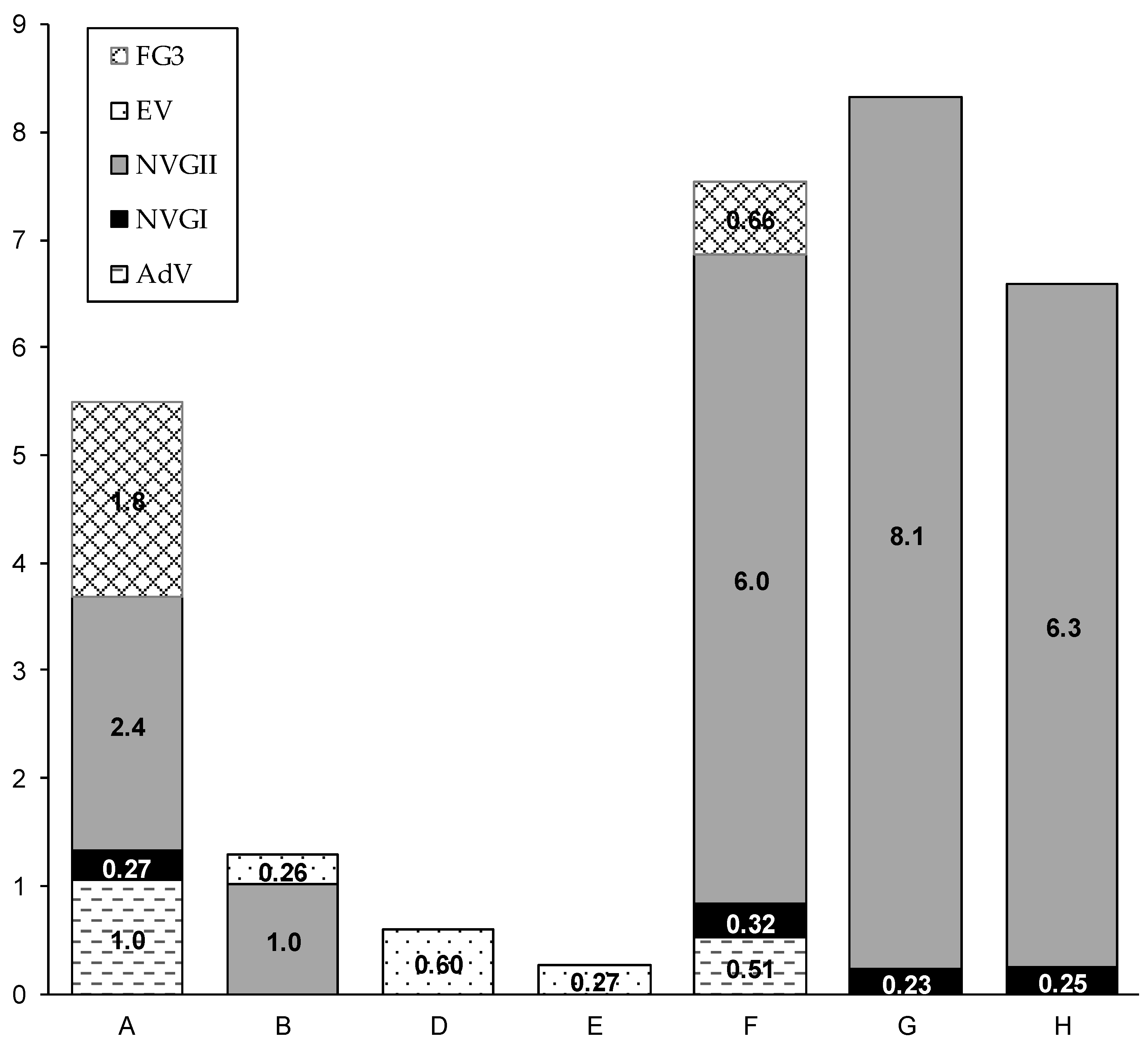
3.2. Application to Wastewater Treatment Plant
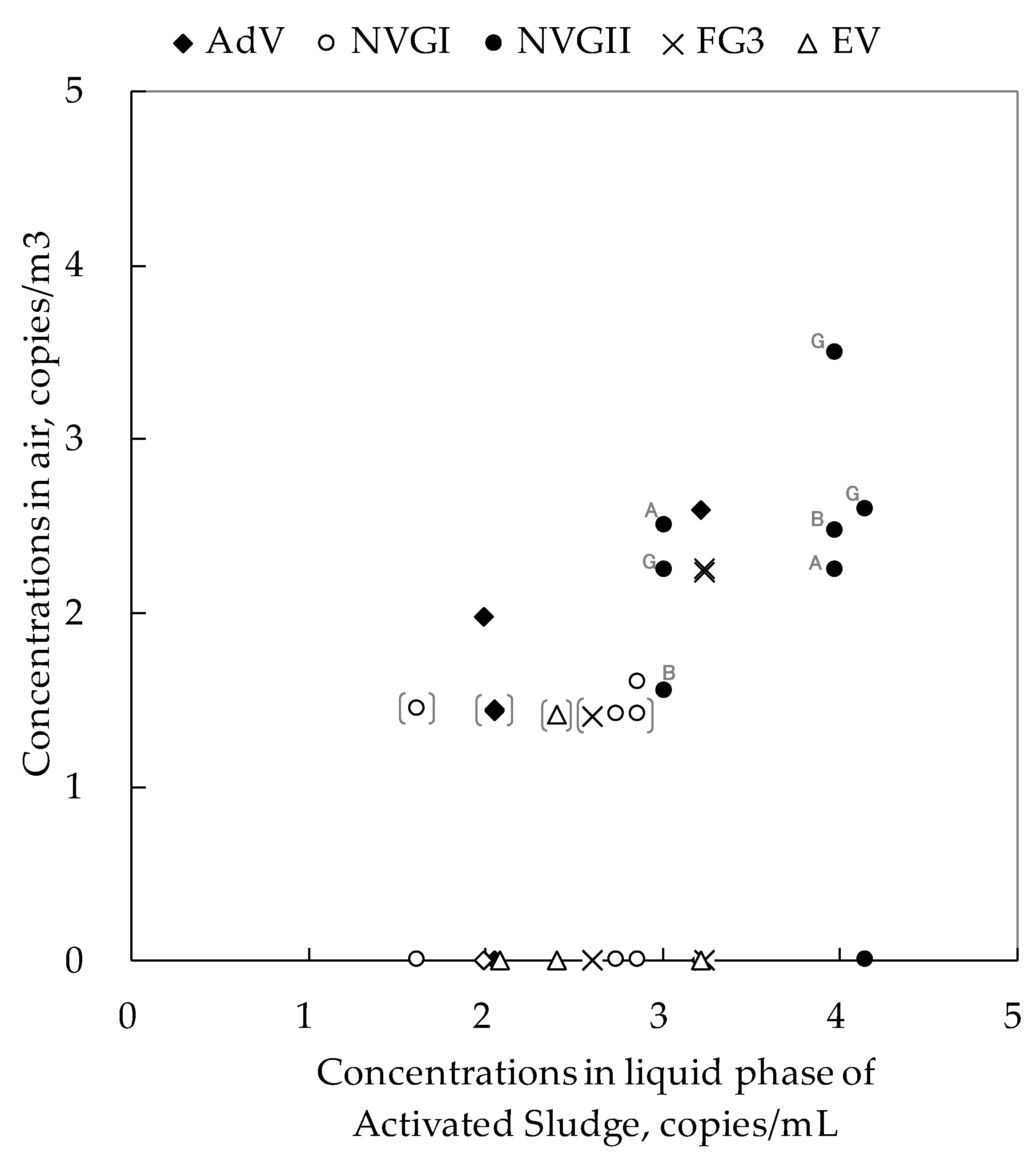
3.3. Comparison of Virus Concentration in the Water and Air
3.4. Comparison with Liquid-Based Sampler
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Adams, A.P.; Spendlove, J.C. Coliform aerosols emitted by sewage treatment plants. Science 1970, 169, 1218–1220. [Google Scholar] [CrossRef] [PubMed]
- Fannin, K.F.; Vana, S.C.; Jakubowski, W. Effect of an activated sludge wastewater treatment plant on ambient air densities of aerosols containing bacteria and viruses. Appl. Environ. Microbiol. 1985, 49, 1191–1196. [Google Scholar] [PubMed]
- Sawyer, L.A.; Murphy, J.J.; Kaplan, J.E.; Pinsky, P.F.; Chacon, D.; Walmsley, S.; Schonberger, L.B.; Phillips, A.; Forward, K.; Goldman, C.; et al. 25 to 30nm virus particle associated with a hospital outbreak of acute gastroenteritis with evidence for airborne transmission. Am. J. Epidemiol. 1988, 127, 1261–1271. [Google Scholar] [CrossRef] [PubMed]
- Uhrbrand, K.; Schultz, A.C.; Madsen, A.M. Exposure to Airborne Noroviruses and Other Bioaerosol Components at a Wastewater Treatment Plant in Denmark. Food Environ. Virol. 2011, 3, 130–137. [Google Scholar] [CrossRef]
- Orsini, M.; Laurenti, P.; Boninti, F.; Arzani, D.; Lanni, A.; Romano-Spica, V. A molecular typing approach for evaluating bioaerosol exposure in wastewater treatment plant workers. Water Res. 2002, 36, 1375–1378. [Google Scholar] [CrossRef]
- Wallis, C.; Melnick, J.L.; Rao, V.C.; Sox, T.E. Method for detecting viruses in aerosols. Appl. Environ. Microbiol. 1985, 50, 1181–1186. [Google Scholar] [PubMed]
- Haramoto, E.; Katayama, H.; Oguma, K.; Yamashita, H.; Tajima, A.; Nakajima, H.; Ohgaki, S. Seasonal profiles of human noroviruses and indicator bacteria in a wastewater treatment plant in Tokyo, Japan. Water Sci. Technol. 2006, 54, 301–308. [Google Scholar] [CrossRef] [PubMed]
- Marks, P.J.; Vipond, I.B.; Regan, F.M.; Wedgwood, K.; Fey, R.E.; Caul, E.O. A school outbreak of Norwalk-like virus: Evidence for airborne transmission. Epidemiol. Infect. 2003, 131, 727–736. [Google Scholar] [CrossRef] [PubMed]
- Marks, P.J.; Vipond, I.B.; Carlisle, D.; Deakin, D.; Fey, R.E.; Caul, E.O. Evidence for airborne transmission of Norwalk-like virus (NLV) in a hotel restaurant. Epidemiol. Infect. 2000, 124, 481–487. [Google Scholar] [CrossRef] [PubMed]
- Bartnicki, E.; Cunha, J.B.; Kolawole, A.O.; Wobus, C.E. Recent advances in understanding noroviruses. F1000Research 2017, 6, 79. [Google Scholar] [CrossRef] [PubMed]
- Brisebois, E.; Veillette, M.; Dion-Dupont, V.; Lavoie, J.; Corbeil, J.; Culley, A.; Duchaine, C. Human viral pathogens are pervasive in wastewater treatment center aerosols. J. Environ. Sci. 2018, 67, 45–53. [Google Scholar] [CrossRef] [PubMed]
- Hogan, C.J.; Kettleson, E.M.; Lee, M.H.; Ramaswami, B.; Angenent, L.T.; Biswas, P. Sampling methodologies and dosage assessment techniques for submicrometre and ultrafine virus aerosol particles. J. Appl. Microbiol. 2005, 99, 1422–1434. [Google Scholar] [CrossRef] [PubMed]
- Matsubara, K.; Haramoto, E.; Katayama, H.; Ohgaki, S. Detection method for enteric viruses in bioaerosol from sewage treatment plant with quantitative real-time PCR. In Proceedings of the 14th International Symposium on Health-Related Water Microbiology, Tokyo, Japan, 9–15 September 2007; pp. 321–322. [Google Scholar]
- Katayama, H.; Shimasaki, A.; Ohgaki, S. Development of a virus concentration method and its application to detection of enterovirus and norwalk virus from coastal seawater. Appl. Environ. Microbiol. 2002, 68, 1033–1039. [Google Scholar] [CrossRef] [PubMed]
- Limsawat, S.; Ohgaki, S. Fate of liberated viral RNA in wastewater determined by PCR. Appl. Environ. Microbiol. 1997, 63, 2932–2933. [Google Scholar] [PubMed]
- Kitajima, M.; Oka, T.; Tohya, Y.; Katayama, H.; Takeda, N.; Katayama, K. Development of a broadly reactive nested reverse transcription-PCR assay to detect murine noroviruses, and investigation of the prevalence of murine noroviruses in laboratory mice in Japan. Microbiol. Immunol. 2009, 53, 531–534. [Google Scholar] [CrossRef] [PubMed]
- Heim, A.; Ebnet, C.; Harste, G.; Pring-Åkerblom, P. Rapid and quantitative detection of human adenovirus DNA by real-time PCR. J. Med. Virol. 2003, 70, 228–239. [Google Scholar] [CrossRef] [PubMed]
- Ogorzaly, L.; Gantzer, C. Development of real-time RT-PCR methods for specific detection of F-specific RNA bacteriophage genogroups: Application to urban raw wastewater. J. Virol. Methods 2006, 138, 131–139. [Google Scholar] [CrossRef] [PubMed]
- Kageyama, T.; Kojima, S.; Shinohara, M.; Uchida, K.; Fukushi, S.; Hoshino, F.B.; Takeda, N.; Katayama, K. Broadly reactive and highly sensitive assay for Norwalk-like viruses based on real-time quantitative reverse transcription-PCR. J. Clin. Microbiol. 2003, 41, 1548–1557. [Google Scholar] [CrossRef] [PubMed]
- Imai, T.; Sano, D.; Miura, T.; Okabe, S.; Wada, K.; Masago, Y.; Omura, T. Adsorption characteristics of an enteric virus-binding protein to norovirus, rotavirus and poliovirus. BMC Biotechnol. 2011, 11, 123. [Google Scholar] [CrossRef] [PubMed]
- Michaud, J.M.; Thompson, L.R.; Kaul, D.; Espinoza, J.L.; Richter, R.A.; Xu, Z.Z.; Lee, C.; Pham, K.M.; Beall, C.M.; Malfatti, F.; et al. Taxon-specific aerosolization of bacteria and viruses in an experimental ocean-atmosphere mesocosm. Nat. Commun. 2018, 9, 2017. [Google Scholar] [CrossRef] [PubMed]
| Trial | Method | Concentration of Viruses in the Bubbled Water Sample (Copies/mL Water) | Dissipated Water Volume (mL) | Air Volume (m3) | Captured Viruses per Air (Copies/m3 Air) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Qβ | PV | MNV | Qβ | PV | MNV | |||||||
| Before | After | Before | After | Before | After | |||||||
| 1 | HA vortex | 2.9 × 108 | 2.7 × 108 | 2.5 × 106 | 1.6 × 106 | 7.7 × 105 | 1.5 × 106 | 2.06 | 121 | 1.3 × 102 | 2.5 × 100 | 1.9 × 103 |
| Liquid Collector | 4.33 | 375 | 6.7 × 101 | 2.1 × 101 | 3.2 × 102 | |||||||
| 2 | HA vortex | 3.1 × 108 | 3.3 × 108 | 2.4 × 106 | 1.6 × 106 | 1.4 × 106 | 7.2 × 105 | 2.01 | 121 | 5.4 × 101 | 9.5 × 100 | 3.9 × 102 |
| Liquid Collector | 3.52 | 375 | 4.9 × 101 | 2.3 × 101 | 1.6 × 102 | |||||||
| 3 | HA vortex | 3.3 × 108 | 2.9 × 108 | 2.4 × 106 | 2.1 × 106 | 1.4 × 106 | 7.2 × 105 | 2.02 | 121 | 3.5 × 101 | 1.2 × 101 | 3.5 × 102 |
| Liquid Collector | 4.37 | 375 | 5.5 × 101 | 2.1 × 101 | 2.8 × 102 | |||||||
| Trial | Sample Water Type | Virus Concentration, Copies/mL Water | ||||
|---|---|---|---|---|---|---|
| AdV | NV GI | NV GII | FG3 | EV | ||
| Nov-07 | Activated Sludge | 1.1 × 102 | 4.1 × 101 | 1.0 × 103 | 1.7 × 103 | 1.2 × 102 |
| Dec-07 | Activated Sludge | 9.7 × 101 | 7.4 × 102 | 9.4 × 103 | 4.0 × 102 | 2.5 × 102 |
| Drain from Mist Separator | 5.2 × 10-1 | 1.7 × 100 | 1.5 × 102 | 3.8 × 100 | + | |
| Jan-08 | Activated Sludge | 1.6 × 103 | 5.5 × 102 | 1.4 × 104 | 4.0 × 102 | 1.6 × 103 |
| Jan-08 | Raw Sewage | 4.4 × 103 | 4.1 × 102 | 2.5 × 104 | 1.3 × 103 | 2.5 × 103 |
| Jan-08 | Drain from Mist Separator | ND | 1.1 × 101 | 9.4 × 102 | 1.1 × 101 | 7.8 × 100 |
| Sampling Period | Site A (Copies/mL) | |||||
|---|---|---|---|---|---|---|
| HA Vortex | Liquid Collector | |||||
| NV GI | NV GII | FGIII | NV GI | NV GII | FGIII | |
| December-07 | + | 1.8 × 102 | - | - | + | - |
| January-08 | - | - | - | 1.2 × 103 | 3.1 × 103 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Matsubara, K.; Katayama, H. Development of a Portable Detection Method for Enteric Viruses from Ambient Air and Its Application to a Wastewater Treatment Plant. Pathogens 2019, 8, 131. https://doi.org/10.3390/pathogens8030131
Matsubara K, Katayama H. Development of a Portable Detection Method for Enteric Viruses from Ambient Air and Its Application to a Wastewater Treatment Plant. Pathogens. 2019; 8(3):131. https://doi.org/10.3390/pathogens8030131
Chicago/Turabian StyleMatsubara, Koichi, and Hiroyuki Katayama. 2019. "Development of a Portable Detection Method for Enteric Viruses from Ambient Air and Its Application to a Wastewater Treatment Plant" Pathogens 8, no. 3: 131. https://doi.org/10.3390/pathogens8030131
APA StyleMatsubara, K., & Katayama, H. (2019). Development of a Portable Detection Method for Enteric Viruses from Ambient Air and Its Application to a Wastewater Treatment Plant. Pathogens, 8(3), 131. https://doi.org/10.3390/pathogens8030131




