What Is Injury in Ice Hockey: An Integrative Literature Review on Injury Rates, Injury Definition, and Athlete Exposure in Men’s Elite Ice Hockey
Abstract
1. Introduction
2. Materials and Methods
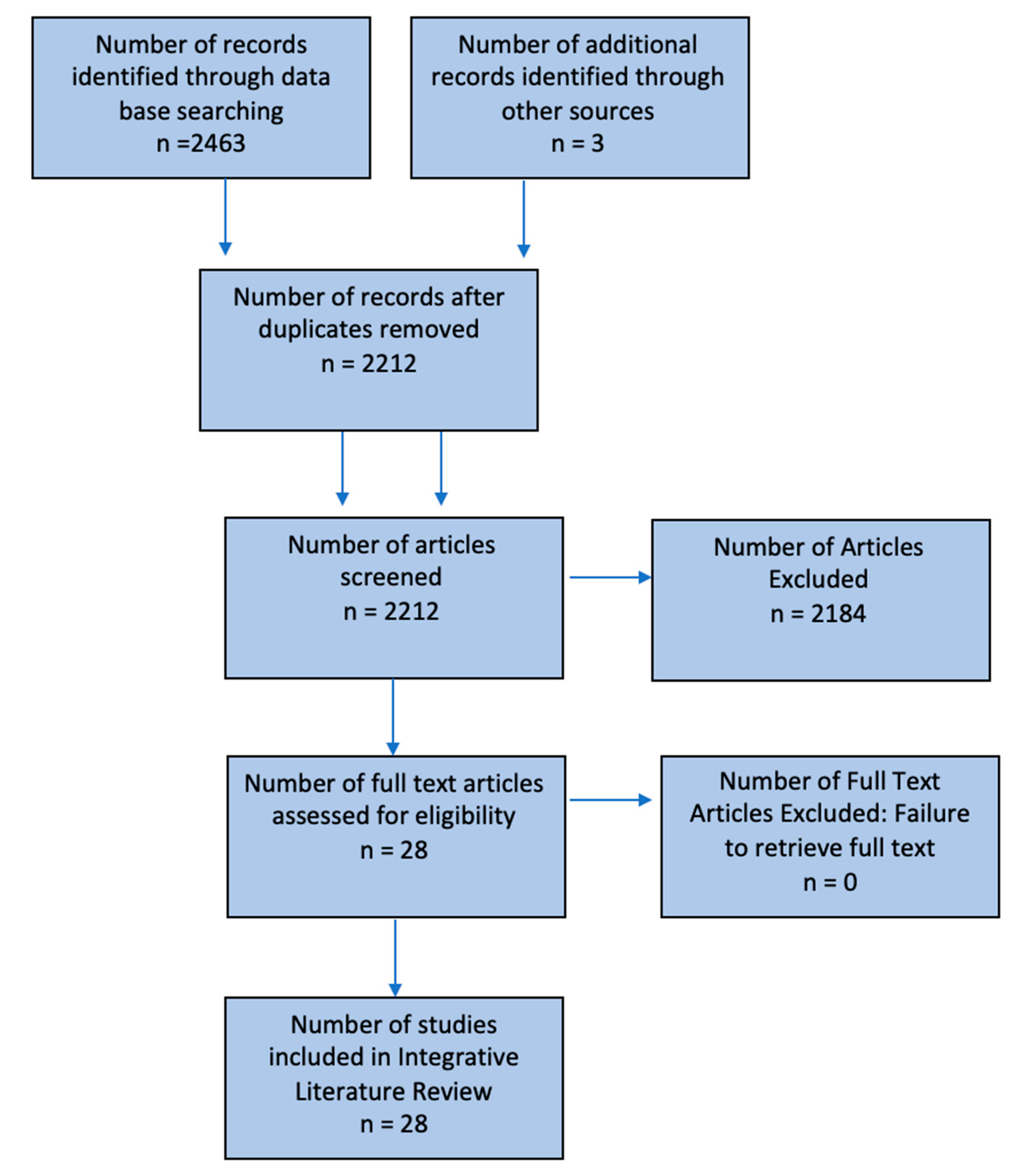
Literature Search
3. Results
3.1. Rate of Musculoskeletal Injuries in Men’s Elite Ice Hockey (Question #1)
3.2. Injury Definition in Men’s Elite Ice Hockey (Question #2)
3.3. Athlete Exposure Metric in Men’s Elite Ice Hockey (Question #3)
4. Discussion
Limitations
5. Conclusions
Further Research
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Sim, F.H.; Simonet, W.T.; Melton, L.J., 3rd; Lehn, T.A. Ice hockey injuries. Am. J. Sports Med. 1987, 15, 30–40. [Google Scholar] [CrossRef] [PubMed]
- Caputo, P.; Mattson, D.J. Recreational ice hockey injuries in adult non-checking leagues: A United States perspective. J. Sports Sci. Med. 2005, 4, 58–65. [Google Scholar] [PubMed]
- Emery, C.A.; Kang, J.; Shrier, I.; Goulet, C.; Hagel, B.E.; Benson, B.W.; Nettel-Aguirre, A.; McAllister, J.R.; Hamilton, G.M.; Meeuwisse, W.H. Risk of injury associated with body checking among youth ice hockey players. JAMA 2010, 303, 2265–2272. [Google Scholar] [CrossRef] [PubMed]
- McKay, C.D.; Tufts, R.J.; Shaffer, B.; Meeuwisse, W.H. The epidemiology of professional ice hockey injuries: A prospective report of six NHL seasons. Br. J. Sports Med. 2014, 48, 57–62. [Google Scholar] [CrossRef] [PubMed]
- Donaldson, L.; Li, B.; Cusimano, M.D. Economic burden of time lost due to injury in NHL hockey players. Inj. Prev. 2014, 20, 347–349. [Google Scholar] [CrossRef] [PubMed]
- Hodgson, L.; Gissane, C.; Gabbett, T.J.; King, D.A. For debate: Consensus injury definitions in team sports should focus on encompassing all injuries. Clin. J. Sport Med. 2007, 17, 188–191. [Google Scholar] [CrossRef]
- Wennberg, R. Effect of ice surface size on collision rates and head impacts at the World Junior Hockey Championships, 2002 to 2004. Clin. J. Sport Med. 2005, 15, 67–72. [Google Scholar] [CrossRef]
- Finch, C.F. An overview of some definitional issues for sports injury surveillance. Sports Med. 1997, 24, 157–163. [Google Scholar] [CrossRef]
- Cropper, E.; Thorpe, C.M.; Roberts, S.; Twist, C. Injury Surveillance during a European Touch Rugby Championship. Sports 2019, 7, 71. [Google Scholar] [CrossRef]
- Fuller, C.W.; Ekstrand, J.; Junge, A.; Andersen, T.E.; Bahr, R.; Dvorak, J.; Hägglund, M.; McCrory, P.; Meeuwisse, W.H. Consensus statement on injury definitions and data collection procedures in studies of football (soccer) injuries. Scand. J. Med. Sci. Sports 2006, 16, 83–92. [Google Scholar] [CrossRef]
- Fuller, C.W.; Molloy, M.G.; Bagate, C.; Bahr, R.; Brooks, J.H.; Donson, H.; Kemp, S.P.; McCrory, P.; McIntosh, A.S.; Meeuwisse, W.H. Consensus statement on injury definitions and data collection procedures for studies of injuries in rugby union. Br. J. Sports Med. 2007, 41, 328–331. [Google Scholar] [CrossRef]
- Ekstrand, J.; Karlsson, J. The risk for injury in football. There is a need for a consensus about definition of the injury and the design of studies. Scand. J. Med. Sci. Sports 2003, 13, 147–149. [Google Scholar] [CrossRef]
- Crowley, S.G.; Trofa, D.P.; Vosseller, J.T.; Gorroochurn, P.; Redler, L.H.; Schiu, B.; Popkin, C.A. Epidemiology of Foot and Ankle Injuries in National Collegiate Athletic Association Men’s and Women’s Ice Hockey. Orthop. J. Sports Med. 2019, 7, 2325967119865908. [Google Scholar] [CrossRef]
- Comstock, R.; Currie, D.; Pierpoint, L. Convenience Sample Summary Report: National High School Sports-Related Injury Surveillance Study: 2008–2018 School Years. Available online: http://www.ucdenver.edu/academics/colleges/PublicHealth/research/ResearchProjects/piper/projects/RIO/Pages/Study-Reports.aspx (accessed on 21 October 2019).
- Emery, C.; Kang, J.; Shrier, I.; Goulet, C.; Hagel, B.; Benson, B.; Nettel-Aguirre, A.; McAllister, J.; Meeuwisse, W. Risk of injury associated with bodychecking experience among youth hockey players. CMAJ 2011, 183, 1249–1256. [Google Scholar] [CrossRef]
- Torraco, R.J. Writing integrative literature reviews: Using the past and present to explore the future. Hum. Resour. Dev. Rev. 2016, 15, 404–428. [Google Scholar] [CrossRef]
- Falagas, M.E.; Pitsouni, E.I.; Malietzis, G.A.; Pappas, G. Comparison of PubMed, Scopus, web of science, and Google scholar: Strengths and weaknesses. FASEB J. 2008, 22, 338–342. [Google Scholar] [CrossRef]
- Lorentzon, R.; Wedren, H.; Pietilä, T.; Gustavsson, B. Injuries in international ice hockey: A prospective, comparative study of injury incidence and injury types in international and Swedish elite ice hockey. Am. J. Sports Med. 1988, 16, 389–391. [Google Scholar] [CrossRef]
- Flik, K.; Lyman, S.; Marx, R.G. American collegiate men’s ice hockey: An analysis of injuries. Am. J. Sports Med. 2005, 33, 183–189. [Google Scholar] [CrossRef]
- Pelletier, R.L.; Montelpare, W.J.; Stark, R.M. Intercollegiate ice hockey injuries: A case for uniform definitions and reports. Am. J. Sports Med. 1993, 21, 78–81. [Google Scholar] [CrossRef]
- Stuart, M.J.; Smith, A. Injuries in junior A ice hockey: A three-year prospective study. Am. J. Sports Med. 1995, 23, 458–461. [Google Scholar] [CrossRef]
- Tuominen, M.; Stuart, M.J.; Aubry, M.; Kannus, P.; Parkkari, J. Injuries in world junior ice hockey championships between 2006 and 2015. Br. J. Sports Med. 2017, 51, 36–43. [Google Scholar] [CrossRef]
- McKnight, C.M.; Ferrara, M.S.; Czerwinska, J.M. Intercollegiate ice hockey injuries: A three-year analysis. J. Athl. Train. 1992, 27, 338–343. [Google Scholar]
- Tegner, Y.; Lorentzon, R. Ice hockey injuries: Incidence, nature and causes. Br. J. Sports Med. 1991, 25, 87–89. [Google Scholar] [CrossRef]
- Hayes, D. Hockey injuries: How, why, where, and when? Physician Sports Med. 1975, 3, 61–65. [Google Scholar] [CrossRef]
- Sutherland, G.W. Fire on ice. Am. J. Sports Med. 1976, 4, 264–269. [Google Scholar] [CrossRef]
- Hayes, D. An injury profile for hockey. Can. J. Appl. Sport Sci. 1978, 3, 61–64. [Google Scholar]
- Rielly, M. The nature and causes of hockey injuries: A five year study. Athl. Train. 1982, 17, 88–90. [Google Scholar]
- Meeuwisse, W.H.; Fowler, P.J. Frequency and predictability of sports injuries in intercollegiate athletes. Canad. J. Sport Sci. 1988, 13, 35–42. [Google Scholar]
- Lorentzon, R.; Wedrèn, H.; Pietilä, T. Incidence, nature, and causes of ice hockey injuries: A three-year prospective study of a Swedish elite ice hockey team. Am. J. Sports Med. 1988, 16, 392–396. [Google Scholar] [CrossRef]
- Pettersson, M.; Lorentzon, R. Ice hockey injuries: A 4-year prospective study of a Swedish elite ice hockey team. Br. J. Sports Med. 1993, 27, 251–254. [Google Scholar] [CrossRef]
- Cunningham, C.; Cunningham, S. Injury surveillance at a national multi-sport event. Aust. J. Sci. Med. Sport 1996, 28, 50–56. [Google Scholar] [PubMed]
- Mölsä, J.; Airaksinen, O.; Näsman, O.; Torstila, I. Ice hockey injuries in Finland: A prospective epidemiologic study. Am. J. Sports Med. 1997, 25, 495–499. [Google Scholar] [CrossRef] [PubMed]
- Pinto, M.; Kuhn, J.E.; Greenfield, M.; Hawkins, R.J. Prospective analysis of ice hockey injuries at the junior A level over the course of one season. Clin. J. Sport Med. 1999, 9, 70–74. [Google Scholar] [CrossRef] [PubMed]
- Mölsä, J.; Kujala, U.; Näsman, O.; Lehtipuu, T.-P.; Airaksinen, O. Injury profile in ice hockey from the 1970s through the 1990s in Finland. Am. J. Sports Med. 2000, 28, 322–327. [Google Scholar] [CrossRef]
- Agel, J.; Dompier, T.P.; Dick, R.; Marshall, S.W. Descriptive epidemiology of collegiate men’s ice hockey injuries: National Collegiate Athletic Association Injury Surveillance System, 1988–1989 through 2003–2004. J. Athl. Train. 2007, 42, 241–248. [Google Scholar]
- Rishiraj, N.; Lloyd-Smith, R.; Lorenz, T.; Niven, B.; Michel, M. University men’s ice hockey: Rates and risk of injuries over 6-years. J. Sports Med. Phys. Fitness 2009, 49, 159–166. [Google Scholar]
- Kuzuhara, K.; Shimamoto, H.; Mase, Y. Ice hockey injuries in a Japanese elite team: A 3-year prospective study. J. Athl. Train. 2009, 44, 208–214. [Google Scholar] [CrossRef]
- Agel, J.; Harvey, E.J. A 7-year review of men’s and women’s ice hockey injuries in the NCAA. Can. J. Surg. 2010, 53, 319–323. [Google Scholar]
- Engebretsen, L.; Steffen, K.; Alonso, J.M.; Aubry, M.; Dvorak, J.; Junge, A.; Meeuwisse, W.; Mountjoy, M.; Renstrom, P.; Wilkinson, M. Sports injuries and illnesses during the Winter Olympic Games 2010. Br. J. Sports Med. 2010, 44, 772–780. [Google Scholar] [CrossRef]
- Kerr, Z.Y.; Dompier, T.P.; Snook, E.M.; Marshall, S.W.; Klossner, D.; Hainline, B.; Corlette, J. National Collegiate Athletic Association Injury Surveillance System: Review of methods for 2004–2005 through 2013–2014 data collection. J. Athl. Train. 2014, 49, 552–560. [Google Scholar] [CrossRef]
- Tuominen, M.; Stuart, M.J.; Aubry, M.; Kannus, P.; Parkkari, J. Injuries in men’s international ice hockey: A 7-year study of the International Ice Hockey Federation Adult World Championship Tournaments and Olympic Winter Games. Br. J. Sports Med. 2015, 49, 30–36. [Google Scholar] [CrossRef]
- Kerr, Z.Y.; Marshall, S.W.; Dompier, T.P.; Corlette, J.; Klossner, D.A.; Gilchrist, J. College Sports-Related Injuries—United States, 2009–10 Through 2013-14 Academic Years. MMWR Morb. Mortal. Wkly. Rep. 2015, 64, 1330–1336. [Google Scholar] [CrossRef]
- Lynall, R.C.; Mihalik, J.P.; Pierpoint, L.A.; Currie, D.W.; Knowles, S.B.; Wasserman, E.B.; Dompier, T.P.; Comstock, R.D.; Marshall, S.W.; Kerr, Z.Y. The First Decade of Web-Based Sports Injury Surveillance: Descriptive Epidemiology of Injuries in US High School Boys’ Ice Hockey (2008–2009 Through 2013–2014) and National Collegiate Athletic Association Men’s and Women’s Ice Hockey (2004–2005 Through 2013–2014). J. Athl. Train. 2018, 53, 1129–1142. [Google Scholar]
- Clarsen, B.; Bahr, R. Matching the choice of injury/illness definition to study setting, purpose and design: One size does not fit all! Br. J. Sports Med. 2014, 48, 510–512. [Google Scholar] [CrossRef]
- Timpka, T.; Alonso, J.-M.; Jacobsson, J.; Junge, A.; Branco, P.; Clarsen, B.; Kowalski, J.; Mountjoy, M.; Nilsson, S.; Pluim, B. Injury and illness definitions and data collection procedures for use in epidemiological studies in Athletics (track and field): Consensus statement. Br. J. Sports Med. 2014, 48, 483–490. [Google Scholar] [CrossRef]
- MacDonald, K.J.; Palacios-Derflingher, L.M.; Emery, C.A.; Meeuwisse, W.H. The Effect of Injury Definition and Surveillance Methodology on Measures of Injury Occurrence and Burden in Elite Volleyball. Int. J. Sports Med. 2018, 39, 860–866. [Google Scholar] [CrossRef]
- Orchard, J.; Hoskins, W. For debate: Consensus injury definitions in team sports should focus on missed playing time. Clin. J. Sport Med. 2007, 17, 192–196. [Google Scholar] [CrossRef]
- Dick, R.; Agel, J.; Marshall, S.W. National Collegiate Athletic Association injury surveillance system commentaries: Introduction and methods. J. Athl. Train. 2007, 42, 173–182. [Google Scholar]
- Longstaffe, R.; Leiter, J.; MacDonald, P. Anterior Cruciate Ligament Injuries in the National Hockey League: Epidemiology and Performance Impact. Clin. J. Sport Med. 2018, in press. [Google Scholar] [CrossRef]
- Orchard, J.; Newman, D.; Stretch, R.; Frost, W.; Mansingh, A.; Lelpus, A. Methods for injury surveillance in international cricket. South. Afr. J. Sports Med. 2005, 17, 18–28. [Google Scholar]
- Orchard, J.W.; Seward, H.; Orchard, J.J. Results of 2 decades of injury surveillance and public release of data in the Australian Football League. Am. J. Sports Med. 2013, 41, 734–741. [Google Scholar] [CrossRef] [PubMed]
- West, S.W.; Williams, S.; Kemp, S.; Cross, M.J.; Stokes, K.A. Athlete Monitoring in Rugby Union: Is Heterogeneity in Data Capture Holding Us Back? Sports 2019, 7, 98. [Google Scholar] [CrossRef] [PubMed]
| Factor | Inclusion Criteria | Exclusion Criteria | Rationale for This Criterion |
|---|---|---|---|
| Publication Type | Peer-reviewed original research articles only | Review papers, non-peer reviewed articles, editorials, abstracts, book chapters and conference proceedings | For practical reasons, it was deemed to exclusively review primary research articles, rather than non-peer reviewed or abbreviated sources. |
| Language | English language | Non-English | For practical reasons, it was deemed acceptable to only include studies published in English. |
| Publication Date | November 1976 to April 2019 | Publications prior to January 1975 | The characteristics of ice hockey injury reporting may change over time due to rule changes, technological advancements and education. Literature was captured backdated to 1988 to capture these potential developments. |
| Study Design | Multi-center studies, randomized control trials, cohort studies, case-controlled studies and cross-sectional studies. | Case studies | Study design was chosen to ensure reasonable empirical support, and high methodological rigor in defining injury and injury rates amongst competitive hockey players. |
| Gender and Age | Men athletes aged > 16-years participating in a competitive league/team | Women only studies or men ages < 16, age unspecified involved in youth sport | The primary outcome of interest was injury definition and injury rate calculation in competitive ice hockey played by men. Studies that compared rates between males and females and have separate data for both genders were also included for baseline comparisons. Men athletes aged > 16 were considered appropriate. This age demographic represents elite players. |
| Playing Level | Competitive participation | Recreational sport/training | The primary outcomes of interest are injury definition, injury rates, mechanism and anatomical location sustained during competitive ice hockey. |
| Sport | Injuries must be sustained during ice hockey games and practices | Any sport other than ice hockey | Sports included other than ice hockey may result in definitions, and injury rates that are too broad. |
| Types of Injury | Injuries to the musculoskeletal system, including strains, sprains, breaks | Concussions, spinal injuries, head/face, lacerations | The primary outcomes of interest are soft tissue injuries of the upper and lower extremity during competitive ice hockey |
| Outcome Measures | Injury definition, injury rates, athlete exposure, mechanisms, anatomical location | Outcomes other than injury definition, injury rate, and athlete exposure, mechanisms and anatomical location | The primary outcomes of interest are injury definition, injury rates, mechanisms and anatomical location. |
| Authors | Year | Demographic | Injury Definition | Type | Injury Rate | Mechanism of Injury | Injury Type | Injury Rate Computation |
|---|---|---|---|---|---|---|---|---|
| Hayes [25] | 1975 | Intercollegiate Ice hockey | “An event requiring some attention by the team trainer or physician or both.” | Medical Attention | 1.14 injuries per game (Canada) 1.28 injuries per game (USA) | Collision | Head and face, knee, shoulders | Total injuries/Total number of games |
| Sutherland [26] | 1976 | Youth-Pro | The injuries were classified according to the standard nomenclature of athletic injuries as recommended by the American Medical Association | N/A | Pro Group: 143/1000 AE (practice and games) | N/A | Scalp and face 60.8%, Groin 9.1%, knee 7.8%, shoulder 5.9% | N/A |
| Hayes [27] | 1978 | Youth-Pro | “Any change in the normal, healthy state of the individual that requires medical attention and disables a player either temporarily or permanently.” | Medical Attention | University: 1.17/Game Professional: 1.15/Game | Stick and puck contact | Contusions and lacerations | Total injuries/Total number of games |
| Rielly [28] | 1982 | College Hockey | “A reportable injury was defined as being one that required definitive physical evaluation and medical treatment.” | Medical Attention Definition | 1/12.7 h of play ** | Player contact (43.3%), puck contact 27% | Face, hips, shoulders | N/A |
| Meeuwisse et al. [29] | 1988 | Canadian University | Injury was defined as any disability arising either in practice or competition that required physical attention. | Medical Attention Definition | As calculated by percentage. Hockey had the greatest percentage of players injured. | N/A | Knee, ribs, low back | N/A |
| Lorenzton, Wedren, Pietila [30] | 1988 | Swedish Elite Team | “Injury was defined as any injury occurring during on-ice practice or games and causing the player to miss the next practice session or game. Facial lacerations, which are common in ice hockey but do not cause absence from practice or game are reported separately.” | Time Loss Definition | 78.4/1000 player game hours, 1.4/1000 player practice hours | Checking 32.9%, Player contact 25%, Puck contact 14.5%, stick contact 11.8%, collision with boards 6.6%, cutting, 6.6%, skate contact 2.6% | Contusions, strains and sprains were the most common types of injury. Knees were the most commonly injured joint (5 injuries were complete tears of the MCL). 53.7% of injuries were localized in the lower limb. | Practice Injury Rate = number of injuries/Practice Hours × Roster (23.4). Games Injury Rate = number of injuries/Game hours × Total Players on ice (6). |
| Lorenzton, Wedren, Pietila, Gustavsson [18] | 1988 | Swedish National Team (40 International games) | “Injury was defined as any injury occurring during games and causing the player to miss the next practice session or game. Facial lacerations, which are common in ice hockey but do not cause absence from practice or game are reported separately.” | Time Loss Definition | 79.2/1000 player game hours | Player contact 42.1%, checking 31.6%, collision with boards 10.5%, puck/skate contact 5.3% | Contusions, strains and sprains were the most common types of injury. Knees were the most commonly injured joint, followed by the thigh and wrist. | Total Injuries/Total AE × 1000; Total AE = games × Total players on ice (6) |
| Tegner, Lorentzon [24] | 1991 | Swedish Elite League (12 teams) | “Injury was defined as any injury occurring during ice practices or games and causing the player to stop playing or to miss the next practice session or game. Facial lacerations, which are common in ice hockey, but do not cause absence from practice or games, are also reported.” | Time Loss Definition | 53/1000 player game hours (76% of injuries occurred during games) | Stick contact 25.5%, player contact 24%, puck contact 11.2%, collision with boards or goal posts 9.7% | Strain, laceration and contusions were the most common types of injury. Knees were the most common joint injured (13.2%), followed by the hip (12.1%) | Total Injuries/Total AE × 1000 Total AE = games × Total players on ice (6) |
| McKnight, Ferrara, Czerwinska [23] | 1992 | Collegiate (Div. I) | (1). Loss of practice or game time because of injury/illness, (2). Injury that required sutures even if no time loss was involved, (3). Injury in which a fracture or dislocation/subluxation occurred even if the athlete was able to continue participation | Time Loss/Medical Attention Definition | Total: 10.22/1000 AE Games: 14.73/1000 game hours. Practice: 2.52/1000 practice hours | Person/Ice Impact 42%, impact with the boards 32%. The shoulder and knee had the highest rate of injury when compared to other body parts | Contusions and strains were the most common types of injury | number of Injuries/Total AE × 1000 (games and practice) |
| Pelletier, Montelpare, Stark [20] | 1993 | Canadian Inter-collegiate | “Any brain concussion causing cessation of the athlete’s participation for physical observation before return to play, any dental injury requiring professional attention, any injury/illness causing cessation of an athlete’s customary participation throughout the participation day following day of onset, or any injury/illness requiring substantive professional attention before the athlete’s return to competition.” | Time Loss/Medical Attention Definition | 19.95/1000 AE (player games) | Body checking 44.6%, collision (accidental) 28.8%, stick 12.2%, fighting 6.5%, illegal body check 5.8%, non-contact 2.2% | Sprains (31%) and contusions (21%) were the most common type of injury. Knees were most frequently injured (18.6%), followed by teeth and eyes (17.6%), and shoulders (14.9%), | Total Injuries/Total AE × 1000 Total AE = games × Total players on team (19) |
| Pettersson, Lorentzon [31] | 1993 | Swedish Elite League | “Injury was defined as any injury occurring during on-ice practice or games and requiring medical attention and treatment. Injuries causing the player to miss the next practice or game have been analyzed separately.” | Medical Attention Definition | 74.1/1000 game hours | Stick contact 26.1%, player contact 23.9%, puck contact 16%, collision with boards 7.2%, fall (no contact) 4% | Contusions, lacerations, sprains and strains are the most common mechanisms of injury. Knees were the most common joint injured followed by the thigh, groin and shoulder | Total Injuries/Total AE × 1000 Total AE = games × Total players on ice (6) |
| Stuart, Smith [21] | 1995 | United States Hockey League | “Injury was defined as an event that kept a player out of practice or competition for 24 h, required the attention of a team physician (e.g., suturing lacerations) and included all dental, eye and nerve injuries and concussions.” | Time Loss/Medical Attention Definition | Overall injury rate was 9.4/1000 player hours, game injury rate was 96.1/1000 player hours, practice injury rate was 3.9/1000 player hours | Collision 51%, stick contact 14%, skate/puck contact 11%, off-ice injuries 8% | Strains, lacerations and contusions were most common mechanism. Aside from the face, the shoulder, hip, lumbar spine and knee were the most common anatomical sites of injury | Total Injury/AE × 1000 = Practice Injury Rate; Practice AE = Practice Hours × Roster (25) Total injuries/Total AE × 1000; Total AE = number of games × Total players on ice (6) |
| Cunningham [32] | 1996 | University Games | “A recordable injury was defined as any incident occurring during warm-up or competition and which required medical attention, on-field management to enable continued participation, or removal from the playing field.” | Medical Attention | 33.5% of injuries in relation to total number playing the sport | Player collision | Muscle strains and hematoma (21.7%) | Number of injuries/number of players participating |
| Molsa, Airaksinen, Nasman, Torstila [33] | 1997 | Finnish National League, Finnish First Division | “An injury was defined as any trauma occurring during practices or games and causing absence from the next practice or game or needing treatment (ex. stitches), examination by a physician (ex. radiographs), or rehabilitation prescribed by a physician (ex. physical therapy). Injuries due to overuse were excluded.” | Time Loss/Medical Attention Definition | 66/1000 player-game hours, 36/1000 player game hours (Div. I) | Checking 29.7%, stick 14.6%, contact with opponent 14.6%, puck 7.9% | Contusions, strains and sprains were the most common type of injury, the knee joint and groin were the most common locations | Total Injury/AE × 1000 = Practice Injury Rate Practice AE = Practice Hours × Roster (21) Total Injuries/Total AE × 1000; Total AE = number of games × Total players on ice (6) |
| Pinto, Kuhn, Greenfield, Hawkins [34] | 1999 | Junior A Hokey Players (22 players) | “An injury was defined as any event that required the attention of a physician or trainer.” | Medical Attention Definition | 121/1000 player game hours | Contact with stick 16.2%, overuse 13.5% | Sprains/subluxations/dislocations were the most common, aside from the face, the shoulder and knee were the most common | Total Injury/AE × 1000 = Practice Injury Rate; Practice AE = Practice Hours x Roster (22) Total Injuries/Total AE x1000 Total AE = #games × Total players on ice (6) |
| Molsa, Kujala, Nasman, Lehtipuu, Airaksinen [35] | 2000 | Finnish Elite League (7 teams, 3 different decades) | “An injury was defined as any sudden trauma occurring during practice or game that led to examination and treatment by a physician.” Minor injuries requiring no absence were also included, but minor injuries needing no medical care and injuries due to overuse were excluded | Medical Attention Definition | Game injury rate increased from 54/1000 player hours in the 70’s to 83/1000 player hours in the 90’s, most common mechanism was collision | Checking, stick, falling, collision with opponent, puck, collision with boards | Contusions, sprains/strains and lacerations were the most common mechanisms of injury. The knee was the most common major injury of the lower quadrant | Player years of exposure, (Seasons × Teams × Players) × Practice Hours x Roster = Practice Injury Rate: Player years of exposure, (Seasons × Teams × Players) × Game Hours × Roster (6) = Game Injury Rate. |
| Flik, Lyman, Marx, [19] | 2005 | American Men’s Collegiate Ice Hockey (8 teams/1 season) | “An injury was defined specifically as any injurious episode that led to loss of participation in the immediate subsequent AE, whether it was a practice or game.” | Time Loss Definition | Overall injury rate was 4.9/1000 AE, 13.8/1000 AE games, 2.2/1000 AE practice | Collision with opponent 32.8%, collision with boards 18.6%, overuse 8%, puck 6.2% | Concussions were the most common, followed by knee (MCL) and shoulder injuries | Total Injury/AE × 1000 = Practice Injury Rate Practice AE = Practice Hours × Roster Est Total Injuries/Total AE × 1000; Total AE = number of games × Total player avg attendance |
| Agel, Dompier, Dick, Marshall [36] | 2007 | NCAA Men’s Ice Hockey (16 years of data: Div. I-III) | “A reportable injury in the ISS was defined as one that (1) occurred as a result of participation in an organized intercollegiate practice or competition and (2) required medical attention by a team certified athletic trainer or physician and (3) resulted in restriction of the student-athlete’s participation or performance for 1 or more calendar days beyond the day of injury. The injury definition was expanded in the ‘94–95’ academic year to include any dental injury occurring in an organized practice or game, regardless of time lost.” | Time Loss Definition | 16.27/1000 AE games, 1.96/1000 AE practice | Player contact 50%, other contact 39.6%, no contact 9.7% (game numbers). Injury was 8x higher in games. | Knee internal derangement (13.5%) was the most common lower extremity injury reported during games, followed by concussions and AC injuries. Whereas pelvis and hip strains (13.1%) were the most common injury reported at practice. | Total Injury/AE × 1000 = Practice Injury Rate; Practice AE = Practice Hours × Roster (26) Total Injuries/Total AE × 1000 Total AE = number of games × Total players (19) |
| Rishiraj, Lloyd-Smith, Lorenz, Michel [37] | 2009 | Men’s Varsity Ice Hockey (Canada) | “Any event, during team or team related game, practice, and/or activity (on or off the ice), requiring any attention by the team’s therapist and/or physician and subsequent game and/or practice time loss.” | Time Loss Definition | 3.7/1000 player game and practice exposure | Non-contact, ice/board contact, body contact | Sprains 20%, strains 20%, concussions 13% and contusions 12% | Total Injury/AE × 1000; Practice AE = Practice Hours × Roster Total Injuries/Total AE x1000 Total AE = number of games × Roster Selected |
| Kuzuhara, Shimamoto, Mase [38] | 2009 | Japanese Elite Team | “An injury was defined as any event that occurred during on-ice practices or games that required medical attention and treatment.” | Medical Attention Definition | 74.3/1000 player game hours, 11.7/1000 player-game hours for injuries resulting in any time loss, 11.2/1000 player-practice hours, 1.1/1000 player-practice hours for injuries resulting in any time loss | Overuse 52%, puck contact 21%, stick contact 15%, falling 12% | Contusions 35.4%, strains 15.6%, lacerations 9.3% | Overall injury rate (regardless of time loss): #of injuries/number of hours per 1000 player-hours number of injuries causing time loss (>1 day)/number of hours per 1000 player-hours Number of player: 2003 (20 players/game, 25 players/practice), 2004 (20 players/game, 37players/practice), 2005 (22 players/game, 32 players/practice) |
| Agel, Harvey [39] | 2010 | NCAA Men’s and Women’s Ice Hockey (Div. I and III) | Same as Dick et al. above | Time Loss Definition | 18.69/1000 AE games, 2.23/1000 AE practice for men, 12.10/1000 AE games, 2.90/1000 AE practice for women | Player contact 48% | The most common injury among men was concussion followed by shoulder and knee ligamentous in juries | Number of Injuries/Number of AE (games or practice × roster) × 1000 |
| Engebretsen, Steffen, Alonso, Dvorak, Junge, Meeuwisse, Mountjoy, Renstrom, Wlikinson [40] | 2010 | Olympic Sport | “An athlete was defined as injured or ill if he/she received medical attention regardless of the consequences with respect to absence from competition or training.” | Medical Attention Definition | A total injury rate of 111.8/1000 AE was reported for both males and females. A total of 276 males were registered with 44 total injuries (16%) in men’s elite ice hockey. | N/A | N/A | Number of Injuries/Athlete Exposure |
| Kerr, Dompier, Snook, Marshall, Klossner, Hainline, Corlette [41] | 2014 | NCAA Sports | “Any injury occurring during an organized intercollegiate practice or game.” (1982) “A reportable injury was defined as an injury that (1) occurred as a result of participation in an organized intercollegiate practice or competition, (2) required attention from an AT or physician, and (3) resulted in restriction of the student-athlete’s participation for 1 or more days beyond the day of injury.” Multiple injuries from one event could be included. In addition, AT’s were asked to include any dental injuries that occurred in an organized practice or game, regardless of time lost. 2003-onward). Beginning in 2009–2010 academic year, non-time loss injuries were also monitored. | Time Loss/Medical Attention Definition | N/A | N/A | N/A | Number of Injuries/AE (average team roster) × 1000 |
| McKay, Tufts, Shaffer, Meeuwisse [4] | 2014 | NHL Players (2006–2012) | “Any event captured by the IIE form, and restricted to those designated as practice-related or game related, resulting in one or more-man games lost. | Time Loss Definition | 15.6/1000 AE based on estimated AE’s. Based on recorded TOI *, the injury rates were roughly threefold higher at 49.4/1000 player-game hours | Body checking was the most common mechanism | Most commonly injured body regions were the head (16.8%), thigh (14%), and knee (13%) | Estimated AEs = 82 games × 19 players (including goalie) TOI (NHL.com) = number of injury events/sum of individual AE time |
| Tuominen, Stuart, Aubry, Kannus Parkkari [42] | 2015 | Men’s International Ice Hockey (2006–2013) | “The definition of an injury was made in accordance with the accepted international ice hockey norms: (1) Any injury sustained in a practice or a game that prevented the player from returning to the same practice or game, (2) any injury sustained in a practice or a game that caused the player to miss a subsequent practice or game, (3) a laceration that required medical attention, (4) all dental injuries, (5) all concussions, (6) all fractures | Time Loss/Medical Attention Definition | 14.2/1000 AE player games, 52.1/1000 AE player game hours For WC A-pool tournaments and Olympic games the injury rate was 16.3/1000 player-games, 69.6/1000 player-game hours | Body contact and puck contact were the mechanisms | Most common types of injuries were lacerations, sprains, strains, and contusions. The knee was the most commonly injured lower body segment, MCL was the most common, and the shoulder was the most common site of an upper body injury. | Player game injury rate (based on 22 players on each team): Number of injuries/number of players (two teams)/number of games × 1000, Player game-hour injury rate (based on 6 players on ice at once): number of injuries/number of players on ice at the same time (two teams)/number of games × 1000 |
| Kerr et al. [43] | 2015 | NCAA Ice Hockey | Injuries were defined as those that occurred in an organized NCAA-approved practice or competition and required medical attention by a physician or athletic trainer. An athlete-exposure was defined as one student-athlete’s participation in one practice or one competition. | Medical Attention Definition | 9.5/1000 AE | N/A | Concussions, contusions, fractures | Number of Injuries/Number of Athlete Exposures |
| Tuominen, Stuart, Aubry, Kannus, Parkkari [22] | 2016 | World Junior Hockey Players (ages 18–20) | “The definition of an injury was made in accordance with the accepted international ice hockey norms: (1) Any injury sustained in a practice or a game that prevented the player from returning to the same practice or game, (2) any injury sustained in a practice or a game that caused the player to miss a subsequent practice or game, (3) a laceration that required medical attention, (4) all dental injuries, (5) all concussions, (6) all fractures | Time Loss/Medical Attention Definition | 11/1000 AE player-games, 39.8/1000 player-game hours | Body checking 32%, stick 13%, and puck contact 13% | The knee was the most frequent site of lower body injury in WJ and U20 tournaments (33%), MCL sprain was most common, the shoulder was the most common upper body injury. | Player game injury rate (based on 20–22 players on each team): number of injuries/number of players (two teams)/number of games × 1000, Player game-hour injury rate (based on 6 players on ice at once): number of injuries/number of players on ice at the same time (two teams)/number of games × 1000 |
| Lynall, Mihalik, Pierpoint, Currie, Knowles, Wasserman, Dompier, Comstock, Marshall, Kerr [44] | 2018 | Collegiate Men’s and Women’s Hockey (2004–2005, 2013–2014) | “An injury that (1) occurred as a result of participation in an organized practice or competition; (2) required medical attention by a certified AT or physician; and (3) resulted in restriction of the student-athlete’s participation for 1 or more days beyond the day of injury. Since the 2007–2008 academic year, HS RIO has also captured all concussions, fractures, and dental injuries, regardless of time loss.” “Beginning in the 2009–2010 academic year, the NCAA-ISP also began to monitor all non–time-loss injuries. A non–time-loss injury was defined as any injury that was evaluated or treated (or both) by an AT or physician but did not result in restriction from participation beyond the day of injury.” | Medical Attention/Time Loss Definition | Collegiate Men: 13.45/1000 AE | Collision | Strains/Sprains | Total Injuries/Total Athlete Exposure |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Donskov, A.S.; Humphreys, D.; Dickey, J.P. What Is Injury in Ice Hockey: An Integrative Literature Review on Injury Rates, Injury Definition, and Athlete Exposure in Men’s Elite Ice Hockey. Sports 2019, 7, 227. https://doi.org/10.3390/sports7110227
Donskov AS, Humphreys D, Dickey JP. What Is Injury in Ice Hockey: An Integrative Literature Review on Injury Rates, Injury Definition, and Athlete Exposure in Men’s Elite Ice Hockey. Sports. 2019; 7(11):227. https://doi.org/10.3390/sports7110227
Chicago/Turabian StyleDonskov, Anthony S., David Humphreys, and James P. Dickey. 2019. "What Is Injury in Ice Hockey: An Integrative Literature Review on Injury Rates, Injury Definition, and Athlete Exposure in Men’s Elite Ice Hockey" Sports 7, no. 11: 227. https://doi.org/10.3390/sports7110227
APA StyleDonskov, A. S., Humphreys, D., & Dickey, J. P. (2019). What Is Injury in Ice Hockey: An Integrative Literature Review on Injury Rates, Injury Definition, and Athlete Exposure in Men’s Elite Ice Hockey. Sports, 7(11), 227. https://doi.org/10.3390/sports7110227







