Validity and Reliability of a New Wearable Chest Strap to Estimate Respiratory Frequency in Elite Soccer Athletes
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Setting
2.3. Participants
2.4. Variables
2.5. Data Sources/Measurement
2.5.1. Exercise Test
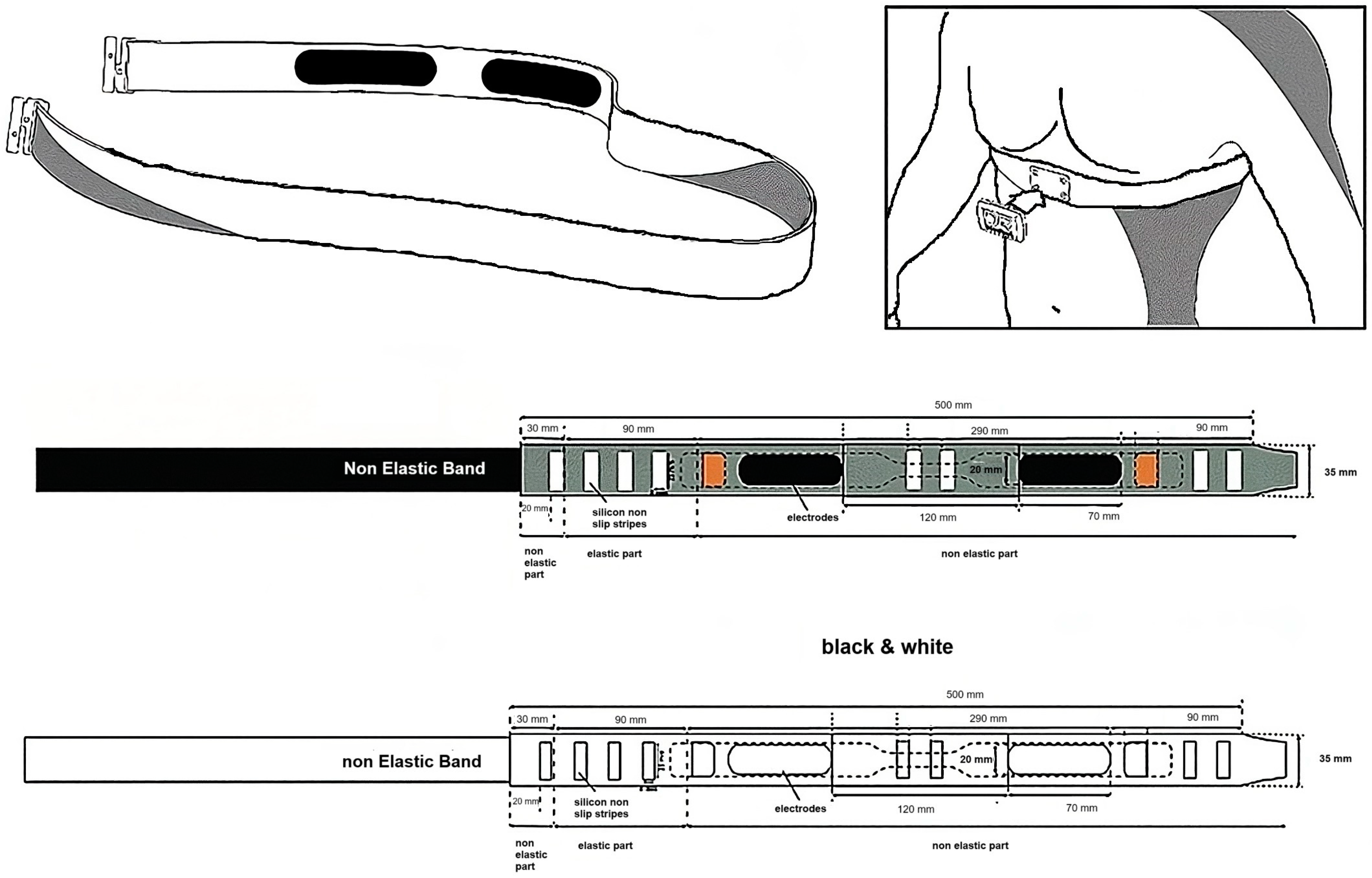
2.5.2. Novel Wearable Device Description
- (i)
- Moisten the heart rate electrodes by dampening the sensors located on the inner side of the chest strap.
- (ii)
- Secure the strap around the chest, ensuring the four front contacts are centered. Adjust for comfort, making sure it is neither too tight nor likely to slip.
- (iii)
- Attach the transmitter module to the strap using the clip.
- Transmission module with an integrated BLE radio system;
- Heart rate reading module;
- Respiratory signal amplification section;
- Inertial system for energy-efficient operation control;
- Auxiliary acoustic signaling system.
2.5.3. Data Acquisition
2.6. Sample Size
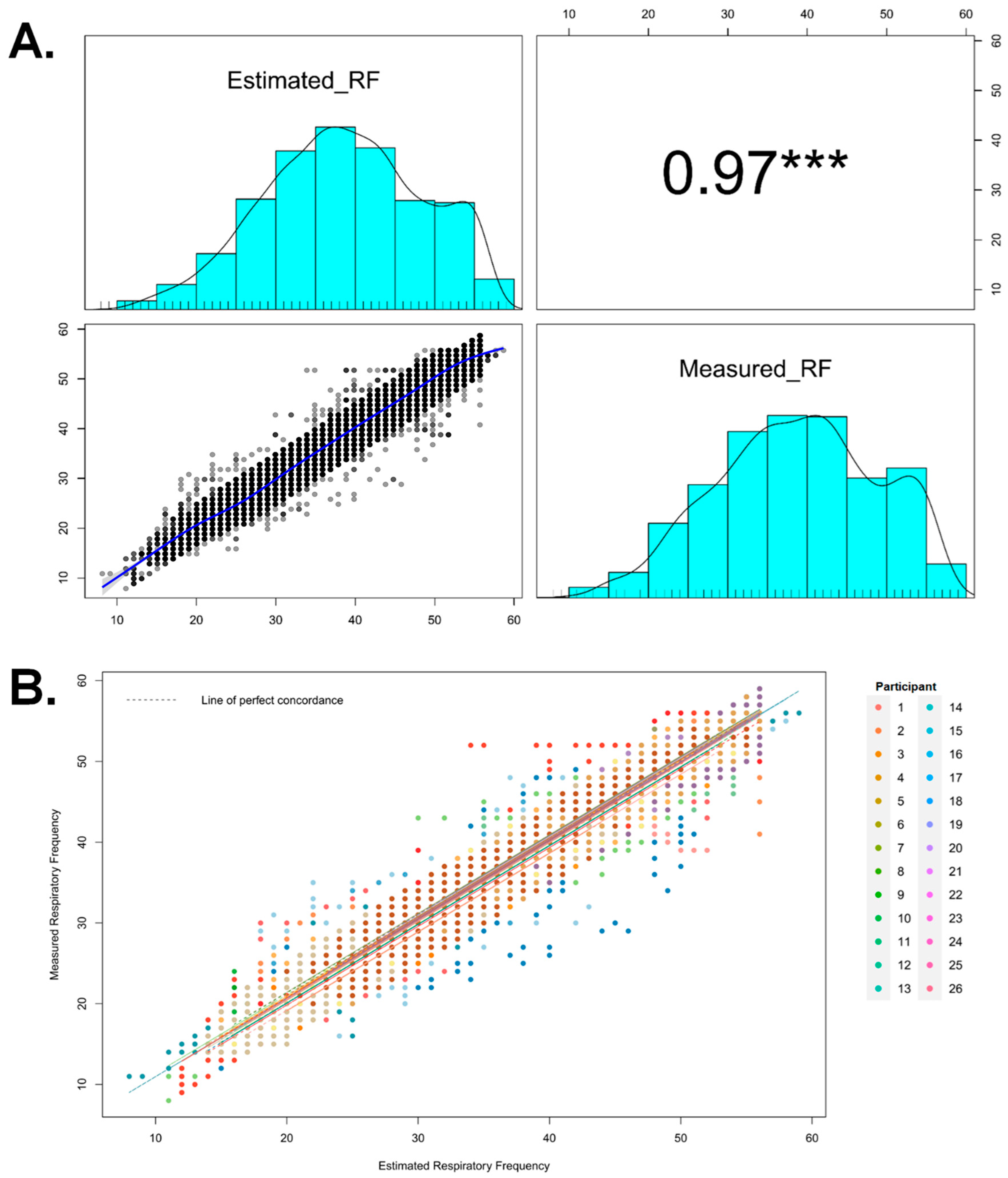
2.7. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lee, E.C.; Fragala, M.S.; Kavouras, S.A.; Queen, R.M.; Pryor, J.L.; Casa, D.J. Biomarkers in Sports and Exercise: Tracking Health, Performance, and Recovery in Athletes. J. Strength Cond. Res. 2017, 31, 2920–2937. [Google Scholar] [CrossRef] [PubMed]
- Bestwick-Stevenson, T.; Toone, R.; Neupert, E.; Edwards, K.; Kluzek, S. Assessment of Fatigue and Recovery in Sport: Narrative Review. Int. J. Sports Med. 2022, 43, 1151–1162. [Google Scholar] [CrossRef] [PubMed]
- Bonilla, D.A.; Perez-Idarraga, A.; Odriozola-Martinez, A.; Kreider, R.B. The 4R’s Framework of Nutritional Strategies for Post-Exercise Recovery: A Review with Emphasis on New Generation of Carbohydrates. Int. J. Environ. Res. Public Health 2020, 18, 103. [Google Scholar] [CrossRef]
- Bobba-Alves, N.; Juster, R.P.; Picard, M. The energetic cost of allostasis and allostatic load. Psychoneuroendocrinology 2022, 146, 105951. [Google Scholar] [CrossRef]
- Guidi, J.; Lucente, M.; Sonino, N.; Fava, G.A. Allostatic Load and Its Impact on Health: A Systematic Review. Psychother. Psychosom. 2021, 90, 11–27. [Google Scholar] [CrossRef]
- Manresa-Rocamora, A.; Flatt, A.A.; Casanova-Lizon, A.; Ballester-Ferrer, J.A.; Sarabia, J.M.; Vera-Garcia, F.J.; Moya-Ramon, M. Heart rate-based indices to detect parasympathetic hyperactivity in functionally overreached athletes. A meta-analysis. Scand. J. Med. Sci. Sports 2021, 31, 1164–1182. [Google Scholar] [CrossRef]
- Manresa-Rocamora, A.; Sarabia, J.M.; Javaloyes, A.; Flatt, A.A.; Moya-Ramon, M. Heart Rate Variability-Guided Training for Enhancing Cardiac-Vagal Modulation, Aerobic Fitness, and Endurance Performance: A Methodological Systematic Review with Meta-Analysis. Int. J. Environ. Res. Public Health 2021, 18, 10299. [Google Scholar] [CrossRef] [PubMed]
- Impellizzeri, F.M.; Marcora, S.M.; Coutts, A.J. Internal and External Training Load: 15 Years On. Int. J. Sports Physiol. Perform. 2019, 14, 270–273. [Google Scholar] [CrossRef] [PubMed]
- Davletyarova, K.; Vacher, P.; Nicolas, M.; Kapilevich, L.V.; Mourot, L. Associations Between Heart Rate Variability-Derived Indexes and Training Load: Repeated Measures Correlation Approach Contribution. J. Strength Cond. Res. 2022, 36, 2005–2010. [Google Scholar] [CrossRef]
- Tran, D. Cardiopulmonary Exercise Testing. Methods Mol. Biol. 2018, 1735, 285–295. [Google Scholar] [CrossRef]
- Sánchez-Rojas, I.A.; Mendoza Romero, D.; Paola Argüello-Gutiérrez, Y.; Castro-Jiménez, L.E.; Triana-Reina, H.R.; Perez-Cebreros, E.A.; Petro, J.L.; Bonilla, D.A. Valores de referencia para las pruebas de Cooper y de 20 m de ida y vuelta en población residente en altitud elevada. [Reference values for Cooper and Shuttle Run Tests in population living at high altitude]. RICYDE Rev. Int. Cienc. Deporte 2021, 17, 221–233. [Google Scholar] [CrossRef]
- Nicolo, A.; Marcora, S.M.; Sacchetti, M. Respiratory frequency is strongly associated with perceived exertion during time trials of different duration. J. Sports Sci. 2016, 34, 1199–1206. [Google Scholar] [CrossRef]
- Nicolo, A.; Massaroni, C.; Schena, E.; Sacchetti, M. The Importance of Respiratory Rate Monitoring: From Healthcare to Sport and Exercise. Sensors 2020, 20, 6396. [Google Scholar] [CrossRef] [PubMed]
- Nicolo, A.; Massaroni, C.; Passfield, L. Respiratory Frequency during Exercise: The Neglected Physiological Measure. Front. Physiol. 2017, 8, 922. [Google Scholar] [CrossRef] [PubMed]
- di Paco, A.; Dube, B.P.; Laveneziana, P. Changes in Ventilatory Response to Exercise in Trained Athletes: Respiratory Physiological Benefits Beyond Cardiovascular Performance. Arch. Bronconeumol. 2017, 53, 237–244. [Google Scholar] [CrossRef]
- Di Paco, A.; Catapano, G.A.; Vagheggini, G.; Mazzoleni, S.; Micheli, M.L.; Ambrosino, N. Ventilatory response to exercise of elite soccer players. Multidiscip. Respir. Med. 2014, 9, 20. [Google Scholar] [CrossRef]
- Romano, C.; Nicolo, A.; Innocenti, L.; Sacchetti, M.; Schena, E.; Massaroni, C. Design and Testing of a Smart Facemask for Respiratory Monitoring during Cycling Exercise. Biosensors 2023, 13, 369. [Google Scholar] [CrossRef]
- Romano, C.; Nicolo, A.; Innocenti, L.; Bravi, M.; Miccinilli, S.; Sterzi, S.; Sacchetti, M.; Schena, E.; Massaroni, C. Respiratory Rate Estimation during Walking and Running Using Breathing Sounds Recorded with a Microphone. Biosensors 2023, 13, 637. [Google Scholar] [CrossRef]
- Massaroni, C.; Nicolo, A.; Girardi, M.; La Camera, A.; Schena, E.; Sacchetti, M.; Silvestri, S.; Taffoni, F. Validation of a Wearable Device and an Algorithm for Respiratory Monitoring During Exercise. IEEE Sens. J. 2019, 19, 4652–4659. [Google Scholar] [CrossRef]
- Massaroni, C.; Nicolo, A.; Lo Presti, D.; Sacchetti, M.; Silvestri, S.; Schena, E. Contact-Based Methods for Measuring Respiratory Rate. Sensors 2019, 19, 908. [Google Scholar] [CrossRef]
- Force, E.R.S.T.; Palange, P.; Ward, S.A.; Carlsen, K.H.; Casaburi, R.; Gallagher, C.G.; Gosselink, R.; O’Donnell, D.E.; Puente-Maestu, L.; Schols, A.M.; et al. Recommendations on the use of exercise testing in clinical practice. Eur. Respir. J. 2007, 29, 185–209. [Google Scholar] [CrossRef]
- Vandenbroucke, J.P.; von Elm, E.; Altman, D.G.; Gotzsche, P.C.; Mulrow, C.D.; Pocock, S.J.; Poole, C.; Schlesselman, J.J.; Egger, M.; Initiative, S. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): Explanation and elaboration. PLoS Med. 2007, 4, e297. [Google Scholar] [CrossRef] [PubMed]
- Sietsema, K.E.; Stringer, W.W.; Sue, D.Y.; Ward, S. Wasserman & Whipp’s: Principles of Exercise Testing and Interpretation: Including Pathophysiology and Clinical Applications, 6th ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2020. [Google Scholar]
- Pan, J.; Tompkins, W.J. A real-time QRS detection algorithm. IEEE Trans. Biomed. Eng. 1985, 32, 230–236. [Google Scholar] [CrossRef] [PubMed]
- Nagele, P. Misuse of standard error of the mean (SEM) when reporting variability of a sample. A critical evaluation of four anaesthesia journals. Br. J. Anaesth. 2003, 90, 514–516. [Google Scholar] [CrossRef]
- Lang, T. Twenty statistical errors even you can find in biomedical research articles. Croat. Med. J. 2004, 45, 361–370. [Google Scholar]
- O’Shaughnessy, P.; Cavanaugh, J.E. Performing T-tests to Compare Autocorrelated Time Series Data Collected from Direct-Reading Instruments. J. Occup. Environ. Hyg. 2015, 12, 743–752. [Google Scholar] [CrossRef] [PubMed]
- Dürre, A.; Fried, R.; Liboschik, T. Robust estimation of (partial) autocorrelation. Wiley Interdiscip. Rev. Comput. Stat. 2015, 7, 205–222. [Google Scholar] [CrossRef]
- Nuzzo, R.L. An Introduction to Bayesian Data Analysis for Correlations. PM&R 2017, 9, 1278–1282. [Google Scholar] [CrossRef]
- Gómez-Miranda, L.M.; Bimbela, J.E.; Rodríguez-Chávez, Á.; Merlo, R.; Palma, L.H.; Bonilla, D.A. Exploring the validity of perceived velocity in lower-limb resistance exercises with a cluster-set configuration. Retos 2024, 60, 561–567. [Google Scholar] [CrossRef]
- Bernards, J.R.; Sato, K.; Haff, G.G.; Bazyler, C.D. Current Research and Statistical Practices in Sport Science and a Need for Change. Sports 2017, 5, 87. [Google Scholar] [CrossRef]
- R Core Team. R: A Language and Environment for Statistical Computing, v4.0.2; R Foundation for Statistical Computing: Vienna, Austria, 2017.



| Communication Type | Bluetooth (BLE) Long Range * |
|---|---|
| Allowable distance | 130 m (real-time); greater distance under datalogger management (automatic switch) |
| Features and function mode | Real-time transmission of heart rate (HR) and breath rate (BR), with datalogger function (maximum 1 h) and automatic management/data download upon returning to real-time distance. |
| Data measurement | Direct measurement of heart rate and respiratory frequency (breath rate) with estimation of VO2 and VE |
| Battery type | Button-style CR 2025 |
| Battery lifetime | Typically 100 h (variable with usage distance) |
| Operating temperature | −10 °C to +50 °C (14 °F to 122 °F) |
| Device material | ABS, Nylon PA12, tinned coated brass |
| Device weight | 30 g (with battery installed) |
| Belt materials | Polyamide and elastane with anti-slip silicone prints |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Di Paco, A.; Bonilla, D.A.; Perrotta, R.; Canonico, R.; Cione, E.; Cannataro, R. Validity and Reliability of a New Wearable Chest Strap to Estimate Respiratory Frequency in Elite Soccer Athletes. Sports 2024, 12, 277. https://doi.org/10.3390/sports12100277
Di Paco A, Bonilla DA, Perrotta R, Canonico R, Cione E, Cannataro R. Validity and Reliability of a New Wearable Chest Strap to Estimate Respiratory Frequency in Elite Soccer Athletes. Sports. 2024; 12(10):277. https://doi.org/10.3390/sports12100277
Chicago/Turabian StyleDi Paco, Adriano, Diego A. Bonilla, Rocco Perrotta, Raffaele Canonico, Erika Cione, and Roberto Cannataro. 2024. "Validity and Reliability of a New Wearable Chest Strap to Estimate Respiratory Frequency in Elite Soccer Athletes" Sports 12, no. 10: 277. https://doi.org/10.3390/sports12100277
APA StyleDi Paco, A., Bonilla, D. A., Perrotta, R., Canonico, R., Cione, E., & Cannataro, R. (2024). Validity and Reliability of a New Wearable Chest Strap to Estimate Respiratory Frequency in Elite Soccer Athletes. Sports, 12(10), 277. https://doi.org/10.3390/sports12100277









