Psychodynamic Therapies for the Treatment of Substance Addictions: A PRISMA Meta-Analysis
Abstract
1. Introduction
1.1. Rationale
1.2. Objectives
2. Method
2.1. Eligibility Criteria
2.2. Information Sources
2.3. Search Strategy
- Psychodynamic AND (addiction OR substance use disorder)
- (Psychodynamic OR psychoanalytic OR psychodyn* OR psychoan* OR “ego psychology” OR “self-psychology” OR “object relation” OR “intensive expressive” OR “interactional group”) AND (addiction OR substance dependence OR “substance use disorder” OR alcohol OR heroin OR opioid OR cocaine OR marijuana OR hallucinogen OR barbiturates OR methadone OR ketamine OR amphetamines OR methamphetamine OR MDMA) AND (therapy OR psychotherapy OR treatment).
2.4. Selection Process
- Screening of titles and abstracts;
- Full reading of the articles;
- Analysis of data;
2.5. Data Collection Process
2.6. Data Items
- Substance use:Grams/liter per week;Reported use or reported abstinence.
- Other symptomatic conditions:Pre-post evaluation of co-present psychological problems;Assessment of how comorbidities evolve over the time of treatment.
- Participation:Participation or non-participation frequency;Completer and non-completer report.
2.7. Study Risk of Bias Assessment
2.8. Effect Measures
2.9. Synthesis Methods
2.10. Reporting Bias Assessment
2.11. Certainty Assessment
3. Results
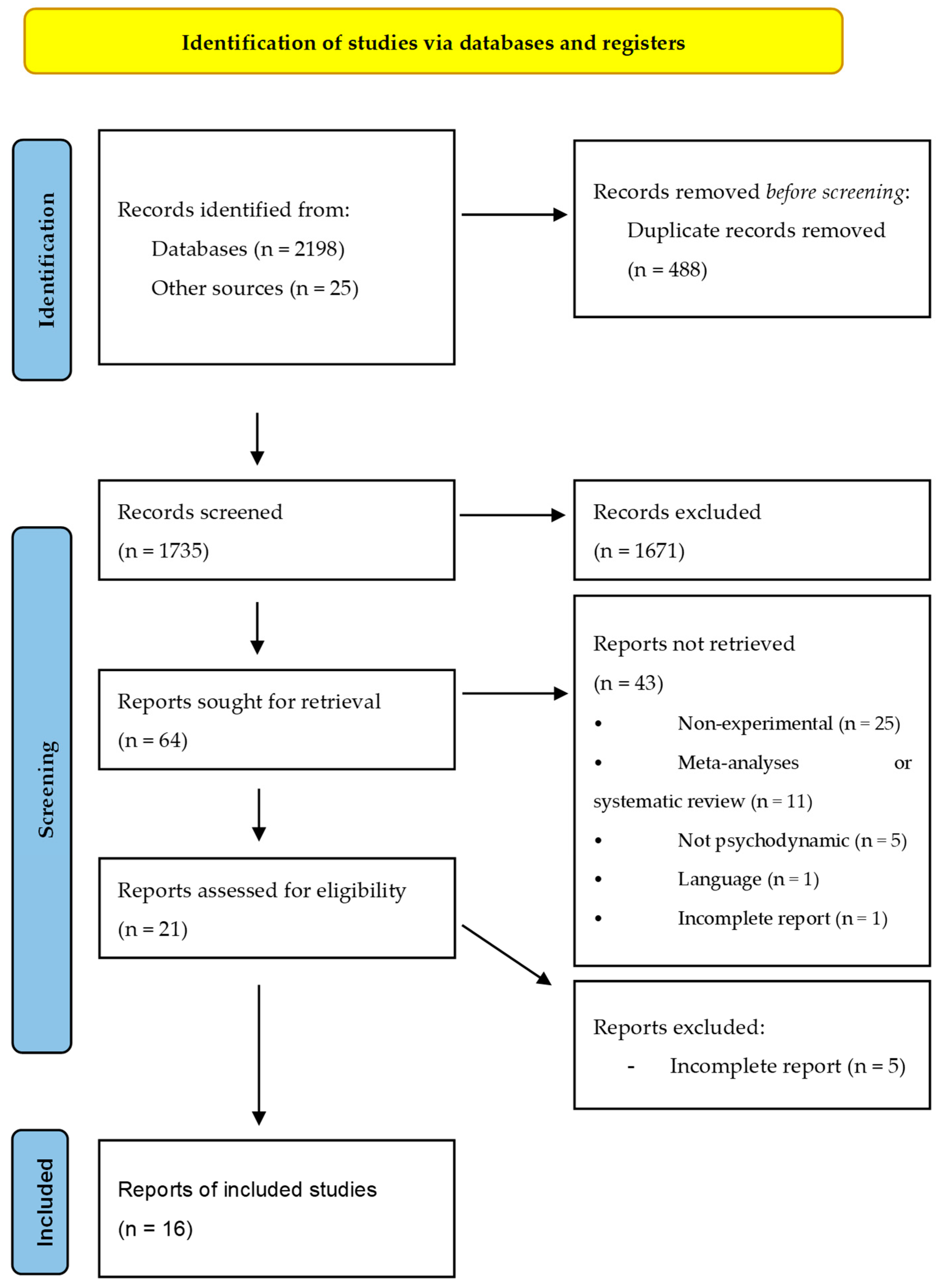
3.1. Study Selection
3.2. Study Characteristics
3.3. Risk of Bias in Studies
3.4. Results of Individual Studies
3.5. Results of Syntheses
3.5.1. Risk of Bias
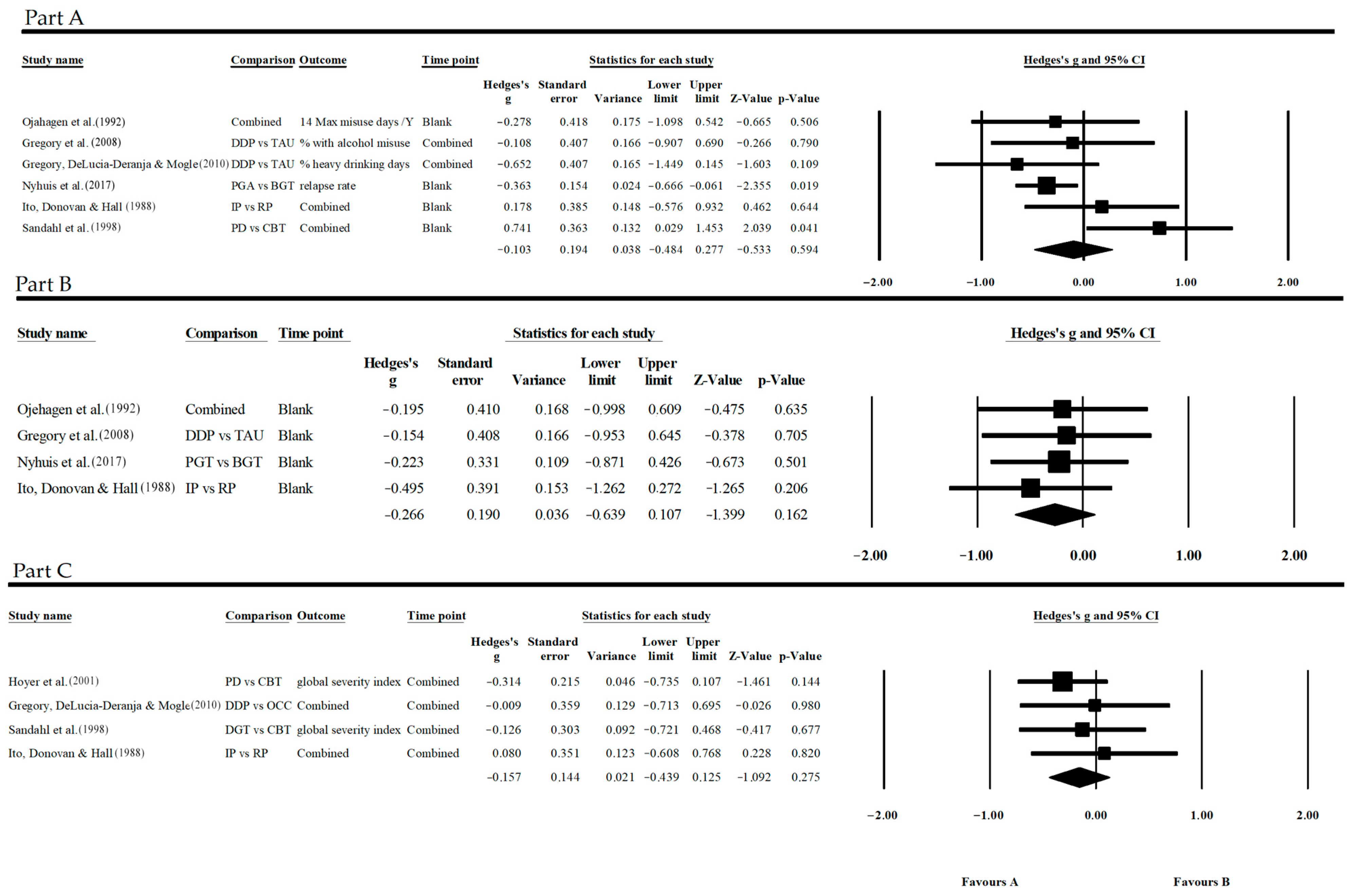
3.5.2. Alcohol Results
- Substance use: G = −0.103, p = 0.594, CI = 95%;
- Participation: G = −0.266, p = 0.162, CI = 95%;
- Other symptomatic conditions: G = −0.157, p = 0.275, CI = 95%.
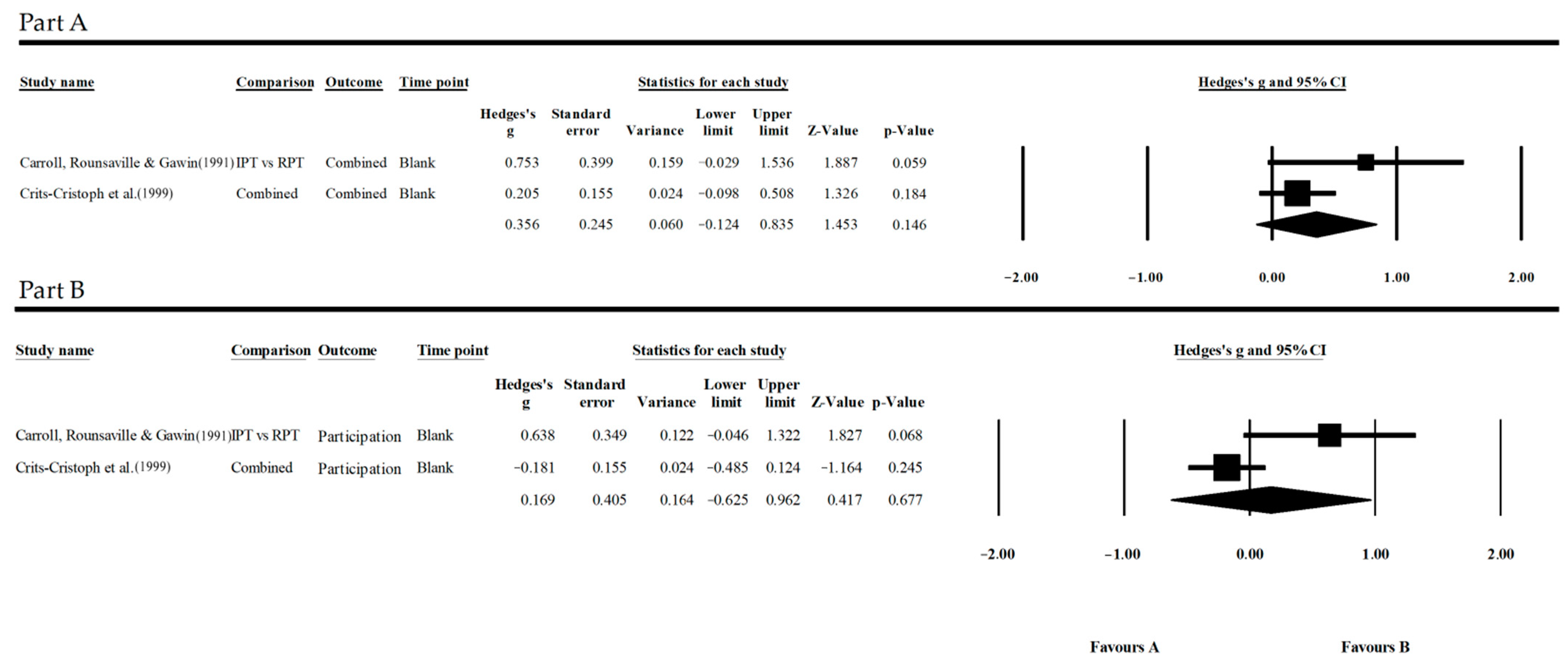
3.5.3. Cocaine Results
- Substance use: G = 0.276, p = 0.055, CI = 95%;
- Participation: G = 0.169, p = 0.677, CI = 95%.
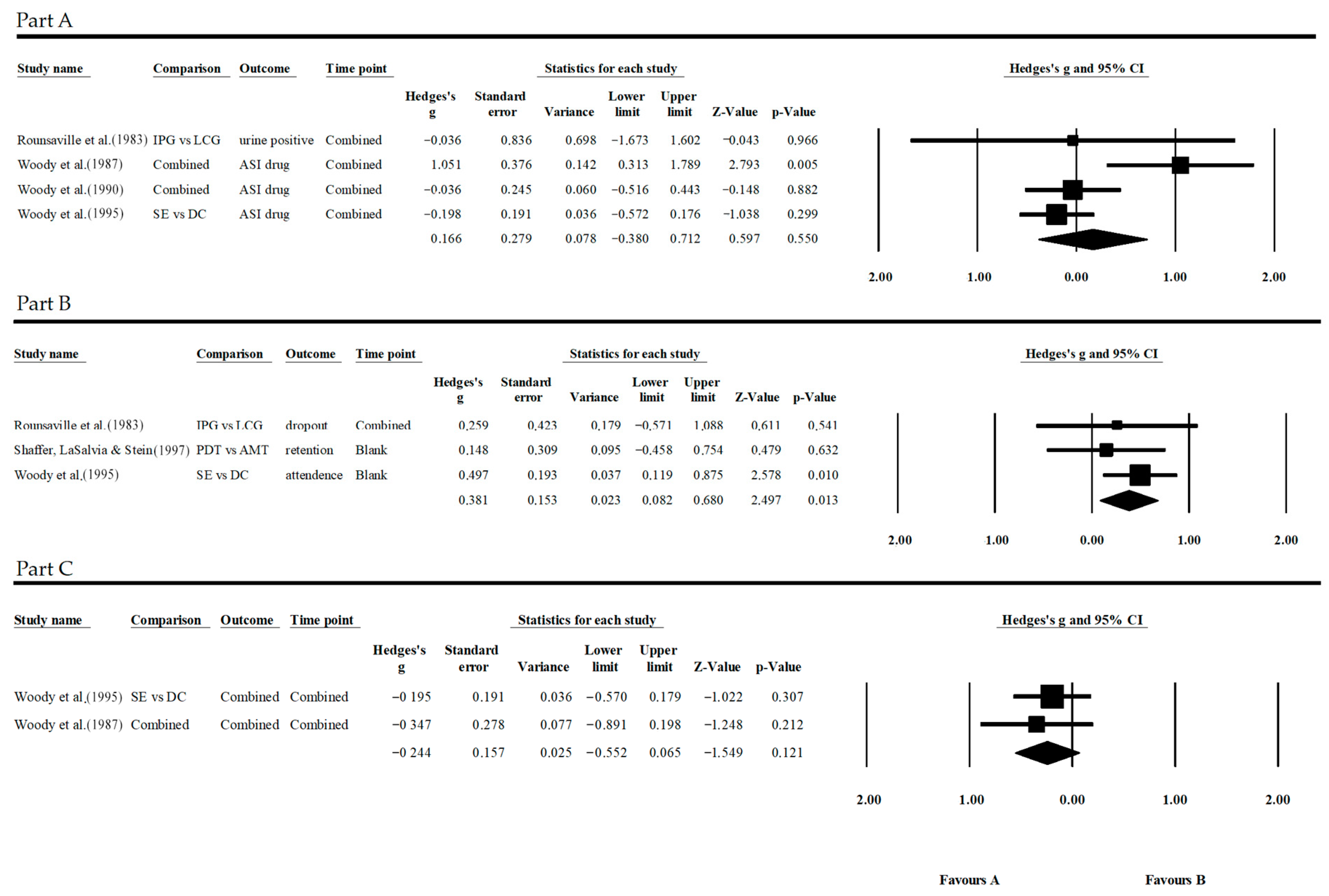
3.5.4. Opioid Results
- Substance use: G = 0.025, p = 0.855, CI = 95%;
- Participation: G = 0.381, p = 0.013, CI = 95%;
- Other symptomatic condition: G = −0.244, p = 0.121, CI = 95%.
3.6. Heterogeneity
3.7. Publication Bias
3.8. Certainty Assessment
4. Discussion
Limits
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Leichsenring, F.; Luyten, P.; Hilsenroth, M.J.; Abbass, A.; Barber, J.P.; Keefe, J.R.; Leweke, F.; Rabung, S.; Steinert, C. Psychodynamic therapy meets evidence-based medicine: A systematic review using updated criteria. Lancet Psychiatry 2015, 2, 648–660. [Google Scholar] [CrossRef] [PubMed]
- Glower, E. On the Aetiology of Drug Addiction. Int. J. Psychoanal. 1932, 13, 298–328. [Google Scholar]
- Radó, S. The psychoanalysis of pharmacothymia (drug addiction). J. Subst. Abuse Treat. 1933, 1, 60–68. [Google Scholar] [CrossRef]
- Knight, R.P. The psychodynamics of chronic alcoholism. J. Nerv. Ment. 1937, 86, 538–548. [Google Scholar] [CrossRef]
- Simmel, E. Alcoholism and addiction. Psychoanal. Q. 1948, 17, 6–31. [Google Scholar] [CrossRef]
- Yalisove, D.L. Essential Papers on Addiction; New York University Press: New York, NY, USA; London, UK, 1997. [Google Scholar]
- Potik, D. Psychodynamic Approaches for Treatment of Drug Abuse and Addiction: Theory and Treatment; Routledge: New York, NY, USA, 2021. [Google Scholar]
- Gibbons, M.B.; Crits-Christoph, P.; Hearon, B. The empirical status of psychodynamic therapies. Annu. Rev. Clin. Psychol. 2008, 4, 93–108. [Google Scholar] [CrossRef]
- Fonagy, P. The effectiveness of psychodynamic psychotherapies: An update. World Psychiatry 2015, 14, 137–150. [Google Scholar] [CrossRef]
- Leichsenring, F.; Leweke, F.; Klein, S.; Steinert, C. The empirical status of psychodynamic psychotherapy—An update: Bambi’s alive and kicking. Psychother. Psychosom. 2015, 84, 129–148. [Google Scholar] [CrossRef]
- Leichsenring, F.; Abbass, A.; Heim, N.; Keefe, J.R.; Kisely, S.; Luyten, P.; Rabung, S.; Steinert, C. The status of psychodynamic psychotherapy as an empirically supported treatment for common mental disorders—An umbrella review based on updated criteria. World Psychiatry 2023, 22, 286–304. [Google Scholar] [CrossRef]
- Leichsenring, F.; Steinert, C.; Rabung, S.; Ioannidis, J.P.A. The efficacy of psychotherapies and pharmacotherapies for mental disorders in adults: An umbrella review and meta-analytic evaluation of recent meta-analyses. World Psychiatry 2022, 21, 133–145. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, e1–e34. [Google Scholar] [CrossRef] [PubMed]
- Crits-Christoph, P.; Siqueland, L.; Blaine, J.; Frank, A.; Luborsky, L.; Onken, L.S.; Muenz, L.R.; Thase, M.E.; Weiss, R.D.; Gastnd, D.R.; et al. Psychosocial treatments for cocaine dependence: National Institute on Drug Abuse Collaborative Cocaine Treatment Study. Arch. Gen. Psychiatry 1999, 56, 493–502. [Google Scholar] [CrossRef]
- De Crescenzo, F.; Ciabattini, M.; D’Alò, G.L.; De Giorgi, R.; Del Giovane, C.; Cassar, C.; Janiri, L.; Clark, N.; Ostacher, M.J.; Cipriani, A. Comparative efficacy and acceptability of psychosocial interventions for individuals with cocaine and amphetamine addiction: A systematic review and network meta-analysis. PLoS Med. 2018, 15, e1002715. [Google Scholar] [CrossRef]
- Leichsenring, F.; Rabung, S. Long-term psychodynamic psychotherapy in complex mental disorders: Update of a meta-analysis. BJPsych 2011, 199, 15–22. [Google Scholar] [CrossRef]
- Shaffer, H.J.; LaSalvia, T.A.; Stein, J.P. Comparing Hatha yoga with dynamic group psychotherapy for enhancing methadone maintenance treatment: A randomized clinical trial. Altern. Ther. Health Med. 1997, 3, 57–66. [Google Scholar] [PubMed]
- Kadden, R.M.; Cooney, N.L.; Ronald, M.; Litt, M.D.; Getter, H. Matching alcoholics to coping skills or interactional therapies: Two-year follow-up results. J. Consult. Clin. Psychol. 1991, 59, 598–601. [Google Scholar] [CrossRef]
- Woody, G.E.; McLellan, A.T.; Luborsky, L.; O’Brien, C.P. Psychotherapy in community methadone programs: A validation study. Am. J. Psychiatry 1995, 152, 1302–1308. [Google Scholar] [CrossRef]
- Frederickson, J.; DenDooven, B.; Abbass, A.; Solbakken, O.A.; Rousmaniere, T. Pilot study: An inpatient drug rehabilitation program based on intensive short-term dynamic psychotherapy. J. Addict. Dis. 2019, 37, 195–201. [Google Scholar] [CrossRef]
- Kang, S.-Y.; Kleinman, P.H.; Woody, G.E.; Millman, R.B.; Todd, T.C.; Kemp, J.; Lipton, D.S. Crack and Cocaine Abusers in Outpatient Psychotherapy. In NIDA Research Monograph 104; National Institute on Drug Abuse: Rockville, MD, USA, 1990. [Google Scholar]
- Kang, S.-Y.; Kleinman, P.H.; Woody, G.E.; Millman, R.B.; Todd, T.C.; Kemp, J.; Lipton, D.S. Outcomes for cocaine abusers after once-a-week psychosocial therapy. Am. J. Psychiatry 1991, 148, 630–635. [Google Scholar] [CrossRef]
- Regier, D.A.; Farmer, M.E.; Rae, D.S.; Locke, B.Z.; Keith, S.J.; Judd, L.L.; Goodwin, F.K. Comorbidity of mental disorders with alcohol and other drug abuse. Results from the Epidemiologic Catchment Area (ECA) Study. JAMA 1990, 264, 2511–2518. [Google Scholar] [CrossRef]
- NIDA. Common Comorbidities with Substance Use Disorders Research Report, Introduction. Available online: https://nida.nih.gov/publications/research-reports/common-comorbidities-substance-use-disorders/introduction (accessed on 19 December 2022).
- Luborsky, L.; Mark, D. Short-term supportive-expressive psychoanalytic psychotherapy. In Handbook of Short-Term. Dynamic Psychotherapy; Crits-Christoph, P., Barber, J.P., Eds.; Basic Books: New York, NY, USA, 1991; pp. 110–136. [Google Scholar]
- Khantzian, E.J.; Weegman, M. Treating Addiction: Beyond the Pain; Rowman & Littlefield Publishers: Lanham, MD, USA, 2018. [Google Scholar]
- Gregory, R.J.; DeLucia-Deranja, E.; Mogle, J.A. Dynamic deconstructive psychotherapy versus optimized community care for borderline personality disorder co-occurring with alcohol use disorders: A 30-month follow-up. J. Nerv. Ment. 2010, 198, 292–298. [Google Scholar] [CrossRef] [PubMed]
- Flores, P.J. Group Psychotherapy with Addicted Populations: An Integration of Twelve-Step and Psychodynamic Theory, 3rd ed.; The Haworth Press: Binghamton, NY, USA, 2007. [Google Scholar]
- Center for Substance Abuse Treatment. Brief Interventions and Brief Therapies for Substance Abuse. In Treatment Improvement Protocol (TIP) Series, N. 34, HHS Publication No. (SMA); Substance Abuse and Mental Health Services Administration: Rockville, MD, USA, 1999. [Google Scholar]
- Higgins, J.P.T.; Thomas, J.; Chandler, J.; Cumpston, M.; Li, T.; Page, M.J.; Welch, V.A. (Eds.) Cochrane Handbook for Systematic Reviews of Interventions Version 6.3; Updated February 2022; Cochrane: UK, London, 2022; Available online: www.training.cochrane.org/handbook (accessed on 25 March 2022).
- Hedges, L.V.; Higgins, J.P.T.; Rothstein, H.R.; Borenstein, M. Introduction to Meta-Analysis. Wiley & Sons: Hoboken, NJ, USA, 2009. [Google Scholar]
- Borenstein, M.; Hedges, L.; Higgins, J.; Rothstein, H. Comprehensive Meta-Analysis Version 3; Biostat: Englewood, NJ, USA, 2022. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Academic Press: New York, NY, USA, 1969; pp. 101–105. [Google Scholar]
- Gregory, R.J.; Chlebowski, S.; Kang, D.; Remen, A.L.; Soderberg, M.G.; Stepkovitch, J.; Virk, S. A controlled trial of psychodynamic psychotherapy for co-occurring borderline personality disorder and alcohol use disorder. Psychother. Theor. Res. Pract. Train. 2008, 45, 28. [Google Scholar] [CrossRef] [PubMed]
- Ito, J.R.; Donovan, D.M.; Hall, J.J. Relapse prevention in alcohol aftercare: Effects on drinking outcome, change process, and aftercare attendance. Br. J. Addict. 1988, 83, 171–181. [Google Scholar] [CrossRef] [PubMed]
- Nyhuis, P.W.; Niederhofer, E.; Scherbaum, N.; Schifano, F.; Bonnet, U.; Dembski, N.; Niederhofer, A.; Specka, M.; Tenbergen, M. Effectiveness of Psychoanalytic-Interactional Group Therapy vs. Behavioral Group Therapy in Routine Outpatient Treatment of Alcohol-Dependent Patients. Subst. Use Misuse 2018, 53, 426–431. [Google Scholar] [CrossRef] [PubMed]
- Sandahl, C.; Herlitz, K.; Ahlin, G.; Rönnberg, S. Time-limited group psychotherapy for moderately alcohol dependent patients: A randomized controlled clinical trial. Psychother. Res. 1998, 8, 361–378. [Google Scholar] [CrossRef]
- Ojehagen, A.; Berglund, M.; Appel, C.P.; Andersson, K.; Nilsson, B.; Skjaerris, A.; Wedlin-Toftenow, A.M. A randomized study of long-term out-patient treatment in alcoholics. Psychiatric treatment versus multimodal behavioural therapy, during 1 versus 2 years of treatment. Alcohol Alcohol. 1992, 27, 649–658. [Google Scholar]
- Carroll, K.M.; Rounsaville, B.J.; Gawin, F.H. A comparative trial of psychotherapies for ambulatory cocaine abusers: Relapse prevention and interpersonal psychotherapy. AJDAA 1991, 17, 229–247. [Google Scholar] [CrossRef]
- Rounsaville, B.J.; Glazer, W.; Wilber, C.H.; Weissman, M.M.; Kleber, H.D. Short-term interpersonal psychotherapy in methadone-maintained opiate addicts. Arch. Gen. Psychiatry 1983, 40, 629–636. [Google Scholar] [CrossRef]
- Woody, G.E.; Luborsky, L.; McLellan, A.T.; O’Brien, C.P.; Beck, A.T.; Blaine, J.; Herman, I.; Hole, A. Psychotherapy for opiate addicts. Does it help? Arch. Gen. Psychiatry 1983, 40, 639–645. [Google Scholar] [CrossRef]
- Hoyer, J.; Fecht, J.; Lauterbach, W.; Schneider, R. Changes in conflict, symptoms, and well-being during psychodynamic and cognitive-behavioral alcohol inpatient treatment. Psychother. Psychosom. 2001, 70, 209–215. [Google Scholar] [CrossRef]
- Lappan, S.N.; Brown, A.W.; Hendricks, P.S. Dropout rates of in-person psychosocial substance use disorder treatments: A systematic review and meta-analysis. Addiction 2020, 115, 201–217. [Google Scholar] [CrossRef] [PubMed]
- Marlatt, G.A.; Gordon, J.R. Relapse Prevention; Guilford Press: New York, NY, USA, 1985. [Google Scholar]
- Marlatt, G.A.; Donovan, D.M. Relapse Prevention: Maintenance Strategies in the Treatment of Addictive Behaviors, 2nd ed.; The Guilford Press: New York, NY, USA, 2005. [Google Scholar]
- Lazarus, A.A. Technical eclecticism and multimodal therapy. In Twenty-First Century Psychotherapies: Contemporary Approaches to Theory and Practice; Lebow, J.L., Ed.; John Wiley & Sons Inc.: Hoboken, NJ, USA, 2008; pp. 424–452. [Google Scholar]
- Longabaugh, R.; Zweben, A.; Locastro, J.S.; Miller, W.R. Origins, issues and options in the development of the combined behavioral intervention. JSAD 2005, 15, 179–187. [Google Scholar] [CrossRef]
- Santa Ana, E.J.; Martino, S.; Ball, S.A.; Nich, C.; Frankforter, T.L.; Carroll, K.M. What is usual about “treatment-as-usual”? Data from two multisite effectiveness trials. J. Subst. Abuse Treat. 2008, 35, 369. [Google Scholar] [CrossRef] [PubMed]
- NIDA. Substance Use and Co-Occurring Mental Disorders. Available online: https://www.nimh.nih.gov/health/topics/substance-use-and-mental-health#:~:text=Studies%20found%20that%20people%20with,the%20symptoms%20worse%20over%20time (accessed on 10 June 2023).
- Delaney, J.A.; Nance, R.M.; Whitney, B.M.; Altice, F.L.; Dong, X.; Trejo, M.E.P.; Matsuzaki, M.; Taxman, F.S.; Chander, G.; Kuo, I.; et al. Brief Report: Reduced Use of Illicit Substances, even without Abstinence, Is Associated with Improved Depressive Symptoms among People Living with HIV. J. Acquir. Immune Defic. Syndr. 2018, 79, 283–287. [Google Scholar] [CrossRef] [PubMed]
- Woody, G.E.; McLellan, A.T.; Luborsky, L.; O’Brien, C.P. Corrections and Revised Analyses for Psychotherapy in Methadone Maintenance Patients. Arch. Gen. Psychiatry 1990, 47, 788–789. [Google Scholar] [CrossRef]
- Woody, G.E.; McLellan, A.T.; Luborsky, L.; O’Brien, C.P. Twelve-month follow-up of psychotherapy for opiate dependence. Am. J. Psychiatry 1987, 144, 590–596. [Google Scholar] [CrossRef]
- Frank, J.D.; Frank, J.B. Persuasion and Healing: A Comparative Study of Psychotherapy, 3rd ed.; JHU Press: Baltimore, MD, USA, 1993. [Google Scholar]
- Wampold, B.E. The Great Psychotherapy Debate: Models, Methods, and Findings; Lawrence Erlbaum Associates Publishers: Mahwah, NJ, USA, 2001. [Google Scholar]
- Carroll, K.M. Integrating psychotherapy and pharmacotherapy to improve drug abuse outcomes. Addict. Behav. 1997, 22, 233–245. [Google Scholar] [CrossRef]
- Ray, L.A.; Meredith, L.R.; Kiluk, B.D.; Walthers, J.; Carroll, K.M.; Magill, M. Combined Pharmacotherapy and Cognitive Behavioral Therapy for Adults with Alcohol or Substance Use Disorders: A Systematic Review and Meta-analysis. JAMA Netw. Open 2020, 3, e208279. [Google Scholar] [CrossRef]
- Elias, D.; Kleber, H.D. Minding the brain: The role of pharmacotherapy in substance-use disorder treatment. Dialogues Clin. Neurosci. 2017, 19, 289–297. [Google Scholar] [CrossRef]
- Kessler, R.C. The epidemiology of dual diagnosis. Biol. Psychiatry 2004, 56, 730–737. [Google Scholar] [CrossRef]
- Buckley, P.F. Prevalence and consequences of the dual diagnosis of substance abuse and severe mental illness. JCP 2006, 67 (Suppl. 7), 5–9. [Google Scholar]
- Han, B.; Compton, W.M.; Blanco, C.; Colpe, L.J. Prevalence, Treatment, And Unmet Treatment Needs of US Adults With Mental Health And Substance Use Disorders. Health Aff. 2017, 36, 1739–1747. [Google Scholar] [CrossRef] [PubMed]
| Reference | Substance | D1 | D2 | D3 | D4 | D5 | Overall |
|---|---|---|---|---|---|---|---|
| Gregory et al. [34] | alcohol |  |  |  |  |  |  |
| Gregory, DeLucia-Deranja and Mogle [27] | alcohol |  |  |  |  |  |  |
| Ito, Donovan and Hall [35] | alcohol |  |  |  |  |  |  |
| Nyhuis et al. [36] | alcohol |  |  |  |  |  |  |
| Sandahl et al. [37] | alcohol |  |  |  |  |  |  |
| Ojehagen et al. [38] | alcohol |  |  |  |  |  |  |
| Carroll, Rounsaville and Gawin [39] | cocaine |  |  |  |  |  |  |
| Crits-Cristoph et al. [14] | cocaine |  |  |  |  |  |  |
| Rounsaville et al. [40] | opiates |  |  |  |  |  |  |
| Shaffer, LaSalvia and Stein [17] | opiates |  |  |  |  |  |  |
| Woody et al. [41] | opiates |  |  |  |  |  |  |
| Woody et al. [19] | Opiates |  |  |  |  |  |  |
| Reference | Substance | D1 | D2 | D3 | D4 | D5 | Overall |
|---|---|---|---|---|---|---|---|
| Gregory et al. [34] | alcohol |  |  |  |  |  |  |
| Ito, Donovan and Hall [35] | alcohol |  |  |  |  |  |  |
| Ojehagen et al. [38] | alcohol |  |  |  |  |  |  |
| Gregory, DeLucia-Deranja and Mogle [27] | alcohol |  |  |  |  |  |  |
| Carroll, Rounsaville and Gawin [39] | cocaine |  |  |  |  |  |  |
| Crits-Cristoph et al. [14] | cocaine |  |  |  |  |  |  |
| Rounsaville et al. [40] | opiates |  |  |  |  |  |  |
| Shaffer, LaSalvia and Stein [17] | opiates |  |  |  |  |  |  |
| Woody et al. [19] | opiates |  |  |  |  |  |  |
| Reference | Substance | D1 | D2 | D3 | D4 | D5 | Overall |
|---|---|---|---|---|---|---|---|
| Gregory et al. [34] | alcohol |  |  |  |  |  |  |
| Gregory, DeLucia-Deranja and Mogle [27] | alcohol |  |  |  |  |  |  |
| Hoyer et al. [42] | alcohol |  |  |  |  |  |  |
| Ito, Donovan and Hall [35] | alcohol |  |  |  |  |  |  |
| Sandahl et al. [37] | alcohol |  |  |  |  |  |  |
| Gregory et al. [27] | alcohol |  |  |  |  |  |  |
| Carroll, Rounsaville and Gawin [39] | cocaine |  |  |  |  |  |  |
| Crits-Christoph et al. [14] | cocaine |  |  |  |  |  |  |
| Rounsaville et al. [36] | opiates |  |  |  |  |  |  |
| Woody et al. [41] | opiates |  |  |  |  |  |  |
| Woody et al. [19] | opiates |  |  |  |  |  |  |
| Outcome | Q-Value | Df (Q) | p-Value | I-Squared |
|---|---|---|---|---|
| Substance use | 10.10 | 5.00 | 0.07 | 50.52 |
| Participation | 0.46 | 3.00 | 0.92 | 0.00 |
| Other symptomatic conditions | 1.16 | 3.00 | 0.76 | 0.00 |
| Outcome | Q-value | Df (Q) | p-Value | I-Squared |
|---|---|---|---|---|
| Substance use | 1.667 | 1.00 | 0.196 | 40.015 |
| Participation | 4.581 | 1.00 | 0.032 | 78.172 |
| Outcome | Q-Value | Df (Q) | p-Value | I-Squared |
|---|---|---|---|---|
| Substance use | 8.867 | 3.00 | 0.031 | 66.168 |
| Participation | 1.014 | 2.00 | 0.602 | 0.00 |
| Other symptomatic conditions | 0.206 | 1.00 | 0.649 | 0.00 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zuccon, M.; Topino, E.; Musetti, A.; Gori, A. Psychodynamic Therapies for the Treatment of Substance Addictions: A PRISMA Meta-Analysis. J. Pers. Med. 2023, 13, 1469. https://doi.org/10.3390/jpm13101469
Zuccon M, Topino E, Musetti A, Gori A. Psychodynamic Therapies for the Treatment of Substance Addictions: A PRISMA Meta-Analysis. Journal of Personalized Medicine. 2023; 13(10):1469. https://doi.org/10.3390/jpm13101469
Chicago/Turabian StyleZuccon, Marco, Eleonora Topino, Alessandro Musetti, and Alessio Gori. 2023. "Psychodynamic Therapies for the Treatment of Substance Addictions: A PRISMA Meta-Analysis" Journal of Personalized Medicine 13, no. 10: 1469. https://doi.org/10.3390/jpm13101469
APA StyleZuccon, M., Topino, E., Musetti, A., & Gori, A. (2023). Psychodynamic Therapies for the Treatment of Substance Addictions: A PRISMA Meta-Analysis. Journal of Personalized Medicine, 13(10), 1469. https://doi.org/10.3390/jpm13101469








